Racial and ethnic minority and low-income children are disproportionately affected by childhood obesity, which increases the risk of CVD throughout the lifespan and thereby life-long disparities in morbidity and mortality( Reference Ogden, Carroll and Kit 1 – 3 ). Disparities in childhood obesity may be increasing despite increased prevention and treatment efforts and a levelling off of overall childhood obesity rates( Reference Ogden, Carroll and Kit 1 ). It is critical to improve our understanding of modifiable risk factors of paediatric obesity.
Latino children have among the highest rates of early childhood overweight and obesity of any racial or ethnic group in the USA( Reference May, Freedman and Sherry 4 , Reference Ogden, Carroll and Kit 5 ). In a national cross-sectional sample, 26 % of Latino children were obese at 3 years of age in comparison to 14·8 % of Whites and 16·2 % of Blacks( Reference Ogden, Carroll and Kit 5 ). Low income is a strong independent risk factor for childhood obesity and may compound the risk of obesity for many Latino children, who are over-represented among low-income children in the USA( Reference May, Freedman and Sherry 4 , Reference Lee, Andrew and Gebremariam 6 – Reference Zilanawala, Nazroo and Sacker 8 ).
Abnormal acceleration in growth during early childhood, including infancy, has been shown to increase the likelihood of obesity later in childhood as well as in adolescence( Reference Baird, Fisher and Lucas 9 – Reference Taveras, Rifas-Shiman and Belfort 13 ). Factors operating as early as infancy and that affect growth trajectories may contribute significantly to disparities in early childhood obesity( Reference Baird, Fisher and Lucas 9 , Reference Taveras, Rifas-Shiman and Oken 14 – Reference Monteiro and Victora 16 ). For example, adjusting for infancy and early-life risk factors significantly attenuated the finding that Latinos were more likely than non-Latino Whites to be obese at age 7 years( Reference Taveras, Gillman and Kleinman 17 ). In a national sample, higher odds of obesity at age 5 years for Mexican-American children compared with non-Hispanic White children were no longer seen after adjusting for sociodemographic markers( Reference Zilanawala, Nazroo and Sacker 8 ). Yet, comprehensive data specifically examining growth trajectories of low-income Latinos are lacking despite clear epidemiological evidence that this population experiences significant disparities in obesity later in life.
Obesity prevention interventions that include infants and toddlers are lacking. Modifiable risk factors for early infant weight gain include exclusivity and duration of breast-feeding, feeding practices and infant sleep( Reference Taveras, Gillman and Kleinman 17 , Reference Mihrshahi, Battistutta and Magarey 18 ). In a 2014 systematic review( Reference Laws, Campbell and van der Pligt 19 ) of obesity prevention interventions for socio-economically disadvantaged children, Laws et al. identified fourteen published reports of interventions focused on children less than 12 months old of which one reported a reduced risk of obesity. Laws et al. also identified five published reports of interventions that included children between the ages of 1 and 2 years of which three showed an improvement in obesity-related behaviours or practices, but none reported an impact on childhood obesity.
Specific guidelines or tools, such as BMI for children older than 2 years, to identify children younger than 2 years at high risk of obesity are needed for use in paediatric primary care. Identification of infants and toddlers at high risk of obesity would facilitate paediatric clinicians’ efforts to provide targeted and appropriate behavioural counselling to parents aimed at obesity prevention. Paediatric primary-care interventions targeting modifiable risk factors for excess weight gain among infants and toddlers should be tested simultaneous with efforts to more fully understand antecedents of rapid weight gain and early childhood obesity.
The goal of the present study was to examine early growth trajectories in a population that is both under-represented in the literature and at especially high risk for childhood obesity: low-income Latino and non-Latino patients. In 2003, the year of participants’ birth, Medicaid was available in Maryland for children of families living at or below 200 % of the federal poverty limit, an annual household income of $US 36 800 for a family of four( 20 , 21 ). The specific aims were to examine: (i) the association between Latino ethnicity and change in weight-for-length Z-score (WLZ) during infancy (i.e. in first 2 years of life); and (ii) the relationship between change in WLZ during infancy and BMI Z-score (BMIZ) at age 3 years. Study hypotheses were: (i) low-income Latino 3-year-olds will be more likely to be obese (BMI>95th percentile) than low-income non-Latinos; and (ii) WLZ between birth and 2 years will be positively associated with obesity at age 3 years.
