Introduction
“To be buried while alive is, beyond question, the most terrific of the…extremes which has ever fallen to the lot of mere mortality,” Footnote 1 Edgar Allan Poe once proclaimed in The Premature Burial. Poe had the literal meaning in mind; however, persons with locked-in syndrome (LIS), and particularly those with completely locked-in syndrome (CLIS), have a similar fate. They are conscious, but trapped within their own bodies, unable to move or communicate. With the development and refinement of the use of brain–computer interfaces (BCIs), Footnote 2 an elaborate assistive technology that provides an interface between a human being and a computer or a machine, hopes have been raised that this confinement may be breached.
A BCI for communication Footnote 3 detects and uses different patterns of electric, magnetic, or metabolic neural activity to control an external device; for example, a computer cursor or a visual P300 speller, thereby overriding the need for residual movement to connect with the outside world. The BCI can be invasive or noninvasive. Invasive interfaces are surgically implanted, although with a varying degree of invasiveness dependent on where the electrodes are placed, whereas noninvasive interfaces are externally attached to the scalp. Although implantable BCIs can obtain neural signals of higher quality, this advantage has to be weighed against the risks involved in a surgical procedure, such as the use of anaesthesia, for which risks are significantly higher for LIS patients, and risks of infections or of damaging neural tissue. Therefore, even though the neural signals recorded by noninvasive BCIs have important limitations, for example that they must pass through bone and skin tissue before being picked up, which lowers signal quality and thereby may decrease the system’s reliability to sort out the needed signals, Footnote 4 noninvasive BCIs have, hitherto, dominated the research on BCIs for communication.
Although the first successful attempts to use BCIs for communication in severely disabled patients had already been undertaken in the 1990s, Footnote 5 this field of BCI research has led a marginalized existence in the shadow of the hyped fields of neural prosthetics and brain stimulation devices. As a consequence, few medical professionals or potential users, are aware of BCIs’ potential as an assistive technology. Even fewer have firsthand experiences of using a BCI for communication, because this access in most cases requires participation in a research study.
We will argue that there are compelling ethical reasons to raise the awareness both of LIS, and of BCIs for communication. The current ignorance strikes a person in LIS twofold. First by the impairments caused by the medical condition, but in addition, by being locked in, the person also faces substantial social prejudices and confinements, here captured in the figurative expression of being “locked out.” The main contributions of this article are (1) to show how persons in LIS are being locked out, including how key issues addressed in the existing literature on ethics, LIS, and BCIs for communication, such as autonomy, quality of life and advance directives, may reinforce these confinements; (2) to show how these practices violate the United Nations Convention on the Rights of Persons with Disabilities, and to suggest that we have a moral responsibility to prevent and stop this exclusion; and (3) to discuss the role of BCIs for communication as one means to this end, and to suggest that a novel approach to BCI research is necessary to acknowledge the moral responsibility toward the end users and avoid violation of the human rights of persons in LIS. Footnote 6
Life with LIS
LIS is a very rare condition. Although the actual incidence and prevalence are unknown, one rough estimate of the latter is 1–2 cases per 1,000,000. Footnote 7 Brain stem stroke is the most common etiology, though more than 20 causes have been documented, such as advanced stages of amyotrophic lateral sclerosis (ALS), head trauma, tumors, and infections. Footnote 8 In the medical literature, the term "LIS" was introduced by Plum and Posner in 1966, although the condition is occasionally referred to as "pseudocoma" or “de-efferented state." The condition is, after Bauer 1979, divided into three varieties: classical, total, and incomplete. Footnote 9 Classical LIS is characterized by muteness Footnote 10 and close to complete paralysis, in which only vertical eye movements and blinks remain under voluntary control. In total LIS, also known as complete LIS (CLIS), Footnote 11 even these limited displays of motor control are lacking, leaving the person completely paralyzed. In incomplete LIS, the person has some residual voluntary muscle control in addition to eye movements, such as lip twitches, control over fingers, or neck movement. In all varieties of LIS, the persons are still aware, with intact cognitive functions, but because of the paralysis, they are unable to break their bodily confinement. In addition, most still see, hear, smell, taste, and experience heat and cold, as well as pain and pleasure. Footnote 12
Being cognitively intact has been a defining criterion differentiating CLIS from disorders of consciousness. However, to establish if a person assumed to be in CLIS de facto has these functions is another matter, because no communication, and thereby social interaction, is possible. Because of previous failures to reestablish communication with persons in CLIS, it has been hypothesized that the lack of motor control could lead to a “cessation of voluntary cognitive activity, goal directed thinking and imagery.” Footnote 13 In short, if brain activity and behavioral responses are no longer connected to or acted out as a consequence of conscious decisions and intentions, over time, the actual ability to form intentions; that is, the will, will vanish. This hypothesis is referred to as the “extinction of goal directed thinking,” or the “extinction of thought.” Footnote 14 However, in 2014, it was reported that communication was reestablished with a woman who had been in CLIS for more than 2 years. Footnote 15 In this study, a near-infrared spectroscopy (NIRS)-based BCI was used, which measured frontocentral oxygenation changes in response to questions requiring a “yes” or “no” thought. The same research group later duplicated these promising results in four CLIS patients. Footnote 16 An important technical advancement in the latter study was the combination of NIRS and electroencephalographic (EEG) recordings, which allowed for sleep detection to increase the BCI system’s reliability. Although in LIS circadian rhythm is largely preserved, continuous electrocorticography (ECoG) sleep polysomnographic recordings in a CLIS patient showed increased fragmentation of slow wave sleep (SWS), even during daytime hours. Footnote 17 As a consequence, BCI communication can be substantially impeded in CLIS because of short episodes of SWS, sometimes lasting only a few tens of seconds. Three of four study participants answered open questions containing quality of life estimation repeatedly with a “yes” response, so that the authors inferred a positive attitude toward the present situation and toward life in general. Although only reporting on five cases, these studies remain an important proof of principle, as they show that there are people in CLIS who are cognitively intact, thus confirming that CLIS is a valid diagnosis. With this said, there could still be persons in CLIS who will not be able to use a BCI to enable communication, either because of the shortcomings in present day BCIs, or because of medical challenges such as an “extinction of thoughts” or severe sleep fragmentation.
