Breast milk is the ideal source of infant nutrition mostly because of its nutritional, immunological and psychological benefits( 1 ). Breast milk contains thousands of components( Reference Xi 2 ) that are necessary for infant development. In particular, it can help build the infant’s immune system and prevent diseases and infections, as well as having long-term consequences for metabolism and diseases later in life( Reference Oddy 3 ).
Formula milk as a product of advanced technology has been formulated to imitate breast milk, but the former does not have the same effects on babies as the latter. Different feeding patterns, such as exclusive breast-feeding (EBF), mixed feeding with breast milk and infant formula (MBF) and exclusive formula-feeding (EFF), have different effects on infants. Previous studies have suggested that breast-feeding, including EBF, predominant breast-feeding for at least 6 months and partial breast-feeding for up to 1 year, may reduce the risk of diarrhoea, respiratory illness and other common diseases in infants( Reference Lopez-Alarcon, Villalpando and Fajardo 4 – Reference Dey, Chisti and Das 9 ). However, for allergic diseases, such as wheezing/asthma, eczema, allergic rhinitis and atopic dermatitis, whether breast-feeding is protective or a risk remains controversial( Reference van Odijk, Kull and Borres 10 – Reference Soto-Ramirez, Karmaus and Yousefi 13 ).
In China, previous studies have investigated the association of feeding pattern and different infant illnesses. However, most of these studies focused on clinical cases only and recruited subjects from a single hospital( Reference Gu and Shen 8 , Reference Ye 14 , Reference Jihong, Xiaolan and Shiyuan 15 ). In the present study, the participants were selected from the general infant population aged 0–11·9 months in eight cities, regardless of whether they had ever had a disease or been hospitalized for treatment. We aimed to investigate the effect of different feeding patterns on the occurrence of diseases in Chinese infants.
Methods
Participants
Infants aged 0–11·9 months were included in the present study, which is part of the Maternal Infant Nutrition and Growth (MING) study. The MING study is a cross-sectional study that was conducted between October 2011 and March 2012. A multiple stratified sampling design was applied. In the first stage, eight Chinese cities, namely Beijing, Shanghai, Guangzhou, Chengdu, Shenyang, Suzhou, Zhengzhou and Lanzhou, were selected via a purpose sampling method. In the second stage, two maternal and child health hospitals in each city were randomly selected. In the third stage, infants were recruited from out-patient clinics (Department of Child Care) when they returned to the hospitals for routine follow-up visits and they were not hospitalized. These infants were stratified by age group (0–2·9, 3–5·9 and 6–11·9 months) and feeding pattern (for those infants aged 6 months and below) when they came for the follow-up visit, and we recruited every fifth infant in each group. A total of 1654 infants were included, with details as follows: 671 aged 0–2·9 months (255 for EBF, 237 for MBF and 179 for EFF), 501 aged 3–5·9 months (185 for EBF, 171 for MBF and 145 for EFF) and 482 aged 6–11·9 months.
Data collection
In each selected hospital, several trained medical researchers administered structured questionnaires to obtain participant information during face-to-face interviews at the Department of Child Care. The collected information included the following: (i) general information including the infant’s age, sex, ethnicity, birth weight and length, delivery mode, parents’ education level and per capita family income; (ii) physical information; and (iii) dietary information. Parents’ education level was assessed using a categorical scale of ‘middle school or lower’, ‘high school’, ‘junior college’ and ‘college and above’. Per capita family income was also assessed using the categorical scale of ‘≤1500 RMB’, ‘1501–2000 RMB’, ‘2001–3000 RMB’, ‘3001–4000 RMB’, ‘4001–6000 RMB’ and ‘>6000 RMB’.
Information on infant illness was determined by the following questions. Caregivers were asked, ‘Has your baby ever been ill since s/he was born?’ Those answered ‘yes’ were asked, ‘The disease s/he had was (i) diarrhoea; (ii) respiratory disease (cold, bronchitis, pneumonia, etc.); (iii) allergic disease (eczema, atopic dermatitis, rhinitis, asthma, etc.); and (iv) others’. Caregivers were allowed to select as many as were applicable. Information on infant hospitalization was determined by the following questions. Caregivers were asked, ‘Has your baby ever been hospitalized for treatment of disease since s/he was born?’ Those answered ‘yes’ were asked, ‘The cause for hospitalization was (i) diarrhoea; (ii) respiratory disease (cold, bronchitis, pneumonia, etc.); (iii) allergic disease (eczema, atopic dermatitis, rhinitis, asthma, etc.); and (iv) others’. Caregivers were also allowed to select all applicable cases.
