The 2016 Global Report on Diabetes( 1 ) brought attention to diabetes as a problem that health systems face across the world and stated that the number of diabetes cases in the world has doubled over the past 30 years. More than 80 % of deaths from diabetes occur in low- and middle-income countries. Due to high costs of care, among other factors, carrying out preventive interventions to stem the disease presents difficulties for health systems in these countries. The WHO points out that public policies focusing on health promotion related to treatment of chronic diseases such as diabetes have not had the desired effect( 2 ). One possible explanation is that health programmes generally fail to consider the impact of socio-economic status and vulnerable social environments as well as the influence of these factors on behaviours, including dietary changes promoted by health-care systems. Some studies show higher diabetes prevalence among the poorest and most socially excluded strata of populations, but other studies report lower risk among patients at lower socio-economic levels living in their places of origin, because of more limited access to a hyperenergetic diet and higher levels of physical activity( Reference Hee 3 , Reference Pérez-Escamilla 4 ). This evidence generated from around the world points to the complexity of intersecting situations that affect patients’ adoption of healthy lifestyles promoted as a central part of the treatment of diabetes and to the fact that individual responses to treatment are influenced by social determinants that shape behaviours( Reference Garcia, Gold and Wang 5 ).
The development of diabetes is related to unhealthy lifestyles including poor eating habits and a sedentary lifestyle, as well as genetic factors. Diabetes can lead to serious complications due to co-morbidities (obesity, dyslipidaemia and hypertension, among others) and associated consequences (blindness, kidney disease and limb amputation) at advanced stages. Diabetes has no cure but it can be controlled by following prescribed treatment and lifestyle change; the goal is for the patient to be able to self-manage the disease( 6 , 7 ). Furthermore, one of the risk factors for developing diabetes is eating foods with little nutritional value and high energy and fat content( 8 ). Thus, a central component of treatment is promotion of changes in eating habits, basically by incorporating foods with higher nutritional value into the daily diet. However, only a relatively small percentage of patients comply with dietary recommendations; for example, in Mexico recent data show that only 26·8 % of persons with diabetes diagnosis changed their eating habits( Reference Jiménez-Corona, Aguilar-Salinas and Rojas-Martínez 9 ).
On the other hand, regarding the Mexican population with diabetes, data on indigenous ethnicity are not available, as is true for other countries such as Guatemala( Reference Moreira Díaz 10 , Reference Bream, Breyre and Garcia 11 ). Although literature exists on the lived experience of diabetes among indigenous groups in Mexico( Reference Franck and Durden 12 – Reference Eroza-Solana 15 ), few publications focus mainly on food and diet. Recent exceptions are a study among the Chontal in Tabasco( Reference Cruz-Sánchez, Tuñon-Pablos and Villaseñor-Farías 16 ) and a study by Montesi in the Ikojts in Oaxaca( Reference Montesi 17 ), which discuss ambivalent food experiences among indigenous people with diabetes. Results from studies on native, indigenous or aboriginal groups in countries such as Australia, Canada, the USA and New Zealand( Reference Hee 3 ) show that these populations also have difficulties in incorporating and sustaining changes in food practices to adhere to dietary regimens related to diabetes treatment( Reference Hee 3 , Reference Macaulay, Cargo, Bisset, Ferreira and Lang 18 – Reference Epple, Wright and Joish 20 ).
From the perspective of the anthropology of food, the function of food is ‘the satisfaction of an indispensable life need combining cultural, psychological and biological domains’( Reference Mintz 21 , Reference De Garine and Hernandez 22 ). Food is linked with non-material aspects such as social origin, ethnicity, familial organization, religious beliefs, values, taste, affectivity and the dietary rules of different human groups (i.e. social norms on forbidden and allowed foods, the way food can be eaten)( Reference Harris 23 ). On the other hand, the current era is marked by what one author has called a ‘new food order’( Reference Gracia Arnaiz 24 ), characterized by the rapid development of the food industry and transnational companies that produce and distribute industrialized foods globally. One consequence of this is the increased homogenization of food habits worldwide. And indigenous populations have not been immune to this globalization process.
An important part of the cultural ethos of all human groups is anchored in the foods one eats, with whom one consumes them and in which situations specific foods represent social facts that produce meaning in daily life( Reference Harris 23 , Reference Fischler 25 – Reference Contreras and Gracia Arnáiz 27 ). The present paper is based on a cross-cultural approach( Reference Kirmayer, Guzder and Rousseau 28 , Reference Young 29 ) that alludes to the importance of understanding culture and other aspects of the specific context of different population groups. In the paper we also attempt to show how Mexican Mayans with diabetes respond to the clinical care processes that are focused on controlling the disease through diet, which is commonly recommended for type 2 diabetes management( 30 ). We analyse as well changes in food habits to understand the way culture shapes people’s responses to these processes. Our main research questions are: (i) How do Mayan people with diabetes change their eating habits in response to medical recommendations? (ii) How do sociocultural aspects influence this change of behaviour or lack thereof? Our questions stem from the hypothesis that the lack of adherence to dietary changes in this population is influenced by the cultural gap between hegemonic modern medical care and indigenous culture, which in turn leads to rejection and incomprehension (not mainly cognitive but cultural) of dietary recommendations among indigenous people.
