Osteoporosis is often referred to as a ‘silent disease’, a description which alludes to its slow, steady but undetected development during adulthood and older age as the balance between bone formation and resorption shifts in favour of resorption. Acquisition of peak bone mass during the first three decades and the subsequent retention of bone through middle age are important determinants for reducing the risk of osteoporosisReference Martin, Coviak, Gendler, Kim, Cooper and Rodrigues-Fisher1. Yet osteoporosis is regarded as a disease of old age and thus a distant threat to those at the age when preventive behaviour is most effective. Also, the disease is essentially incurableReference Sato, Grese, Dodge, Bryant and Turner2, Reference Follin and Hansen3 and so a preventive public health approach is required. The challenge for osteoporosis prevention programmes is to promote early identification of risk factors and encourage the adoption of risk-reducing behaviours in women from adolescence to premenopause.
Role of knowledge and health belief in the prevention of osteoporosis
The influence of nutrition knowledge on healthy eating has been the subject of many studies over the past two decades. Most authors conclude that whilst behaviours are unlikely to change without an increase in knowledge, knowledge alone is insufficient to bring about significant improvement in preventive behaviourReference Wardle, Parmenter and Waller4, Reference Worsley5. Knowledge can, however, influence health-related behaviours when mediated by attitudes, beliefs, self-efficacy and an effective call to actionReference Green and Kreuter6.
Previous studies investigating osteoporosis knowledge amongst women from adolescence to postmenopause, in countries including TurkeyReference Ungan and Tümer7, AustraliaReference Winzenberg, Oldenburg, Frendin and Jones8, SingaporeReference Saw, Hong, Lee, Wong, Chan and Cheng9 and the USAReference Martin, Coviak, Gendler, Kim, Cooper and Rodrigues-Fisher1, Reference Terrio and Auld10–Reference Ailinger and Emerson12, have revealed a number of commonalities. Although awareness of the existence of the disease is relatively high, knowledge about prevention, treatment and the severity of its consequences is poor. Also common to these studies is an awareness of the importance of calcium intake and physical activity, but poor knowledge of other risk factors such as hormonal changes, smoking, vitamin D deficiency and ethnicity. This apparent lack of understanding about the severity of osteoporosis, coupled with poor knowledge of preventive behaviours, suggests that women are unlikely to be taking action to reduce their risk of developing osteoporosis.
The Health Belief Model (HBM) has been used as a conceptual framework to help explain why some individuals choose to engage in health-promoting behaviours and some do notReference Green and Kreuter6. The HBM suggests that health behaviours are associated with certain beliefs, and postulates that an individual will make behavioural changes for the benefit of their health if they have a perceived personal susceptibility to the disease, belief in the seriousness of the disease, belief in the effectiveness of recommended preventive behaviours, belief that the advantages of such behaviours outweigh the costs, and the motivation to engage in health-promoting behavioursReference Janz and Becker13.
It has been reported that whilst an education programme focusing on osteoporosis increased knowledge, there was no change in health beliefs or osteoporosis-preventing behaviourReference Sedlak, Doheny and Jones11. This suggests that greater emphasis should be placed on health belief in future prevention programmes.
However, Turner et al. demonstrated a positive behavioural change using an intervention designed to address both health beliefs and knowledgeReference Turner, Hunt, DiBrezzo and Jones14. Subjects were given powerful demonstrations of the severity of osteoporosis (disability and death) and a total-body dual X-ray densitometry test which increased perceived susceptibility in many participants. The programme resulted in increased perceived susceptibility and seriousness of the disease. A follow-up study demonstrated that many participants had either made behavioural changes or were intending to do soReference Turner, Wallace, Hunt and Gray15. Similarly, Tussing et al. designed an osteoporosis prevention programme based on the HBM and the Theory of Reasoned Action, incorporating components specifically designed to increase awareness of the severity of the disease and perceived susceptibilityReference Tussing and Chapman-Novakofski16. Post-intervention testing demonstrated increases in perceived susceptibility and calcium intake.
