The prevalence of obesity in the Australian population rose from 9% in 1989/90 to 15% in 20011. Sixty-five per cent of male and 45% of female adults were overweight or obese in 2001Reference Cameron, Welborn, Zimmet, Dunstan, Owen and Salmon2. Not only does obesity contribute to an estimated 5000 deaths each year in Australia, it also poses a major risk factor for chronic diseases including cardiovascular disease, stroke, type II diabetes mellitus, atherosclerosis, hypertension, gallbladder disease and some cancers3, Reference Bray4. Many of these diseases can often be treated and prevented through improvements in nutrition and/or increasing physical activity. Considering that general practitioners (GPs) in Australia have access to over 90% of the population in the course of a year5 and are viewed by the general public as being reliable and credible sources of nutrition informationReference Serra-Majem, Calvo, Male, Ribas and Lainez6, general practice is likely to be an ideal setting for health promotion.
Approximately 50% of visits to GPs are made by overweight or obese patientsReference Britt, Miller, Knox, Charles, Valenti and Pan7 and approximately 25% of all visits are nutrition-relatedReference Kolasa8. Consequently, GPs have many opportunities to offer nutrition advice. Studies have demonstrated that GPs can be effective in improving health behaviours such as increasing smoking cessation ratesReference Wilson, Wakefield, Steven, Rohrsheim, Esterman and Graham9, Reference Slama, Redman, Perkins, Reid and Sanson-Fisher10, reducing alcohol consumptionReference Wallace, Cutler and Haines11 and increasing physical activityReference Elley, Kerse, Arroll and Robinson12, Reference Campbell, Browne and Waters13. One study suggested that patients may be more likely to lose weight if prompted by their GPReference Colvin and Olson14. Nutrition advice has also proved to be effective when offered as part of a time-intensive interventionReference Laws15. However, as time is a major limitation for practitioners, nutrition/lifestyle information needs to be available in a condensed form that can be provided to patients during a standard consultation.
The Active Script Programme (ASP) is a brief and effective physical activity intervention used in general practice. Developed in 1999, the ASP is run by the Victorian Council on Fitness and General Health (VICFIT). The aim of this intervention is to increase the number of GPs who deliver brief, effective physical activity advice to inactive patientsReference Huang and Naccarella16. GP outcomes attributed to the ASP include improved competence in promoting physical activity; increased knowledge of the benefits of physical activity; and improvements in assessing, managing and counselling patients in relation to physical activity. The ASP has also resulted in an increase in knowledge and physical activity levels among patientsReference Huang and Naccarella16. However, VICFIT recognised that more effective lifestyle advice should include both nutrition and physical activity recommendations. VICFIT set up an advisory group who then developed specific nutrition advice to complement the physical activity advice in the ASP. This led to the development of the Active Nutrition Prescription (ANS), a brief ( < 5 min) nutrition and physical activity tool for use in general practice. The aim of the present study was to evaluate GPs' use of the ANS in general practice to prevent weight gain among the healthy to overweight population.
Methods
Development of the ANS
VICFIT convened a small expert working party with representatives from education, government and non-government organisations to provide content expertise in the development of the ANS. Over several meetings, the working party identified overall themes to be explored and finally developed five specific nutrition messages based on the most recent scientific evidence for the prevention of weight gain. The ANS was developed in the form of a paper-based script pad with a view to create an electronic version after the pilot study. Once the ANS script pad was developed and the target group was defined, input into further development of the tool was gathered from GPs, consumers and key stakeholders before the tool was pilot-tested in general practices.
Target group
The ANS was targeted at people with a body mass index (BMI) of between 23 and 30 kg m− 2, and was aimed at preventing weight gain and improving nutritional habits among this group. The ANS was not designed to result in weight loss in the short term, but had the potential to prevent weight gain in the long term. Therefore, it is not an appropriate treatment for obesity where weight loss is the goal. The working party recognised that the obese group would require more intensive treatment.
Nutrition messages
The nutrition messages developed were:
(1) Eat five servings of vegetables each day;
(2) Eat two servings of fruit each day;
(3) Drink water in place of sweetened soft drinks, cordial, sports drinks and fruit juice;
(4) Limit high-fat convenience and take-away foods to once per week; and
(5) If hungry, snack on fruit and vegetables between meals.
