The assessment and clinical management of risk of patients harming themselves or others is an integral part of good psychiatric practice (Royal College of Psychiatrists Special Working Party on Clinical Assessment and Management of Risk, 1996). Patients with learning disabilities present an increased risk because of their high prevalence of mental health problems and/or behaviour disorders (Reference Corbett, James and SmithCorbett, 1979; Reference LundLund, 1985; Reference Mcgrother, Bhaumik and ThorpMcGrother et al, 2002). However, mental health problems are often unrecognised because of linguistic and other communication problems (Reference Bhaumik, Collacott and GandhiBhaumik et al, 1995).
The care programme approach (CPA) was introduced in 1991 to provide a framework for effective multidisciplinary mental health care, with subsequent guidance and refinement (Department of Health, 1990, 1998b , 1999b ). It has four stages: systematic assessment of an individual's needs for health and social care; agreement of a package of care with the individual, carers and professionals; identification of a keyworker; and regular review of the individual's needs and delivery of care. The CPA is now integrated with care management, and has two levels- standard and enhanced. The use of CPA in specialist learning disability services was established later than in mainstream mental health services, and its use has been patchy (Reference RoyRoy, 2000).
With the introduction of clinical governance and strengthening of CPA (Department of Health, 1998a , 1999a ), risk assessment and management became crucial to preventing or reducing severe critical incidents and providing high-quality services. Good risk assessment/management is an explicit, logical process benefiting patients, carers and service managers (Reference Saunders, Thompson and MathiasSaunders, 1998). Risk assessment/management and CPA are complementary. For successful CPA, every patient must have a clear risk management plan. Risk assessment/management is essential for identifying appropriate residential placements and day services. Information on CPA and risk management plans should be shared with relevant professionals and carers both during the patient's stay in hospital and on return to the community. Clear, accessible documentation is vital (Reference Saunders, Thompson and MathiasSaunders, 1998).
For people with a dual diagnosis, risks posed by mental health problems and behavioural disorders are compounded by inherent risks arising from the learning disability. Some risks directly caused by mental and behavioural disorders can be reduced by treating the underlying condition. However, despite training and support, many inherent risks will be lifelong. Risk assessment should cover inherent and mental health risks, and risks related to environmental hazards, social and family circumstances, communication difficulties, inadequate coping skills and being easily influenced by others.
In 1992, Leicestershire Health Authority established an acute 12-bedded specialist treatment unit for adults with learning disabilities needing short-term assessment and clinical management of mental health problems, behaviour disorders and/or refractory epilepsy. The unit is a low secure unit with a locked door facility. A multidisciplinary team comprising consultant psychiatrists, nurses, speech and language therapists, occupational therapists and physiotherapists devised a risk assessment screening proforma, which was modified after a 6-month pilot study and introduced in June 1999 as a risk assessment and management tool. The proforma is used to assess risks related to mental health problems and behaviour disorders as well as inherent risks arising from the learning disability (Box 1). It is used to identify risk on admission to the unit, and also initiates CPA. Care programme approach screening is done on admission and shortly before discharge.
Box 1. Key domains of the risk assessment/management tool

| Forensic history |
| Self-neglect and self-harm |
| Safety risks, such as fire, damage to property, absconding, falling or choking |
| Vulnerability, exploitation |
| Aggression or harm to others |
| Mental health |
| Misuse of alcohol, drugs and other substances |
The aim of the audit reported here was to evaluate the effectiveness of CPA - including risk assessment and management - of patients admitted to the treatment unit. The specific objectives were to determine whether staff carried out risk assessment and CPA screening; whether they recorded the clinical decision regarding risk; and whether they shared the information with the clinical team and relevant agencies.
Method
A retrospective audit of the records of all patients admitted to the treatment unit between 1 April 1999 and 30 September 1999 was carried out by members of the specialist psychiatric team. It preceded publication of the Department of Health's audit pack (Department of Health, 2001). The standards for the audit were set by a local multidisciplinary audit group, comprising representatives from psychiatry and professions allied to medicine and a practice development nurse (Box 2).
Box 2. Standards for care programme approach (CPA) and risk assessment/management

