Childhood obesity is associated with considerable adverse physical, psychosocial and economical outcomes, both in the short term and the long term (Freedman, Khan, Dietz, Srinivasan, & Berenson, Reference Freedman, Khan, Dietz, Srinivasan and Berenson2001). Indeed, obesity is a serious medical disorder potentially leading to a number of comorbidities (e.g., cardiovascular diseases, diabetes, skeletal problems) and has a severe impact on the overall quality of life (Dixon, Reference Dixon2010). The most prominent consequence of childhood obesity seems to be the significantly increased risk of remaining obese into adulthood. In children aged between 10 and 15 years, up to 80% of the obese children remained obese by age 25 (Whitaker, Wright, Pepe, Seidel, & Dietz, Reference Whitaker, Wright, Pepe, Seidel and Dietz1997). Similar evidence emerged from a meta-analysis that included 25 longitudinal studies from around the world: all studies reported a moderate persistence of childhood overweight into adulthood (Singh, Mulder, Twisk, van Mechelen, & Chinapaw, Reference Singh, Mulder, Twisk, van Mechelen and Chinapaw2008). The finding that childhood obesity is not a transient developmental phenomenon is alarming given the association between adult obesity and several morbidities, and given the fact that extremely obese children may suffer cumulative effects of their ‘pound-years’ (Xanathakos & Inge, Reference Xanthakos and Inge2007). Statistical and clinically meaningful weight loss can be achieved with behavioural lifestyle interventions (multidisciplinary obesity treatments; MOTs) focusing on diet, exercise and psychological techniques, including parental involvement (Braet, Tanghe, Decaluwé, Moens, & Rosseel, Reference Braet, Tanghe, Decaluwé, Moens and Rosseel2004; Ho et al., Reference Ho, Garnett, Baur, Burrows, Stewart, Neve and Collins2013; Luttikhuis et al., Reference Luttikhuis, Baur, Jansen, Shrewsbury, O'Malley, Stolk and Summerbell2009). However, those who successfully lost weight after MOT often regained weight when treatment was terminated (Braet, Reference Braet2006; Moens, Braet, & Van Winckel, Reference Moens, Braet and Van Winckel2010).
One explanation for the modest results of existing treatments is the decreased self-regulatory capacities of obese individuals (Smith, Hay, Campbell, & Trollor, Reference Smith, Hay, Campbell and Trollor2011). In several studies, compared to non-overweight children and despite similar IQ, age and social status, overweight children tended more often to disregard long-term goals and take the immediately available smaller reward (Graziano, Calkins, & Keane, Reference Graziano, Calkins and Keane2010; Nederkoorn, Braet, Van Eijs, Tanghe, & Jansen, Reference Nederkoorn, Braet, Van Eijs, Tanghe and Jansen2006; Seeyave et al., Reference Seeyave, Coleman, Appugliese, Corwyn, Bradley, Davidson, Kaciroti and Lumeng2009; Verbeken, Braet, Claus, Nederkoorn, & Oosterlaan, Reference Verbeken, Braet, Claus, Nederkoorn and Oosterlaan2009; Verbeken, Braet, Bosmans, & Goossens, Reference Verbeken, Braet, Bosmans and Goossens2014). In other words, they lack the skills to successfully resist temptation of the currently ever-present, calorie-rich food stimuli that automatically capture attention (Freijy, Mullan, & Sharpe, Reference Freijy, Mullan and Sharpe2014; Kemps, Tiggemann, & Hollitt, Reference Kemps, Tiggemann and Hollitt2014; Loeber et al., Reference Loeber, Grosshans, Korucuoglu, Vollmert, Vollstadt-Klein, Schneider and Kiefer2012; Mann & Ward, Reference Mann and Ward2004) and drive action tendencies to approach and eat palatable food (Brignell, Griffiths, Bradley, & Mogg, Reference Brignell, Griffiths, Bradley and Mogg2009; Kemps & Tiggemann, Reference Kemps and Tiggemann2015; Kemps, Tiggemann, Martin, & Elliott, Reference Kemps, Tiggemann, Martin and Elliott2013).
The assumption that in obese individuals overeating is triggered by exaggerated reactivity to stimuli associated with high-caloric food is supported by neuro-imaging research: compared to average weight controls, in obese individuals, a greater activation to high-caloric food images was found within a wide range of brain regions mediating motivational and attentional salience of food cues (Stoeckel et al., Reference Stoeckel, Weller, Cook, Twieg, Knowlton and Cox2008; Yokum, Ng, & Stice, Reference Yokum, Ng and Stice2011). Furthermore, increased brain activation to high-calorie food pictures in obese individuals predicted less weight loss during therapy and poorer weight-loss maintenance posttreatment (Murdaugh, Cox, Cook, & Weller, Reference Murdaugh, Cox, Cook and Weller2012). Consequently, previous findings suggest that a high attentional bias for food cues is detrimental to weight control among obese individuals and that obesity treatment programs could benefit from approaches that target brain regions involved in attentional reactivity. As suggested by dual process models of behaviour regulation, obese children have both strong attentional bottom-up reactivity and a decreased top-down ability to inhibit the automatic impulses (Appelhans, Reference Appelhans2009; Strack & Deutch, Reference Strack and Deutch2004), leaving them at highest risk to become the plaything of environmental stimuli. Indeed, Guerrieri, Nederkoorn, and Jansen (Reference Guerrieri, Nederkoorn and Jansen2008) argue that focusing on inhibitory control alone will not be enough, without taking into account also attentional bottom-up processes. This is also in line with the view of Rollins, Dearing, and Epstein (Reference Rollins, Dearing and Epstein2010) that bottom-up processes may be a more powerful independent predictor of food intake than the ability to inhibit.
