The health burden of non-communicable diseases in Malaysia has reached alarming levels. Non-communicable diseases contribute to approximately 73% of the total deaths of Malaysian individuals within the reproductive age group(1). The National Health and Morbidity Survey in 2015 reported an increasing trend for all non-communicable disease risk factors in the country, especially among adults above the age of 18 years(1). At least 63% of all adults were obese, had high blood pressure, high blood sugar level or high cholesterol level(1).
The concept of food addiction is linked to obesity, overeating and binge eating habits(Reference Corsica and Pelchat2). The idea of ‘food addiction’ was conceptualized to describe substance dependence related to the consumption of foods high in sugar, fat and salt(Reference Corsica and Pelchat2–Reference Gearhardt, Grilo and DiLeone6). Consequently, the Yale Food Addiction Scale (YFAS) was devised to quantify the predisposition to ‘food addiction’ (based on the criteria of the Diagnostic and Statistical Manual of Mental Disorders, 4th edition (DSM-IV-R))(Reference Gearhardt, Corbin and Brownell7). The YFAS demonstrated excellent psychometric properties(Reference Gearhardt, Corbin and Brownell7). The scale was successfully validated into German, French, Italian, Spanish, Turkish, Malay and Chinese languages(Reference Brunault, Ballon and Gaillard8–Reference Sevincer, Konuk and Bozkurt14).
The publication of an updated YFAS 2.0 in 2016 and the validated Malay Binge Eating Scale (BES) in 2013 paved the way for a complete evaluation of the use of the YFAS in Malaysia(Reference Schulte and Gearhardt15,Reference Robert, Rohana and Suehazlyn16) . The newer YFAS 2.0 incorporated four criteria for the diagnosis of addiction in accordance with the Diagnostic and Statistical Manual of Mental Disorders, 5th edition (DSM-V): (i) ‘craving’; (ii) ‘use despite interpersonalor social consequences’; (iii) ‘failure in role obligations’; and (iv) ‘use in physically hazardous situations’.
The YFAS has not been extensively evaluated in Malaysia. A current review suggests the exploration of the addictive effects of ‘hyperpalatable food’ as a way to explain the rise of obesity in the country(Reference Swarna Nantha17). In line with this recommendation, an initiative was undertaken to screen obese patients using a validated Malay YFAS 1.0(Reference Swarna Nantha, Abd Patah and Ponnusamy Pillai11). However, the inventory was not utilized to screen obese individuals for food addiction tendencies due to the inadequate assessment of construct validity and goodness-of-fit(Reference Swarna Nantha, Abd Patah and Ponnusamy Pillai11).
The primary objective of the present study is to evaluate the psychometric properties of a Malay version of the YFAS 2.0 in an undifferentiated population at a regional primary-care clinic. We aimed to confirm the factor structure and determine the internal consistency and overall validity of the questionnaire.
Materials and methods
Study design and study population
The random sampling of patients attending the Seremban Primary Care Clinic was implemented using a cross-sectional study design between November 2017 and June 2018. A nominal list was generated to allow the random selection of patients based on the daily clinical appointments. Patients who were ineligible or refused to participate in the study were randomly replaced with other available participants on the nominal list. The inclusion criteria for patient recruitment were: (i) individuals between the age of 18 and 65 years; and (ii) fluency in the Malay language. Participants were excluded if they were suffering from a combination of psychological and neurological illnesses identified via individual case record examinations.
The permission to translate and validate the original version of the YFAS 2.0 questionnaire in the Malay language was obtained from Dr Ashley Gearhardt.
Instruments (Yale Food Addiction Scale and Binge Eating Scale)
The YFAS is a psychological inventory measuring food addiction symptoms experienced by individuals over a 12-month time period(Reference Gearhardt, Corbin and Brownell7). The questionnaire comprises thirty-five items that represent the twelve food addiction criteria in tandem with DSM-V (for more detailed description, see Table 1)(18,Reference Gearhardt, Corbin and Brownell19) .