Perceived barriers to risk-reducing behaviour and perceived susceptibility to the disease appear to be the most powerful HBM components in terms of bringing about behavioural changeReference Janz and Becker13, Reference Abood, Black and Feral17. It is arguable that health promotion programmes which address only knowledge and ignore health beliefs such as perceived susceptibility will fail to initiate an appreciable increase in risk-reducing behaviours in their target audience.
An understanding of the knowledge and attitudes that young and middle-aged women have about osteoporosis is essential for the development and delivery of effective health promotion programmes. Therefore, the objective of the present study was to investigate women's knowledge about osteoporosis risk factors, their beliefs about susceptibility to developing the disease and their attitudes towards preventive behaviours. It is likely that age may be a predictive factor in the outcome of women's knowledge, beliefs and attitudes.
Subjects and methods
Participants in this study were women aged between 20 and 49 years living in Auckland, New Zealand. Geographic locality was limited in an attempt to control for differences between urban and rural populations, which might influence access to the Internet, attitudes to health, calcium intake and level of physical activity. Additionally, previous studies have shown substantial, but unexplained, regional differences in hip fracture rates among older peopleReference Norton, Yee, Rodgers, Gray and MacMahon18.
Subjects were invited to participate in a web-based survey by email letter. The letter was sent to an initial group of 52 women known to the researcher, inviting them to (1) participate in the study and (2) send the letter on to any other women who fulfilled the criteria. As one aim of the study was to compare knowledge and health beliefs across different age groups, the respondents were divided into three age groups (Table 1). Education was measured in number of years from age five. In New Zealand, 16 years of education usually equates to a bachelor's degree or the equivalent.
Table 1 Age and education characteristics of subjects
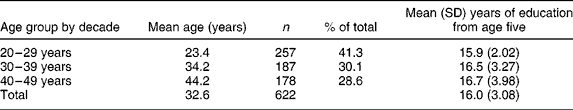
SD – standard deviation.
The questionnaire
The web-based questionnaire was completed on-line, and responses were captured by a database on the website. It consisted of two individual instruments, the Osteoporosis Knowledge Test (OKT) and the Osteoporosis Health Belief Scale (OHBS), both developed by Kim et al. Reference Kim, Horan and Gendler19. The instruments are subject to copyright and were used with permission of the developers. Responses could not be submitted if incomplete.
The OKT is a 26-item questionnaire of multiple-choice questions which assess knowledge about osteoporosis prevention and risk including dietary intake and sources of calcium, level and type of physical activity, hormonal status, heredity and ethnicity. The OKT was modified by the researcher to include two questions on vitamin D. There is only one correct answer for each question and the maximum score for the OKT is 26. Mean total scores were compared for the three age groups, as were the mean scores for individual questions.
The OHBS measures health beliefs related to osteoporosis and comprises 42 response items, each rated by the subject on a standard Likert scale of 1 (strongly disagree) to 5 (strongly agree). The scale is divided into seven subscales: perceived susceptibility, perceived seriousness of the disease, barriers to preventive behaviours (calcium intake and exercise), benefits of preventive behaviours (calcium intake and exercise), and health motivation. The internal reliability coefficients ranged from 0.61 to 0.80Reference Kim, Horan, Gendler and Patel20.
Tables 3–6 show the responses for disagree and strongly disagree, and agree and strongly agree, which were combined for the sake of clarity.
Statistical analysis
Data from the OKT and OHBS were assessed for normality with normal Q–Q plots and de-trended Q–Q plots. The distribution of most variables was appreciably normal, therefore parametric tests were used. For variables with some skewness, confirmatory non-parametric tests were performed.
Differences between age groups were studied using one-way analyses of variance. Univariate linear regression analysis was used to study the predictive effect of attitudinal and knowledge factors.