Only 13% of the persons in LIS survive the first 4 months, but once the acute phase has passed, there can be a life expectancy of decades unless other medical complications occur. Footnote 18 It is important to keep in mind that these survival rates are likely to increase over time as a result of technological and medical advances, and that the prognoses may differ among different etiologies. Footnote 19 For example, of all individuals diagnosed with ALS, only 10–20% survive the first 60 months, although nowadays a life expectancy of decades is not uncommon, as ALS per se is not a deadly disease. The cause of death in ALS does not directly relate to the degradation of the upper and lower motor neurons, but rather to the clinical complications associated with this process; that is, respiratory failure, infections, or poor circulation caused by immobilization. Footnote 20 Although LIS can be transient, some—albeit few—patients do recover, LIS is generally chronic, and only minor improvements are expected: to regain a fraction of an inch in limb control, to eat without using a gastric tube, or to breathe without the help of a respirator. Once initial hospital care is completed, only a minority of the patients stay as permanent hospital residents or move to nursing homes. The majority return to their homes where they receive full care by hired assistance, volunteers, or family and friends. By adapting the home environment and providing wheelchairs and assistive technology such as computer-assisted communication, persons in LIS can start to reclaim their lives. Footnote 21
Several studies have shown that a maintained ability to communicate is paramount for the well-being and quality of life experienced by persons in LIS. Some persons still have the ability to exercise a rudimentary form of communication. “Yes,” for example, can be expressed either by one wink of the eyes or by looking up, and “no” can be expressed by two winks or looking down. There are also assistive technologies such as communication boards or speech-generating devices. The former require intact eye movements, and can either be used by gazing at letters, symbols, and phrases written either on a piece of paper or a whiteboard, or on the screen of an electronic device, and then scanned and read out by a speaking partner. There is also the more expensive option in which the speaking partner is substituted for by an eye-tracking system. This high-tech system then facilitates communication by generating either written text or an electronic voice, a so-called “speech- generation device.” A well-known user of the latter is physicist and ALS patient Stephen Hawking, although his speech-generation device was first maneuvered by a joystick and later upgraded to recognize minute facial movements (this only works for persons with incomplete LIS, as some residual muscle control is required). Although these communication aids are beneficial for many persons in LIS, they have important limitations, such as being gaze dependent. If the control of eye movement is lost, so is the ability to communicate. Footnote 22
Although many persons with LIS initially feel despair over their condition, studies on quality of life show that most, over time, express that they are content with their lives. Footnote 23 Contrary to many outsiders’ assumptions when imagining a life with LIS, it consists of family life, including everything from obligations as a spouse or parent to an active sex life, going out, pursuing hobbies and meeting friends, or for some persons in LIS, returning to work. Footnote 24 Philippe Vigand, locked in and author of the book Only The Eyes Say Yes: A Love Story, describes some of his activities as being playing bridge with friends, dabbling in the stock market, reading books and newspapers, going to dinner parties (and occasionally getting tipsy) and the cinema, participating in hunting trips, and watching soccer, in addition to writing a book, fathering a child, and contemplating getting a job. Footnote 25
Although the degree of activity varies from person to person, a study from 2003 mentions that 11 of the 13 participants left their home more than once a month, and were engaged in activities such as “TV, radio, music, books on tape, visiting with family, visit vacation homes, e-mail, telephone, teaching, movies, shows, the beach, bars, school, and vocational training.” Footnote 26 An attorney in LIS continued to give legal opinions, another person used a speech-generating device to teach spelling and math to third graders, and yet another was such a big fan of a local college team that he was depicted in a news piece. The article further reports that the interviewers who conducted the study of this cohort of persons in LIS were “impressed with the real and substantial social interactions;” for example, that “the patients were actively involved in family and personal decisions, and that their presence was valued at home.” Footnote 27
Locked Out
It is now 2017. More than 25 years have passed since the Americans with Disabilities Act was ratified, and it was 11 years ago that the United Nations General Assembly adopted the Convention on the Rights of Persons with Disabilities and its Optional Protocol. Because the latter is globally ratified, our argumentation rests on this convention. Key features in the United Nations convention include promoting dignity, autonomy, and independence; nondiscrimination, ranging from a right to life, equal recognition before the law, and accessibility, to fighting stereotypes, prejudices, and harmful practices; acknowledging and promoting the abilities and contributions of persons with disabilities in their families and local communities and as citizens; and the importance of depicting these abilities and contributions of persons with disabilities in the media. Nevertheless, prejudice, discrimination, and exclusion are still a reality not only for persons with LIS, but also for the roughly 650,000,000 people worldwide living with a disability. Footnote 28
Although the available accounts of life with LIS from an insider’s perspective are rare, they have one theme in common: once a person enters LIS, most people no longer treat that person as a person. This change is manifested in the person in LIS being avoided or ignored; in the assumptions that muteness and paralysis imply being mentally impaired or being devoid of feelings or preferences; or in that person being perceived to be, and therefore treated as, a vegetable. Julia Tavalaro, who wrote Look Up for Yes, was for more than 6 years referred to as "the vegetable" by the employees of the chronic care ward where she was staying, Footnote 29 Jean-Dominique Bauby, author of the international bestseller The Diving Bell and the Butterfly, declares “henceforth I belonged on a vegetable stall and not to the human race,” Footnote 30 and Phillipe Vigand explains that one of his main reasons for writing a book depicting life with LIS was “to alter the way others look at me, so that I’m no longer considered a vegetable.” Footnote 31
Examples of not being acknowledged as an autonomous person include being avoided or overlooked by strangers, former friends, or family members, as well as by some healthcare professionals. This loss of acknowledgement was also pointed out by Martin Pistorius, Footnote 32 author of Ghost Boy, who confirms that people rarely speak to him directly: “Most people speak at, around, over or about me, so everybody who treats me like a cut above the average root vegetable is unforgettable.” Footnote 33 A similar experience is described by Vigand’s wife “It was my duty to repeat over and over again to the doctors and nurses that it was their responsibility to talk to him, or at least treat him like a full-fledged human being, one more sensitive than most, a man with his own sufferings, desires, and needs.” Footnote 34 Or as Vigand himself adds, “Nothing is worse than being taken for a baby when you are in your thirties.” Footnote 35 Other examples that also show the failure to treat persons with LIS as sentient beings with interests and preferences worthy of being taken into account are serving them meals either too hot or too cold, giving them ice cold showers or leaving them in cold baths, placing them in uncomfortable positions or neglecting to ask if they are in pain, shutting off the TV in the middle of an important soccer game, or leaving them in front of a movie that they have no interest in watching. Footnote 36 Although these accounts are anecdotal, they nevertheless indicate that some persons in LIS have had their fundamental human rights, such as respect for dignity and autonomous choices, violated.
