Poor diet quality and excess weight gain are common among people in recovery from substance addiction( Reference Cowan and Devine 1 – Reference Emerson, Glovsky and Amaro 4 ), although nutritional status may vary with personal characteristics and addiction and health history( Reference Barry and Petry 5 – Reference Saeland, Haugen and Eriksen 7 ). Public health initiatives to improve nutritional status in this population are critical given the central role that nutrition plays in health, obesity prevention and diet-related chronic diseases for which recovering addicts are at increased risk( Reference Howard, Arnsten and Gourevitch 8 – Reference Kuehn 13 ).
A substantial number of adults in North America and Europe abuse or are dependent on alcohol or illicit drugs( 14 – 16 ), and drug abuse is increasing in non-Western countries (e.g. ( Reference Nazrul Islam, Hossain and Ahmed 17 , 18 )). An estimated four million people receive treatment at specialty substance-abuse settings such as rehabilitation facilities in the USA, and about one million Europeans receive treatment for substance abuse annually. Abstinence from drug and alcohol use is usually the main focus of treatment modalities. Considerable time and effort is spent to facilitate sobriety in the lives of the recovering addicts, but little attention is given to dietary behaviours and weight management even though there is strong evidence for concern. RHEALTH was designed as an environmental and educational nutrition intervention to improve the diets and body composition of men in residential drug-treatment facilities.
Interventions that address the organizational food environment have emerged as a new strategy to support individual behaviour change, especially in worksite and school settings( Reference Beresford, Shannon and McLerran 19 – Reference Steckler, Ethelbah and Martin 22 ), but the combined contributions of environmental change and educational programming have not been examined in community residential settings such as those for treatment of substance abuse.
Increasing emphasis has been placed on the use of process evaluations to determine the success of field-based health interventions( Reference Matheson, Doherty and Grant 23 – Reference Baranowski, Cerin and Baranowski 25 ). Process evaluation can capture variability in programme implementation in multiple community settings and be an effective set of tools for understanding why a programme succeeded or failed( Reference Baranowski and Stables 26 , Reference Saunders, Evans and Joshi 27 ).
The purpose of the present research was to investigate the implementation of the educational and environmental elements of an intervention designed to promote healthy eating and reduce excess weight gain among men in residential substance-abuse treatment facilities. Specifically, the investigators wanted to learn to what extent the intervention was implemented and how study outcomes differed by site. We hypothesized that sites with high participation and implementation fidelity would report more positive changes in diet quality and anthropometric measures of study participants.
Experimental methods
Intervention design
RHEALTH (Recovery healthy eating and active learning in treatment houses) used a quasi-experimental design with a 6-week control period followed by a 6-week treatment period in each of six residential urban drug-treatment facilities in Upstate New York. The study participants, who were ethnically diverse men aged 18 years and older residing in each of the drug-treatment facilities, served as their own controls. Residents in sites 1–5 served on rotating cook teams that prepared the evening meals five days a week; site 6 hired cooks.
The six study sites were recruited through referrals and prior research within the study population; all sites agreed to participate when approached. All residents of the six treatment facilities (n 107) were invited to participate in the study through house meetings, signs and individual interactions. The main intervention outcomes were dietary intake (total energy, percentage of energy from fat, percentage of energy from sweets, daily servings of fats, oils and sweets, daily servings of fruits and vegetables), BMI and waist circumference.
Dietary intake was assessed using the Block 2005 FFQ( 28 ) during three face-to-face interviews: (i) at baseline, followed after 6 weeks by (ii) a pre-intervention assessment, then a 6-week treatment period, followed by (iii) a post-intervention assessment. At each of the three assessments, data were also collected on participants’ sociodemographic characteristics, addiction history, and measured height, weight and weight circumference. Physical activity was evaluated by self-report( 29 ). The study was approved by the Cornell University Institutional Review Board, and was conducted between June 2007 and June 2008.
The RHEALTH intervention targeted eating behaviour, cooking skills and changes in the food environment in the six residential drug-treatment facilities based on formative research in this population( Reference Cowan 2 ), a social ecological framework( Reference Green and Kreuter 30 ) and social cognitive theory( Reference Bandura 31 ).