Central tendencies are reported as mean (standard deviation, SD). Differences with P < 0.05 were considered significant. Data management and analysis were performed using SPSS for Windows, release 13.0 (2004; SPSS Inc.).
Results
Subjects
A total of 622 women aged 20–49 years completed the on-line questionnaire. The majority of women were New Zealand European (82%) and 6% were Asian, which is similar to the ethnic distribution in Auckland21. New Zealand Maori (4%) and Pacific (1%) women were under-represented. Fifty-nine per cent of the women held an undergraduate degree or equivalent, compared with 13% of the Auckland population21.
Osteoporosis knowledge
The OKT has a maximum possible score of 26. Responses to the OKT, stratified by age, are presented in Table 2. There was a significant difference in mean scores by age group (P = 0.001), with the younger women (20–29 years) demonstrating the lowest level of knowledge (mean score 15.8 (SD 3.9)) and the older women (40–49 years) the highest (mean score 17.3 (SD 4.0)). The mean total score for all subjects was 16.4 (SD 4.0) or 63%. A weak correlation (r = 0.121, P = 0.002, n = 622) was found between OKT total scores and years of education.
Table 2 Responses to the Osteoporosis Knowledge Test stratified by age

† Figures represent within-group % of correct responses.
Statistically significant difference between age groups: *P = 0.019, **P = 0.009, ***P < 0.001.
Health beliefs about osteoporosis
Health beliefs about osteoporosis were determined by responses to the seven subscales of the OHBS, as listed below.
Perceived susceptibility
No significant difference was found between the age groups in this subscale. Overall, perceived susceptibility was low, with 28.6% of women agreeing that their chances of getting osteoporosis are high and 10.6% believing that they are extremely likely to get the disease. Twenty-one per cent considered that their family history makes them more likely to get osteoporosis.
Perceived seriousness
There was no significant effect of age on perceived seriousness. Although 64% of women agreed that it would be serious if they got osteoporosis, only 22.5% considered it to be a crippling disease.
Attitudes towards osteoporosis-preventing behaviours
Belief in the benefits of exercise and calcium intake for the prevention of osteoporosis was strong across all age groups (Tables 3 and 4) and no significant difference between ages was detected.
Table 3 Subjects' responses to statements on benefits of exercise
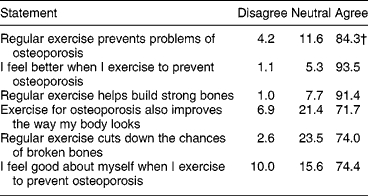
† Figures represent % of total.
Table 4 Subjects' responses to statements on benefits of calcium intake
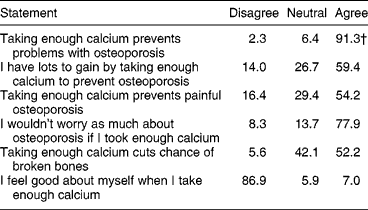
† Figures represent % of total.
There was a statistically significant difference across the age groups in the responses to the ‘Barriers to Exercise’ section of the OHBS. Responses from all subjects are reported in Table 5. Younger women (20–29 years) reported the most barriers to exercise, and the older age group (40–49 years) reported the least barriers to exercise (P < 0.001). The attitude of a spouse or other family member to exercise was the strongest demotivator in the group overall (23% of subjects). However, there was a strong effect of age with younger women (20–29 years) being particularly influenced.
Table 5 Subjects' responses to statements on barriers to exercise
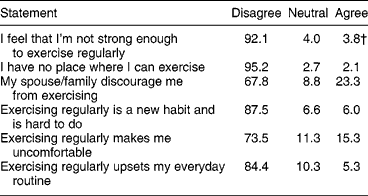
† Figures represent % of total.
Overall, perceived barriers to calcium intake were unaffected by age, and results are presented in Table 6. However, 77.2% of subjects agreed that calcium-rich foods have too much cholesterol, and there was a significant difference in response by age group with older women (40–49 years) more likely to agree with the statement (P = 0.002, data not shown).
