Introduction
Mental disorders are common and pervasive. Recent systematic reviews have reported high prevalence of mental disorders worldwide, but a comparatively low prevalence in East and Southeast Asia even after adjusting for methodological differences (Ferrari et al., Reference Ferrari, Somerville, Baxter, Norman, Patten, Vos and Whiteford2013; Steel et al., Reference Steel, Marnane, Iranpour, Chey, Jackson, Patel and Silove2014). According to a recent WHO report, the proportion of the global population with depression in 2015 was estimated to be 4.4% while those with anxiety disorders was 3.6%. The total estimated number of people living with depressive and anxiety disorders had increased from 2005 to 2015, which is attributable to the overall growth of the global population, ageing, as well as a proportionate increase in the age groups at which depression is more prevalent (WHO, 2017).
The first Singapore Mental Health Study was initiated in 2010 (Subramaniam et al., Reference Subramaniam, Vaingankar, Heng, Kwok, Lim, Yap and Chong2012a) (hereafter referred to as SMHS 2010). This nationwide epidemiological study found that the prevalence of at least one life-time mood, anxiety, or AUD was 12.0% in the adult population of Singapore (Chong et al., Reference Chong, Vaingankar, Abdin and Subramaniam2012). While this study provided important data pertaining to the mental health of the nation, the findings also serve as a baseline to track the trend of the subsequent mental health status of the general population as well as to evaluate the effectiveness of population-wide interventions/ programmes that had been initiated and implemented in the intervening years.
Epidemiological surveys have compared the prevalence of mental disorders across different countries (Bromet et al., Reference Bromet, Andrade, Hwang, Sampson, Alonso, de Girolamo, De Graaf, Demyttenaere, Hu, Iwata, Karam, Jaur, Kostyuchenko, Lepine, Levinson, Matschinger, Mora, Browne, Posada-Villa, Viana, Williams and Kessler2011; Corbani et al., Reference Corbani, Rucci, Iapichino, Quartieri Bollani, Cauli, Ceruti, Gala and Bassi2017) but only a few studies have made comparisons over time within countries using the same methodology. Repeated surveys conducted across time in Canada (Patten et al., Reference Patten, Williams, Lavorato, Wang, McDonald and Bulloch2016), Korea (Cho et al., Reference Cho, Seong, Park, Chung, Lee, Bae, Ahn, Lee, Bae, Cho, Park, Son, Chang, Hahm, Lee, Sohn, Kim and Hong2015) and Japan (Ishikawa et al., Reference Ishikawa, Tachimori, Takeshima, Umeda, Miyamoto, Shimoda, Baba and Kawakami2018) have reported differing findings. Patten et al. (Reference Patten, Williams, Lavorato, Wang, McDonald and Bulloch2016) found that both the lifetime and 12-month prevalence of major depressive episodes did not increase from 2002 to 2012 in Canada, while Cho et al. (Reference Cho, Seong, Park, Chung, Lee, Bae, Ahn, Lee, Bae, Cho, Park, Son, Chang, Hahm, Lee, Sohn, Kim and Hong2015) reported that the 12-month prevalence of MDD and anxiety disorders increased from 2006 to 2011, while the prevalence of nicotine dependence and AUD decreased in the same period in Korea. Ishikawa et al. (Reference Ishikawa, Tachimori, Takeshima, Umeda, Miyamoto, Shimoda, Baba and Kawakami2018) found that the 12-month prevalence of mood and substance use disorders were slightly higher in the second World Mental Health Japan Survey conducted in 2013–2015) (WMHJ2) as compared to the first World Mental Health Japan Survey conducted in 2002–2006 (WMHJ1) while the prevalence of GAD and post-traumatic stress disorder were significantly lower in the WMHJ2 as compared to WMHJ1. These results suggest that prevalence of mental disorders changes across time and that these changes may be specific to countries/regions.
