Data from large-scale epidemiological surveys has revealed that about one in four young children in developed countries experiences a range of sleep problems(Reference Touchette, Petit and Paquet1,Reference Smaldone, Honig and Byrne2) . Poor child sleep, characterized by insufficient sleep duration or suboptimal sleep quality, is linked to poor academic and educational outcomes(Reference Sadeh, Gruber and Raviv3,Reference Dewald, Meijer and Oort4) . Cumulative evidence summarized by recent systematic reviews and meta-analyses supports a consistent association between short sleep duration in childhood and obesity risk later in life(Reference Cappuccio, Taggart and Kandala5–Reference Chen, Beydoun and Wang7). Further, among toddlers and children of pre-school age, sleep problems are associated with increased risk of emotional and behavioural problems in the school-age years(Reference Kobayashi, Yorifuji and Yamakawa8,Reference Sivertsen, Harvey and Reichborn-Kjennerud9) and early adulthood(Reference Armstrong, Ruttle and Klein10). Understanding the contextual factors associated with poor child sleep is critical to identify, target and intervene at an early age to achieve healthy development and better health outcomes across the lifespan.
Food insecurity, defined as a limited or uncertain availability of nutritionally adequate and safe foods or the limited ability to acquire food in socially acceptable ways(Reference Coleman-Jensen, Rabbitt and Gregory11), has been proposed as a stressor that influences health-related behaviours, such as sleep and adverse mental health indicators. Several large population-based surveys indicate that food-insecure adults are more likely to report shorter sleep duration(Reference Ding, Keiley and Garza12–Reference Whinnery, Jackson and Rattanaumpawan15), poorer sleep quality(Reference Jordan, Perez-Escamilla and Desai14), longer sleep latency and more sleep complaints(Reference Ding, Keiley and Garza12) compared with food-secure adults. However, this research has been limited primarily to adults. According to the US Department of Agriculture, nearly 6·5 million children under the age of 18 years lived in food-insecure households in 2017 and the prevalence of food-insecure households with children under the age of 6 years was 16·4 %, a number that was higher than the national average of 11·8 %(16). Although the exact mechanism is still unclear, poor sleep could be a potential mechanism through which food insecurity may affect various chronic health conditions that may emerge in childhood, including increased cardiometabolic risk(Reference Rocha, Milagres and Novaes17), coexisting obesity(Reference Eisenmann, Gundersen and Lohman18) and behavioural and emotional problems(Reference Shankar, Chung and Frank19).
Although research efforts have been directed at better understanding the health implications of food insecurity, little is known about the sleep quantity and quality of young children in relation to their food security status. The primary aim of the present study was to examine the association between food security and sleep outcomes in a sample of children of pre-school age from low-income families enrolled in Head Start. Food insecurity is commonly associated with parent stress, anxiety and depressive symptoms(Reference Maynard, Andrade and Packull-McCormick20), which in turn, may influence parenting(Reference Lovejoy, Graczyk and O’Hare21) and child sleep behaviours(Reference Mindell, Li and Sadeh22). Thus, the secondary aim of the study was to explore whether parent psychosocial factors, namely perceived stress, parenting self-efficacy and depressive symptomology, mediated any observed associations between food security status and child sleep outcomes.
Methods
Study design and participants
The current study utilized data from a needs assessment survey designed to characterize the home environments of families among a disadvantaged population of caregivers with young children. The survey was distributed to over 1000 caregivers of children enrolled in Head Start pre-school classrooms within four rural counties in central Pennsylvania, USA. Head Start teachers distributed the survey, which included informed consent and instructions for completing and returning the survey packet using a pre-paid envelope. Caregivers were mailed a $US 25 gift card for participation. Data collection spanned May 2017–May 2018. The response rate was 29·6 % (379 surveys returned of the 1279 distributed). Given that the majority of caregiver respondents were parents (90 %), we refer to caregivers as ‘parents’ throughout. Parents were instructed to complete the survey for their oldest child enrolled in Head Start. Nine surveys were excluded because a parent had completed a survey for more than one child. Four participants were ineligible based on the child’s date of birth (e.g. age outside the range of Head Start pre-school eligibility) and an additional four were removed due to missing data, resulting in a final study sample of 362. The study was approved by the Office for Research Protections at The Pennsylvania State University, University Park, PA, USA.
