Case study
Mr A, aged 83, presented at an accident and emergency department, where he was verbally abusive and physically aggressive. A mild cognitive impairment was noted and he was admitted to the psychiatric hospital under section 2 of the Mental Health Act 1983. Episodes of aggression, although not sexual behaviour, continued. After 6 months in hospital he was discharged under guardianship to a residential home, where he would sometimes threaten people with his stick. He always refused all medication. Four years later the aggression had worsened and he was readmitted to the general hospital with an infection, and transferred on section back to the psychiatric hospital. By this time his cognitive impairment had progressed and a diagnosis of dementia was made. Further aggression occurred on the ward. Several months later he was discharged to a nursing home, still refusing medication.
In the home he now began to approach a female resident with sexual suggestions. Initially the staff managed this by moving him to a different floor, but the behaviour continued with other residents and he was readmitted to hospital because of the difficulty of managing it. On the first day in hospital he began to initiate sexually inappropriate behaviour with female patients who themselves had dementia. He became angry and threatening if staff intervened, for example to ask him to return to his room. He would also hit other patients with his stick if angry. Behavioural strategies were tried with only very limited success. Eventually the team came to the view that the level of risk to others was unacceptable despite the behavioural measures used, and he was detained under the Mental Health Act 1983 with a view to managing his behaviour with medication. The plan was to initiate this orally, but he refused, and so an intramuscular injection of 25 mg chlorpromazine was given to test his response to antipsychotic medication (which he had never had before). This was followed a week later by an injection of short-acting zuclopenthixol acetate (50 mg) and a week after that a depot injection of zuclopenthixol decanoate (50 mg). The depot was continued at monthly intervals. Over the next 2 months the disinhibited behaviours reduced, although he developed moderate extrapyramidal side-effects.
He was discharged on the depot on leave to a nursing home. However, despite being given full information about his legal status (which authorised the use of the depot even without his consent) and the reason for giving the depot, staff at the home did not feel able to administer it to him. The sexual behaviours began to return very intrusively. He repeatedly mutually masturbated a mentally incompetent female resident, who appeared to enjoy his attentions. The home found it difficult to discuss the situation with that person’s husband. He touched and kissed other residents as well. He was moved to another wing, but managed to get back into the original wing.
When this became known he was recalled to hospital. A few weeks later he developed a chest infection, but refused treatment and died.
Prevalence of hypersexuality
Studies of the prevalence of sexually disinhibited behaviour in people with dementia report rates of 2–17%. Reference Burns, Jacoby and LevyBurns et al (1990) found that 6.9% of 178 people with Alzheimer’s disease living at home, in residential care or in hospital showed sexually inappropriate behaviour (exposure, obscene sex language, masturbation, propositioning others), with about equal frequency in men (8%) and women (7%). There was a significant positive association with severity of dementia.
Reference Sourander, Sjogren, Wolstenholme and O'ConnorSourander & Sjogren (1970) studied 132 cases of Alzheimer ’s disease verified on post-mortem examination, reporting abnormal sexual behaviour in 17%. Reference Rabins, Mace and LucasRabins et al (1982) interviewed the caregivers of 55 people with dementia and found that only one family (2%) reported the occurrence of inappropriate sexual behaviour. Reference Kumar, Koss and MetzlerKumar et al (1988) compared questionnaire data relating to 28 people with Alzheimer’s disease and normal controls and found no significant difference in assaultative or sexually inappropriate behaviour (7% in both groups). Reference Drachman, Swearer and O'DonnellDrachman et al (1992) reported hypersexual behaviour in 17% of out-patients with dementia and 8% of in-patients.