Lacunas in the Academic Debate on Ethics, LIS, and BCIs for Communication
According to the few accounts available, persons with LIS often face stereotypes, prejudices, and harmful practices in their everyday lives. It is important to recognize that such biases are present and are also expressed among healthcare professionals and researchers, and in the contemporary academic literature on ethics, LIS and BCIs for communication. As a consequence, we—both healthcare professionals and researchers—must not forget to reflect on how we approach and portray persons with LIS so that we do not unintentionally uphold stereotypes and prejudices. In other words, we must pay attention to the explicit and implicit messages conveyed in the research we pursue and publish. As regards persons in LIS, how issues such as quality of life and advance directives are approached and discussed is one example, whereas actively avoiding a one-sided depiction of life in LIS is another.
Advance directives are probably the most discussed ethical concern raised by BCIs for communication. Many healthy individuals do express, in a living will, directly to family or friends, or as participants in a research study, that life support, in case of a fatal disease such as ALS or for medical complications resulting in LIS, should not be employed, or conversely, that the withdrawal of such treatments could be morally justified. Footnote 37 This view is shared by many clinicians. In addition, it has been shown that clinicians often tend to make medical decisions accordingly. By limiting life-sustaining treatments and telling the patient’s significant others that death is a preferred option, many patients with LIS are faced with a premature death. Footnote 38 In a study in which German neurologists were interviewed, 10% out of 154 neurologists said that life-sustaining treatment should always be limited for persons in LIS, and 81% agreed that it should be limited under certain circumstances; only 9% stated that life-sustaining treatment should never be limited for persons in LIS. Footnote 39 However, several studies have shown that these preferences seldom correspond with the preferences expressed by persons in LIS; once the initial phase of adaptation and despair has faded, most still find life worth living. Footnote 40
The validity of advance directives for persons in LIS has been problematized and questioned, because research has shown that most persons in severe paralysis, regardless of previously held preferences against such a life, are leading fulfilling lives. What foremost have been debated are the ethical and legal implications of the right to terminate one’s life, expressed through an advance directive, versus the right to life; for example, issues regarding the legal status of changes to a living will communicated through a BCI alone. Footnote 41 We do not question that these issues need ethical elaboration and analysis, but the debate thus far has lacunas that also need to be addressed. We will argue that there are compelling reasons to broaden the current perspectives. Primarily, we call for an explicit discussion regarding the actual content of the lives persons with LIS lead, instead of only providing the numbers from studies showing that the vast majority of these persons are content with their lives. In short, we suggest that there are compelling ethical reasons to acknowledge that life with LIS not only revolves around the physical impairment. As previously mentioned, it can also include being a spouse, having an active sex life, being a parent, managing a job, meeting with friends, and pursuing hobbies.
The first argument is pragmatic. By emphasizing all those things that a person actually can do while being locked in, it is more likely that the public, healthcare professionals, and other stakeholders will be able to comprehend and relate to reports of high self-esteem and satisfaction in private as well as in work life. Footnote 42 Academic discourse is one way to get the message across; however, public awareness campaigns and firsthand accounts depicted in media, books, and movies are likely to reach a wider audience. Dismantling prejudice regarding life in LIS may not only influence a clinician’s treatment regimes, but, in addition, may also reduce the number of advance directives targeting severe paralysis drawn up in the first place. Although a change will not occur over night, a growing awareness of all the sides to life with LIS has the potential to save lives that currently are lost.
The second argument for changing how persons with LIS are depicted in the current academic literature follows from the United Nations Convention on the Rights of Persons with Disabilities. Article 8 states the obligation: (b) “To combat stereotypes, prejudices and harmful practices relating to persons with disabilities, including those based on sex and age, in all areas of life”. Footnote 43 A study by Schicktanz et al., in which ten chronic patients eligible for BCI use were interviewed, indicates that a biased and stereotypical view on severe disability still prevails.
Some interviewees expressed strong concern about the social identity given to persons with disability. According to their perception a particular image of disability prevails within medical sciences, healthcare, and the public. Disability is interpreted as a ‘deficit model’ meaning that the patient’s life is depicted in a rather negative way by setting the focus on activities the patient is unable to do but are considered as “normal” and ‘necessary’ (e.g., walking, eating by using hands). Some reported how they experienced the expression of pity or taboos by others about their disability as stigmatizing or discriminating. Footnote 44
According to Schicktanz et al., the interviewees emphasized the difference between how they themselves perceive their disability, and the negative view of disability often held and expressed by other people. Because of the small number of participants in this study, more research is needed to establish how common such and other stereotypes are. It would be desirable both to ask persons with LIS, or comparable cohorts, about their experiences of being locked out, and to undertake studies designed to detect implicit biases among healthcare professionals and researchers.
Article 8 further states the obligation: 1 (c) “To promote awareness of the capabilities and contributions of persons with disabilities,” and 2 (a) (iii) “To promote recognition of the skills, merits and abilities of persons with disabilities, and of their contributions to the workplace and the labour market.” Footnote 45 All accounts, academic and other, that fail to depict those in LIS as persons with diverse personalities and interests, as well as skills and abilities, not only reinforce a view of persons with LIS, in accordance with the “deficit model” mentioned, as passive recipients of care primarily defined by their impairment, but fail to respect the fundamental rights of persons with disabilities.
Ethical Implications for BCI Research
Based on the United Nations Convention on the Rights of Persons with Disabilities, a moral responsibility toward persons in LIS can be established. This responsibility also has implications for BCI research. We suggest that this moral responsibility compels us to pursue and further BCI research.
The incentives for promoting research on BCIs for communication are compelling. For example, article 4 (g) explicitly states: “To undertake or promote research and development of, and to promote the availability and use of new technologies, including information and communications technologies, mobility aids, devices and assistive technologies, suitable for persons with disabilities, giving priority to technologies at an affordable cost.” Footnote 46
The need to pursue this research becomes even more urgent considering that the technology, as previously shown, is the key to exercising other fundamental rights, as stated in Article 3 of the United Nations Convention on Disability: (a) Respect for inherent dignity, individual autonomy including the freedom to make one’s own choices, and independence of persons; (b) Non-discrimination; (c) Full and effective participation and inclusion in society. Footnote 47 In other words, a functional assistive technology is required to enable fundamental rights; for example, to restore agency and to be able interact with, and make new contributions to, the outside world.