Child sleep
Child sleep duration was calculated based on parent reports of their child’s typical bedtime and wake time in hours and minutes. Two items from an expanded version of the Brief Infant Sleep Questionnaire (BISQ)(Reference Sadeh, Mindell and Luedtke23) were used to measure bedtime routine and sleep quality. Bedtime routine was assessed with parent reports of how often (1 = ‘never’ to 5 = ‘every night’) their child has the same bedtime routine in a typical 7 d week. Sleep quality was assessed with parent ratings of how well their child usually sleeps at night (1 = ‘very poorly’ to 6 = ‘very well’). Sleep quality was grouped as ‘poor’ (if response was 1–5) and ‘very well’ (if response was 6). The BISQ has been validated against actigraphy and sleep logs(Reference Sadeh24) and used in previous studies with pre-school children(Reference Mindell, Sadeh and Kwon25,Reference Kushnir and Sadeh26) .
Food security status
The eighteen-item US Department of Agriculture Household Food Security Module was used to measure household, adult and child food security status(Reference Coleman-Jensen, Rabbitt and Gregory11). Households and adults were independently classified as ‘food insecure’ if participants responded affirmatively to three or more items and ‘food secure’ if two or fewer items were affirmative on the respective full eighteen-item scale and the ten-item adult food security subscale. Child food security status was assessed using the eight child-referenced questions and children were considered ‘food insecure’ if participants responded affirmatively to two or more items(Reference Gundersen and Ziliak27).
Parent psychosocial factors
Parent perceived stress levels were assessed using the ten-item Perceived Stress Scale (PSS-10)(Reference Cohen, Kamarck and Mermelstein28), a widely used and validated measure of the degree to which respondents believe their life to be unpredictable, uncontrollable and overwhelming(Reference Lee29). Response options for the ten items (α = 0·85) ranged from 1 = ‘never’ to 5 = ‘very often’. A standardized PSS-10 Z-score (mean = 0, sd = 1) was calculated, with higher scores indicating higher levels of stress over the past month.
The five-item version of the Parenting Sense of Competency self-efficacy subscale (PSOC-5)(Reference Gilmore and Cuskelly30) was used to assess general parenting confidence. The PSOC-5 was validated in a large, non-clinical sample of parents(Reference Gilmore and Cuskelly30) and has been reliably used among mothers with children of pre-school age(Reference Heerman, Taylor and Wallston31). Response options for the five items (α = 0·79) ranged from 1 = ‘strongly agree’ to 6 = ‘strongly disagree’. All items were reverse coded, a total PSOC-5 score was calculated and then standardized such that higher scores reflect greater perceived parenting self-efficacy.
The Center for Epidemiological Studies Depression Scale-10 (CESD-10)(Reference Andresen, Malmgren and Carter32), a well-validated measure with acceptable test–retest and predictive validity, was used to assess parent depressive symptomology. Response options for the ten items (α = 0·82) ranged from 0 = ‘rarely or not at all’ to 3 = ‘most days.’ A total CESD-10 score was calculated and then standardized, with higher scores indicating higher levels of depressed mood during the past week.
Covariates
Key parent demographic characteristics were considered as covariates to adjust for potential confounding effects, including child age and sex, parent age, education, marital status, employment status, number of children in the household, number of people supported by household income, participation in assistance programmes (e.g. Special Supplemental Nutrition Program for Women, Infants, and Children (WIC); Supplemental Nutrition Assistance Program (SNAP)), household income and region. The analytic sample was constrained to participants who had complete data on food insecurity, sleep outcomes and adjusting covariates. Household income was missing in seventy-four of 362 households (20·4 %). Missing income was imputed based on WIC and SNAP status, parent education, marital status and employment using PROC MI in SAS and imputed income was adjusted in sensitivity analysis.