The second SMHS was carried out in 2016 (hereafter referred to as SMHS 2016) with the intent of tracking the state of mental health of Singapore. The two studies (SMHS 2016 and SMHS 2010) employed the same methodology i.e., similar sampling strategy, same instrument – WMH CIDI 3.0, which was administered using computer assisted personal interviewing (CAPI), and the same trainers were involved in the training of the interviewers and quality assessments of interviews and data using standardised protocols.
The SMHS 2016 aimed to (i) establish the 12-month and lifetime prevalence and correlates of MDD, dysthymia, bipolar disorder, GAD, OCD and AUD (which included alcohol abuse and dependence) and (ii) compare the prevalence of these disorders with reference to data from the SMHS 2010.
Materials and methods
Survey population and subjects
The SMHS 2016 was conducted following the same procedures as the SMHS 2010 (Subramaniam et al., Reference Subramaniam, Vaingankar, Heng, Kwok, Lim, Yap and Chong2012a). This population-based, cross-sectional epidemiological study included Singapore residents aged 18 years and above living in Singapore. The sampling frame was based on a national population registry database of all citizens and permanent residents in Singapore which is updated regularly. A probability sample was randomly selected using a disproportionate stratified sampling design with 16 strata defined according to ethnicity (Chinese, Malay, Indian, Others) and age groups (18–34, 35–49, 50–64, 65 and above). Residents aged 65 and above, Malays and Indians were over-sampled to ensure that sufficient sample size would be achieved to improve the reliability of estimates for the subgroup analysis. The sampling frames used in 2010 and 2016 were independent of each other, since the data is completely de-identified at the completion of the survey, we were unable to determine if some of the participants were common to both surveys.
The sample size numbers were produced by running statistical power calculations for binary proportions to determine what sample sizes are necessary overall, as well as for sub-groups, to produce a precise estimate with a margin of error equal to 0.05 for different disorders. A statistical power of 0.80 was assumed, while the Type 1 error rate is controlled at α = 0.05, as is standard. Note that if Type 2 error = ß, then power = 1- ß. Power calculations for estimated rates of mental disorders were generated from low prevalence (GAD = 0.9%) to high prevalence disorders (MDD = 5.8%) as identified in SMHS 2010 (Chong et al., Reference Chong, Vaingankar, Abdin and Subramaniam2012). The sample size was adjusted to account for deviations from simple random sampling. The estimated design effect (DEFF) after oversampling on age (those aged >65) and ethnicity (Malay and Indian) was 1.942. Realistic sample sizes were assumed (e.g., n = 5,500, 6000 and 6500) and margin of error was then computed for each disorder. We found the target sample size of 6000 adequate to provide sufficient precision to measure the prevalence of all disorders. The margin of error for the overall prevalence estimate was between 0.3% to 0.8%, while the margin of error for the subgroups defined by age and ethnic groups was between 0.7% to 1.8%.
A total number of 6126 respondents were interviewed. The response rate among the eligible adults was 69.0% and the acceptability of the interview was high as there were very few who agreed to begin the interview but did not complete it subsequently (incomplete cases = 25).
Study procedures
An invitation letter was sent to each subject followed by a personal home visit by a trained interviewer to obtain his/her agreement to participate in the survey. Trained interviewers from a survey research company conducted face-to-face interviews with those who agreed to participate in the study. The questionnaires were available in English, Chinese and Malay and respondents were asked to choose the language they were most comfortable with before the interviewer initiated any study related procedures. Those residents who were incapable of doing an interview due to severe physical or mental conditions, language barriers, were living outside the country, institutionalized or hospitalized at the time of the survey, and those who were not contactable due to incomplete or incorrect address, were excluded from the survey.
Questionnaires
WHO-CIDI
The fully-structured CAPI version of the WHO-CIDI 3.0 (Kessler and Ustün, Reference Kessler and Ustün2004) was used in the study. The CIDI 3.0 assesses lifetime and 12-month prevalence of disorders using the definitions and criteria of the DSM-IV (APA, 1994) as well as the International Classification of Disease, 10th Revision (ICD-10) Classification of Mental and Behavioral Disorders (WHO, 1992). A screening section was administered to all respondents. All participants who answered positively to a specific screening question were then referred to the respective diagnostic section of the questionnaire.
