Significant numbers of people suffer from chronic depression, in which clinically low mood and associated symptoms continue unabated for 2 years or more and which without effective treatment may become a lifelong problem. A diagnosis of chronic depression is known to be associated with high use of general medical services. The socio-economic consequences for individuals are substantial, with increased risk of marital breakdown, unemployment, days off work, and reduced social and economic standing (Reference Wells, Burnam and RogersWells et al, 1992). There is an urgent need to develop effective treatments to meet the needs of this population (Reference Thase, Nolen, Zohar and RooseThase, 1994).
Psychological therapy may confer some benefit to patients with difficult-to-treat residual symptoms. For example, Reference Paykel, Scott and TeasedalePaykel et al(1999) demonstrated that cognitive therapy reduces both relapse rates for acute major depression and recent, persistent severe residual symptoms. Two therapists from that study went on to propose a cognitive and behavioural conceptualisation of chronic depression and offer a treatment protocol based on an adaptation of ‘standard’ cognitive–behavioural therapy for acute depression (Reference Moore and GarlandMoore & Garland, 2003). However, patients who meet diagnostic criteria for chronic depression present particular challenges to psychological therapists that established psychotherapies have not been able to address. A large multi-centre clinical trial (Reference Keller, McCullough and KleinKeller et al, 2000) has demonstrated that The cognitive behavioural analysis system of psychotherapy (CBASP) appears to be an effective therapy with a structure that assists therapists in meeting the challenges that these patients present.
What is CBASP?
Developed to treat individuals with chronic depressive disorders, CBASP is currently the only therapy specifically designed for this patient group. When administered with antidepressant medication, CBASP has been shown to be an effective treatment (see ‘The evidence base’ below).
CBASP is the result of over 30 years’ research and clinical experience by James P. McCullough, Jr, Professor of Psychology and Psychiatry at the Virginia Commonwealth University in the USA. The development of CBASP took place through a trial and error, stepwise clinical research process underpinned theoretically by work on interpersonal theory (Reference KieslerKiesler, 1983), behavioural change achieved through the use of reward and reinforcement schedules (Reference SkinnerSkinner, 1969), social learning theory (Reference BanduraBandura, 1977) and Jean Reference PiagetPiaget's (1923) theory of cognitive–emotional development. These varied ideas about development and behaviour have been combined to allow the therapist an opportunity to address cognitive, emotional and behavioural domains as they interact with the patient's environment. In addition, specific interpersonal skills are taught.
The theoretical model
The theoretical premise of CBASP is that arrested maturational development is the aetiological basis of chronic depression. For most patients with early-onset chronic depression the experience of maltreatment or of lower-grade but protracted decrease or absence of nurturing, or the loss of significant others in the family are thought to have led to an arrest of the cognitive–emotive maturational process at the Piagetian preoperational stage of development (Box 1). Patients with late-onset (aged 21 or over) chronic depression rarely present with antecedent dysthymia: they can more often pinpoint a stressful event that precipitated the depression (Reference McCulloughMcCullough, 2000: p. 48). This unyielding emotional state of depression leads to the conclusion that the world is unworkable (hopelessness) and its problems are irresolvable (helplessness). This uncontrollable dysphoric condition becomes all-consuming and leads to preoperational thinking and the conclusion that ‘things will always be this way’. This heightened emotionality has an impact on rational thought and leads to general functional regression to the Piagetian preoperational stage.
Box 1 Piaget's concept of the preoperational stage of cognitive development
Piaget believed that cognitive development occurs in four stages, characterised by qualitative changes in the nature of thinking:
-
1 Sensorimotor stage (0–2 years of age)
-
2 Preoperational stage (2–7 years)
-
3 Concrete operational stage (8–12 years)
-
4 Formal operational stage (12–15 years)
By observing children's play, Piaget demonstrated that towards the end of the second year a qualitatively new kind of psychological functioning occurs. An ‘operation’ in Piagetian theory is any procedure for mentally acting on objects. The hallmark of the preoperational stage is sparse and logically inadequate mental operations. The preoperational stage is characterised by:
-
• Symbolic functioning – the use of mental symbols, words or pictures to represent something that is not physically present
-
• Centration – focusing or attending to only one aspect of a stimulus or situation. For example, in transferring liquid from a narrow beaker into a shallow dish, a preschool child might judge the quantity of liquid to have decreased, because its level is ‘lower’, i.e. the child attends to the height of the water, but not to the compensating increase in the diameter of the container
-
• Intuitive thought – the child is able to believe in something without knowing why
-
• Egocentrism – a version of centration, this is the child's tendency to think only from their own point of view and to be unable to take the point of view of others
-
• Inability to conserve – lack perception of conservation of mass, volume and number after the original form has changed
The model emphasises CBASP's ‘person × environment’ focus (Fig. 1) and teaching the patient their ‘stimulus value’ (discussed below) within that environment. The potential for change within interpersonal interactions is central, as patients with chronic depression are seen as repeating patterns of behaviour, trapped in a repetitive experience of ‘sameness’. The therapist teaches Piagetian formal operations problem-solving and empathic responsivity in the conduct of social interactions.

