Personality disorders are ‘pervasive, inflexible, maladaptive’ collections of traits that impair individuals and interfere with their ability to function productively (American Psychiatric Association, 1994). These disorders co-occur frequently with axis I disorders in psychiatric patients and can complicate their treatment and worsen their prognosis (Reference Hirschfeld, Russell and DelgadoHirschfeld et al, 1998; Reference Seiverwright, Tyrer and JohnsonSeiverwright et al, 1998; Reference Skodol, Stout and McGlashanSkodol et al, 1999). In addition, personality disorders are associated with adverse consequences in the general population, including occupational difficulties, marital dissolution and criminal behaviours (Reference McCranie and KahanMcCranie & Kahan, 1986; Reference Bland, Stebelsky and OrnBland et al, 1988; Reference Johnson, Cohen and SmailesJohnson et al, 2000). In the current study, we assessed the frequency of DSM-IV (American Psychiatric Association, 1994) and ICD-10 (World Health Organization, 1993) personality disorders, and the relationships between DSM-IV personality disorder ‘clusters’ and demographic characteristics, in a community sample of 742 subjects, ages 34-94, evaluated between 1997 and 1999.
METHOD
Sample
Subjects participating in the Hopkins Epidemiology of Personality Disorder Study were sampled from the Baltimore Epidemiologic Catchment Area follow-up survey, which has been described previously (Reference Eaton, Anthony and GalloEaton et al, 1997). In brief, 3481 adult household residents of east Baltimore were sampled probabilistically and were interviewed using the Diagnostic Interview Schedule (DIS); 810 of these individuals were also examined by psychiatrists as part of the Clinical Reappraisal (Reference Anthony, Folstein and RomanoskiAnthony et al, 1985). Between 1993 and 1996, 1920 (73%) of the surviving subjects were re-interviewed.
From these 1920 subjects, we selected all those who were examined by psychiatrists in 1981, as well as all subjects who were identified by the DIS as having a lifetime diagnosis of mania, depression, panic disorder, obsessive—compulsive disorder, alcohol use disorders, or drug use disorders at follow-up. In addition, a random sample (222/884; 25%) was selected from the remaining subjects. Of the 1258 subjects selected with these criteria, 516 could not be interviewed because they: (a) could not be traced (n=144); (b) refused participation (n=134); (c) were deceased (n=103); or (d) were too ill or elderly to participate (n=92); another 43 subjects had an interview pending when data collection was terminated for budgetary reasons at the end of 1999. A total of 742 subjects completed the personality examinations between 1997 and 1999. The gender and ethnic distributions of these subjects were similar to those of the 516 subjects who were not interviewed; however, the interviewed subjects were younger (mean age 47 years) than non-interviewed subjects (mean age 61 years) (t1256=15.6, P<0.001). The gender and ethnic distributions of the study subjects were also similar to those of the 3481 subjects examined in 1981, although the study subjects were younger.
Personality disorder assessment
The personality disorder assessments were conducted by four masters-level clinical psychologists. The psychologists obtained informed consent prior to the interview. They interviewed the subjects about family background, childhood behaviours, academic performance, social activities and impairments; they also administered the General Health Questionnaire (Reference GoldbergGoldberg, 1972) and Parental Bonding Instrument (Reference ParkerParker, 1979). The psychologists conducted a comprehensive assessment of personality disorders using the International Personality Disorder Examination (IPDE) (Reference Loranger, Sartorius and AndreoliLoranger et al, 1994). The IPDE is a semi-structured instrument designed to be administered by clinicians to detect all the relevant criteria for diagnosis of all DSM-IV or ICD-10 personality disorders. The version used in this study combined the DSM-IV and ICD-10 versions into a single instrument, under the guidance of Dr Armand Loranger. The psychologists were directed to evaluate abnormal personality traits manifest over the subject's entire adult life. Each criterion was rated ‘0’ (absent), ‘1’ (accentuated or exaggerated), ‘2’ (criterion level or pathological) or ‘9’ (missing or unknown). In 40 jointly rated interviews, the intraclass correlation co-efficients for number of DSM-IV personality disorder traits rated present (‘1’ or ‘2’) were: schizoid (0.81); schizotypal (0.58); paranoid (0.63); antisocial (0.80); borderline (0.76); histrionic (0.62); narcissistic (0.62); avoidant (0.89); dependent (0.76); and obsessive—compulsive (0.70).