Only select modules of the CIDI were included in the survey. These modules were identified based on inputs from a Stakeholder Board comprising representatives from various stakeholders (Ministry of Health, voluntary organizations working with mentally ill clients, clinicians, sociologists, and representatives from the major ethnic groups in Singapore) during SMHS 2010 and the decision to include them was revisited with the policy makers before the current survey. The disorders were selected based on the relevance to the country and its policy-makers and service providers. This approach was also taken to alleviate respondent burden which coupled with the extant stigma towards mental illnesses in Asian populations (Subramaniam et al., Reference Subramaniam, Abdin, Picco, Pang, Shafie, Vaingankar, Kwok, Verma and Chong2017a) could affect the overall response rate. All diagnoses were made using organic exclusions and diagnostic hierarchy rules.
Socio-demographic questionnaire
Data on sex, age, ethnicity (Chinese, Malay, Indian, and Others), marital status (single, married, divorced/separated or widowed), educational level (primary and below, secondary, pre-university/junior college, vocational/ITE, diploma and university), employment status (employed, unemployed and economically inactive i.e., students, homemakers and retirees) and household income was collected. Household income was calculated as the sum of all pre-tax income in the past 12 months, of all family members living in the same household.
Statistical analysis
In order to account for the stratified disproportionate sampling design and ensure that the survey findings were representative of the Singapore adult population, all estimates were weighted to adjust for over sampling, non-response and post-stratified for age and ethnicity distributions between the survey sample and the Singapore resident population in 2014. Descriptive analyses were performed to establish 12-month and lifetime prevalence of mental disorders as well as describe the socio-demographic profile of the study population. Persistence of disorders was estimated with two prevalence ratios; the 12-month prevalence among lifetime cases and 30-day prevalence among 12-month cases (Kessler et al., Reference Kessler, Avenevoli, Costello, Georgiades, Green, Gruber, He, Koretz, McLaughlin, Petukhova, Sampson, Zaslavsky and Merikangas2012). Associations between lifetime mental disorders and socio-demographic variables were examined using logistic regression. To examine the change in prevalence across the two surveys, data from SMHS-2016 were reanalyzed using similar sampling weight as the SMHS-2010 study. Significant differences in prevalence were tested using Chi-square tests followed by pooled logistic-regression analyses (Kessler et al., Reference Kessler, Demler, Frank, Olfson, Pincus, Walters, Wang, Wells and Zaslavsky2005) with time (0 = year 2010, 1 = year 2016) treated as a primary predictor of each disorder after controlling for age, gender and ethnicity. Standard errors (SE) and significance tests were estimated using the Taylor series linearization method. All statistical analyses were performed using the Statistical Analysis Software (SAS) system version 9.3 (Cary, NC, USA).
Results
Socio-demographic characteristics of the sample
Supplementary Table 1 shows the socio-demographic distribution of the sample.
Lifetime and 12-month prevalence and persistence of disorders
Table 1 shows the weighted prevalence of lifetime and 12-month mental disorders in the population. Lifetime prevalence of at least one mood, anxiety or alcohol use disorder was 13.9% (95% CI: 12.7–15.2) in the adult population. The lifetime prevalence of mood disorders was 8.0% (95% CI: 7.0–9.0) while that of anxiety disorders (GAD and OCD only) was 4.8% (95% CI: 4.1–5.6). The prevalence of AUD was 4.7% (95% CI: 3.9–5.5). The 12-month prevalence of any DSM-IV mental disorder was 6.5% (95% CI: 5.7–7.4) and anxiety disorders had the highest 12-month prevalence (3.6%, 95% CI: 3.0–4.3), followed by mood disorders (3.3%, 95% CI: 2.7–4.0).