Given previous research showing an association between factors within the home environment and child sleep(Reference Appelhans, Fitzpatrick and Li33,Reference Boles, Halbower and Daniels34) , household chaos and family functioning were also considered as covariates. Household chaos was assessed using the Confusion, Hubbub, and Order Scale (CHAOS)(Reference Matheny, Wachs and Ludwig35), a measure of structural disorganization in the home marked by high noise levels, crowding, and lack of predictability and family routines. The concurrent validity of the scale was demonstrated against direct observational measures in the home and has acceptable test–retest reliability(Reference Matheny, Wachs and Ludwig35). CHAOS has been used with diverse samples of parents with young children(Reference Corapci36,Reference Dumas, Nissley and Nordstrom37) . The item ‘The telephone takes up a lot of our time at home’ was replaced with ‘There is usually a television turned on somewhere in our home’(Reference Hart, Petrill and Deater-Deckard38). Response options for the fifteen items (α = 0·86) ranged from 1 = ‘definitely untrue’ to 5 = ‘definitely true’. A mean score was calculated with higher scores indicating greater chaos. Family functioning was assessed with the general family functioning subscale from the Family Assessment Device (FAD)(Reference Epstein, Baldwin and Bishop39). The FAD is widely used and has been shown to have acceptable test–retest reliability and concurrent and discriminant validity(Reference Miller, Epstein and Bishop40). Response options for the twelve items (α = 0·91) ranged from 1 = ‘strongly disagree’ to 4 = ‘strongly agree’. A mean score was calculated, with higher scores indicating better family functioning.
Statistical analysis
To test for differences in the distribution of covariates (e.g. demographics), parent psychosocial factors and child sleep outcomes (i.e. wake time, bedtime, sleep duration and sleep quality) by food security status, the t test, χ 2 test and Mann–Whitney U test were used for normally distributed continuous variables, categorical variables and non-normal continuous variables, respectively. Sleep quality was the only child sleep outcome that differed significantly by food security status, thus subsequent analyses focus on sleep quality only. The unadjusted association between food security status (household, adult and child level) and sleep quality was quantified using logistic regression models (Model 1). Separate multivariable logistic regression models were applied to quantify the adjusted relationship between food security status (household, adult and child) and sleep quality controlling for household income and covariates that showed a significant bivariate relationship (P < 0·05) with food security status (Model 2).
Mediation analysis was conducted to test whether the adjusted relationship detected in Model 2 was mediated by parent psychosocial factors (Fig. 1). Specifically, the statistical modelling included three steps. Step 1 was to obtain the adjusted coefficients between food security status and the mediator by constructing linear regression models of continuous parent psychosocial factor scores as a function of food security status with the same adjustment included in Model 2 (depicted as path a in Fig. 1). Step 2 was to construct multivariable logistic regression models between food security status and the dichotomous child sleep outcomes, controlling for the mediator while adjusting for covariates included in Model 2. The second step generated two coefficients: the first representing the adjusted association between the mediator and sleep quality, controlling for food security status (depicted as path b in Fig. 1); and the second representing the indirect association between food security status and sleep quality, controlling for the mediator (depicted as path c′ in Fig. 1). Step 3 was to compare the total adjusted effect of food security status on sleep quality from Model 2 (depicted as path c in Fig. 1) with the indirect effect obtained from step 2 (depicted as path c′ in Fig. 1). All coefficients were standardized by multiplying by the standard deviation of the independent variable and dividing by the standard deviation of the dependent variable to achieve comparable coefficients obtained from linear and logistic models(Reference MacKinnon and Dwyer41). To quantify the magnitude of a potential mediation effect, two indicators were calculated using the standardized coefficients: (i) the percentage of the total effect that was mediated, calculated as  $a \times b/(a \times b + {c^\prime })$; and (ii) the ratio of the indirect effect to the direct effect, calculated as
$a \times b/(a \times b + {c^\prime })$; and (ii) the ratio of the indirect effect to the direct effect, calculated as  $a \times b/{c^\prime }$. The Sobel test was used to evaluate if the mediating path was statistically different from zero (the Sobel test statistic was calculated as the standardized coefficient a × b)(Reference Preacher and Hayes42). All analyses were conducted using the statistical software package Stata SES 15.0 and imputation was performed using the statistical software package SAS version 9.4.