Methods
Study setting
The Children’s Medical Practice (CMP) is an urban, academic general paediatric practice. Almost all patients, regardless of ethnicity, are publicly insured. The majority of patients are Latino children of parents recently immigrated from Mexico or Central America with limited English proficiency. Approximately half of the clinic’s Latino patients’ parents are of Mexican origin. Many Latino parents of CMP patients have limited health literacy in addition to limited English proficiency, defined as speaking English other than very well( Reference Ryan 22 ). In a cross-sectional survey of forty-nine, randomly selected, immigrant Latino CMP patients’ parents with limited English proficiency and whose preferred health-care language was Spanish, the mean score on the Spanish Parental Health Literacy Activities Test was 41 %, indicating marginal health literacy (LR DeCamp, personal communication, March 2015).
Procedures
This study was a retrospective cohort study of 0–4-year-old, low-income, Latino and non-Latino CMP patients. Inclusion criteria were: (i) date of birth in calendar year 2003; (ii) insured by Medicaid or the State Children’s Health Insurance Program; (iii) first clinic visit by 4 months of age; and (iv) at least one clinic visit between the ages of 3 and 4 years. Sample size calculations were based upon the power to detect an 11 % difference in obesity prevalence at 3 years of age in Latino v. non-Latino children with 80 % power and a significance level of 5 %.
Weight and height measurements from all visits between birth and 4 years were extracted from both paper and electronic medical records. One of the authors (S.P.) conducted the record review with assistance from two research assistants. The author (S.P.) double-reviewed 10 % of each research assistant’s charts as a quality control measure and adjudicated all questions during the record review. Premature infants were excluded.
Participant measures
Demographics
Parents reported their child’s race, ethnicity, Latino or non-Latino, and sex when establishing care at the CMP. Data on race are available for non-Latinos only as race and ethnicity were asked with a single question and were thereby mutually exclusive. Clinic staff verified insurance at each clinic visit and only patients insured through Medicaid or the State Children’s Health Insurance Program were included in the study. Date of birth and date of each visit were extracted from the record and used to calculate age at visit.
Anthropometric measurements
Clinical staff recorded all measurements. Body weight was measured to the nearest 0·1 kg on a digital scale. From birth to 24 months, infants were weighed naked on a digital scale (UMF Medical 5900). Subsequently, children were weighed standing in light clothes but no shoes (Seca). Body height was measured to the nearest 0·1 cm. From birth to 24 months, infants were measured while supine using a measuring tape. Subsequently, children were measured with their shoes off using a wall-attached stadiometer.
Standardized anthropometric measurements
Weights were standardized according to height, sex and age as WLZ. WLZ for a healthy child is expected to be zero. WLZ less than zero indicates that a child weighs less than expected for his/her given height and conversely a WLZ greater than zero indicates that a child weighs more than expected for his/her given height. A change over time in WLZ of zero indicates consistent growth in weight and height, regardless of the starting WLZ( 23 ). An increase in WLZ indicates a greater than expected increase in weight given the change in height. WLZ was standardized according to the 2000 Centers for Disease Control and Prevention (CDC) Growth Reference( Reference Kuczmarski, Ogden and Grummer-Strawn 24 ).
BMI, a measure of adiposity, was calculated by dividing weight (kg) by height squared (m2), using measurements from the visit closest to age 3 years and prior to age 4 years. Children with a BMI greater than the 95th percentile for their age and sex are classified as obese, while those with a BMI between the 85th and 95th percentile are considered overweight. In order to ease interpretation and enhance the meaning of the inferences, we converted the BMI to a sex- and age-specific standardized Z-score (BMIZ) according to the 2000 CDC Growth Charts( Reference Kuczmarski, Ogden and Grummer-Strawn 24 , Reference Inokuchi, Matsuo and Takayama 25 ). Analyses are stratified by ethnicity according to study aims and by sex in keeping with standardized anthropometric measurement tools.