During the informed consent procedure, the subject was asked to provide the names of three individuals who knew him/her well over most of his/her adult life. Following the interview, the examiners interviewed at least one of these informants by telephone, using questions from the IPDE and scored as above. The examiners were required to evaluate more than half of the criteria for each of the personality disorders, and they were also encouraged to enquire from the informant about additional criteria. The required criteria were those that occurred most frequently, based on prior studies in eastern Baltimore (Reference Samuels, Nestadt and RomanoskiSamuels et al, 1994). The total personality assessment (subject and informant) took about 3 h, on average, to complete. After the interviews, the psychologists formulated a final rating for each criterion based on their clinical judgment of both subject and informant reports, and they completed a case summary describing the personality of each subject.
Statistical analysis
Diagnoses of the specific personality disorders were generated by algorithms based on DSM-IV and ICD-10 criteria, as operationalised by Lorangeret al (Reference Loranger, Sartorius and Andreoli1994). About 2% of the subjects were missing information on more than one criterion for each of the personality disorders. If at least half of the criteria for diagnosis were recorded, the diagnostic algorithm operated by assigning the value of ‘0’ to data items that were missing. If fewer than half of the items were recorded, then the disorder was coded as missing.
To estimate the prevalence of personality disorders in the eastern Baltimore population, we used weights to account for the unequal selection probabilities. The weights are the product of the two selection probabilities from the baseline study and the subsequent screening at follow-up. Weighted results better represent the population, whereas unweighted results better represent the sample. The major advantage that these sample data have is that they do not suffer from either of the two major sources of bias in epidemiology — the bias of the clinic (socalled Berkson's, or treatment-seeking, bias; Reference BerksonBerkson, 1946) or the bias of chronicity (sometimes called Neyman bias, or the clinician's illusion; Reference Cohen and CohenCohen & Cohen, 1984). In the current research design, the major advantage of weighting the data is to remove a third bias that can result from selecting a sample with prevalence of axis I disorders higher than that in the general population. This logic leads us to compare the weighted and unweighted data, in early analyses, and then to follow with presentations of the more straightforward unweighted data.
Confidence intervals, and statistical inference in general, are important in understanding the results. This sample has been selected probabilistically from the population, but it is a multi-stage clustered sample which has suffered multiple sources of attrition over more than a decade, and multiple logics of selection. It is difficult, and misleading, to attempt to represent the multiple sources of selection and sources of attrition as aspects of sample design for use in typical statistical algorithms for complex sample variance estimation (Reference Lehtonen and PakkinenLehtonen & Pakkinen, 1995). In this situation, we have estimated sample variances with the bootstrap strategy (Reference Efron and TibshiraniEfron & Tibshirani, 1986) as implemented in Stata (StataCorp, 1999). Ten thousand resamples of individuals were selected randomly with replacement from the original sample and were of the same sample size (n=742) as the original sample. Each standard error was calculated as the square-root of the ‘sample variance’ of the corresponding weighted prevalence estimate across the 1000 re-samples. The boot-strapped variances have been compared with variances estimated as if the sample were a simple random sample, and the differences (presented below) are not great. The logic of selecting individuals with axis I psychopathology (as discussed above) presumably increases the variance in prevalence estimates of personality disorders, as higher axis I psychopathology is likely to be associated with higher axis II psychopathology, and the higher prevalence will be associated with larger variance. Therefore, we consider the bootstrap estimates presented below to be conservative.
DSM-IV groups the personality disorders into three clusters: cluster A or ‘odd—eccentric’ disorders (paranoid, schizoid, schizotypal); cluster B or ‘dramatic—emotional’ disorders (antisocial, borderline, histrionic, narcissistic); and cluster C or ‘anxious—fearful’ disorders (avoidant, dependent, obsessive—compulsive). The occurrence of each of these clusters was compared across demographic characteristics using χ2 tests. Multivariate logistic regression (Reference Hosmer and LemeshowHosmer & Lemeshow, 1989) was used to evaluate the association between demographic characteristics and each of the clusters. For each cluster, the adjusted model presents the magnitude of the association between the cluster and the demographic characteristics, controlling for the other characteristics in the model.
