Few childhood conditions designated as psychiatric disorders are as mired in controversy as attention-deficit hyperactivity disorder (ADHD) (Reference Timimi and TaylorTimimi/Taylor 2004). Diagnosis is generally made on the basis of behavioural checklists, and there are continual debates about the status of such diagnoses. Some mental health professionals see ADHD as a developmental disorder, some as genetically driven and some as a set of symptoms that are indistinguishable from the effects of childhood trauma.
In a previous article in BJPsych Advances (Reference Swanepoel, Sieff and MusicSwanepoel 2016) we argued that the traditional disease model, still dominant in psychiatry, is less than ideal for making sense of a range of psychological issues, such as the effects of early childhood experiences on development. We argued that a model based on evolutionary thinking can deepen understanding and aid clinical practice by showing how behaviours, bodily responses and psychological beliefs tend to occur for reasons that are evolutionarily adaptive, even when these might on first appearance seem pathological.
In the present article we apply this reasoning to ADHD, the most commonly diagnosed neuro-developmental disorder (Reference Thapar and CooperThapar 2016). ADHD, characterised by hyperactivity, impulsivity and inattention, appears to be linked to serious consequences, including educational failure, substance misuse and criminal involvement. The prevalence of diagnosis seems to be increasing, but the reasons for this are hotly disputed (Reference Thapar and CooperThapar 2016).
Here, we do not argue for a single explanation for the widespread occurrence of ADHD. Indeed, we caution against too simplistic an understanding of the condition – including a belief either that all ADHD diagnoses are faulty or that the condition can always be objectively identified and straightforwardly treated with medication. Our hope is that an evolutionary perspective will prove useful to clinicians and others faced with high rates of referral of children (or adults) presenting with symptoms of ADHD. We argue that the environment of evolutionary adaptedness (EEA) did not prepare children to sit still and concentrate for hours every day and that the difficulties that many children experience can be understood in terms of this mismatch (Box 1).
BOX 1 Evolutionary mismatch
When the environment in which an organism lives is significantly different from that in which it evolved, traits that were once adaptive may become pathological. This is termed an ‘evolutionary mismatch’ (Reference CofnasCofnas 2016). One example is that humans evolved to survive food scarcity by craving and eating high-calorie foods when these were available. In the current environment of generally plentiful food, this leads to widespread obesity. Thus, a trait that may have conferred survival advantage in the past may lead to vulnerability to disorder if the environment changes.
ADHD classification and identification
In DSM-4, ADHD fell under ‘disruptive behaviour disorders’, along with oppositional defiant disorder, intermittent explosive disorder and conduct disorder. In DSM-5, ADHD was moved into the category of neurodevelopmental disorders, alongside autism spectrum disorders, intellectual disabilities, communication disorders and motor disorders. A neurodevelopmental disorder is one in which ‘the development of the central nervous system is disturbed’ (American Psychiatric Association 2013). Common characteristics of ADHD are that onset is in early childhood, that there are cognitive as well as behavioural deficits, and that the symptomatic and functional impairments tend to persist. There is typically a preponderance among males of both neurodevelopmental disorders in general and ADHD in particular, and these disorders tend to have a degree of heritability. There is a large overlap of different neurodevelopmental disorders – co-occurrence is the rule rather than the exception (Reference Dyck, Piek and PatrickDyck 2011; Reference Posner, Rothbart and SheesePosner 2014).
In support of a neurodevelopmental view, the Ben-Gurion infant development study showed that sons of fathers with ADHD were more irritable than sons of fathers without ADHD (Reference Auerbach, Atzaba-Poria and BergerAuerbach 2004). The at-risk infants also indicated less clearly what was bothering them, making parenting them more difficult, as evidenced by more inadequate responses to their needs. This was confirmed by Reference Elberling, Linneberg and OlsenElberling et al (2014), who found that mother–infant interaction problems were more likely with at-risk infants. Interestingly, expressed emotion (parental hostility) is child-specific, not parent-specific (Reference Cartwright, Bitsakou and DaleyCartwright 2011).