Table 1 Criteria of the Diagnostic and Statistical Manual of Mental Disorders, 5th edition (DSM-V), items retained and omitted within solved factors of the Malay Yale Food Addiction Scale 2.0
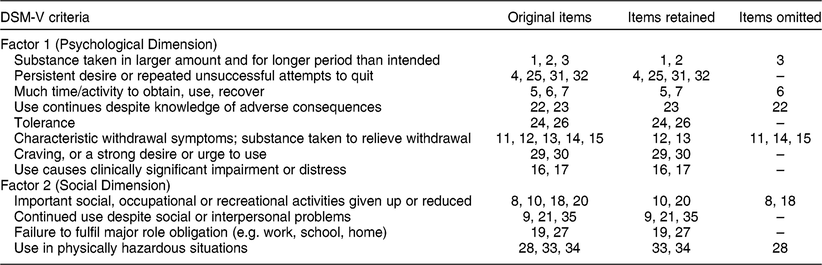
The scores for symptom count and the diagnosis of food addiction were calculated based on the responses to all thirty-five items in the questionnaire. The classification of the twelve DSM-V diagnostic criteria was determined from cut-offs that were consistent with the original YFAS study (a diagnostic score of 1 translates into the endorsement of any criterion)(Reference Gearhardt, Corbin and Brownell19). The scores for the symptom count version range from 0 to 7. On the other hand, the diagnosis of food addiction was defined by: (i) two or more symptoms in the previous 12 months; plus (ii) concurrent evidence of clinically significant impairment or distress.
The BES comprises a sixteen-item questionnaire that identifies binge eating behaviour in participants with a score of ≥18. The scale has been validated in the Malay language and the Cronbach’s α in our study was 0·81(Reference Robert, Rohana and Suehazlyn16).
Translation of the Yale Food Addiction Scale 2.0
The translation process of the YFAS 2.0 questionnaire into the Malay language was done by a team of medical professionals and linguistic experts. The translation procedure was conducted in two phases. The initial phase was carried out by a general practitioner and a professional linguist from a recognized language translation institute. Subsequently, the back-translation of the validated questionnaire into English was conducted by two general practitioners and a language expert.
Pilot testing
Initially, thirty participants were recruited by closely adhering to the inclusion criteria of the study. Feedback was obtained with consideration to the difficulties faced while answering the items in the questionnaire. This information was then utilized to improve the accuracy of the questions, so they represent the concepts measured in the study correctly. The amended version of the questionnaire was tested on an additional fifty participants, giving an excellent preliminary Kuder–Richardson’s α (KR-20) reliability for both the symptom count and diagnostic version of the questionnaire (α = 0·97 and 0·92, respectively).
Consequently, the decision to approve the final version of the questionnaire was based on a consensus obtained from a panel of experts comprising a family medicine consultant, two general practitioners, a dietitian and senior primary-care nurse. Consensus was achieved via the iterative process of: (i) scrutinizing feedback solicited from participants during the pilot phase of the study; (ii) improving contextual accuracy of each question by examining the information obtained during the forward- and back-translation of the questionnaire; and (iii) repeated analysis of the responses and comments from participants who answered the revised version of the questionnaire.
Formal Malay Yale Food Addiction Scale 2.0 validation study
The formal validation process was then conducted using the revised version of the translated questionnaire. Once informed consent was obtained, participants were requested to complete the translated Malay YFAS 2.0 questionnaire containing three sections: demographics, the translated YFAS 2.0 questionnaire and the Malay BES inventory. Following completion of the questionnaire, the height and weight of the patients were measured to facilitate the calculation of individual BMI values.
Ethical considerations
Ethical approval to conduct the study was granted by the Medical Research Ethics Committee, Ministry of Health Malaysia (NMRR ID: NMRR-14-1426-22829).
Data and statistical analysis
Data from the study were evaluated using two statistical software packages: IBM SPSS Statistics version 20 and Stata version 15.0, IC Edition 64-bit. The data set was examined to account for missing or invalid values. Subsequently, outliers were removed from the final data set.