Nature of hypersexuality in dementia
As with non-demented people, the range of sexual behaviours shown by people with dementia is very wide. In a study of 40 people with dementia living in a long-term care home, Reference Zeiss, Davies and TinklenbergZeiss et al (1996) systematically observed each of the residents on nine separate 5-minute occasions, coding for each minute of observation whether a sexual behaviour was present and if so whether it was appropriate, inappropriate or ambiguous. Examples of inappropriate behaviour were: making explicit sexual comments, touching someone other than a partner on the breast or genitals, touching a partner on the breast or genitals in public, exposing breasts or genitals in public. Many behaviours were coded as ambiguous, for example being undressed outside the bedroom or bathroom, or sitting with stilled hands cupped over genitals. Of the 1800 one-minute segments coded, inappropriate behaviour occurred in 27 (1.6%) and ambiguous behaviours in 67 (3.7%). Only 18% of the individuals ever displayed inappropriate behaviour during observation, and a similar proportion, 20%, displayed appropriate sexual behaviour. A further 28% showed ambiguous behaviour.
There is no widely agreed definition of when a behaviour becomes abnormal, and so the decision is usually based either on a judgement of what is normal for a person in a particular situation (which is likely to be different according to whether they are in their own home, in a residential home or in hospital), or on the level of risk or discomfort to others. Little research has been carried out on the expression of sexuality in older people on which to base a judgement of what is normal, particularly in institutional settings, and it may be preferable to give greater attention to whether those involved experience the behaviour as distressing rather than whether it is normal.
Boxes 1 and 2 list major factors in the aetiology of changes in sexual behaviour in dementia.
Box 1 Why does sexual behaviour decrease in dementia?
-
• Organic changes of ageing: neuropathy, vasculopathy, reduced sex hormones, erectile dysfunction
-
• Relationship changes: bereavement, shift to caregiver/care recipient relationship
-
• Associated conditions such diabetes and depression
-
• Drugs can impair sexual drive and performance: anticholinergics and antipsychotics can cause impotence and impaired ejaculation
Box 2 Why does sexual behaviour increase in dementia?
Disease-related factors
-
• Sexual disinhibition is a recognised feature of frontal lobe lesions (Reference LishmanLishman, 1998) and forms part of Kluver–Bucy syndrome, originally described following bilateral temporal lobectomy in monkeys (Reference Kluver and BucyKluver & Bucy, 1937)
-
• Disinhibition due to organic brain disease (especially frontotemporal dementias)
-
• Normal etiquette may be forgotten
-
• Delusions, hallucinations, misidentifications
-
• Sensory impairments
Social factors in inappropriate sexual behaviour
-
• Lack of usual sexual partner(s)
-
• Lack of privacy
-
• Understimulating environment
-
• Misinterpretation of cues such as those seen on television or in opposite-gender carers
-
• Unfamiliar environments
Psychological factors
-
• Premorbid patterns of sexual activity and interest exercise a strong effect which continues after the development of dementia
-
• Changes in mood state are commonly seen in dementia. Both depression and mania will affect sexual interest
Drugs
-
• Alcohol and benzodiazepines can produce behavioural and sexual disinhibition in both healthy people and those with dementias
-
• l-dopa can cause hypersexuality in people with Parkinson’s disease
Ethical issues
People with dementia have the same rights as anyone else to express sexual feelings. Carers expect to help these people with their personal care and basic physical needs. Yet the lack of explicit discussion of sexual behaviour in older people often makes carers uneasy about even noticing such behaviours, let alone assisting or allowing those in their care to satisfy their needs. In Zeiss et al’s study cited above, staff did not respond to any of 94 episodes of sexually inappropriate or ambiguous behaviour (although another patient did), and staff ignored 10 out of 17 appropriate sexual behaviours.
Sexual behaviour can also present risks of harm or discomfort to those involved and their families, and people with dementia can themselves be very vulnerable to exploitation and distress. In deciding how to react to sexual behaviour, staff and institutions must consider the legal and ethical framework within which they work.
