What exactly is comorbidity?
Comorbidity was first properly defined by Reference FeinsteinFeinstein in 1970 as ‘any distinct additional clinical entity that has existed or that may occur during the clinical course of a patient who has the index disease under study’. I think the important word in this definition is ‘distinct’. Comorbid disease is common, particularly in older people, in whom conditions such as osteoarthritis and hypertension often coexist but are genuinely quite independent, and the same applies to comorbid mental and physical disease such as schizophrenia and rheumatoid arthritis.
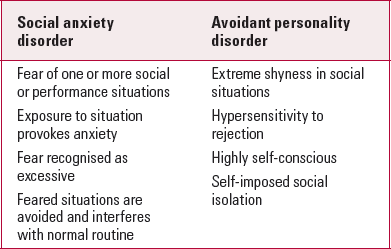
The main problem with comorbidity in psychiatric disorders is the difficulty in deciding what is distinct and what is not. When DSM-III was introduced in the USA (American Psychiatric Association 1980), diagnosis was almost reified, and many articles were published on the comorbidity of different psychiatric disorders. Thus, for example, a condition such as social anxiety disorder (formerly called social phobia) was found to be ‘highly comorbid’ with avoidant personality disorder, a completely different type of disorder in Axis II of the classification. But the simplest comparison of the definition of the two disorders shows there is bound to be an overlap (Table 1). This is an example of false comorbidity or even consanguinity (i.e. an intimate relationship between two disorders so that they are really one and the same (Reference TyrerTyrer 1996)).
TABLE 1 Main features of social anxiety disorder and avoidant personality disorder
Alternatives to comorbidity
Although there are some cogent arguments for placing, for example, social anxiety disorder and avoidant personality disorder in different parts of psychiatric classification, it would be ridiculous to maintain that they are distinct, and therefore comorbid, conditions. In the forthcoming ICD-11 classification, avoidant and anxious personality disorders will no longer be diagnostic entities (Reference Tyrer, Reed and CrawfordTyrer 2015), so this difficulty will not arise.
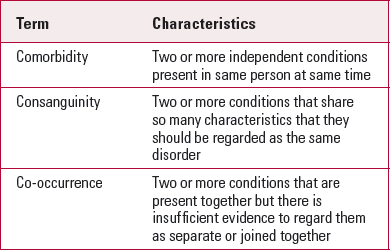
But there are many other examples of common mental disorders that are found together and these can be divided into three groups, determined by comorbidity, consanguinity and co-occurrence (Table 2).
TABLE 2 Suggested terminology for combinations of disorders
Comorbidity
Comorbid conditions are distinct disorders that occur together, according to Feinstein's definition. A common example is comorbid schizophrenia (or psychosis) and substance misuse. These are distinct conditions, but they are very often found together and have an impact on management, so there is selective attention given to this combined group (e.g. Reference Barrowclough, Haddock and WykesBarrowclough 2010).
Consanguinity
Consanguineous conditions are very closely related and should be thought of as one disorder. Because diagnosis in psychiatry is always open to change in the light of new evidence, there may be some merit, but not much, in keeping more than one diagnosis open while research is still being carried out. Examples of consanguineous disorders are dissociative amnesia and dissociative fugue, somatisation disorder and undifferentiated somatoform disorder, post-partum psychotic and (equivalent) other psychotic disorders, all categorical personality disorders, and simple schizophrenia and schizoid personality disorder. In many of these disorders there is one tiny element that is different between the two disorders, but not enough to give it separate diagnostic status. As one of the aims of good psychiatric classification is to promote greater utility, and as 90% of current diagnostic codes are very rarely used, there is room for rationalisation here.
Co-occurrence
Co-occurring conditions describe disorders that very commonly occur together and that may or may not be comorbid or consanguineous. In other words, the jury is still out on whether they should be joined or separate, but at present they can be thought of as interconnected in some way.
The best example of a common co-occurring disorder is mixed anxiety and depression. Anxiety and depression are different moods and so could be regarded as distinct, but they occur together more commonly than not. More importantly for the public health perspective, they have a much worse outcome together than when separate, and so cannot be ignored, however messy a combined diagnosis may appear to be. One solution that is increasingly being offered for such disorders is to define them in dimensional terms (Reference Das-Munshi, Goldberg and BebbingtonDas-Munshi 2008).
Conclusions
Diagnosis in psychiatry can be improved by thinking more carefully about the relationship between different disorders instead of putting them all into a junk box marked ‘comorbidity’.





eLetters
No eLetters have been published for this article.