Statistical analysis
In order to characterize their growth trajectory, a series of statistical models was applied to the children’s height and weight data. First, we performed a longitudinal analysis of each individual’s growth, using WLZ, from birth to age 2 years using a mixed-effects model. A mixed-effects model consists of two components, fixed effects and random effects. The fixed-effects component of the model describes the growth curve for the entire sample. The random-effects component of the model describes each child’s deviation from the sample’s growth curve. A desired feature of the mixed-effects model is that it allows for the use of all available data, serial measures within individuals which vary by individual in quantity and timing( Reference Fitzmaurice, Laird and Ware 26 ). A major advantage of mixed-effects models is the ability to derive estimates of the individual’s WLZ at birth (intercept) and change in WLZ (slope) from a weighted average of each child’s data and the population average which not only serve as descriptors of the growth in the first 2 years of life but also allows for their use as refined exposures to predict the obesity of the children at age 3 years( Reference Johnson, Balakrishna and Griffiths 27 ).
At the second stage of the analysis, we examined the relationship between change in WLZ from birth to age 2 years and BMIZ at age 3 years using multivariate linear regression. The primary exposure measurements are WLZ at birth and change in WLZ: individual intercept and slope, respectively, estimated during the first phase of analysis. The primary null hypothesis was that the rate of change of the WLZ during the first 2 years of life, hereafter referred to as ‘change in WLZ’, does not predict BMIZ at age 3 years.
Results
Results supported our study hypotheses that: (i) low-income Latino 3-year-olds will be more likely to be obese (BMI>95th percentile) than low-income non-Latinos; and (ii) WLZ between birth and 2 years will be positively associated with obesity at age 3 years.
Characteristics of the sample at birth
The study sample consisted of 210 Latino and 253 non-Latino patients of the CMP with approximately equal representation of males and females. Of non-Latino children, 51·4 % were African American and 38·4 % were White. On each of these children we had repeated WLZ measures during the first 2 years of life to characterize their trajectories. At birth, weight and length were available for 152 (72 %) Latino and 145 (57 %) non-Latino participants. Mean birth weight for the entire cohort was 3·38 kg (range 2·14–4·74 kg). Mean length at birth of the cohort was 51·40 cm (range 36·50–58·00 cm). WLZ at birth was slightly less than zero for all four sex- and ethnicity-based groups (Table 1). There was no significant difference in observed birth weight, birth length or WLZ at birth by sex or ethnicity (Table 1).
Table 1 Descriptive statistics at birth of a retrospective cohort of low-income, non-Latino and Latino children born in 2003–2004 in Baltimore, MD, USA

WLZ, weight-for-length Z-score.
Growth from birth to 2 years
Table 2 shows that WLZ increased with age for all groups. For non-Latino boys, mean WLZ increased from −0·38 (sd 1·22) between birth and 0·5 years of age to 0·0 (sd 1·31) between the ages of 1·5 and 2·0 years. In comparison, for Latino boys mean WLZ exceeded zero between birth and 0·5 years of age (0·10 (sd 1·14)) and increased to 0·34 (sd 1·30) by between 1·5 and 2·0 years of age. Non-Latino and Latino girls had mean WLZ less than zero between birth and 0·5 years (−0·25 (sd 1·22) and −0·20 (sd 1·04), respectively) that subsequently increased with age.
Table 2 Weight gain from birth to 2 years and BMI between 2·5 and 4 years in a retrospective cohort of low-income, non-Latino and Latino children born in 2003–2004 in Baltimore, MD, USA
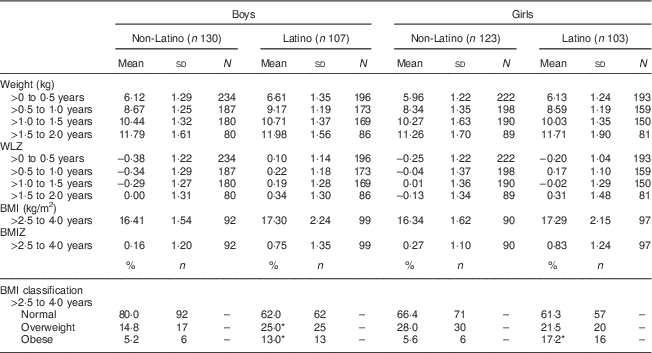
n, number of children; N, number of observations; WLZ, weight-for-length Z-score; BMIZ, BMI Z-score.