One objection may come to mind; article 4 (g) explicitly states that priority should be given to affordable technologies, whereas BCIs for communication is a high-cost assistive technology. Footnote 48 Although this critique is relevant for persons in incomplete or classical LIS, for whom there are alternative means of communicating, it does not apply to persons in CLIS, because at present, BCIs are the only way to reestablish communication. Therefore, as there are currently no alternatives to facilitate communication for those in CLIS, this group suffices to call for a moral responsibility to pursue targeted research on BCIs for communication. Does this, in turn, imply that we shall focus technology development on persons in CLIS alone? This may not necessarily be the case. Although present-day assistive technologies for communication represent an important breakthrough, they still display major shortcomings. Dependence on a spell board assistant infringes both on independence and on privacy. In addition, responses and communication are only possible if the assistant is at hand when a matter occurs, and an actual real-time communication is not possible, because it takes time to spell out a message. Although an eye-tracking device and a speech generator device are better options with regard to independence and privacy, these devices still cannot handle the challenges of real-time interaction, nor can the current generation of BCIs. In urgent situations, such as when someone is in severe pain or, in the words of Vigand “that my son, who has been playing by the window, is now dangling from the ledge,” Footnote 49 the time it takes to get a message across matters. Time also influences the degree of participation possible in everyday conversations. It does impact the interaction to have a time lag of 10–15 minutes when responding to anything from a joke to a comment. These examples show that improvements of the current assistive technologies are warranted, and that BCIs in some cases may prove to be the best solution not only for persons in CLIS but also for persons in LIS with some residual muscle control.
Realizing the goal of creating a functional BCI for communication requires commitment on many levels and involves more stakeholders than skilled engineers and clinicians. As a first step, the key bottlenecks that prevent the finalizing of an improved BCI must be identified and then addressed. The current technical and medical bottlenecks probably come to mind first; however, there are also, for example, structural and epistemic bottlenecks. As these are less discussed, we have chosen to focus on the two latter, the structural and epistemic bottlenecks that impact both the process of developing a functional BCI, and to what extent the technology will reach the end users. In addition, it is useful to differentiate between the bottlenecks foremost connected to BCI research and those connected to a future stage when BCIs will be broadly available for home use; that is, have become available to the end user as an established assistive technology intended for everyday life.
The structural bottlenecks are here understood as the overarching frameworks that influence (1) the development of BCIs; that is, the factors impacting the ability to pursue targeted research on BCIs, and (2) distribution; that is, the factors impacting to what extent the technology will reach persons in LIS. These bottlenecks take time to impact; therefore, it is of importance that they be addressed at an early stage. During the research phase, one example of structural dependencies are the current healthcare and research policies. Another example are trends within research; that is, in-vogue research areas more likely to obtain funding. Without proper funds, creating the next generation of BCIs for communication will not be possible. Taking a longer perspective, when the technology has become available to the end user, other structural bottlenecks become central. Insurance policies are probably the first example that comes to mind. Considering the high price of BCIs for communication (the combined NIRS/EEG BCI system used in Chaudhary et al. Footnote 50 costs approximately 70,000–80,000 USD, not including the costs for the system’s individual adaptation and training of the caregivers to operate the system), insurance policies that cover the costs of acquiring a BCI are a prerequisite to make the technology available to all eligible potential end users, not only the wealthy ones.
With this said, we do not argue that all persons in LIS automatically should be entitled to a BCI. The moral responsibility toward persons in LIS consists in enabling a functional way to communicate; the means to this end, the assistive technology employed, should vary from user to user depending on the circumstances. Therefore, LIS as such is not a sufficient criterion for receiving a BCI. From the perspective of justice, we suggest that if a person with LIS can communicate via a cheaper assistive technology, with comparable performance, it is not justified that health insurance should cover a BCI. Reimbursement should be reserved for the cases in which a BCI is required to enable communication; for example, for persons with CLIS, or when the BCI outperforms other assistive technologies. It may, in individual cases, be difficult to determine when a BCI provides a sufficient improvement to allow for the higher cost; therefore, the insurance policies developed for BCIs must be able to also handle these less clear-cut cases. These borderline cases are also of interest from a moral standpoint; therefore, more research on where the responsibilities stipulated by the United Nations disability act stop and the demands of justice take precedence is warranted. Footnote 51
Epistemic bottlenecks are here understood to be concerns related to ignorance. We will discuss two kinds of epistemic bottlenecks. The first, we argue, arises as a consequence of the fact that most present-day BCI research resides within an old research paradigm. The core of this paradigm is that it is the professionals such as researchers, clinicians, and engineers who have the necessary and sufficient knowledge for developing new technology. This view has, in recent years, been challenged. The opposition has called for a broader view of knowledge, in which user preferences and experiences also are integrated as a necessary corrective in technology development; in other words, to employ a participatory research design when developing technology acknowledges that persons in LIS have a unique expertise that complements that of the other stakeholders in the research process. Footnote 52 Through their firsthand experiences and perspective, input from persons in LIS—as well as their significant others or the caregivers who are intended to handle the technology once it reaches home use Footnote 53 —is likely to improve the end product in terms of answering to the actual needs of persons in LIS rather than relying solely on the preconceptions of a functional BCI held by clinicians and researchers. As previously noted, persons in LIS often have a different take on, for example, preferences, desires, and quality of life than that of the general public or that of clinicians and researchers, but they also may have a different take than their significant others. Footnote 54 To our knowledge, there is currently no BCI project explicitly integrating user preferences and experiences in the development of the next generation of BCIs for communication, a choice that may impact the efficiency and usability of the end product.
Therefore, what kind of correctives can be expected by integrating user preferences? One example is a recent study in which persons in LIS with intact gaze control with access to both a BCI, a visual P300 speller, and an eye tracker, expressed that they preferred the latter technology because it was faster and more accurate, and resulted in less fatigue than using the BCI. Footnote 55 This user input generates new questions that could be of relevance when developing a functional BCI; for example how do users rank parameters such as speed, accuracy, and fatigue? Further, are there (from a user perspective) other relevant parameters not surfacing in this study; and are these preferences heeded in the development of novel BCIs? With this said, it is also of importance to identify the span of preferences held by persons in LIS. Currently there are too few studies to tell what, if any, differences may emerge. Therefore, targeted research addressing those questions may add important correctives to the current development of BCIs for communication. By adding and integrating a firsthand perspective to the knowledge of the clinicians and engineers, the next generation of BCIs for communication will be better suited to accommodate the actual needs and preferences of persons in LIS.