Fig. 1 Person × environment interactions: (a) cognitive connection means that emotional change is possible; (b) preoperational disconnection with the environment precludes emotional change. (Adapted from Reference McCulloughMcCullough, 2006: p. 125. With permission.)
The focus of CBASP
As with many psychotherapies a particular language is used in CBASP, and a glossary of some of the terms used appears in Box 2.
Box 2 Glossary of terms
Causal theory conclusions A conclusion drawn by the patient with the assistance of the therapist about each significant other in the patient's life that describes the particular effect or stamp that the significant other has had on the patient
Contingent personal responsivity A contingent response administered by the therapist for maladaptive behaviour exhibited by the patient during a clinical session. Contingent personal responsivity is used to connect the patient to the consequences of their destructive social behaviour during sessions as a model for interactions outside of therapy
Disciplined personal involvement The therapist's personal involvement in the patient's problems, using both the interpersonal discrimination exercise and contingent personal responsivity. It demonstrates for the patient that behaviour has consequences and allows them the opportunity for a new interpersonal reality
Hot spot A behaviour/reaction/event involving the patient and therapist that occurs during a therapy session and implicates the transference hypothesis. The therapist uses the hot spot as a signal to administer an interpersonal discrimination exercise
Interpersonal discrimination exercise An exercise that helps the patient to distinguish the person of the therapist from the influential maltreating significant other who has interpersonally injured the patient
‘Significant other’ history During the second session of therapy the patient is invited to list up to seven individuals (significant others) in their life history who have played a major informing role in their development, i.e. have influenced them to be the kind of person they are today. These influences can be positive or negative, for good or for bad
Situational analysis This is carried out, as far as possible, in every session. The primary technique within CBASP, situational analysis connects the patient to the consequences of their behaviour and identifies cognitive and behavioural strategies that interfere with adaptive living. This provides a platform for remediation of old, dysfunctional repertoires and the rehearsal of new functional ones
Transference hypothesis On the basis of the ‘significant other’ history, the therapist constructs one transference hypothesis that depicts the major theme characterising the causal theory conclusions. The hypothesis will fall into one of four domains: patient and therapist intimacy; patient's disclosure of emotional need; patient's failure or mistakes during sessions; and feeling or expressing negative affect towards the therapist
CBASP focuses on teaching patients to become aware of and examine the consequences of their interpersonal behaviour. A social problem-solving algorithm drawing on cognitive, behavioural and interpersonal techniques is used to address interpersonal difficulties. It is important to note that CBASP differs from cognitive therapy by focusing primarily on interpersonal interactions (including those with the therapist). Patients learn how their cognitive and behavioural patterns produce and perpetuate their interpersonal problems and how to alter these maladaptive patterns of interpersonal behaviour.
The main therapy technique is situational analysis, which is used to exacerbate psychopathology in sessions using techniques that have been designed to facilitate behavioural change (Box 3). Negative reinforcement is the essential motivational strategy, i.e. a change in behaviour will result in reduced distress. Areas of problem behaviour (both present and absent) are identified and behaviours are modified where they exist and taught where they are missing. Many strategies familiar to mental health professionals, such as assertiveness, problem-solving and modelling, are used. Therapists are encouraged to practise disciplined personal involvement with patients. The aim of this is to modify behaviour through use of the interpersonal discriminatory exercise educated by a transference hypothesis generated from the patient's ‘significant other’ history. Transference hypothesis ‘hot spots’ are proactively challenged throughout therapy whenever they arise.
Box 3 The key mechanisms of change
-
• Situational analysis
-
• Disciplined personal involvement
-
• Interpersonal discrimination exercises
-
• Contingent personal responsivity
-
• Strategies such as assertiveness training, problem-solving and modelling
The evidence base
The model was developed initially through single-case investigative research (Reference McCulloughMcCullough, 1984, Reference McCullough1991) and more recently through a large multi-centre study comparing CBASP with antidepressant medication. The latter resulted in as a series of publications (Reference Keller, McCullough and KleinKeller et al, 2000; Reference Hirschfield, Dunner and KeitnerHirschfield et al, 2002; Reference Arnow, Manber and BlaseyArnow et al, 2003; Reference Nemeroff, Heim and ThaseNemeroff et al, 2003; Reference Schatzberg, Rush and ArnowSchatzberg et al, 2005), of which the first is central (Reference Keller, McCullough and KleinKeller et al, 2000). The study involved three treatment groups comparing CBASP alone with nefazodone (a serotonergic antidepressant), and a combination of the two. There was no placebo group. Of the 681 adults randomised, 662 attended at least one treatment session and 519 completed the study. The study lasted 12 weeks, with individual sessions of CBASP occurring twice weekly for the first 4 weeks and weekly thereafter until week 12. Additional sessions were permitted up to a maximum of 20 sessions.