The intervention included: (i) an education component consisting of weekly on-site nutrition and cooking classes for all residents, led by the primary researcher, to improve dietary behaviour and cooking skills; and (ii) a food environment component consisting of policy and procedural changes in the residential food service environment to increase healthy food choice opportunities for all residents. For the food environment component, the same researcher worked with eight food service staff (one each in four sites, two each in two sites) to implement ten essential food environment elements (nine food elements plus researcher meetings with staff). The food elements included: providing lower-fat milks; omitting Kool-Aid and other sugary drinks; providing water and 100 % juices daily; offering fruit and/or vegetable salads at dinner; offering choices of fruits and vegetables daily; offering a vegetarian or meatless dish at least once weekly; offering lower-fat snacks; limiting the amount of sweetened and sugary foods; and limiting fried foods. Food service staff were also asked to participate in one initial and three follow-up meetings. Intervention details are available elsewhere( Reference Cowan 2 ).
Process evaluation
The RHEALTH process evaluation documented: (i) nutrition class attendance; (ii) completeness of the nutrition education (dose delivered); (iii) participant satisfaction (feedback) with nutrition classes and cooking activities; and (iv) food environment changes (fidelity and completeness) through direct observations and interviews with key staff and residents( Reference Saunders, Ward and Felton 21 , Reference Steckler, Ethelbah and Martin 22 , Reference Baranowski and Stables 26 , Reference Saunders, Evans and Joshi 27 , Reference Linnan and Steckler 32 ). Finally, (v) contextual factors that might have influenced the completeness of RHEALTH implementation and the quality of the programme were documented in order to interpret the findings( Reference Johnson, Lai and Rice 20 , Reference Saunders, Evans and Joshi 27 , Reference Linnan and Steckler 32 ). The primary investigator implemented and assessed all of the nutrition education elements. The food service coordinator in each site was responsible for implementing all food environment elements in his/her site. The process evaluation components and measures of each are presented in Table 1.
Table 1 Process measures of class attendance, nutrition education and food environment elements of the RHEALTH intervention

| Essential elements | Data collection tools | Time collected | Process evaluation components | Rating scale |
| Class attendance | Attendance log, programme and admission information | End of class | Participation | RHEALTH enrolment/facility occupancy |
| Nutrition education elements | ||||
| Six weekly nutrition classes | Class checklist, field notes | End of class | Dose delivered | 3 = all; 2 = most; 1 = some; 0 = no/none |
| Handouts with key nutrition concepts | Class checklist, field notes | End of class | Dose delivered | 3 = all of the time; 2 = most of the time; 1 = sometimes; 0 = no/none |
| Class activities | Class checklist, field notes | End of class | Dose delivered | As above |
| Cooking activities including all recipes | Recipe checklist, field notes | End of class | Dose delivered | As above |
| Tasting | Recipe checklist, field notes | End of class | Dose delivered | As above |
| Food Guide Pyramid poster displayed | Direct observation | During intervention | Dose delivered | As above |
| Weekly take-home challenges | Direct observation | During intervention | Dose delivered | As above |
| Participant satisfaction | Class feedback questionnaire | End of class | Exposure | 2 = class fun & interesting, recipes great; 1 = class & recipes ok, not bad; 0 = class boring, recipes disliked |
| Food environment elements | ||||
| Food elements (n 9) | Shopping list, observation, food inventory, interviews with staff and residents | Before, during, end of 6-week intervention | Dose fidelity | 3 = yes, completely; 2 = most of the time; 1 = sometimes; 0 = no/none |
| Meetings with food service staff (initial+3 follow-ups) | Implementer log | Before, during, end of 6-week intervention | Dose fidelity | Yes or no each meeting (initial = 3 points; follow-up = 1 point each of 3) |
Class attendance
Class attendance (participation) in each of the six weekly nutrition classes was recorded to document class participation. Programme admission records from each site provided treatment facility occupancy. Participants were recruited into the classes through the face-to-face interviews conducted prior to the intervention, personal interactions with the primary researcher, and peer and staff reminders. All of the site residents were eligible and encouraged (but not required) to participate.