The following psychometric properties of the scale were analysed: (i) factor structure; (ii) item statistics; and (iii) internal consistency. The consensus on the adequacy of the sample size required for factor analysis remains mixed(Reference Tabachnick and Fidell20,Reference DeVellis21) . In line with pre-existing statistical ratios, a benchmark of 200 participants was considered sufficient as the questionnaire did not involve more than forty items(Reference Tabachnick and Fidell20,Reference DeVellis21) .
The tetrachoric correlation coefficients of the dichotomous data were reconstituted into a correlation matrix. Subsequently, this matrix was used in the exploratory factor analysis of the responses obtained from the survey(Reference Brunault, Ballon and Gaillard8,Reference Meule, Heckel and Kübler9,Reference Kubinger22,Reference Pursey, Stanwell and Gearhardt23) . Inter-item correlation, the Kaiser–Meyer–Olkin statistic (>0·80) and Bartlett’s test of sphericity (P < 0·05) were used to assess sampling adequacy(Reference Tabachnick and Fidell20). The number of factors to be retained was verified by assessing scree plots and eigenvalues(Reference DeVellis21). Internal consistency of the Malay YFAS 2.0 was calculated using McDonald’s ω and the KR-20 test(Reference Kuder and Richardson24). The factor structure of the Malay YFAS 2.0 in the diagnostic version of the scale was confirmed by conducting factor analysis on the twelve dichotomous diagnostic criteria. Finally, structural equation modelling was performed to estimate the goodness-of-fit of the Malay version of the YFAS 2.0 as a theoretical model. The model fit was assessed based on path analysis using the Satorra–Bentler scaled χ 2 test for all categorical variables. The following cut-offs were used as indicators of excellent validity and reliability of the psychometric model: KR-20 internal reliability coefficient > 0·7, McDonald’s ω > 0·9, comparative fit index > 0·90, Tucker–Lewis index > 0·90 and root-mean-square error of approximation < 0·08(Reference Hu, Bentler and Hu25,Reference Nunnaly26) .
Convergent validity was established by determining Pearson’s correlation coefficient r between items in the questionnaire. Discriminant analysis was performed using one-way ANOVA to determine the variance between categorical and continuous variables.
Results
Participant characteristics
Out of the 382 invited participants, twenty-four patients were excluded from the final analysis. This step was taken to preserve statistical accuracy by excluding missing values as a consequence of incomplete questionnaires (due to the failure to answer any of the thirty-five items on the Malay YFAS 2.0 questionnaire). Thus, approximately 358 participants were retained in the eventual process of factor analysis.
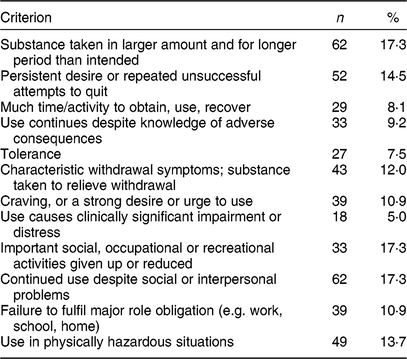
Analysis of participant characteristics from the pilot study revealed a mean age and mean BMI of 36·67 (sd 26·75) years and 30·54 (sd 2·25) kg/m2, respectively. The mean age derived from the final study population (Table 2) was 32·37 (sd 12·76) years. These participants had a mean BMI of 25·77 (sd 6·00) kg/m2. The mean for the Malay YFAS 2.0 symptom count was 1·4 (sd 2·3). The prevalence of food addiction within this sample was 5·0%, with approximately eighteen participants fulfilling the criteria required for the diagnosis. Table 3 summarizes the endorsement rates of the twelve criteria that constitute food addiction symptoms.