The study population comprised individuals with chronic major depressive disorder (i.e. lasting for at least 2 years), current major depressive disorder superimposed on dysthymic disorder (‘double depression’) or recurrent major depressive disorder with incomplete inter-episode recovery. Participants were aged 18–75 years. It is worth noting that one-third of all depressive episodes experienced by the general population last for more than 2 years. The intention-to-treat analysis using a score on the Hamilton Rating Scale for Depression as a measure of improvement revealed that 48% of participants improved in the nefazodone group, 48% in the CBASP group and 73% in the combined treatment group. Combined treatment had significantly greater effect on psychosocial improvement than either single therapy. In the CBASP group, the effect of the therapy on psychosocial function was evidenced by decreased escape avoidance and increased planful problem-solving (Reference Blalock, Fouladi and CinciripiniBlalock et al, 2007).
The researchers found a very high prevalence of early-life trauma in their sample of people with chronic depression (Reference Nemeroff, Heim and ThaseNemeroff et al, 2003): 65% reported an experience of trauma as a child; only 35% with chronic depression had had no childhood trauma. Childhood trauma events detailed in the study include, in descending order of frequency: physical abuse, parental loss, sexual abuse and neglect. Out of the 65% who reported trauma, 37% had experienced one type of trauma, 18% had experienced two, 8% three and 2% four types. CBASP, whether alone or supplemented by medication, was superior to antidepressant medication for individuals with a history of early-life trauma, independent of gender, age, race and severity of depression. This group of researchers is conducting a second ongoing trial comparing CBASP with brief supportive psychotherapy (n = 850).
The CBASP process
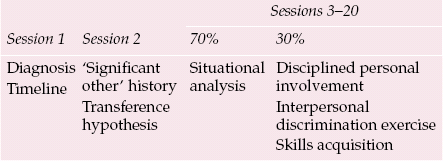
As with other therapies, CBASP has clearly defined and operationalised stages that the therapist follows. This ‘conceptual map’ is set out in Table 1.
Table 1 Operationalised stages of the CBASP process
| Sessions 3–20 | |||
|---|---|---|---|
| Session 1 | Session 2 | 70% | 30% |
| Diagnosis Timeline |
‘Significant other’ history Transference hypothesis |
Situational analysis | Disciplined personal involvement Interpersonal discrimination exercised Skills acquisition |
To illustrate the steps and process of CBASP we will present the case of Morag, a fictitious patient based on our clinical experience over many years of treating large numbers of with people chronic depression.
Case scenario: Morag
Morag is a 45-year-old single woman with a 20-year history of dysthymia and depression. Her current episode of depression has lasted 3 years with only partial response to a variety of antidepressant medication. Electroconvulsive therapy was last given 12 months ago with limited effectiveness. No treatment has cured her chronic depression.
Establishing the diagnosis
CBASP has been developed specifically to address the interpersonal, cognitive and behavioural deficits of individuals with chronic depression and it makes no claims for effectiveness in other disorders. It is therefore essential to establish that the patient meets diagnostic criteria for chronic depression and does not have either an acute disorder or an episodic disorder with insufficient duration of the current episode and remission between episodes.
Step 1: Diagnosis and timeline
This is established in two stages. First, the presenting problems must be consistent with unipolar depressive disorder (either major depressive disorder or dysthymic disorder). Second, a clear picture of the duration of the current disorder must be formed. The Depression Timeline Worksheet (Reference McCulloughMcCullough, 2003) is a graphical way of working collaboratively with the patient in mapping out the severity and duration of depressive symptoms. Two questions are answered: is the disorder chronic or acute and episodic? And if the present disorder is chronic, was dysthymia present prior to this episode?
The same characteristics are charted for all other depressive episodes to enable a precise diagnosis. In addition to the mapping of severity, duration and variation in depressive symptoms over time, clinical experience has taught us that this process reveals useful information for treating the patient in subsequent sessions.