Although MOTs already focus on improving impulse control by means of learning self-regulation skills (Braet et al., Reference Braet, Tanghe, Decaluwé, Moens and Rosseel2004; Duffy & Spence, Reference Duffy and Spence1993), these vital skills seem hard to implement in daily life and are not very effective in the long term as children often relapse. It seems likely that, as long the supposed underlying core neurocognitive processes of poor impulse control are not modified, the acquired self-control skills remain of limited capacity. To reduce biased bottom-up processes, a number of cognitive bias modification (CBM) techniques were developed, aimed specifically at altering automatic, impulsive reactions to disorder-related cues (Koster, Fox, & Macleod, Reference Koster, Fox and MacLeod2009). In the domain of eating behaviour, several studies using adult samples suggest that CBM training may be effective for sustained weight loss (Kakoschke, Kemps, & Tiggemann, Reference Kakoschke, Kemps and Tiggemannn2014; Kemps, Tiggemann, & Hollitt, Reference Kemps and Tiggemann2015; Kemps, Tiggemann, Orr, & Grear, Reference Kemps, Tiggemann, Orr and Grear2014; Werthmann, Field, Roefs, Nederkoorn, & Jansen, Reference Werthmann, Field, Roefs, Nederkoorn and Jansen2014). One study with obese children participating in an attention modification program (AMP) or control program (CC; Boutelle, Kuckertz, Carlson, & Amir, Reference Boutelle, Kuckertz, Carlson and Amir2014) showed that in a free access session, children in the CC condition significantly increased their caloric intake over time whereas children in the AMP group demonstrated decreased caloric intake, providing evidence for the effects of such a training on eating behaviour also in younger age groups. Further, a recent pilot study with obese children and adolescents (8–16 years) (Warschburger, Gmeiner, Morawietz, & Rinck) showed that approach-avoidance tendencies are trainable in this age group and that the training was well accepted.
As with any form of training, motivation to train plays an important role in reaching a positive treatment outcome, particularly when attempting to treat children and adolescents. Additionally, CBM tasks are often experienced as fairly boring, due to their repetitive nature (Beard & Weisberg, Reference Beard and Weisberg2012). The use of game elements to improve motivation to train may help with this problem (Gladwin, Figner, Crone, & Wiers, Reference Gladwin, Figner, Crone and Wiers2011). While the use of game elements in the field of CBM is still very limited (Boendermaker, Prins, & Wiers, Reference Boendermaker, Prins and Wiers2015), evidence from the field of executive function training showed promising evidence for the efficacy of a gamified EF-training as a weight stabilisation intervention in obese children (Verbeken, Braet, Goossens, & van der Oord, Reference Verbeken, Braet, Goossens and van der Oord2013).
As such, the purpose of this pilot treatment study was to evaluate the feasibility and effectiveness of a novel CBM game training aimed at obese children above the care-as-usual of an intensive 10-month inpatient treatment program. Obese children were randomised to either the CBM training group or a control group provided with equal screen time but without food-related training elements (Tetris; www.TheTetrisGame.com). The CBM training aimed to reduce maladaptive cognitive biases by training both avoidance movements in response to high-caloric food pictures and approach movements in response to low-caloric food pictures. Primary outcome was weight loss maintenance at follow-up, three months after leaving the clinic. The training sessions were performed in the final months of the treatment program. In this way, after the end of the inpatient treatment program, confrontation with the daily food environment at home enabled us to study the long-term effects of a treatment in the natural environment, which is characterised by a high risk of relapse. Training prior to treatment could be useful in outpatient programs but not for inpatient programs, as during the 10-month program, no exposure to high caloric food is possible. We expected that the CBM training would reduce approach bias and craving for unhealthy high caloric food and that these changes would be highly needed when returning home and consequently be associated with better weight loss maintenance at follow-up.
Methods and Procedure
Participants
The participants were obese children attending a 10-month inpatient obesity treatment program in a medical paediatric centre. Inclusion criteria for entering the treatment centre were: primary obesity, age between 10 and 15 years, IQ within the normal range as measured with the Raven Progressive Matrices (RPM; Raven, Reference Raven1938), and absence of pervasive developmental disorders. Patients entered the clinic and started the obesity program in September. In February 2013, all 44 children entering the final phase of the obesity treatment program and their parents received an information letter about the research project in which they were invited to participate in month 8 of the treatment (see flow-chart in Figure 1). Forty children and their parents gave written consent (age M = 12.58 years, SD = 1.43; boys: 47.5%). Three children and/or their parents declined to participate and one child dropped out of therapy before the study started.