Nutrition education (dose delivered)
Nutrition education (dose delivered) was assessed through a checklist, field notes and observations that documented the completion of each of seven planned nutrition education elements with residents.
Participant satisfaction
Participant satisfaction was assessed using a feedback survey that included the level of residents’ exposure to the nutrition education elements and satisfaction with each of the nutrition education classes and cooking activities.
Food environment
Food environment (fidelity of implementation) changes were assessed through direct observations (with field notes) by the primary investigator who reviewed shopping lists, weekly menus and food inventories in each of the six facilities, and observed meals. In addition to initial meetings with key staff, the investigator also conducted three interviews (beginning, midpoint and end of the 6-week intervention period) with the key staff and participant informants in each site. Staff and participant informants were selected because of their food service responsibilities including food inventory and procurement, menu planning and food preparation.
Contextual factors
Contextual factors at intervention sites were also documented during the semi-structured interviews with eight food service staff and twelve key participant informants. Informants were asked to describe in their own words the changes they had noticed in menus, shopping lists and the eating patterns during the programme as well as other relevant events in the treatment facilities.
Data analysis
Descriptive analyses of study participants’ sociodemographic characteristics and addiction histories were conducted; ANOVA and χ 2 analyses were used to compare mean differences among the six sites. Only the fifty-five participants who had at least two assessments (before and after the intervention) were included in the descriptive and mixed-model analyses to assess key study outcomes.
Class attendance/participation was calculated by dividing the total number of participants who attended each nutrition education class by the treatment facility occupancy at the start of study recruitment. Sites were categorized into higher and lower class participation sites based on their mean attendance scores.
Nutrition education dose delivered was calculated by dividing the dose delivered score in each site by the total possible score for the seven nutrition education elements.
Implementation of the food environment elements was calculated by dividing the food environment mean score on the food environment elements by the total possible score for the ten elements.
Treatment programme facilities were categorized as higher or lower implementation sites based on percentile rank of the scores for the participation and food environment components( Reference Saunders, Ward and Felton 21 ). Sites scoring high and low on attendance and food environment were compared on the implementation of essential food environment elements using the Wilcoxon rank sum scores test. A significance level of P ≤ 0·05 was accepted for all tests. Education dose delivered scores were not included in this classification because of high scores for this component at all sites.
A mixed-model analysis of covariance was used to investigate the relationship between the higher and lower participation and implementation sites and the primary study outcomes (changes in dietary intake, BMI and waist circumference). Analyses were adjusted for baseline values and time in treatment programme for the dietary outcomes; age, education and baseline physical activity were included in the adjusted analysis for body composition outcomes. The quantitative data were analysed using the SPSS for Windows statistical software package version 16 (SPSS Inc., Chicago, IL, USA). Qualitative data analysis based on a constant comparison method described by Ryan and Bernard( Reference Ryan and Bernard 33 ) was employed to assess information about contextual factors during the interviews with staff and participants.
Results
At baseline, 103 men (96 % of all occupants in the six treatment facilities) provided baseline data and enrolled in the study. Fifty-five men (55 %) who provided both baseline and post-intervention data across the six study sites remained in the study (Table 2); thirty-two men (31 %) dropped out of the treatment programme (and the study) due to substance-use relapses, and sixteen (16 %) left because of graduation or completion of treatment. Men who dropped out were younger and reported shorter addiction histories( Reference Cowan 2 ). There were statistically significant differences in mean age, addiction histories (time in treatment programme and sobriety) and employment status by site. Notably, participants in site 6 were older, had been in the treatment programme longer and were more likely to be unemployed before their current treatment episode than participants in the other sites.
