The report presented by the Committee on Medical Aspects on Food Policy (COMA) on Nutritional Aspects of Cardiovascular Disease (1) identified sodium, and therefore salt intake, as an important determinant of high blood pressure in the UK population and recommended a reduction in average salt intake by the adult population from 9 g (3·6 g/150 mmol Na), which was the level at the time (1994), to 6 g (2·4 g/100 mmol Na) per day. In 2003, the UK government's Scientific Advisory Committee on Nutrition (SACN) reviewed the evidence linking salt and health and concluded that the evidence of a link between high salt consumption and high blood pressure had strengthened since the review by COMA and that a reduction in the average salt intake of the UK population would proportionally lower average blood pressure levels and confer significant public health benefits by contributing to a decrease in the burden of CVD. It has been estimated that 6 % of deaths in the UK from CHD can be avoided if the number of people with high blood pressure is reduced by 50 %(Reference McPherson, Britton and Causer2), and that a reduction of 2 mmHg in mean adult diastolic blood pressure would result in a 15 % reduction in the risk of stroke and transient ischaemic attacks and in a 6 % reduction in the risk of CHD(Reference Cook, Cohen and Hebert3). Reducing salt intake to 6 g/d in populations equates to approximately 2·5 million preventable deaths globally every year(4). SACN also noted that the relative risk for CVD increases even within what is considered to be the normal blood pressure range (both systolic and diastolic), signifying that a large number of people are at risk(5, Reference Stamler, Stamler and Neaton6).
Following SACN's review, the Food Standards Agency (FSA) and the Department of Health (DH) committed themselves to reducing salt intakes in line with the recommendations made by SACN(5) and set a target to reduce the average salt consumption of adults to 6 g/d and work towards achieving lower targets for children (Table 1). The 2000–2001 National Diet and Nutrition Survey (NDNS)(Reference Henderson, Irving and Gregory7) estimated the average adult salt intake, calculated from urinary Na excretion, to be 9·5 g/d (11 g/d in men and 8·1 g/d in women). This meant achieving a reduction in intakes of approximately 40 %. This target was considered to be an achievable population goal rather than an optimal or ideal level of consumption(5).
The present paper describes the FSA's salt reduction programme and its effectiveness. The importance of working with industry to secure reductions in processed foods is highlighted, along with the improvements in public awareness that were achieved. The future challenges faced in achieving the population average salt reduction target of 6 g/d are also explored.
Taking policy forward to reduce salt intakes
A programme of work was developed to tackle salt reduction. This programme had high-level political leadership and consisted of three key elements: setting targets and working with all sectors of the UK food industry to reformulate foods to reduce salt levels; encouraging the use of improved nutritional labelling to make it easier for consumers to make healthier choices; and undertaking consumer awareness campaigns and working with non-governmental organisations (NGO) and local authorities to raise awareness of salt as a health issue, promote dietary change and stimulate demand for foods with lower salt levels.
Reformulation of processed foods
In the UK and other Western populations, approximately 75–80 % of dietary salt is obtained from processed food(8). Stimulating activity to reformulate such food is therefore an essential part of any salt reduction strategy in countries such as the UK. The FSA began this task by developing a Salt Model(9), which was published in 2003. This was devised to inform discussions with the food industry on reducing the salt content of foods and to illustrate the size of reductions necessary in different product categories to enable the 6 g/d target intake to be achieved, on average, across the population. The model showed the different foods contributing to UK salt intakes, together with the average level of salt for each category and the percentage contribution each category made to average intakes, with the data for each weighted to take account of the different levels of consumption of various foods within each group. It also included an ‘illustrative average target level’ for each category; if each of these was achieved across all products within the category, together with an assumed 40 % (1 g) reduction in consumers’ discretionary salt use, the 6 g/d target intake for adults could be achieved. Although all food categories contributing to the population's salt intake were included in the model, the main focus comprised those food categories providing most salt in the UK diet. The Salt Model showed that reaching the population average intake target of 6 g/d would require a substantial and concerted effort by manufacturers, retailers and food service outlets, as well as a supportive environment backed by the government, to stimulate consumer engagement.