*Latino boys and girls had a significantly higher proportion of overweight/obesity than non-Latino boys and girls: P<0·05.
BMI at 3 years
Latino children had a higher incidence of early childhood obesity than non-Latino children in this low-income sample. Table 2 also shows that all groups had a high incidence of overweight (range according to ethnicity and sex 14·8–28·0 %) and obesity (range 5·2–17·2 %) between 2·5 and 4 years of age. Latino boys were significantly more likely to be overweight (25·0 %) or obese (13·0 %) than non-Latino boys (14·8 % and 5·2 %, respectively). Latino girls were significantly more likely to be obese (17·2 %) than non-Latino girls (5·6 %).
Weight-for-length Z-score at birth: mixed-effects model results
Results of the application of the mixed-effects model are shown in Table 3. Specifically, based on the data of each child and the average trajectory for each of the four groups according to sex and ethnicity (non-Latino, Latino), we derived the expected WLZ at birth and the change of WLZ from birth to 2 years using standard methods (e.g. empirical Bayes or best linear unbiased predictor)( Reference Wang and Chen 28 ). All groups had a WLZ of less than zero at birth. Latino boys had a significantly higher (P=0·028) WLZ at birth than non-Latino boys (−0·47 and −0·74, respectively). There was no significant difference in WLZ at birth for Latino and non-Latino girls.
Table 3 WLZ at birth and change in WLZ (estimate and 95 % CI) from birth to 2 years derived using a mixed-effects model to analyse data from a retrospective cohort of low-income, non-Latino and Latino children born in 2003–2004 in Baltimore, MD, USA

WLZ, weight-for-length Z-score; n, number of children; N, number of observations.
*Latino boys had a significantly higher WLZ at birth than non-Latino boys: P=0·028.
Change in weight-for-length Z-score: mixed-effects model results
Table 3 also shows that for all groups within this cohort the change in WLZ exceeded zero. A WLZ of zero signifies an optimal relationship between height and weight and indicates that a child is growing at the 50th percentile. A change in WLZ of zero occurs when a child maintains a constant relationship between height and weight as he/she grows; negative values for change in WLZ correspond to a relative decrease in weight-for-height and positive values for change in WLZ to a relative increase in weight-for-height. Change in WLZ was significantly greater than zero for all groups, indicating an increase in weight-for-height over time. Change in WLZ did not differ significantly by ethnicity, although for both sexes the Latino children had greater WLZ increases than the non-Latinos.
BMI Z-score at 3 years according to weight-for-length Z-score at birth and change in weight-for-length Z-score
Table 4 provides the results of using a multivariate linear regression model to assess the association between WLZ at birth, change in WLZ from birth to 2 years and BMIZ at age 3 years. BMIZ at 3 years was available for 55 % (=72/130), 64 % (=69/107), 61 % (=75/123) and 68 % (=70/103) of non-Latino boys, Latino boys, non-Latino girls and Latino girls, respectively.
Table 4 Multivariate linear regression results (coefficient and 95 % CI) for the relationship between predicted WLZ at birth and change in WLZ from birth to 2 years with the outcome of BMIZ at 3 years from a retrospective cohort of low-income, non-Latino and Latino children born in 2003–2004 in Baltimore, MD, USA

WLZ, weight-for-length Z-score; BMIZ, BMI Z-score; n, number of children.
† Corresponds to predicted BMIZ at 3 years if both WLZ at birth and change in WLZ from birth to 2 years are equal to zero.