Table 2 Sociodemographic characteristics and addiction histories of participants (n 55) at six urban residential drug-treatment facilities in Upstate New York

| Site 1 | Site 2 | Site 3 | Site 4 | Site 5 | Site 6 | |||||||
| Site n* | 9 | 10 | 5 | 7 | 15 | 9 | ||||||
| Programme occupancy† | 18 | 16 | 13 | 12 | 28 | 20 | ||||||
| Mean | sd | Mean | sd | Mean | sd | Mean | sd | Mean | sd | Mean | sd | |
| Age (years)‡ | 47·7 | 7·1 | 41·7 | 11·0 | 45·3 | 5·7 | 39·6 | 6·0 | 43·4 | 7·8 | 50·6 | 2·9 |
| Time in treatment programme (months)§ | 5·8 | 5·0 | 5·7 | 4·0 | 3·6 | 2·2 | 2·2 | 0·98 | 2·8 | 1·3 | 6·4 | 1·8 |
| Drug treatments | 5·4 | 5·1 | 4·1 | 1·7 | 7·8 | 3·1 | 7·1 | 6·8 | 7·3 | 4·8 | 5·5 | 5·3 |
| Sobriety (months)∥ | 15·1 | 14·9 | 7·4 | 4·0 | 4·4 | 2·1 | 4·5 | 5·6 | 5·0 | 2·7 | 8·8 | 6·7 |
| Addiction years | 25·7 | 7·6 | 21·7 | 10·6 | 32·4 | 5·3 | 20·1 | 10·0 | 24·6 | 10·5 | 28·2 | 7·4 |
| n | % | n | % | n | % | n | % | n | % | n | % | |
| Race | ||||||||||||
| White | 4 | 44 | 4 | 40 | 1 | 20 | 4 | 57 | 6 | 40 | 1 | 11 |
| Black | 4 | 44 | 4 | 40 | 3 | 60 | 3 | 43 | 5 | 33 | 6 | 67 |
| Hispanic | 1 | 12 | 0 | 0 | 0 | 0 | 0 | 0 | 3 | 20 | 1 | 11 |
| Other | 0 | 0 | 2 | 20 | 1 | 20 | 0 | 0 | 1 | 7 | 1 | 11 |
| Education | ||||||||||||
| ≥High school/GED | 9 | 100 | 8 | 60 | 4 | 80 | 7 | 100 | 12 | 80 | 6 | 67 |
| Marital status | ||||||||||||
| Single/divorced/separated | 7 | 77 | 9 | 90 | 5 | 100 | 7 | 100 | 15 | 93 | 9 | 100 |
| Unemployed before treatment¶ | 5 | 56 | 4 | 40 | 4 | 80 | 6 | 86 | 13 | 87 | 9 | 100 |
GED, general educational development.
*Study participants who provided data at both baseline and follow-up points.
†Treatment programme occupancy at baseline.
‡Overall F = 2·49, P = 0·044.
§Overall F = 3·32, P = 0·012.
∥Overall F = 2·82, P = 0·026.
¶Overall χ 2 = 12·77, P = 0·026.
The mean nutrition education class participation rate across the six study sites was 63 %. Four sites (1, 3, 4 and 5) were placed in the higher class participation group (64–76 %) and two sites (2 and 6) comprised the lower class participation (50–56 %) group (Table 3).
Table 3 RHEALTH class participation, nutrition education dose delivered and food environment element implementation across the six urban residential drug-treatment facilities in Upstate New York

| Site 1 | Site 2 | Site 3 | Site 4 | Site 5 | Site 6 | |||||||
| Mean class participation (%)* | 67 | 56 | 64 | 76 | 65 | 50 | ||||||
| Mean score | % | Mean score | % | Mean score | % | Mean score | % | Mean score | % | Mean score | % | |
| Nutrition education | ||||||||||||
| Dose delivered† | 21 | 100 | 19 | 90 | 20 | 95 | 18 | 86 | 20 | 90 | 20 | 95 |
| Food environment | ||||||||||||
| Implementation‡ | 73 | 84 | 53 | 61 | 67 | 77 | 69 | 79 | 66 | 76 | 31 | 36 |
*Mean attendance across six nutrition education classes.
†Nutrition education elements delivered (out of 21 total points).
‡Food environment elements implemented (out of 87 total points).