Methods
The present paper is part of a larger research project; full details of the entire methodological design can be consulted elsewhere( Reference Juárez-Ramírez, Théodore and Villalobos 31 ).
Study design and integration of mixed methods
High levels of morbidity and mortality due to type 2 diabetes was the principal criterion for selecting indigenous communities for study. We thus chose the states of Chiapas, Quintana Roo and Yucatan. We identified all primary health-care clinics in each of the selected states and we reviewed the relevant statistics on indigenous people with type 2 diabetes treated in these health facilities. The resulting sample included six primary health-care clinics in six different communities. The sample of Mayan (indigenous) participants was purposive. People were considered indigenous if they spoke a native (Mayan) language. These people often belong to the lowest socio-economic strata in the Mexican population. The inclusion criteria were: (i) being a patient at the primary health-care clinic; (ii) having been diagnosed with type 2 diabetes at least 1 year prior to the study year; (iii) being an active member of a mutual support group organized by the health-care clinic, which indicated that the person was actively engaged in medical treatment; (iv) being at least 18 years old at the time of the study; and (v) having other family members with type 2 diabetes.
We used a partially( Reference Leech and Onwuegbuzie 32 ) sequential mixed methods( Reference Johnson, Onwuegbuzie and Turner 33 , Reference Morse and Niehaus 34 ) where each completed phase guides the subsequent steps in the inductive investigation. According to Leech and Onwuegbuzie, ‘with partially mixed methods, the quantitative and qualitative phases are not mixed within or across stages’( Reference Leech and Onwuegbuzie 32 ).
The first, exploratory, phase aimed to understand the context of the study setting, identifying the principal issues related to diabetes among Mayan persons with this health condition. Through ethnographic observation (in six communities) we generated information on access to health care, food and religious practices. For this we used mixed methods with a focus on development( Reference Greene, Caracelli and Graham 35 ) of the further study; that is, as indicated by Greene et al.( Reference Greene, Caracelli and Graham 35 ), we sought to use the results from the ethnographic observation to develop the questionnaire and the interview guide of the second phase.
The second phase aimed at exploring the experience of living with diabetes among Mayan individuals by qualitative and quantitative research conducted simultaneously. The eighty-nine-item questionnaire sought to generate quantitative information on personal characteristics (e.g. socio-economic profile, housing, family composition) and experience with diabetes (e.g. evolution of the disease, adherence to medical treatment) of Mayan patients receiving care at primary health-care clinics. Through the medical staff we invited Mayans patients who participated in the mutual support group to answer the questionnaire and 195 accepted. For the present paper, in addition to sociodemographic data, we analysed the difficulty of abstaining from certain foods.
Both brief and in-depth interviews sought to further explore Mayans’ experience of diabetes. A sub-sample was selected for the brief qualitative interviews and we interviewed 103 out of the 195 people selected through the questionnaire. Subsequently, on the basis of longer health-care trajectory or more severe diabetes-related complications and ability to narrate the experience, we selected a smaller group of individuals (n 20) to do in-depth interviews.
The interview guide topics explored in the present paper are: disease onset; diabetes knowledge; quality of care; disease management; health services utilization; family and social support network (see online supplementary material).
Data collection
To ensure the validity of the collected data all team members received training to standardize their knowledge about project objectives, data collection techniques and fieldwork procedures. Additionally, three anthropology students of indigenous origin who spoke the local language were hired as translators and data collectors. Special emphasis was placed on training them in the meaning of the questionnaire and interview guide questions, so that the information was appropriately translated into Spanish after collection and before entry in the database. They were also instructed about asking questions considering local culture. This training was especially important given the frequent illiteracy among the indigenous people that were interviewed.
All research team members had previous data collection experience. None of the interviewers had a previous relationship with the interviewees. The team received training on ethical issues for working with indigenous populations. The principal researchers were trained on ethics with the University of Miami’s online Collaborative Institutional Training Initiative (CITI Program) course. To prevent biased responses of the indigenous participants, the primary-care staff had no influence on selection of respondents and were not present during the interviews.
With illiterate respondents, the interviewers filled in the questionnaires directly. Qualitative interviews with indigenous participants were conducted in their native language (either Maya or Tzotzil). As an extra measure of quality control, some of the interviews conducted in Maya and Tzotzil were chosen at random and translated by other local residents. The brief interviews lasted approximately 30 min and the in-depth interviews lasted approximately 150 min and were carried out over two or three sessions. The saturation point of each category explored was discussed with the entire research team.