Box 3 summarises the assessment of competency. At both legal and ethical levels, the patient’s competence is central. If a patient in an institution is not competent to decide whether he or she wishes to proceed with a sexual contact, the staff have a duty of care towards him or her to ensure that no harm results. Whether it is ethical for a non-competent patient to take part in a sexual contact of any sort is a difficult decision which will need to be carefully considered in the light of the person’s background and previous choices, and the nature of the contact. It will normally be helpful to discuss the situation with the patient’s family.
Box 3 Assessment of competency to engage in a sexual relationship (after Lichtenberg & Reference Lichtenberg and StrzepekStrzepek, 1990)
Patient’s awareness of the relationship
-
• Is the patient aware of who is initiating sexual contact?
-
• Does delusion or misidentification affect the patient’s choice, for example by mistaking the other person for their spouse?
-
• Can the patient state what level of sexual intimacy they would be comfortable with?
Can the patient avoid exploitation?
-
• Is the behaviour consistent with previously held beliefs and values?
-
• Does the patient have the capacity to say ‘no’ to uninvited sexual contact?
Is the patient aware of potential risks?
-
• Does the patient realise that the relationship may be time-limited (e.g. if a placement is temporary)?
-
• Can the patient describe how they will react when/if the relationship ends?
For a competent patient, the situation is ethically clearer in that the choice is primarily for the patient to make. Staff may have a role in supporting this decision (for example by ensuring access to private space). Attitudes of staff are very variable, and teams will need to discuss these issues explicitly to ensure that staff are adequately trained and supported. Reference BarrettBarrett (2004) engagingly describes the difficulties that arose when an elderly non-demented man living in a residential home wished to pay for sexual services from female visitors.
Assessment
Clear assessment of the behaviours displayed is essential for a balanced management plan to be developed. A full understanding of both the behaviours and the contexts in which they occur is required. This is best based on direct observation and discussion, either using a standardised system such as dementia care mapping (Reference Kitwood and BredinKitwood & Bredin, 1992) or, more commonly, written observational records made by care staff. Clinical psychologists and other professionals can be very helpful in defining and analysing the behaviours, as well as managing them. A simple and convenient general method of recording behaviours is known as the ABC system, where staff record the antecedents (A), behaviours themselves (B) and consequences (C) (for an account of the system see Reference WellsWells, 1997: pp. 36–37). It is important to know the frequencies of the behaviours, what they are, when and where they occur, and with whom. The effects of interventions cannot be properly evaluated without good baseline records.
Since many of the interventions discussed below themselves carry risks, it is important to balance the risks presented by the behaviour against those of the intervention. Predisposing factors, physical, psychiatric and social need should also be reviewed.
Box 4 summarises the goals of assessment.
Box 4 Assessment of sexually disinhibited behaviour
-
• What form does the behaviour take?
-
• In what context?
-
• How frequent is it?
-
• What factors contribute?
-
• Is it a problem?
-
• To whom?
-
• What are the risks involved?
-
• To whom?
-
• Are the participants competent?
Management
Box 5 summarises important steps in management. Since none of the drugs described below is licensed for the treatment of sexually disinhibited behaviour and many of them carry significant risk of adverse events, it is important to ensure that clear goals of treatment are identified and that all reasonable steps have been taken to manage the behaviours in other ways first. The assessment of the degree of risk to the patient and others will play a key part in the decision whether or not to use medication.
Box 5 Management of sexually disinhibited behaviour
-
• Define target behaviours
-
• Rule out delirium
-
• Consider mood disorder (depression, mania) or psychosis
-
• Review environmental factors
-
• Review cognitive and sensory factors
-
• Educate and support caregivers
-
• Consider specific behavioural methods
-
• Consider drug treatment
-
• Involve other interested parties if necessary
-
• Review progress
Behavioural treatments
We could find no published reports that describe specific behavioural methods of management in this context. Reference Oppenheimer, Jacoby and OppenheimerOppenheimer (2002) gives a helpful review of sexual behaviour in older people, including a discussion of abnormal sexual behaviours in dementia and their management. Reference Grossman, Martis and FichtnerGrossman et al (1999) review behavioural strategies in non-demented sexual offenders. The presence of dementia presents particular difficulties in behavioural treatment strategies because of the impairment of new learning due to the disease.