The mean nutrition education dose delivered for all study sites combined was 94 % with no meaningful differences across sites. The educational dose delivered ranged from 100 % (site 1) to 86 % (site 4; Table 3).
Participants in all study sites reported a high level of positive satisfaction with the nutrition classes and cooking activities (data not shown). Rarely did the percentage reporting satisfaction with the nutrition class or recipes drop below 80 %; lower satisfaction was noted for the portion control (site 4) and vegetables classes (sites 4 and 5).
The fidelity of implementation of the combined food environment elements ranged from 36 % to 84 % among sites (Table 3). On average, the six study sites implemented nine of the ten required food environment elements. The most frequently adopted food environment element for all of the sites combined was ‘offer choices of fruits and vegetables daily’. No site implemented the vegetarian/meatless dish option on the weekly dinner menu. Sites 2 (61 %) and 6 (36 %) had the lowest fidelity rates and were put into the low implementation group because the scores were at or below the lower quartile; the four remaining sites (1, 3, 4 and 5), with fidelity rates from 76 to 84 %, were classified as high implementers.
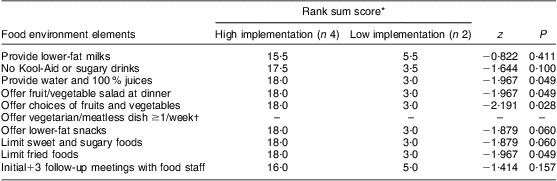
A comparison of fidelity on the food environment elements (Table 4) confirmed that sites in the high participation and implementation group did report significantly higher implementation for four out of the nine essential food environment elements: providing water and 100 % juices daily, offering fruit and/or a vegetable salad at each dinner, offering choices of fruits and vegetables daily, and limiting fried foods on the weekly menus.
Table 4 Comparison of food environment element implementation for sites scoring high (1, 3, 4 and 5) and low (2 and 6) on participation and implementation among the six urban residential drug-treatment facilities in Upstate New York
| Rank sum score* | ||||
| Food environment elements | High implementation (n 4) | Low implementation (n 2) | z | P |
| Provide lower-fat milks | 15·5 | 5·5 | −0·822 | 0·411 |
| No Kool-Aid or sugary drinks | 17·5 | 3·5 | −1·644 | 0·100 |
| Provide water and 100 % juices | 18·0 | 3·0 | −1·967 | 0·049 |
| Offer fruit/vegetable salad at dinner | 18·0 | 3·0 | −1·967 | 0·049 |
| Offer choices of fruits and vegetables | 18·0 | 3·0 | −2·191 | 0·028 |
| Offer vegetarian/meatless dish ≥1/week† | – | – | – | – |
| Offer lower-fat snacks | 18·0 | 3·0 | −1·879 | 0·060 |
| Limit sweet and sugary foods | 18·0 | 3·0 | −1·879 | 0·060 |
| Limit fried foods | 18·0 | 3·0 | −1·967 | 0·049 |
| Initial+3 follow-up meetings with food staff | 16·0 | 5·0 | −1·414 | 0·157 |
*See Table 1 for scoring details on each element.
†Not implemented in any site and not scored.
The sites grouped as high (1, 3, 4 and 5) and low (2 and 6) for both class participation and implementation of the food environment elements were the same. The two sites that were placed in the low implementation group had scores that were at or below the lower quartile, an approach that is consistent with prior research in this area( Reference Saunders, Ward and Felton 21 ). All six sites scored very high in nutrition class implementation; therefore these scores were not included in subsequent analysis. As hypothesized, participants in the high participation and implementation sites reported greater reductions in mean total energy, percentage of energy from sweets, daily servings of fats, oils and sweets and BMI than those in the lower implementation sites (Table 5). The overall effect of the implementation levels on changes in these dietary outcomes remained significant even after adjusting for baseline values and the length of time spent in the treatment programme. Unexpectedly, participants in the lower implementation sites reported significantly greater reductions in percentage of energy from fat at the end of the intervention than participants in the higher implementation sites.