Previous to data collection, we pre-tested the questionnaire and interview guide to assess whether questions in both tools were clear to Mayan informants.
We carried out the fieldwork from 2008 to 2012, with multiple visits to the different communities included in the research.
Data analysis
From the project’s data set, we selected qualitative and quantitative data linked to the management of diabetes. Quantitative data collected with the questionnaires were data entered and explored using the statistical software package PASW Statistics for Windows, version 18.0. We used Student’s t test to estimate significant differences in mean age and Pearson’s χ 2 test for independence to analyse relationships between categorical variables. We did microanalysis of the qualitative data within the Grounded Theory framework( Reference Glaser and Strauss 36 ). Qualitative interviews were audio-recorded and transcribed literally. We then selected in-depth interviews to manually develop the main categories and codes( Reference Juárez-Ramírez, Théodore and Villalobos 31 ). Subsequently we used the previously identified manually developed codes in Atlas.ti version 6 to code the rest of the interviews (please see description in the online supplementary material, Supplemental Fig. S1, for the definition of each category). The current paper presents the results for the category Disease Management, defined empirically as any mention by participants of activities and changes made since their diagnosis of diabetes, including dietary habits, exercise and medication to manage the disease. From the previous central category, we identified three sub-codes: (i) Effect on diet, defined as any mention made or reasons given by respondents in relation to how they changed their diet, how changes affected them and what eating habits they did not change; (ii) Medications, defined as any references that interviewees made to actions taken to follow medication regimens or not follow them as prescribed; and (iii) Food meanings, defined as how interviewees understood dietary recommendations and what these changes meant in their cultural and economic context (please see description in the online supplementary material, Supplemental Fig. S2, to understand how the information was analysed).
The results were interpreted and organized into the following themes: (i) Poverty-based food culture; (ii) Cultural beliefs on origins of diabetes and their relationship to food practices and low adherence to dietary regimes; (iii) Misunderstood cultural practices from the perspective of interviewees: meaningless health talk; and (iv) Diet adjustments in a socially vulnerable context.
Ethics approval and consent to participate
The Declaration of Helsinki Ethical Principles for Medical Research Involving Human Subjects were considered for the present study. The participants provided verbal informed consent.
Results
The results are divided into three sections: characteristics and context of the study population; elements that shaped the participants’ food-related experiences; and a typology of responses to dietary recommendations made by the medical staff.
Characteristics and context of the study population
Medical care consisted of routine assessments that aimed to achieve metabolic control and prevent diabetes-related complications. Nevertheless, some participants had already experienced complications including lower-extremity amputation, retinopathy and kidney damage. The principal technique used by the medical staff to achieve metabolic control of Mayan people was group educational sessions focused on lifestyle changes within mutual support groups. Among other topics, group participants were given health education on how to change or improve their eating habits. Despite living in a context of extreme economic difficulty, interviewees mentioned that they made an effort to adhere to restrictive dietary recommendations. Below we describe the most relevant related points.
Of the 195 people surveyed (recruited at health-care clinics), 86 % were women, 75 % were over the age of 50 years and 39 % had no schooling. Comparison of Mayan people who said they fully understood the doctor’s explanations about their disease with those who said they did not shows that those who answered affirmatively were more likely to be housewives (86·7 v. 72·0 %, P = 0·048). No significant differences were observed by sex, marital status, schooling or family composition (Table 1).
Table 1 Sociodemographic characteristics of the study population according to their understanding of the doctor’s recommendations: sample of adult Mayans with type 2 diabetes from Chiapas, Quintana Roo and Yucatan, Mexico, 2008–2012
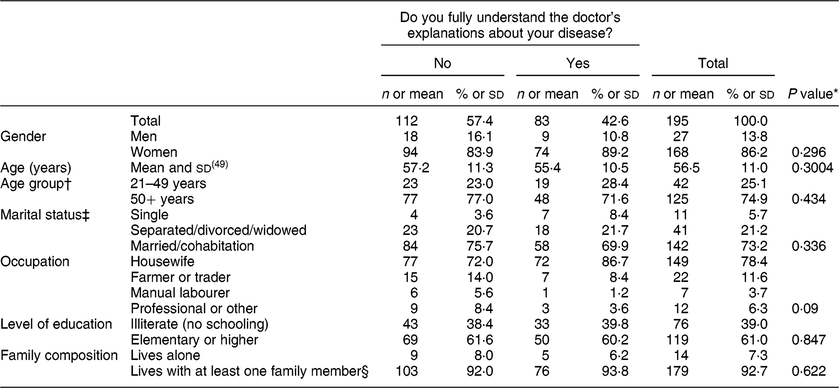
* Pearson’s χ 2 test, Fisher’s exact test or Student’s t test (to estimate a significant difference in mean age).
† Twenty-eight Mayan people who did not specify age, five Mayan people who did not specify occupation and five Mayan people who did not specify education level were excluded.