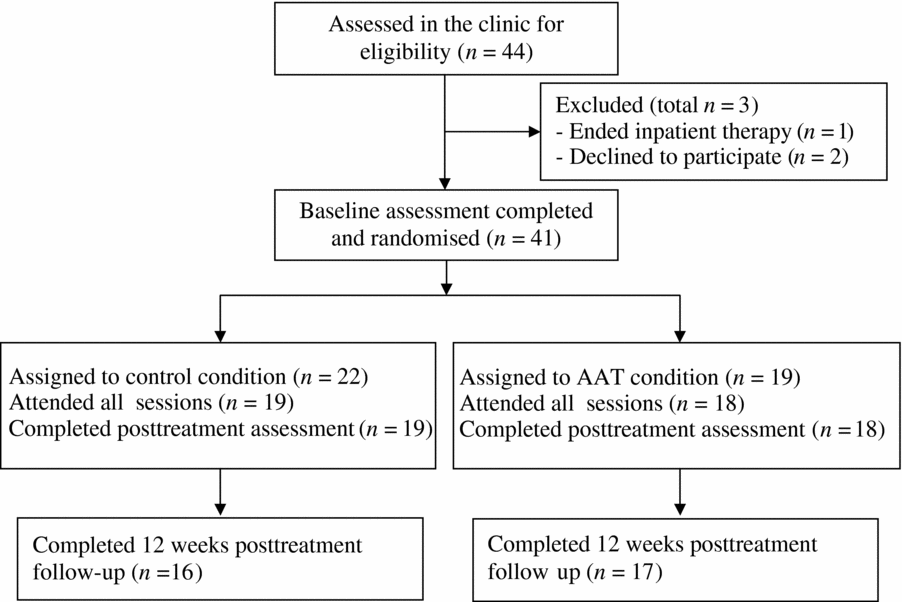
FIGURE 1 Flow of participants through the trial.
Measures
Body weight
The body mass index (BMI, calculated as weight/height²) was determined for each child at pretraining, posttraining, and 12 weeks follow-up. Participants were defined as overweight if their BMI was at or above the 85th percentile, corresponding to a z score of 0.97, according to the Centers for Disease Control and Prevention (83rd CDC percentile). In order to make BMI comparisons between children and adolescents of different ages, an adjusted BMI was calculated as (actual BMI/percentile 50 of BMI for age and sex) × 100, meaning a percentage over ideal BMI. However, since CDC z scores are based on data of children who live in the United States, percentiles of the BMI for age and sex were based on normative Dutch data (Frederiks, van Buuren, Wit, & Verloove-Vanhorick, Reference Fredriks, van Buuren, Wit and Verloove-Vanhorick2000).
General Food Cravings Questionnaire — State (G-FCQ-S; Nijs, Franken, & Muris, Reference Nijs, Franken and Muris2007)
The G-FCQ-S is a 15-item, self-report scale measuring situational desire for food. The scale consists of five factors: (1) an intense desire to eat, (2) anticipation of relief from negative states and feelings as a result of eating, (3) craving as a physiological state, (4) obsessive preoccupation with food or lack of control over eating, and (5) anticipation of positive reinforcement that may result from eating. Participants were asked to rate how true each statement would be for them now, at this moment, using a 5-point scale ranging from 1 (totally not true) to 5 (totally true). A higher total score indicated that more craving was experienced in response to specific situations. The alpha coefficients in the present study for the pretest score was .84 and for the posttest score it was .96.
General Food Cravings Questionnaire — Trait (G-FCQ-T; Nijs et al., Reference Nijs, Franken and Muris2007)
The G-FCQ-T is a 21-item, self-report scale measuring general desire for food and desire to eat. The scale consists of four factors: (1) preoccupation with food (i.e., obsessively thinking about food and eating), (2) loss of control (i.e., the tendency to demonstrate disinhibited eating behavior when exposed to food cues), (3) positive outcome expectancy (i.e., believing eating to be positively or negatively reinforcing), and (4) emotional craving (i.e., the tendency to crave food when experiencing negative emotions). Participants were asked to rate how true each statement would be for them now, at this moment, using a 6-point scale ranging from 1 (totally not true) to 6 (totally true). A higher total score indicated that more craving was experienced across times and situations. The alpha coefficients in the present study for the pretest score was.94 and for the posttest score it was .92.
Approach/avoidance task
The approach avoidance task used in this study was an adaptation of Wiers, Rinck, Kordts, Houben, and Strack (Reference Wiers, Rinck, Kordts, Houben and Strack2010), using a PC keyboard (the up and down arrow) instead of a joystick for responses. This measurement version used a set of 10 unique pictures of healthy food (e.g., a carrot) and 10 unique pictures of unhealthy food (e.g., chips), as well as four filler pictures of neutral stimuli (e.g., office supplies) for 16 practice trials (based on Pronk et al., Reference Pronk, van Deursen, Beraha, Larsen and Wiers2015). The picture stimuli themselves were matched on various visual aspects; for example, white background, active (with person eating) or passive (food only). The pictures were all tilted slightly (3 degrees) to the left or to the right. Participants were only instructed to respond to the tilt of the pictures with an approach movement (arrow down key on the keyboard) to all pictures that were tilted 3 degrees to the left and to respond with an avoidance movement (arrow-up key) to pictures tilted 3 degrees to the right. This tilt-response contingency (left = pull and right = push, versus left = push and right = pull) was counterbalanced over participants. To generate a sensation of approach or avoidance, making the approach movement increased the size of the picture, and pushing the picture away decreased its size. The instruction was to respond only to the tilt of the picture as quickly and accurately as possible, and to keep the key pressed down until the maximum or minimum zoom was reached (500 ms). As such, the required response was unrelated to the food depicted. The measurement phase consisted of 80 trials, where there was a 50/50 matching between tilt and content, that is, 50% of the unhealthy pictures was tilted to the left and 50% to the right, and the same was true for the unhealthy pictures. Approach bias scores towards unhealthy food were calculated by subtracting the mean reaction times for unhealthy food-related pull trials from unhealthy food-related push trials. Similarly, bias scores toward healthy food were calculated by subtracting the mean reaction times for healthy food-related pull trials from healthy food-related push trials.