In 2005, the FSA began the process of setting targets for levels of salt in foods. The purpose of these targets was to address the request from some UK food businesses for guidance on the reductions they should be aiming for and to provide a benchmark for monitoring progress in salt reduction. The targets were also intended to encourage a reduction across the board within a category, by the designated date, by stimulating the reformulation of the majority of products within a category towards those already on the market with lower salt levels. It was recognised that gradual, stepwise reductions made across categories were more likely to prove acceptable to consumers, provided the reformulation process allowed sufficient time for consumers’ palates to adjust to the lower salt levels and to the change in taste of familiar foods. Underpinning this approach was the belief that, over time, there would be no commercial benefit for those companies maintaining higher salt levels in products, as these would ultimately be rejected by consumers as tasting too salty. Product surveys conducted by the NGO and consumer groups highlighted those companies with higher salt levels in their products, putting them at a possible commercial disadvantage.
The first set of salt reduction targets for the food industry was published in March 2006. The targets covered eighty-five food types in thirty different food categories and were designed to be met by 2010 to allow for gradual stepwise reduction in salt levels.
In developing the targets, expert advice on safety issues and the technical feasibility of salt reduction targets in the various food groups were considered by the FSA, along with information on the reductions in salt levels already achieved, current dietary intakes and salt levels in foods. A key consideration was that there already existed products on the market with salt levels lower than those of others in their category, illustrating the potential for salt levels to be reduced, in most cases, across the category. The targets were also subjected to extensive consultation with stakeholders, particularly with the food industry. In addition, nationally representative data on food consumption from the NDNS(Reference Henderson, Irving and Gregory7) were used to examine the contribution of different types of food products to salt intake in adults and young people. As the main food categories that contributed to salt intakes were found to be generally similar for both adults and children, separate targets aimed at foods developed specifically for children were deemed unnecessary.
At the time of publishing the salt targets in 2006, the FSA announced its intention to conduct a review of progress made by food manufacturers and retailers towards achieving the category-based targets. This took place in 2008. The main findings were that many companies had made significant reductions and that, for some foods, reductions had gone further than that which the industry had indicated would be possible before the 2006 targets were published. However, the review also found that the range of levels among similar products was still wide and therefore there was the potential to reduce levels further in many products.
After consulting in 2008 on proposals for revisions to the targets, in May 2009 the FSA published a new set of stricter salt target levels to be achieved by 2012, covering all existing product categories (with some minor exceptions). These newer targets were considered challenging for the industry to achieve (because of a combination of technical and consumer acceptance reasons) and the government has continued to work in partnership with industry to ensure that the maximum reductions that can be achieved are accomplished. This has included the development of guidance for small businesses.
Importantly, apart from setting targets, the FSA worked to create an environment that supported a continued commitment from the food industry to reduce levels of salt in food; this was recognised to be key to the achievement of the programme's goal of reducing salt intake because of the amount of salt that is already in the food when it is purchased. The FSA showcased achievements by individual companies involved in the salt reduction programme in the FSA's salt commitments table published on its website (www.food.gov.uk).
Front-of-pack labelling
Between 2004 and 2010, the FSA worked with stakeholders to explore how best to provide additional nutritional information on the front of packs (FOP) of food to help consumers make healthier choices. In March 2006, the FSA recommended a principle-based approach for the provision of voluntary FOP nutritional labelling to help consumers make ‘at a glance’ healthier choices using traffic-light colour coding(10). FOP labels typically indicate the amount (in grams) of fat, saturated fat, sugar and salt in a portion of the product, and some also provide information on energy. Some labels accompany this information with text or traffic-light colours to indicate whether the level of these nutrients is ‘low’, ‘medium’ or ‘high’ and others depict the contribution a portion of the product represents in terms of the percentage of the guideline daily amount (GDA)(11, Reference Rayner, Scarborough and Williams12) of the relevant nutrients. Products with more greens (low) and ambers (medium) and fewer reds (high) represent healthier choices. The amber/red (medium/high) boundaries are based on UK Dietary Reference Values as advised by COMA and SACN. The low (green) criterion reflects values set in the EU Nutrition and Health Claims Regulation (EC no. 1924/2006).
A number of UK food manufacturers and retailers voluntarily introduced FOP labels that adhered to some or all of the FSA's recommendations. The various FOP labels in the UK marketplace mainly differed with respect to the interpretative elements used within them. Food businesses have reported that the introduction of FOP labels has helped to drive product reformulation activity and has encouraged manufacturers and retailers to develop a wider range of healthier foods for consumers to purchase, and that this extra information is appreciated and valued by their customers.