‡ Includes participants who lived with their parents, siblings, grandparents, spouse, children or some other relative.
§ Includes people who said they lived with their parents, siblings, grandparents, spouse, children or some other relative.
With regard to disease-related characteristics, 36 % had been diagnosed with diabetes 3 years or less before time of the interview, 52 % had family history of diabetes and 30 % had experienced a chronic complication related to diabetes (Table 2).
Table 2 Illness-related characteristics of the study population according to their understanding of the doctor’s recommendations: sample of adult Mayans with type 2 diabetes from Chiapas, Quintana Roo and Yucatan, Mexico, 2008–2012
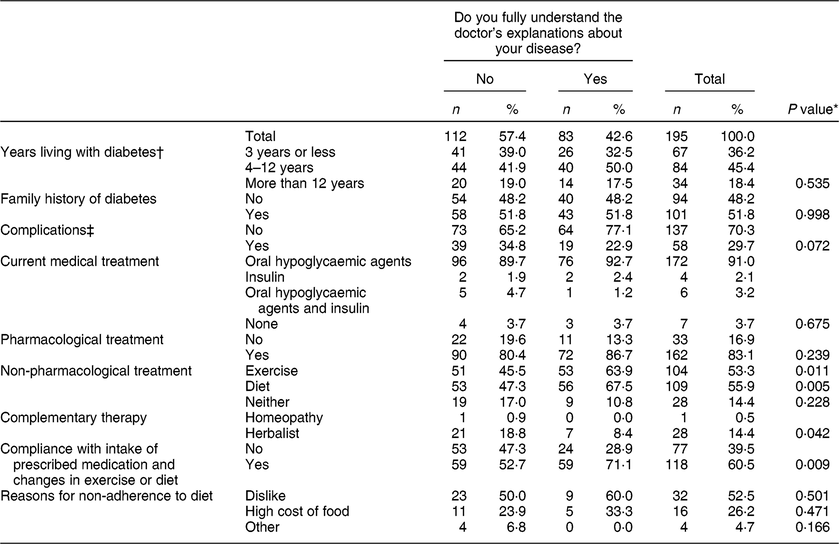
* Pearson’s χ 2 test or Fisher’s exact test.
† Ten Mayan people who did not specify number of years living with diabetes and four Mayan people who did not answer the question about compliance with medical recommendations were excluded.
‡ Complications included ulcers, kidney damage, visual impairment and diabetic coma.
Cultural beliefs on the origin of diabetes and their relationship to food practices and low adherence to dietary treatment
We grouped the experiences of the interviewees into five cultural explanations of their acquiring the disease, which mix elements of the information learned in the health education sessions (with medical staff) with their ancestral indigenous beliefs about the origin of the disease. Both aspects are related to foods that can or cannot be consumed. We identified five explanations for the disease. (i) Suffering from extreme emotions caused by violence, tension or precarious conditions: anger, fear, sadness, pain. (ii) Individual suffering as a punishment from God for having committed a deplorable act (disease as moral reparation). (iii) Magical beliefs related to being the object of revenge via a spell: ‘the evil eye’, ‘negative energy’ or ‘bad air’. (iv) Contamination of everyday foods due to farming with chemicals. (v) Consumption of foods high in sugar or fat (Table 3).
Table 3 Mayan people’s cultural beliefs about diabetes origin and their relationship with food habits and adherence to dietary treatment, Chiapas, Quintana Roo and Yucatan, Mexico, 2008–2012
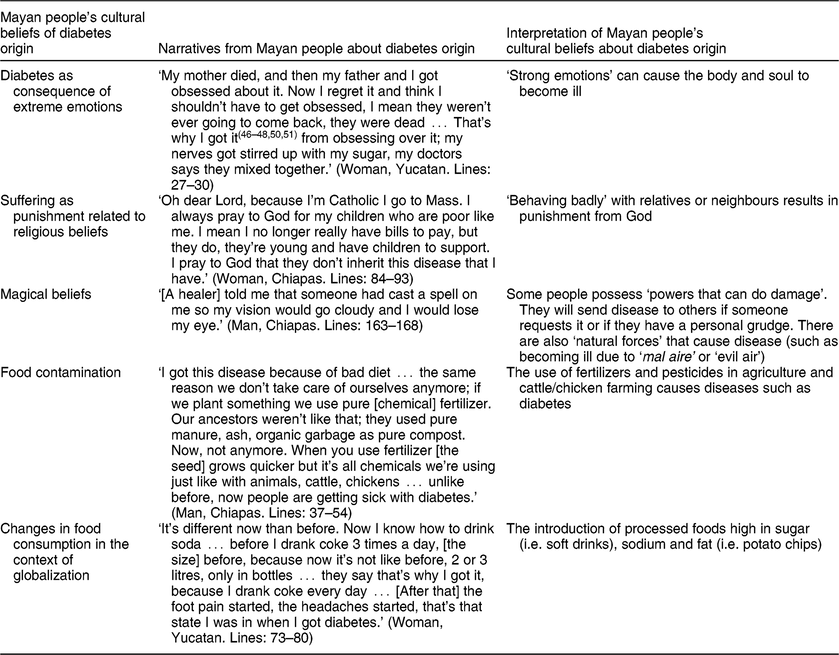
The informants’ narratives convey meanings and explanations of the origin of the disease from their cultural perspective, which in turn defines how the treatment process is understood. From the point of view of most Mayan people, the disease is rooted in emotional aspects; the food factor did not emerge in these explanations (Table 3).
