Introduction
Are loneliness, social isolation and living alone the same or different? Researchers and theorists have long hypothesised that loneliness, social isolation and living alone are separate constructs despite overlapping features (Victor et al. Reference Victor, Scambler, Bond and Bowling2000). The identification of typologies of loneliness and social isolation has long been of interest to researchers (Townsend Reference Townsend, Shanas, Townsend, Wedderburn, Friis, Milhoj and Stehouwer1980; Tunstall Reference Tunstall1966; Weiss Reference Weiss1973). Identifying typologies tells us how these concepts are related and can help us to identify better those people who may be at high risk of the adverse consequences of loneliness and social isolation such as poor health and wellbeing (Heinrich and Gullone Reference Heinrich and Gullone2006; Luanaigh and Lawlor Reference Luanaigh and Lawlor2008; Valtorta et al. Reference Valtorta, Kanaan, Gilbody, Ronzi and Hanratty2016b). Andersson (Reference Andersson1986) proposed a four-fold typology to summarise the relationship between loneliness and social isolation: neither lonely nor isolated, isolated but not lonely, lonely but not isolated, and both lonely and isolated. However, little research has explicitly examined whether these typologies may reflect the lived experience of older adults nor how different typologies might link with physical and mental health.
The concepts of loneliness, social isolation and living alone
Loneliness has been conceptualised in a number of different ways: as a discrepancy between a persons desired and perceived quality and quantity of social relationships (Walton et al. Reference Walton, Shultz, Beck and Walls1991), a perceived deprivation in social contact (Townsend Reference Townsend, Shanas, Townsend, Wedderburn, Friis, Milhoj and Stehouwer1980), perceived social isolation (Hawkley and Cacioppo Reference Hawkley and Cacioppo2010) or a lack of people with whom to share emotional and social experiences (Rook Reference Rook1984). On the other hand, social isolation has been conceptualised as the measure of a person's integration and meaningful communication with their community, family and friends (Victor et al. Reference Victor, Scambler, Bond and Bowling2000), the objective experience of being alone (Hawkley and Cacioppo Reference Hawkley and Cacioppo2010), a lack of meaningful social ties (Lubben and Gironda Reference Lubben, Gironda, Berkman and Harootyan2003) or a lack of integration with social networks (Rook Reference Rook1984). Whilst these definitions suggest conceptual overlap, research shows there is only a moderate association between loneliness and social isolation (Golden et al. Reference Golden, Conroy, Bruce, Denihan, Greene, Kirby and Lawlor2009).
Social isolation and loneliness can also be theoretically differentiated from living alone, a simple enumeration of household size (Victor et al. Reference Victor, Scambler, Bond and Bowling2000). The evidence for the relationship of loneliness and social isolation with living alone is mixed, with studies variously reporting no association between loneliness (Zebhauser et al. Reference Zebhauser, Hofmann-Xu, Baumert, Häfner, Lacruz, Emeny, Döring, Grill, Huber and Peters2014) or social isolation (Larson, Zuzanek and Mannell Reference Larson, Zuzanek and Mannell1985) and living alone, high levels of loneliness/isolation amongst those living alone (Tunstall Reference Tunstall1966) or that living alone is a strong risk factor for loneliness (Sundström et al. Reference Sundström, Fransson, Malmberg and Davey2009). Despite possible theoretical differences, living alone has been included in measures of social isolation (Shankar et al. Reference Shankar, McMunn, Banks and Steptoe2011, Reference Shankar, Hamer, McMunn and Steptoe2013; Steptoe et al. Reference Steptoe, Shankar, Demakakos and Wardle2013b; Victor et al. Reference Victor, Scambler, Bond and Bowling2000) rather than being evaluated as a potentially separate category.
Loneliness, social isolation, living alone and health
Existing theory and evidence suggest that a more nuanced examination of the relationships between these three concepts could be useful, especially in developing our understanding of the association of these issues with health and wellbeing outcomes. Previous qualitative research provides us with rich and meaningful data on the lived experiences of loneliness, social isolation and living alone. They indicate that loneliness and social isolation are complex individual experiences which have different perceived causes and consequences (Cloutier-Fisher, Kobayashi and Smith Reference Cloutier-Fisher, Kobayashi and Smith2011; Dahlberg Reference Dahlberg2007). However, quantitative work has typically defined loneliness and social isolation in predetermined, binary and stringent ways (Shankar et al. Reference Shankar, McMunn, Banks and Steptoe2011, Reference Shankar, Hamer, McMunn and Steptoe2013; Steptoe et al. Reference Steptoe, Shankar, Demakakos and Wardle2013b) that may not accurately encapsulate the complexity of these experiences.