Table 5 Changes in diet, BMI and waist circumference according to high and low class participation and food environment implementation in participants from the six urban residential drug-treatment facilities in Upstate New York

| Class participation and food environment implementation group* | ||||||||||
| Unadjusted | Adjusted† | |||||||||
| Higher (n 36) | Lower (n 19) | Higher (n 36) | Lower (n 19) | |||||||
| Change in outcomes | Mean | sd | Mean | sd | Mean | se | Mean | se | F | P |
| Total energy (kJ) | –2687 | 4224 | –2077 | 3098 | –2738 | 883 | –1976 | 624 | 3·321 | 0·030 |
| Total energy (kcal) | −642 | 1009 | −496 | 740 | −654 | 211 | −472 | 149 | 3·321 | 0·030 |
| % of energy from fat | −1·30 | 4·0 | −2·41 | 5·3 | −1·03 | 0·65 | −2·92 | 0·91 | 8·650 | <0·001 |
| % of energy from sweets | −3·53 | 1·1 | −3·07 | 1·4 | −3·54 | 1·50 | −3·05 | 2·10 | 15·200 | <0·001 |
| Daily servings of fats, oils, sweets | −1·38 | 1·9 | −0·34 | 2·6 | −1·25 | 0·33 | −0·58 | 0·46 | 6·504 | <0·005 |
| Daily servings of vegetables | 0·853 | 2·0 | 1·23 | 2·5 | 0·73 | 0·37 | 1·46 | 0·52 | 1·054 | 0·370 |
| Daily servings of fruit | 0·631 | 1·0 | 0·88 | 1·3 | 0·54 | 0·19 | 1·05 | 0·26 | 2·700 | 0·060 |
| BMI (kg/m2) | −0·66 | 0·2 | −0·80 | 3·1 | −2·50 | 0·46 | −2·00 | 0·50 | 7·410 | <0·001 |
| Waist circumference (cm) | −0·913 | 5·2 | −2·79 | 4·4 | −1·65 | 1·50 | 2·77 | 1·60 | 1·196 | 0·320 |
*Sites 1, 3, 4 and 5 were in the higher participation and implementation group; sites 2 and 6 in the lower participation and implementation group.
†Controlling for site, baseline values and time in treatment programme for diet; age, education and baseline physical activity for BMI; P ≤ 0·05.
Contextual factors from interviews with key staff and participant informants and from observations indicated that variation in implementation and participation may have been related to events or activities outside the intervention, including staff involvement, staff turnover and resident turnover.
There was evidence of high staff involvement in high participation and high implementation sites. Staff members in these sites strongly encouraged residents to attend the weekly nutrition classes. For example, one participant reported: ‘The supervisor has been a big promoter of this too [the intervention]’; and a staff informant said: ‘The project is a good idea because it provides insight into proper nutrition ... good timing, good hands-on experience for the guys!’
The sites with low class participation and food environment implementation had the least staff involvement. The staff food service coordinator in one site wore ‘multiple hats’ in the treatment programme. He was responsible for coordinating all the food service activities as well as housekeeping and maintenance activities in the facility, and he was sent to another treatment facility in a different city to assist with programme management during the intervention period.
Low implementation was reported by residents in the low-implementing sites. When asked about the food service implementation one key informant interviewed midway into the intervention implementation said:
They haven't made much change since you've been here; they still haven't been serving a lot of vegetables, still a lot of fried foods, no diabetic menus. I brought it up to staff that they have nutrition class but still haven't changed the nutrition.
All six intervention sites were operating below full capacity at the beginning of the intervention, and they were constantly admitting new residents because of staff-initiated discharges resulting from substance-abuse relapses. These events changed the dynamics of the treatment environment and the food culture as new eating behaviours relating to residents’ stages of recovery were exhibited. For example, during the intervention period, one high implementation site experienced a high resident turnover that affected the food culture and environment. The staff food service coordinator described the changes this way:
The new residents are out of control … a whole new culture because of the new guys came into the house … it's hard to believe that two or three people can change the culture of the house.
More in-depth descriptions of the contextual factors are available elsewhere( Reference Cowan 2 ).