Implicit associations task
To see if the training effect on the approach/avoidance bias might translate to other cognitive processes, a single category implicit association task (SC-IAT) (Karpinski & Steinman, Reference Karpinski and Steinman2006) was used to measure the children's implicit pleasant and unpleasant associations with unhealthy food. The SC-IAT is a shortened version of the implicit association task (IAT) originally developed by Greenwald, McGhee, and Schwartz (Reference Greenwald, McGhee and Schwartz1998), which uses only one target category and is shortened to three blocks of trials. In the first block, 20 trials were used to practise with typical pleasant and unpleasant exemplar words, such as ‘friendly’ and ‘angry’, with the pleasant (‘fun’) or unpleasant (‘annoying’) labels respectively. The participants were instructed to categorise the words, which were presented in the centre of the screen, with either one of the two labels, presented on the left and right top of the screen. They did so by pressing the left or right arrow key on the keyboard respectively as quickly and accurately as possible. In the second block, a third category label ‘food’ was added, which only had unhealthy food exemplars (as there was no healthy food category, the category label was kept neutral) on either side of the screen, resulting in a response matching between ‘fun’ and ‘food’ on one side versus ‘annoying’ on the other, or vice versa, depending on the counterbalancing. In the final block, the ‘food’ label switched sides to match response key with the other label. The bias was calculated through the standardised difference in latencies (D score) between the second and third block, following the guidelines specified by Greenwald, Nosek, and Banaji (Reference Greenwald, Nosek and Banaji2003).
Attentional bias task
To see whether the training effect on the approach/avoidance bias might translate to other cognitive processes, a visual probe task (VPT) based on the task used by Schoenmakers et al. (Reference Schoenmakers, de Bruin, Lux, Goertz, Van Kerkhof and Wiers2010) was used to measure the attentional bias for unhealthy food. During the VPT, two visually similar pictures, one of healthy and one of unhealthy food (based on Pronk et al., Reference Pronk, van Deursen, Beraha, Larsen and Wiers2015) were shown simultaneously on the screen, positioned on the left and right side of the screen for 500 ms. When the pictures disappeared, a small arrow was shown at the centre of the position where one of the pictures used to be. The arrow could point upwards or downwards, and the participant was instructed to respond to the arrow's direction as quickly and as accurately as possible by pressing the corresponding up or down arrow key on the keyboard. The placement of the healthy and unhealthy food picture was evenly distributed between the left and right position, and the arrow would appear in the unhealthy spot as often as in the healthy spot. The resulting mean reaction times on unhealthy food trials were subtracted from those on healthy food trials to calculate the attentional bias toward unhealthy food.
Description of Interventions
Inpatient treatment as usual
The inpatient treatment consisted of a 10-month, non-diet healthy lifestyle program. The aim was to achieve a healthy body weight through teaching the children to make healthy food choices at fixed times during the day, and to provide daily physical activities. Cognitive behavioural therapy (CBT) principals were integrated as part of the program. The program (description and evaluation in Braet et al., Reference Braet, Tanghe, De Bode, Franckx and Van Winckel2003) consists of three phases of approximately three months each: introduction phase, maintenance phase, and termination phase. A follow-up study showed that treated children lost a significant amount of overweight (with a mean loss of 50%) over the 10-month period, whereas their non-treated case controls continued to gain weight (Braet, Tanghe, De Bode, Franckx, & Van Winckel, Reference Braet, Tanghe, De Bode, Franckx and Van Winckel2003). In the last phase, when children were prepared for ‘returning home’ (termination phase), a mean of 10% additional weight loss was achieved, and at discharge, overweight was reduced to 20–30%. However, follow-up data showed that after leaving the clinic, children regained some of their weight, and at the 14-month follow-up, the children had regained about 20% weight, resulting in about 44.1% of overweight (Braet et al., Reference Braet, Tanghe, Decaluwé, Moens and Rosseel2004). At the 6-year follow-up, overweight children returned to 53% (Goossens, Braet, Verbeken, Decaluwe, & Bosmans, Reference Goossens, Braet, Verbeken, Decaluwe and Bosmans2011).