Script pad (ANS)
The ANS script pad included three sections: patient details, a physical activity component and a nutrition component. In the first section, the GP documented the patient's date of birth, sex, height, weight, and waist circumference. The second section was for physical activity prescription and includes type, levels and frequency of activity recommended. In the third section, the GP has the option to select any combination of the five nutrition messages they think are applicable to the patient. Each script could be personalised, with additional space for comments, an option to refer the patient to a dietitian, and a space to indicate a time for a review or to make a follow-up appointment. There was additional information that included examples of serving sizes, alternative snack options and other general nutrition advice.
GP pilot test
Recruitment and education
Some GPs were recruited by personal invitation at GP conferences and seminars; however, many were recruited via a divisional newsletter. Victorian Divisions were contacted and asked to place an advert in their regular newsletter requesting expressions of interest from GPs to participate in the pilot study of the ANS. Interested GPs who faxed back a response were sent a letter of invitation. Recruited GPs were asked to administer the prescription to 10 suitable patients over a 2-week period if full-time or a 4-week period if part-time, but were given more time if needed. Participating GPs were visited at their practices by an ANS representative and given a brief (approximately 15 min) education session in which they were shown how to use the script, given details about the target group and given the script pad. The script pad included 10 carbon copies that were collected for analysis post-intervention. A semi-structured telephone interview was administered by a research assistant within 7 days of the completion of the scripts. This phone interview lasted approximately 15 min and each GP was reimbursed $AUD 50 for his or her time.
Feedback form regarding patients
Each GP was asked to fill in a feedback form after writing each script. The GP was asked to note the initial reason for the visit, diagnosis, additional comments, and the reason for writing the script. The latter was indicated by ticking one or more options, consisting of weight reduction, weight maintenance, poor nutrition knowledge, poor nutrition/activity habits, patient requested the advice, patient not active, chronic disease or to motivate the patient.
Materials provided to the GP
Each GP was supplied with one script pad of 10 scripts with carbon copies, 10 feedback forms (regarding patients), a GP information sheet, and six to 10 physical activity patient questionnaires, which included a physical activity scoring sheet. The physical activity patient questionnaire and scoring sheet were used to briefly assess physical activity level. These physical activity patient questionnaires were provided but were not compulsory to complete (data not collected). The GP information sheet included information on the target group; evidence supporting the nutrition messages; a list of resources; details on physical activity assessment; how to measure waist circumference and BMI; and risk of disease at different levels of waist circumference and BMI categories. GPs were also provided with 10 orange cards with details of VICFIT's Physical Activity Infoline number to be given to recipients of the script at the GP's discretion.
Results
GP characteristics
Of the 32 GPs who expressed interest in participating in the pilot study, 25 were trained in how to apply the ANS and 19 completed or partially completed the required number of scripts (63% female). Reasons given by the GPs for not participating once trained included a lack of time, being away on holidays, forgetting to participate and believing that participation in the study was too difficult.
Patient characteristics
Active Nutrition Scripts were written for 145 patients, with a median of nine scripts written per GP. Of the patients whose gender was recorded (83%), 69% were female. The mean ( ± standard deviation) waist circumference of the patients was 105.9 ± 11.9 cm for males and 98.4 ± 15.5 cm for females. Mean BMI was in the obese range (Table 1). Forty-three per cent of patients were in the target group (i.e. BMI of between 23 and 30 kg m− 2) and 52% were obese.
Table 1 Patient characteristics
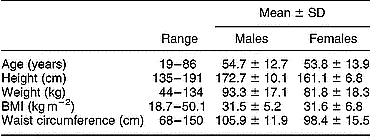
SD – standard deviation; BMI – body mass index.
Physical activity prescription
GPs prescribed physical activity to 97% of ANS recipients. GPs prescribed walking to the majority of patients (61%), with gym exercises being the next most frequently prescribed activity (4%) for the recipients. Twenty-five per cent received exercise prescription without a suggestion for a specific activity. Thirty minutes of daily activity was prescribed to 69% of patients. GPs prescribed 65% of patients to exercise 5–7 times per week, 19% to exercise 4–5 times per week and 8% to exercise 1–2 times per week (data were missing for 8% of the prescriptions).