RESULTS
Characteristics of the study sample
As shown in Table 1, 63% of the study subjects were female. The age range of subjects was 34-94 years (mean 51). Sixty per cent were White, and 37% were African American. The number of years of schooling completed ranged from 0 to 17 years (mean 12); 34% of the subjects had not graduated from high school. Nearly 60% of subjects currently were married or widowed; 26% were separated or divorced, and 16% had never married. Annual household income ranged from less than US$1000 to US$150 000 and over; 35% of the subjects had a household income below US$20 000.
Table 1 Demographic characteristics of the Hopkins Epidemiology of Personality Disorders sample (n=742)

| n | (%) | |
|---|---|---|
| Age in years | ||
| 34-44 | 267 | (36) |
| 45-54 | 248 | (33) |
| 55-94 | 227 | (31) |
| Gender | ||
| Male | 274 | (37) |
| Female | 468 | (63) |
| Ethnicity | ||
| White | 444 | (60) |
| Black | 273 | (37) |
| Other | 25 | (3) |
| Current marital status1 | ||
| Married or widowed | 434 | (58) |
| Separated or divorced | 189 | (26) |
| Never married | 116 | (16) |
| Highest grade completed2 | ||
| Not high school graduate | 252 | (34) |
| High school graduate | 214 | (29) |
| Post-high school | 271 | (37) |
| Household income, annual (US$)3 | ||
| <20 000 | 224 | (35) |
| 20 000-49 999 | 247 | (38) |
| > 49 999 | 176 | (27) |
Prevalence of personality disorders
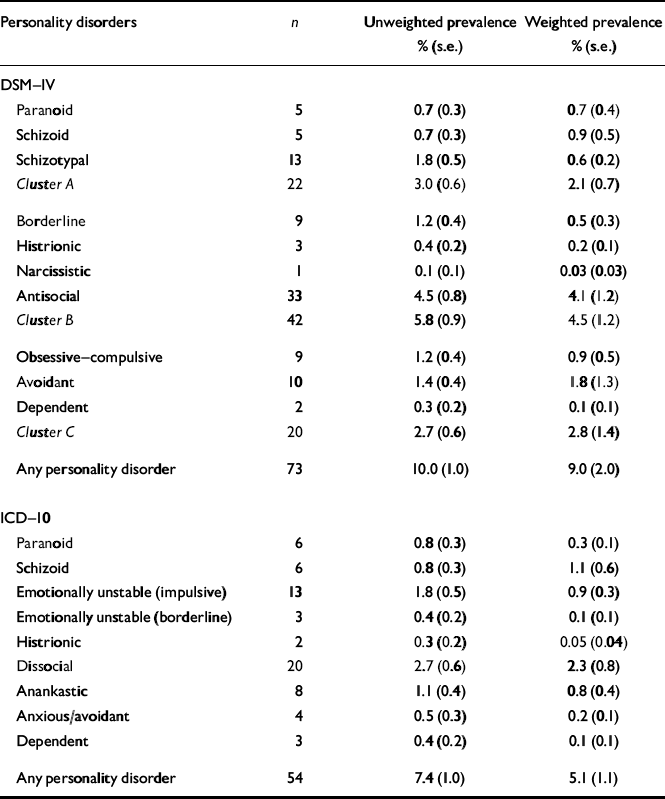
Overall, 10% of the subjects (9% weighted) had one or more DSM-IV personality disorders (Table 2). The prevalence of most individual disorders was 1-2%. Antisocial personality disorder was the most frequent, occurring in nearly 5% of the sample; narcissistic and dependent personality disorders were uncommon. For most disorders, there was little difference between unweighted and weighted estimates. For schizotypal, borderline and narcissistic personality disorders, however, the weighted estimates were less than half the unweighted estimates. Nevertheless, for all disorders, the 95% confidence intervals overlap for unweighted and weighted estimates.
