Introduction
In low- and middle-income countries (LMICs), the discrepancy between the high prevalence rates of mental disorders on the one hand, and limited availability of mental health services on the other hand, is well documented (Kessler et al., Reference Kessler, Angermeyer, Anthony, De Graaf, Demyttenaere, Gasquet, De Girolamo, Gluzman, Gureje, Haro, Kawakami, Karam, Levinson, Medina Mora, Oakley Browne, Posada-Villa, Stein, Adley Tsang, Aguilar-Gaxiola, Alonso, Lee, Heeringa, Pennell, Berglund, Gruber, Petukhova, Chatterji and Üstün2007; WHO, 2009). As a response to this ‘treatment gap’ (Saxena et al., Reference Saxena, Thornicrof, Knapp and Whiteford2007), the World Health Organisation (WHO) launched the mental health Gap Action Programme (mhGAP, WHO, 2008) which aims at scaling up services for mental, neurological and substance use disorders, particularly in LMICs. Integrating mental health into primary health care (PHC) is a key component of the mhGAP programme. By integrating mental health into PHC, people in need of treatment can access services easily and be transferred to specialised care if necessary (Funk et al., Reference Funk, Saraceno, Drew and Faydi2008). Additionally, the mhGAP programme supports training community health workers in taking on limited tasks in the care of people with mental illness, such as case detection, referral to PHC and providing psychosocial support (Keynejad et al., Reference Keynejad, Dua, Barbui and Thornicroft2018).
This task-sharing approach (Patel, Reference Patel2009), in which care of people with mental illness is transferred from specialists to also involve primary care and community health workers, has been increasingly implemented in many LMICs over the past decade. WHO has developed an Intervention Guide (IG) for mental, neurological and substance use disorders in non-specialised health settings (WHO, 2016) in order to support this task-sharing process. A recent systematic review compiled evidence on the practical implementation of the WHO mhGAP-IG in LMICs and showed promising results (Keynejad et al., Reference Keynejad, Dua, Barbui and Thornicroft2018). Despite these efforts to enhance provision of mental health care in LMICs, and increasing evidence showing their positive results, many people with mental illness in LMICs still do not receive adequate treatment.
Mental health-related stigma is a key barrier to mental health care (Saxena et al., Reference Saxena, Thornicrof, Knapp and Whiteford2007). ‘Stigma’ can be conceptualised in terms of knowledge (i.e. ignorance or misinformation), attitude (i.e. prejudice) and behaviour (i.e. discrimination, violence, hostility and human rights abuses) (Thornicroft, Reference Thornicroft2006). A systematic review revealed stigmatising beliefs, attitudes and discriminatory behaviours among primary and specialised health care professionals in both high-income countries (HICs) and LMICs (Henderson et al., Reference Henderson, Noblett, Parke, Clement, Caffrey, Gale-Grant, Schulze, Druss and Thornicroft2014). Thus, even if people with mental illness overcome barriers and seek help in PHC, they are still at risk of being confronted with stigmatising beliefs, negative attitudes and discrimination, which hinders their right to adequate care.
Empirical evidence on how to reduce stigma in specific populations (e.g. health care workers) is generally scarce, as most studies merely assess stigma but do not test interventions to actually address it (Evans-Lacko et al., Reference Evans-Lacko, Courtin, Fiorillo, Knapp, Luciano, Park, Brunn, Byford, Chevreul, Forsman, Gulacsi, Haro, Kennelly, Knappe, Lai, Lasalvia, Miret, O'Sullivan, Obradors-Tarrago, Rusch, Sartorius, Svab, van Weeghel, Van Audenhove, Wahlbeck, Zlati, McDaid and Thornicroft2014). Studies in the general population showed that interventions containing social contact and first-person narratives were more effective than others (Mehta et al., Reference Mehta, Clement, Marcus, Stona, Bezborodovs, Evans-Lacko, Palacios, Docherty, Barley, Rose, Koschorke, Shidhaye, Henderson and Thornicroft2015), a finding that could not be confirmed for health professionals (Henderson et al., Reference Henderson, Noblett, Parke, Clement, Caffrey, Gale-Grant, Schulze, Druss and Thornicroft2014). Evidence from LMICs is particularly limited (Henderson et al., Reference Henderson, Noblett, Parke, Clement, Caffrey, Gale-Grant, Schulze, Druss and Thornicroft2014; Mehta et al., Reference Mehta, Clement, Marcus, Stona, Bezborodovs, Evans-Lacko, Palacios, Docherty, Barley, Rose, Koschorke, Shidhaye, Henderson and Thornicroft2015), especially when it comes to evidence on effective interventions, on how best to target key groups such as healthcare staff, or on how to culturally adapt interventions to local contexts (Semrau et al., Reference Semrau, Evans-Lacko, Koschorke, Ashenafi and Thornicroft2015).