Providing staff with explanation, support and opportunities for discussion is extremely helpful. Reference Holmes, Reingold and TeresiHolmes et al (1997) report a questionnaire survey of attitudes of professional carers in nursing homes towards sexuality in cognitively impaired residents. Most (74–83%) staff supported the idea that ‘sexual expression among residents with dementing illness is perfectly healthy and may contribute to their positive quality of life’. About one-third of clinicians (33%) but almost two-thirds of administrators (61%, difference not significant) agreed that ‘genital contact between residents with dementing illness should be discouraged’. There was less agreement on behaviours such as hugging and kissing. Almost all staff agreed that staff training should be available.
Any behavioural approach needs to start with a careful assessment of the behaviour, followed by the development of a care plan agreed with staff and other interested parties such as the resident’s family. It is important to provide staff supervision. If these steps fail, it may be necessary to consider removal to another setting.
Physical treatments
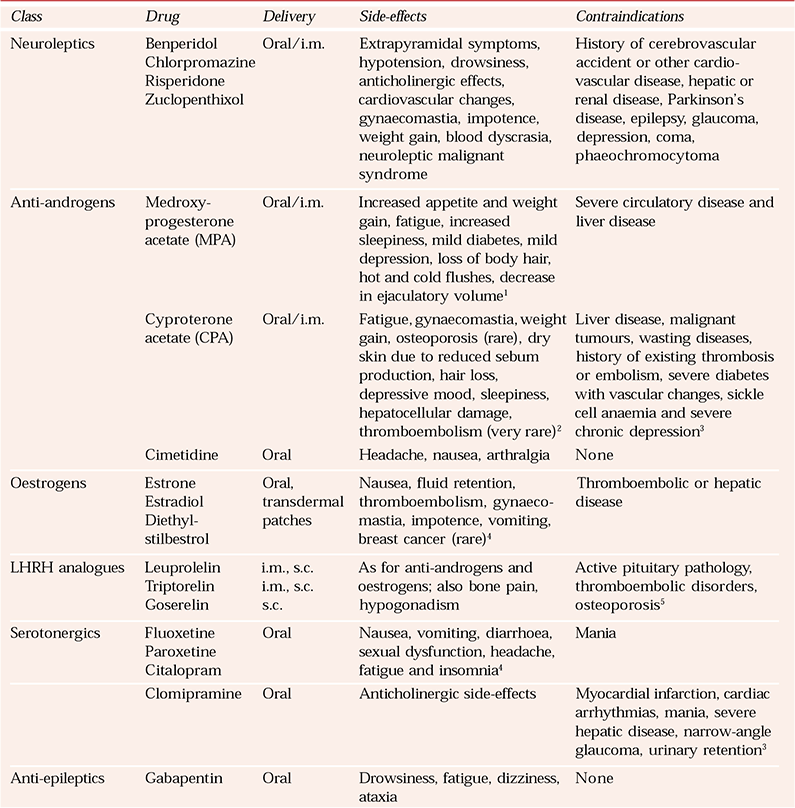
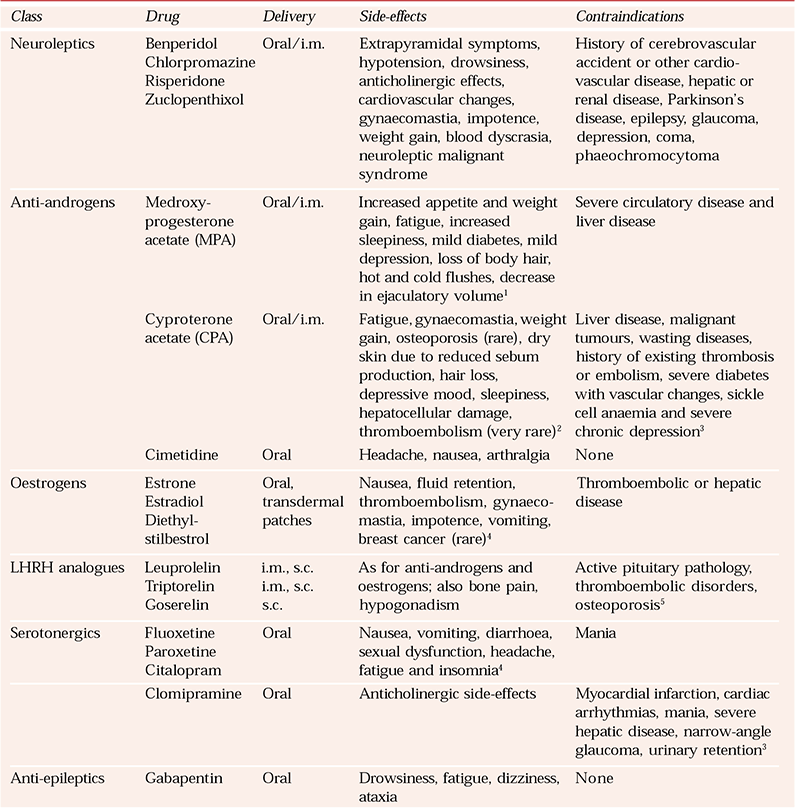
There are no drugs currently licensed in the UK for the treatment of sexual disinhibition in people with dementia. Box 6 summarises the classes of drug that have been used off-licence in this area, and Table 1 gives further details. The manufacturers’ summaries of product characteristics (SPCs) should be consulted for comprehensive information. Little published information exists on drug treatment of hypersexual behaviour in dementia, although a number of treatment studies of sexual offenders and people with paraphilias have been published (for a review see Reference Grossman, Martis and FichtnerGrossman et al, 1999).
Table 1 Characteristics of drugs which have been used off-licence in hypersexuality in dementia
| Class | Drug | Delivery | Side-effects | Contraindications |
|---|---|---|---|---|
| Neuroleptics | Benperidol Chlorpromazine Risperidone Zuclopenthixol |
Oral/i.m. | Extrapyramidal symptoms, hypotension, drowsiness, anticholinergic effects, cardiovascular changes, gynaecomastia, impotence, weight gain, blood dyscrasia, euroleptic malignant syndrome | History of cerebrovascular accident or other cardiovascular disease, hepatic or renal disease, Parkinson’s disease, epilepsy, glaucoma, depression, coma, phaeochromocytoma |