Table 1. Lifetime and 12-month Weighted Prevalence of Mental Disorders in the Singapore Mental Health Study 2016
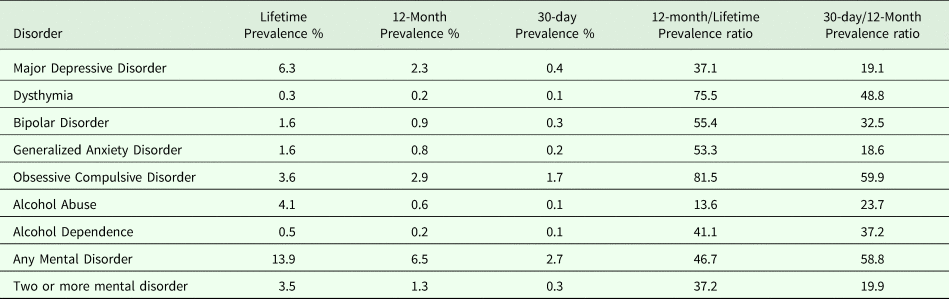
Any mental disorder: Has at least one of the mental disorders assessed by the Composite International Diagnostic Interview in the study.
Table 2 shows the distribution of the lifetime prevalence of mental disorders (as diagnosed by DSM-IV criteria) by age, gender and ethnic status. Table 3 shows the distribution of the 12-month prevalence of mental disorders (as diagnosed by DSM-IV criteria) by age, gender and ethnic status.
Table 2. Prevalence of lifetime mental disorders by age, gender and ethnicity in the Singapore Mental Health Study 2016

Any mental disorder: Has at least one of the mental disorders assessed by the Composite International Diagnostic Interview in the study; GAD Generalised anxiety disorder; MDD Major Depressive Disorder; OCD Obsessive Compulsive Disorder.
Table 3. Prevalence of 12-month mental disorders by age, gender and ethnicity in the Singapore Mental Health Study 2016

Any mental disorder: Has at least one of the mental disorders assessed by the Composite International Diagnostic Interview in the study; GAD Generalised anxiety disorder; MDD Major Depressive Disorder; OCD Obsessive Compulsive Disorder.
Socio-demographic correlates of lifetime mental disorders
The results of logistic regression analyses examining the association of socio-demographic predictors with lifetime prevalence, of DSM-IV disorders are shown in Table 4.
Table 4. Sociodemographic correlates for lifetime mental disorders in the Singapore Mental Health Study 2016

Any mental disorder: Has at least one of the mental disorders assessed by the Composite International Diagnostic Interview in the study; ITE: Institute of Technical Education; Pre-U Pre-University; SGD Singapore Dollar.
Note: Due to lower number of cases, regression was not estimated for dysthymia and alcohol dependence.
The odds of MDD were lower among those aged 50–64 years (OR, 0.3; 95%CI, 0.2–0.6) and 65 years and above (OR, 0.3; 95%CI, 0.1–0.7) as compared to those aged 18–34 years. A similar pattern was observed for OCD and alcohol abuse, with lower odds of OCD and alcohol abuse among those aged 50–64 years (OR, 0.1; 95%CI, 0.1–0.2 and OR, 0.2; 95%CI, 0.1–0.5 respectively) as well as those aged 65 years and above (OR, 0.1; 95%CI, 0.01–0.3 and OR, 0.1; 95%CI, 0.01–0.2) as compared to those aged 18–34 years. Those aged 18–34 years had higher odds of bipolar disorder or any mental disorder as compared to all other age groups.
Malays had higher odds of OCD (OR, 1.6; 95%CI, 1.01–2.4) and lower odds of alcohol abuse (OR, 0.6; 95%CI, 0.4–0.9) as compared to those of Chinese ethnicity. Those who were divorced or separated were more likely to have MDD (OR, 3.9; 95%CI, 2.2–7.1), bipolar disorder (OR, 3.0; 95% CI, 1.1–8.4) and any mental disorder (OR, 2.7; 95% CI, 1.7–4.3) as compared to those who were married.