It is now widely accepted that FOP labelling is useful and valued by consumers, making it easier for them to make healthier choices when shopping(10, Reference Borgmeier and Westenhoefer13, Reference Cowburn and Stockley14). However, the qualitative phase of independent research to evaluate FOP labelling, published in May 2009, suggested that the coexistence of various FOP labels with differing interpretive elements was causing a degree of confusion and distraction for UK consumers(Reference Malam, Clegg and Kirwan15). The researchers also concluded that, although the words ‘high, medium and low’ had the greatest influence on comprehension, combining this information with traffic-light colour coding and percentage GDA information enabled more consumers to make healthier choices(Reference Malam, Clegg and Kirwan15). This view was echoed by consumers who took part in a series of citizens’ forums(Reference Stockley, Jordan and Hunter16).
In March 2010, the FSA Board considered the available research on FOP and agreed upon an FOP framework that they believed would strengthen arrangements further. The FSA then encouraged all food and drink businesses to move to a single FOP labelling format that contained the three interpretative elements: text indicating whether the level of a nutrient is high, medium or low; traffic-light colour coding; and percentage GDA, all of which had been found in research to be helpful to consumers in making healthier choices.
Public awareness campaign
Reformulation work was complemented by the FSA's public awareness campaign that aimed to: improve consumers’ knowledge of the link between salt and health; increase consumers’ demand for lower-salt products; and educate them on what they can do to reduce their salt intakes and how to make lower-salt choices. The campaign was conducted in four phases: in September 2004, October 2005, March 2007 and October 2009. The campaign involved television, radio, press and poster advertisements; leaflets and other materials for consumers; experiential activity at supermarkets (interactive activity involving quizzes, provision of information and product tasting); digital advertising; and information published on the FSA's websites.
Phase 1 of the campaign featured ‘Sid the Slug’ and aimed to increase public awareness of the risks of high salt consumption. Phase 2, ‘Talking Food’, emphasised the 6 g/d salt target and encouraged consumers to ‘check the label’ for the salt content of individual foods. Phase 3, the ‘Full of It’ campaign, focused on informing consumers that 75 % of the salt they consume is already in the everyday foods they purchase; therefore, they should check the labels and choose options lower in salt. Phase 4 reinforced messages from the previous campaign phases and also highlighted foods with ‘hidden’ salt and offered practical solutions for reducing salt intake.
The public awareness campaign's main target group comprised women aged 25–65 years in social demographic groups C1, C2 and D, as women in the household are considered to be the main gatekeepers when it comes to food and health. However, all adults were exposed to the campaign messages. During the second and third phases of the campaign, some food companies and some NGO carried out work to help disseminate the campaign messages to hard-to-reach groups. This included, for example, educational and practical programmes such as cooking classes, tasting sessions and grocery shop tours. The target groups for the initiatives included black and minority ethnic groups, inner-city communities, young parents, Hindu and Sikh populations and housing association staff and residents (more information on some of these projects can be found at http://www.food.gov.uk/news/newsarchive/2008/jun/saltpart).
Other Food Standards Agency work that may have contributed to reducing UK salt intakes
As well as working with retail and manufacturing organisations to reduce the levels of salt in food, the FSA also had a specific programme of work in association with the catering sector. A flexible framework was devised to highlight the four areas in which those providing food eaten away from home could take action. This approach had some considerable success, with forty-five companies across several key areas within the catering sector (suppliers to the catering sector, quick-service restaurants, workplace caterers, pub and high-street restaurant chains and coffee and sandwich shops) committing to take action to provide healthier food when people eat away from home. This included taking action to procure foods with lower levels of salt, reviewing kitchen practices and menu planning and considering the information available to customers to help them make informed choices. Although the catering sector was not a priority at the beginning of the salt reduction programme and, as a result, was not as far advanced as other parts of the UK food industry, some companies engaged themselves with the salt reduction programme for a number of years and made good progress with their salt reduction initiatives. In addition, a programme of engagement with small- and medium-sized, often independent outlets was also taken forward.
