Prolactin is a polypeptide hormone secreted by the lactotroph cells of the anterior pituitary gland. It is responsible primarily for breast enlargement in pregnancy and subsequent milk production. Dopamine is the primary inhibitor of prolactin release, and it is produced in the hypothalamus by the tuberoinfundibular neurons, then transported to the pituitary gland via the hypophyseal portal circulation. Dopamine receptor antagonists such as antipsychotics cause hyperprolactinaemia by reducing inhibition of prolactin secretion.
Since prolactin inhibits the release of gonadotrophin-releasing hormone, hyperprolactinaemia can indirectly lead to decreased oestrogen levels in women and decreased testosterone levels in men (Reference Haddad and WieckHaddad 2004).
Macroprolactin is a prolactin immunoglobulin complex with lower biological activity than prolactin. Some laboratories do not routinely measure macroprolactin, but those that do do not always show its contribution to the total prolactin reading. Clinicians should therefore always check whether reported total prolactin includes a macroprolactin component, especially in patients with asymptomatic hyperprolactinaemia. This can avoid unnecessary further investigation (Reference Melmed, Casanueva and HoffmanMelmed 2011).
Prolactin is secreted in a pulsatile manner, typically peaking in the middle of the night and reaching a trough level after midday. The physiological peak can be four times greater than the trough (Reference Haddad and WieckHaddad 2004). The normal range of serum prolactin is generally below 530 mIU/L (25 ng/mL) in women and 424 mIU/L (20 ng/mL) in men (Reference Peveler, Branford and CitromePeveler 2008).
Symptoms of hyperprolactinaemia
The primary symptoms of hyperprolactinaemia are galactorrhoea, menstrual disturbance, infertility, decreased libido and gynaecomastia. Psychiatrists may fail to detect these symptoms either because they do not ask about them directly, or because patients are embarrassed to mention them or do not think them a medication side-effect (Reference Haddad and WieckHaddad 2004).
Causes of hyperprolactinaemia
Physiological causes of hyperprolactinaemia include pregnancy, lactation, stress, sexual inter course and sleep. There are a large number of pathological causes, including prolactinoma (usually associated with extremely elevated prolactin levels), chronic renal failure, liver cirrhosis, trauma and seizures. Non-functioning pituitary tumours can cause pituitary stalk compression and mild hyperprolactinaemia. Importantly, therefore, mild hyperprolactinaemia does not rule out a pituitary mass lesion (Reference Melmed, Casanueva and HoffmanMelmed 2011).
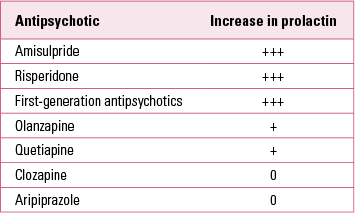
Many medications can raise prolactin, particularly antipsychotics, but also antidepressants, oral oestrogens, oral contraceptives and opioids. Hyper prolactinaemia is particularly associated with amisulpride, risperidone and first-generation antipsychotics (Table 1). Nearly all antidepressants are associated with hyperprolactinaemia, though to a much lesser extent than antipsychotics. Clomipramine is the antidepressant most associated with hyperprolactinaemia (Reference MolitchMolitch 2008). Routine monitoring of prolactin when prescribing antidepressants is not recommended (Reference Coker and TaylorCoker 2010).
TABLE 1 Effects of antipsychotics on prolactin levels
Long-term consequences of hyperprolactinaemia
Hyperprolactinaemia is associated with loss of bone mineral density as a consequence of sex hormone deficiency (Reference Haddad and WieckHaddad 2004). Even a few months of mild hyperprolactinaemia with amenorrhoea may affect bone mineral density (Reference Peveler, Branford and CitromePeveler 2008).
Data suggest that prolactin has an important role in the development of some breast cancers (Reference Tworoger, Eliassen and SlussTworoger 2007, Reference Tworoger, Eliassen and Zhang2013) and prolactin elevation should be avoided where there is a history of breast cancer (Reference Peveler, Branford and CitromePeveler 2008).
Clinical management of patients on antipsychotics
Psychiatrists should inform patients about the symptoms of hyperprolactinaemia and enquire about these periodically. There is no consensus in various clinical guidelines about routine measurement of serum prolactin. Obtaining a baseline prolactin reading is strongly advised when commencing an antipsychotic associated with hyperprolactinaemia. Additionally, it appears prudent to measure serum prolactin 3 months after dose stabilisation and 3 months after any dose increase (Reference Peveler, Branford and CitromePeveler 2008).
In the presence of a recent normal baseline prolactin level, hyperprolactinaemia following initiation of an antipsychotic is almost certainly medication induced. If confirmation of this is required, clinicians might consider discontinuing an oral antipsychotic as a trial for 3 days, by which time a drug-induced hyperprolactinaemia will usually normalise (Reference Melmed, Casanueva and HoffmanMelmed 2011); this approach might not be feasible because of the risk of relapse.
The following management strategies may also be considered:
-
review the need for ongoing antipsychotic medication; if appropriate, the antipsychotic might be discontinued permanently
-
reduce the dose of antipsychotic (Reference Haddad and WieckHaddad 2004)
-
change the antipsychotic to one with a lower risk of hyperprolactinaemia (Reference Melmed, Casanueva and HoffmanMelmed 2011).
If hyperprolactinaemia above 1000 mIU/L persists and aetiology is unclear, it may be necessary to discuss with an endocrinologist and consider other investigations, including liver, renal and thyroid function tests. In some cases, magnetic resonance imaging (MRI) of the hypothalamus and pituitary to exclude a mass lesion might be considered. A history of headaches or visual field disturbance raises the suspicion of a pituitary tumour.
When it is necessary to continue the antipsychotic in the presence of hyperprolactinaemia, the following could be considered, after consultation with an endocrinologist:
-
adding oestrogen or testosterone for patients with long-term hypogonadism (hypogonadal symptoms or low bone mass) associated with hyperprolactinaemia (Reference Melmed, Casanueva and HoffmanMelmed 2011)
-
bone mineral density measurement for women with hyperprolactinaemia and 12 months of amenorrhoea (Reference Haddad and WieckHaddad 2004)
-
adding aripiprazole as an adjunct to the existing antipsychotic, which may normalise antipsychotic-induced hyperprolactinaemia (Reference Shim, Shin and KellyShim 2007)
-
adding a dopamine agonist such as bromocriptine or cabergoline, as this can normalise the prolactin level; this strategy carries a risk of exacerbating a psychosis (Reference Chang, Chen and LuChang 2008; Reference MolitchMolitch 2008).
Conclusions
Antipsychotic-induced hyperprolactinaemia is a common and overlooked problem with potential long-term consequences. This overview offers some guidance on management, but difficult clinical judgements may still be required. Careful prolactin monitoring, including a baseline result for all patients receiving prolactin-raising antipsychotics, should be considered just as important as pre-lithium renal and thyroid function tests.




eLetters
No eLetters have been published for this article.