$a \times b/{c^\prime }$. The Sobel test was used to evaluate if the mediating path was statistically different from zero (the Sobel test statistic was calculated as the standardized coefficient a × b)(Reference Preacher and Hayes42). All analyses were conducted using the statistical software package Stata SES 15.0 and imputation was performed using the statistical software package SAS version 9.4.
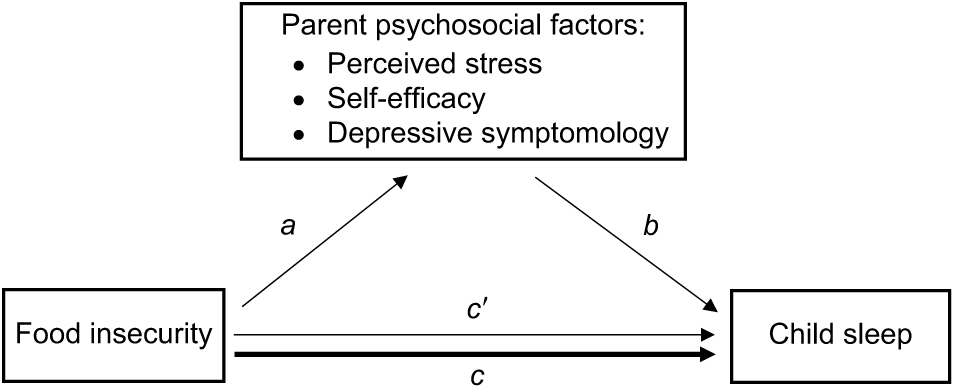
Fig. 1 Hypothesized mediation effect of parent psychosocial factors in the association between food insecurity and child sleep outcomes. a represents the adjusted association between food insecurity and the hypothesized mediator; b represents the adjusted association between the hypothesized mediator and child sleep outcome, controlling for food insecurity; c represents the total adjusted association between food insecurity and child sleep outcome (obtained from Model 2 in Table 2); and c′ represents the adjusted association between food insecurity and child sleep outcome, controlling for the hypothesized mediator. The adjusted associations were controlled for number of people supported by household income, participation in assistance programmes, household income level, household chaos score and family functioning score
Results
Sample characteristics
The majority of parents (95·8 % female) and children were White (parents: 93·9 %, children: 86·9 %) non-Hispanic (parents: 97·9 %, children: 95·8 %). Additional sample characteristics, parent psychosocial factors and child sleep outcomes are presented in Table 1 by food security status. Of 362 parents included in the study, the prevalence of household, adult and child food insecurity was 37·3, 31·8 and 17·7 %, respectively. Household, adult and child food insecurity was associated with higher household chaos (all P < 0·005) and lower family functioning (all P < 0·02). Participation in SNAP was greater when participants reported household (food secure v. food insecure: 69·1 v. 85·0 %, P = 0·001) or adult (69·6 v. 86·7 %, P = 0·0005) but not child (73·6 v. 82·3 %, P = 0·153) food insecurity. Participation in WIC was less common among households with food insecurity (73·1 v. 62·7 %, P = 0·045) but did not differ by adult or child food security status. Parent perceived stress and depressive symptomology were significantly higher among families reporting food insecurity at all three levels (all P ≤ 0·0002), while the parent self-efficacy score was significantly lower only in parents reporting child food insecurity (P = 0·043), but not household or adult food insecurity. Household chaos and family functioning were correlated with parent stress (r CHAOS = 0·51, r FAD = −0·46), depressive symptomology (r CHAOS = 0·41, r FAD = −0·37) and lower self-efficacy (r CHAOS = −0·30, r FAD = 0·31), all P < 0·01 after Bonferroni correction.