In the models presented in Table 4, the intercept represents the predicted BMIZ for individuals for whom WLZ at birth and change in WLZ were both zero (i.e. children with both a weight-for-length at birth and a change in WLZ at the 50th percentile). For the four groups the 95 % CI of the intercept contains zero, supporting the validity of the model whereby a birth weight at the median and normal growth from birth to 2 years results in a BMIZ in the normal range at 3 years of age. A BMIZ>1 corresponds with overweight and a BMIZ>2 corresponds with obesity( Reference Wang and Chen 28 ). In all subgroups both the WLZ at birth and the change in WLZ from birth to 2 years were significantly and positively associated with an increase in BMIZ at 3 years of age. Notably, the magnitude of the effect of the change in WLZ on BMIZ at 3 years was twofold higher than that of WLZ at birth. For example, for Latino boys a one-unit increase in change in WLZ would be expected to increase the BMIZ by 1·78 (95 % CI 1·17, 2·39), while a one-unit increase in WLZ at birth would be expected to increase the BMIZ by 0·76 (95 % CI 0·49, 1·02).
Discussion
The results presented herein build upon previous findings that accelerated growth during the first years of life increases the risk of early childhood obesity. Latino ethnicity is a risk factor for early childhood obesity in this sample of low-income children. These findings suggest that efforts to prevent childhood obesity should begin in infancy and target those at highest risk of future obesity. There are well-documented prenatal risk factors for early childhood obesity, such as maternal obesity and maternal gestational weight gain, but often it is not practical to intervene prenatally( Reference Kaar, Crume and Brinton 29 ). Low-income mothers may not have reliable access to health care for themselves, although they do have access to routine care for their children via Medicaid and the State Children’s Health Insurance Program. While the full impact of the Affordable Care Act on health-care access remains to be seen, benefits do not extend to all adults, including many low-income, immigrant Latino women such as those whose children comprised a large proportion of the cohort for the present study. Routine paediatric care during infancy involves frequent preventive care visits during the first 2 years of life. Future efforts should include the development and testing of tools, specifically risk assessment tools, to guide clinicians’ discussions of practices that promote healthy growth. It is critical to capitalize on clinical encounters during infancy for all children, but especially those most at risk of future obesity such as low-income, Latino and non-Latino children.
Modifiable risk factors for the observed disparity in early childhood obesity in Latino children include non-exclusive breast-feeding, consumption of sugar-sweetened beverages and quantities of both screen time and sleep( Reference Taveras, Rifas-Shiman and Oken 14 , Reference Taveras, Gillman and Kleinman 17 , Reference Taveras, Gillman and Kleinman 30 – Reference Huh, Rifas-Shiman and Taveras 33 ). Culture is integral to health behaviours including diet and physical activity and should be considered in the design of interventions. For example, the belief held by many Latinos that a heavier child is a healthier child may drive a variety of obesogenic parenting practices( Reference Crawford, Gosliner and Anderson 34 , Reference Lindsay, Sussner and Greaney 35 ).
Paediatric providers might benefit from partnering with other professionals to promote healthy growth given the extent of the obesity problem, the scarcity of Spanish/English bilingual health professionals, including paediatric providers, and the short duration of paediatric primary-care visits. Attributes of successful interventions are that they are family-focused, multidisciplinary and culturally tailored( Reference Chin, Walters and Cook 36 ). A recent primary case-based obesity prevention trial for infants and their mothers paired paediatricians and health educators and showed success improving maternal feeding practices, although it was not powered to detect differences in infant growth( Reference Taveras, Blackburn and Gillman 37 ). In another randomized controlled trial, obese, 5- to 12-year-old Latinos who with their parents attended group sessions led by a paediatrician, a nutritionist and a promotora had a decrease in their BMI( Reference Falbe, Cadiz and Tantoco 38 ). Paediatricians are trusted sources of health-care information and lend credibility to interventions. Nutritionists can provide content expertise. Finally, promotoras have been partnered with health professionals to overcome cultural and linguistic barriers and to increase both the cultural competence and cultural salience of interventions( Reference Ayala, Vaz and Earp 39 ).
The present analysis contributes to previous work due to two key strengths of the data set. First, the cohort included children at high risk of future obesity, namely low-income infants and toddlers and Latinos. Latino children are generally under-represented in the medical literature. Second, the method of analysis maximized the available data by deriving a WLZ for each cohort member based on all available height and weight data for each individual as well as the entire cohort. A major advantage of the mixed-effects model is the ability to include all available data regardless of the number or timing of an individual’s weight and height measurements.