Table 2 Prevalence of personality disorders in eastern Baltimore, 1997-1999
| Personality disorders | n | Unweighted prevalence | Weighted prevalence |
|---|---|---|---|
| % (s.e.) | % (s.e.) | ||
| DSM—IV | |||
| Paranoid | 5 | 0.7 (0.3) | 0.7 (0.4) |
| Schizoid | 5 | 0.7 (0.3) | 0.9 (0.5) |
| Schizotypal | 13 | 1.8 (0.5) | 0.6 (0.2) |
| Cluster A | 22 | 3.0 (0.6) | 2.1 (0.7) |
| Borderline | 9 | 1.2 (0.4) | 0.5 (0.3) |
| Histrionic | 3 | 0.4 (0.2) | 0.2 (0.1) |
| Narcissistic | 1 | 0.1 (0.1) | 0.03 (0.03) |
| Antisocial | 33 | 4.5 (0.8) | 4.1 (1.2) |
| Cluster B | 42 | 5.8 (0.9) | 4.5 (1.2) |
| Obsessive—compulsive | 9 | 1.2 (0.4) | 0.9 (0.5) |
| Avoidant | 10 | 1.4 (0.4) | 1.8 (1.3) |
| Dependent | 2 | 0.3 (0.2) | 0.1 (0.1) |
| Cluster C | 20 | 2.7 (0.6) | 2.8 (1.4) |
| Any personality disorder | 73 | 10.0 (1.0) | 9.0 (2.0) |
| ICD—10 | |||
| Paranoid | 6 | 0.8 (0.3) | 0.3 (0.1) |
| Schizoid | 6 | 0.8 (0.3) | 1.1 (0.6) |
| Emotionally unstable (impulsive) | 13 | 1.8 (0.5) | 0.9 (0.3) |
| Emotionally unstable (borderline) | 3 | 0.4 (0.2) | 0.1 (0.1) |
| Histrionic | 2 | 0.3 (0.2) | 0.05 (0.04) |
| Dissocial | 20 | 2.7 (0.6) | 2.3 (0.8) |
| Anankastic | 8 | 1.1 (0.4) | 0.8 (0.4) |
| Anxious/avoidant | 4 | 0.5 (0.3) | 0.2 (0.1) |
| Dependent | 3 | 0.4 (0.2) | 0.1 (0.1) |
| Any personality disorder | 54 | 7.4 (1.0) | 5.1 (1.1) |
The overall prevalence of ICD-10 personality disorders was 7% (5% weighted) (Table 2). The prevalence of most individual disorders ranged from 1-2%. Dissocial personality disorder was the most frequent (3%), whereas emotionally unstable (borderline), histrionic and dependent personality disorders were uncommon. Although the weighted estimates are generally lower than the unweighted estimates, especially for histrionic personality disorder, the 95% confidence limits of unweighted and weighted estimates overlap.
Association with demographic characteristics
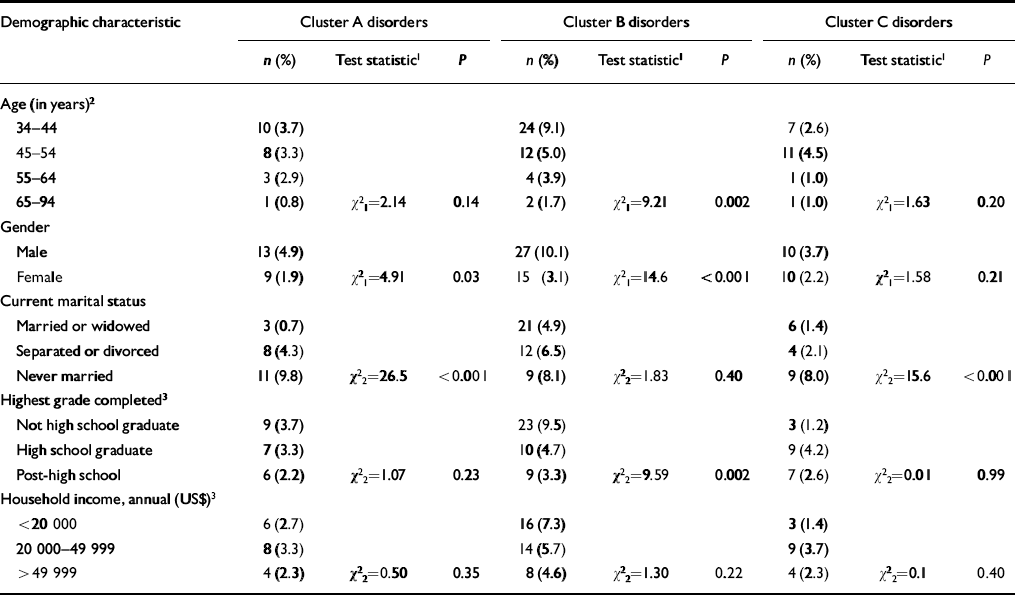
The overall prevalence of cluster A disorders was significantly greater in men than women (Table 3). The prevalence of this cluster also varied across categories of marital status; subjects who were separated or divorced had a greater prevalence, and subjects who had never married had an even greater prevalence of this cluster of disorders, compared with subjects who were married or widowed.