Table 6 Subjects' responses to statements on barriers to calcium
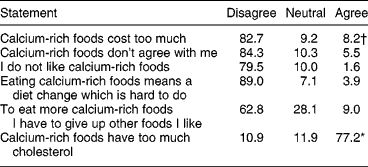
† Figures represent % of total.
Significant difference across age groups: *P = 0.002.
A significant inverse correlation was found between belief in the statement that calcium-rich foods have too much cholesterol and the following item in ‘Benefits of Calcium’: ‘I feel good about myself when I take enough calcium’ (r = − 0.295, P < 0.001, n = 622).
Health motivation
An analysis of the six OHBS questions about health motivation demonstrated that older women (40–49 years) were more highly motivated to take care of their health than younger women (20–29 years) (P < 0.001). Univariate linear regression analyses showed the OHBS subscales ‘Benefits of Exercise’ and ‘Benefits of Calcium’ were significant predictors of ‘Health Motivation’ (P < 0.001), and ‘Barriers to Calcium’ and ‘Barriers to Exercise’ were significant negative predictors of ‘Health Motivation’ (P < 0.001). There was no significant relationship between ‘Health Motivation’ and OHBS ‘Seriousness’, and a weak, inverse correlation between ‘Health Motivation’ and OHBS ‘Susceptibility’ (r = − 0.08, P = 0.049, n = 622).
Discussion
The goal of this study was to gather baseline information on the knowledge levels of premenopausal women about osteoporosis, their attitudes towards the disease, and their beliefs and barriers to the readily identified preventive behaviours of physical activity and calcium intake. It was hypothesised that as women approached menopause their knowledge and concern about the disease would increase. This, however, was not the case. Although there was a small, significant increase in knowledge with increasing age, perceptions of personal susceptibility and seriousness were unaffected.
Osteoporosis knowledge
The total osteoporosis knowledge score was lower than expected in this group of well-educated women. The mean total score for knowledge achieved by all subjects, out of a possible score of 26, was 16.4 or 63%. Other studies utilising the OKT or similar instruments have also reported poor to moderate levels of knowledge, with mean total scores between 63% and 74%Reference Sedlak, Doheny and Jones11, Reference Kim, Horan and Gendler19, Reference Werner22. These studies found, as did we, that whilst women had a good level of knowledge about the importance of calcium and physical activity for the prevention of osteoporosis, they were less aware of other factors that increase risk such as hormonal status and taking steroids.
In this study knowledge about osteoporosis increased with increasing age. In particular, the 40–49-year-old women demonstrated greater knowledge about the risks of being menopausal and having an ovariectomy. It is likely that older women become more aware of the implications of hormonal change as they approach menopause. However, as there was no correlation between knowledge of hormonal effects on bone health and feelings of personal susceptibility to osteoporosis, older women did not consider that hormonal changes put them at greater risk of developing the disease.
The subjects were aware that dairy products are a good source of calcium, but were less knowledgeable of other sources such as vegetables or sardines. There was low awareness of the recommended daily intake (RDI) for calcium and how much milk was required to meet the RDI. Fewer than 50% of subjects were able to accurately answer the two questions on vitamin D. As there is no routine fortification of food with vitamin D in New Zealand and dietary sources are negligible, sunlight remains an important source of vitamin D. In light of the growing awareness of vitamin D deficiency in New Zealand23–Reference Skeaff and Green25, it is important that this lack of knowledge is addressed. Women need to be made aware that vitamin D is essential for the absorption of calcium, that short periods of exposure to the sun is sufficient for vitamin D synthesis, and that if they choose to remain completely protected from the sun, the vitamin must be obtained from other sources.