Table 1 Distribution of sample characteristics, parental psychological factors and child sleep outcomes by food security status* in the sample of low-income Head Start children of pre-school age (n 362) and their caregivers from four rural counties in central Pennsylvania, USA, May 2017–May 2018
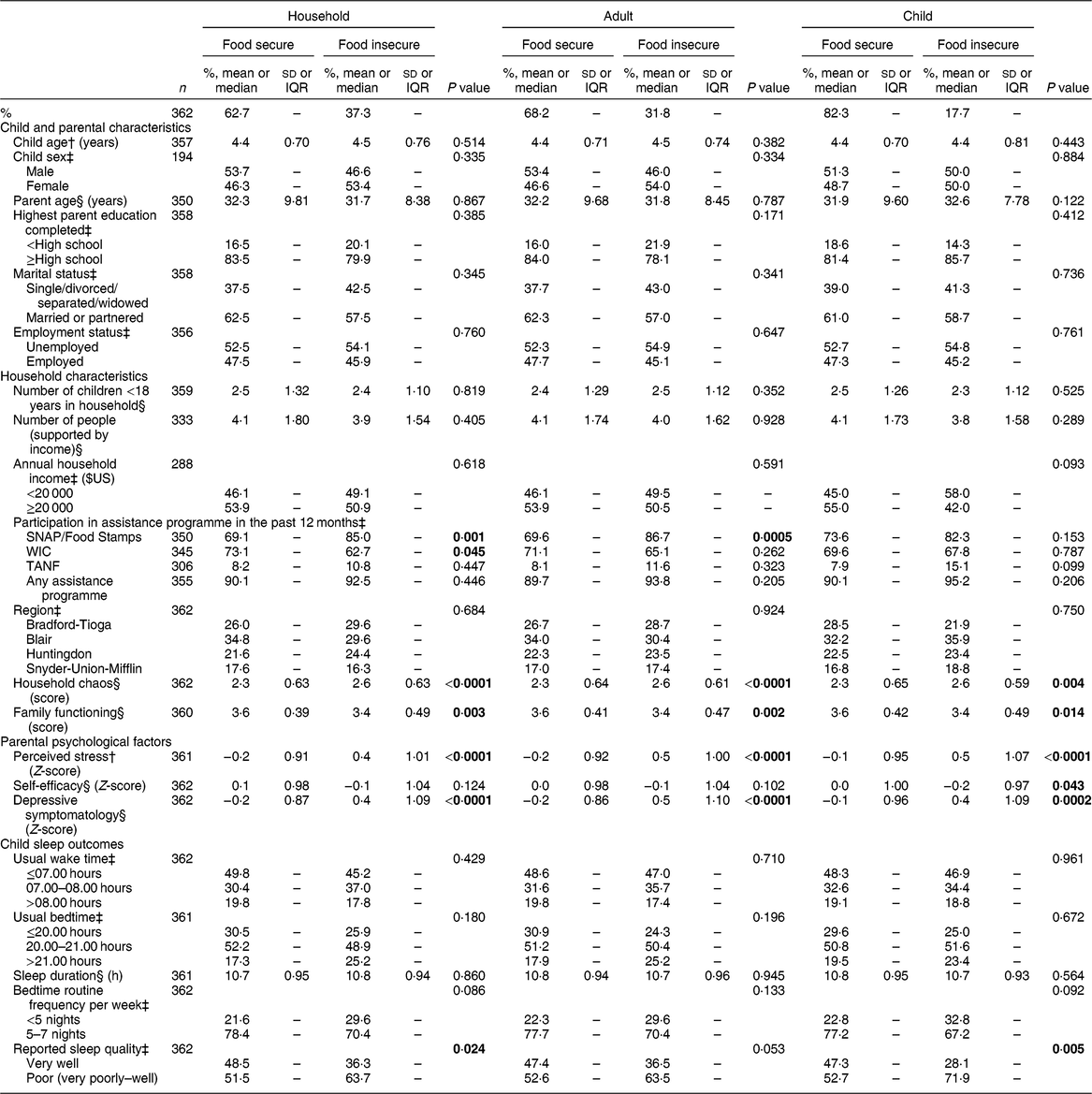
IQR, interquartile range; SNAP, Supplemental Nutrition Assistance Program; WIC, Special Supplemental Nutrition Program for Women, Infants, and Children; TANF, Temporary Assistance for Needy Families.
