Lithium is an effective therapeutic agent in the control of mood in affective disorders (Reference Baastrup and SchouBaastrup & Schou, 1967; Reference Prien, Caffey and KlettPrien et al, 1973; Reference Prien and PotterPrien & Potter, 1990). However, the dramatic success of lithium has been tempered by poor levels of patient compliance (Reference Van PUTTENVan Putten, 1975; Reference Bech, Vendsborg and RaphaelsenBech et al, 1976; Cochran, Reference Cochran1984, Reference Cochran1986). Various factors have been associated with patient compliance in affective disorders (Reference Jamison, Gerner and GoodwinJamison et al, 1979; Reference Connelly, Davenport and NurnbergerConnelly et al, 1982). Harvey and Peet (Reference Harvey and Peet1991) found that a controlled education programme resulted in improved reported tablet omissions and serum lithium levels, suggesting that knowledge and attitudes were related to compliance. Patient satisfaction has been claimed to increase the likelihood of medication compliance in a range of medical settings (Reference DavisDavis, 1968; Reference Francis, Korsch and MorrisFrancis et al, 1969; Reference LeyLey, 1976; Reference Ley, Bradshaw and KinceyLey et al, 1982). However, little is known about the role of satisfaction in compliance in patients suffering from affective disorder.
Lithium non-compliance is a prevalent problem in patients with affective disorder (Reference Strober, Morrell and LampertStrober et al, 1990). The current study aims to investigate the role of the following factors in compliance: patient satisfaction, lithium attitudes and knowledge and prescribed dosage of lithium. Compliance will be examined using a wide range of measures. By evaluating the possible precursors of lithium compliance, this might bring us closer to identifying and managing lithium non-compliance more effectively.
The study
Patients eligible for study entry had a clinical diagnosis of affective illness, were in attendance at a lithium maintenance clinic and had been prescribed with lithium or carbamazepine. Patients with schizoaffective disorder were excluded from the study. A total of 42 patients were approached. Thirty patients gave informed consent (28 lithium, 2 carbamazepine) and comprised 14 women and 16 men whose mean age was 45.3 years (s.d.=12.4; range 25-64 years). Eighteen patients were clinically diagnosed with manic depression and 12 with major depression. The mean age of onset of the affective disorder was 30.4 years (s.d.=12.6; range, 13-60 years). Patients had been taking lithium for an average of 7.7 years (s.d.=9.4; range, 5 months—30 years). Thirty per cent of patients had received formal psychological or psychiatric counselling of significant duration. Twenty-four patients were receiving additional medication (range, 1-9). Data were not available for the 12 patients who declined to give consent to participate.
A staff psychiatrist saw all patients at the lithium maintenance clinic and invited those willing to participate to sign a patient consent form. Ethical approval from the local health board was granted for the study. Questionnaires were administered by an independent assessor during a single appointment, under the supervision of a research clinical psychologist. The following measures were taken.
Compliance assessments
-
(a) Objective — the most recent serum assays were inspected. The number of missed appointments and the percentage of acceptable assays during the previous 12 months were recorded.
-
(b) Subjective — patients were asked, ”How good do you think you are at following doctor's advice for taking your tablets?” (Scale: 1 (excellent) to 7 (extremely poor).) Using the same scale, the psychiatrist rated patients on how well they followed advice for taking their tablets, and documented any history of non-compliance.
Patients were defined as non-compliant if they met both of the following criteria:
-
(a) serum lithium levels below 0.4 mmol/l and/or less than 75% acceptable assays during the previous year;
-
(b) patient rating of compliance below 'average' (4 or lower) and/or a psychiatrist rating of compliance below 'average' (4 or lower).
Other measures
Patients rated the level of care they received at the clinic by completing a satisfaction questionnaire (based on Reference Roghmann, Hengst and ZastownyRoghmann et al, 1979), with 25 statements on a scale ranging from 1 (very strongly agree) to 7 (very strongly disagree). The Lithium Knowledge Test (LKT; consisting of seven multiple choice questions) and the Lithium Attitudes Questionnaire (LAQ; 19 'yes' or 'no' statements) (Reference Peet and HarveyPeet & Harvey, 1991) were administered by the psychiatrist to lithium patients. Prescribed dosage of lithium was also recorded.
Findings
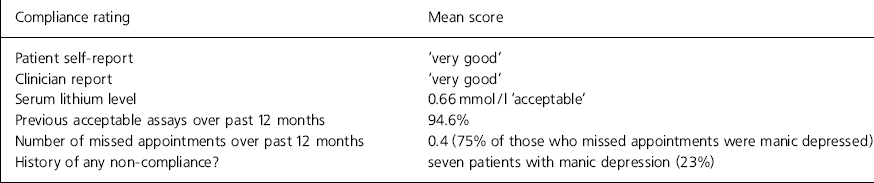
Details of the results of the compliance assessment are shown in Table 1.
