Suboptimal vitamin D status among the South Asian UK population has been recognised for over 40 years, and is widely reported(Reference Serhan and Holland1–Reference Dunnigan, Paton and Haase4). Vitamin D deficiency impairs Ca and P absorption, resulting in poor mineralisation of the skeleton(Reference Holick5), and is frequently associated with secondary hyperparathyroidism(Reference Serhan and Holland1, Reference Alfaham, Woodhead and Pask6); therefore the impact of vitamin D deficiency on bone health is of concern, particularly among the elderly(Reference Solanki, Hyatt and Kemm3).
There is a lack of data regarding bone health and fracture risk in European minority ethnic populations, particularly those from the Indian subcontinent. As part of the recent Oslo Health Study, vitamin D status and biochemical markers of bone turnover were measured in Pakistanis aged 40–60 years living in Oslo and compared with those of the local age-matched Norwegian population. Data from this study revealed that despite a high prevalence of vitamin D deficiency and secondary hyperparathyroidism in the Pakistani group, there was no difference in bone mineral density (BMD) measured at the forearm and there were only minor differences in bone turnover markers compared with the local Norwegian population(Reference Holvik, Meyer and Sogaard7). The authors speculated that altered vitamin D metabolism in the Pakistani population protected their skeleton from bone loss. In contrast, studies of vitamin D status and bone mass in young (aged 18–40 years) UK South Asian women revealed an adverse effect of vitamin D insufficiency on bone mineral mass at the hip and wrist(Reference Roy, Berry and Pye2, Reference Hamson, Goh and Sheldon8).
The aims of the present study were to determine the vitamin D and parathyroid hormone (PTH) status of postmenopausal South Asian and Caucasian women attending the same health centre in Blackburn and to compare the associations between these, bone quality and biochemical markers of bone turnover in the two ethnic groups.
Subjects and methods
Study population
Apparently healthy postmenopausal Caucasian and South-Asian women aged 50–65 years were identified from the health centre database at a general practice in an area of Blackburn (Lancashire, UK) that serves a large South Asian population. Exclusion criteria included menstrual bleeding within the previous 12 months, use of steroid medication, Ca and/or vitamin D supplementation, hormone replacement therapy, renal diseases, diuretic use and gastrointestinal disorders. Eligible patients were invited to participate in the study by telephone. The present study was conducted according to the guidelines laid down in the Declaration of Helsinki and all procedures involving human subjects/patients were approved by the University of Central Lancashire, Faculty of Science Ethics Committee and from the Preston, Chorley and South Ribble Local Research Ethics Committee. Written informed consent was obtained from all participating women.
Anthropometry, diet and lifestyle
Subjects were weighed with light clothing, on a medical scale (Seca, Macclesfield, Cheshire, UK). Height was measured with a wall-mounted stadiometer (Seca).
Vitamin D and biochemical markers of bone turnover
Fasting morning blood was taken from sixty-six South Asian and forty-two Caucasian postmenopausal women between the months of May and September. Serum and plasma samples were stored frozen at − 70°C until analysed. All assays were performed in the Department of Clinical Chemistry, Royal Liverpool Hospital (Liverpool, UK).
The plasma concentrations of type-1 collagen β C-telopeptide (βCTX), a marker of bone resorption, and of procollagen type-1 amino-terminal propeptide (P1NP), a marker of bone formation, were measured using electrochemiluminescence assays (Roche Diagnostics, Lewes, East Sussex, UK). Serum intact PTH levels were measured using sandwich immunoassay (PTH STAT; Roche Diagnostics) and bone-specific alkaline phosphatase (BAP) activity by immunoassay (Metra BAP EIA kit; Technoclone Ltd, Dorking, Surrey, UK). Vitamin D status was determined by measuring serum 25-hydroxycholecalciferol (25(OH)D3) and 25-hydroxyergocalciferol (25(OH)D2) by HPLC–MS/MS. The lower limit of detection for both D2 and D3 was 2·5 nmol/l (1 ng/ml). For statistical analysis, concentrations below the detection limit were assigned a value of 1·25 nmol/l. At the low end of the detection range, the within-batch precisions (CV) for measures of D2 and D3 were 9·2 and 7·0 %, respectively, and the between-batch precisions were 10·0 and 8·2 %, respectively. Quality assurance of the data was monitored through participation in the Vitamin D External Quality Assessment Scheme (DEQAS).