In two large clinic samples of young people diagnosed with ADHD before school age, only 10% were in the ‘normal’ range of functioning at 15–18 years old – thus there appears to be continuity (Reference Lahey, Lee and SibleyLahey 2016). Persistent classroom inattention is a strong predictor of not obtaining a high school diploma by age 22 (Reference Pingault, Tremblay and VitaroPingault 2011). ADHD in preschool boys has been associated with a 10-point reduction in General Certificate of Secondary Education (age 16) scores (Reference Washbrook, Propper and SayalWashbrook 2013). A 7–12 point average IQ deficit has been noted in individuals with ADHD (Reference Simonoff, Pickles and WoodSimonoff 2007), although there is considerable variability and some individuals with ADHD have an IQ well above average. It has also been shown that preschool ADHD incurs a 17-fold greater economic burden due to increased needs in education, health and social care and makes it more likely that children will be bullies or the victims of bullying (Reference Verlinden, Jansen and VeenstraVerlinden 2015).
There appear to be no discernible differences in the brains of infants with ADHD compared with those of unaffected infants (Reference Ghassabian, Herba and RozaGhassabian 2013); however, by 6–8 years of age, children with ADHD had thinner cortices in the primary somatosensory area (Reference Mous, Muetzel and El MarrounMous 2014). Adults with ADHD have also been found to show abnormal reactivity in this area (Reference Dockstader, Gaetz and CheyneDockstader 2009), although new studies show that there is not necessarily continuity between childhood and adult ADHD. Some have argued that the criterion that ADHD must have started before the age of 12 should therefore be dropped (Reference Caye, Rocha and AnselmiCaye 2016).
Epidemiological issues
One notable fact about ADHD is that rates of recognition, diagnosis and treatment vary widely between and within countries. In 2012, at least 9% of school-aged children in the USA were diagnosed with ADHD; the corresponding figure for France was less than 0.5% (Reference WedgeWedge 2012). The rate of ADHD diagnosis in preschool children varies too, even between quite similar countries: in Denmark it is 1% (Reference Elberling, Linneberg and RaskElberling 2016), whereas it is 3.8% in Iceland (Reference Gudmundsson, Magnusson and SaemundsenGudmundsson 2013). The rates even differ substantially across states in the USA (Reference Fulton, Scheffler and HinshawFulton 2015). They have also increased considerably in many countries, including the USA and UK, in recent decades. Such variations may be due to differences in how the condition is defined and the ways data are gathered (Reference Polanczyk, Willcutt and SalumPolanczyk 2014).
Another significant finding about ADHD is that, in large samples in many countries, there is a hugely increased likelihood of the diagnosis if a child is in the youngest group in a school year cohort. For example, children in Denmark born just before the cut-off for the next year were about 2.5 times more likely to have an ADHD diagnosis than their older classmates (Reference Krabbe, Thoutenhoofd and ConradiKrabbe 2014), and similar results have been seen in a number of other countries, including Germany (Reference Schwandt and WuppermannSchwandt 2016), Canada (Reference Chen, Fortin and PhippsChen 2015), Taiwan (Reference Chen, Lan and BaiChen 2016) and Israel (Reference Hoshen, Benis and KeyesHoshen 2016). At the very least, this suggests an increase in diagnoses in children who are less emotionally mature and less able to be still.
There are also cultural differences in diagnosis rates (Reference Ghosh, Holman and PreenGhosh 2015), which might be explained by a range of factors. Some cultures place a higher value on emotion regulation, for example, so that problems with self-regulation is more common among US than Asian males (Reference Wanless, McClelland and LanWanless 2013). Cultures that value close bodily contact and a quick response to signals of distress, and where there are clear imperatives for children to abide by rules, are ones in which self-regulation tends to develop earlier and more fully. Children in more interdependent cultures are generally also quicker to develop skills in compliance and emotion regulation (Reference Wanless, McClelland and LanWanless 2013). Despite these cultural variations, it is nevertheless clear that there is a group of children, principally boys, who show symptoms (identified as ADHD) that cause concern and whose longer-term trajectories might not be good (Reference Thapar and CooperThapar 2016).