Approach Avoidance Training
An AAT game was developed, based on the approach/avoidance task, and was used to retrain the children's approach tendencies away from unhealthy food in 10 training sessions. Each training session took approximately 30 minutes and consisted of a training block of 12 minutes, followed by 3 minutes of ‘game time break’ (GTB), then another training block of 12 minutes and a final 3 minutes GTB. During these GTBs, the children were allowed to do bonus training trials to collect more points or to use their points in an online game. The session ended with an additional bonus block of 3 minutes maximum when the children were allowed to train for extra points, which could only be spent in the next session. Including bonus trials, the participants trained on 292 trials on average (10% of which were filler trials) per session. Each correct response (i.e., matching the tilt with the correct response button) resulted in points, with a bonus for speed — for example, 1 point for a correct reaction time above 1,200 ms until 5 points for a correct reaction time below 300 ms. The daily achievement goal (in terms of points) was fixed, and equal for all children, only becoming a little higher each session.
The AAT used a 100/0 matching between tilt and content, that is, all unhealthy pictures were tilted to match the push (avoid) instruction, and all the healthy pictures were tilted to match the pull (approach) instruction. A set of 8 unique pictures of healthy food and 8 unique pictures of unhealthy food was used during each session, meaning each picture was repeated on average 18 times per session. At the start of each training session, the child was given a daily goal to gain a certain number of points, which upon achievement would earn them bonus points. The AAT was embedded inside an online game that allowed the children to use points earned through training to build a virtual city of little houses, trees, roads, and so on. A social element was added by letting the children view the cities of other participants, which they were also allowed to rate with a ‘thumbs up’.
Treatment acceptability
After each session the child completed a diary assessing the acceptability of the computer task (training or Tetris). In particular, children were asked how much they liked the computer task on a 5-point Likert scale (from very nice to very boring) and how difficult they found the computer task on a 5-point Likert scale (from very difficult to very easy).
Tetris
The computer game Tetris was downloaded from www.TheTetrisGame.com and served as the control condition. This was done to allow us to keep two variables (screen time, game element) constant in both conditions.
Procedure
At the start of the ‘returning home phase’ after 6 months of inpatient treatment (April 2013) participants (N = 40) were randomly assigned to either a Tetris-control condition (n = 19) or to an active AAT condition (AAT, n = 21). Randomisation (using random number generator by a person blind to the study) was stratified on sex and age. After randomisation, the 10 computer sessions were spaced out over 4 weeks. The training took place on weekdays with approximately one non-training day in between, dependent on the therapeutic and school program of the children. Children were invited to a classroom and provided with a computer. It was ensured that this computer was placed at a location in the clinic with limited distractions.
Before the beginning of the AAT, the pretest was conducted (April 2013). The children were assessed in the clinic with the G-FCQ-T, G-FCQ-S, the Raven, the Visual Probe Task, the Approach Avoidance Task, and the Implicit Association Task. The assessment phase was spread over two days and took approximately 1.5 hours. One week after the training, participants in both conditions received the same posttest measures (June 2013), BMI was determined, and one week later the children left the clinic. A follow-up was 3 months after the posttest (September 2013), when children returned to the clinic for BMI determination (see flow chart in Figure 1). The assessors for the posttest and follow-up measures were blind to treatment condition. The Ethics Committee of the Ghent University approved the study. Demographic characteristics from children in both conditions are presented in Table 1.
TABLE 1 Differences in Demographic Characteristics Between Children in the AAT and Control Conditions

Note: adjBMI = adjusted body mass index.
Data Analyses
The primary outcome variable was adjusted BMI at 3 months’ follow-up. Intermediate variables were changes in action tendencies (as registered on the AAT), changes in attentional bias (as registered on the VPT), changes in children's implicit pleasant and unpleasant associations of unhealthy food (as registered on the SC-IAT), and changes in craving (as measured with G-FCQ-S and G-FCQ-T).
ANOVAs and chi-square analyses were used for testing differences at baseline on outcome measures between participants of both treatment conditions. There were no significant differences between the two conditions on any of the variables. Outlier analysis showed no outliers on any of the dependent variables. During the training three children dropped out (two in the AAT group, one in the control group).
The change from baseline in action tendencies, attentional bias, implicit pleasant and unpleasant associations with unhealthy food and craving were analysed using linear regression models with group as factor, adjusted for age and sex. The change in the adjusted BMI over time (pretraining, posttraining, follow-up) was assessed using linear mixed models with fixed effects for group, time as factor and group-by-time interaction, age and sex, and a correlated random intercept and random slope for time.
Finally, paired t tests were used to analyse pre–post changes in bias and craving scores per condition.
Results
Evaluation of AAT on Measures of Automatic Processes
Pretraining scores of participants across conditions are shown in Table 2. There were no significant differences in baseline values between both conditions. Overall, at baseline, the results showed a significant approach bias for unhealthy and healthy food (both p < .05), and a marginally significant attentional bias for unhealthy food (p < .10).
TABLE 2 Pretraining Scores of the AAT Condition, Control Condition and Total Group
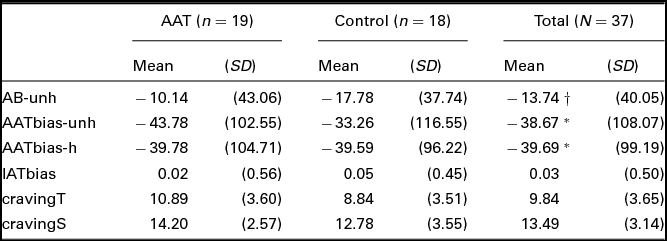
Note: AB-unh = attentional bias score towards unhealthy food; AATbias-unh = approach bias score for unhealthy food; AATbias-h = approach bias score for healthy food; IATbias = implicit association bias score; cravingT = total score on the General Food Cravings Questionnaire – Trait; cravingS = total score on the General Food Cravings Questionnaire – State.