Stigma can be addressed in specific interventions with PHC staff, but ideally it is incorporated into training as an integral part of health and mental health education. In LMICs, in the context of implementing the mhGAP, professional health staff in primary care as well as lay community mental health workers is increasingly trained in the detection and evidence-based treatment of mental disorders. Stigma would ideally be integrated into these training sessions, but evidence is still lacking on how to address stigma in these settings. In a systematic review, Mehta et al. (Reference Mehta, Clement, Marcus, Stona, Bezborodovs, Evans-Lacko, Palacios, Docherty, Barley, Rose, Koschorke, Shidhaye, Henderson and Thornicroft2015) reviewed interventions to reduce mental health-related stigma among different populations. This review revealed three interventions targeting health professionals in LMICs, hence evidence is limited.
Previous systematic reviews also showed that outcome assessments to quantify the effectiveness of stigma interventions remain an empirical challenge. While knowledge and attitudes can be measured using questionnaires, discriminatory behaviours are more difficult to assess. In the systematic review by Henderson et al. (Reference Henderson, Noblett, Parke, Clement, Caffrey, Gale-Grant, Schulze, Druss and Thornicroft2014) among health care staff, little evidence was found on behavioural outcomes of stigma interventions, and none of these studies were conducted in LMICs. This lack of evidence might be explained by the fact that behavioural outcomes are ideally measured by asking patients about their experiences with health professionals, and such data are more difficult to collect than assessments of knowledge and attitudes. And finally, stigma is most likely shaped by culture (Yang et al., Reference Yang, Kleinman, Link, Phelan, Lee and Good2007; Yang et al., Reference Yang, Thornicroft, Alvarado, Vega and Link2014). Systematic reviews show that cultural adaptation of psychological interventions increases their effectiveness (e.g. Harper Shehadeh et al., Reference Harper Shehadeh, Heim, Chowdhary, Maercker and Albanese2016), but this has not yet been tested for stigma interventions.
In summary, it is most relevant to better understand how mental health-related stigma can be addressed in trainings with health workers in the context of task-sharing approaches in LMICs. Previous reviews have not answered this question. The current study aims to close this gap by providing evidence on interventions for reducing mental health-related stigma among PHC workers in LMICs, with a primary focus on attitudes and behaviours. It therefore covers a small intersection of studies that were included in previous reviews (Henderson et al., Reference Henderson, Noblett, Parke, Clement, Caffrey, Gale-Grant, Schulze, Druss and Thornicroft2014; Mehta et al., Reference Mehta, Clement, Marcus, Stona, Bezborodovs, Evans-Lacko, Palacios, Docherty, Barley, Rose, Koschorke, Shidhaye, Henderson and Thornicroft2015; Semrau et al., Reference Semrau, Evans-Lacko, Koschorke, Ashenafi and Thornicroft2015). A new search was run to also include studies that have been published since these previous reviews. Furthermore, by using a ‘magnifying glass strategy’, a closer look is taken on the content and didactic methods used in stigma interventions for PHC staff in LMICs, and on the cultural adaptation of such interventions. With this approach, the current review aims to highlight future directions for designing effective interventions, thereby contributing to enhancing the quality of mental health care in primary care settings in LMICs.