Genes, epigenetics and adaptation
According to evolutionary thinking, behaviour traits that have survived and been passed down the generations must have had adaptive value in the past, and possibly still have today. It is certainly conceivable, for example, that more adventurous individuals in hunter-gatherer society sometimes did better in terms of having viable offspring, perhaps because those individuals were more willing to explore (Box 2). It is worth asking why it could be adaptive for a child to have a version of a gene or set of genes that appears to give rise to such a poor prognosis as ADHD. It seems that such a ‘temperament’ might well be advantageous in some environments. For example, when we examine the genes of descendents of people involved in major migrations of the distant past, we see that a higher proportion than average have the same ‘novelty-seeking’ genetic variant that is associated with ADHD in children (Reference Matthews and ButlerMatthews 2011). One can speculate that being a carrier of that novelty-seeking variant might have aided the likelihood of survival by making such individuals more predisposed to seek new pastures when danger loomed, and hence survive to pass on this variant.
BOX 2 How a gene associated with ADHD may have been adaptive: an example
About one-seventh of a Kenyan tribe, the Ariaal, have the long version of the DRD4 gene, which is associated with novelty-seeking. Pastoralists, some Ariaal still lead a nomadic life, moving from place to place, whereas others now have a more settled way of living. A study found that men with the novelty-seeking allele who lived a nomadic life were well nourished and healthy. In contrast, those with this same allele living a settled life were on average less well nourished (Reference Eisenberg, Campbell and GrayEisenberg 2008). It seems that having the ‘ADHD-inducing’ variant might well be a better option when living a less settled kind of life, and that different genetic variations aid survival or success in some environments but not others.
Although genes alone are most unlikely to cause ADHD symptoms, gene–environment interaction is looking increasingly likely to play a central role. It seems, for example, that carriers of the long allele (7-repeat allele) of the dopamine D4 receptor gene DRD4 are more likely to show ADHD symptoms (Reference Faraone, Doyle and MickFaraone 2001) and this genetic variant also increases the likelihood that children will be novelty-seeking. For these children, insensitive parenting in the early years predicts more externalising behaviours, although this is not the case for carriers of the short variant (Reference Windhorst, Mileva-Seitz and LintingWindhorst 2015). Inheriting this allele also predicts poorer emotion regulation, and indeed more likelihood of disorganised attachment styles (Reference Pappa, Mileva-Seitz and Bakermans-KranenburgPappa 2015). Thus, this and other genes may predispose for ADHD, but will only ever be a partial explanation.
Interestingly, one study looked at hyperactive children who were adopted (Reference Harold, Leve and BarrettHarold 2013). Where these adopted children received sensitive and attuned parenting the symptoms of hyperactivity were not subsequently seen. As so often, we find that experiences and genes, nature and nurture interact to produce their effects (Reference van Ijzendoorn and Bakermans-Kranenburgvan Ijzendoorn 2015). Thus, what we are seeing is that some children are born with more genetic susceptibility for ADHD-type symptoms, but also that certain kinds of environmental influence, such as cultural values or parenting, including closely monitoring a child's behaviour, can hugely reduce the potential effects of genes that otherwise might give rise to worrying behaviours.
Epigenetic research is showing that some children are more susceptible to the influence of their environment than others, what Belsky and others have called ‘the differential susceptibility to rearing’ influence (Reference Belsky, Ellis and BjorklundBelsky 2004). Belsky has argued that successful reproduction of one's genes is more likely if some of one's offspring are more influenced by the current environment than others, because in such scenarios, in the face of both continuity and major change, those offspring will survive to pass on their genes. Thus, we should now think not of vulnerability genes (e.g. for ADHD), but rather in terms of relative plasticity (Reference Belsky and HartmanBelsky 2014), because some individuals are simply more influenced by experiences than others, owing at least in part to their genes.