Table 3 Unweighted prevalence of DSM—IV personality disorder clusters, by demographic characteristics — eastern Baltimore, 1997-1999
| Demographic characteristic | Cluster A disorders | Cluster B disorders | Cluster C disorders | ||||||
|---|---|---|---|---|---|---|---|---|---|
| n (%) | Test statistic1 | P | n (%) | Test statistic1 | P | n (%) | Test statistic1 | P | |
| Age (in years)2 | |||||||||
| 34-44 | 10 (3.7) | 24 (9.1) | 7 (2.6) | ||||||
| 45-54 | 8 (3.3) | 12 (5.0) | 11 (4.5) | ||||||
| 55-64 | 3 (2.9) | 4 (3.9) | 1 (1.0) | ||||||
| 65-94 | 1 (0.8) | χ 2 1=2.14 | 0.14 | 2 (1.7) | χ 2 1=9.21 | 0.002 | 1 (1.0) | χ 2 1=1.63 | 0.20 |
| Gender | |||||||||
| Male | 13 (4.9) | 27 (10.1) | 10 (3.7) | ||||||
| Female | 9 (1.9) | χ 2 1=4.91 | 0.03 | 15 (3.1) | χ 2 1=14.6 | <0.001 | 10 (2.2) | χ 2 1=1.58 | 0.21 |
| Current marital status | |||||||||
| Married or widowed | 3 (0.7) | 21 (4.9) | 6 (1.4) | ||||||
| Separated or divorced | 8 (4.3) | 12 (6.5) | 4 (2.1) | ||||||
| Never married | 11 (9.8) | χ 2 2=26.5 | <0.001 | 9 (8.1) | χ 2 2=1.83 | 0.40 | 9 (8.0) | χ 2 2=15.6 | <0.001 |
| Highest grade completed3 | |||||||||
| Not high school graduate | 9 (3.7) | 23 (9.5) | 3 (1.2) | ||||||
| High school graduate | 7 (3.3) | 10 (4.7) | 9 (4.2) | ||||||
| Post-high school | 6 (2.2) | χ 2 2=1.07 | 0.23 | 9 (3.3) | χ 2 2=9.59 | 0.002 | 7 (2.6) | χ 2 2=0.01 | 0.99 |
| Household income, annual (US$)3 | |||||||||
| <20 000 | 6 (2.7) | 16 (7.3) | 3 (1.4) | ||||||
| 20 000-49 999 | 8 (3.3) | 14 (5.7) | 9 (3.7) | ||||||
| > 49 999 | 4 (2.3) | χ 2 2=0.50 | 0.35 | 8 (4.6) | χ 2 2=1.30 | 0.22 | 4 (2.3) | χ 2 2=0.1 | 0.40 |
Cluster B disorders were significantly more prevalent in men than in women. The occurrence of this cluster was inversely related to age, being most prevalent in the youngest age group and least prevalent in the oldest age group. In addition, these disorders were most prevalent in subjects who had not graduated from high school and least prevalent in subjects who continued their education after high school (Table 3).
The occurrence of cluster C disorders was related to current marital status. This cluster was most prevalent in subjects who had never married (Table 3).