Definitions
In the present study, EBF refers to an infant being fed breast milk as the only source of milk and not infant formula or animal milk, with or without water, vitamin supplements, prescribed medicines and solids.
For infants aged 6 months and below, they were considered EBF if they had been exclusively breast-fed since they were born, MBF if they had been fed with both breast milk and infant formulas since they were born, or EFF if they had been fed exclusively with infant formulas since they were born.
For infants aged 6–11·9 months, they were considered EBF if they had been exclusively breast-fed before 6 months of age, MBF if they had been fed with both breast milk and infant formulas before 6 months of age, or EFF if they had been fed exclusively with infant formulas before 6 months of age.
The infants’ birth weights were classified into three categories: low birth weight (<2·5 kg), adequate birth weight (2·5–3·9 kg) and macrosomia (≥4·0 kg).
Statistical analyses
The proportions of infants’ illness and hospitalization (including total illness, diarrhoea, respiratory disease and allergic disease) were calculated by feeding pattern and age group. The differences in proportions among different feeding patterns (EBF, MBF and EFF) were determined using both the trend χ 2 test and χ 2 test. For the proportions of infants’ illness, subgroup analyses by infants’ sex, birth weight, delivery mode, their mothers’ education and per capita monthly income were also performed.
Multiple logistic regression models were used to investigate the potential influence factors for infants’ illness. Dependent variables included total illness, diarrhoea, respiratory disease, allergic disease and (total) hospitalization. Independent variables included in the models were infants’ feeding pattern, age group, sex, birth weight, delivery mode, their mothers’ education and per capita monthly income.
The statistical software package SAS version 9·2 was used for statistical analyses. Two-tailed P<0·05 was considered statistically significant.
Results
A total of 1654 infants were included, 671, 501 and 482 aged 0–2·9 months, 3–5·9 months and 6–11·9 months, respectively. The proportions of illness among infants aged 0–2·9 months are shown in Table 1. For total illness, the proportion was 19·2 % among EBF infants, 24·1 % among MBF infants and 26·3 % among EFF infants. The proportion of diarrhoea ranged from 4·2 % to 5·1 %, which was lower than those of respiratory (8·2 % to 13·4 %) and allergic diseases (5·1 % to 9·5 %). The results from the subgroup analyses showed that the proportions of total illness, respiratory disease and allergic disease among EBF infants were lower than those among MBF and EFF infants (P<0·05). Significant difference was not found between MBF and EFF after adjusting for sex, birth weight, delivery mode, mother’s education and monthly income.
Table 1 Feeding mode and proportion of illness in infants aged 0–2·9 months from eight large cities in China, Maternal Infant Nutrition and Growth (MING) study, October 2011–March 2012

EBF, exclusive breast-feeding; MBF, mixed feeding with breast milk and infant formula; EFF, exclusive formula-feeding.
Total illness included diarrhoea, respiratory disease, allergic disease and other illness. n varied slightly due to missing data on some variables.
* P value from χ 2 test for trend <0·05 (EBF, MBF, EFF).
† P value from χ 2 test <0·05 (EBF, MBF, EFF).
As shown in Table 2, 41·6 % of EBF infants, 45·6 % of MBF infants and 51·0 % of EFF infants aged 3–5·9 months had been ill. The proportion of diarrhoea ranged from 11·4 % to 18·7 %, which was lower than that of respiratory disease (29·7 % to 37·2 %) but higher than that of allergic disease (6·9 % to 9·4 %).
Table 2 Feeding mode and proportion of illness in infants aged 3–5·9 months from eight large cities in China, Maternal Infant Nutrition and Growth (MING) study, October 2011–March 2012
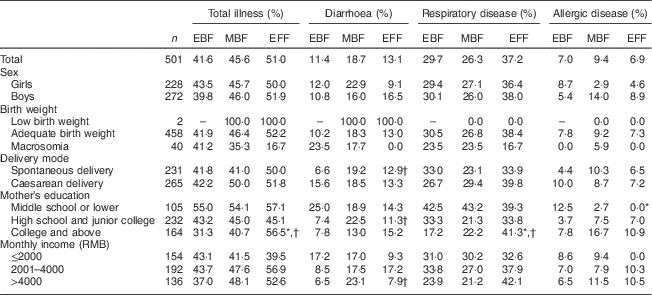
EBF, exclusive breast-feeding; MBF, mixed feeding with breast milk and infant formula; EFF, exclusive formula-feeding; –, no data exist for this section.