Nutrition prescription
GPs ticked all five nutrition boxes for 55% of recipients. GPs did not offer nutrition advice for 3% of the recipients (i.e. these recipients only received physical activity prescription). More than 80% of all patients received advice to consume two servings of fruit each day, five servings of vegetables each day and to drink water in place of sweet drinks (Table 2). GPs ticked the box ‘drink water in place of sweetened soft drinks, cordial, sports drinks and fruit juice’ more frequently for overweight/obese (BMI >25 kg m− 2) patients than they did for patients in the healthy weight range (BMI ≤ 25 kg m− 2) (Table 3). GPs ticked the water and take-away messages more frequently for patients under the age of 50 years than they did for those over the age of 50 (Table 3).
Table 2 Percentage each nutrition advice/message box was ticked in relation to gender

* Gender was recorded in 83% of patients.
Table 3 Percentage each nutrition message box was ticked in relation to BMI and age categories

* Pearson chi-square test.
Referral to a dietitian/review/full assessment
Sixteen patients (11%) were referred to a dietitian, 106 (73%) were asked to make a follow-up appointment (review) and 17 (12%) were asked to make an appointment for a full dietary, physical activity and social assessment with the GP so that a more thorough weight management plan could be developed at a future date. Of the 73% of patients who received a recommendation for a review, the median months for the review was 2 months for males and 1 month for females. The patients who did not receive a recommendation for a review were less likely to be referred to a dietitian (P = 0.048), less likely to be asked to make an appointment for a full assessment (P = 0.006), were older (P = 0.019), had a lower BMI (P = 0.005) and were less likely to be asked to increase their vegetable intake to at least five servings per day (P = 0.009).
Feedback form – reported reasons for GP visit, diagnoses and administration of the script
Patient information was available for 95% of patients who received an ANS prescription. The main reasons for the GP visit, as recorded by the GP, included a blood pressure check (22%), a general check-up (18%), a session addressing weight concerns (16%), obtaining a repeat script (10%) and a cholesterol check (9%). The diagnoses included overweight (43%), hypertension (26%), lipid disorders (19%), diabetes (11%) and others (9%). Encouraging weight reduction was the main reason given by GPs for writing the script (78%), followed by efforts to motivate the patient (48%), reduce inactivity (30%), address poor nutrition or activity habits (23%) and reduce chronic disease (19%).
GP interview
Seventeen of the 19 participating GPs were interviewed (90%) following completion of the scripts. The mean number of years in practice was 23 (range: 3–40 years), with a mean of 99 patients seen each week (range: 20–200). Ten GPs worked part-time. The time reported for delivering the script was approximately 4.9 min per script. All interviewed GPs indicated that the messages were clear and simple to deliver, and would have liked to continue using the script post-pilot. Forty-seven per cent stated that they would be more likely to initiate a nutrition or physical activity discussion with their patients in the future and 29% reported that they were now more likely to routinely ask new patients about nutrition and physical activity.
Discussion
This study explored GPs' use of a brief nutrition and exercise prescription (ANS) that was developed to complement an existing exercise prescription intervention for a more integrated lifestyle resource for GPs. Although GPs were instructed to administer the ANS to the healthy and/or overweight population, more than half of the patients who received the ANS were obese. However, the obese population is likely to require more intensive interventions and the ANS alone is unlikely to be effective in reducing weight among this group.
There are a number of possible reasons why GPs administered the ANS to obese patients rather than the target group consisting of healthy and/or overweight patients. First, GPs may be keener to use the ANS with the obese population as this group may be viewed to be in greater need of an intervention than healthy/overweight persons. This supports findings that GPs prefer to use nutrition intervention for treatment rather than health promotionReference Lawlor, Keen and Neal17, Reference Laws18. GPs choosing to intervene more often for obese patients than for overweight patients has occurred previouslyReference Laws18–Reference Silagy, Muir, Coulter, Thorogood, Yudkin and Roe20.
Second, the increasing percentage of obese and overweight persons in the population may make it difficult to distinguish overweight people from obese people. Low levels of obesity identification have occurred in previous studiesReference Laws18, Reference O'Brien, Holubkov and Reis21–Reference Stafford, Farhat, Misra and Schoenfeld24. GPs may find it difficult to distinguish between those who are overweight and those who are obese, if BMI is not calculated. GPs were asked to record height and weight on the ANS, and were recommended to calculate BMI. As there were no data to indicate whether BMI was calculated, it could be that GPs were unaware of the BMI of their patients and made an assessment of their BMI visually.