| Anti-androgens | Medroxyprogesterone acetate (MPA) | Oral/i.m. | Increased appetite and weight gain, fatigue, increased sleepiness, mild diabetes, mild depression, loss of body hair, hot and cold flushes, decrease in ejaculatory volume1 | Severe circulatory disease and liver disease |
| Cyproterone acetate (CPA) | Oral/i.m. | Fatigue, gynaecomastia, weight gain, osteoporosis (rare), dry skin due to reduced sebum production, hair loss, depressive mood, sleepiness, hepatocellular damage, thromboembolism (very rare)2 | Liver disease, malignant tumours, wasting diseases, history of existing thrombosis or embolism, severe diabetes with vascular changes, sickle cell anaemia and severe chronic depression3 | |
| Cimetidine | Oral | Headache, nausea, arthralgia | None | |
| Oestrogens | Estrone Estradiol Diethylstilbestrol |
Oral, transdermal patches | Nausea, fluid retention, thromboembolism, gynaecomastia, impotence, vomiting, breast cancer (rare)4 | Thromboembolic or hepatic |
| LHRH analogues | Leuprolelin Triptorelin Goserelin |
i.m., s.c. i.m., s.c. s.c. |
As for anti-androgens and oestrogens; also bone pain, hypogonadism | Active pituitary pathology, thromboembolic disorders, osteoporosis5 |
| Serotonergics | Fluoxetine Paroxetine Citalopram |
Oral | Nausea, vomiting, diarrhoea, sexual dysfunction, headache, fatigue and insomnia4 | Mania |
| Clomipramine | Oral | Anticholinergic side-effects | Myocardial infarction, cardiac arrhythmias, mania, severe hepatic disease, narrow-angle glaucoma, urinary retention3 | |
| Anti-epileptics | Gabapentin | Oral | Drowsiness, fatigue, dizziness, ataxia | None |
Box 6 Classes of drugs used in managing sexually disinhibited behaviour
-
• Neuroleptics
-
• Anti-androgens
-
• Oestrogens
-
• LHRH analogues
-
• Serotonergics
-
• Gabapentin
Neuroleptics
Neuroleptics are probably widely used in managing sexually disinhibited behaviour in dementia, but there is very little published evidence of their efficacy or safety in this group. Recent advice in the UK has emphasised the increased risk of cerebrovascular events in patients with dementia on olanzapine or risperidone. Benperidol has been used in the treatment of paraphilias (Reference FieldField, 1973; British Medical Association & Royal Pharmaceutical Society of Great Britain, 2005). The availability of depot preparations can make their use possible with non-adherent patients, as in the case study that opened this article, provided that appropriate ethical and legal guidelines are followed.
Manipulation of testosterone levels