Environmental influences
There have been a number of studies linking quality of parenting to ADHD diagnosis, concluding that ADHD is related to insecure attachment relationships (e.g. Reference Roskam, Stievenart and TessierRoskam 2014). What much research makes clear (and in accordance with common sense) is that if we expect the environment to be dangerous and unpredictable, we are less relaxed and more hypervigilant and jumpy. Thus, children who grow up in difficult circumstances may be more hyperactive and less likely to settle than children who are used to a relaxed and calm environment. Research (Reference TronickTronick 2007) as well as infant observation over many decades, such as in the Tavistock model (Reference MillerMiller 1989), have shown how even young infants, when feeling less emotionally held, move around more and are less able to concentrate. Infants and children feel calm, more relaxed and stiller when their emotional and physiological states are regulated by an adult attuned to them. Studies show that having a stressful or traumatic childhood is highly predictive of being impulsive, emotionally dysregulated and having poor executive functioning (Reference Ersche, Turton and ChamberlainErsche 2012). In families displaying high levels of negativity, anger or aggression, children tend to struggle much more with emotion regulation (Reference Morris, Silk and SteinbergMorris 2007). Indeed, where there is violence and aggression we see extreme sympathetic nervous system arousal together with externalising behaviours (Reference Panzer and ViljoenPanzer 2005; Reference El-Sheikh, Kouros and ErathEl-Sheikh 2009).
From the perspectives of life history theory (Reference Belsky, Schlomer and EllisBelsky 2012), a speeded up metabolism, less trust, less relaxation, and more suspicion and risk-taking might be adaptive for abusive homes or violent neighbourhoods. In such environments there is little emotional security or expectation that things will work out well. It is a strategy that ensures short-term survival, though at the cost of long-term physical and mental health. Our responses can therefore be seen as adaptive to our environments, triggering neurobiological patterns that have a profound effect on the rest of our lives (Reference Belsky, Schlomer and EllisBelsky 2012). Those born into highly stressed worlds tend to have a speeded up metabolism and more activated stress response systems and develop what some call a ‘fast’, as opposed to a ‘slow’, life history strategy. We see this in a range of other mammals as well as in humans, and it is a strategy that aids survival. Without it, any too trusting and complacent ancestors might well have met a violent end before they had time to reproduce. In many circumstances the best response is to be wary, vigilant and untrusting.
Evidence shows that ADHD symptoms increase in response to adverse social and economic as well as parenting influences. For example, Reference MischelMischel (2014) found that children from low-income families in violent parts of New York's Bronx tended to have below average ability to self-regulate compared with more privileged children. Early severe institutional deprivation is associated with adult ADHD (Reference Kennedy, Kreppner and KnightsKennedy 2016). Other studies have found a link between low socioeconomic status and impaired development of the executive parts of the brain (Reference Noble, Norman and FarahNoble 2005), even linking poverty to chronic stress and neurocognitive outcomes right into adulthood (Reference Evans and SchambergEvans 2009). Indeed, by the age of 6 months, infants from socioeconomically deprived environments have been shown to be less able to pay attention (Reference Clearfield and JeddClearfield 2013). Childhood poverty and the associated stress levels can have a big effect on capacity for emotion regulation, the development of inhibitory brain networks (Reference Kim, Evans and AngstadtKim 2013) and the likelihood of increased risk-taking (Reference Griskevicius, Tybur and DeltonGriskevicius 2011). Being able to defer gratification depends on feeling sufficiently relaxed (high vagal tone) and being helped to bear and regulate one's emotions (Reference Moore and MacgillivrayMoore 2004).
ADHD can be thought of in part as a deficit in executive functioning (Reference BarkleyBarkley 2017) – although many forms of executive function disorder are unrelated to ADHD. Those diagnosed with ADHD struggle, for example, with planning, emotion regulation, focusing, concentrating, putting plans into action – all of which are aspects of executive functioning (Reference BrownBrown 2013). People able to delay gratification have more activity in prefrontal brain regions, central to abstract thinking, planning, working memory and emotion regulation – again, all of which are aspects of executive functioning (Reference BarkleyBarkley 2012). Those with more impulsive character traits tend to lack these prefrontal ‘brakes’ on their impulsivity (Reference McClure, Laibson and LoewensteinMcClure 2004). Instead, more primitive subcortical brain areas are active. This also is seen in trauma and in stressful situations generally, which is partly why many children who display symptoms that fit with ADHD checklists for other reasons are misdiagnosed as having ADHD (Reference DeJongDeJong 2010).