* p < .05, † p < .10
Table 3 shows the mean change between scores on pretraining and posttraining for the bias scores, craving scores, and adjusted BMI in both conditions. The linear regression models revealed no significant differences between both conditions on any of the outcomes (all ps > .30).
TABLE 3 Change Scores (Pre–Post Training) for the Different Outcome Measures
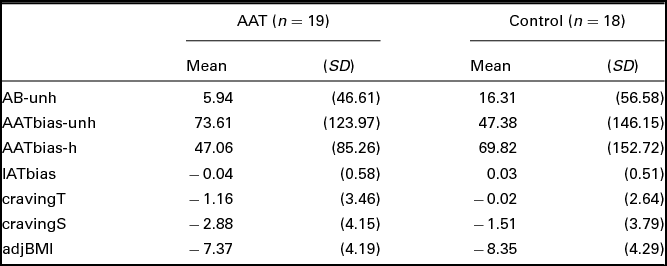
Note: AB-unh = attentional bias score towards unhealthy food; AATbias-unh = approach bias score for unhealthy food; AATbias-h = approach bias score for healthy food; IATbias = implicit association bias score; cravingT = total score on the General Food Cravings Questionnaire – Trait; cravingS = total score on the General Food Cravings Questionnaire – State; adjBMI: adjusted BMI.
In the AAT condition, paired t tests showed from pre- to posttraining a significant reduction in approach bias toward unhealthy food cues (p = .022) and toward healthy food cues (p = .032), and a significant reduction in cravings (p = .022). In the control group, no significant change over time was found for the different variables. The mean pre- and posttraining, bias and craving scores per condition are presented in Figure 2.
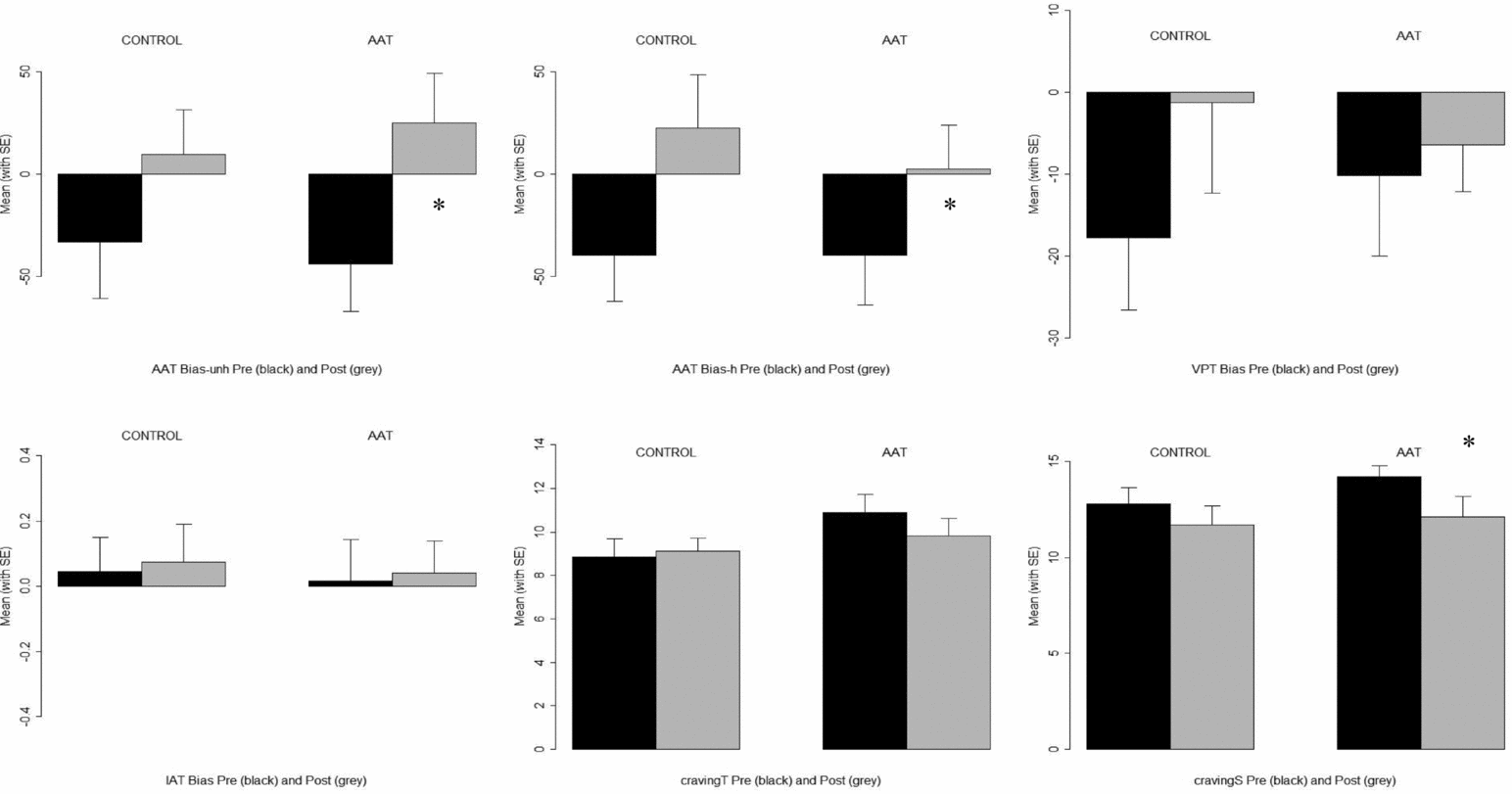
FIGURE 2 Graph of the mean approach bias scores, attention bias scores, IAT bias scores and craving scores (with standard errors) per condition (control/AAT).