Total illness included diarrhoea, respiratory disease, allergic disease and other illness. n varied slightly due to missing data on some variables.
* P value from χ 2 test for trend <0·05 (EBF, MBF, EFF).
† P value from χ 2 test <0·05 (EBF, MBF, EFF).
Table 3 shows that 67·0 % of EBF infants, 73·4 % of MBF infants and 67·7 % of EFF infants aged 6–11·9 months had been ill. The proportion of diarrhoea ranged from 24·8 % to 30·4 %, which was lower than that of respiratory disease (48·1 % to 52·8 %) but higher than that of allergic disease (6·5 % to 9·7 %).
Table 3 Feeding mode and proportion of illness in infants aged 6–11·9 months from eight large cities in China, Maternal Infant Nutrition and Growth (MING) study, October 2011–March 2012
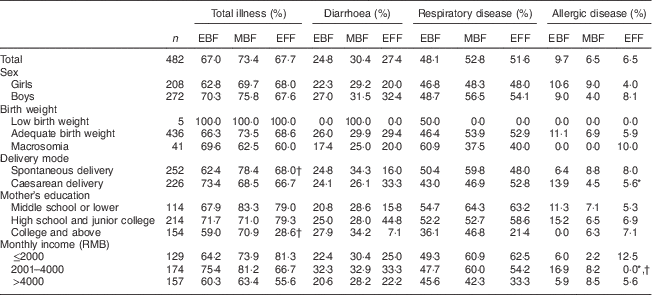
EBF, exclusive breast-feeding; MBF, mixed feeding with breast milk and infant formula; EFF, exclusive formula-feeding.
Total illness included diarrhoea, respiratory disease, allergic disease and other illness. n varied slightly due to missing data on some variables.
* P value from χ 2 test for trend <0·05 (EBF, MBF, EFF).
† P value from χ 2 test <0·05 (EBF, MBF, EFF).
The proportions of hospitalization among infants aged 0–11·9 months are shown in Table 4. A total of 3·9 % to 8·4 % of infants aged 0–2·9 months had been hospitalized one or more times. The corresponding proportions were 6·4 % to 8·1 % among those aged 3–5·9 months and 8·4 % to 12·1 % among those aged 6–11·9 months. The most frequent reported cause for hospitalization was respiratory disease.
Table 4 Feeding mode and hospitalization by age in infants aged 0–11·9 months from eight large cities in China, Maternal Infant Nutrition and Growth (MING) study, October 2011–March 2012
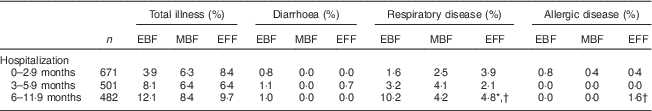
EBF, exclusive breast-feeding; MBF, mixed feeding with breast milk and infant formula; EFF, exclusive formula-feeding.
Total illness included diarrhoea, respiratory disease, allergic disease and other illness.
* P value from χ 2 test for trend <0·05 (EBF, MBF, EFF).
† P value from χ 2 test <0·05 (EBF, MBF, EFF).
As shown in Table 5, compared with EBF infants, MBF infants had significantly higher odds of having (total) illness and EFF infants had higher odds of having (total) illness and respiratory disease. The odds of having (total) illness, diarrhoea and respiratory disease increased significantly with age. However, such trend was not found in allergic disease. A low birth weight increased the odds of having (total) illness. A high mother’s education level decreased the odds of having (total) illness and respiratory disease. A moderate monthly family income (2001–4000 RMB per capita) was related to high odds of having (total) illness and allergic disease.