As well as providing information and advice to consumers through the specific public awareness work on salt referred to earlier, the FSA's ‘eatwell’ website provided online information about why it is important to cut down on salt and how much salt we should have in a day; it highlighted those foods that are key sources of salt in the diet, provided guidance on how to check food labels for the level of salt contained in a food item and included a section giving consumers tips for reducing their salt intake. Activity also focused on guidance on the procurement of food served in public sector institutions, including the procurement, cooking and serving of foods to reduce salt intake, and this added to the demand for industry to produce lower-salt alternatives. Other FSA initiatives, such as those with football and rugby clubs (‘Something to Chew On’ and ‘Kick and Cook’) and with social networks (e.g. blink), also contributed to the salt reduction programme by including messages and suggested actions to help young people choose, cook and eat safe and healthy food, including those foods lower in salt.
Overall effectiveness of the Food Standards Agency's salt reduction programme
Change in the population's average salt intake has been monitored using urinary Na excretion data collected through surveys, with samples representative of the UK population. This is the method of choice because assessment of salt intake using dietary records is notoriously difficult, not least because of the challenge of assessing discretionary salt addition at the table and in cooking. In 2000–2001, using this methodology, salt intake in adults was estimated to be 9·5 g. By 2005–2006, average intake among adults had fallen by 0·5 g/d to 9·0 g/d. Urinary Na levels were assessed again in 2008, and the average adult population salt intake was estimated to be 8·6 g/d(17). The 0·9 g reduction in UK salt intakes (since 2001) is assumed to be the direct result of efforts across the manufacturing, retail and (more recently) food service sectors to reformulate products, coupled with changes in consumers’ dietary practices.
Effectiveness of reformulation by the food industry
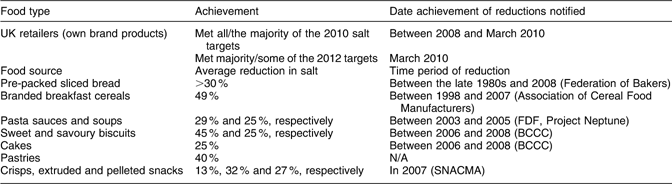
The FSA has gathered information through a number of routes on the reductions achieved in the salt content of foods over the time that its salt reduction programme has been running. These routes included collecting data on salt levels in products, both directly from food companies and by purchasing label data from a market research company. In addition, more general information was collected from food companies about past successes and future intentions. Examples of progress are provided in the ‘salt commitments table’ on the FSA website. Organisations such as the Food and Drink Federation (FDF) and British Retail Consortium published regular reports on the progress achieved by their members, and other trade associations collected data from their members (generally manufacturers of branded products) and submitted them to the FSA. The extent of this information served to underline the considerable commitment and work across all sectors of the food industry – retailers, manufacturers and food service providers – which have together contributed to the reduction in UK salt intake achieved to date. It is noteworthy that significant reductions have been achieved often by manufacturers working together; for example, ‘Project Neptune’ of the FDF, which focused on soups and sauces, and action by the Association of Breakfast Cereal Manufacturers. Some examples of this are shown in Table 2.
Effectiveness of the Food Standards Agency's public awareness campaign
The success of all four phases of the FSA's public awareness campaign was evaluated using data obtained by placing questions in a continually running survey that gathered answers from a nationally representative sample (approximately 2000 people) of the UK adult population. The data showed that the campaign was successful in highlighting the link between eating too much salt and increased blood pressure and in instigating changes in consumers’ claimed behaviour. Data collected at the end of 2009, following the fourth phase of the campaign, showed that 43 % of all adults claimed to have made a special effort to cut down on salt in their diet compared with 34 % of adults in August 2004 (26 % increase), before the awareness campaign commenced. Of them, 21 % claimed to be doing so by checking food labels compared with only 7 % before the campaign started (200 % increase). The percentage of adults who claimed to look at food labels to find out the salt content increased to 50 % following the fourth phase of the campaign, compared with 29 % in August 2004 (72 % increase). Similar increases were seen in the target audience (women aged 25–65 years in social class categories C1, C2 and D).
The consumer awareness work carried out by NGO during the second and third phases of the public awareness campaign (mentioned previously) was evaluated by each organisation individually using various methods, such as face-to-face interviews, questionnaires and focus groups. Findings from eight evaluation projects are available on the FSA website(18). These findings highlight a number of achievements regarding increased awareness and knowledge (such as the practical food-based interventions involving participants that have great potential to create an impact on hard-to-reach groups), as well as difficulties in running the project (such as time constraints to conduct the intervention) or in implementing the evaluation methodologies.