Weight change was measured comparing change on adjusted BMI between pretraining and posttraining follow-up. Figure 3 shows the change of the adjusted BMI over time. There were no significant differences between both conditions at any time point (all ps > .13).

FIGURE 3 Evolution of the adjusted BMI over time for the AAT condition and control condition. Thick lines represent group means and fine lines represent individual scores.
Treatment Acceptability
From the 19 children in the training condition, 10 completed the diaries. Among these children, 20% experienced the training as boring, 50% as neutral, and 30% as nice to very nice (mean = 2.80, SD = .92). Further, 10% experienced the training as very difficult, 50% as neutral, and 40% as easy to very easy (mean = 3.30, SD = 1.06).
Discussion
The current pilot study was conducted to evaluate the acceptability and effectiveness of adding an AAT with game elements to a 10-month inpatient treatment program for obese children. It was hypothesised that a retraining of automatic approach tendencies toward food cues embedded in a traditional care-as-usual model may help to weaken the children's automatic reactions to unhealthy food-related cues and help maintain initial weight loss.
For the main clinical outcome measure, no significant effects were found: the weight change between pretraining, posttraining and follow-up was the same in both conditions. For these obese children, a retraining of approach-avoidance tendencies toward healthy/unhealthy food cues did not seem to affect their weight-control capacity. This finding is in contrast with literature in adults and children, where CBM training results in decreased caloric intake and sustained weight loss (Boutelle et al., Reference Boutelle, Kuckertz, Carlson and Amir2014; Kakoschke et al., Reference Kakoschke, Kemps and Tiggemannn2014; Kemps & Tiggemann, Reference Kemps and Tiggemann2015; Kemps et al., Reference Kemps, Tiggemann and Hollitt2014; Werthmann et al., Reference Werthmann, Field, Roefs, Nederkoorn and Jansen2014). The results also showed no significant group differences in approach and attentional bias change to food images over time, nor in the implicit associations and craving toward food from pre- to posttraining. Finally, results showed that overall, the training sessions had reasonable acceptability ratings from the children.
There may be several factors contributing to these findings. First, all children had lost significant weight during the inpatient treatment, and significant changes in their neuronal response to food-related cues might have been already established before the training intervention started. A decrease in activity in regions mediating motivational and attentional salience of food cues has previously been shown in people with a weight-reduced state (Rosenbaum, Sy, Pavlovich, Leibel, & Hirsch, Reference Rosenbaum, Sy, Pavlovich, Leibel and Hirsch2008). This neuronal effect of weight reduction may have attenuated effective group differences due to the AAT. Furthermore, neuro-imaging research has shown decreased brain activation to high-calorie food cues in individuals following a cognitive-behavioural weight-loss treatment (Murdaugh, Cox, Cook, & Weller, Reference Murdaugh, Cox, Cook and Weller2012). However, in the current study, the scores at pretraining, which is after 8 months of inpatient cognitive-behavioural weight-loss treatment and considerable weight loss, still reflect an approach bias for food present in these obese children.
Alternatively, attentional bias, approach tendencies and craving may be low overall due to the absence of tempting food cues within the treatment facility, making it less likely to capture training effects. Addiction literature has shown that attentional bias may peak during high-risk situations for relapse (Field, Marhe, & Franken, Reference Field, Marhe and Franken2014). Therefore, since the current food environment entails a continual ‘high-risk’ situation for obese children, future studies in ambulatory settings may be more adequate to evaluate the impact of the CBM training on approach and attentional bias and craving strength. Further, weight maintenance studies argue that in obesity treatment, initial weight response strongly predicts long-term outcome, and therefore it is recommended to facilitate in therapy early behavioural change (Goldschmidt et al., Reference Goldschmidt, Stein, Saelens, Theim, Epstein and Wilfley2011; Jelalian et al., 2011). So, this means that implementing the training in the first weeks of treatment may be more effective, possibly with extra sessions as a maintenance training delivered via handheld devices such as smart phones that can be used when tempting cues are present or when craving is high.
Further, Boendermaker et al. (Reference Boendermaker, Prins and Wiers2015) put forward that the lack of game elements during the postmeasurement after a training game may demotivate participants to perform well and in this way possible training effects on the bias measures may also be indiscernible. In future research, game elements may be added to the measurement versions of the assessment tasks as well. Additionally, making it possible that training points could be collected across the entire task (from pre- to posttraining) may be also a way to avoid a decrease in motivation toward the end of the training.