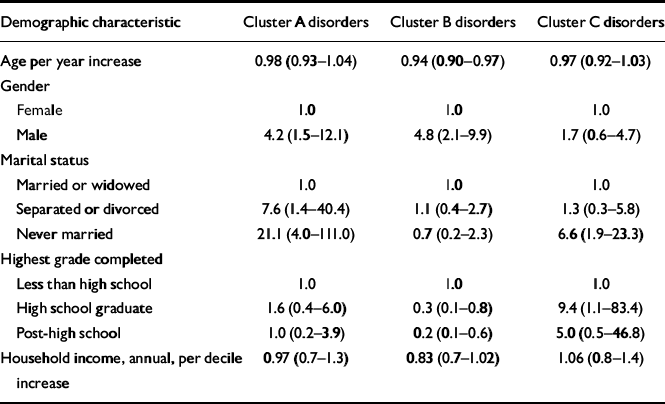
We investigated the relationship between each personality disorder cluster and demographic characteristics in multivariate logistic regression models. As shown in Table 4, the odds of having a cluster A disorder were four times greater in men than women, controlling for all other characteristics in the model. Compared with subjects who were married or widowed, those who were separated or divorced had almost an eightfold increase in the odds of having a cluster A disorder; subjects who were never married were more than 20 times as likely to have one of these disorders.
Table 4 Adjusted odds ratios (and 95% CIs) of DSM—IV personality disorder clusters, by demographic characteristics, eastern Baltimore, 1997-1999
| Demographic characteristic | Cluster A disorders | Cluster B disorders | Cluster C disorders |
|---|---|---|---|
| Age per year increase | 0.98 (0.93-1.04) | 0.94 (0.90-0.97) | 0.97 (0.92-1.03) |
| Gender | |||
| Female | 1.0 | 1.0 | 1.0 |
| Male | 4.2 (1.5-12.1) | 4.8 (2.1-9.9) | 1.7 (0.6-4.7) |
| Marital status | |||
| Married or widowed | 1.0 | 1.0 | 1.0 |
| Separated or divorced | 7.6 (1.4-40.4) | 1.1 (0.4-2.7) | 1.3 (0.3-5.8) |
| Never married | 21.1 (4.0-111.0) | 0.7 (0.2-2.3) | 6.6 (1.9-23.3) |
| Highest grade completed | |||
| Less than high school | 1.0 | 1.0 | 1.0 |
| High school graduate | 1.6 (0.4-6.0) | 0.3 (0.1-0.8) | 9.4 (1.1-83.4) |
| Post-high school | 1.0 (0.2-3.9) | 0.2 (0.1-0.6) | 5.0 (0.5-46.8) |
| Household income, annual, per decile increase | 0.97 (0.7-1.3) | 0.83 (0.7-1.02) | 1.06 (0.8-1.4) |
The multivariate odds of having a cluster B personality disorder were nearly five times greater in men than women. The occurrence of cluster B disorders was inversely related to age; the odds of having one of these disorders declined about 6% for every year increase in age. Furthermore, compared with subjects who had not graduated from high school, those who graduated and those with post-high school education had one-third and one-half the odds of having a cluster B disorder, respectively (Table 4).
The odds of having a cluster C personality disorder were nearly seven times greater in subjects who had never married compared with those who were married or widowed. In addition, subjects who had graduated from high school, but had not continued their education, had a ninefold increase in the odds of having a cluster C disorder, compared with those who were not high school graduates (Table 4).
We repeated these analyses separately in men and women. In general, the magnitude of the relationships between demographic characteristics and personality disorder clusters were similar in men and women. There was, however, one major difference: the relationship between marital status and cluster A disorders was much greater in men than in women. In women, those who had never married did not have a significantly greater risk of having a cluster A disorder, compared to those who were married or widowed (odds ratio 4.3, 95% CI 0.3-71.7, P=0.32). In contrast, men who had never married were at much greater risk of a cluster A disorder (odds ratio 45.9, 95% CI 4.9-432.9, P<0.001).