Data collection, extraction and analysis
This study was listed in the PROSPERO register for systematic reviews (registration number CRD42017065436). Data collection included two different strategies. First, the existing systematic reviews on either stigma among PHC staff (Henderson et al., Reference Henderson, Noblett, Parke, Clement, Caffrey, Gale-Grant, Schulze, Druss and Thornicroft2014; Mehta et al., Reference Mehta, Clement, Marcus, Stona, Bezborodovs, Evans-Lacko, Palacios, Docherty, Barley, Rose, Koschorke, Shidhaye, Henderson and Thornicroft2015; Semrau et al., Reference Semrau, Evans-Lacko, Koschorke, Ashenafi and Thornicroft2015) or training of PHC staff in LMICs (Liu et al., Reference Liu, Jack, Piette, Mangezi, Machando, Rwafa, Goldenberg and Abas2016; Keynejad et al., Reference Keynejad, Dua, Barbui and Thornicroft2018) were searched for studies that met the inclusion criteria of the current review. Second, a new search was done, covering the time since the previous reviews, i.e. January 2013 to May 2017. The new search was run on 6 May 2017 and covered the following databases: PsycINFO, MEDLINE (Ovid), CINAHL, Social Sciences Citation Index and Cochrane (only Trials). Five search concepts were combined in order to capture relevant literature: stigma (e.g. stigma, discrimination or stereotype); mental health (e.g. depression, anxiety or schizophrenia); intervention (e.g. randomised controlled trial, evaluation or pre-post); PHC staff (e.g. general practitioners or health care workers) and LMICs classified according to the World Bank (2016), using their names (e.g. Afghanistan) and population adjectives (e.g. Afghan). The search strategies were adapted from the previous reviews. The complete search strategy (only Medline) can be accessed in the online Supplementary Material. The PRISMA diagram showing the data collection process is given in Fig. 1.
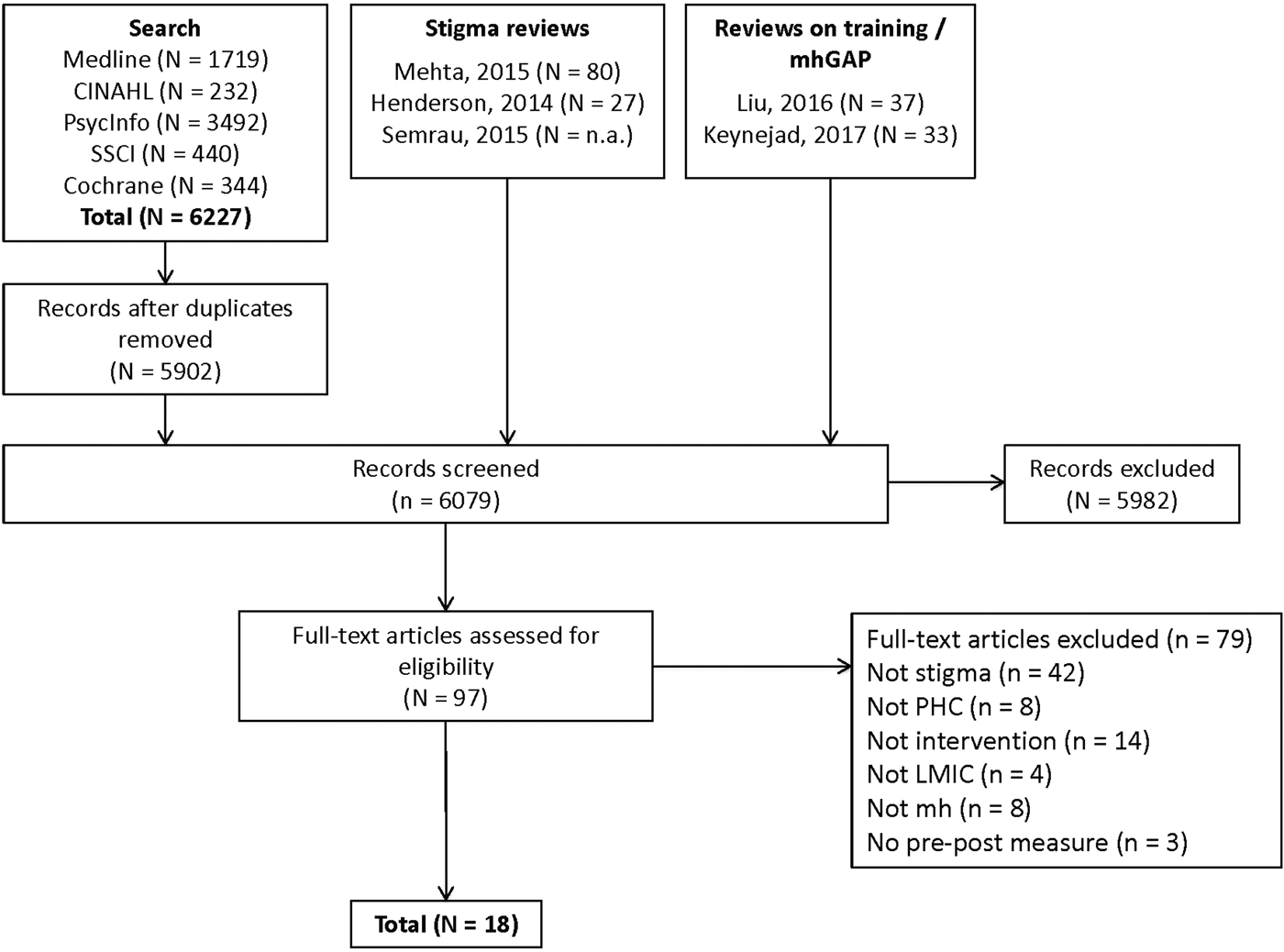
Fig. 1. Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) diagram with a systematic search and selection process.