The second epistemic constraint is created by a different kind of ignorance; the risks posed by a lack of knowledge. To promote further research on BCIs for communication, it must be made clear that this technology exists and why this research matters. We have shown, by using the few firsthand accounts available, how discrimination follows in the wake of ignorance, and that the ultimate consequence of prejudice and misconceptions regarding a life in LIS is premature deaths. Footnote 56 Therefore, it is essential to raise awareness of what LIS is, and the current situation for persons in LIS. In addition, it is crucial to ensure that, for example, clinicians, potential users, and policymakers are made aware that BCIs for communication exist, and how this technology potentially can transform the lives of persons in LIS. Footnote 57 One example of this already being a concern is indicated in a research study from 2013 in which persons in LIS listed a lack of adequate information on communication aids, and their condition, as important (currently unfulfilled) needs. Footnote 58 During the research phase, awareness campaigns could, for example, enable clinicians to refer more persons in LIS to research studies and help to raise money for BCI research.
In addition, key stakeholders involved in BCI research must be made aware that there are ratified disability acts, such as the United Nations Convention on the Rights of Persons with Disabilities. Otherwise, how can they possibly take these rights into account when conducting research, or address the current failures to answer to these rights? Ignorance can also be a bottleneck when BCIs no longer are restricted to research studies, but will be introduced for broader use at home. If neither the clinicians nor the intended users are aware of the existence of BCIs for communication, this will limit the number of persons in LIS who will receive, and be able to benefit from, a BCI. Footnote 59 Although we have argued for promoting a growing awareness of BCIs for communication, we nevertheless want to emphasize that a growing awareness of BCIs may not have only positive outcomes. When introducing BCIs to the general public, it is of great importance to give a correct depiction of the technology; that is, to make clear what the technology can, and cannot, do. If not, one form of ignorance will be replaced by another, either through creating unrealistic hopes and expectations on the one hand or unfounded fears more related to science fiction than to science on the other. Therefore, setting realistic expectations is paramount when introducing the technology to persons with LIS and other stakeholders. Footnote 60
There are a number of limitations of BCI-based technologies used for restoration of communication. These mainly relate to technical constraints that are specific to the BCI modality (EEG, functional NIRS [fNIRS], ECoG) and the cause of paralysis (e.g., ALS, brain stem stroke, spinal cord lesion, or other neurodegenerative disorders). Although EEG systems have greatly advanced over recent years in terms of size, user-friendliness, required preparation time (for example, because of the use of solid-gel electrodes) and associated costs, NIRS systems are relatively new on the market and still rather expensive (30,000–70,000 USD). There is no commercial system available that was specifically designed for day-to-day restoration of communication in severe paralysis. Most companies hesitate to develop such systems because of the relatively small market size and the high costs associated with the required medical device certification.
Although most BCI studies used EEG for restoration of communication (see Table 1 and Appendix), Footnote 61 up to now not a single patient in CLIS was able to operate such a system. The reason for this limitation is not entirely clear, but it seems to relate to pathophysiological processes associated with severe paralysis, particularly CLIS. As BCI systems based on sensory-evoked brain responses (visual, tactile, auditory) depend on the user’s integrity of sensory processing, late stages of ALS may compromise use of such BCIs. Implantation of an ECoG, providing higher signal quality of brain oscillatory activity than EEG, did not result in the ability to communicate with a BCI after the onset of CLIS. Footnote 62 Up until now, the only studies reporting successful restoration of communication despite CLIS were reported by the Birbaumer group for five cases. Footnote 63 NIRS-based BCI communication was rather slow with “yes” and “no” answers decoded over 15 seconds with at least 10 repetitions to increase classification accuracy. To further increase the communication speed, identifying the specific physiological mechanisms underlying NIRS signal modulation in this paradigm will be important. This might allow identification of other physiological features (including electrical) that will provide faster communication.
Table 1. Modalities and Paradigms Used for Brain–Computer Interface (BCI)-Based Restoration of Communication in Paralysis
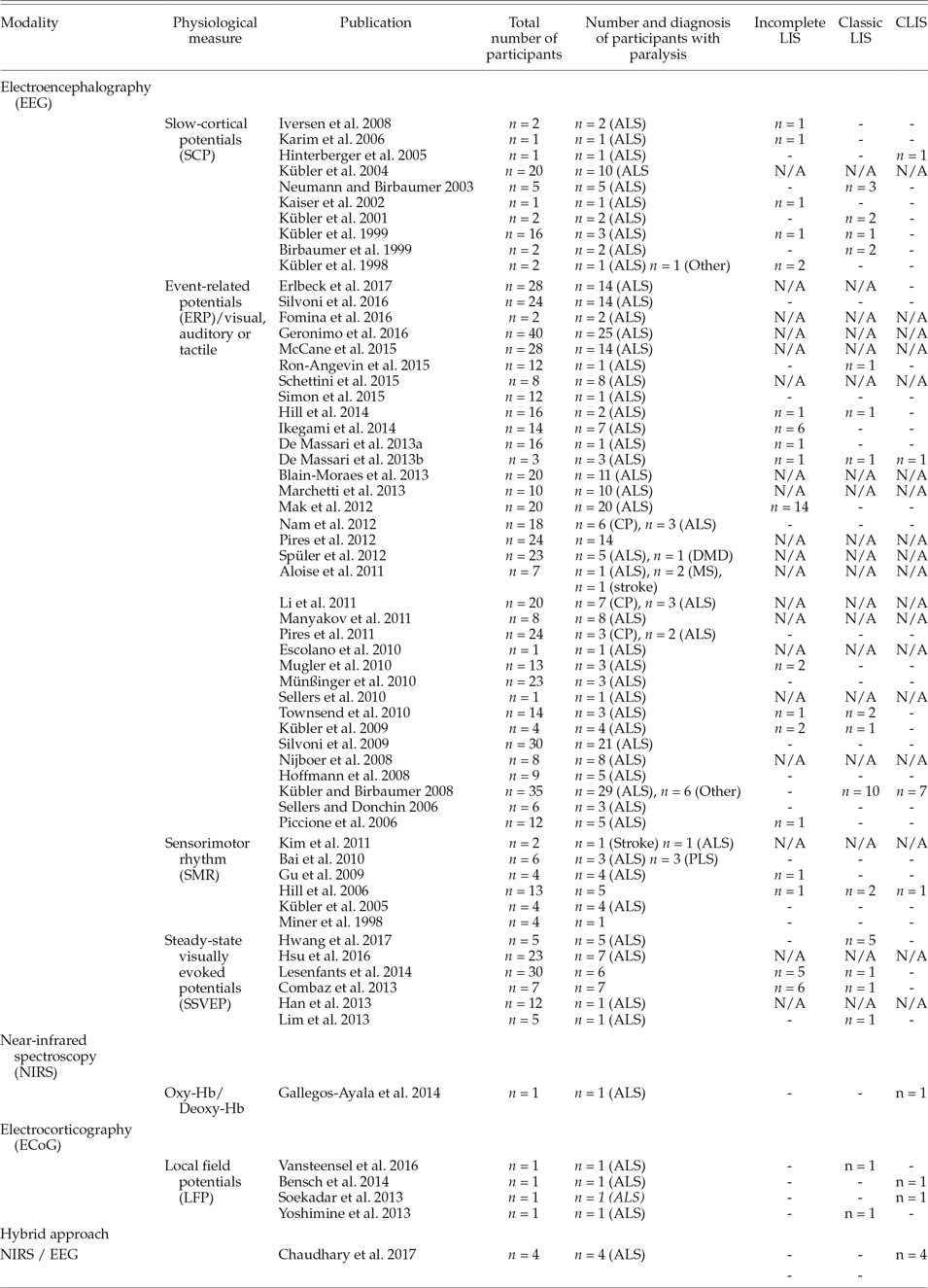
References cited in this table that are not in the article Notes are found in the Appendix.