Misunderstood cultural practices: meaningless health talk
The interviewees referred to the eating guidelines provided by the medical staff as a diet. This diet was seen as based on prohibiting or limiting the intake of beverages with high sugar content, foods with high fat content and carbohydrates. As shown by the narratives in Table 4, corn products (e.g. tortillas), sweets (e.g. soft drinks and pastries) and foods containing pork have a special value in community festivities and religious holidays, because most of these convivial get-togethers involve offering and consuming these types of foods. In Chiapas in particular, the informants mentioned the use of soft drinks in acts of religious syncretism and healing ceremonies. The habit of eating these foods, their association with culturally important holidays and the pleasure of eating them for their emotional symbolic value were important reasons for not following dietary recommendations.
Table 4 Medical recommendations about change of food habits according to Mayan people’s narratives, Chiapas, Quintana Roo and Yucatan, Mexico, 2008–2012

Of all restrictions, the most controversial were corn, pork and sugar-based foods. The consumption of these foods, even in economically marginalized populations, is not only the norm but also gives meaning to daily food practices. Across all three states, testimonies reflected a wide predilection for industrialized foods consumed on a daily basis, ranging from ingredients for meal preparation and salty snacks to multiple kinds of inexpensive sweet snacks and soft drinks. The ban on consuming these foods led to feelings of frustration and stress, and was perceived as ‘not being allowed to eat anything’ while being deprived of the ingredients they needed to prepare foods seen as traditional. In addition, these types of foods provide high satiety and have an important function in the real and everyday context of poverty.
Food restrictions from medical staff were accompanied by recommendations, the most common being about eating a lot of vegetables, having three meals per day along with two light meals or snacks, and stopping frying food in oil and/or lard (Table 4). Interviewees said they commonly used vegetables in small quantities to make different types of salsas, but they were not used to eating them alone. Furthermore, participants did not usually eat dinner, as recommended in the medical staff guidelines. Eating a ‘snack’ between meals was also a foreign, ‘medical’ concept; for indigenous participants, snacking was an unknown habit so this suggestion made no sense to them.
During the ethnographic observation we found that the medical staff provided contradictory information, especially about certain types of foods such as meat, because some doctors recommended eating meat and others did not. When Mayans said they did not understand medical recommendations this seemed to be multifactorial. Sometimes it happened due to lack of shared knowledge between Mayan people and providers, other times medical recommendations were misaligned with local cultural norms, and in other cases medical staff lacked cultural competence or the level of formal education was dissimilar between Mayan people and health-care providers. The questionnaire data show that individuals who did not understand the doctor’s instructions (30 % v. only 18 % who did understand) reported having problems reducing red meat consumption (P = 0·051, Table 5). Furthermore, a statistically significant association occurred between Mayans’ report on ‘fully understanding the doctor’s explanations about their disease’ and their report on adherence to treatment and changes in exercise or diet (P = 0·009, Table 2).
Table 5 Elimination of specific foods from the diet according to Mayan people’s understanding of doctor’s recommendations, gender, education and years with diabetes diagnosis, Chiapas, Quintana Roo and Yucatan, Mexico, 2008–2012
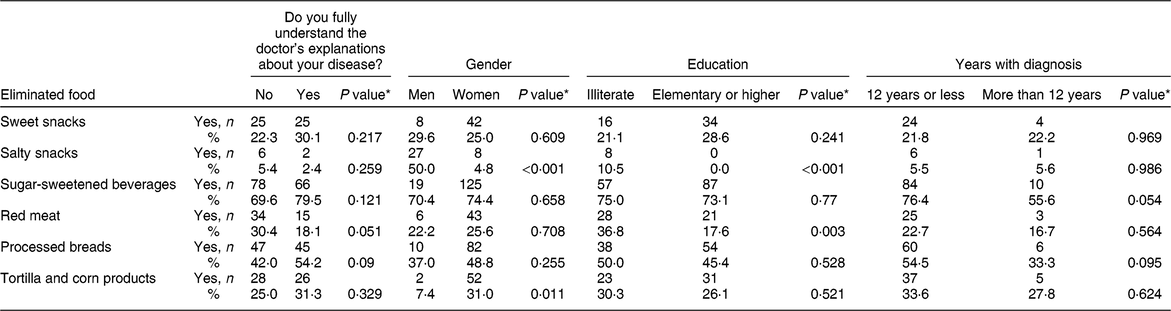
* Pearson’s χ 2 test.