Inclusion and exclusion criteria were defined along the participants, interventions, comparators and outcomes (PICO) approach. Participants in stigma interventions were PHC staff in LMICs (including non-professionals). The intervention had to be a mental health-related training programme addressing PHC workers’ knowledge, attitudes and behaviours in terms of professional skills. Studies were excluded if they trained or evaluated knowledge and behaviour/skills only, without an attitudinal (stigma-related) component, or if they did not include a pre-training assessment. Accordingly, outcomes had to include an attitudinal assessment, aside from knowledge and/or skills. Both qualitative and quantitative studies were included, and no comparator was defined.
The included full-texts were introduced to the qualitative data analysis software MAXQDA (version 12.3.3). A coding system was developed including the following categories: stigma intervention content (e.g. theory, diagnostic skills, relationship skills), didactic methods (e.g. lecture, role plays, contact with patients), the mental disorder the intervention focused on (e.g. depression, psychosis), whether the intervention was culturally adapted, the type of outcome measure (e.g. validated or non-validated questionnaire, qualitative interviews, behavioural observation) and primary outcomes. The analysis of outcomes focused only on attitudes and behaviour, not on knowledge. Outcome measures regarding knowledge are very diverse and would provide results that are hardly comparable, and knowledge was not the main focus of the current review. Two raters coded the full-texts independently and discussed possible differences until finding an agreement. Additionally, we used a category system to critically appraise the methodological quality of the included studies considering the following five criteria: control group, random allocation, random sequence generation, allocation concealment and incomplete data. A meta-analysis was originally planned but could not be calculated for the reasons given below.
Results
Eighteen studies were included in the analysis (see Table 1). The studies were from 11 different countries and included a broad range of participants, such as nurses, general practitioners (GPs) or community mental health workers. Sample sizes ranged from lower than N = 30 to N > 200, with seven studies having sample sizes of N > 100. Most studies (N = 11) covered mental disorders in general, but some studies addressed one particular disorder, such as depression (N = 4) and schizophrenia (N = 2).