LIS, locked-in syndrome; CLIS, complete locked-in syndrome, complete immobility, including all eye movements, combined with preserved consciousness; incomplete LIS, with remnants of voluntary movements; classical LIS, total immobility except for vertical eye movements or blinking; CLIS, ALS, amyotrophic lateral sclerosis; PLS, primary lateral sclerosis; DMD, Duchenne muscular dystrophy; CP, cerebral palsy; MS, multiple sclerosis.
Conclusions
This article identifies and elaborates on some of the lacunas in the current debate on ethics, LIS, and BCIs for communication. By using some of the few available accounts of life in LIS, told by persons with LIS, it becomes clear that they face social exclusion and stigmatization that creates barriers often perceived as more impairing than their physical condition. Although this discrimination has been discussed in other articles, one of our novel contributions is to use both academic research and autobiographies to show how these practices violate the human rights stated in the United Nations Convention on the Rights of Persons with Disabilities. It is only by providing a functional technology for communication that enabled persons in LIS to break their mental confinement and to share their experiences, that these stereotypes, discrimination, and malpractices have been outed. Therefore, these persons have a specific vulnerability, because a functional assistive technology is necessary to disclose abuse and to argue one’s own case. Another implication of our findings is that both researchers and healthcare professionals must pay careful attention to what biases and assumptions our work may unintentionally express; for example, how we perceive and depict persons in LIS, and what we include or omit in the research we publish. Thus we call for a greater awareness of the dangers of ignorance.
Furthermore, we have shown how establishing a functional way of communicating is necessary for these persons to exercise many fundamental human rights in addition to enabling participation and being a means for them to contribute to society and significant others. As a consequence, this is an ethical problem to which a technological advancement is an important part of the solution. Footnote 64 Present-day BCIs for communication have flagrant shortcomings, such as infringing on independence and privacy and being painstakingly slow. In addition, there are also persons in LIS for whom it has not been possible to establish a reliable communication; and for persons in CLIS, BCIs are currently their only hope for connecting with the outside world. Unless one’s “voice: is restored, one really is “buried alive,” alone with one’s own thoughts and sensations, with the mental capabilities for making autonomous choices intact, but with no opportunity to express agency, personality, affection, or pain. A functional assistive technology is necessary to answer to the obligations as a spouse, parent, friend, and employee, and is thereby an important tool for participation and leading a life that goes beyond “patienthood.”
Therefore, if we do not want to violate the United Nations Convention on the Rights of Persons with Disabilities, the moral imperative to ensure that every person in LIS does have a voice, either through a BCI or another comparably efficient assistive technology for communication, must be heeded. This moral imperative, in turn, requires us to take the necessary measures, as identified, to further the development of present-day BCIs for communication and to make the technology accessible to the end user. With this said, there are also other moral responsibilities toward patients in LIS, such as setting realistic expectations regarding the technology; detecting and treating depressive symptoms and failures to adjust to a life in LIS; and, when needed, providing psychological assistance. In terms of clarity, we also want to emphasize that the right to an assistive technology does not imply that a person in LIS has to use that technology. It must always be up to the individual to decide whether or when to use a BCI for communication. In addition, it is important to stress the limitations of our conclusion. This article focuses on moral considerations connected to responsibility and ignorance, raised by BCIs for communication for persons with severe paralysis. We do not claim to have covered all moral concerns—both potential harms and benefits—raised by the issue of using BCIs for communication. Footnote 65
Currently there is no cure for ALS and the majority of diseases resulting in LIS or CLIS, although we can prevent persons in LIS from being locked out. By battling ignorance—for example, through raising awareness of life in LIS and the assistive technologies available and learning from the lived experience of persons in LIS and the social barriers they are facing; by employing a healthy dose of self-reflection in all academic endeavors; and by answering the moral imperative to provide a functional technology for communication—we take important steps toward tearing down the barriers that create the locked-out state.
Appendix
Aloise F, Schettini F, Aricò P, Salinari S, Guger C, Rinsma J, et al. Asynchronous P300-based brain–computer interface to control a virtual environment: initial tests on end users. Clinical EEG and Neuroscience 2011;42:219–24.
Bai O, Lin P, Huang D, Fei DY, Floeter MK. Towards a user-friendly brain–computer interface: Initial tests in ALS and PLS patients. Clinical Neurophysiology 2010;121:1293–1303.
Bensch M, Martens S, Halder S, Hill J, Nijboer F, Ramos A, et al. Assessing attention and cognitive function in completely locked-in state with event-related brain potentials and epidural electrocorticography. Journal of Neural Engineering 2014;11(2):026006.
Birbaumer N, Ghanayim N, Hinterberger T, Iversen I, Kotchoubey B, Kübler A, et al. A spelling device for the paralysed. Nature 1999;398:297–8.
Blain–Moraes S, Mashour GA, Lee H, Huggins GE, Lee U. Altered cortical communication in amyotrophic lateral sclerosis. Neuroscience Letters 2013;543;172–6.
Chaudhary U, Xia B, Silvoni S, Cohen LG, Birbaumer N. Brain–computer interface-based communication in the completely locked-in state. PLoS Biology 2017;15(1):e1002593.
Combaz A, Chatelle C, Robben A, Vanhoof G, Goeleven A, Thijs V, et al. A comparison of two spelling brain–computer interfaces based on visual p3 and ssvep in locked-in syndrome. PloS One 2013:8(9):e73691.