Discussion
These process evaluation results demonstrate the importance of examining the separate and combined contributions of an intervention that combines environmental and educational components. The educational components were successful in all sites, due in part to delivery by a single external individual; however the success of environmental changes in food service differed by site characteristics and changes in those characteristics. This evaluation illuminates areas in which the RHEALTH intervention worked as planned and areas needing improvement.
These process data demonstrate that dose and implementation of the nutrition education curriculum was high across all intervention sites. The successful implementation of RHEALTH may have been based, in part, on having a single individual conducting all of the activities. High participant satisfaction ratings indicated that the nutrition education classes and cooking activities were enthusiastically received by most participants.
Process evaluation data also suggest moderate fidelity (69 %) and completeness of implementation scores across the six intervention sites. Meta-analysis of data from a variety of health promotion programmes suggests that few studies attain implementation levels above 80 %; and that implementation levels of about 60 % produce positive outcome results( Reference Durlak and DuPre 34 ).
There is evidence that contextual factors such as residents’ autonomy, staff involvement and the existing food environment may have contributed to the differences in the higher and lower participation and implementation sites. Contextual factors can pose threats to intervention implementations, and should be considered when interpreting process evaluation results( Reference Johnson, Lai and Rice 20 , Reference Saunders, Evans and Joshi 27 , Reference Linnan and Steckler 32 ).
Variation in programme participation across the intervention sites may have reflected different resident characteristics and level of autonomy. Sites with low participation had, on average, residents with longer residence in the treatment programmes than residents in the high participation sites. One explanation may be that longer time in the treatment facility afforded residents more autonomy and greater opportunities to participate in activities outside the facility, and less involvement within the residential facility. This assumption is consistent with treatment models and developmental stages in recovery( Reference Gorski 35 , Reference Gorski and Miller 36 ). With longer treatment time, people in recovery are usually encouraged to establish meaningful training, employment and social ties outside the treatment facility.
Demographic differences in different sites may also have contributed to programme outcomes. It is not completely clear why participants in the lower participation and implementation sites showed better programme outcomes in terms of percentage of energy from fat, although this difference may be related to more limited exposure to the intervention and demographic differences including being in the treatment programme longer. If residents spend more time away from the food environment, it is also reasonable to assume that the food environment, regardless of the implementation level, would have less impact on their dietary intake. Residents who are more involved in structured activities, e.g. work or training away from the treatment facility, may snack less throughout the day and thus consume a lower percentage of energy from fat than those who spend more time sitting and snacking in the treatment facility. Further research is necessary to understand how recovery stages, outside programme activities and intervention implementation level may affect dietary outcomes and body composition.
Interviews with residents and staff suggested that lower staff involvement and staff turnover in low participation and implementation sites may have also played a role in participation and fidelity rates in some sites. Because staff involvement and turnover is a fact of life in real-world settings, monitoring and communication with all key staff in intervention sites are necessary to address unexpected events as they arise.
Differences in food service staffing may also have played a role in findings. One of the low participation and implementation sites, site 6, had a paid cook instead of rotating resident cooks. This individual may have had less exposure to and investment in the intervention than the resident cooks in other sites.
Key differences were found in the implementation of different aspects of the food environment elements. Variability in intervention fidelity and completeness of implementation has been consistently reported in a variety of study settings( Reference Saunders, Ward and Felton 21 , Reference Baranowski and Stables 26 , Reference Durlak and DuPre 34 , Reference Dusenbury, Brannigan and Falco 37 – Reference Harachi, Abbott and Catalano 39 ). It is not practical to expect perfect or near-perfect implementation of interventions in real-world settings. For example, providing lower-fat milks and 100 % juices, and adding daily fruits and vegetables were implemented fairly well across the six sites. Vegetarian or meatless dishes were not implemented at any site. It may be easier to add healthy food options such as fruits and vegetables than to eliminate some higher-fat foods such as meats( Reference Hagler, Norman and Zabinski 40 ). Another potential explanation for the lack of implementation of the vegetarian option may be that meat and other energy-dense foods are viewed as masculine foods in many cultures( Reference Fagerli and Wandel 41 , Reference Roos, Prattaala and Koski 42 ). A future modification would be to offer leaner meats or reduced portions of meat on the menus instead of a meatless option.