Calcaneal broadband ultrasound measurements
Broadband ultrasound attenuation (BUA) measurements of the calcaneus were determined by contact ultrasound sonometry using a McCue CUBA Clinical Bone Sonometer (McCue plc, Southampton, Hants, UK). All data were collected by the same operator and the two population groups were measured concurrently over an 18-month period and as close as practically possible to the time of blood sampling for markers of bone turnover and vitamin D status. The ultrasound sonometer was calibrated at the start of each session using a ‘phantom’. Precision of the instrument was monitored on the heel of the same individual and the CV was calculated to be 1·98 %. Results were recorded as BUA (dB/MHz) and also as the ‘percentage expected’ compared with an age-matched population mean. The McCue CUBA Clinical Bone Sonometer (McCue plc) uses for comparison purposes young, healthy Caucasian subjects. It was therefore not possible to compare South Asian data against South Asian normative BUA values.
Data analysis
Statistical tests were performed using SPSS 15.0 for Windows software (SPSS, Inc., Chicago, IL, USA). The normality of distribution was checked for all study parameters. Apart from percentage expected BUA, height and BMI, all parameters measured were skewed and/or kurtotic in at least one of the groups, and the usual methods of normalisation were unsuccessful. Therefore the non-parametric Mann–Whitney U test was used for comparison between groups and Spearman's rank correlation test was used for correlation analysis. A value of P ≤ 0·05 was considered statistically significant. Analysis of covariance was used to examine the effect of BMI, weight and height on vitamin D status and BUA.
Results
The median age of the South Asian women was significantly lower than that of the Caucasian women (median age: South Asians 55 v. Caucasians 60 years; P < 0·001) and the former were significantly shorter (median height: South Asians 1·53 v. Caucasians 1·59 m; P < 0·001) with a higher BMI (median BMI: South Asians 30·9 v. Caucasians 26·5 kg/m2; P < 0·001).
Parathyroid hormone levels and 25-hydroxyvitamin D
The results of the analysis of the biomarkers for vitamin D status and PTH levels are presented in Table 1. The reported values for 25(OH)D3 were below the levels of detection in 11 % (seven out of sixty-six) of the South Asian women and none of the Caucasian women. The reported values for 25(OH)D2 were below the levels of detection in 62 % (forty-one out of sixty-six) of the South Asian and 67 % (twenty-eight out of forty-two) of the Caucasian women. The South Asian women had significantly (P < 0·001) lower serum 25(OH)D3 levels than the Caucasians. Considering total serum 25(OH)D (D2 plus D3), it is widely accepted that concentrations of less than 50 nmol/l represent vitamin D deficiency(Reference Holick9, Reference Bischoff-Ferrari, Giovannucci and Willett10), although a more conservative threshold of less than 25 nmol/l is also used(11). Figure 1 shows that 97 % (sixty-four out of sixty-six) of the South Asian women had vitamin 25-hydroxyvitamin D (25(OH)D) levels below 50 nmol/l, with 85 % (fifty-six out of sixty-six) of the women with levels less than 25 nmol/l. Of the Caucasian women, 60 % (twenty-five out of forty-two) fell in the deficient range below 50 nmol/l and 10 % (four out of forty-two) had levels less than 25 nmol/l (Fig. 1). The serum PTH concentration of the South Asian group was significantly higher than that of the Caucasian group (P < 0·001) (Table 1). When analysed by ethnicity, there was a significant inverse relationship between PTH and 25(OH)D in the South Asian women (P = 0·001; r − 0·389) but no correlation between PTH and 25(OH)D was observed in the Caucasian women (P = 0·78; r − 0·045) (Fig. 1).