Several limitations deserve mention. Anthropometric data collected for clinical care use, as in this case, are known to be inaccurate. Any measurement error, however, is expected to be random and should not differ systematically by ethnicity. As such, information bias is not of concern. The data set did not include a number of known risk factors for childhood obesity such as maternal gestational weight gain, parental BMI and infant feeding practices( Reference Taveras, Gillman and Kleinman 17 , Reference Kaar, Crume and Brinton 29 ). Additionally, while premature infants or infants identified at birth to have chronic conditions affecting feeding and growth were excluded, children identified later with chronic medical conditions affecting feeding and growth were not excluded. Inclusion of such children may have affected our results, although the population served by the practice is generally healthy. Our findings are not likely to be explained by reverse causality, that children with greater BMIZ at age 3 years were larger to begin with, given that observed WLZ at birth did not differ according to ethnicity and sex (Table 1). Finally, BMI is a well-accepted proxy, but not a direct measure, of adiposity.
More importantly and for consideration in future research efforts, the heterogeneity of the Latino population is not reflected in its classification here as simply Latino or non-Latino. All Latino children are collapsed into a single category, which does not allow an examination of within-group differences. It is possible that results driven by the Mexican subpopulation are being attributed to all Latinos or that the effect is attenuated by Mexicans but is really a phenomenon only relevant for Central Americans. Additionally, the non-Latino comparison group, composed of low-income White and African-American infants, is at high risk of early childhood obesity. Risk of overfeeding and excessive weight gain early in life is also prevalent among these populations( Reference May, Freedman and Sherry 4 ). As such, the effect of Latino ethnicity might be attenuated from what would be expected if the comparison group were more reflective of the broader population of non-Latinos in the USA. Finally, low income is a strong independent risk factor for childhood obesity for which public insurance may be an inadequate proxy. It is possible that Latino children in this cohort are poorer than their non-Latino peers and that the excess rate of overweight and obesity attributed to ethnicity may in fact be attributable to poverty. Despite these limitations, these data provide further evidence of the relevance of infant growth to future obesity risk in a high-risk, understudied population.
We hope that these findings will inform future efforts to prevent obesity in Latino children. There are 50·5 million Latinos living in the USA according to the 2010 Census( 40 ). Latinos are projected to account for 35 % of US children by 2050( Reference Passel and Cohn 41 ). Health disparities that disproportionately affect Latinos should be addressed now in order to avoid their persistence and amplification. In new destination cities such as Baltimore where the present study was conducted, rapid demographic changes, due primarily to the migration of foreign-born Latinos of low socio-economic status, have far outpaced the development of culturally and linguistically appropriate health care, social services or outreach programmes. This scarcity of services may exacerbate existing disparities in a variety of health conditions, including childhood overweight/obesity. Primary care provides an important opportunity to provide health information and counselling to parents and children. Prediction tools to identify infants at high risk of future obesity could allow paediatric primary-care providers to tailor their care.
Acknowledgements
Acknowledgements: The authors gratefully acknowledge the clinical staff of the CMP for their attention to detail and their dedication to excellent patient care. Thanks are also extended to Avenell Dodge for data collection and to Mónica Guerrero Vázquez and Kate Leifheit for help with manuscript preparation. Financial support: S.P. received support from the National Institutes of Health (grant number 5KL2RR025006-06). The National Institutes of Health had no role in the design, analysis or writing of this article. Conflict of interest: The authors have no conflicts of interest to disclose. Authorship: S.P. conceptualized and designed the study including the data collection instruments, coordinated and supervised data collection, drafted the initial manuscript and approved the final manuscript as submitted. R.J.T. reviewed and revised the manuscript and approved the final manuscript as submitted. L.C. reviewed and revised the manuscript and approved the final manuscript as submitted. A.M. supervised data analysis, reviewed and revised the manuscript, and approved the final manuscript as submitted. Ethics of human subject participation: This study was conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving human subjects/patients were approved by the Institutional Review Board of the Johns Hopkins Medical Institutions.