Anti-androgens, oestrogens and luteinising hormone releasing hormone (LHRH) agonists have been used in sexual offenders, but little is known about their use in older people with dementia. These agents decrease testosterone levels, which may reduce sexual drive (Reference Schiavi and WhiteSchiavi & White, 1976). However, it is unclear how far serum testosterone correlates with hypersexual behaviour (Reference Kravitz, Haywood and KellyKravitz et al, 1996; Levitsky & Reference Levitsky and OwensOwens, 1999).
The secretion of testosterone is regulated by a feedback mechanism in the hypothalamus–pituitary–testes axis. The hypothalamus produces gonadotrophin-releasing hormone, which stimulates the pituitary gland to produce luteinising hormone and follicle-stimulating hormone. Luteinising hormone stimulates the release of testosterone from the testes.
Circulating testosterone levels are maintained by a homoeostatic mechanism. When circulating testosterone levels decrease, an increase in production is promoted by luteinising hormone, which in turn is stimulated by LHRH. An increase in testosterone levels has an inhibitory effect on the hypothalamus and the pituitary.
Anti-androgens
The most widely used anti-androgens are medroxyprogesterone acetate (MPA) and cyproterone acetate (CPA).
Medroxyprogesterone acetate
This is a potent progestogen that decreases serum testosterone levels by inhibiting luteinising hormone release through negative feedback on hypothalamic receptors, hence reducing testosterone secretion from the testes as described above.
There are no controlled studies supporting the use of anti-androgens for the treatment of hyper-sexuality or paraphilias in older people with dementia (Levitsky & Reference Levitsky and OwensOwens, 1999). In two studies without controls, men with dementia were given intramuscular doses of 150–300 mg MPA every 1 or 2 weeks; their inappropriate sexual behaviour stopped within 2 weeks (Reference CooperCooper, 1987; Reference Weiner, Denke and WilliamsWeiner et al, 1992). In a case report, marked disinhibited and disruptive sexual behaviour ceased in a man with dementia following intramuscular MPA treatment (Reference AmadeoAmadeo, 1996).
Cyproterone acetate
Another potent progestogen, CPA also possesses testosterone antagonistic activity by blocking androgen receptors.
Reference Haussermann, Goecker and BeierHaussermann et al (2003) reported that administration of CPA to a man with vascular dementia and another with Parkinson’s disease with associated dementia successfully reduced sexual acting out.