Table 2 Characteristics of participants: random sample of patients (n 358) from a regional primary-care clinic in the district of Seremban, Malaysia, November 2017–June 2018
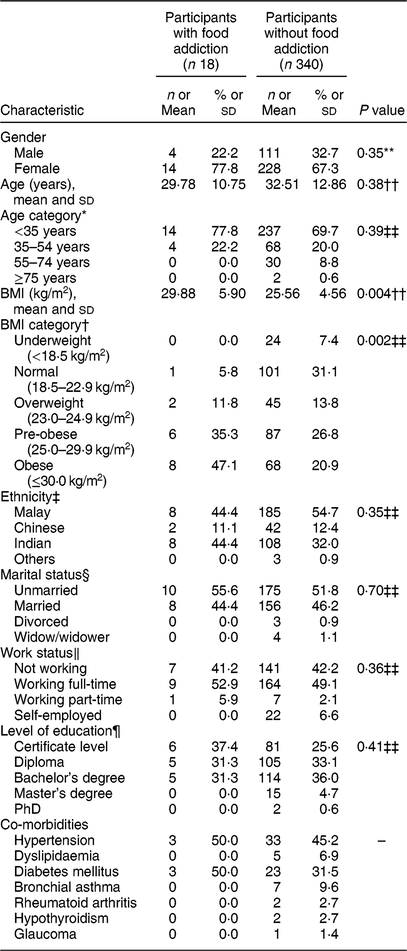
Data presented are n and% unless indicated otherwise.
* Missing, n 3.
† Missing, n 15.
‡ Missing, n 2.
§ Missing, n 2.
‖ Missing, n 7.
¶ Missing, n 25.
** χ 2 test.
†† Independent t test.
‡‡ Mann–Whitney U test.
Table 3 Endorsement rates for food addiction symptoms among the participants (n 358) from a regional primary-care clinic in the district of Seremban, Malaysia, November 2017–June 2018
Factor structure, internal consistency and model fit
The symptom count component of the translated Malay YFAS 2.0 scale was first evaluated using exploratory factor analysis, followed by structural equation modelling. A two-factor model had acceptable fit indices (
![]() $\chi _{(281)}^2 = 402 \cdot 66$
, P < 0·001; comparative fit index = 0·89, Tucker–Lewis index = 0·88, root-mean-square error of approximation =0·035) with all factor loadings greater than 0·5 (Table 4). We retained a two-factor solution because the one-factor model did not result in noticeably improved fit (comparative fit index = 0·70, Tucker–Lewis index = 0·66, root-mean-square error of approximation = 0·053). Additionally, a scree plot examination showed an elbow break at the second factor. Hence, the two-factor structure was retained as it fulfilled the criteria of factor selection as described by Cattell(Reference Nunnaly26). Furthermore, the one-factor solution revealed cumulative variance of only 38·9%. The cumulative variance increased to 53·9% when a two-factor solution was chosen. The two extracted factors in the symptom count version gave a McDonald’s ω > 0·90 (ω
factor 1 = 0·92 and ω
factor 2 = 0·93) and a KR-20 internal reliability coefficient α > 0·86 (α
factor 1 = 0·86 and α
factor 2 = 0·88).
$\chi _{(281)}^2 = 402 \cdot 66$
, P < 0·001; comparative fit index = 0·89, Tucker–Lewis index = 0·88, root-mean-square error of approximation =0·035) with all factor loadings greater than 0·5 (Table 4). We retained a two-factor solution because the one-factor model did not result in noticeably improved fit (comparative fit index = 0·70, Tucker–Lewis index = 0·66, root-mean-square error of approximation = 0·053). Additionally, a scree plot examination showed an elbow break at the second factor. Hence, the two-factor structure was retained as it fulfilled the criteria of factor selection as described by Cattell(Reference Nunnaly26). Furthermore, the one-factor solution revealed cumulative variance of only 38·9%. The cumulative variance increased to 53·9% when a two-factor solution was chosen. The two extracted factors in the symptom count version gave a McDonald’s ω > 0·90 (ω
factor 1 = 0·92 and ω
factor 2 = 0·93) and a KR-20 internal reliability coefficient α > 0·86 (α
factor 1 = 0·86 and α
factor 2 = 0·88).