De Massari D, Matuz T, Furdea A, Ruf CA, Halder S, Birbaumer N. Brain–computer interface and semantic classical conditioning of communication in paralysis. Biological Psychology 2013a;92:267–74.
De Massari D, Ruf CA, Furdea A, Matuz T, van der Heiden L, Halder S, et al. Brain communication in the locked-in state. Brain 2013b;136:1989–2000.
Erlbeck H, Mochty U, Kübler A, Real RG. Circadian course of the P300 ERP in patients with amyotrophic lateral sclerosis – implications for brain–computer interfaces (BCI). BMC Neurology 2017;17(1):3.
Escolano C, Murguialday AR, Matuz T, Birbaumer N, Minguez J. A telepresence robotic system operated with a P300-based brain–computer interface: initial tests with ALS patients. Conference Proceedings: … Annual International Conference of the IEEE Engineering in Medicine and Biology Society 2010;4476–80.
Fomina T, Lohmann G, Erb M, Ethofer T, Schölkopf B, Grosse–Wentrup M. Self-regulation of brain rhythms in the precuneus: A novel BCI paradigm for patients with ALS. Journal of Neural Engineering 2016;13(6):066021.
Gallegos–Ayala G, Furdea A, Takano K, Ruf CA, Flor H, Birbaumer N. Brain communication in a completely locked-in patient using bedside near-infrared spectroscopy. Neurology 2014;82(21):1930–2.
Geronimo A, Simmons Z, Schiff SJ. Performance predictors of brain–computer interfaces in patients with amyotrophic lateral sclerosis. Journal of Neural Engineering 2016;13(2):026002.
Gu Y, Farina D, Murguialday AR, Dremstrup K, Montoya P, Birbaumer N. Offline identification of imagined speed of wrist movements in paralyzed ALS patients from single-trial EEG. Frontiers in Neuroscience 2009;3:62.
Han CH, Hwang HJ, Lim JH, Im CH. Development of an “eyes-closed” brain–computer interface system for communication of patients with oculomotor impairment. Conference Proceedings: Annual International Conference of the IEEE Engineering in Medicine and Biology Society 2013;2236–9.
Hill NJ, Lal TN, Schröder M, Hinterberger T, Wilhelm B, Nijboer F, et al. Classifying EEG and ECoG signals without subject training for fast BCI implementation: Comparison of nonparalyzed and completely paralyzed subjects. IEEE Transactions on Neural Systems and Rehabilitation Engineering 2006;14:183–6.
Hill NJ, Ricci E, Haider S, McCane LM, Heckman S, Wolpaw JR, et al. A practical, intuitive brain–computer interface for communicating ‘yes’ or ‘no’ by listening. Journal of Neural Engineering 2014;11(3):035003.
Hinterberger T, Birbaumer N, Flor H. Assessment of cognitive function and communication ability in a completely locked-in patient. Neurology 2005;64:1307–8.
Hoffmann U, Vesin J, Ebrahimi T, Diserens K. An efficient P300-based brain–computer interface for disabled subjects. Journal of Neuroscience Methods 2008;167:115–25.
Hsu HT, Lee IH, Tsai HT, Chang HC, Shyu KK, Hsu CC, et al. Evaluate the feasibility of using frontal SSVEP to implement an SSVEP-based BCI in young, elderly and ALS Groups. IEEE Transactions on Neural Systems and Rehabilitation Engineering 2016;24(5):603–15.
Hwang HJ, Han CH, Lim JH, Kim YW, Choi SI, An KO, et al. Clinical feasibility of brain-computer interface based on steady-state visual evoked potential in patients with locked-in syndrome: Case studies. Psychophysiology 2017;54:444–51.
Ikegami S, Takano K, Kondo K, Saeki N, Kansaku K. A region-based two-step P300-based brain–computer interface for patients with amyotrophic lateral sclerosis. Clinical Neurophysiology 2014;125(11):2305–12.
Iversen IH, Ghanayim N, Kübler A, Neumann N, Birbaumer N, Kaiser J. A brain–computer interface tool to assess cognitive functions in completely paralyzed patients with amyotrophic lateral sclerosis. Clinical Neurophysiology 2008;119:2214–23.
Kaiser J, Kübler A, Hinterberger T, Neumann N, Birbaumer N. A non-invasive communication device for the paralyzed. Minimally Invasive Neurosurgery 2002;45(1):19–23.
Karim AA, Hinterberger T, Richter J, Mellinger J, Neumann N, Flor H, et al. Neural internet: Web surfing with brain potentials for the completely paralyzed. Neurorehabilitation and Neural Repair 2006;20:508–15.
Kim SP, Simeral JD, Hochberg LR, Donoghue JP, Friehs GM. Point-and-click cursor control with an intracortical neural interface system by humans with tetraplegia. IEEE Transactions on Neural Systems and Rehabilitation Engineering 2011;19:193–203.
Kübler A, Birbaumer N. Brain–computer interfaces and communication in paralysis: extinction of goal directed thinking in completely paralysed patients? Clinical Neurophysiology 2008;119:2658–66.
Kübler A, Furdea A, Halder S, Hammer EM, Nijboer, Kotchoubey B. A brain–computer interface controlled auditory event-related potential (p300) spelling system for locked-in patients. Annals of the New York Academy of Science 2009;1157;90–100.
Kübler A, Kotchoubey B, Hinterberger T, Ghanayim N, Perelmouter J, Schauer M, et al. The thought translation device: A neurophysiological approach to communication in total motor paralysis. Experimental Brain Research 1999;124:223–32.
Kübler A, Kotchoubey B, Salzmann HP, Ghanayim N, Perelmouter J, Hömberg V, et al. Self-regulation of slow cortical potentials in completely paralyzed human patients. Neuroscience Letters 1998;252;171–4.
Kübler A, Neumann N, Kaiser J, Kotchoubey B, Hinterberger T, Birbaumer N. Brain–computer communication: Self-regulation of slow cortical potentials for verbal communication. Archives of Physical Medicine and Rehabilitation 2001;82:1533–9.
Kübler A, Neumann N, Wilhelm B, Hinterberger T, Birbaumer N. Predictability of brain–computer communication. Journal of Psychophysiology 2004;18:121–9.
Kübler A, Nijboer F, Mellinger J, Vaughan TM, Pawelzik H, Schalk G, et al. Patients with ALS can use sensorimotor rhythms to operate a brain–computer interface. Neurology 2005;64:1775–7.
Lesenfants D, Habbal D, Lugo Z, Lebeau M, Horki P, Amico E, et al. An independent SSVEP-based brain–computer interface in locked-in syndrome. Journal of Neural Engineering 2014;11(3):035002.