Table 1. Summary of included studies describing training with PHC workers
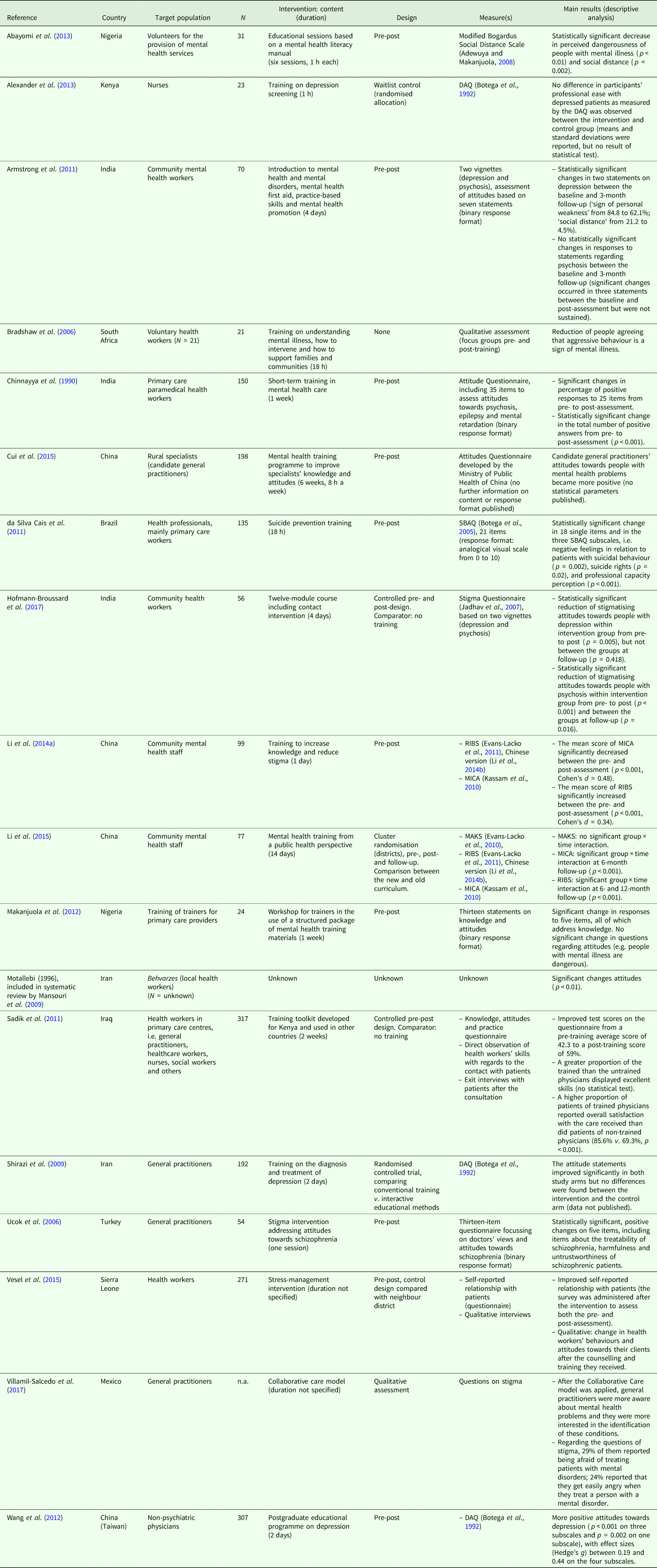
Note: DAQ, Depression Attitude Questionnaire; SBAQ, Suicide Behaviour Attitude Questionnaire; VAS, Violence Attitude Scale; RIBS, Reported and Intended Behaviour Scale; MICA, Mental Illness: Clinicians’ Attitudes Scale; MAKS, Mental Health Knowledge Schedule.
The majority of interventions (N = 15) provided theoretical information, such as symptoms, prevalence and aetiology of mental disorders, relationship between the mental and physical health or social consequences of mental disorders. In seven studies, stigma was explicitly addressed in this theoretical introduction. As an example, Ucok et al. (Reference Ucok, Soygur, Atakli, Kuscu, Sartorius, Duman, Polat and Erkoc2006) described their intervention as follows: ‘the slide presentation lasted approximately 45 minutes and included current information on the course of schizophrenia and its treatment, the impact of stigma on schizophrenia, and description of GPs’ roles’ (p. 440).
The majority of the studies (N = 11) covered the treatment of mental disorders, describing a variety of interventions, such as treatment guidelines, medication, counselling, referral to specialists, psychological first aid, problem-solving or interpersonal therapy. Of those studies, four reported that they had explicitly addressed the relationship with patients, e.g. promoting communication skills. As an example, Bradshaw et al. (Reference Bradshaw, Mairs and Richards2006) described that their community volunteers’ education programme included ‘examining interactions which may increase or reduce stress for the patient’ (p. 100). A great number of studies (N = 11) aimed at improving participants’ diagnostic skills. Some interventions covered mental health policy (N = 3), mental health promotion in communities and psychosocial interventions (N = 3) and stress management (N = 2).