Previous work argues that researchers, policy makers and practitioners need to appreciate how we define and measure loneliness, isolation and living alone so we can better identify how these experiences might be linked with important health and wellbeing outcomes (Perissinotto and Covinsky Reference Perissinotto and Covinsky2014; Valtorta and Hanratty Reference Valtorta and Hanratty2012; Valtorta et al. Reference Valtorta, Kanaan, Gilbody and Hanratty2016a).
Loneliness, living alone and social isolation are all independently associated with similar health outcomes such as depression (Alpass and Neville Reference Alpass and Neville2003; Dean et al. Reference Dean, Kolody, Wood and Matt1992; Hawthorne Reference Hawthorne2008), poorer cognitive functioning (Bassuk, Glass and Berkman Reference Bassuk, Glass and Berkman1999; Cacioppo and Hawkley Reference Cacioppo and Hawkley2009; Zunzunegui et al. Reference Zunzunegui, Alvarado, Del Ser and Otero2003), cardiovascular disease (Orth-Gomér, Rosengren and Wilhelmsen Reference Orth-Gomér, Rosengren and Wilhelmsen1993; Valtorta et al. Reference Valtorta, Kanaan, Gilbody, Ronzi and Hanratty2016b), poorer self-rated health (Kharicha et al. Reference Kharicha, Iliffe, Harari, Swift, Gillmann and Stuck2007; Lee et al. Reference Lee, Jang, Lee, Cho and Park2008; Nummela, Seppänen and Uutela Reference Nummela, Seppänen and Uutela2011), worsened physical functioning (Iliffe et al. Reference Iliffe, Kharicha, Harari, Swift, Gillmann and Stuck2007; Kharicha et al. Reference Kharicha, Iliffe, Harari, Swift, Gillmann and Stuck2007; Perissinotto, Cenzer and Covinsky Reference Perissinotto, Cenzer and Covinsky2012) and lifestyle (Alpass and Neville Reference Alpass and Neville2003; Davis et al. Reference Davis, Murphy, Neuhaus and Lein1990).
When researchers examine loneliness and social isolation with health simultaneously results are often mixed, with studies reporting loneliness and social isolation being associated with different health outcomes (Cornwell and Waite Reference Cornwell and Waite2009; Elovainio et al. Reference Elovainio, Hakulinen, Pulkki-Råback, Virtanen, Josefsson, Jokela, Vahtera and Kivimäki2017; Holwerda et al. Reference Holwerda, Deeg, Beekman, van Tilburg, Stek, Jonker and Schoevers2013; McHugh et al. Reference McHugh, Kenny, Lawlor, Steptoe and Kee2017; Shankar et al. Reference Shankar, McMunn, Banks and Steptoe2011; Steptoe et al. Reference Steptoe, Shankar, Demakakos and Wardle2013b). However, there is a lack of work that examines how the experiences of living alone, loneliness and social isolation combine, and how these groups might be linked with health.
One way to determine whether meaningful typologies based on shared characteristics of social isolation, loneliness and living alone can be uncovered quantitatively is to use data-driven methods such as Latent Class Analysis (LCA) as a method to identify distinct sub-groups based on social relationships in older populations (Burholt, Dobbs and Victor Reference Burholt, Dobbs and Victor2017; Ellwardt, Aartsen and van Tilburg Reference Ellwardt, Aartsen and van Tilburg2016). The first aim of our study was to identify groups of older people based on shared characteristics of loneliness, social isolation and living alone using LCA. The second aim of this study was to determine how each of these groups differed in terms of health and socio-demographic characteristics.
Methods
Data-set and participants
This study utilised data from Wave 7 of the English Longitudinal Study of Ageing (ELSA). ELSA is a longitudinal prospective cohort study of adults aged 50 or older that has been ongoing since 2002 (Wave 1). Baseline participants were sampled from eligible participants who had taken part in the Health Survey for England (HSE) in either 1998, 1999 or 2001 (Steptoe et al. Reference Steptoe, Breeze, Banks and Nazroo2013a). Core data collection for the ELSA study takes place every two years. As well as following-up baseline participants, refreshment sampling (i.e. sampling new participants from HSE) for ELSA has taken place at Waves 3, 4, 6 and 7. Our analysis utilises Wave 7, the most recently published wave of ELSA (data collection 2014–2015). A total of 8,249 people took part in this wave. We excluded people aged less than 50 (N = 76), those who had a proxy answer on their behalf (N = 597) or had incomplete data for indicators of loneliness, social isolation and living alone (N = 544), giving an analytic sample of 7,032 (mean age = 67.3; 55% female).
Indicators of loneliness and social isolation
The indicators of loneliness and social isolation used for our analysis were based upon previous work from ELSA exploring these topics. Our indicators of loneliness were the three questions from the three-item University of California, Los Angeles (UCLA) Loneliness Scale (Hughes et al. Reference Hughes, Waite, Hawkley and Cacioppo2004): How often do you feel you lack companionship? How often do you feel left out? How often do you feel isolated? Responses were: hardly ever/never, sometimes or always.