Changes in lifetime and 12-month prevalence of mental disorders from 2010 to 2016
Lifetime prevalence of mental disorders assessed in SMHS 2016 (13.8%) was significantly higher than that in SMHS 2010 (12.0%) (p < 0.005) (Table 5). Lifetime prevalence of any mood disorder was not different (7.9% vs. 7.0%, p = 0.058), while lifetime prevalence of anxiety disorders (4.8% vs. 3.6%, p = 0.007) and AUD (4.6% vs. 3.6%, p = 0.024) were significantly higher in the SMHS 2016 than in the SMHS 2010.
Table 5. Lifetime prevalence of Mental Disorders in the Singapore Mental Health Study 2010 (n = 6616) and the Singapore Mental Health Study 2016 (n = 6126)

a To compare the prevalence between two surveys, data from SMHS-2016 were reanalyzed using similar sampling weight as the SMHS-2010 study.
b Chi-Square Test.
c Pooled logistic-regression analyses with time (0 = year 2010, 1 = year 2016) treated as a primary predictor of each disorder after controlling for age, gender and ethnicity.
Statistical significant was evaluated at the p value <0.05.
12-month prevalence of any mental disorder increased significantly from SMHS 2010 (4.4%) to SMHS 2016 (6.4%) (Table 6). Prevalence of anxiety disorders was significantly higher (3.6% vs. 1.5%, p < 0.001) in the SMHS 2016 than in the SMHS 2010. The 12-month prevalence of GAD (0.8% vs. 0.4%, p = 0.033) and OCD (2.9% vs. 1.1%, p < 0.001) were significantly higher in SMHS 2016 as compared to SMHS 2010.
Table 6. 12-month prevalence of Mental Disorders in the SMHS 2010 (n = 6616) and the SMHS 2016 (n = 6126)
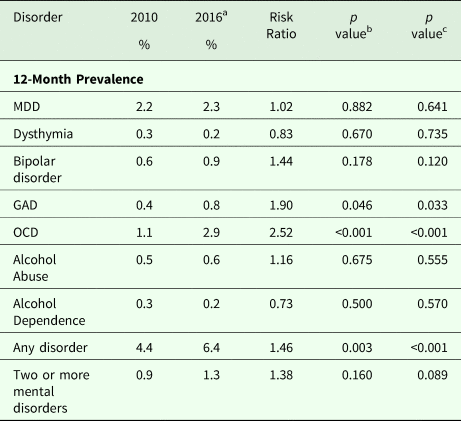
a To compare the prevalence between two surveys, data from SMHS-2016 were reanalyzed using similar sampling weight as the SMHS-2010 study; Statistical significant was evaluated at the p value <0.05.
b Chi-Square Test.
c Pooled logistic-regression analyses with time (0 = year 2010, 1 = year 2016) treated as a primary predictor of each disorder after controlling for age, gender and ethnicity.
Discussion
This study is the second, national mental health survey using a similar methodology as the previous national study to assess and compare the prevalence of mental disorders in Singapore based on a representative sample of community residents.
The high prevalence of lifetime and 12-month OCD is somewhat unique to this population. The 12-month to lifetime persistence ratio was the highest for OCD in the current study and this with the lower 30-day to 12-month prevalence ratio suggests that the disorder is highly persistent due to episode recurrence rather than chronicity. The lifetime and 12-month prevalence of OCD were 0.7% and 0.6% respectively in the Korean population (Cho et al., Reference Cho, Seong, Park, Chung, Lee, Bae, Ahn, Lee, Bae, Cho, Park, Son, Chang, Hahm, Lee, Sohn, Kim and Hong2015). A meta-analysis of studies from China reported the current and lifetime prevalence as 0.9% and 3.2% (Guo et al., Reference Guo, Meng, Huang, Fan, Zhou, Ling, Jiang, Long and Su2016). The authors found that individuals in urban areas were likely to have a higher risk of OCD than those in rural areas. Singapore is a city-state-country and the urban nature may lend to stress in the form of competition, higher workload and a strive for perfectionism which may contribute to the higher risk of OCD (Wu and Cortesi, Reference Wu and Cortesi2009; Soreni et al., Reference Soreni, Streiner, McCabe, Bullard, Swinson, Greco, Pires and Szatmari2014).