The ‘significant other’ history and construction of the transference hypotheses
Many individuals with chronic depression have experienced adversity in their relationships with significant others during early childhood which can lead to early-onset depression (before 21 years of age). For other individuals whose index episode of depression occurs later in life (late-onset depression) the psychosocial sequelae of depression can lead to significant, and often pervasive, interpersonal problems. The story of learning (the ‘learning biography’) as a result of the experience of adverse events in early childhood and/or interpersonal sensitivity and difficulty in maintaining attachment bonds in early adulthood (and beyond) may lead individuals to adopt negative expectations about the course of subsequent relationships. In chronic depression the maxim is ‘the way things have played out for me in life with others is the way things will play out for me with this therapist’. This transference, or the learned behavioural patterns that patients enact in their everyday life, will be played out with the therapist. Transference is an important concern and target for CBASP therapists. It is proactively managed and specifically subject to collaborative assessment and analysis early in therapy, through the taking of a ‘significant other’ history in session 2 (Table 1). Together, the therapist and patient deduce causal theory conclusions from the ‘significant other’ history and construct one transference hypothesis that relates to the relationships that will exist between patient and therapist in the context of their work together. This transference of learned behaviour will, more often than not, be enacted with the therapist.
Step 2: The ‘significant other’ history
The patient is invited to think back over their life and identify up to seven individuals who they feel have exerted the most influence on the direction their life has taken. These influences may be positive or negative. The therapist should note the content and order of the significant other list. Our clinical experience is that this is a step that patients find challenging. A guiding principle of CBASP is ‘let the patient do the work’, and the therapist's task is to facilitate the construction of this list. A maximum of six significant others is sufficient.
Case scenario: Morag
Morag listed five people: her mother, father, grandfather, younger brother and a family friend Paul. Each person on the list was discussed and Morag was asked how they had affected the course of her life; what it was like growing up or being around them; and how they had influenced the kind of person she now is. Some of her responses to these questions were as follows.
Regarding her mother: ‘She was overprotective and anxious. She talked a lot but never listened and if an opinion contrary to hers was expressed this brought punishment in both implicit and explicit ways.’ The causal theory conclusion regarding her mother, effectively the ‘stamp’ that she had left on Morag (in Morag's own view), was encapsulated in the sentence: ‘I don't want to be seen to be like my Mum so I keep my thoughts and opinions to myself.’
Regarding her father: ‘He was disinterested in me and rarely spent time with me.’ The causal theory conclusion or stamp for her father was: ‘People and relationships are difficult and hurtful, so it is best to keep to yourself.’
The other people on the list were discussed in a similar way and the following causal theory conclusions were derived:
-
• for the grandfather: ‘No matter what I do I'm not interesting.’
-
• for the younger brother: ‘I can be likeable.’
-
• for Paul: ‘I can have opinions and people will listen.’
Step 3: Construction of the transference hypothesis
On completion of the ‘significant other’ history, the therapist formulates one transference hypothesis. In effect this relates to how the patient might transfer his or her expectation of and habitual responses to significant others to the relationship with the therapist. Four transference domains of potential interactions are targeted within CBASP:
-
• intimacy: expression of interpersonal intimacy by either patient or therapist
-
• failure: situations in which the patient fails at something or makes a mistake in a session
-
• emotive need: the patient's direct or indirect expression of emotional need towards the therapist
-
• expression of negative affect: the patient's experience or expression of negative affect (directly or indirectly) towards the therapist.
The task here is to consider these four domains and to place the content of the transference hypothesis in one of them. To do this, the therapist takes the causal theory conclusions (stamps) derived from the ‘significant other’ history into account and, using their clinical experience, judgement and acumen, generates a transference hypothesis they feel will come into play during therapy. For Morag a possible transference hypothesis might be: ‘If I get close to Mr Swan and let him know how I feel then he will punish, reject or ridicule me’ (intimacy domain).
The transference hypothesis alerts the therapist to interpersonal ‘hot spots’ that will emerge during the therapy process. When hot-spot moments occur, they are addressed with the interpersonal discrimination exercise (Box 2 and below).
The situational analysis
Situational analysis is the major technique available to CBASP therapists to help modify the cognitive, behavioural, emotional and interpersonal dysfunction that patients with chronic depression bring to therapy. Situational analysis is a clearly operationalised procedure designed to address the preoperational individual by presenting them with a cognitive–emotional challenge requiring formal operational thinking, i.e. thinking at a more advanced level.
In situational analysis, the patient must also become aware that their actions and words have consequences for themselves and others. Moments of ‘interpersonal causality’ are used to teach the patient that they have a stimulus value in their environment and that it is their style of interaction with others that maintains their depressive position. Furthermore, the clear structure of situational analysis provides a framework for both therapist and patient that inhibits the typically detached monologue style of chronically depressed individuals by facilitating a collaborative dialogue with their therapists. Situational analysis is an iterative procedure and makes up 70% of the therapeutic endeavour (Table 1).