Statistically significant P values are shown in bold.
* Values presented are percentages, or as means and standard deviations, or as medians and interquartile ranges.
† The t test was conducted to determine differences between normally distributed continuous variables and binary food security status.
‡ The χ 2 test was conducted to determine differences between categorical variables and binary food security status.
§ The Mann–Whitney U test was used to determine differences between non-normal continuous variables and binary food security status.
Child sleep outcomes by food security status
In the overall sample, about half of parents reported that their child woke up prior to 07.00 hours (48·1 %) and went to bed between 20.00 and 21.00 hours (51·0 %). Mean (sd) sleep duration at night was 10·7 (0·9) h. Reported wake time, bedtime and sleep duration did not differ by food security status (all P > 0·1). The proportion of parents reporting maintaining a bedtime routine for more than 5 d/week was higher among food-secure (range: 77·2–78·4 %) compared with food-insecure (range: 67·2–70·4 %) families, but these differences did not reach statistical significance (all P > 0·08). Compared with the food secure referent, the proportion of parents reporting poor child sleep quality (very poorly–well) was higher among parents reporting household (51·5 v. 63·7 %, P = 0·024), adult (52·6 v. 63·5 %, P = 0·053) and child (52·7 v. 71·9 %, P = 0·005) food insecurity.
Food security status and child sleep quality
Table 2 presents odds ratios of poor child sleep quality by food security status before and after adjusting for participation in assistance programmes (e.g. SNAP), household chaos, family functioning and household income as covariates. In the unadjusted Model 1, household food insecurity was significantly associated with a 1·65-fold increased odds (95 % CI 1·07, 2·55) of poor child sleep quality and child food insecurity was significantly associated with a 2·30-fold increased odds (95 % CI 1·27, 4·14) of poor child sleep quality (both P < 0·05). However, food insecurity at the household level was not significantly associated with child sleep quality when covariates were included in Model 2. Child food insecurity was independently significantly associated with a 2·27-fold increased odds (95 % CI 1·12, 4·59) of poor child sleep quality in the adjusted Model 2.
Table 2 Unadjusted and adjusted odds ratios (and 95 % confidence intervals) of the associations between reported poorer child sleep quality and food security status at household, adult and child level in the sample of low-income Head Start children of pre-school age (n 362) and their caregivers from four rural counties in central Pennsylvania, USA, May 2017–May 2018
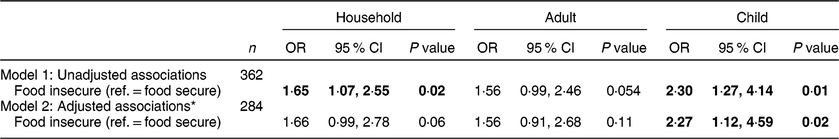
Ref., referent category.
Statistically significant values are shown in bold.
* Adjusted for participation in assistance programmes, household income level, household chaos score and family functioning score.
Mediation tests of parent psychological factors
The results from mediation tests of parent psychosocial factors are presented in Table 3. Compared with the adjusted odds of 2·27 (95 % CI 1·12, 4·59) in Model 2 (representing path c depicted in Fig. 1), including parent psychosocial factors (perceived stress, self-efficacy and depressive symptomology Z-scores) in the model changed the odds for child food insecurity only slightly. The quantitative measure for the percentage of the effect mediated (all ≤4·1 %) and the ratio between the indirect and direct effect were small (all ≤0·05). According to the Sobel test, none of the parent psychosocial factors significantly mediated the relationship between child food insecurity and child sleep quality (all Sobel test P > 0·5).