Gender-based differential rates
Why are rates of ADHD typically higher in males than in females? One common evolutionary explanation for differential rates such as this is that males have had to be more risk-taking to compete for mates, since a higher proportion of males than females fail to have children and pass on their genes. Thus, sexual competition between adult males is high, and this can be compounded when males have to leave their families to seek out mates.
Also, research might suggest a trade-off in evolutionary history between the need to be risk-taking and explore and the capacity to concentrate and be still. For example, boys seem to be more sensitive than girls to the consequences of suboptimal parental care. From birth onwards girls on average are better equipped to regulate their emotions and are less badly affected by disruptions in parenting. Parents may need to work harder to imitate and respond to their sons than to their daughters, and researchers have suggested that boys need more input in order to feel emotionally regulated (Reference Tronick, Weinberg, Johnson, Hayes and FieldTronick 2000). Following maternal postnatal depression it seems that boys tend to fare worse, having less capacity for object constancy at 18 months and showing more behavioural problems at school age (Reference Murray, Kempton and WoolgarMurray 1993). Reference SanderSander (2007) looked at newborns separated from their parents and placed with new carers. After a few days the girls had all entrained to their new carers’ day–night rhythms, but the boys took several days longer to adjust, suggesting that they were more vulnerable to disruptions of care.
Reference TronickTronick (2007) found that mothers with depression consistently showed angrier emotional expressions to their sons than to their daughters. By 6 months the boys were gesturing more anxiously and were three times more likely than the girls to resort to self-comforting strategies such as sucking their thumbs. It seems that boys generally are more demanding of their interactive partners. A study in France showed that mothers with a propensity for depression were more likely to become depressed if they had male babies (Reference de Tychey, Briançon and Lighezzolode Tychey 2008), who were presumably more demanding than female ones.
Social changes
Some ADHD symptoms might still (in contemporary society) make adaptive sense, such as being vigilant and wary in the face of violence and prioritising survival and safety over the higher executive functions such as empathy, self-reflection and emotion regulation (Reference MusicMusic 2016).
However, the social environment for children has changed dramatically over the past century or two. Whereas most boys would once have typically learnt a trade from their father or another relative, this all changed with the professionalisation of schooling. One result is that there is a mismatch between the strengths of children with ADHD – i.e. their tendency to explore, to challenge and to try out new ways of doing things – and their environment (today's schools). ADHD is unusual in that its diagnosis is most often made in the context of schooling, with most cases being diagnosed in children between the ages of 6 and 12 (NHS Choices 2016).
The standard model of schooling, in which 20 or more young people of the same age are taught in classrooms for about 5 hours a day, 5 days a week, 200 days of the year from age 6 to 16, certainly runs counter to our evolved behavioural strategies. Furthermore, a child's ADHD symptoms will affect other children in the room and the teacher's very capacity to teach. As the website ADHD Solutions (2017) puts it: ‘a child with ADHD can be extremely challenging’. Schooling therefore favours some young people at the expense of others, including those with ADHD. To add to this, schools, especially primary schools, can be seen as feminised institutions, the large majority of teachers being women. Indeed, in England in 2015, 80% of the total teaching workforce in state-funded schools (primary and secondary) was female (Department for Education 2016). As we have noted, ADHD predominantly affects males: a 2006 survey reported male:female prevalence of child and adolescent ADHD varying from 3:1 in Norway to 16:1 in Austria (ADHD Institute 2016). This gender imbalance decreases in adulthood. It is likely that schools typically favour the sorts of fairly passive, acquiescent behaviour that society all too often deems particularly appropriate for females.