Cimetidine
Cimetidine is a histamine H2-receptor antagonist with non-hormonal anti-androgen properties in rats (Reference Lardinois and MazzaferriLardinois & Mazzaferri, 1985). It has been reported to decrease libido and hypersexual behaviour in 14 out of 20 patients with dementia without serious side-effects (Reference Wiseman, McAuley and FreidenbergWiseman et al, 2000). The other six patients responded to combinations of cimetidine with ketoconazole, spironolactone or both, drugs that also exhibit anti-androgen action.
Oestrogens
Oestrogens (estrone, estradiol and diethylstilbestrol) have a strong negative feedback effect on hypothalamic and pituitary hormone secretion. They decrease luteinising hormone and follicle-stimulating hormone production, which leads to a reduction in the production of testosterone.
There are few reports on the use of oestrogens for the treatment of hypersexuality in people with dementia, possibly because of the greater presence of cardiovascular and thromboembolic risk factors in the older population and the association between cardiovascular-related deaths and oestrogen use in men treated with diethylstilbestrol for prostate cancer (Levitsky & Reference Levitsky and OwensOwens, 1999).
In one study, although few details are given, a marked improvement in sexual behaviour was seen in 38 out of 39 men with cognitive impairment when treated with oral oestrogen (0.625 mg/day) or with transdermal oestrogen patches (0.005–0.1 mg) (Reference Lothstein, Fogg-Waberski and ReynoldsLothstein et al, 1997). In a case report, the hypersexual behaviour of a man with cognitive impairment stopped when he was given 1 mg diethylstilbestrol twice a day (Reference Kyomen, Nobel and WeiKyomen et al, 1991).
LHRH analogues
Gonadotrophin-releasing hormone (or gonadorelin agonists) are LHRH analogues. These reversibly suppress the pituitary–gonadal axis by down-regulating the gonadotrophin cells. They stimulate the release of follicle-stimulating hormone and luteinising hormone from the pituitary, increasing androgen and oestrogen production. With continued administration of LHRH agonists, the pituitary no longer responds to endogenous LHRH, reducing the secretion of follicle-stimulating hormone and luteinising hormone, which causes a marked decrease in testosterone secretion. To remain effective, LHRH analogues have to be used on a continuous basis (Reference Rosler and WitztumRosler & Witztum, 1998).
Leuprorelin, triptorelin and goserelin
These three LHRH analogues offer a treatment option for sex offenders and people with severe paraphilia (Reference Briken, Hill and BernerBriken et al, 2003). However, there is a case report of the use of leuprolide acetate (leuprorelin) to treat sexual aggression in a patient with dementia and Kluver–Bucy syndrome (Reference OttOtt, 1995), and Reference Rich and OvsiewRich & Ovsiew (1994) report that it was effective in the treatment of exhibitionism in a patient with Huntington’s disease.
Serotonergics and noradrenergics
Selective serotonin reuptake inhibitors
Fluoxetine, paroxetine, citalopram and sertraline have been reported to be effective against sexual disinhibition and paraphilias (Reference Greenberg, Bradford and CurryGreenberg et al, 1996). In addition to their antilibidinal effect, these drugs have anti-obsessive properties, tying in with the suggestion that hypersexuality and paraphilia might be related to obsessive–compulsive disorder (Reference Perilstein, Lipper and FriedmanPerilstein et al, 1991; Reference McElroy, Phillips and KeckMcElroy et al, 1994).
Reference Stewart and ShinStewart & Shin (1997) describe a reduction in sexual disinhibition in a patient with dementia when treated with paroxetine. A dramatic improvement in sexual aggression was also seen in a similar patient treated with citalopram (Reference Raji, Liu and WallaceRaji et al, 2000).
The use of these agents may be attractive because of their relatively safe profile compared with other drugs.