Table 1. Compliance assessment
| Compliance rating | Mean score |
|---|---|
| Patient self-report | ‘very good’ |
| Clinician report | ‘very good’ |
| Serum lithium level | 0.66 mmol/l ‘acceptable’ |
| Previous acceptable assays over past 12 months | 94.6% |
| Number of missed appointments over past 12 months | 0.4 (75% of those who missed appointments were manic depressed) |
| History of any non-compliance? | seven patients with manic depression (23%) |
Subjective compliance measures
Approximately half of the patients were rated by themselves and the psychiatrist as 'excellent' at following the doctor's advice for taking their tablets. The mean overall patient response was 'very good' and this was corroborated by the psychiatrist's ratings. Although the psychiatrist rated 7% of patients as 'poor' at taking their tablets, none of the patients rated their compliance levels as 'less than average'.
Serum levels
All patients indicated serum lithium levels above the recommended level of 0.4 mmol/l (range, 0.44-1.07 mmol/l), with the exception of two patients who showed good subjective compliance ratings. Both of the carbamazepine patients were compliant on all measures. Six patients had shown unacceptable serum assays in the past year (range, 50-89% acceptable). Although five patients met one of the two criteria required for non-compliance, none of the patients met both. Thus, according to the specified criteria employed here, all patients were defined as currently compliant.
Missed appointments
Eight (27%) patients had missed appointments during the past year (six of these had been diagnosed with manic depression).
History of non-compliance
The seven patients with a history of non-compliance had exclusively had manic depression (Fisher's exact test, P<0.05) and rated their current compliance levels as significantly poorer than patients with no history of non-compliance (t=-2.1, df=29, P<0.05). They had also been prescribed a significantly larger dose (+500 mg) of lithium (t=-2.8, df=29, P<0.05).
Patient satisfaction
Patients were very satisfied with the care received at the clinic, with a mean score of 1.6 ('strongly satisfied') obtained, suggesting that patients perceived the care positively, and the psychiatrist to be caring and willing to listen to their concerns. Patients were least satisfied about the waiting time before an appointment, and about doctor availability. Patient satisfaction was weakly, although not significantly, related to patient compliance ratings (r=0.28, NS).
Patient scores on questionnaires
Patients achieved a mean overall score of 13.1% in the LAQ (s.d.=14.04; range 0-32%), and a mean of 52.6% in the LKT (s.d.=9.38; range, 18-73%). These scores were not significantly associated with compliance measures. Patients with manic depression scored significantly worse on the LAQ than patients with major depression (t=-2.91, df=21, P<0.01). LKT scores worsened highly significantly (r=-0.55, P<0.01) with increasing age. Lithium attitudes decreased significantly with increased years of taking lithium (r=-0.56, P<0.05), thus patients became more negative about their medication with increased years of use.
Comment
The patients investigated in the present study were all defined as currently compliant. This finding contrasts markedly to previous research, where approximately one-quarter of patients maintained on lithium regimens failed to comply with physicians' instructions (Reference Jamison, Gerner and GoodwinJamison et al, 1979; Reference Connelly, Davenport and NurnbergerConnelly et al, 1982; Reference CochranCochran, 1986). It should be noted that the patients in the current study were all attending a specialist lithium maintenance clinic and this may account for the high compliance rates found here. The lack of association obtained between compliance and diagnostic category is consistent with the findings of Connelly et al (Reference Connelly, Davenport and Nurnberger1982). However, patients who had a history of non-compliance had manic depression, were mostly male and tended to rate themselves as less compliant than those with no history of non-compliance. Thus, poor previous adherence to lithium regimens is generally predictive of poor current levels of compliance, supporting the trends observed by Frank et al (Reference Frank, Prien and Kupfer1985). Patients with a history of non-compliance had been prescribed higher doses of lithium, possibly leading to the increased presence of side-effects (Reference Jamison and AkiskalJamison & Akiskal, 1983; Reference Gitlin, Cochran and JamisonGitlin et al, 1989). Also, more unstable illness may have produced both poorer compliance, causing more symptoms, and a higher subsequent prescribed dosage of lithium. Patients perceived the standard of care received at the clinic to be very high. The weak and non-significant association between patient satisfaction and compliance was inconsistent with the strong association found by Francis et al (Reference Francis, Korsch and Morris1969). In the present study, however, any possible association may have been masked owing to the high ceiling effect for both variables. Also, our sample was small and may not have been representative of all lithium patients, as those who did not participate may have been dissatisfied. Patient knowledge about lithium was moderate and decreased with age. Attitudes toward lithium were generally poor, particularly among patients with manic depression and with increased years taking lithium. In contrast to the findings of Peet and Harvey (Reference Peet and Harvey1991) LKT and LAQ scores were not associated with compliance. The LKT scores were similar to the community psychiatric nurse scores obtained by Peet and Harvey (Reference Peet and Harvey1991), and also similar to the scores of Peet and Harvey's (Reference Peet and Harvey1991) patients after their educational programme.
Cade's (Reference Cade1949) original claim that lithium could be described as the 'magic wand' for patients can only be supported in the presence of adequate current compliance. Patients in the current study were all currently compliant, in striking contrast to previous research. These findings collectively have clinical relevance for existing lithium clinics, and it is suggested that educational interventions should be directed particularly towards older patients with manic depression who have been taking lithium for a number of years.
Acknowledgements
We are indebted to Dr Elaine McCabe, staff psychiatrist, for her support of the study and access to the Lithium Clinic, and also, of course, to the patients who participated in the study.




eLetters
No eLetters have been published for this article.