Treatment
Treatment types
The main treatments for ADHD are medication and psychological interventions. Methylphenidate can improve irritability in ADHD (Reference de la Cruz, Simonoff and McGoughFernández de la Cruz 2015), and a Cochrane meta-analysis showed that it also improves teacher ratings of ADHD and does not have serious adverse side-effects, although the data quality is poor (Reference Storeb⊘, Simonsen and GluudStorebø 2016). Psychological interventions for ADHD show small effects on non-blinded outcome ratings, but no effect on blinded ratings (Reference Abikoff, Thompson and Laver-BradburyAbikoff 2015).
There is accordingly much controversy about the medication of ADHD, with two main opposing camps. On the one hand, there is some evidence to show that ADHD has a biological component and responds to medication (at least in the short term) and that children who are treated generally have better educational outcomes and are less likely to misuse drugs or get in trouble with the law (Reference Thapar and CooperThapar 2016). On the other hand, many clinicians argue that normal children are being medicated to make them compliant and ‘less naughty’ and that medication is being used as a form of social control. Even among ourselves as authors, we are not of one mind on this matter.
Newer evidence reveals a differential susceptibility to the development of oppositional defiant disorder and conduct disorder in children genetically more susceptible to developing ADHD (Reference Bakermans-Kranenburg and van IJzendoornBakermans-Kranenburg 2015). The efficacy of interventions might be underestimated or even go undetected as a main effect when it is hidden in gene-by-environment (G × E) analysis. These children will be more likely to develop ADHD and the attendant serious behavioural complications if experiencing low warmth in their relationships with their caregivers – but will be less likely than average children to develop these difficulties if they experience warm parenting. It is therefore too simplistic to just link genetic traits to outcomes: once again, there are significant gene–environment interactions at play.
Ethics
From an ethical point of view, a serious question needs to be asked: ‘Should psychiatrists prescribe medication to help a child to fit into an environment that is not ideal?’ Many ADHD services do not have any behavioural support services to which they can refer. This puts pressure on psychiatrists to prescribe, even if psychological or social measures might be more appropriate. It is also questionable whether prescribing is ethically justifiable when it is undertaken because of the shortcomings of the school environment. Furthermore, there is often a clear conflict of interest between what is best for the child and what is easiest for parents and teachers. In a rare study that examined the views of children with ADHD, Reference SinghSingh (2012) found that, in both the UK and the USA, children wanted more treatment options outside of medication, but that these were not available. The question of informed consent becomes difficult with younger children, who are completely dependent on their parents. More widely, there are important ethical considerations to be addressed by health, education and social care services (Reference RichardsRichards 2013). Some of the complexities that can arise are illustrated by the case vignettes in Box 3.
BOX 3 The range and complexities of children with ADHD: case vignettesFootnote a
Redressing the mismatch
Alex is 17 years old. He was diagnosed with ADHD at age 8 and treated with stimulant medication until he finished his GCSEs at 16. He was able to stop using medication when he went to a football college. He explained that at college they do 2 hours of football training and then break for an hour of, say, maths, before doing another 2 hours of training and then having a lesson of English. He said that this worked very well for him and he was able to sit still and concentrate without needing medication.
The influence of nurture
Nine-year-old Joe, who was on a local authority child protection plan because of neglect by his drug-misusing mother, was treated with stimulant medication for ADHD. After he was placed in foster care, his school work improved dramatically and he was able to stop his medication. One of the reasons for this was that the ‘breakfast’ his mother had assured professionals she was giving him with his stimulant medication before school consisted of a can of caffeinated energy drink.
Successful use of medication
Mohammed, 14 years old, was on the verge of exclusion from school because of his disruptive behaviour in class, fighting in the playground and rudeness to teachers. He had been diagnosed with ADHD at age 8, but his parents had been opposed to medication. The family now agreed to a trial of stimulant medication, which was a resounding success. The boy explained that he was now able to concentrate and think before he acted. He thrived on the positive feedback he was getting at school and his behaviour and attainment improved.