Except for OCD, the observed lifetime and 12-month prevalence of the other disorders were still lower than that reported from Western populations but similar to that reported from other Asian countries like Japan and Korea except for AUD which was lower in the Singapore study (Demyttenaere et al., Reference Demyttenaere, Bruffaerts, Posada-Villa, Gasquet, Kovess, Lepine, Angermeyer, Bernert, de Girolamo, Morosini, Polidori, Kikkawa, Kawakami, Ono, Takeshima, Uda, Karam, Fayyad, Karam, Mneimneh, Medina-Mora, Borges, Lara, de Graaf, Ormel, Gureje, Shen, Huang, Zhang, Alonso, Haro, Vilagut, Bromet, Gluzman, Webb, Kessler, Merikangas, Anthony, Von Korff, Wang, Brugha, Aguilar-Gaxiola, Lee, Heeringa, Pennell, Zaslavsky, Ustun and Chatterji2004; Steel et al., Reference Steel, Marnane, Iranpour, Chey, Jackson, Patel and Silove2014). The low prevalence of common mental disorders in Asian countries has been noted in previous studies (Shen et al., Reference Shen, Zhang, Huang, He, Liu, Cheng, Tsang, Lee and Kessler2006; Park et al., Reference Park, Kim and Jhun2008; Ishikawa et al., Reference Ishikawa, Kawakami and Kessler2016). While it is possible that the lower prevalence is a result of under-reporting by the population due to the stigma of mental illnesses (Subramaniam et al., Reference Subramaniam, Abdin, Picco, Pang, Shafie, Vaingankar, Kwok, Verma and Chong2017a), the lower population risk for common mental disorders in Singapore may be due to other factors like cultural stoicism (Liao et al., Reference Liao, Chen, Lee, Lung, Lai, Liu, Lin, Yang and Chen2012) and/or the use of DSM-IV criteria which are pre-dominantly based on affective symptoms rather than the expression of somatic symptoms in Asian populations (Ryder et al., Reference Ryder, Yang, Zhu, Yao, Yi, Heine and Bagby2008). Further, certain social determinants of mental health like high quality antenatal care, compulsory primary education, social support, low rates of crime/violence, low unemployment rates and attributes of built environment promoting health – facets of Singapore – may have influenced the risk of mental disorders.
Our study found a significant increase in the prevalence of both lifetime and 12-month anxiety disorders. The high persistence of OCD coupled with the wide treatment gap in the local population (Subramaniam et al., Reference Subramaniam, Abdin, Vaingankar and Chong2012b) could explain the increase in the 12-month prevalence of OCD. The increase in the prevalence of GAD is however more difficult to explain. It is possible that excessive use of smartphones and associated phenomenon like ‘nomophobia’ (Cheever et al., Reference Cheever, Rosen, Carrier and Chavez2014) may contribute to anxiety in countries like Singapore which has one of the world's highest mobile connectivity (GSMA, 2018). A recent review by De-Sola Gutiérrez et al. (Reference De-Sola Gutiérrez, Rodríguez de Fonseca and Rubio2016), suggests that anxiety may be related with problematic cell-phone use while problematic internet use may be more likely to be associated with depression. However, the current study did not assess the extent of internet or smartphone use in the population; given that excessive use of smartphone and the effects of its restriction are a relatively new phenomenon, more research is needed before drawing any definite conclusions.