Challenges associated with the Food Standards Agency's salt reduction programme
A number of challenges have been identified, including concerns regarding the effect of salt reduction on the microbiological safety of food, as well as consumers’ acceptance of salt-reduced foods, along with specific technological barriers. Although these are significant issues that apply to a number of foods, as mentioned below there are various actions that can be taken to mitigate at least some of the obstacles that arise.
Although many foods do not rely solely upon salt to prevent the growth of pathogens or spoilage micro-organisms, it is recognised that salt usage can be an important factor in the safety and quality of certain foods, such as meat products. In these foods, salt reduces the amount of ‘available’ water present in the food, which is required for microbial growth, causing micro-organisms to grow more slowly or not at all. Consequently, when reducing the level of salt in these foods, manufacturers need to consider potential effects on microbiological safety. However, concurrent with salt reduction, it may be possible to adjust other properties of the food, such as acidity (i.e. pH), or use different processing/packing systems so that safety is not compromised and shelf-life is not shortened.
The FSA considered the consequences of its salt reduction programme on food safety by commissioning research(Reference Stringer and Pin19) and consulting with the Advisory Committee on the Microbiological Safety of Food (ACMSF, an independent advisory committee to the FSA). The ACMSF considered the FSA's strategy on salt reduction to be sound(20, 21). In addition, the FSA reiterated to manufacturers, through stakeholder engagement and guidance documents, the importance of assessing the potential impact that reformulation might have on microbiological safety and identified approaches to mitigate risk(22).
In those food categories in which the main obstacle to salt reduction is consumers’ acceptability, it has been demonstrated that a series of small stepwise reductions over time can limit rejection by consumers. It may be necessary for some of the salt to be replaced by other flavouring ingredients or for the balance of ingredients and flavourings in the recipe to change to account for the reduction in salt level and maintain consumers’ acceptability. In addition, research suggests that palates adapt to a lower salt concentration over a period of approximately 8 weeks, as after this time participants were seen to reject the higher-salt diet they consumed previously(Reference Blais, Pangborn and Borhani23). Although some food industry sectors indicated an increase in complaints of bland food, the most serious issues occurred when a higher percentage of salt was removed in a single step or when fat and salt reductions were attempted simultaneously. Data suggest that consumers are adjusting to lower-salt diets; sales of table salt declined between 2004 and 2007 and remained relatively static in 2008–2009 once sales were adjusted for increased purchases following heavy snowfall in February 2009.
Salt has a technical, functional role in the manufacture or processing of a number of foods, such as bread, cheese and some meat products. In bread it controls yeast fermentation and hence dough development, and in cheese production it is required to separate the whey from the curds from which cheese develops. It is likely that, for some of these foods, overcoming technical issues will be particularly challenging and may therefore take more time and be dependent on technological advances and on the introduction of new processing techniques and/or new ingredient solutions. However, work carried out by the FSA to review progress in 2008 showed that there remained a range of salt levels among similar products, even within these more challenging categories, showing that it is possible to manufacture products with lower salt levels and organoleptic properties that remain acceptable to consumers. The FSA has supported industry in those product areas in which technological issues apply and has funded two projects that aim to assist with reducing the salt level in bread(24, 25).
There were challenges associated with running campaigns providing public awareness messages about salt. These included various areas such as: the significant costs associated with undertaking work of this kind; identifying the primary target audience that would be most receptive to messages and that would take action as a result (adults in general, as opposed to a subgroup, are likely to be a secondary audience); ensuring that the whole campaign package provided the most effective approach(es) to getting messages across and the best value for money; ensuring that the messages themselves remained effective and motivational, particularly as successive phases of the campaign followed; and recognising that messages about salt were just one of many health messages that encouraged behavioural change.
International context
The FSA's approach to salt reduction is now being used as a model for activity in other parts of the world. The European Commission has an established framework for action on salt reduction, which includes the same areas of activity as the UK programme. All twenty-seven member states are now signatories and have indicated that they are undertaking some action related to the framework. The New York City Health Department is coordinating The National Salt Reduction Initiative, a coalition of cities, states and health organisations working to help food manufacturers and restaurants voluntarily reduce the amount of salt in their products, and has recently published a set of salt targets(26); and plans for salt reduction work in Canada, published on 29 July 2010, also follow the UK approach(27).