Treat the environment, not the child
Seven-year-old Alfie was being treated with short-acting ADHD medication to cover him at school, but neighbours in the flat below complained about his jumping around in the evenings and at the weekends. Members of the multidisciplinary team agreed that medication should not be prescribed in this instance and decided to write a letter to the local housing office instead.
a These children are fictitious, but representative of individuals we meet in clinical practice.
Conclusions
We believe that an evolutionary perspective, which points out the mismatch between biological predispositions and current environments, including schools, has a lot to add to debates about ADHD diagnosis and treatment. This paves the way for a more informed discussion about whether to medicate or not. Understanding ADHD as a biological variant in some individuals that has adaptive value for living in unpredictable situations may help shift perceptions of the child as being ‘naughty’ to seeing someone caught in an evolutionary mismatch. Behavioural strategies in school, for example, could then focus on allowing the child plenty of physical activity and a fidget toy to fiddle with when they have to sit still, as well as making eye contact with the child before giving instructions and keeping instructions single and simple (for further suggestions see LD Online 2017). Over the longer term, we may need to rethink how schools are organised, conceptualised and run. Increasingly, the emphasis in schooling is only on academic subjects. Subjects that involve movement and the development of physical skills (physical education, metalwork, home economics, etc.) have largely disappeared from the curricula in a number of countries.
It may help for adults with ADHD to understand what their strengths are and to seek jobs where these are valued, for example in sport, adventure tours, the military or any other job where physical activity and rapid decision-making are highly valued.
Of course, there are downsides to having ADHD – individuals are more likely to perform poorly in cognitive tasks, die in accidents and become involved in criminal activity. They are also more likely to follow a fast life history strategy and tend to have more children at a younger age in whom they invest less – this may lead to an intergenerational transmission of problem behaviours linked to a biological susceptibility to ADHD (Reference Thapar and CooperThapar 2016).
In sum, we believe that an evolutionary view can help both professionals and patients understand ADHD in a broader sense, where it can be thought of as both a liability and a strength and where attempts are made to adapt the environment before resorting to medication to adapt the individual.
MCQs
Select the single best option for each question stem
-
1 Viewing ADHD as an ‘evolutionary mismatch’ means that:
-
a there is a single explanation for the widespread occurrence of ADHD
-
b all diagnoses of ADHD are faulty
-
c the condition can always be objectively identified
-
d previous selection pressures have not adapted us to our present environment
-
e diagnosis can made using behavioural checklists.
-
-
2 The fact that ADHD is so much rarer among children in France than in the USA is most likely due to:
-
a the presence of far more child psychiatrists in the USA compared with France
-
b different cultural presumptions between the two countries as to what behaviour constitutes ADHD
-
c better school food in France
-
d higher rates of teenage pregnancy in the USA
-
e higher rates of divorce in the USA.
-
-
3 The most likely explanation why younger children in a school year are more likely to be diagnosed with ADHD is that such children:
-
a are more likely to be bullied
-
b need to go to the toilet more often
-
c have more difficulties sitting still and paying attention to their teachers
-
d are behind their peers in respect of reading and writing
-
e are less likely to make friends with their peers.
-
-
4 It is not true that infants at high-risk of ADHD:
-
a are more irritable than controls
-
b signal their needs less clearly
-
c are parented less effectively
-
d experience more hostility from their parents
-
e have parents who are more hostile in general.
-
-
5 According to evolutionary science, the high prevalence of ADHD in school-aged children can be explained by the concept of:
-
a fast life history, in which the emphasis is on ensuring short-term survival even if at the cost of long-term suffering
-
b mismatch, in which our ancestral environment did not prepare us for current environmental demands
-
c evolutionary trade-off between physical fitness and academic excellence
-
d natural selection of active children
-
e survival of the fittest, which favours children who can work on their own.
-
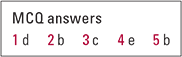
| 1 | d | 2 | b | 3 | c | 4 | e | 5 | b |



eLetters
No eLetters have been published for this article.