We used the social isolation index developed for use with ELSA (Shankar et al. Reference Shankar, McMunn, Banks and Steptoe2011) based on the five items of:
1. Household composition (living alone, living in multi-person household).
2. Participation in societal/social activities (not involved/involved). This included participation in any social/recreational activities (e.g. evening classes, social clubs and sports clubs), societal (e.g. political parties or tenants groups) or voluntary activities.
3. Communication with family (more than once a month/less than once a month/no family).
4. Communication with relatives (more than once a month/less than once a month/no family).
5. Communication with friends (more than once a month/less than once a month/no family).
Socio-demographic characteristics
We examined the following socio-demographic characteristics: age, sex (male/female), ethnicity (white/non-white), marital status (married/not married/divorced or separated/widowed), employment status (employed/unemployed/retired), education (no qualifications/high school or college-level qualifications/higher education qualifications), net wealth minus pension (quintiles 1 and 2/quintiles 3–5) – an indicator of wealth used in similar studies (Shankar et al. Reference Shankar, McMunn, Banks and Steptoe2011).
Health-related outcomes (physical and mental health)
Functioning was assessed by calculating the number of issues with the following activities of daily living (ADLs): getting out of bed, dressing, walking, bathing, eating and/or using the toilet. Groups were categorised according to whether they experienced no issues or one or more issues with ADLs in line with previous work (Gale, Cooper and Aihie Sayer Reference Gale, Cooper and Aihie Sayer2015).
Number of chronic conditions involved summing the number of chronic conditions people reported having from a list of 19 included in ELSA (for a list of conditions, see Dhalwani et al. Reference Dhalwani, O'Donovan, Zaccardi, Hamer, Yates, Davies and Khunti2016). Conditions were categorised as none, one, or two or more (multi-morbidity) (Dhalwani et al. Reference Dhalwani, Zaccardi, O'Donovan, Carter, Hamer, Yates, Davies and Khunti2017).
Self-rated health was assessed using a single item where people rated their own health on a five-point scale that ran from excellent to poor. Responses were dichotomised as excellent/very good/good or fair/poor in line with previous work (Badawi et al. Reference Badawi, Pagé, Smith, Gariépy, Malla, Wang, Boyer, Strychar, Lesage and Schmitz2013).
Depressive symptoms were measured using the eight-item Center for Epidemiological Studies Depression Scale (CES-D 8). This item measures the past week experience of eight indicators of depressive symptomatology (responses yes/no). For the sake of this analysis, the item on loneliness (‘I have felt lonely’) was removed in line with previous work that has examined loneliness and depressive symptoms using ELSA (Shankar et al. Reference Shankar, McMunn, Banks and Steptoe2011). Responses were then categorised as high (⩾4) versus low (<4) depressive symptoms in line with previous work (Au et al. Reference Au, Smith, Gariépy and Schmitz2015; Hamer et al. Reference Hamer, Molloy, de Oliveira and Demakakos2009). However, as this cut-point was validated for the full eight-item scale we also ran sensitivity analyses with a cut-point of 3 (cut-point identified for the 10% with the highest depressive symptom score) to check our results.
Analysis
The indicators of loneliness, social isolation and living alone were grouped into meaningful groups using LCA (Latent Gold 5.0). LCA uses mathematical modelling to group categorical and/or continuous variables into classes (in this paper referred to as groups) based on likelihood estimates (Hagenaars and McCutcheon Reference Hagenaars and McCutcheon2002; McCutcheon Reference McCutcheon1987; Vermunt and Magidson Reference Vermunt, Magidson, Hagenaars and McCutcheon2002). These classes represent groupings of data where people responded similarly to our indicators of loneliness, social isolation and living alone. To determine the optimal number of groups to derive we compared model fit from one to ten groups (run with 10,000 iterations). We determined the best model fit by examining the Bayesian Information Criteria (BIC), log-likelihood ratio (LLR), p-value and number of parameters. The model that demonstrated parsimony between the lowest number of parameters, highest p-value, and lowest BIC and LLR was chosen.
Once the optimal number of groups was identified, we examined the latent (previously unobserved) shared loneliness, social isolation and living alone characteristics that defined each group. Groups were then compared on socio-demographic characteristics and health-related outcomes using chi-squared analysis for categorical variables and one-way analysis of variance for continuous variables. We then ran logistic regression analyses to examine the relationship between group membership and each health and wellbeing outcome (issues with ADLs, self-rated health, multi-morbidity and depressive symptoms) by comparing all groups who reported loneliness, isolation and/or living alone to a reference group that was neither lonely nor isolated. Logistic regression analyses were first run unadjusted and then adjusted for socio-demographic characteristics (age, sex, marital status, wealth, employment and education). All analyses were conducted with SPSS 23.0.