The patient is required to complete at least one Coping Survey Questionnaire (CSQ; Fig. 2) between each session. The CSQ records the details of a problematic interpersonal encounter that the patient has experienced. The therapist uses CSQs to teach the patient the social problem-solving skills that are characteristically absent or dormant in people with chronic depression. The goal is to teach the patient how to complete the steps of the situational analysis until they can successfully submit at least two accurately recorded and revised situational analyses without reference to the therapist.

Fig. 2 Elicitation phase of situational analysis using the Coping Survey Questionnaire. © James P. McCullough, Jr., Virginia Commonwealth University.
Situational analysis consists of two phases: elicitation and remediation (Box 4).
Box 4 The stages of the situational analysis
Elicitation phase
-
1 Describe what happened in this situation
-
2 Describe your interpretation(s) of what happened
-
3 Describe what you did in this situation
-
4 Describe how the event came out for you (What was the actual outcome?)
-
5 Describe how you would have wanted the event to come out for you (What was your desired outcome?)
-
6 Did you get what you wanted here? (Why? Why not?)
Remediation phase
-
1 How did each interpretation contribute to your obtaining your desired outcome?
-
2 How did your behaviour help you obtain the desired outcome?
-
3 What have you learned in going through this situational analysis?
-
4 How does what you have learned in this situation apply to other similar situations?
The elicitation phase is an assessment and diagnostic tool for both therapist and patient. As patients are guided through a behavioural analysis of a problematic interpersonal exchange, the forms and consequences of dysfunctional behavioural, cognitive and interpersonal pathology are distilled and revealed. The CSQ in Fig. 2 shows the results of the elicitation phase from a situational analysis brought to the session by Morag.
Once this phase is complete, these pathological patterns of thinking, behaving and relating are targeted in the remediation phase. The dysfunctional patterns are revised until new action tendencies establish themselves and previously problematic exchanges with the social environment (other people) are brought to more desirable or functional conclusions. The remediation phase of the situational analysis introduced in Fig. 2 is outlined in Box 5.
Box 5 Remediation phase of situational analysis using the Coping Survey Questionnaire
The link question between the elicitation phase and the remediation phase is ‘why?’ Having ascertained that Morag did not get what she wanted (her desired outcome), for her the question is ‘why not?’ Without elaboration the therapist directs Morag's attention back to the situation and to her interpretations in the first instance.
In the elicitation phase these interpretations (‘reads’) were accepted as Morag had offered them and written them down. In the remediation phase the therapist's role is to return to these interpretations and help the patient see that they have consequences in the sense that they act as a rudder for behaviour. Each interpretation is examined in turn.
Step 1A Reviewing the interpretations

| Therapist | So Morag, let's get back to the situation and see what you might have changed to get what you wanted. The first thing we will look at is the way you interpreted or read the situation. In your first interpretation you said ‘I'm useless at speaking to people.’ Is this read relevant and accurate? |
| Morag | No.[after a prolonged pause] It's too general. |
| Therapist | What could you have thought during the initial part of the situation? Let me remind you of your description: ‘I attended a meeting with my colleagues. My supervisor went round the table asking people in turn if they had any problems they wanted to bring up’. |
| Morag | [after a pause] I could have thought ‘I've spoken in front of all these people before’. |
| Therapist | Is that accurate and relevant to the situation? |
| Morag: | Yes. |
(This is a challenging question designed to focus the patient's attention on the consequences of thinking in generalised or situationally irrelevant ways. Discussion and exploration of the effects of this thinking often follows.)

| Therapist | In your second interpretation … [each interpretation is taken in turn and the above steps followed] |
Note: Interpretation 2 (‘They all thought I was odd and stupid’) is inaccurate and irrelevant. It includes mind-reading and emotional thinking. Interpretation 3 (‘It's part of my job and I should be able to do these things’) is both accurate and relevant.
Step 1B The action interpretation
(If there is no action interpretation among the patient's interpretations one is sought at this point.)