Based on the results of the logistic regression analyses, we investigated whether specific demographic features would be useful in identifying subgroups having a large proportion of individuals with personality disorders. We found that 8 (22%) of the 37 men who had never married had a cluster A personality disorder: 5 schizotypal; 2 paranoid; and 1 schizoid. Also, 10 (23%) of the 43 males who were younger than 55 years of age and who had not graduated from high school had a cluster B disorder: 9 antisocial and 1 histrionic. In addition, 7 (11%) of the 61 never-married subjects who were high school graduates had a cluster C disorder; 5 avoidant; 2 obsessive—compulsive, and 1 dependent (1 subject had both avoidant and obsessive—compulsive personality disorders).
DISCUSSION
Prevalence of personality disorders
The estimated overall prevalence of DSM-IV disorders in this sample is 9%, which is comparable to estimates of 9-13% obtained from prior studies of non-patient samples that used DSM-III or DSM-III-R criteria (American Psychiatric Association, 1980, 1987; Reference Zimmerman and CoryellZimmerman & Coryell, 1989; Reference Reich, Yates and NduagubaReich et al, 1989; Reference Maier, Lichtermann and KlingerMaier et al, 1992; Reference Samuels, Nestadt and RomanoskiSamuels et al, 1994; Reference Torgersen, Kringlen and CramerTorgersen et al, 2001). However, we found a considerably higher prevalence of antisocial personality disorder and considerably lower prevalences of histrionic and dependent personality disorders than did these prior studies. Different results between these studies could reflect methodological differences, such as in the diagnostic criteria used (DSM-III, III-R, or IV), source of study subjects (community sample or relatives of psychiatric patients and controls), type of assessment (self-report or direct interview), experience and training of examiners for cross-examination of subjects, and collection of information from informants (Reference ZimmermanZimmerman, 1994). In addition, differences in prevalences could reflect differences in the populations from which the samples are drawn. Furthermore, there may have been actual changes in the prevalence of specific disorders over time, as has been proposed for antisocial personality disorder (Reference Cohen, Nestadt and SamuelsCohen et al, 1994). The methodological strengths of the current study are that the subjects were drawn from a community sample; participants were interviewed directly by clinical psychologists with extensive training in cross-examination, and additional information about personality features of study subjects was obtained by interviewing knowledgeable informants.
In general, the weighted DSM-IV prevalence estimates were smaller than the unweighted ones. The biggest differences between unweighted and weighted estimates were found for borderline, histrionic and narcissistic personality disorders. These impulsive disorders are often comorbid with several of the most frequent axis I disorders on which the sample was overselected (e.g. major depression, drug and alcohol use disorders) (Reference Samuels, Nestadt and RomanoskiSamuels et al, 1994; Reference Skodol, Stout and McGlashanSkodol et al, 1999), and the weighting procedure minimised this bias.
The estimated overall weighted prevalence of ICD-10 personality disorders in this sample is 5.1%, similar to the 6.5% reported from the Australian National Survey (Reference Jackson and BurgessJackson & Burgess, 2000). The current study allowed comparison of the prevalence of ICD-10 and DSM-IV disorders in the same subjects evaluated by the same interviewers, using the same instrument, at the same time. We found that, for most of the disorders, ICD-10 prevalence estimates are lower than DSM-IV; the difference was most pronounced for histrionic, dissocial (antisocial) and anxious/avoidant disorders. It is noteworthy that for these disorders, ICD-10 has a greater threshold than does DSM-IV (i.e. a greater proportion of criteria must be present for the diagnosis to be made). These higher diagnostic thresholds, as well as fewer total number of disorders, help explain why the overall prevalence of ICD-10 personality disorders is lower than that of DSM-IV (5% v. 9%).
Demographic correlates
In general, the prevalence of personality disorders in this community sample was higher in men than in women; higher in formerly married and highest in never-married, compared with ever-married individuals; and higher in people who dropped out of high school than in graduates. There also was a striking decline in prevalence with age of the subject. This could reflect a decline in the expression of these disorders with age, especially for the most common cluster B disorders. In addition, individuals born in earlier generations might be less likely to have the disorders (cohort effect). Alternatively, individuals with personality disorders could be less likely to be included in the sample because of attrition (e.g. mortality) (Reference Cohen, Nestadt and SamuelsCohen et al, 1994).