Poverty-based food culture
Poverty, ethnicity/cultural identity and gender arose as important limitations for the interviewees to adhere to a diet regimen. In contradiction to the medical recommendation to consume fruits, vegetables, and white and lean meats and to restrict red meat, sugars, carbohydrates and fats, most participants depended on beans and corn as the main sources of daily nutrients. People referred to the doctor’s recommendations or restrictions as ‘dieting’. Most of the interviewees were self-sufficient in terms of food production. They produced their own food on small farms or in their gardens – a form of self-sufficiency described as ‘food for poor people’. They considered that medical dietary recommendations were feasible only with money to buy foods different from those they normally ate. Some said that to ‘follow the diet’ one had to ‘be rich’. The capacity to select and purchase specific foods and products to ‘follow the diet’ did not seem ‘achievable’. Also, most of them had their own interpretations regarding the origin of diabetes and the way to cure it, which contradicted the information received at health education sessions.
Diet adjustments in a socially vulnerable context
Questionnaire data show that Mayan people had difficulties reducing the consumption of certain foods such as fats, carbohydrates, red meat and sugary drinks (when recommended by their doctor). They reported difficulties cutting sweetened beverages (74 %), commercially processed bread (47 %), corn (28 %), sweet snacks (26 %) and red meat (25 %). Women reported greater difficulty in reducing the consumption of corn compared with men (31 v. 7 %, P = 0·011). Participants with less education had greater problems reducing red meat compared with those with higher education (37 v. 18 %, P = 0·003). The same pattern was observed for intake of salty snacks (11 and 0 %, respectively, P < 0·001). As for time from diabetes diagnosis, there was a borderline difference in the reduction of sugary beverages between those with time from diagnosis less than 12 years and those with time greater than 12 years (76 v. 56 %, P = 0·054, Table 5).
The qualitative interview data and the questionnaire provided evidence of three profiles of patients in terms of management of dietary restrictions: (i) those who strictly adhered to medical dietary recommendations; (ii) those who made some changes but allowed themselves some margin in their adherence to dietary changes; and (iii) those who did not follow the dietary recommendations at all (Table 6).
Table 6 Mayan people’s cultural adaptations to medical dietary recommendations, Chiapas, Quintana Roo and Yucatan, Mexico, 2008–2012
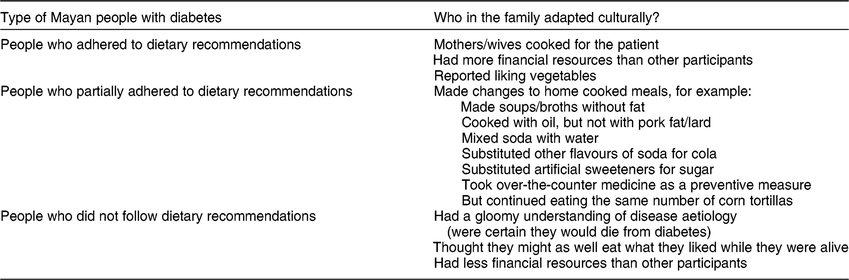
People who adhered to dietary recommendations
The majority of these people were male heads of household whose wives prepared diet foods and excluded unhealthy foods. Women fond of vegetables and young adults still living at parents’ home – and whose mother prepared the food – also fell into this category. In most of these cases, redefining food practices to adhere to recommendations was considered as beneficial to the entire family. Wives in families of more financial resources tended to prepare two meals: one for the person with diabetes and another for the rest of the family.
People who adhered to some dietary recommendations
These Mayan people did not adhere strictly to dietary recommendations as a strategy to make life tolerable and to protect themselves against the emotional suffering caused by dietary restrictions. The most common means of adaptation was to consume less sugar and use artificial sweeteners instead; others continued to drink sodas but mixed with water, and some others replaced colas with other flavours of soda (thinking that cola contains more sugar than other types of sodas due to its colour). Some participants continued to eat the same amount of corn but substituted handmade for store-bought tortillas (believing the former were ‘less fattening’), whereas others took non-prescription medications as a pre-meal prophylactic.
People who did not follow dietary recommendations at all
People who reported not making any doctor-recommended dietary changes considered the diet too restrictive. For example, they thought that ‘adhering to recommendations meant not eating at all or starving to death’. They mentioned the importance of eating and drinking the same things as before their diagnosis. Some justified eating particular foods and beverages that either were their favourites or were necessary to perform their daily activities. They were willing to ‘pay the price’ and in some cases even experienced diabetic complications. For other persons, not having any diabetes-related complications so far meant that their food practices were fine, so changing them was unnecessary.