Results
LCA: identifying groups based on shared loneliness and isolation characteristics
The LCA showed that the lowest BIC value was demonstrated by the seven-group model (see Table 1), although the value for the six-group model was comparable. As the number of groups increased, the LLR indicated that model fit improved (see Table 1), however, the number of parameters indicated that fewer groups was preferable whilst the p-value indicated any model fit from three groups onwards had a good fit. We used the six-group model as it demonstrated the greatest parsimony between the four model-fit indicators (for model-fit statistics, see Table 1).
Table 1. Model fit based on the number of groups to which the data are fitted
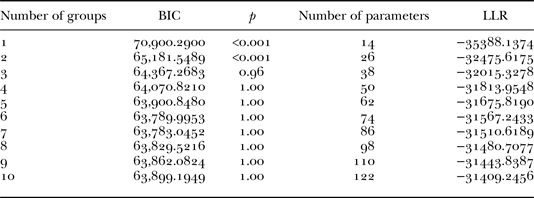
Notes: BIC: Bayesian Information Criteria. LLR: log-likelihood ratio. Lower numbers for indicators of model fit (BIC and LLR) indicate better model fit. Higher p-values also indicate better model fit. The best match between model fit and p-values that results in the lowest number of parameters represents the optimum number of groups.
The six groups identified differed in terms of their likelihood to exhibit different loneliness and living alone characteristics (see Table 2) which we characterised as:
• Group 1: no loneliness or isolation (46.97% of sample).
• Group 2: moderate loneliness (17.19% of sample).
• Group 3: living alone (11.79% of sample).
• Group 4: moderate isolation (11.17% of sample).
• Group 5: moderate loneliness, living alone (9.03% of sample).
• Group 6: high loneliness, moderate isolation (with high likelihood of living alone) (3.85% of sample).
Table 2. Characteristics of the six groups (classes) uncovered with Latent Class Analysis
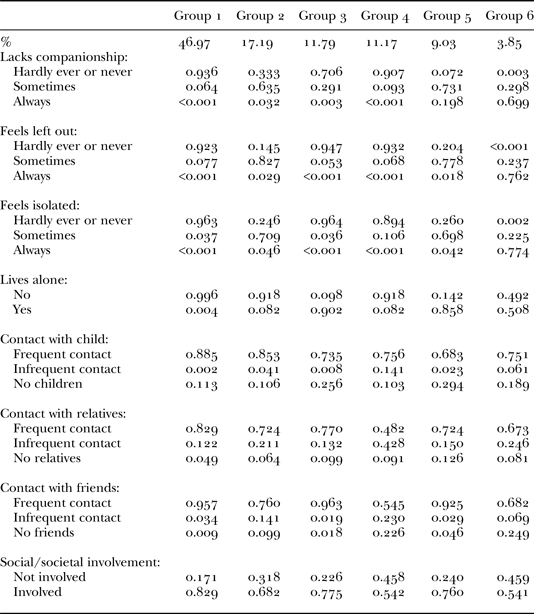
Notes: Group 1: no/low loneliness and isolation. Group 2: moderate loneliness. Group 3: lives alone. Group 4: moderate isolation. Group 5: moderate loneliness, lives alone. Group 6: high loneliness and moderate isolation. Results shown are likelihood estimates of members within each group responding in a particular way to each question (e.g. 0.171 indicates a 17.1% likelihood of giving that response/meeting that criteria). Results are rounded up to three decimal places and so not all results may add up to 100.
When differentiating groups based on loneliness, those groups with low loneliness were identified by a high likelihood of responding ‘hardly ever or never’ to loneliness questions. Those groups with moderate loneliness were identified by a high likelihood of responding ‘sometimes’ to loneliness questions. Finally, those groups with high loneliness were identified by a high likelihood of responding ‘always’ to loneliness questions. When differentiating groups based on isolation, low isolation was indicated by a high likelihood of frequent contact with friends, children and family plus having social/societal involvement. Groups with moderate isolation were identified by having a higher likelihood of reporting positively to one or two of the social isolation indicators such as indicating less-frequent contact with friends, relatives or children plus reporting no social/societal involvement. High social isolation would be indicated by a higher likelihood of responding positively to all indicators of social isolation.