Table 4 Factor loadings for the multiple factor structure of the Malay Yale Food Addiction Scale (YFAS) 2.0
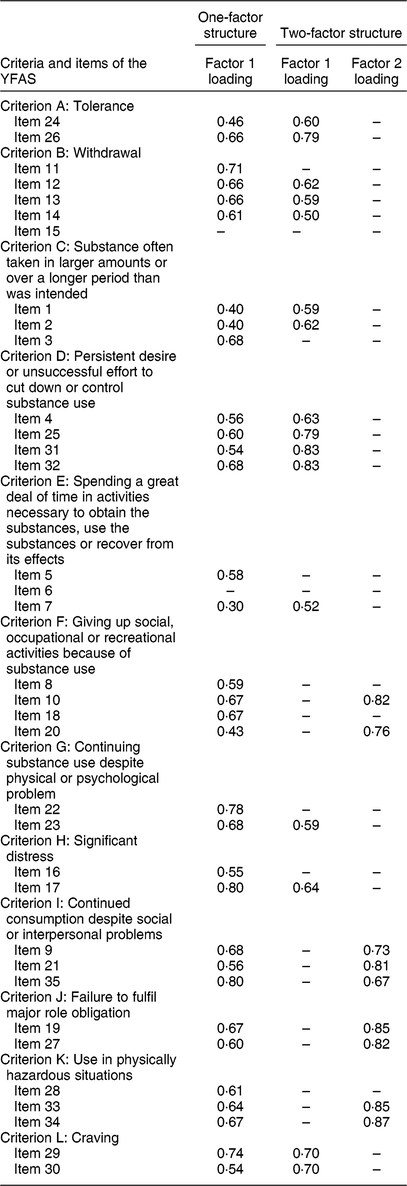
Exploratory factor analysis of the diagnostic component of the questionnaire was based on the twelve dichotomous diagnostic criteria in DSM-V. Structural equation modelling revealed a two-factor solution with factor loadings of each criterion greater than 0·4 (Table 4)(Reference Gearhardt, Corbin and Brownell19). The alternative one-factor solution revealed a cumulative variance of 38·0%. However, the cumulative variance increased to 51·4% when a two-factor solution was chosen. The evaluation of the items within the diagnostic criteria gave a McDonald’s ω > 0·90 (ω
factor 1 = 0·94 and ω
factor 2 = 0·90) and KR-20 internal reliability coefficient α > 0·7 (α
factor 1 = 0·82 and α
factor 2 = 0·74). Similarly, confirmatory factor analysis revealed that the two-factor model of the Malay YFAS 2.0 fit the data (
![]() $\chi _{(54)}^2 = 127 \cdot 7$
, P < 0·001, comparative fit index = 0·92, Tucker–Lewis index = 0·91, root-mean-square error of approximation = 0·046).
$\chi _{(54)}^2 = 127 \cdot 7$
, P < 0·001, comparative fit index = 0·92, Tucker–Lewis index = 0·91, root-mean-square error of approximation = 0·046).
Sampling adequacy was evidenced by a Kaiser–Meyer–Olkin value of 0·86 and the Bartlett’s test of sphericity of P < 0·01. Mean inter-item correlation was 0·48.
Item analysis and omission from scale
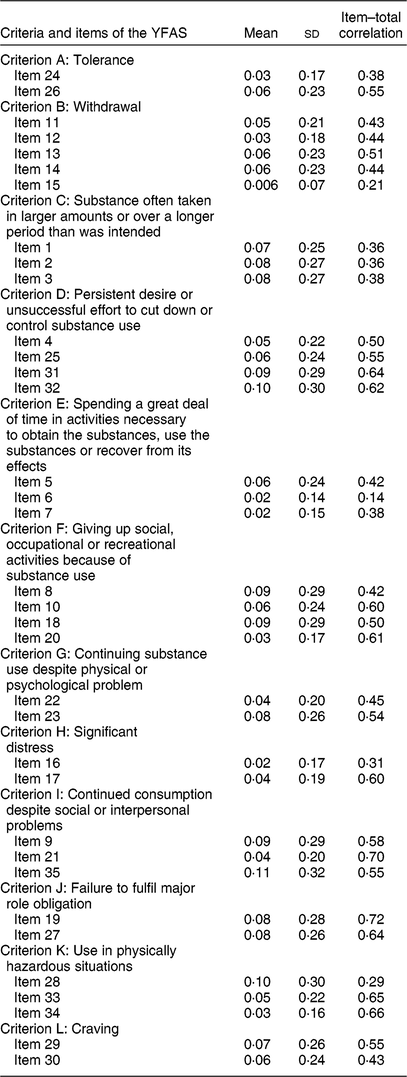
Items with the lowest factor loadings also had the lowest item–total correlation (Tables 4 and Tables 5). Therefore, items 6, 15 and 28 were omitted from the scale due to poor factor loading and item–total correlation. The remaining items in the scale had an item–total correlation of more than 0·30. Although questions 3, 8, 11, 14, 15, 18, 22 and 28 had good item–total correlation, these items were omitted from the construct due to cross-loading between the extracted factors (Tables 4 and 5).