Table 5 Odds ratios for the proportion of illness in infants aged 0–11·9 months from eight large cities in China, Maternal Infant Nutrition and Growth (MING) study, October 2011–March 2012
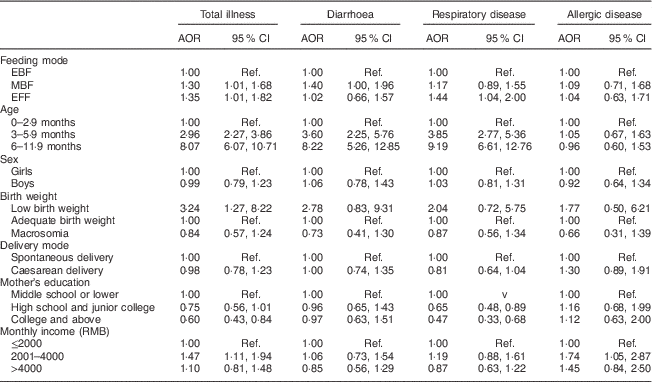
AOR, adjusted odds ratio; EBF, exclusive breast-feeding; MBF, mixed feeding with breast milk and infant formula; EFF, exclusive formula-feeding; Ref., reference category.
Total illness included diarrhoea, respiratory disease, allergic disease and other illness.
The result from the multiple logistic regression model showed that feeding pattern was not related to hospitalization (Table 6). Infants aged 6–11·9 months had higher odds (OR=1·83; 95 % CI 1·13, 2·98, P=0·014) of hospitalization compared with those aged 0–2·9 months. A low birth weight increased the odds of hospitalization (OR=9·28; 95 % CI 3·50, 24·62, P<0·001).
Table 6 Odds ratios for total hospitalization in infants aged 0–11·9 months from eight large cities in China, Maternal Infant Nutrition and Growth (MING) study, October 2011–March 2012
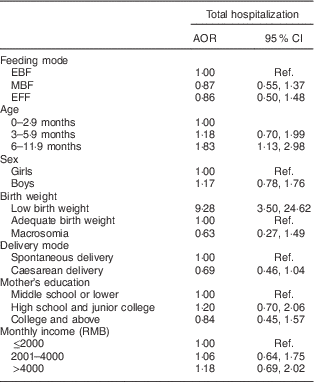
AOR, adjusted odds ratio; EBF, exclusive breast-feeding; MBF, mixed feeding with breast milk and infant formula; EFF, exclusive formula-feeding; Ref., reference category.
Discussion
Two major findings were obtained in the current study. First, EBF infants had lower odds of having total illness compared with MBF and EFF infants. No statistical association was found between feeding pattern and allergic disease. Second, the proportions of infants having been ill or having had diarrhoea or respiratory disease increased with age in infants, whereas this increase was not observed for allergic disease.
Breast milk provides infants with thousands of components that help build the immune system and protect them from infection( Reference Gribble 16 ). Moreover, breast milk, with its optimal amount of nutrients, helps maintain the good nutritional status of infants. The number of EBF infants who had been ill was lower compared with MBF and EFF infants, and this result is consistent with those of previous studies( Reference Cushing, Samet and Lambert 5 – Reference Dey, Chisti and Das 9 , Reference Pardo-Crespo, Perez-Iglesias and Llorca 17 – Reference Mihrshahi, Oddy and Peat 20 ). One study reported that full breast-feeding is associated with the lowest illness (diarrhoea, cough, wheeze and vomiting) rates and minimal (less) breast-feeding is not protective( Reference Raisler, Alexander and O’Campo 21 ). Furthermore, a previous multicentre cohort study reported that non-breast-fed infants have a higher risk of dying compared with predominantly breast-fed (adjusted hazard ratio=10·5) and partially breast-fed infants (adjusted hazard ratio=2·46)( Reference Bahl, Frost and Kirkwood 18 ).
Diarrhoeal disease accounted for 11 % of the estimated 7·6 million deaths among under-5s globally in 2010( Reference Lopez-Alarcon, Villalpando and Fajardo 4 ). In the present study, EBF had a borderline significant protective effect against diarrhoea compared with MBF (P=0·05). Many studies have suggested that breast-feeding, especially EBF, may protect infants against diarrhoeal disease. Dewey et al.( Reference Dewey, Heinig and Nommsen-Rivers 22 ) reported that the incidence of diarrhoea among breast-fed infants is half that among formula-fed infants in the first year of life. Similar results were found by other studies( Reference Gu and Shen 8 , Reference Brown, Black and Lopez 23 – Reference Arifeen, Black and Antelman 25 ). The mechanism behind the protective effect of breast milk is that antibodies and living cells in breast milk can prevent infection or attack/kill pathogens that are harmful. Glycans can be recognized by pathogens and become sites of attachment. As a result, the pathogens become harmless and passed out in the faeces. Oligosaccharides and lactose facilitate the growth of beneficial bacteria, such as bifidobacteria and lactobacilli( Reference Gribble 16 ).