| Therapist | Nothing takes us to your desired outcome. What could you have thought? How could you have behaved? |
| Morag | I need to prepare the sentence in my head and then tell my supervisor ‘I have a problem’. |
| Therapist | If you had thought that, would you have got closer to your goal? |
| Morag | Yes I would. |
Step 2

| Therapist | If you had thought of the action interpretation you just mentioned how would your behaviour have changed? |
| Morag | I would have felt less on the spot, I could have rehearsed the statement in my head and been ready for my turn. I may not have frozen if I'd done that. |
| Therapist | If you had behaved in this way would you have got your desired outcome? |
| Morag | I think so, yes. |
Step 3

| Therapist | What have you learned here? |
| Morag | I need to practise in my head what I need to say at meetings and then say it. |
| Therapist | What do you need to do to allow that? |
| Morag | I need to be able to stay calm. |
| Therapist | We can look at ways to help you do that. |
Step 4
| Therapist | Can you think of any similar situation where you can apply what you have learned here? |
(Or the therapist could ask ‘How is this situational analysis similar to previous ones?’)
| Morag | This happens all the time – at work, with my parents, here … |
| Therapist | We have a lot to work on! |
Both the elicitation and remediation phases of situational analysis are complex and often difficult: the fictional example shown here is necessarily abbreviated.
People with chronic depression have been found to think prelogically and in a precausal manner. Clinically, this appears as a tendency to engage in generalised thinking, for example ‘I'm just useless – a total failure.’ In our experience the situational analysis technique helps to inhibit this by anchoring the analysis of problematic interpersonal exchanges in a discrete ‘slice of time’. This step also prevents the tendency of people with chronic depression to present different problems from a range of separate interactions as if they were contiguously related. In such a situation, the therapist ends up ‘fighting fires’, with little opportunity to complete a cycle of problem-solving; much is explored, little is remediated and shared hopelessness may blossom. This hopelessness is ameliorated when, in learning to carry out the situational analysis, the patient begins to discern that there is order and pattern in seemingly chaotic events over which they perceive they have little or no influence.
Disciplined personal involvement
In CBASP, the therapist is expected to take a non-neutral role: first, the psychological needs of individuals with chronic depression require this and, second, CBASP is a learning acquisition model of therapy. This role is achieved through the therapist's ‘disciplined personal involvement’ in sessions. The therapist exhibits appropriate interpersonal behaviour and uses ‘contingent personal responsivity’ (Box 2 and below) in response to any maladaptive behaviour on the part of the patient during a session (this response has been called the consequation of behaviour). The healing of any early traumatic experiences is accomplished when the patient is able successfully to discriminate the therapist from the individuals guilty of maltreating them in the past (Reference McCulloughMcCullough, 2006).
Most therapists find the concept and practice of disciplined personal involvement is one of the most challenging aspects of CBASP. They must be willing to express both the positive and negative feelings and reactions that arise in interactions during sessions. People with chronic depression come to therapy with a well-established dysfunctional interpersonal style. This style may have a destructive impact on their social environment. A significant problem is that they are often genuinely unaware of the interpersonal effects they have on others: they simply do not understand their inextricable connection to others. In CBASP, patients are taught to recognise the interpersonal consequences of their behaviour. Once they are able to see the effects they have on others, they achieve a level of psychosocial functioning that is labelled ‘perceived functionality’.
Through the medium of disciplined personal involvement, CBASP seeks to provide therapists with a clearly defined role and operationalised procedures and goals for confronting the dysfunctional interpersonal style typical of a person with chronic depression (Fig. 1). This is done using two techniques: the interpersonal discrimination exercise to heal early trauma, and contingent personal responsivity to modify interpersonal behaviour that is destructive. The therapist has two sources of information that inform their use of these techniques: the ‘transference hypothesis’, which we have already discussed, and the Impact Message Inventory.
The Impact Message Inventory
In behavioural terms both patient and therapist have a stimulus value in the therapy arena (and in their everyday social environment). Social behaviour operates on or influences the social environment (stimulus properties) and ‘pulls for’ (elicits) complementary responses (consequences) from others in the environment. For example, hostile ways of speaking and behaving pull for hostile responses; friendly ways of speaking and behaving pull for friendly responses. Passive ways of speaking or behaving generally pull for a dominant or ‘taking charge’ response from others (Reference KieslerKiesler, 1983). One way of assessing a patient's stimulus value is through the Impact Message Inventory (IMI; Reference Kiesler and SchmidtKiesler & Schmidt, 1993), a 56-item self-report inventory that provides a graphical representation in eight domains of the patient's stimulus value.
Case scenario: Morag
The IMI data for Morag were plotted and showed peak scores on the ‘hostile’, ‘hostile-submissive’ and ‘submissive’ domain. The peak score on the ‘hostile’ domain makes it likely that she will try to keep the therapist at a distance; the therapist might well be annoyed by her hostility, perhaps hoping that she will miss sessions or longing for the therapy to end. The therapist's task is to avoid responding in kind but instead to help Morag relate to a person (the therapist) who will not be pushed away or reciprocate the hostility.