The first group, almost half of the sample, had a high likelihood of not being lonely, socially isolated or living alone. Groups 2–4 demonstrated a high probability of experiencing one of our three factors. Group 2 had the highest likelihood of reporting moderate feelings of loneliness (responding sometimes to feelings of loneliness). Group 4 had the highest likelihood of being isolated as measured by contact with family, friends and children when compared with other groups. Group 3 had a high likelihood (90%) of living alone but a low likelihood of exhibiting loneliness or other isolation characteristics. Groups 5 and 6 demonstrated combinations of our three indicators. The fifth group showed a high likelihood of reporting moderate loneliness and living alone but a high likelihood of frequent contact with people and social/societal involvement and the highest likelihood of having no children (29%) or relatives (13%). The sixth group was most likely to report always being lonely, and also had a relatively high likelihood (51%) of living alone and not being involved in social/societal activities (46%). While not as high as Group 4, this group also demonstrated a greater likelihood of having less frequent contact with relatives (25%) and a relatively high likelihood of having no children (19%) and the highest likelihood of having no friends (25%).
Comparing groups on socio-demographic and health-related outcomes
We firstly compared groups on socio-demographic characteristics (see Table 3), and there were significant differences for age, gender, marital status, net wealth, employment and education between the six groups. In terms of age, Groups 3 and 5, both characterised by a high probability of living alone, were the oldest, the most likely to be retired and had the highest proportions of widows. Two of the three groups that had the highest proportion of married and employed participants had been characterised by a low likelihood of being lonely (Groups 1 and 4). However, the group that was characterised by moderate loneliness also had a high proportion of married and employed respondents (Group 2). Furthermore, the group characterised by experiencing no issues with loneliness or social isolation (Group 1) were the best educated. Those groups with the highest proportions of females were the groups most likely to live alone (Groups 3, 5 and 6) whilst the group with the highest proportion of males was the group that reported moderate isolation (Group 4). The group that had the highest proportion of respondents in the two lowest wealth quintiles and the highest proportion of unemployment was Group 6 (high loneliness, moderate isolation, high likelihood of living alone).
Table 3. Associations of group membership with socio-demographics, physical health and mental health
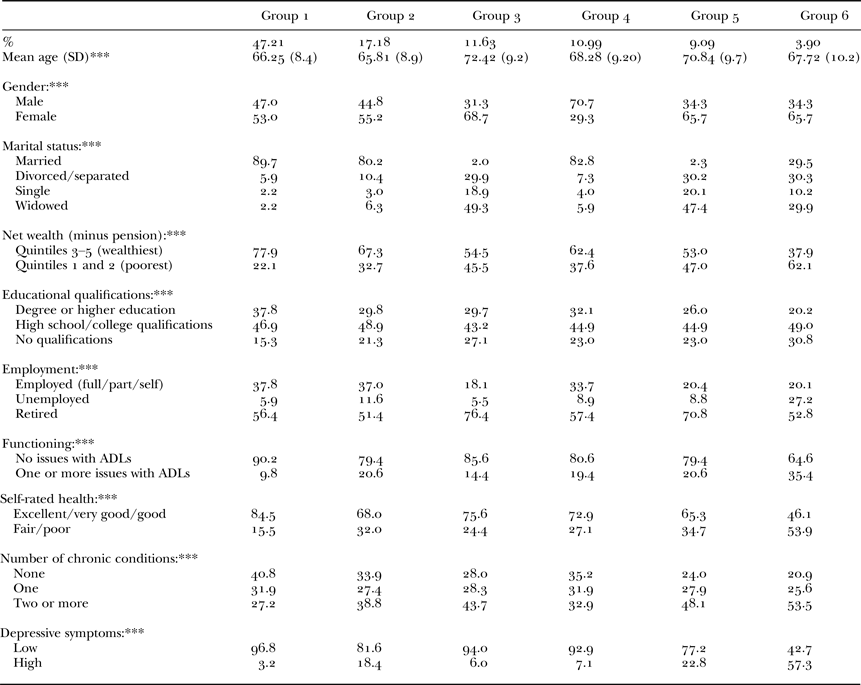
Notes: SD: standard deviation. ADL: activities of daily living. Group 1: no/low loneliness and isolation. Group 2: moderate loneliness. Group 3: lives alone. Group 4: moderate isolation. Group 5: moderate loneliness, lives alone. Group 6: high loneliness and moderate isolation.
Significance levels: *p < 0.05, **p < 0.01, ***p < 0.001.
There were also significant differences between the six groups for all four health and wellbeing outcomes: functioning (issues with ADLs), self-rated health, number of chronic conditions and depressive symptoms (see Table 3). The groups who reported isolation and/or loneliness (Groups 2, 4, 5 and 6) had the highest proportion of two or more issues with ADLs). This association was strongest in the group with both high loneliness and isolation (Group 5). All of the groups who experienced loneliness (Groups 2, 5 and 6) had a high likelihood of reporting fair/poor self-rated health (see Table 3) and this was most pronounced in the group characterised by high loneliness and social isolation. The three groups who had the highest proportion of multi-morbidity (two or more chronic conditions) were the group characterised by living alone (Group 3) and the two characterised by shared loneliness and social isolation (Groups 5 and 6). All groups experiencing isolation and/or loneliness were more likely to exhibit high depressive symptoms (Groups 2, 4, 5 and 6). This association was strongest in the group with high loneliness and isolation (Group 6).