Third, GPs may have seen a need to assist their obese patients with weight management but had few options available to them and, thus, perceived the ANS as an appropriate substitute.
There is a need for nutrition interventions to be brief; however, they also need to be effective for patients. Practitioners in The Eating Patterns Study provided a self-help nutrition education booklet along with a motivational message to patients in less than 3 minReference Beresford, Curry, Kristal, Lazovich, Feng and Wagner25. Although both the control and intervention groups reduced their fat intake, the changes were significantly larger for the intervention group at the 3- and 12-month follow-ups. Another brief nutrition education tool, the Patient Information Letters (PIL) developed by the Dutch College of General PractitionersReference van Binsbergen and Drenthen26, provided nutrition advice on selected diagnoses. Only 5% of physicians reported using the letters sufficiently, with 63% agreeing that they did not use them enough. The main barriers to using the PIL included not thinking of it at the right moment, not knowing the content well enough and finding it too time-consumingReference van Binsbergen and Drenthen26.
Although some GPs feel that they can be effective in nutrition intervention and agree that nutrition is important in managing diseaseReference Morris, Lean, Hankey and Hunter27, they generally lack confidence in offering more detailed nutrition advice due to insufficient knowledge, which is a result of gaps in nutrition training throughout undergraduate and postgraduate studies. Other barriers to offering nutrition advice include time constraints, a lack of incentives or reimbursements, inadequate support materials, complex advice to offer, lack of training in counselling skills, and a long delay between intervention and observable effectsReference van Binsbergen and Drenthen26, Reference Kushner28. Where interventions were designed specifically for weight reduction, some studies have revealed that GPs felt their influence on weight reduction was limited compared with other professionalsReference Morris, Lean, Hankey and Hunter27, Reference Fogelman, Vinker, Lachter, Biderman, Itzhak and Kitai29. However, other studies have found that GPs rated themselves as ‘quite effective’ in influencing patients' dietsReference Paxton and Tighe30 and influencing patients to lose weightReference Kristeller and Hoerr19.
Many studies designed for weight-loss purposes are often more time-intensive than the current study and have included detailed dietary assessments, weight management plansReference Moore, Summerbell, Greenwood, Tovey, Griffiths and Henderson31, multiple GP training sessions and frequent patient visitsReference Laws15, Reference Laws18. For example, the Counterweight Programme in the UKReference Laws15, Reference Laws18 included lifestyle advice offered either individually or as part of a group on frequent occasions (six 10–30 min appointments over 3 months for the individual sessions or six 1 h group sessions), with quarterly follow-ups recommended. In the Counterweight Programme, 34% of patients lost 5% or more of their initial weight in 12 months. Although the programme was effective, it was time-intensive and may be difficult to apply permanently within a general practice setting.
Cost-effective health promotion delivery methods during consultation might include the use of other allied health personnel. For example, it may be more reasonable for practice nurses (PNs) to run such health promotion programmes for population health outcomes, particularly to minimise any time concerns of the GP. On average, GP consultation time is 14.6 min per patient (median 12 min)Reference Sayer, Britt and Horn32, which does not allow much room for lifestyle intervention. In the Counterweight Programme, only 15% of GPs reported spending up to 10 min of the consultation discussing weight, compared with 76% of PNsReference Laws15, Reference Laws18. A survey conducted by Steptoe et al.Reference Steptoe, Doherty, Kendrick, Rink and Hilton33 on 107 GPs and 58 PNs in the UK revealed the majority of GPs and PNs agreed that it was most appropriate for PNs to deliver health promotion advice to their patients. The majority of PNs also stated they had the time for preventive medicine, as opposed to only 30% of GPs. Although utilising PNs for health promotion in general practice would remove some of the time constraints placed on GPs, few studies have assessed patient attitudes and consequent behaviour change towards receiving advice from a PN as opposed to a GP. Moreover, less than half of all practices in Australia employ PNs or health professionals other than GPs.