Table 3 Test of mediation effect of parental psychological factors in the associations between child food insecurity (FI) and poor child sleep quality* in the sample of low-income Head Start children of pre-school age (n 362) and their caregivers from four rural counties in central Pennsylvania, USA, May 2017–May 2018
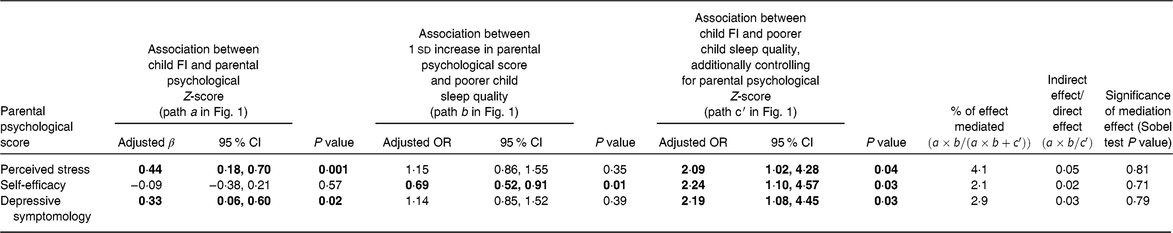
Statistically significant values are shown in bold.
* All models were adjusted for participation in assistance programmes, household income level, household chaos score and family functioning score.
Discussion
To our knowledge, the present study is the first to explore the association between food security status and sleep outcomes among young children of low-income families. We found a significant association between child, but not household or adult, food insecurity and sleep quality in children of pre-school age after adjusting for a number of potential confounders and covariates, including the number of people supported by household income, participation in assistance programmes (e.g. SNAP), household chaos, family functioning and household income. In contrast to our hypothesis, the association between child food insecurity and child sleep quality was not mediated by the parent psychosocial factors of interest.
As hypothesized, food-insecure children were about two times more likely to have poor sleep quality compared with food-secure children. Several mechanisms may explain the association in the present study. One potential pathway may be related to children’s emotional and behavioural health. Although food insecurity experience is rarely expressed in young children, food insecurity as a direct stressor was found to increase risk of several behavioural problems in pre-school children(Reference Melchior, Chastang and Falissard43,Reference Weinreb, Wehler and Perloff44) , which correlated with shorter sleep duration(Reference Lavigne, Arend and Rosenbaum45) and other sleep problems(Reference Hiscock, Canterford and Ukoumunne46). The biological pathway explaining stress as a potential mediator is hypothesized to be related to an impaired immune system and disrupted hypothalamic–pituitary–adrenal axis activity(Reference Barazzetta and Ghislandi47), which are both involved in modulating sleep(Reference Buckley and Schatzberg48). Although food insecurity is not a measure of hunger, children directly impacted by food insecurity may be more likely to experience hunger, which could affect sleep quality particularly if a child goes to bed hungry.
The present study observed a lack of association of household and adult food insecurity with child sleep outcomes. The lack of association may be interpreted in light of the growing literature exploring the relationship between low socio-economic status (SES) and the home environment on child sleep outcomes. Several studies have reported that children aged 1–17 years from low-SES families have more sleep problems such as short sleep duration and poor sleep quality compared with their higher-income counterparts(Reference El-Sheikh, Kelly and Buckhalt49,Reference El-Sheikh, Bagley and Keiley50) . Recent evidence from longitudinal studies further supports the association of low SES and material deprivation, defined through the quality of the house and neighbourhood where a child lives, with sleep later in childhood and adolescence(Reference Barazzetta and Ghislandi47,Reference Doane, Breitenstein and Beekman51) . Among pre-school children, Crabtree et al.(Reference Crabtree, Korhonen and Montgomery-Downs52) found higher impaired sleep scores and problematic bedtime behaviours in children from lower-SES groups than in those from higher-SES groups in a large sample of children aged 2–7 years (n 3371). Emerging evidence supporting the association between SES and child sleep outcomes may explain, in part, why we did not see an association between adult and household food insecurity and child sleep quality after adjusting for household income and home environment factors (i.e. chaos and family functioning).