Table 5 Item statistics for the Malay Yale Food Addiction Scale (YFAS) 2.0
Convergent validity
The Malay YFAS 2.0 symptom counts were associated with higher binge eating severity (r = 0·46, P < 0·001). Similarly, the diagnosis of food addiction was associated with an increase in binge eating severity (r = 0·25, P < 0·001). Symptom counts and the diagnosis of food addiction had a small positive correlation with higher BMI level (r = 0·14, P < 0·01 and r = 0·16, P < 0·01, respectively). Food addiction symptom counts and BES scores were also associated with the diagnosis of type 2 diabetes (r = 0·15, P < 0·01 and r = 0·17, P < 0·01, respectively). However, symptom count and food addiction scores were not associated with gender, age, race or education.
Incremental validity
In a simple linear regression, binge eating score was a predictor of BMI (t = 22·3, β = 0·18, P < 0·001), accounting for 6·1% of the variance. Similarly, Malay YFAS 2.0 symptom count score was also a predictor of BMI (t = 66·7, β = 0·37, P < 0·001), accounting for 2·0% of the variance. In hierarchical multiple regression, when binge eating score was entered in the model, Malay YFAS 2.0 symptom count was not a significant predictor (t = 0·96, β = 0·15, P = 0·34).
Discriminant validity
There was a statistically significant difference between BES severity and symptom count score (F (2355) = 60·9, P < 0·001). A Bonferroni post hoc test revealed that mean symptom count was statistically significantly higher in participants with severe binge eating symptoms (3·18 (sd 2·98)) compared with participants with moderate (0·73 (sd 1·43)) and no binge eating symptoms (0·36 (sd 0·94)). On the other hand, the diagnosis of food addiction was associated with higher BES score (r t = 0·211, P < 0·001). There was a statistically significant difference in mean BES score between participants with (33·2 (sd 7·77)) and without (23·3 (sd 8·14)) the diagnosis of food addiction (t (356) = −5·01, P < 0·001).
Discussion
Main findings
In this renewed attempt at validating the Malay version of the YFAS 2.0 questionnaire, greater emphasis was placed on inclusivity. This objective was achieved by obtaining undifferentiated participants from a community-based setting. The results from the study indicate that both the symptom count and the diagnostic version of the scale have a two-factor structure solution. Although this factor structure differs from the original study and translated versions of the YFAS, the validity of the model is supported by excellent internal consistency of the scale in its diagnostic and symptom count versions(Reference Gearhardt, Corbin and Brownell7–Reference Innamorati, Imperatori and Manzoni10).
The responses from the participants appear to support the concept of duality in terms of food addiction symptoms. The validity (factor loadings > 0·4) and the reliability (α > 0·80) of both versions were excellent. Hence, the two-factor solution for the symptom count and diagnostic version of the questionnaire demonstrates the dichotomous perspective through which the Malaysian populace views the concept of food addiction: a psychological and a social dimension. This discovery allows the creation of exclusive interventions for food addiction symptoms that are inclined towards either the psychological or social perspective.
Interestingly, the removal of items 3 and 18 from the scale was consistent with a previous preliminary analysis of the scale in Malaysia where similar items were dropped from the YFAS 1.0 scale(Reference Swarna Nantha, Abd Patah and Ponnusamy Pillai11). Items 6 (much time/activity to obtain, use, recover), 8 (important social, occupational or recreational activities given up or reduced), 11, 15 (characteristic withdrawal symptoms; substance taken to relieve withdrawal), 16 (use causes clinically significant impairment or distress), 18, 22 (use continues despite knowledge of adverse consequences) and 28 (use in physically hazardous situations) were uniquely new items that had to be removed from this scale while preserving the overall integrity of the scale.