Tricyclic antidepressants
Clomipramine, a tricyclic that inhibits the reuptake of serotonin and noradrenaline, was also effective in treating sexual disinhibition in two people with dementia (Reference Leo and KimLeo & Kim, 1995). Careful monitoring of elderly people is required during treatment with clomipramine because of the risk of orthostasis, falls and worsened confusion.
Gabapentin
Gabapentin is an anti-epileptic structurally related to the central nervous system inhibitory neuro-transmitter gamma-aminobutyric acid (GABA). Gabapentin may increase GABA synthesis in the brain while decreasing the release of monoamine transmitters (Reference Semanchuk and LabinerSemanchuk & Labiner, 1997).
In Alzheimer’s disease, behavioural disturbances are associated with deficits of GABA in brain tissue (Reference Hardy, Cowburn and BartonHardy et al, 1987). Gabapentin has been successfully used for the management of agitation in Alzheimer’s disease (Reference Regan and GordonRegan & Gordon, 1997). It has also been reported to be effective in treating behavioural symptoms of dementia (Reference Herrmann, Lanctot and MyszakHerrmann et al, 2000; Reference Roane, Feinberg and MecklerRoane et al, 2000).
In a case report, a patient with vascular dementia showed reduced agitation and inappropriate sexual behaviour when treated with gabapentin (Reference MillerMiller, 2001). In three nursing home residents, two with Alzheimer’s disease and the other with vascular dementia, sexual disinhibition was effectively treated with gabapentin (Reference Alkhalil, Tanvir and AlkhalilAlkhalil et al, 2004).
Gabapentin is a relatively safe drug in elderly people.
Other drugs
Other psychotropic medications have been used to treat hypersexuality in people with dementia, with mixed results. Antimanic drugs (carbamazepine and valproic acid), often prescribed as adjuncts for behavioural symptoms of dementia, offer some effectiveness against disinhibition. Cholinesterase inhibitors, buspirone, propranolol, trazodone and benzodiazepines have also been tried (Reference Lesser, Hughes and JemelkaLesser et al, 2005).
MCQs
-
1 Sexually disinhibited behaviour in dementia:
-
a occurs at some point in most people with the disease
-
b is reported to be more common in men than in women
-
c rarely occurs outside institutions.
-
d is more common in mild than in severe dementia.
-
-
2 Assessment of sexually disinhibited behaviour:
-
a should always be undertaken by a psychologist
-
b is best carried out using standardised rating scales
-
c requires a careful study of its frequency, severity and context
-
d needs to consider risks to others.
-
-
3 A person’s competency to engage in a sexual relationship:
-
a can be assessed using the Mini-Mental State Examination
-
b can be assessed by determining whether they enjoy the behaviour
-
c could be affected by misidentification
-
d is not relevant to how sexual behaviour is managed.
-
-
4 Gabapentin:
-
a is an analogue of gamma-aminobutyric acid
-
b is licensed for the treatment of hypersexuality in dementia
-
c inhibits GABA synthesis in the brain
-
d can be administered either subcutaneously or intra-muscularly.
-
-
5 Of the drugs used in the treatment of sexual disinhibition in dementia:
-
a triptorelin is an LHRH antagonist
-
b clomipramine has potential anticholinergic side-effects
-
c progestogens should be avoided if the patient has liver disease
-
d diethylstilbestrol increases luteinising hormone and follicle-stimulating hormone production.
-
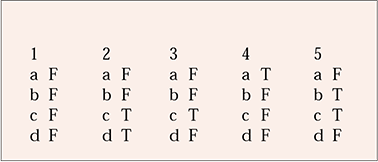
MCQ answers
| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | F | a | F | a | T | a | F |
| b | F | b | F | b | F | b | F | b | T |
| c | F | c | T | c | T | c | F | c | T |
| d | F | d | T | d | F | d | F | d | F |



eLetters
No eLetters have been published for this article.