Process evaluation can be an effective tool to explain the effects of intervention implementation on study outcomes( Reference Johnson, Lai and Rice 20 , Reference Steckler, Ethelbah and Martin 22 , Reference Helitzer, Yoon and Wallerstein 43 ). Higher levels of behavioural change have been related to greater exposure to the intervention( Reference Saunders, Ward and Felton 21 , Reference Davis, Baranowski and Resnicow 44 ), consistent with our study findings. Participants in the higher participation and food environment implementation sites reported better dietary outcomes than those in the lower-implementing sites.
The primary investigator conducted all of the intervention and evaluation activities including the collection of process evaluation data. The lack of separation of intervention and evaluation personnel may have introduced some bias. However, the investigator's exposure to the evaluation activities may have increased the homogeneity of intervention protocols, and thereby led to increased fidelity. The results of the present evaluation can only be generalized to men in similar facilities exposed to similar intervention protocols and to the use of a single instructor to administer the nutrition education component. The study limitations also include the non-random sample of men in the small number of residential treatment facilities. However, the sample size provided greater than 80 % power to detect differences between the high and low implementation groups for five of the eight study outcomes (change in total energy, percentage of energy from fat and from sweets, daily servings of fats, oils and sweets, and BMI); although the small sample size meant that we lacked the power to detect differences in three outcomes. A multi-site randomized study is needed to assess the effectiveness of the RHEALTH intervention in a scaled-up version with multiple instructors.
More convenient class schedules and repetition of weekly classes to maximize participation should be considered, as well as nutrition classes tailored to specific recovery stages or addiction histories( Reference Cowan and Devine 1 ). Interventions to improve dietary patterns of men in substance-abuse treatment must consider these factors to appropriately address nutritional needs associated with varied addiction and health histories( Reference Forrester 45 ).
Overall, there is evidence that an educational and environmental intervention can be successful in spite of the challenges of residential substance-abuse treatment facilities. This was demonstrated by the delivery of nutrition education and food environment intervention elements, the improvements in participants’ dietary intake and body composition( Reference Cowan 2 ). The process evaluation allowed for a comprehensive assessment of site-specific intervention experiences of participants and staff. A strength of this evaluation was the use of multiple data sources( Reference Saunders, Ward and Felton 21 , Reference Saunders, Evans and Joshi 27 , Reference Linnan and Steckler 32 ) and data triangulation in the analysis( Reference Saunders, Ward and Felton 21 , Reference Richardson 46 ).
The identification of a priori key intervention elements provided an effective structure for collecting and summarizing evaluation data from multiple sources. These essential elements also enabled researchers to assess the fidelity and completeness of intervention delivery efficiently. Observations and interviews provided data on contextual factors, including unrelated activities in the intervention sites, which facilitated interpretation of the evaluation results.
The present report illustrates the value of process evaluation in monitoring and assessing programme implementation and fidelity in real-world settings, particularly for environmental elements that depend on fit with site-specific characteristics. Variations in the food environment implementation highlight the need for close collaboration with treatment staff to tailor the intervention to the setting, and to increase staff ownership and support. The need for firm commitment to the intervention protocols as well as ongoing supervision and consultation is warranted for successful programme implementation in residential drug-treatment facilities. The present process evaluation illuminates conditions needed for educational and environmental interventions to improve dietary intake and body composition of men in recovery. The study results also have policy implications for food service guidelines in residential treatment facilities to improve resident nutrition and long-term health.
Acknowledgements
This research was supported by a grant from the Division of Nutritional Sciences at Cornell University and the National Institute of Health Training Grant. The authors declare that they have no competing interests. Both authors have contributed substantially to the paper, and both approve the version being submitted. The authors would like to acknowledge the helpful comments of Professors Barbara Strupp, John Cawley and Mark Constas, and the contributions of the residents and staff in the six treatment facilities for their generous support and accommodation.