The questionnaire data complemented the above qualitative descriptions. Over half (57 %) of the study participants reported not adhering to doctor-recommended diabetes treatment (including medication, diet or exercise). The two principal reasons were dislike of recommended foods (52·5 %) and high cost of foods (26·2 %, Table 2).
Discussion
The findings of the present study highlight the gap between biomedical modern culture and Mayan culture, which leads to low compliance with medical staff’s recommendations on the part of Mayans with diabetes because of lack of understanding and existence of issues related to the social construction of taste. In this respect, Bourdieu maintains that taste is socially and historically constructed and is tied to certain contexts such as social class (class-specific tastes) and poverty or economic disadvantage, in which case there is a ‘taste of necessity’( Reference Bourdieu 37 , Reference De Morais Sato, Gittelsohn and Fernandez Usain 38 ).
In addition, historians( Reference Warman 39 ) and anthropologists( Reference González Torres 40 , Reference Broda, Broda and Eshelman 41 ) have emphasized the central place that corn occupies in Mesoamerican indigenous cultures up to the present day. A fundamental part of socially constructed taste among Mayans is the symbolic importance assigned to corn. This, in combination with economic reasons, account in good part for the difficulty that Mayans have in reducing or excluding tortillas (made from corn) from their diet. In many cases, the foods or dietary restrictions proposed by the doctor do not correspond to the Mayans’ culturally constructed taste. Nevertheless, the social construction of taste is not monolithic, as shown by our finding of different profiles of more or less adherence to biomedical dietary (and other) recommendations among Mayans with diabetes.
Interrelationships between food practices, culture and social context
Our results show that although medical staff define adherence to treatment as an individual process, the ability to follow treatment was limited by poverty and by social and cultural characteristics of the Mayan patients interviewed in the present study. The historic and sociocultural context shapes gender roles in kinship interactions, including who is in charge of food preparation. This explains in part why men have an easier time adhering to dietary recommendations, because on the basis of prescribed gender roles women have to accommodate their dietary preferences and needs to those of all members of the family (diabetic and non-diabetic), whereas men usually have their meals prepared for them.
Another finding has to do with the struggle between socioculturally constructed taste for food and cultural values v. nutrition as defined by health-care guidelines and institutions, with dietary recommendations that seemingly value only macronutrients and energy: that is, a battle against fat and sugar. This trend among modern societies is called ‘lipofobia’, as Fischler points out( Reference Fischler 42 ), which implies a view of food consumption as an isolated practice. On the contrary, our findings confirm the observations of other authors that the experience of eating and food practices are both social and cultural activities, encompassing the social and family environment as well as community religious and cultural holidays( Reference Kemper and Long 43 ). Furthermore, another theme that emerged from Mayans’ narratives was the enjoyment of certain foods (restricted according to medical recommendations) and dislike of doctor-recommended foods, which was often seen as a valid justification for not adhering to treatment. In this regard, taste, defined as a set of preferences and aversions, is not an individual choice, but is developed instead through interactions with one’s social group of origin, as several authors have previously documented( Reference Bourdieu 37 , Reference Douglas and Hernandez 44 , Reference Goody 45 ). Also, the qualitative and quantitative data revealed that poverty as a contextual factor imposes practical and taste-related (‘taste of necessity’) barriers to adherence to dietary recommendations made by medical staff that are not culturally competent and do not take into account the extreme economic limitations of many Mayans with diabetes.
The political dimension of disease
Some authors agree that the increased consumption of processed foods and beverages with high fat, sodium and sugar content, coupled with the reduction of physical activity, has negatively impacted the health of the global population during the last century. Historically, international political events have played a role in transforming the availability of food, as discussed by Mintz in the case of the production, distribution and consumption of sugar, a product that was democratized and whose consumption increased as a result of the colonization process in the Americas( Reference Mintz 26 ).
In the case of Mayan people with diabetes, the social and environmental conditions in which they live hinder lifestyle changes to improve health. Any preventive health interventions compete with excessive media advertising promoting the consumption of beverages with high sugar content, of snacks with high salt and energy content, and of other foods with low nutrient density. The transnational companies that produce industrialized foods employ modern images and values as a dissemination strategy, selling the idea that modernity can be achieved through the consumption of their products( Reference Blanding 46 ). Moreover, these industrialized items with low nutritional value are widely distributed and are non-perishable, which make them highly available. All the above affects people’s food practices and is especially harmful in a context of scarce nutrient sources (i.e. individual and community poverty). Thus, asking people to change their eating habits without changing the obesogenic environment that surrounds them perpetuates the myth that keeping a disease in people’s ‘control’ depends solely on their willpower. This way of thinking transfers all responsibility to the individual, leaving out the political sphere of influence on food practices.
The importance of culture in health behaviours
The qualitative results of the present study point to cultural beliefs about the disease origin that do not align with medically defined causes. These beliefs reflect aspects of moral, emotional and natural–supernatural forces and the social violence of poverty and gender. For the interviewees, a proper treatment has more to do with their beliefs about the origin of the disease. In contrast, the medical perspective calls for changing and regulating food practices from an individualized logic that does not make sense within the explanatory framework or the socio-economic context of Mayans’ daily life.