Prevalence of lifetime AUD increased from SMHS 2010 to SMHS 2016. Globalization, economic development, adoption of a more liberal culture and normalization of alcohol use have all led to increased drinking in the Asian region (Tang et al., Reference Tang, Xiang, Wang, Cubells, Babor and Hao2013; World Health Organization, Mental Health and Substance Abuse Unit, 2013). Data from WHO suggests that the per capita consumption of alcohol is increasing in China, Malaysia and Singapore (Babor, Reference Babor2014) which in turn can lead to increased prevalence of AUD in the population.
In terms of socio-demographic correlates, younger age was significantly associated with mental disorders. Epidemiological data across studies, using a range of different methods, has shown higher overall rates of depression over time as well as in successively younger birth cohorts (Wittchen and Uhmann, Reference Wittchen and Uhmann2010). A systematic review by (Ferrari et al., Reference Ferrari, Somerville, Baxter, Norman, Patten, Vos and Whiteford2013) identified a ‘time effect’ which suggested that the prevalence of MDD had increased over time. However, the authors acknowledged that other methodological and environmental factors may have resulted in this finding and that further investigation was needed. Other explanations for the higher prevalence include recall bias leading to under-reporting among older adults, lower stigma and better knowledge of mental disorders in the younger cohort leading them to endorse symptoms more openly (Subramaniam et al., Reference Subramaniam, Abdin, Picco, Pang, Shafie, Vaingankar, Kwok, Verma and Chong2017a).
Surprisingly, gender was not strongly associated with MDD in the current study. A few factors could explain the lack of association between gender and MDD in the current study. The last SMHS identified a significant gender difference (Picco et al., Reference Picco, Subramaniam, Abdin, Vaingankar and Chong2017) which was widely reported by the local media. Experts in mood disorder as well as those with a lived experience of mental illness have elaborated on the tendency of males downplaying the symptoms of depression due to gender norms as well as stigmatization (Addis, Reference Addis2008). Extensive coverage could have improved awareness in males. Further examination of our findings revealed that while the prevalence of depression in females did not decrease since 2010, there was an increase in lifetime depression among males from 4.3% in SMHS 2010 to 5.6% in SMHS 2016. Van de Velde et al. (Reference Van de Velde, Bracke and Levecque2010) examined gender differences in depression across 23 countries in Europe (European Social Survey −3) using the Center for Epidemiological Studies Depression Scale. In general women reported significantly higher levels of depression than men, except in Ireland, Finland and Slovakia. Hierarchical linear models found that socioeconomic and family-related factors moderated the relationship between gender and depression. It is thus evident that gender differences in depression vary across countries and both macrosocial and microsocial factors may moderate or mediate the relationship between the two. Future studies need to investigate such contextual factors in further detail in Asian countries to gain a deeper understanding of the gender differences in depression.
Those of Malay ethnicity had lower odds of alcohol abuse and higher odds of OCD as compared to those of Chinese ethnicity. The lower prevalence and risk of alcohol abuse among Malays is readily explained: most Malays in Singapore are Muslims and in Islam, consumption of alcohol is forbidden. However, the higher odds of OCD are difficult to explain and needs further research to elucidate the underlying cause(s).
Educational status was strongly associated with alcohol abuse where those with lower education were more likely to be associated with alcohol abuse. This association has been found in previous studies in the local population (Subramaniam et al., Reference Subramaniam, Abdin, Vaingankar, Phua, Tee and Chong2012c; Reference Subramaniam, Mahesh, Peh, Tan, Fauziana, Satghare, Gupta, Gomathinayagam and Chong2017b) as well as in other countries (Andrade et al., Reference Andrade, Walters, Gentil and Laurenti2002; Park et al., Reference Park, Kim and Jhun2008). It has been suggested that better-educated people are less likely to engage in risky behaviors, such as smoking and drinking, and are more likely to have healthy behaviors related to diet and exercise. It is also possible that those with lower education adopt unhealthy ways of coping with stress which includes alcohol consumption (Zimmerman and Woolf, Reference Zimmerman and Woolf2014). Lastly, education is associated with the wider and more complex issue of socioeconomic status which has a significant influence on alcohol intake, abuse and the general health of populations.