Results from the multivariate analyses indicate that the patterns of demographic associations were different between the three DSM-IV personality disorder clusters. Cluster A disorders were extremely prevalent in men who had never married. Cluster B disorders were most prevalent in younger males who had not completed high school, and cluster C disorders were most prevalent in high school graduates who had never married. These demographic features are useful in identifying subgroups having personality disorders at rates much higher than in the sample at large. Although the cross-sectional nature of this study precludes discriminating precursors from consequences of personality disorders, it is plausible that the cognitive and social difficulties of individuals with cluster A disorders, the impulsive behaviours of individuals with cluster B disorders, and the social anxiety of individuals with cluster C disorders impede marital and educational achievements.
Limitations
Several limitations of the present study must be considered. We were unable to interview subjects in the target sample who were deceased, unable or unwilling to participate, or could not be traced. However, we did find that the sample reflected fairly closely the demographic distribution of the original Epidemiologic Catchment Area sample from 1981, except that the study subjects were significantly younger than those who could not be interviewed; this could have influenced the rates of specific disorders. We also found that, among subjects who had a personality disorder assessment as part of the clinical reappraisal in 1981, the rates of personality disorder clusters did not differ between those who were and were not interviewed in the current study (data not shown).
Although we examined nearly 750 subjects, the sample size precluded investigation of the demographic distribution of rare disorders. Our results for DSM-IV clusters reflect primarily the most prevalent disorders, namely antisocial, schizotypal, avoidant and obsessive—compulsive disorders. Progress in understanding the epidemiology of abnormal personality would benefit from studying greater numbers of subjects with specific personality disorders, either by sampling a larger number of subjects or by developing screening instruments to enrich the sample for specific disorders (Reference Lenzenweger, Loranger and KorfineLenzenweger et al, 1997).
Some subjects may have under— or over-reported specific personality features, either deliberately or because they lacked insight. In addition, the assessment of personality features by subjects and their informants might have been influenced by current symptoms (Reference Reich, Noyes and CoryellReichet al, 1986). However, the examining psychologist did not rely exclusively on a subject's self-report; in making a final assessment, the psychologist took into consideration information provided by an informant who knew the subject over a long period of time, as well as characteristics of the subject that emerged during the interview. Furthermore, the examiner attempted to elicit enduring personality features present over the subject's entire adult life.
In this paper, we have addressed personality disorders categorically, as required by the DSM and ICD and in conformity with clinical tradition. We recognise that a dimensional approach has merit for understanding personality pathology (Reference FrancesFrances, 1982). In future studies, we will investigate the utility of assessing personality from these alternative perspectives.
Implications
Despite these limitations, the results provide estimates of the occurrence and demographic distributions of DSM-IV personality disorders in this community sample. Overall, we estimate that 9% of the subjects have maladaptive patterns of personality traits that are severe enough to cause them, and others around them, difficulties. The results also indicate that there are demographic subgroups of the community in which personality disorders are over-represented. These subgroups would be useful for investigating the determinants and consequences of these disorders, and the service needs of people suffering from them.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
• Approximately 9% of community residents may have a personality disorder.
-
• Certain demographic subgroups have especially high prevalence of personality disorders.
-
• The psychiatric service needs of these subjects needs to be investigated.
LIMITATIONS
-
• Not all selected subjects could be examined.
-
• The sample size precluded investigation of rare disorders.
-
• The assessment of personality features by subjects and informants might be influenced by current symptoms.
Acknowledgements
The authors thank the many subjects participating in the study; Ms Gail Bendit, Ms Stacie Johnson, Ms Carolyn Newcomb and Ms Valerie Wadja-Johnson for conducting personality assessments; Drs Bernadette Cullen, Leigh Ellison, David Gotlib and William Howard for conducting clinical evaluations; and Armand Loranger and Alan Romanoski for consultation on the study. We also thank Ms Margaret Dees, Ms Sandra Hensley, Ms April Ravert and Ms Krista Vermillion for their efforts in coordinating the study.







eLetters
No eLetters have been published for this article.