However, it is also possible that the control condition was an active training. Recent research proved that playing Tetris may reduce craving strength and attentional bias (Skorka-Brown, Andrade, & May, Reference Skorka-Brown, Andrade and May2014). This research was built on the elaborated intrusion theory (Kavanagh, Andrade, & May, Reference Kavanagh, Andrade and May2005), implying that craving arises from visual images stored in the visuospatial sketchpad of working memory. The rapid rotations and movements of geometric shapes required during playing of Tetris loads heavily on the visuospatial working memory and competes with the encoding of visual ‘craving-images’ (Kavanagh et al., Reference Kavanagh, Andrade and May2005). Van Dillen and Andrade (Reference Van Dillen and Andrade2016) found that playing Tetris was associated with reduced craving and attentional bias to food pictures and a reduced choice of high calorie food. Therefore, in future research, new control conditions must be selected (e.g., a version of the approach-bias retraining with 50% of unhealthy food pictures to be pushed).
Attentional bias modification is a retraining paradigm with promising results in addiction (Schoenmakers et al., Reference Schoenmakers, de Bruin, Lux, Goertz, Van Kerkhof and Wiers2010). In the current study, although between-condition changes were not significant, analyses per condition showed that our 10 sessions of AAT resulted in a significant reduction in approach tendencies toward unhealthy and healthy food pictures. This finding is in line with previous research showing that during a six-session AAT, obese children successfully learned to reduce their automatic approach tendencies toward snack food pictures, but otherwise the study of Warschburger and colleagues (Reference Warschburger, Gmeiner, Morawietz and Rinck2017) showed an increase in approach tendencies toward vegetable items. Further, the current training resulted also in a significant reduction in craving but failed to reduce the attentional bias toward unhealthy food pictures. Since attentional bias may be the more basic eliciting factor in the theoretical models (Franken, Reference Franken2003; Yokum et al., Reference Yokum, Ng and Stice2011) and was shown in obesity research to be related to a greater responsiveness to food cues (Nijs et al., Reference Nijs, Franken and Muris2007), adding an attentional bias modification training may improve the effectiveness in reducing craving and enhancing weight-control.
Finally, the dual process model of obesity (Appelhans, Reference Appelhans2009) suggests that executive functioning interacts with the automatic processes to resist temptation and regulate eating behaviour. It was shown that obese children and adolescents have decreased behavioural self-control capacities compared to normal weight peers: they lack the skills of resisting temptation (Grazaino et al., Reference Graziano, Calkins and Keane2010; Nederkoorn et al., Reference Nederkoorn, Braet, Van Eijs, Tanghe and Jansen2006; Seeyave et al., Reference Seeyave, Coleman, Appugliese, Corwyn, Bradley, Davidson, Kaciroti and Lumeng2009; Verbeken et al., Reference Verbeken, Braet, Claus, Nederkoorn and Oosterlaan2009; Verbeken et al., Reference Verbeken, Braet, Bosmans and Goossens2014). Basic research demonstrated that this can be explained by poor executive functions (EFs) needed to overrule automatic behaviours. EFs are neuropsychological processes that activate and regulate goal-directed behaviour and responses to the environment. It was also shown that EFs have an influence on obesity treatment, with impulsive individuals having more difficulties losing weight (Nederkoorn et al., Reference Nederkoorn, Jansen, Mulkens and Jansen2007; Kulendran et al., Reference Kulendran, Vlaev, Sugden, King, Ashrafian, Gately and Darzi2014; Weygandt et al., Reference Weygandt, Mai, Dommes, Leupelt, Hackmack, Kahnt and Haynes2013), maintaining weight loss (Weygandt et al., Reference Weygandt, Mai, Dommes, Ritter, Leupelt, Spranger and Haynes2015), and leaving the treatment more often (Bjorvell & Edman, Reference Bjorvell and Edman1989). Therefore, future research may need to include training of both bottom-up and top-down processes (embedded in MOT) to be effective for the sustained behaviour change needed to maintain initial weight loss and improve health outcomes.
A limitation of this study was certainly the rather low power. Replication in larger samples is required before firm conclusions about the effectiveness of AAT for obese children can be drawn. Although the current results prompt the tentative conclusion that AAT means no added value on top of the care-as-usual in childhood obesity treatment, it is possible that it is effective and helpful in a waitlist group of obese children. Further, adequately powered studies may include moderators in effect analyses. It is possible that AAT is more effective for children with higher BMI, higher craving scores, or stronger bias for unhealthy food at baseline.
To conclude, although significant effects were absent in the current pilot study, the fact that self-regulation is crucial for long-term successful weight control in children (Appelhans, Reference Appelhans2009) and that this ability is undermined by strong automatic processes in obese children (Murdaugh et al., Reference Murdaugh, Cox, Cook and Weller2012; Yokum et al., Reference Yokum, Ng and Stice2011) makes further research on the added value of treatments to attenuate or retrain automatic processes in obese children essential. Future large-scale RCTs are needed, taking into account the lessons learned concerning the inclusion of motivational elements, the point of time in the therapeutic process, and the observed limitations of the setting and control group, before firm conclusions can be drawn about the clinical usefulness of CBM for weight control in childhood obesity. Further, also moderator analyses are needed.