Li Y, Nam CS, Shadden BB, Johnson SL. A P300-based brain–computer interface: effects of interface type and screen size. International Journal of Human-Computer Interaction 2011;27:52–68.
Lim JH, Hwang HJ, Han CH, Jung KY, Im CH. Classification of binary intentions for individuals with impaired oculomotor function: “eyes–closed” SSVEP–based brain–computer interface (BCI). Journal of Neural Engineering 2013;10:026021.
Mak JN, McFarland DJ, Vaughan TM, McCane LM, Tsui PZ, Zeitlin DJ, et al. EEG correlates of P300–based brain–computer interface (BCI) performance in people with amyotrophic lateral sclerosis. Journal of Neural Engineering 2012;9:026014.
Manyakov NV, Chumerin N, Combaz A, Van Hulle MM. Comparison of classification methods for P300 brain–computer interface on disabled subjects. Computational Intelligence and Neuroscience 2011;2011:519868;
Marchetti M, Piccione F, Silvoni S, Gamberini L, Priftis K. Covert visuospatial attention orienting in a brain-computer interface for amyotrophic lateral sclerosis patients. Neurorehabilitation and Neural Repair 2013;27(5)430–438.
McCane LM, Heckman SM, McFarland DJ, Townsend G, Mak JN, Sellers E, et al. P300–based brain–computer interface (BCI) event-related potentials (ERPs): People with amyotrophic lateral sclerosis (ALS) vs. age-matched controls. Clinical Neurophysiology 2015;126(11):2124–31.
Miner LA, McFarland DJ, Wolpaw JR. Answering questions with an electroencephalogram-based brain–computer interface. Archives of Physical Medicine and Rehabilitation 1998;79:1029–33.
Mugler EM, Ruf CA, Halder S, Bensch M, Kubler A. Design and implementation of a P300-based brain–computer interface for controlling an internet browser. IEEE Transactions on Neural Systems and Rehabilitation Engineering 2010;18:599–609.
Münßinger JI, Halder S, Kleih SC, Furdea A, Raco V, Hösle A, et al. Brain painting: First evaluation of a new brain–computer interface application with ALS–patients and healthy volunteers. Frontiers in Neuroscience 2010;4:182.
Nam CS, Woo J, Bahn S. Severe motor disability affects functional cortical integration in the context of brain–computer interface (BCI) use. Ergonomics 2012;55:581–91.
Neumann N, Birbaumer N. Predictors of successful self control during brain–computer communication. Journal of Neurology, Neurosurgery, and Psychiatry 2003;74;1117–21.
Nijboer F, Sellers EW, Mellinger J, Jordan MA, Matuz T, Furdea A, et al. A P300-based brain–computer interface for people with amyotrophic lateral sclerosis. Clinical Neurophysiology 2008;119:1909–16.
Piccione F, Giorgi F, Tonin P, Priftis K, Giove S, Silvoni S, et al. P300-based brain computer interface: reliability and performance in healthy and paralysed participants. Clinical Neurophysiology 2006;117:531–7.
Pires G, Nunes U, Castelo–Branco M. Comparison of a row–column speller vs a novel lateral single-character speller: assessment of BCI for severe motor disabled patients. Clinical Neurophysiology 2012;123:1168–81.
Pires G, Nunes U, Castelo–Branco M. Statistical spatial filtering for a P300-based BCI: Tests in able-bodied, and patients with cerebral palsy and amyotrophic lateral sclerosis. Journal of Neuroscience Methods 2011;195:270–81.
Ron-Angevin R, Varona–Moya S, da Silva–Sauer L. Initial test of a T9-like P300-based speller by an ALS patient. Journal of Neural Engineering 2015;12(4):046023.
Schettini, F, Riccio, A, Simione, L, Liberati, G, Caruso, M, Frasca, V, et al. Assistive device with conventional, alternative, and brain-computer interface inputs to enhance interaction with the environment for people with amyotrophic lateral sclerosis: a feasibility and usability study. Archives of Physical Medicine and Rehabilitation 2015;96(3):S46–S53
Sellers EW, Donchin E. A P300-based brain–computer interface: Initial tests by ALS patients. Clinical Neurophysiology 2006;117:538–48.
Sellers EW, Vaughan TM, Wolpaw JR. A brain–computer interface for long-term independent home use. Amyotrophic Lateral Sclerosis and Frontotemporal Degeneration 2010;11:449–55.
Silvoni S, Volpato C, Cavinato M, Marchetti M, Priftis K, Merico A, et al. P300-based brain–computer interface communication: evaluation and follow-up in amyotrophic lateral sclerosis. Frontiers in Neuroscience 2009;3:60.
Silvoni S, Konicar L, Prats-Sedano MA, Garcia-Cossio E, Genna C, Volpato C, Cavinato M, Paggiaro A, Veser S, De Massari D, Birbaumer N. Tactile event-related potentials in amyotrophic lateral sclerosis (ALS): Implications for brain-computer interface. Clinical Neurophysiology 2016;127:936–45.
Simon N, Käthner I, Ruf CA, Pasqualotto E, Kübler A, Halder S. An auditory multiclass brain–computer interface with natural stimuli: Usability evaluation with healthy participants and a motor impaired end user. Frontiers in Human Neuroscience 2015;8:1039.
Soekadar SR, Born J, Birbaumer N, Bensch M, Halder S, Murguialday AR, et al. Fragmentation of slow wave sleep after onset of complete locked-in state. Journal of Clinical Sleep Medicine 2013;9(9):951–3.
Spüler M, Bensch M, Kleih S, Rosenstiel W, Bogdan M, Kübler A. Online use of error-related potentials in healthy users and people with severe motor impairment increases performance of a P300-BCI. Clinical Neurophysiology 2012;123(7):1328–37.
Townsend G, Lapallo BK, Boulay CB, Krusienski DJ, Frye GE, Hauser CK, et al. A novel P300-based brain–computer interface stimulus presentation paradigm: Moving beyond rows and columns. Clinical Neurophysiology 2010;121:1109–20.
Vansteensel MJ, Pels EG, Bleichner MG, Branco MP, Denison T, Freudenburg ZV, et al. Fully implanted brain–computer interface in a locked-in patient with ALS. New England Journal of Medicine 2016;375(21):2060–6.
Yoshimine T, Yanagisawa T, Sawada J, Hazama T, Mochizuki H, Hirata M. Communication with ALS patients: neurosurgical approach [in Japanese]. Rinsho Shinkeigaku 2013;53(11):1405–7.