Along with barriers that can be overcome, such as a lack of knowledge and limited available resourcesReference Lazarus34, Reference Maiburg, Rethans, Schuwirth, Mathus-Vliegen and van Ree35, other barriers including time constraints and a lack of reimbursement may limit GPs' ability to offer detailed lifestyle assessments and provide individualised weight management plans on a frequent basis. If time constraints cannot be easily altered and increasing reimbursement to GPs is found to be too expensive, it may be more realistic that lifestyle advice is provided by nurses or allied health personnel. GP practice has traditionally been treatment-focused, which is likely to be a further barrier preventing GPs from participating in health promotion activities.
Less time-intensive interventions such as the ANS are likely to be adopted more readily by GPs due to their simplicity and usability within a usual consultation; however, the effectiveness of such brief interventions in general practice needs to be evaluated further. The ANS pilot study assessed the acceptability of the ANS for GPs. No information was collected on the effectiveness of the ANS for the patients in terms of increasing physical activity and/or improving eating behaviours, and this must be assessed before this programme can be implemented on a population level.
Limitations
One of the limitations of this study was the limited number of GP participants. Participating GPs were more likely to be interested in nutrition than the general GP population. There was also a high rate of incomplete or incorrectly filled out scripts. For example, some patients received exercise prescription without any specific activity to partake in. Gender and waist circumference data were missing for 17% and 23% of patients, respectively. Finally, GPs generally took 3–6 weeks to write nine scripts. This figure has the potential to be higher considering that about half of all GP visits are made by overweight or obese personsReference Britt, Miller, Knox, Charles, Valenti and Pan7 and the GPs in this study saw about 100 patients per week. However, the newness of the ANS and the brief training may have contributed to this low number, along with the traditional barriers towards utilising health promotion in the general practice setting.
Conclusions and recommendations
GPs found the ANS messages and process to be acceptable in the clinical setting. GPs administered the script to obese patients for the purpose of weight loss despite being instructed to administer the script to healthy and overweight patients to prevent weight gain. GPs may not have been aware of who was obese as BMI was not necessarily recorded and documented. In addition, GPs may have been resistant to initiate preventive health messages as their traditional role is related to treatment delivery. Future research needs to identify barriers to GP attitudes and behaviour towards using health promotion interventions with lower-risk groups. Additionally, an assessment is needed on whether other health practitioners can provide effective lifestyle advice, with the support of GPs, resulting in patient behaviour change.
Increasing awareness and identification of obesity should be a priority for public health policy. An option includes advising GPs to calculate BMI for all patients to assist with overweight and obesity identification. Education on the benefits of health promotion should also be implemented. To improve BMI identification for the ANS, BMI could be calculated by the GP and recorded on the script. Utilising other allied health staff, where possible, could alleviate some time constraints. Referral options for obese patients also need to be identified. Finally, tools such as the ANS need to be integrated into the practice systems and processes to improve uptake. Process barriers within the practice need to be assessed by identifying support available and resources needed.
If the ANS was to be implemented more widely, it would be important to develop a method that could determine the effect of the ANS at the patient level and to gain patients' input and opinions towards receiving the ANS. The GP education session may also need to be revised to educate and support GPs in using the ANS on the target population and to further educate GPs in correctly and completely filling in the script.
Preventing weight gain is important in tackling the obesity epidemic that faces the world today. Nations, particularly Australia, the UK and the USA, are becoming more and more overweight. The average weight has increased significantly over the past decade; therefore, an intervention designed to prevent weight gain is clearly beneficial. A brief tool such as the ANS has the potential to contribute towards this goal as it can be implemented by GPs within a normal consultation time.
Acknowledgements
The researchers gratefully acknowledge the contribution of Ms Veronica Graham, Public Health Nutritionist for the Department of Human Services Victoria; the Bendigo & District Division of General Practice consumer group and staff; and participating GPs. The following key stakeholders are also acknowledged: Dietitians Association Australia, Diabetes Australia, National Heart Foundation, SIGNAL, Nutrition Australia, General Practice Divisions Victoria, The Commonwealth Department of Health and Ageing, Department of Human Services Victoria, International Diabetes Institute, The Cancer Council Victoria, Jean Hailes Foundation, Professor Boyd Swinburn and Associate Professor Gary Eggar. This work was supported by the Commonwealth Department of Health and Ageing and VICFIT Incorporated.