| All patients should have CPA screening on admission and before discharge |
| All patients should have a CPA planning meeting before discharge |
| All patients should have an appropriate risk management plan on discharge |
| All patients should have evidence of information about risk being shared with appropriate professionals and carers |
| Professionals and carers should perceive risk reduction during admission in at least 80% of patients |
| The risk management plans of all patients should be shared with appropriate professionals and carers |
| All professionals should be aware of the CPA screening proforma |
Professionals on the unit completed a structured audit questionnaire about each patient. This collected details about the admission; demographic and clinical data; CPA screening on admission and discharge; and risk assessment/management during admission. Risks were categorised as major risks (significant or serious present risks requiring activation of the risk management plan) or minor risks (possible risks not requiring specific preventive action at the time).
Another audit questionnaire was sent to the patients’ carers and any professionals involved in their care in the community. This asked about their perceptions of risk on admission and discharge, and sharing of information about the patient's risk management plan.
The data were analysed using the Statistical Package for the Social Sciences, version 11.5. The results were reported to the staff on the unit and the multidisciplinary audit group. The latter drew up and implemented a list of recommendations.
Results
Response rates
Fifteen patients were admitted to the unit during the audit period. Completed questionnaires were received from the staff about all of them. The carers of 1 patient did not participate in the audit; carers’ questionnaires were received about the other 14 patients. The nursing notes, including CPA documentation, were missing for 3 patients.
Patient characteristics
The patient sample comprised 10 men and 5 women, with a mean age of 38 years (range 25-59). Four patients lived with their families, 8 in residential homes and 1 in an adult placement scheme. Two patients were admitted from a National Health Service hospital. Two patients were admitted under section 2 of the Mental Health Act 1983 and 1 under section 3; the other 12 had informal admissions.
Nature and prevalence of risks
Three patients were admitted with mental health needs, and 7 because they were judged to be a risk to others. Most patients presented with more than one risk. Of 16 categories of risk on the screening proforma, the mean number of major risks was 6 and the mean number of minor risks was also 6. Over the audit period, the risks most commonly presented by patients were aggression, dependency and mental health problems, each in 13 patients. In addition, 11 patients had physical health problems; 8 were at sexual risk, either of abusing others or of being abused; 6 were at risk of exploiting others; 6 of self-injury and 5 of deliberate self-harm. One patient presented the risk of arson and another that of compulsive drinking.
Care programme approach standards
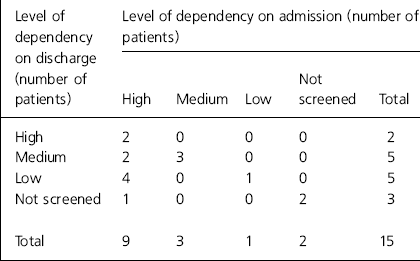
Thirteen patients (87%) received CPA screening on admission and 12 (80%) before discharge (Table 1). Of those who were screened on both occasions, 9 were assessed as having high dependency on admission, and 3 as having medium dependency. Before discharge, 6 patients had a lower level of dependency following treatment and 6 remained the same.
Table 1. Level of dependency on admission and discharge
| Level of dependency on discharge (number of patients) | Level of dependency on admission (number of patients) | ||||
|---|---|---|---|---|---|
| High | Medium | Low | Not screened | Total | |
| High | 2 | 0 | 0 | 0 | 2 |
| Medium | 2 | 3 | 0 | 0 | 5 |
| Low | 4 | 0 | 1 | 0 | 5 |
| Not screened | 1 | 0 | 0 | 2 | 3 |
| Total | 9 | 3 | 1 | 2 | 15 |
Only 9 patients (60%) had a CPA planning meeting before discharge, and only 4 (27%) had a demonstrable risk management plan on discharge. Eight patients definitely did not have such a plan. It was unknown whether a risk management plan had been drawn up for the 3 patients with missing nursing notes.
For 8 patients (53%), there was evidence that information about risk had been shared with appropriate professionals and carers. Professionals perceived a definite risk reduction during admission in 12 patients (80%) and carers in 9 (60%). Professionals and carers of 3 patients agreed that there had been no risk reduction. There was a similar difference in professionals’ and carers’ perceptions about sharing risk management plans. Professionals thought that this had happened for 12 patients (80%) and carers for 9 patients (60%).
All the professionals involved with 12 patients (80%) were aware of the CPA screening proforma. For the other 3 patients, at least some staff were unaware of it.
Discussion
The audit revealed major deficiencies in risk identification, risk management and information sharing. At the time of the audit, however, CPA had only been in place for 6 months. Nevertheless, it is of concern that 2 patients did not receive CPA screening on admission. Before discharge, 3 patients were not screened and 6 did not have a CPA planning meeting. This meant that their aftercare arrangements were inadequately planned and would be more likely to break down.
It is alarming that only 4 patients had a risk management plan available on discharge. Thus, the problems for which patients were admitted were likely to continue after discharge.
Sharing information about risk can only be ensured through the meticulous use of written documents. This was grossly inadequate, evidence for sharing only existing for about half of the patients. The discrepancy between professionals’ and carers’ perceptions also reflects problems with the communication systems. The audit identified serious problems with storing nursing records after patients’ discharge from the unit, which led to incomplete data collection for the audit. Missing records also have potentially serious clinical consequences.
Although this was the first CPA audit, the standards were set at a high level. It is vital that appropriate measures are taken to prevent or minimise any critical incidents in the unit, so lowering the audit standards would be unwise. The audit did not reflect the good practices already existing in the unit, such as the weekly multidisciplinary review of every patient. Although not formally recognised as CPA reviews, these may involve planning patients’ care after discharge. Staff on the unit were concerned that other professionals failed to attend these meetings, compounding the difficulties of sharing information.
As a result of the audit, the risk assessment and management process was amalgamated with CPA, and the following recommendations were implemented.
-
• A multidisciplinary team has clear responsibility for a new process that ensures that all patients receive CPA screening on admission and before discharge.
-
• Every professional and carer involved with a patient's care receives a copy of the completed risk assessment proforma.
-
• An addendum to this proforma charts identified risks and respective management plans, with explicit time scales and named individuals responsible for CPA review.
-
• A CPA planning meeting proforma ensures that all patients have a documented CPA planning meeting before discharge.
-
• Sharing of risk management plans is documented on the CPA care plan, which is signed by carers and professionals.
A future CPA audit will include professionals’ attendance rates at CPA and other review meetings.
Declaration of interest
None.
Acknowledgements
The authors thank Gill Gates, Nurse Adviser for the Learning Disability Services, and Alison Rhodes, Staff in Charge of the Treatment Unit, for their help with this audit.






eLetters
No eLetters have been published for this article.