With regards to didactic methods, the vast majority of studies provided lectures (N = 12). Additionally, many studies used interactive methods (N = 9), discussed case studies (N = 8) and used role plays (N = 5). Some interventions handed out written material (N = 5) or used multimedia as a didactic method (N = 3). Only three studies reported that they had used clinical practice and supervision as an intervention, and in one study, a patient told his recovery story to participants. The amount of information provided on the content and didactic methods used in interventions varied greatly. One study published the intervention manual online (Armstrong et al., Reference Armstrong, Kermode, Raja, Suja, Chandra and Jorm2011), whereas other studies provided only minimal information.
Four studies reported that they had adapted their interventions or measures to the specific cultural context, but the descriptions remained rather vague. As an example, Bradshaw et al. (Reference Bradshaw, Mairs and Richards2006) reported that ‘attempts were made to ensure that course materials were culturally appropriate to a South African community’ (p. 99). Outcomes of these interventions were most often measured using non-validated questionnaires (N = 11) or validated questionnaires (N = 6). Additionally, two studies used qualitative interviews for measuring outcomes, one study used interviews with patients and direct observation of health workers' skills, and two studies measured behavioural intentions.
With regards to risk of bias, the quality of the included studies varied greatly, but no study showed low risk of bias (the full risk of bias assessment is available in the online Supplementary Material). Only six studies compared their intervention with a control condition (Shirazi et al., Reference Shirazi, Parikh, Alaeddini, Lonka, Zeinaloo, Sadeghi, Arbabi, Nejatisafa, Shahrivar and Wahlstrom2009; Sadik et al., Reference Sadik, Abdulrahman, Bradley and Jenkins2011; Alexander et al., Reference Alexander, Arnkoff, Glass and Kaburu2013; Li et al., Reference Li, Li, Thornicroft, Yang, Chen and Huang2015; Vesel et al., Reference Vesel, Waller, Dowden and Fotso2015; Hofmann-Broussard et al., Reference Hofmann-Broussard, Armstrong, Boschen and Somasundaram2017), two of which used random allocation. Four studies applied quasi-experimental designs, e.g. testing an intervention in one district and using another district as a control group. All studies had administered self-reported outcome measures; thus, no blinding of outcome assessment was done. Many studies reported high drop-out rates, but only one study used intention-to-treat analysis for dealing with missing data. No meta-analysis could be calculated, for the following reasons: of the six studies that had compared their intervention with a control condition, two studies published no or incomplete data (Shirazi et al., Reference Shirazi, Parikh, Alaeddini, Lonka, Zeinaloo, Sadeghi, Arbabi, Nejatisafa, Shahrivar and Wahlstrom2009; Alexander et al., Reference Alexander, Arnkoff, Glass and Kaburu2013), two studies presented outcome measures that could not be used in meta-analysis (Sadik et al., Reference Sadik, Abdulrahman, Bradley and Jenkins2011; Vesel et al., Reference Vesel, Waller, Dowden and Fotso2015) and one study compared two different didactic methods (Li et al., Reference Li, Li, Thornicroft, Yang, Chen and Huang2015).
The descriptive analysis of the outcomes is displayed in Table 1. Most studies found some kind of positive effects of their intervention on attitudes of PHC staff towards people with mental illness, but some of these effects were rather small, e.g. statistically significant change in the percentage of positive responses to single items with binary response format (Chinnayya et al., Reference Chinnayya, Chandrashekar, Moily, Puttamma, Raghuram, Subramanya, Shanmugham and Udaykumar1990; Ucok et al., Reference Ucok, Soygur, Atakli, Kuscu, Sartorius, Duman, Polat and Erkoc2006; Armstrong et al., Reference Armstrong, Kermode, Raja, Suja, Chandra and Jorm2011). Some studies reported positive outcomes but did not present results of their statistical analyses (Shirazi et al., Reference Shirazi, Parikh, Alaeddini, Lonka, Zeinaloo, Sadeghi, Arbabi, Nejatisafa, Shahrivar and Wahlstrom2009; Cui et al., Reference Cui, Li and Yao2015). No or little effects were found from short training interventions, e.g. a 1-h training on depression screening (Alexander et al., Reference Alexander, Arnkoff, Glass and Kaburu2013) or a one-session stigma intervention for general practitioners (Ucok et al., Reference Ucok, Soygur, Atakli, Kuscu, Sartorius, Duman, Polat and Erkoc2006).