We then ran a series of logistic regression analyses to determine the association between group membership and health and wellbeing, adjusting for socio-demographic characteristics. Crude and adjusted estimates are presented in Table 4. Group 1, no loneliness or isolation, was our reference category for both our crude and adjusted analyses. For all crude analyses, Groups 2–6 inclusive reported poorer outcomes on all four physical and mental health outcomes. All associations were attenuated after adjustment for Group 3 (lives alone). Furthermore, the associations between Group 4 with multi-morbidity was also attenuated after adjustment. The most pronounced associations between group and health was observed for high depressive symptoms, where all groups (except Group 3) were more likely than Group 1 to report high depressive symptoms, and this was particularly pronounced in the group with high loneliness and isolation (Group 6).
Table 4. Logistic regression analyses of association between group membership and physical and mental health
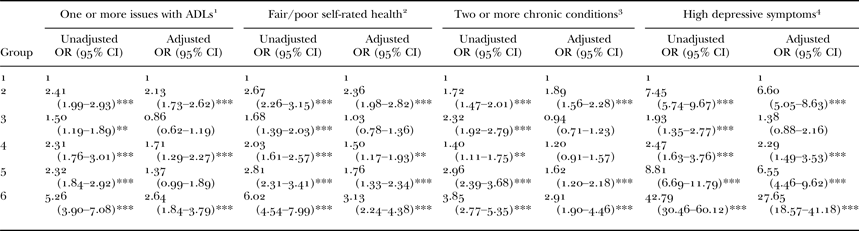
Notes: ADL: activities of daily living. OR: odds ratio. CI: confidence interval. Group 1: no/low loneliness and isolation. Group 2: moderate loneliness. Group 3: lives alone. Group 4: moderate isolation. Group 5: moderate loneliness, lives alone. Group 6: high loneliness and moderate isolation. All adjusted models are adjusted for age, sex (male/female), marital status (married or partner/single/divorced or separated), employment (employed/unemployed/retired), qualifications (university or higher education/high school or college/no qualifications) and net non-pension wealth (top three quintiles/bottom two quintiles). 1. Reference group: no issues with ADLs (N in fully adjusted model = 5,975). 2. Reference group: excellent/very good/good self-rated health (N in fully adjusted model = 6,090). 3. Reference group: no chronic conditions (N in fully adjusted model = 6,088). 4. Reference group: low/no depressive symptoms as indicated by a score of <3 on the Center for Epidemiological Studies Depression Scale (N in fully adjusted model = 6,041).
Significance levels: *p < 0.05, **p < 0.01, ***p < 0.001.
Sensitivity analysis
As the cut-point we used for our depressive symptom analysis (⩾4) was based on a cut-off validated for the eight-item scale, we re-ran our analysis with a cut-point of ⩾3 to see what effect this had on our results. For our cross-tabulation analysis, the association between group membership and depressive symptoms remained highly significant (χ2(5, N = 6,970) = 691.9, p < 0.001). For the proportions of high depressive symptoms, see Table A in the online supplementary material.
When we re-ran the logistic regression analysis with the cut-off of 3, all results remained significant at the same level as when the cut-off was 4, even for unadjusted analyses (see Table B in the online supplementary material). Thus, using a cut-point of 4 produced comparable results to a cut-point of 3.
Discussion
Using clustering methodologies on a large data-set, we have been able to uncover meaningful sub-groups of older people based on shared characteristics of loneliness, living alone and social isolation in a community population of English older adults. Our results indicate that existing typologies that take into account the potential overlap or independence of social isolation and loneliness, such as the groupings suggested by Andersson (Reference Andersson1986), reflect the experience of older adults. However, our work develops this typology further by demonstrating the presence of groups characterised by a high prevalence of living alone. Our work also suggests that we need to differentiate between those experiencing loneliness or isolation, or in combination, and that the severity of those issues may also be important in defining different typologies, as suggested by Victor et al. (Reference Victor, Scambler, Bond and Bowling2000). Therefore, we suggest considering both the number of issues that people have (i.e. none, one issue independently, two or more issues in combination) and the severity of these issues (e.g. is loneliness moderate or severe in its intensity) will be important in defining different typologies in future work.