Contingent personal responsivity
Contingent personal responsivity provides the therapist with the opportunity to direct the patient's attention to the impact of their behaviour on the therapist (and therefore on others). The therapist's interpersonal response to the patient's behaviour is made explicit. The therapist reacts contingently to the patient in a way that acknowledges the impact of the patient's behaviour and draws attention to its consequences, for example: ‘When you said that, I felt devalued [pushed away/ignored/attacked, etc.]’. The therapist then explores the issue with the patient: ‘Why do you want to devalue me or my efforts [push me away, etc.]?’ The aim is to focus attention on the consequences of maladaptive social behaviour, to pinpoint alternative adaptive behaviour and to give the patient continual and contingent feedback in response to adaptive interpersonal behaviour.
The interpersonal discrimination exercise
As noted above, whenever a transference hot spot is experienced the therapist administers the interpersonal discrimination exercise. We can illustrate this procedure using the example of Morag, for whom the following transference hypothesis was generated: ‘If I get close to Mr Swan and let him know how I feel then he will punish, reject or ridicule me’.
Case scenario: Morag
Working with Morag in early sessions was problematic as she found it very difficult to express her thoughts or needs. Both she and the therapist were uncomfortable with the slow progress, long silences and the discomfort caused by requests for information about her thoughts and opinions about people in her life. A hot spot occurred when Morag stated that she was unable to express her opinions about her problems with depression. The transference hypothesis was implicated. An interpersonal discrimination exercise was administered following the steps outlined below.
Step 1 The therapist highlighted that this would be the first time they were going to try an interpersonal discrimination exercise.
Step 2 Morag was asked to concentrate on not being able to express her opinions about her depression.
Step 3 The therapist asked Morag to focus on her mother's reaction (as a significant other person implicated in this domain). Care must be taken to avoid nudging the patient into an observer role. Thus, the therapist asked a direct question: ‘Remember what you just said. How would your Mum have reacted if you told her how you thought?’
Step 4 Morag was then asked to focus on the emotive–behavioural–cognitive impact of her mother on Morag and the therapist through her reaction.
[Steps 3 and 4 were repeated for how her father, as a second significant other, would have reacted.]
Step 5 The therapist asked Morag to focus on his reaction, noting both verbal and non-verbal behaviours: ‘What is my reaction when you express your thoughts or opinions to me? How do I react when you answer my questions?’
Step 6 Morag was asked to focus on the emotive–behavioural–cognitive impact of the therapist on the two of them through his reaction.
Step 7 Morag was invited to compare and contrast the different reactions. This is the interpersonal discrimination question: ‘How do our reactions compare – what are the similarities and what are the differences?’ She was given time to compare and contrast the two differing behavioural consequences of the same behaviour (expressing opinions and thoughts). At this point the patient's distress is often lessened as they can see that the therapist has not reacted in the same way as the significant other. What is wanted is a clear discrimination between the experience with the significant other and that with the therapist.
Step 8 The therapist then asked the final discrimination question: ‘What are the implications for our relationship now that you can see I have not responded to you in the same way as your Mum?’ After a considerable period of puzzling it through, Morag was able to say ‘I think I might be able to tell you what I'm thinking and feeling more easily. You ask questions and then you listen. You seem interested.’
Over the course of treatment, the message of the interpersonal discrimination exercise becomes clearer: ‘You can have a novel interpersonal reality with me, your therapist. You can use this relationship with me to learn different and more productive ways of managing your relationships.’
Discussion
McCullough's conceptualisation of the aetiology and cognitive, behavioural and emotional consequences of chronic depression provides helpful insights into why working within rational-empirical paradigms with individuals who have chronic depression does not confer the same clinical benefits as seen when working in this way with people with acute, mild-to-moderate unipolar depression. Withdrawal and perceptual disengagement from the environment, in combination with deficits in formal operations thinking, make it very difficult for people with chronic depression to fully engage with the range of psychological therapies usually offered.
CBASP is designed directly to address these problems by a focus on skills acquisition in social problem-solving, and reorientation or reconnection with the environment through specifying and analysing troublesome patterns of behaviour, thinking and emoting. In CBASP, patients are persistently engaged with the consequences of these detrimental patterns and are helped to define more desirable outcomes in the social realm. Patients are taught a range of skills familiar to psychological therapists, to aid them in realising desired outcomes or more salubrious consequences in their relationships.
Situational analysis forms the cornerstone of CBASP. The instruction to ‘stay in the slice of time’ and not allow generalisations or intellectualisation seems to be both important and effective. Staying in the slice of time allows individuals to engage with the consequences of their behaviour and it is this engagement that is thought to drive behavioural change and subsequent clinical improvement. It also seems to help prevent the all too frequent generalised discussions that arise with people who are chronically depressed and allows real and accurate discussion and analysis of what happens in specific situations and the consequences of particular behaviours.