Differences regarding types of mental disorders emerged, although inconsistently. Armstrong et al. (Reference Armstrong, Kermode, Raja, Suja, Chandra and Jorm2011) found a change in attitudes towards people with depression but not towards people with psychosis, whereas Hofmann-Broussard et al. (Reference Hofmann-Broussard, Armstrong, Boschen and Somasundaram2017) found a stronger effect on attitudes towards psychosis than depression. Two studies compared different curriculums or didactic methods (Shirazi et al., Reference Shirazi, Parikh, Alaeddini, Lonka, Zeinaloo, Sadeghi, Arbabi, Nejatisafa, Shahrivar and Wahlstrom2009; Li et al., Reference Li, Li, Thornicroft, Yang, Chen and Huang2015), but only one found significant group differences (Li et al., Reference Li, Li, Thornicroft, Yang, Chen and Huang2015). Several studies showed a statistically significant change in total scores or subscales of questionnaires (da Silva Cais et al., Reference da Silva Cais, da Silveira, Stefanello and Botega2011; Wang et al., Reference Wang, Huang, Liu and Lu2012; Li et al., Reference Li, Li, Huang and Thornicroft2014a; Li et al., Reference Li, Li, Thornicroft, Yang, Chen and Huang2015; Hofmann-Broussard et al., Reference Hofmann-Broussard, Armstrong, Boschen and Somasundaram2017), but these results must be interpreted with caution due to risk of bias.
Few studies assessed behavioural outcomes alongside attitudes. In one study (Sadik et al., Reference Sadik, Abdulrahman, Bradley and Jenkins2011), psychiatrists evaluated the job skills of trained and untrained PHC staff. Evaluators were blinded to participants’ group assignment. In addition, patients were interviewed. The study showed differences between the study groups. And two studies (Li et al., Reference Li, Li, Huang and Thornicroft2014a; Li et al., Reference Li, Li, Thornicroft, Yang, Chen and Huang2015) applied the Reported and Intended Behaviour Scale (Evans-Lacko et al., Reference Evans-Lacko, Rose, Little, Flach, Rhydderch and Henderson2011) to assess behavioural discrimination. Li et al. (Reference Li, Li, Thornicroft, Yang, Chen and Huang2015) found a significant group × time interaction, indicating a difference between the two didactic methods tested in the study (see Table 1).
Discussion
This systematic review looked at interventions to reduce stigma among a variety of PHC workers (e.g. general practitioners, nurses, community health workers or volunteers) in LMICs. A total of 18 studies were included. The quality of included studies varied greatly, with a high number of studies showing a high risk of bias. Six studies (33%) have tested their intervention against a control condition, and only two studies (11%) had used random allocation. Moreover, a large number of studies reported high numbers of incomplete data but did not provide any information on how they dealt with missing values. From the present state of the literature, no meaningful conclusions can be drawn on the effectiveness of stigma interventions, key ingredients or target populations within health care. In the following, we aim to highlight suggestions on how to design future studies, in order to enhance the amount and the quality of evidence.
As reported in a previous systematic review on stigma interventions with PHC staff (Henderson et al., Reference Henderson, Noblett, Parke, Clement, Caffrey, Gale-Grant, Schulze, Druss and Thornicroft2014), all included studies measured outcomes by assessing knowledge and attitudes, with only a few studies measuring behavioural outcomes. Accordingly, providing theoretical information through lectures was the most frequent intervention, and more practical interventions targeting discriminatory behaviours, such as role plays or clinical practice under supervision, were rarely used. Studies testing such practical interventions are needed to target communication skills and relationship with patients. The protocol for such a study has been published recently (Kohrt et al., Reference Kohrt, Jordans, Turner, Sikkema, Luitel, Rai, Singla, Lamichhane, Lund and Patel2018).