The largest single group identified within our sample did not experience social isolation, loneliness and did not live alone (Group 1). This group was mostly younger, married, wealthier, better educated and had fewer issues with health and wellbeing. This observation provides support to the idea that health and wellbeing are important correlates of loneliness and social isolation in older adults (Heinrich and Gullone Reference Heinrich and Gullone2006; Luanaigh and Lawlor Reference Luanaigh and Lawlor2008). It is possible that increased community and social contact could have helped this group to maintain their health, however, it could also be the case that this group do not experience loneliness and social isolation because they do not have any health issues (Berkman and Glass Reference Berkman, Glass, Berkman and Kawachi2000; Ferlander Reference Ferlander2007). Future research could examine the direction of causality between maintenance of health and lack of loneliness/social isolation. There is evidence suggesting that loneliness and social isolation are risk factors for the development of serious illness (Valtorta et al. Reference Valtorta, Kanaan, Gilbody, Ronzi and Hanratty2016b) and mortality (Elovainio et al. Reference Elovainio, Hakulinen, Pulkki-Råback, Virtanen, Josefsson, Jokela, Vahtera and Kivimäki2017; Holt-Lunstad et al. Reference Holt-Lunstad, Smith, Baker, Harris and Stephenson2015; Steptoe et al. Reference Steptoe, Shankar, Demakakos and Wardle2013b). However, evidence also suggests that poor health is also a risk factor for the development of loneliness (Victor et al. Reference Victor, Scambler, Bowling and Bond2005). Thus, examining longitudinal relationships between health and loneliness, isolation and living alone could be important.
When creating typologies, we have suggested it could be important to differentiate between groups who experience an issue independently or in combination with another issue. We identified two groups who lived alone. One of these groups only experienced living alone (Group 3), whereas the other group experienced living alone with moderate loneliness (Group 5). Both groups that lived alone were older than all other groups and were more likely to be widowed. However, Group 5 also reported loneliness despite a similar demographic profile to Group 3. When compared to the reference group, Group 5 had a higher likelihood of reporting depressive symptoms and poorer health whereas for Group 3, after adjustment for confounders, there was no association between group membership and health. Depressive symptoms (Barg et al. Reference Barg, Huss-Ashmore, Wittink, Murray, Bogner and Gallo2006; Cacioppo et al. Reference Cacioppo, Hughes, Waite, Hawkley and Thisted2006) and poorer health (Victor et al. Reference Victor, Scambler, Bowling and Bond2005) have previously been pointed to as important issues strongly associated with loneliness. Thus, it is possible the poorer health and mental wellbeing of Group 5 could be why this group also experiences loneliness. Future longitudinal work could further unpick the causality of this association.
The identification of Group 3 was also of theoretical and policy/practice interest. Previous theoretical conceptualisations of loneliness and isolation have differentiated these concepts from living alone, which is simply a measure of the type of household in which a person lives (Victor et al. Reference Victor, Scambler, Bond and Bowling2000). The social isolation index from which our indicators of social isolation used in this analysis were derived includes living alone (Shankar et al. Reference Shankar, McMunn, Banks and Steptoe2011). However, the identification of Group 3 supports the presupposition of Victor et al. (Reference Victor, Scambler, Bond and Bowling2000) that living alone can be differentiated from loneliness and other indicators of social isolation. Further investigation of Group 3 could also be particularly interesting to determine why, in the face of many of the socio-demographic risk factors for experiencing social isolation and loneliness such as living alone, widowhood, being female and older age (Pinquart and Sorensen Reference Pinquart and Sorensen2001a; Wenger et al. Reference Wenger, Davies, Shahtahmasebi and Scott1996), they are less likely to report being lonely or socially isolated.
We also identified two groups who experienced moderate loneliness (Group 2) and some isolation (Group 4) independently. Group 2 were broader similar to Group 1 in socio-demographic terms but had worse health outcomes. Previous work has indicated that loneliness is strongly associated with health status (Luanaigh and Lawlor Reference Luanaigh and Lawlor2008; Victor et al. Reference Victor, Scambler, Bowling and Bond2005), thus it is possible that poorer psychological and physical health explained the moderate loneliness that characterised Group 2. Group 4 was particularly notable as it had a higher proportion of males than all other groups. This could be because men are less likely to report (Pinquart and Sörensen Reference Pinquart and Sörensen2001b) or recognise (Borys and Perlman Reference Borys and Perlman1985) feelings of loneliness compared with women, or that they are more likely to experience social rather than emotional loneliness (Dahlberg and McKee Reference Dahlberg and McKee2014). Our work adds to pre-existing literature by indicating that gender may be an important factor to examine when separating out groups based on loneliness and social isolation.
We have suggested that alongside taking the broad threefold typologies into consideration, the severity of these experiences could be important in differentiating between groups. This is particularly evident for Group 6. This group had the most severe profile of loneliness and social isolation, and also had a high likelihood of living alone. This group had the most pronounced association with all indicators of physical and mental health. Previous work has indicated that loneliness and depression share a strong relationship (Barg et al. Reference Barg, Huss-Ashmore, Wittink, Murray, Bogner and Gallo2006; Cacioppo et al. Reference Cacioppo, Hughes, Waite, Hawkley and Thisted2006). Our work adds to this by showing, when compared with a group with low/no loneliness or isolation, that loneliness, living alone and social isolation are linked with depressive symptoms. Our work also suggests that as loneliness severity increases, the association with depressive symptoms increases, as hypothesised by Victor et al. (Reference Victor, Scambler, Bond and Bowling2000).