The most radical and challenging element of CBASP is the concept and practice of disciplined personal involvement. Professor McCullough asks us to consider that the ‘traditional’ model for psychotherapy is a ‘one-person psychology’. The patient is revealed and their behaviour and emotional state are focused on. In CBASP, McCullough advocates a ‘two-person psychology’: the patient and the therapist both have stimulus value; the relationship is consciously and transparently used as a platform for the patient to have opportunities to access clear feedback on the consequences of their behaviour on others (the therapist). The relationship is then used to help the patient to remedy problematic patterns of relating. Clinicians are therefore required to express their positive and negative responses to their patients. At strategically chosen interpersonal hot spots, the therapist aims to become an ‘interpersonal obstruction’ in the face of the patient's discomfort and associated manoeuvres to placate or withdraw from the therapist. To achieve this, CBASP therapists need to be very experienced and confident in working with people who have chronic depression. In addition to experience, our belief is that potential CBASP therapists require focused training and supervision with an accredited CBASP practitioner.
CBASP has been a long time in evolution, and it continues to evolve (Box 6). It should not be mistaken for a variant of cognitive–behavioural therapy (CBT) or interpersonal psychotherapy. Its theoretical underpinnings and focus are quite different. CBASP is not a third-generation CBT. However, therapists with prior experience of structured therapies such as CBT or interpersonal psychotherapy are most likely to embrace and learn the application of CBASP in their clinical work.
Box 6 Information sources and manuals
-
• Treatment for Chronic Depression: Cognitive Behavioral Analysis System of Psychotherapy (Reference McCulloughMcCullough, 2000): The standard text describing the model and method of CBASP
-
• Skills Training Manual for Diagnosing and Treating Chronic Depression. Cognitive Behavioral Analysis System of Psychotherapy (Reference McCulloughMcCullough, 2001): A series of exercises to help therapists to learn to administer the therapy model effectively
-
• Patient's Manual for CBASP (Reference McCulloughMcCullough, 2003): A concise guide intended to prepare patients for CBASP once the diagnosis of chronic depression has been made
-
• Treating Chronic Depression with Disciplined Personal Involvement: Cognitive Behavioral Analysis System of Psychotherapy (CBASP) (Reference McCulloughMcCullough, 2006): A challenge to the stance of therapist neutrality towards patients, specifically those with chronic depression
-
• http://www.cbasp.org Information on the development of CBASP, patient demographics, research, books, training events
Declaration of interest
A. H. has previously received educational sponsorship and honoraria for presentations from various pharmaceutical companies who market medications used in the pharmacological treatment of chronic depression in the UK. Both J. S. and A. H. have undertaken a 1-week training course run by James P. McCullough in Richmond, Virginia.
MCQs
-
1 The founder of CBASP is:
-
a Bandura
-
b Skinner
-
c Kiesler
-
d McCullough
-
e Nemeroff.
-
-
2 Key procedural stages of situational analysis include:
-
a teaching the patient to interpret what is happening in specific slices of time during the situation
-
b telling the patient why the actual outcome differed from the desired outcome
-
c getting the patient to describe the emotions relating to what they did and/or said in the situation
-
d listing cognitive errors that become apparent during the situation analysis
-
e defining the desired outcome, independent of whether it is realistic or not.
-
-
3 CBASP:
-
a is a type of CBT
-
b has been shown to be effective for a range of psychiatric disorders
-
c is less effective where a history of early-life adversity or abuse exists
-
d replaces the need for antidepressant medication
-
e employs familiar CBT strategies such as assertiveness and problem-solving.
-
-
4 Chronic depression:
-
a is not associated with an increased rate of suicide
-
b is defined as a depressive illness lasting at least 1 year without any period of remission
-
c includes dysthymia as a sub-classification
-
d has been found to respond to various psychological therapies
-
e has been shown to be effectively treated by CBASP only when this therapy is used in combination with antidepressant medication.
-
-
5 Within the practice of CBASP:
-
a free association is often involved
-
b about 70% of the treatment session time should be spent on situational analysis
-
c the diagnosis is not important
-
d the consequation of behaviour is seen as detrimental to recovery from chronic depression
-
e the patient is not expected to perform any ‘between sessions work’ or homework.
-
MCQ answers

| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | F | a | F | a | F | a | F |
| b | F | b | F | b | F | b | F | b | T |
| c | F | c | F | c | F | c | T | c | F |
| d | T | d | F | d | F | d | F | d | F |
| e | F | e | T | e | T | e | F | e | F |
Acknowledgement
We would like to acknowledge the contribution of Professor James P. McCullough, Jr in the writing of this article.






eLetters
No eLetters have been published for this article.