The indigenous cultural horizon (including food habits), the ways of talking about diabetes and the meanings associated with the disease shaped the interviewees’ experience and understanding of disease care and management. Experiences of frustration because of food restrictions were also documented among Ikojts, another Mexican indigenous group( Reference Montesi 17 ).
Medical staff asked people to change their food habits without considering what food meant to some populations both symbolically and in practical terms (financial resources, time needed to prepare two meal options). These types of barriers have also been documented among First Nation youth in Canada and in indigenous populations in other countries( Reference Macaulay, Cargo, Bisset, Ferreira and Lang 18 , Reference Bennett 47 ).
Previous anthropological research on Mexican Mayans with diabetes explores how people explain diabetes and especially the central place of food in the causation of the disease( Reference Franck and Durden 12 – Reference Page-Pliego 14 ). Page-Pliego, for example, describes an array of explanatory models of diabetes, including biomedical understandings and traditional models that are based on Mayan traditions and cultural beliefs( Reference Page-Pliego 13 , Reference Page-Pliego 14 ). Some authors also note how the adoption of lifestyle changes recommended by medical staff, in particular diet, interacts with gender. For instance, similar to our data, these authors found that women with diabetes face greater barriers to diet change given their workload because of gender norms( Reference Franck and Durden 12 ).
This research also shows how poverty, cultural marginalization, and the processed food and sugary beverage industries converge in complex ways to contribute to the development of diabetes among indigenous peoples, including Mexican Mayans, and to create multiple barriers to the adoption of doctor-recommended dietary changes( Reference Franck and Durden 12 ). Page-Pliego specifically investigates the increased consumption of sugary beverages in culturally marginalized groups living in poverty, such as many Mexican Mayans, and its ties with taste but also with political and socio-economic processes that lead to easy availability of these drinks and make them socially desirable( Reference Page-Pliego 13 , Reference Théodore, Blanco-García and Juárez-Ramírez 48 ). Finally, other authors have found, as we did, that another contributing socio-economic process is the displacement of traditional foods (such as fish among indigenous groups in Tabasco, Mexico) by ultra-processed foods, the consumption of which we noted to be extremely common in our study populations( Reference Cruz-Sánchez, Tuñon-Pablos and Villaseñor-Farías 16 , Reference Montesi 17 ).
Strengths and limitations
Several epidemiological studies have shown the impact of diabetes in vulnerable populations and the consequences of health-care inequalities. Less research has delved into the way decisions on food occur in daily life and how they relate to adherence to diabetes treatment. This is the main strength of the present study.
Because the present study is mainly qualitative–ethnographic in nature, the evidence revealed by the data cannot be generalized to other contexts. We finished collecting data in 2012; however, the team continued working with indigenous people and diabetes, and we testified that those people still live today in the same conditions in their communities.
Conclusion
To date, the models of diabetes treatment have largely focused on lifestyle changes and adherence to medical recommendations, with diet having a central role. The main contributions of the present study are the need to recognize the cultural and socio-economic vulnerabilities of Mayans with diabetes; the need for medical staff to promote strategies of behaviour change according to the specific cultural, social (including gender) and economic context( Reference De Garine and Hernandez 22 , Reference Bennett 47 ); and the necessity of countering the influence of an obesogenic social environment. The qualitative and quantitative results support the centrality of both the sociocultural construction of taste and the explanatory models of health and disease (including disease origin) in people with diabetes, in this case, Mexican Mayans.
Acknowledgements
Acknowledgements: Thanks go to the people who participated in the research; to Jesús Lizama (Center for Research and Higher Studies in Social Anthropology (CIESAS)); and to Bonnie Campos and Ligia Sierra (Autonomous University of the State of Quintana Roo (UQROO)), collaborators who allowed us to use the infrastructure of their institutions for the research. Financial support: This work was supported by the National Council of Science and Technology of Mexico (grant number FOSSIS-87041). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript. Conflict of interest: The authors declared no competing interests with respect to the research, authorship and/or publication of this article. Authorship: Conceived and designed the experiments: C.J.-R. Performed the experiments: C.J.-R. Analysed the quantitative data: A.V., A.J.-C. Analysed the qualitative data: C.J.-R., F.L.T., S.L. Wrote the manuscript: C.J.-R., F.L.T., A.V., B.A.-L. Critically revised manuscript: G.N. Ethics of human subject participation: This study was conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving human subjects were approved by the committees of Research and Ethics of the National Institute of Public Health of Mexico (research protocol, instruments and consent procedure on 11 March 2009). The participants provided verbal informed consent.
Supplementary material
To view supplementary material for this article, please visit https://doi.org/10.1017/S1368980019001940