The relationship of unemployment with mental disorders has been established in several studies; unemployment may be a cause or consequence of mental disorders. It is possible that a person with a mental disorder is unable to get or maintain steady employment as a result of the symptoms of the mental disorder. The time that they have to spend on receiving treatment or stigmatization / discrimination on the part of the employers and co-workers (Tsang et al., Reference Tsang, Angell, Corrigan, Lee, Shi, Lam, Jin and Fung2007; Nelson and Kim, Reference Nelson and Kim2011) might pose difficulties in securing and sustaining full employment. On the other hand, the financial strain of unemployment as well as the psychological and emotional impact of unemployment including the strain on family relationships may also lead to mental illness (OECD, 2008).
The findings of the study must be considered in the light of its limitations. It was not possible to establish the prevalence of all mental disorders due to constraints of time, cost, and respondent burden. In this study, we chose those disorders that are likely to have the greatest impact locally through a comprehensive review of the scientific literature, and in consultation with the policy makers in the Ministry of Health of Singapore. However, this limits comparisons with studies which included all the disorders. It is also possible that we inadvertently excluded a disorder which may be associated with significant burden in this population. This was a household sample so it excluded residents of nursing homes, hospitals and prisons. These groups are likely to have higher rates of mental disorders than the general population, but they also comprise a very small proportion of the total Singapore population. About 30% of the sample was not interviewed – this non-response could lead to underestimation of the true prevalence as mental health determinants differ between responders and non-responders (de Winter et al., Reference de Winter, Oldehinkel, Veenstra, Brunnekreef, Verhulst and Ormel2005). Weights were applied to the data to adjust for discrepancies between the sample and population data to account for non-response and sampling variability. Lifetime prevalence estimates are especially subject to recall bias and this may have resulted in lower estimations of the prevalence. Participants may have under-reported or denied their symptoms due to reluctance to share their personal experiences or due to self-stigma. This, however, was minimized in this study by assuring participants that their personal identifiers would not be linked to their individual data and that all results would be presented at the population level and not at the individual level. As this was a cross-sectional study, we are unable to determine incidence of the disorders or the causality and thus are unable to provide explanations for findings that are unique to the population. Lastly, some populations such as those who spoke languages in which the study questionnaires were not available (e.g., Tamil, Chinese dialects) albeit small, would have been excluded from the study thus limiting generalizability to this group.
Conclusion
The present study showed that mental disorders are prevalent in Singapore with 1 in 7 people in the population having a lifetime mood, anxiety or AUD. The high prevalence of OCD and the increase across the two surveys needs to be tackled at a population level both in terms of creating awareness of the disorder and the need for early treatment. Youth emerge as a vulnerable group who are more likely to be associated with mental disorders and thus targeted interventions in this groups with a focus on youth friendly and accessible care centres may lead to earlier detection and treatment of mental disorders. The results also emphasise the need for prospective longitudinal studies focusing both on a deeper understanding of these disorders and assessing the effectiveness of prevention and treatment efforts.
Supplementary material
The supplementary material for this article can be found at https://doi.org/10.1017/S2045796019000179
Availability of data
The data is available on request.
Author ORCIDs
M. Subramaniam, 0000-0003-4530-1096.
Acknowledgements
None.
Financial support
The study was funded by the Ministry of Health Singapore and Temasek Foundation Innovates.
Conflict of interest
The authors have no conflict of interest to declare.
Ethical standards
The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national and institutional committees on human experimentation and with the Helsinki Declaration 1975, as revised in 2008. The study was approved by the National Healthcare Groups’ Domain Specific Review Board. Written informed consent was obtained from all participants and parents or legally acceptable representatives of those aged below 21 years.