Comparison with literature
The prevalence of food addiction in the present study was 5% based on the assessment of a community-based population. This result was comparable to other studies done involving similar populations. The prevalence rates seen in the French and English versions of YFAS 2.0 were 7·9 and 6·0%, respectively(Reference Schulte and Gearhardt15,Reference Brunault, Courtois and Gearhardt27) . The Spanish version of the YFAS 2.0 demonstrated lower food addiction rates in a healthy control group (2·9%)(Reference Granero, Hilker and Agüera28). However, the prevalence of food addiction appears to be higher in participants with morbid obesity (47%) and eating disorders (73%)(Reference Granero, Hilker and Agüera28,Reference Meule, Müller and Gearhardt29) . In our study, obese patients (47%) and participants with severe binge eating disorder (83%) had greater risk of being diagnosed with food addiction. These findings suggest that participants with obesity and eating disorders are predisposed to food addiction tendencies.
In the present study, the highest endorsement rate of 17·3% was exhibited in three criteria, namely ‘substance taken in larger amount and for longer period than intended’, ‘important social, occupational or recreational activities given up or reduced’ and ‘continued use despite social or interpersonal problems’. In a similar study done in Germany, the criterion ‘substance taken in large amount and for a longer period of than intended’ exhibited the highest endorsement rate of 24·0% in a normal population followed by ‘persistent desire or repeated unsuccessful attempts to quit’ (16·7%)(Reference Meule, Müller and Gearhardt29). A sub-study within the same study involving obese patients demonstrated that the ‘persistent desire or repeated unsuccessful attempts to quit’ criterion was the single most important factor contributing to food addiction (48·1%)(Reference Meule, Müller and Gearhardt29).
Strengths and limitations
There were several limitations of the present study. First, the temporal stability of the translated questionnaire was not assessed. However, this shortfall in the study was addressed by undertaking two phases of rigorous pilot testing along with the integration of information derived from participant feedback. Second, we were not able to assess psychological elements related to food intake in the absence of a validated Emotional Overeating Questionnaire (EOQ) in the Malay language. Further refinements can be made to the Malay YFAS 2.0 by controlling potential mediators (e.g. smoking status or alcohol consumption) that might influence eating patterns in participants.
Conclusions
Data on food addiction in a South-East Asian society are scarce. Our study has validated the YFAS 2.0 inventory in a Malay-speaking population and its utility extends to countries such as Malaysia, Indonesia and Singapore. Furthermore, interventions can be designed to address both psychological and social aspects of a susceptible individual.
Acknowledgements
Acknowledgements: The authors would like to thank Dr Ananth Kumar for his support during the process of writing this article. A special thanks to Dr Ashley Gearhardt for her feedback and suggestions that have helped render the manuscript in its current form. The authors would also like to thank the Director General of Health Malaysia for allowing this study to be conducted at the research site and permission to publish this paper. Financial support: This research did not receive any specific grant from any funding agency in the public, commercial or not-for-profit sectors. Conflict of interest: All of the authors have read and approved this manuscript and have no conflict of interest to disclose and industry relationship. Authorship: Y.S.N. contributed to the conception and the design of the study. S.N.Y., A.K., M.P.S., P.S., S.G.K., S.S.P. and N.A.O. contributed to data collection. Y.S.N., A.K. and S.M.S. worked on analysis and interpretation of the data. Y.S.N. wrote the first draft. Y.S.N. and A.K. performed relevant literature review and revision of the manuscript. All authors approved the final version of the manuscript; all persons designated as authors qualify for authorship and all those who are eligible for authorship are listed. Ethics of human subject participation: This study was conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving research study participants were approved by the Medical Research Ethics Committee, Ministry of Health Malaysia (NMRR ID: NMRR-17-2189-36204). Written informed consent was obtained from all participants.