Types of attitudinal outcome measures varied greatly, ranging from single items with binary response format to validated stigma questionnaires. Items with binary response format do not allow for more complex statistical procedures such as principal component analysis, inferential statistics, multiple imputation of missing values or inclusion of the results in meta-analyses. Moreover, the large diversity of questionnaires used across studies makes it difficult to obtain results, since the underlying constructs of these measures may vary. Consensus is needed on how to measure stigma in order to assess the efficiency of stigma interventions in the future.
Having said that, such a consensus should be inclusive for cross-cultural variations in how stigma is assessed and how interventions are designed (Yang et al., Reference Yang, Thornicroft, Alvarado, Vega and Link2014). Several studies reported cultural adaptation of questionnaires, but without using standardised methods for ensuring their validity and reliability, e.g. measurement invariance testing (e.g. Byrne, Reference Byrne2008) or cognitive interviewing. Furthermore, few of the included studies have made an attempt to culturally adapt their interventions. The importance of culturally adapting psychotherapeutic interventions has increasingly been stressed (Chowdhary et al., Reference Chowdhary, Jotheeswaran, Nadkarni, Hollon, King, Jordans, Rahman, Verdeli, Araya and Patel2014). It is most likely that stigma interventions require similar procedures for cultural adaptation, since how stigma is experienced varies across cultures (Yang et al., Reference Yang, Kleinman, Link, Phelan, Lee and Good2007; Yang et al., Reference Yang, Thornicroft, Alvarado, Vega and Link2014). Aside from culture, structural and institutional factors may affect how stigma materialises in PHC, e.g. whether a country has a mental health policy, the amount of financial and human resources allocated for mental health, how the mental health system is composed and the level of training of health workers. Taking into account such structural and institutional factors in future studies would enhance their comparability.
Limitations
This review has several limitations. First, we relied on previous reviews for the time before 2013. Second, included studies were published in English, with one exception. Full-text screening in other languages was done where necessary, but no specific search engines such as Scielo were used, and we did not include grey literature. Third, we did not look at outcomes of the interventions in terms of knowledge. Measuring knowledge in the field of mental health is a broad topic, and summarising this evidence would have been beyond the scope of the current review, due to its main focus on attitudes and behaviour.
Conclusions
This systematic review provides pathways for future research in stigma interventions for PHC staff. More practical interventions should be implemented and tested in LMICs using more rigorous methods with regards to research design, outcome measures, statistical analysis and dealing with missing data. Moreover, consensus is needed on how to measure stigma, alongside cultural adaptation of both assessment instruments and interventions. The global mental health ‘treatment gap’ and the integration of mental health into PHC requires evidence-based interventions for addressing stigma, in order to increase access to treatment and provide high-quality care to people suffering from mental disorders worldwide.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/S2045796018000458
Acknowledgements
The authors would like to thank Lea Muri and Emilia Vasella who helped with the search and data extraction.
Financial support
BAK is supported by the US National Institute of Mental Health (grants K01MH104310 and R21MH111280). GT is supported by the National Institute for Health Research (NIHR) Collaboration for Leadership in Applied Health Research and Care South London at King's College London NHS Foundation Trust, and the NIHR Asset Global Health Unit award. The views expressed are those of the author(s) and not necessarily those of the NHS, the NIHR or the Department of Health. GT acknowledges financial support from the Department of Health via the National Institute for Health Research (NIHR) Biomedical Research Centre and Dementia Unit awarded to South London and Maudsley NHS Foundation Trust in partnership with King's College London and King's College Hospital NHS Foundation Trust. GT is supported by the European Union Seventh Framework Programme (FP7/2007-2013) Emerald project.
Conflict of interest
None of the authors have any conflicts of interest to declare.
Ethical standards
No ethical approval was sought for this systematic review.
Availability of data and materials
The data extraction spread sheet (Excel) is available on request, please contact the corresponding author.