Consistent with previous research, parent psychosocial factors, including depressive symptoms(Reference Whitaker, Phillips and Orzol53,Reference de Jong, Cremone and Kurdziel54) and perceived stress(Reference Laraia, Siega-Riz and Gundersen55,Reference Caldwell and Redeker56) , were associated with higher risk of child food insecurity (Table 1) and poorer child sleep quality (see online supplementary material, Supplemental Table S1). Building on previous research examining a potential relationship between parenting and food insecurity(Reference Heerman, Taylor and Wallston31,Reference Bronte-Tinkew, Zaslow and Capps57) , we found a positive relationship between parenting self-efficacy and both food insecurity and poorer child sleep quality. However, these parent psychosocial factors did not explain the observed association between child food insecurity and poor sleep quality. Given that factors within the home environment, such as higher household chaos and lower family functioning, were associated with increased parent stress, depressive symptoms and lower self-efficacy in the current study sample, adjusting for these home environment factors may have attenuated a true mediation effect. We also cannot rule out the possibility that other unmeasured parental psychosocial constructs may have had a mediating effect that we could not examine in our study.
Findings from the present study need to be interpreted acknowledging a number of limitations. First, the present study was cross-sectional in nature; thus, the temporality of food insecurity and child sleep outcomes and causality could not be determined. Second, sleep outcomes (duration, routine and quality) were assessed via parent report, which is subject to recall bias. For example, errors in reported bedtime and wake time, especially among children who do not follow a regular sleep routine, could have caused some random variability in the calculated sleep duration, which, at least partially, led to the insignificant findings when exploring the relationship between food insecurity and sleep duration. For the sleep quality measure, it is likely that parents have subjectively underestimated their children’s sleep problems, such as night wakings(Reference Sadeh58). Previous research has shown that number of night wakings is one of the major factors by which parents judge the quality of their child’s sleep(Reference Palmstierna, Sepa and Ludvigsson59). Thus, objective sleep measures such as actigraphy may provide more accurate measurements and should be considered in future studies with young children(Reference Meltzer, Biggs and Reynolds60). Third, there were missing data in household income that reduced the analytic sample. However, sensitivity analyses without adjusting for household income and adjusting using imputed household income values showed robust results (see online supplementary material, Supplemental Tables S2 and S3). Finally, we cannot eliminate the risk of non-response bias given the nature of the study design and the moderate survey response rate. Therefore, the external validity of our findings may be limited to certain low-income families. Although less than desirable, the response rate was similar to that in another study utilizing survey data collected in a similar manner from a rural Head Start population in Colorado (i.e. 28·5 %)(Reference McCloskey, Johnson and Benz61). Future studies are warranted to test whether or not our study findings can be generalized beyond Head Start children in rural central Pennsylvania.
Conclusion
In conclusion, results from the present study suggest that child food insecurity may be associated with suboptimal sleep quality among children of pre-school age and this association may not be mediated by parent psychosocial factors. Sleep problems during early stages of life can have detrimental effects on the cognitive, socio-emotional and physical health of children throughout the life course. Food insecurity, particularly at the child level, is a potential modifiable risk factor for reducing sleep-related health disparities in early childhood. Evidence from our study highlights the importance of focusing on children’s experience of food insecurity and its potential impact on their sleep quality and related health outcomes. Future studies are needed to explore the potential mechanisms underlying the associations between child food insecurity and adverse sleep outcomes.
Acknowledgements
Acknowledgements: The authors acknowledge Michele E. Marini at the Center for Childhood Obesity Research, Penn State University, for managing and preparing the data sets for data analysis. Financial support: This research was supported by US Department of Agriculture’s Supplemental Nutrition Assistance Program (SNAP) through the PA Department of Human Services (DHS). The research reported in this publication was supported by the National Center for Advancing Translational Sciences of the National Institutes of Health (grant numbers TL1 TR002016 and UL1 TR002014). The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH. Conflict of interest: The authors have no conflicts of interest relevant to this article. Authorship: J.S.S. designed the study. M.N. conceived the research question, conducted data analysis and prepared the first draft of the manuscript. S.G.E., L.J., K.L. and J.S.S. helped with literature review, data interpretation, manuscript writing and revising. All authors read and approved the final manuscript. Ethics of human subject participation: This study was conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving human subjects were approved by the Office for Research Protections at The Pennsylvania State University, University Park, PA, USA. Implied informed consent was obtained from all subjects.
Supplementary material
To view supplementary material for this article, please visit https://doi.org/10.1017/S136898001900332X