Breast-feeding may protect infants against infection with rotavirus( Reference Gu and Shen 8 , Reference Dey, Chisti and Das 9 , Reference Shen, Li and Zhang 26 ). However, it may lead to diarrhoea if the breast milk contains rotavirus( Reference Ye 14 ). A previous study reported that almost half of the acute diarrhoea hospitalization cases among children are caused by rotavirus( Reference Nakawesi, Wobudeya and Ndeezi 27 ). Thus, healthy breast milk is the key factor in protecting infants’ health.
Respiratory disease is another leading disease among infants. In the current study, respiratory disease was the most common reported illness. EBF also exhibited a protective effect against this disease. Our results are consistent with those of other findings( Reference Cushing, Samet and Lambert 5 , Reference Oddy, Sly and de Klerk 7 , Reference Pardo-Crespo, Perez-Iglesias and Llorca 17 , Reference Arifeen, Black and Antelman 25 ). Soto-Ramirez et al.( Reference Soto-Ramirez, Karmaus and Zhang 28 ) found that compared with direct breast milk, any feeding pattern that includes formula or bottled breast milk seems to be a moderate risk for cough or wheezing episodes in the first 12 months of life. The protective effect of breast milk is biologically plausible. On one hand, breast milk has a direct action against pathogenic agents and an indirect action that is mediated by its capacity to affect the infant’s physiology by modulating mucosal immune responses( Reference Lanari, Prinelli and Adorni 29 ). On the other hand, formulas lack lipids and immune-active components that may help fight foreign pathogens (e.g. viruses, bacteria) and in turn help protect against the development of respiratory diseases, such as viral upper respiratory infections.
The development of allergic disease depends on numerous variables and reflects the interaction between genetic factors and environmental exposure. However, whether or not breast milk prevents or reduces the incidence of allergic diseases remains unclear. Particular elements in breast milk are thought to function as protective agents in infants to prevent the development of allergies, whereas others may function in a different way( Reference Friedman and Zeiger 30 ). In the present study, a significant relationship was not observed between allergic diseases and feeding pattern and the proportion of patients who developed allergic diseases did not increase with age. Previous studies suggested that prolonged breast-feeding and EBF reduce the risk of eczema and allergic diseases in children( Reference van Odijk, Kull and Borres 10 , Reference Ehlayel and Bener 12 , Reference Kull, Wickman and Lilja 31 – Reference Huang, Zhang and Hang 33 ). However, other studies failed to confirm this finding or even found that breast-feeding is associated with an increased risk for childhood asthma in the presence of maternal asthma( Reference Kramer 11 , Reference Soto-Ramirez, Karmaus and Yousefi 13 , Reference Mandhane, Greene and Sears 34 – Reference Zhang, Wang and Chen 36 ). For example, Kramer and Kakuma( Reference Kramer and Kakuma 37 ), in their meta-analysis on optimal duration of EBF, reported that EBF for 6 months has no long-term impact on allergic disease development v. those fed for 3–4 months with continued mixed breast-feeding thereafter. In addition, a study showed that the levels of soluble CD14, total IgA and transforming growth factor-β1 (TGF-β1) in breast milk at either day 7 or day 28 are not associated with subsequent development of eczema or atopic sensitization during the first year of life( Reference Ismail, Licciardi and Oppedisano 38 ). Similarly, but not totally, another study reported that maternal serum and whey levels of IL-5 and IL-13 are risk markers for asthma-like symptoms, whereas whey IgA and TGF-β1 seem to have a protective effect during infancy( Reference Soto-Ramirez, Karmaus and Yousefi 13 ). The composition of human milk can be affected by the diet of lactating women( Reference Emmett and Rogers 39 – Reference Lonnerdal 41 ). Thus, speculating that the exclusion of peanuts, egg, fish and other potentially ‘antigenic’ foods in the maternal diet while breast-feeding may reduce the risk of allergy in infants is reasonable. Several studies found a protective effect on the development of atopic dermatitis in infants when mothers avoided these foods( Reference Lovegrove, Hampton and Morgan 42 , Reference Ip, Chung and Raman 43 ). However, recent studies have concluded that evidence is inadequate to advise women to avoid specific food items during pregnancy or breast-feeding to protect their children from allergic diseases, such as eczema and asthma( Reference Kramer and Kakuma 44 ).