Table 1 25-Hydroxyvitamin D, parathyroid hormone (PTH), bone turnover markers and broadband ultrasound attenuation (BUA) scores in postmenopausal women according to ethnic background
(Mean and median values and interquartile ranges (IQR))
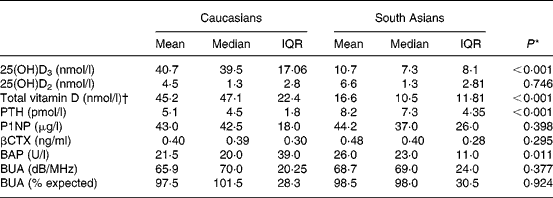
25(OH)D3, 25-hydroxycholecalciferol; 25(OH)D2, 25-hydroxyergocalciferol; P1NP, procollagen type-1 amino-terminal propeptide; βCTX, type-1 collagen β C-telopeptide; BAP, bone-specific alkaline phosphatase.
* Means were compared by the Mann–Whitney U test.
† 25(OH)D3 plus 25(OH)D2.

Fig. 1 Relationship between 25-hydroxyvitamin D (25(OH)D) and parathyroid hormone (PTH) levels in postmenopausal Caucausian (■) and South Asian (![]() ) women. When analysed by ethnicity, there was a significant inverse relationship between PTH and 25(OH)D in the South Asian women (P = 0·001; r − 0·389) but no correlation between PTH and vitamin D status was observed in the Caucausian women (P = 0·78; r − 0·045).
) women. When analysed by ethnicity, there was a significant inverse relationship between PTH and 25(OH)D in the South Asian women (P = 0·001; r − 0·389) but no correlation between PTH and vitamin D status was observed in the Caucausian women (P = 0·78; r − 0·045).
Correlations between 25-hydroxyvitamin D, parathyroid hormone, bone turnover markers and broadband ultrasound attenuation
BAP activity was significantly higher in the South Asian group, indicating elevated osteoblast activity (P = 0·011) and increased bone turnover. No significant differences were observed between the two groups for P1NP, βCTX or BUA scores (Table 1).
There was a weak negative correlation between 25(OH)D and BAP activity (r − 0·241; P = 0·012) when data from both groups were combined. This relationship was not significant when the ethnic groups were analysed separately. There were no significant correlations between total serum 25(OH)D and the other markers of bone turnover or with BUA when data were combined or analysed by ethnicity.
There were weak correlations between PTH and BAP activity (r 0·248; P = 0·01) and PTH and βCTX (r 0·210; P = 0·029). When analysed by ethnicity, only PTH with βCTX in the South Asians remained significant (r 0·246; P = 0·046).
There was a strong, significant correlation between βCTX and P1NP in the combined data (r 0·766; P < 0·001), and when analysed by ethnicity (South Asians: r 0·806, P < 0·001; Caucasians: r 0·76, P < 0·001).
Analysis of covariance
Analysis of covariance revealed that the covariate BMI does not have a significant relationship to total serum 25(OH)D (F(1,105) = 3·5; P = 0·064). Correcting for BMI does reduce the variance due to ethnicity, but the difference in 25(OH)D levels is still significant between the two ethnic groups (F(1,105) = 44·23; P < 0·001). Analysis of covariance revealed that, across the two ethnic groups, BUA was associated with weight, and BMI, but not height. Correcting weight, height or BMI did not result in a significant difference in BUA or expected BUA between the two ethnic groups.
Discussion
The results from the present study reveal a high incidence of vitamin D deficiency and secondary hyperparathyroidism in this group of postmenopausal South Asian women, with 25(OH)D levels significantly lower and PTH levels significantly higher than the postmenopausal Caucasian women attending the same health centre. The sampling time, between May and September, represents the optimal time for 25(OH)D synthesis resulting from sunlight exposure. This time frame was chosen primarily to reduce the effects of seasonal variation which would have been an additional factor to consider in this relatively small sample size. Sampling during the winter is likely to have yielded lower values for 25(OH)D, particularly in the Caucasian women, which may also have had an impact on the relationship with PTH and bone turnover markers.
The reasons for the high prevalence of vitamin D deficiency in this group of South Asian women are likely to include lack of sunlight exposure due to the conservative Muslim dress worn by these women, and darker skin pigmentation requiring greater UV exposure than fair skin to produce the same amount of 25(OH)D. Despite this, measurement of indices of bone formation and resorption in the present study, coupled with ultrasound measures of bone quality, have failed to identify any statistically significant differences between the two groups of women, with the exception of BAP activity. Although it is feasible that the sample size of the present study was not large enough to detect small differences in BUA, P1NP and CTX between the two ethnic groups, the absence of large differences in bone turnover in the presence of such striking differences in vitamin D and PTH levels is worthy of note(Reference Holvik, Meyer and Sogaard7).
