Crossref Citations
This article has been cited by the following publications. This list is generated based on data provided by
Crossref.
Kaleli-Can, Gizem
Hortaç-İştar, Elvan
Ferda Özgüzar, Hatice
Mutlu, Mehmet
Mirza, Hasan Cenk
Başustaoğlu, Ahmet
and
Göçmen, Julide Sedef
2020.
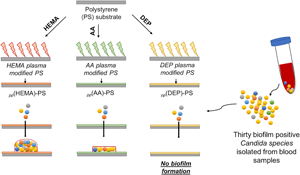
Erratum: Prevention of Candida biofilm formation over polystyrene by plasma polymerization technique–CORRIGENDUM.
MRS Communications,
Vol. 10,
Issue. 4,
p.
704.
Özgüzar, Hatice Ferda
Meydan, Ahmet Ersin
Göçmen, Jülide Sedef
and
Mutlu, Mehmet
2021.
Single-step amphoteric surface modification through plasma polymerization: Antifouling coating for titanium substrate.
MRS Communications,
Vol. 11,
Issue. 4,
p.
523.
Yang, Kai‐Hung
Riley, Parand
Rodenhausen, Keith B.
Skoog, Shelby A.
Stafslien, Shane J.
Vanderwal, Lyndsi
and
Narayan, Roger J.
2022.
Antifungal behavior of silicon‐incorporated diamond‐like carbon by tuning surface hydrophobicity with plasma treatment.
International Journal of Applied Ceramic Technology,
Kim, Ji Hyeon
Ahn, Hyunwoo
Lee, Daehyeop
Lee, Hyunjun
and
Kim, Wang June
2023.
Antibiofilm activity of crude bacteriocin JM01 produced by Pediococcus acidilactici against methicillin‐resistant Staphylococcus aureus (MRSA).
International Journal of Food Science & Technology,
Vol. 58,
Issue. 5,
p.
2580.
Umur, Egemen
Arslan, Fahriye
Bakay, Emel
Sirek, Busra
Ayan, Bugra
Baysoy, Engin
Topaloğlu, Nermin
and
Kaleli-Can, Gizem
2024.
Layer-by-layer assembled melanin nanoparticles thin films for photodynamic activity-based disinfection by ultraviolet A irradiation.
Emergent Materials,
Vol. 7,
Issue. 6,
p.
2547.