These controversial results on the protective effect of breast-feeding on infant allergy from different studies may be attributed to diverse methods, subjects and definitions of EBF, as well as to the fact that allergic disease is related to heredity, family history and other inducing factors, as previously reported. Previous studies reported that breast-feeding increases the risk for atopy among boys with paternal atopy (OR=7·39; 95 % CI, 2·21, 24·66) compared with non-breast-fed boys with paternal atopy, and the result was similar among girls (OR=3·13; 95 % CI, 1·20, 8·14)( Reference Mandhane, Greene and Sears 34 ). Conversely, other studies found that the children who benefited the most from breast-feeding are those with a parental history of atopic disease independent of maternal asthma( Reference van Odijk, Kull and Borres 10 , Reference Kull, Wickman and Lilja 31 ). Thus, whether breast milk has a protective function or is a risk factor may be related to the heredity of infants. However, further studies are recommended.
In the present study, mother’s education was associated with the proportions of total illness and respiratory disease during infancy. A high level of mother’s education indicated a low proportion of total illness and respiratory disease. This result is consistent with those of another Chinese study( Reference Jie, Tao and Yimin 45 ). Usually, mothers are the main caregivers in China. Educated mothers have more knowledge of baby care and they have more access to acquire new and scientific parenting skills than those with less education. In addition, mothers with a high level of education usually have greater financial capacity, thereby allowing them to fully reap the benefits of education, provide their children with more hygienic living environments and obtain greater access to health care( Reference Kramer 11 ). Furthermore, previous studies reported that the level of mother’s education is related with non-healthy behaviours, such as no hair washing, no showering, no teeth cleaning and no indoor air ventilation during the first days after childbirth or even the entire period of puerperium, and maternity blues. Those with a low level of education have a higher incidence of practising non-healthy behaviours and maternity blues( Reference Wu, Mei and Xu 46 , Reference Xue, Zhang and Li 47 ), which may result in an unfavourable effect on infants’ health care.
In the current study, among all the diseases except allergic disease, EBF had a protective effect compared with MBF and EFF. Breast milk is superior to formulas not only in nutrients, immune components and psychological benefits, but also in safety, convenience and feasibility. Infants can make full use of breast milk with their special digestive system in EBF. Thus, EBF should be encouraged for at least 4 to 6 months in infants. However, the extent of the favourable effect of MBF on infants’ health remains unknown. More studies are needed to investigate this issue.
The limitations of our study should be noted. First, for infants aged 6 months and below, they were classified as EBF, MBF or EFF based on how they were fed since they were born because we were unable to obtain information until they were 6 months old. Second, we focused on the proportion of the infants who had a specific disease and had been hospitalized for treatment since they were born but could not obtain information on the prevalence. Third, recall bias may exist. Caregivers may forget to report slight illnesses, such as cough and sneeze, or they may be not able to distinguish between respiratory infectious morbidity and allergic disease, if not diagnosed by a doctor. However, most parents/guardians are sensitive to infants’ health, thereby helping in minimizing recall bias. Fourth, no causal relationships are precisely delineated from a cross-sectional study.
Conclusion
In conclusion, EBF had a protective effect against total illness in Chinese infants. Although we did not find the same result for allergic diseases, breast-feeding, especially EBF, is recommended for babies. Healthy breast milk is the best food to be given to infants worldwide because of its nutritive contents, protective qualities against common diseases, immunological protection against long-term chronic diseases and the psychological benefits.
Acknowledgements
Financial support: This research project was part of the larger MING study, sponsored by Nestlé Nutrition Institute of China and Nestlé Research Center. This research project was a collaborative work between Peking University and Nestlé. The views and opinions expressed in this manuscript are those of the authors and do not necessarily reflect the opinions and recommendations of Nestlé. Conflict of interest: None declared. Authorship: X.Y., W.L. and P.W. contributed to the conception and design of the study. Y.Z. contributed to the conception and design of the study and critical revisions of the manuscript. L.C. contributed to the analysis and interpretation of data and drafted the manuscript. P.Y. contributed to interpretation of data and drafted the manuscript. Ethics of human subject participation: This study was conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving human subjects were approved by the Medical Ethics Research Board of Peking University (approval number IRB00001052-11042). Written informed consent was acquired from all infants’ legal guardian.