Health beliefs
Perceptions of personal susceptibility and belief in the seriousness of a disease are important for influencing behavioural change in disease prevention programmesReference Janz and Becker13. Over two-thirds of the subjects did not consider themselves susceptible to developing osteoporosis and increasing age had no influence on this response. Given estimates from New Zealand (Osteoporosis NZ, personal communication, May 2005), BritainReference Burns, Ashwell, Berry, Bolton-Smith, Cassidy and Dunnigan26 and the USA27 that more than 50% of women over the age of 50 years will develop osteoporosis in their lifetime, this group of women are generally very optimistic about their chances of avoiding the disease. Levels of perceived personal susceptibility as low as 29% have been reported previouslyReference Hsieh, Novielli, Diamond and Cheruva28. There was a higher level of agreement about the seriousness of osteoporosis, but less than a quarter of the subjects regarded osteoporosis as a crippling disease. These attitudes suggest there is an opportunity to improve the effectiveness of future osteoporosis prevention programmes. Initiatives which increase perceived personal susceptibility have been shown to be beneficialReference Turner, Wallace, Hunt and Gray15.
Generally the subjects reported few barriers to exercise and calcium intake. However, the 77% agreement with the statement ‘Calcium-rich foods have too much cholesterol’ suggests that advertising by dairy marketers has not been successful in promoting the range of low-fat/low-cholesterol products available.
Although there was strong agreement with most of the ‘Benefits of Calcium’ items, only 7% of subjects agreed with the statement ‘I feel good about myself when I take enough calcium’. A significant negative correlation was found between this statement and the item ‘Calcium-rich foods have too much cholesterol’. This further emphasises the need to communicate the availability of low-fat/low-cholesterol dairy products. More importantly, these two responses raise questions about the actual calcium intake of these women (not measured in this study), which potentially could be much lower than suggested by the reported strong belief in the benefits of, and lack of barriers to, the intake of calcium.
The subjects demonstrated a high level of health motivation, and there was a trend towards increasing participation in preventive health care with advancing age. A significant correlation was found between knowledge and health motivation, and belief in the benefits of calcium and exercise for the prevention of osteoporosis was highly predictive of health motivation scores. Conversely, those subjects with high levels of health motivation reported low barriers to exercise and to consumption of calcium-containing foods.
Limitations of the study
The subjects in this study were not representative of New Zealand women aged 20–49 years. This was an opportunistic sample of women who reported high levels of education. Recruitment was self-selecting. The number of women who were invited to participate in the web-based survey and the number of women who declined to participate were not ascertained.
Conclusion
This group of well-educated New Zealand women did not demonstrate a high level of knowledge about osteoporosis. Increasing age was predictive of a better level of knowledge, particularly in questions related to the impact of hormonal changes on bone. Perceived personal susceptibility to osteoporosis was low, concurring with the results of other studies. Despite these findings, the majority of subjects were highly motivated to take care of their health, and belief in the benefits of calcium and exercise were strongly predictive of health motivation.
One unexpected finding was the high proportion of subjects who considered calcium-rich foods to contain a lot of cholesterol. This suggests that the benefits of low-fat dairy products are not well understood, especially by the older women. This is an important item to be addressed in any health promotion programme and is worthy of further investigation.
Considering the fact that the women in this study reported educational attainment well above the national average, there is a question about the knowledge of osteoporosis prevention in less-educated women.
This study has provided valuable insight into the knowledge and attitudes of women about osteoporosis. It identifies areas where further research would provide a more comprehensive picture. Such information will be critical to the future development of effective health promotion programmes for the prevention of osteoporosis. An investigation into the OHBS constructs of benefits and barriers and how they relate to actual preventive behaviours would be particularly enlightening.
Acknowledgements
Sources of funding: No funding was sought for this study.
Conflict of interest declaration: There are no conflicts of interest.
Authorship responsibilities: P.v.H. designed and managed the study; both authors contributed to the writing of this paper.
Acknowledgements: The authors would like to acknowledge the contribution of Dmitri Roukin (IFNHH, Massey University, Auckland) in the designing and building of the website used for this study.