Previous studies of the relationship between vitamin D status and bone health in South Asian populations have yielded conflicting results. In a comparative study of Pakistani and Norwegian women living in Oslo, Holvik et al. (Reference Holvik, Meyer and Sogaard7) also reported that hyperparathyroidism coupled with low vitamin D status in the Pakistani women was not associated with increased bone turnover and they had similar BMD to the ethnic Norwegians when measured by dual-energy X-ray absorptiometry(Reference Holvik, Meyer and Sogaard7). In addition, following a comparative study of Gujarati and Caucasian women in Leicester, UK, Hamson et al. (Reference Hamson, Goh and Sheldon8) reported that Gujarati women had lower BMD at the hip and spine. However, vitamin D status was not an independent predictor of BMD and there were no abnormalities of bone biochemistry in a subgroup of patients with low vitamin D compared with those with normal vitamin D status(Reference Hamson, Goh and Sheldon8). In contrast, BMD has been reported to be associated with low vitamin D status in young women in the UK(Reference Roy, Berry and Pye2) and in young healthy men and women in India(Reference Arya, Bhambri and Godbole12). It is important to note that the mean dietary Ca intake of the Indian study volunteers was low at 438·6 mg (range 200 to 696 mg/d), with 74 % of the subjects consuming less than 500 mg/d. Thus the controversy concerning the relationship between vitamin D status and bone health may be explained, at least in part, by differences in dietary Ca intake. Few studies, however, have attempted to measure Ca intakes in this context.
In a placebo-controlled trial, Storm et al. (Reference Storm, Eslin and Porter13) demonstrated that increasing Ca intake by diet or the use of supplements can reduce or prevent seasonal bone loss from the femur in elderly women by suppressing bone turnover during the winter when serum 25(OH)D3 declines and serum PTH increases. The minimum amount of dietary Ca required to elicit this response is not clear and may vary with ethnicity. In the present study the estimated average Ca intake for both groups of women exceeded the reference nutrient intake, with average intakes of 772 and 1090 mg/d in the South Asian and Caucasian women, respectively (data not reported), which may have been sufficient to suppress bone turnover and reduce bone loss.
It has been proposed that, when dietary Ca intake is sufficient, it may be changes in vitamin D status that drive the change in PTH, rather than Ca intake per se (Reference Serhan and Holland1, Reference Storm, Eslin and Porter13, Reference Ooms, Roos and Bezemer14). This hypothesis is supported by the present study and by others that report an inverse relationship between 25(OH)D and serum PTH when dietary Ca intake is adequate(Reference Roy, Berry and Pye2, Reference Malabanan, Veronikis and Holick15). Roy et al. (Reference Roy, Berry and Pye2) suggest a threshold 25(OH)D value of about 36 nmol/l, below which PTH values rise markedly, although this threshold may vary widely depending on dietary Ca intake(Reference Steingrimsdottir, Gunnarsson and Indridason16).
Conclusion
The South Asian women in this sample had significantly higher serum PTH and lower 25(OH)D levels than Caucasian women attending the same health centre. However, this did not result in higher markers of bone resorption, or reduced bone quality measured by BUA in the South Asian women. Further research is required to investigate the complex mechanisms regulating Ca homeostasis, and to identify a potential threshold level of Ca intake that may suppress PTH-induced bone turnover.
Acknowledgements
This research was supported by Lancashire Teaching Hospitals NHS Trust Research Directorate Seedcorn funding. The authors would like to thank the practice manager, staff and patients at Bangor Street Health Centre for their kind support and assistance with the present study. Also, we would like to thank Professor William Fraser and his team at the Royal Liverpool Hospital for vitamin D and bone turnover analyses.
N. M. L. and J. F. M. were responsible for the design of the experiment. I. B. was responsible for recruiting participants. S. R. M. collected the data, and P. C. F., N. M. L. and S. R. M. analysed the data. All authors contributed to writing the paper.
None of the authors has any conflicts of interest that have had an impact on this research.