However, it is important to note that most groups who experienced either social isolation and/or loneliness were all more likely to have high depressive symptoms when compared with the group with no loneliness or isolation, even after we adjusted for socio-demographic variables. This indicates that mental wellbeing should be considered in all people who may be socially isolated or lonely. Past work indicates that loneliness and social isolation share different relationships with health outcomes (Cornwell and Waite Reference Cornwell and Waite2009; Holwerda et al. Reference Holwerda, Deeg, Beekman, van Tilburg, Stek, Jonker and Schoevers2013; Shankar et al. Reference Shankar, McMunn, Banks and Steptoe2011; Steptoe et al. Reference Steptoe, Breeze, Banks and Nazroo2013a). Our work adds to the research in this field by showing that when compared with a group with no loneliness or isolation, any group who experiences loneliness and/or social isolation are more likely to report poor health. This work also indicates identifying groups with differing characteristics of loneliness and social isolation using data-driven methodologies could represent an interesting avenue to tell us more about how loneliness, social isolation and living alone are linked with health.
Limitations and considerations for future work
There are methodological caveats to our findings. When interpreting these results it is important to note that LCA is an exploratory technique, and that model fit is not absolute. Both the number of groups examined and the characteristics of the groups were determined using likelihood estimates. It should be noted that there was considerable within-group heterogeneity for many of the indicators we examined, so while groups were identified as having a high likelihood of exhibiting certain characteristics, this is not to say every single person within this group definitively exhibited these characteristics (just that they were the group they were most likely to belong to based on their profile). Future work could use LCA methodologies within different populations to determine whether the proposed broad typologies are generalisable to different populations and samples. A related consideration for interpretation is that these groups were uncovered in a specific cohort, and may not generalise to other populations or cultures.
Measurement issues should also be considered. Both the loneliness and social isolation indicators examined were short, and likely would not capture the full complexity of experiences of social isolation or loneliness. There is also increasing evidence suggesting that the chronicity and changing nature of loneliness and social isolation are important issues to consider (Dahlberg et al. Reference Dahlberg, Andersson, McKee and Lennartsson2015; Dykstra, Van Tilburg and de Jong Gierveld Reference Dykstra, Van Tilburg and de Jong Gierveld2005; Victor and Bowling Reference Victor and Bowling2012), but we could not address them. Future research could address these limitations by re-running this analysis in a study with more comprehensive loneliness and isolation measures that take chronicity into account.
The indicators of social isolation used in this study have also been used by other researchers to operationalise differing theoretical constructs such as social connectedness (Cornwell and Waite Reference Cornwell and Waite2009) and social detachment (Jivraj, Nazroo and Barnes Reference Jivraj, Nazroo, Barnes, Banks, Nazroo and Steptoe2012; Tomaszewski and Barnes Reference Tomaszewski, Barnes, Banks, Breeze, Lessof and Nazroo2008). Thus, while we have used these items as indicators of social isolation, they could be indicating social connectedness, social detachment or other related concepts such as social exclusion, which future research could try to disentangle. Furthermore, it is important to determine whether isolation was an active or passive process. Qualitative work suggests that one can differentiate between voluntary and involuntary loneliness (Dahlberg Reference Dahlberg2007), and it is plausible to assume these different types of loneliness/isolation will have different associations with health and wellbeing. The cross-sectional nature of this analysis means we cannot infer causality. It is plausible that there is a bi-directional association of loneliness, living alone and social isolation with health and wellbeing, and we will explore this in our future work.
Conclusions and implications
Using LCA we have been able to uncover different groups based on shared experiences of loneliness, social isolation and living alone, showing the different experiences older adults can have. This has important implications for the creation of typologies based on loneliness, social isolation and living alone. Our work indicates considering the number of issues that people have (i.e. none, one, two or more) and then the severity of these is important in defining different typologies. However, in order to make use of these typologies it is important to replicate these results in different samples. We have shown that different groups share different associations with health and wellbeing. This work indicates that the lived experience of loneliness, social isolation and living alone in older adults is complex, and that taking the number of issues and severity of issues into account will be important for researchers and clinicians working with groups of older adults who may be experiencing these issues. It also demonstrates that living alone is conceptually separate from loneliness and isolation, and has limited utility as a measure of these complex concepts.
Supplementary material
To view supplementary material for this article, please visit https://doi.org/10.1017/S0144686X18000132.