The Pan American Health Organization has published a statement outlining the roles of the various stakeholders in reducing salt intakes and is now working to build a coalition for action across the Americas (www.paho.org/cncd_cvd/salt). Work has already advanced in Canada, the USA, Argentina and Chile. NGO are active in some countries where salt is yet to be prioritised in the national agenda (e.g. Australia).
The WHO is working simultaneously to prompt a greater number of countries to take action on salt reduction(4). It has outlined the importance of doing so in several of its key documents on non-communicable diseases, including its Global Strategy for the Prevention and Control of Non-communicable Diseases and the action plan for implementing this strategy. To build on this, the WHO is running platform events during 2010–2011 that aim to spread experience worldwide on salt reduction and provide help and guidance to those countries wanting to reduce the salt intake of their population. This work will focus on the extent to which progress to date is applicable to low- and middle-income countries. The first of these events, organised jointly with the FSA, took place in London on 1–2 July 2010 and was preceded on 30 June 2010 by an Information Exchange Forum with the private sector and NGO. The event comprised short presentations about the progress made to date worldwide and the challenges faced in different parts of the world. For example, in countries such as the UK and the USA, processed food is the major source of dietary salt, whereas in much of the Indian subcontinent and the Far East, street food and home-cooked food are the dominant contributors to salt intake, which can approach 20 g/d. Other countries, such as parts of South America, are in transition between the two extremes.
It was concluded that population-based strategies to reduce salt intake must be multidisciplinary, intersectorial and implemented in several settings. An output of the 2 d event is a report identifying actions for the various stakeholders: member states, the WHO, NGO, civil society and academia, and the private sector.
Actions such as these, which focus on sharing information and experiences, will help in the development and implementation of coordinated and consistent actions on salt reduction across several countries. The FSA-led programme has had demonstrable success in salt reduction, but the UK stands to benefit from action extending around the world because food imported to the UK can often have a higher salt content than that produced locally. Broader global action will facilitate a more level playing field and may serve to reduce the salt content in foods produced overseas but consumed in the UK, thus benefiting the UK consumer. Furthermore, it may encourage further action, particularly in multinational companies that trade across a number of different countries and that might otherwise have to consider manufacturing products with recipes that vary depending on the local preference for salt. Indeed, if all countries in a particular market or world region are signed up for salt reduction, the requirement to produce fewer versions of a particular product may result in cost savings.
Future plans for salt reduction in the UK
Nutritional policy, including salt reduction and FOP labelling, was transferred to the DH on 1 October 2010. Following the publication of the UK government's Public Health White Paper in November 2010(28), the Public Health Responsibility Deal was launched in England in March 2011. The Responsibility Deal aims to build on the potential of businesses and other organisations to improve public health and tackle health inequalities. Initial pledges by businesses have included commitments to meet nationally agreed salt reduction targets for 2012, which are largely based on those set by the FSA in 2009. As of May 2011, fifty-three organisations have ‘signed up’ to the commitment to meet these salt targets(29).
Conclusions
Achieving the salt reduction target of 6 g/d is expected to bring significant public health benefits. Starting with manufacturing and retail, and later embracing food service, substantial efforts have been made on a voluntary basis by all sectors of the UK food industry. This has resulted in some significant reductions in the levels of salt in food, with work set to grow, in particular, within the catering sector. However, continued effort by all stakeholders and retention of an enabling and supportive environment are necessary to maintain progress towards the population average salt intake target of 6 g/d.
Although it is difficult to show causality, the FSA salt reduction programme, which was ground breaking in its coverage of the different areas of work (reformulation, public awareness, increase in information to consumers on pack) and because it aimed to achieve salt reduction across the whole food chain, appears to have reduced salt intakes and increased consumers’ awareness. Effective cooperation and collaboration between the FSA and food industry and with a range of other stakeholders was key to the success of the salt reduction programme. The success of the FSA salt reduction programme highlights the need for future salt evaluation programmes and provides a model for how such work could be taken forward elsewhere. It should also give confidence to other European and international countries and food companies who are considering the adoption of similar salt reduction programmes.
This review was commissioned by the UK Food Standards Agency. The authors declare that they have no conflict of interest. J.L.B. and S.A.S. developed the scope and outline of the review and provided critical revision of the manuscript. L.A.W. wrote the first draft of the manuscript. The FSA provided information for the review and commented on and contributed to various drafts of the manuscript. All authors and contributors read and approved the final manuscript. Information about the British Nutrition Foundation's work, funding and governance can be found at www.nutrition.org.uk.