The FFQ is the most frequently used method to assess habitual diets in large-scale epidemiological studies, given that it is relatively inexpensive and less labour demanding when compared with, for example, food diaries or 24-h dietary recalls (24HDR). Dietary glycaemic index (GI) and glycaemic load (GL) have recently been considered as potential risk factors of chronic diseases such as type 2 diabetes, heart diseases and certain types of cancer(Reference Barclay, Petocz and McMillan-Price1). Several epidemiological studies have been conducted investigating the potential role of dietary GI and GL on disease risks(Reference Cust, Slimani and Kaaks2–Reference Silvera, Jain and Howe5). However, none of the FFQ used in these studies are specifically designed for measuring dietary GI and GL and the reproducibility and validity of GI and GL assessed by these FFQ are mostly unknown.
The FFQ used in the Dutch cohorts of the European Prospective Investigation into Cancer and Nutrition (EPIC) study was designed to capture the habitual intake of nutrients and major food items of the Dutch adult population. It is a self-administered semi-quantitative FFQ, contains 178 food items and has also been used by other Dutch studies apart from EPIC(Reference Du, van der A and van Bakel3). The reproducibility and validity of energy, food and nutrient intake have been investigated before(Reference Ocke, Bueno-de-Mesquita and Goddijn6, Reference Ocke, Bueno-de-Mesquita and Pols7). The present study was conducted, using previously collected data, to examine the reproducibility and relative validity of GI and GL estimated by this FFQ.
Methods
Subjects, study design and dietary assessment
A detailed description of the subject recruitment, FFQ, reference method, data collection and data processing has been published previously(Reference Ocke, Bueno-de-Mesquita and Goddijn6). In brief, the subjects were recruited from the study populations of the Dutch part of the EPIC study from four towns in The Netherlands. Of the 960 people invited by mail, 240 (25 %) responded positively, 288 (30 %) refused to participate and 432 (45 %) did not respond. Out of the 240 who responded positively, we selected 134 subjects equally distributed across the four towns, in 20-year age groups and of both sexes. In total, 121 subjects, 63 men and 58 women, completed the study. They were between 23 and 72 years old and had a mean BMI of 25·2 kg/m2. During 1991–2, the FFQ was administered three times with intervals of 6 months by mailing to the participants at home. 24HDR (one for each weekend day and two for each weekday) were administered monthly throughout a year, either face to face or by telephone interview. Nutrient intake was calculated according to the 1993 version of the Dutch food composition table (Nederlands Voedingsstoffenbestand table)(8). The weighted average of 24HDR was calculated with a weight of one for weekdays and two for weekend days.
Glycaemic index and glycaemic load calculation
In order to calculate dietary GI and GL, GI values were assigned to every carbohydrate-containing food item included in the FFQ and 24HDR. The GI database developed in the EPIC study was used as the main source of information. Methodologies used to compile this GI database have been briefly explained before(Reference Cust, Slimani and Kaaks2, Reference Du, van der A and van Bakel3) and a full descriptive paper is going to be published elsewhere(Reference van Bakel, Slimani and Feskens9). In brief, this GI table was compiled from different published sources(Reference Foster-Powell, Holt and Brand-Miller10–12), including 415 values from the international table of GI and GL values from Foster-Powell et al. (Reference Foster-Powell, Holt and Brand-Miller10), 31 published values for British foods(Reference Henry, Lightowler and Strik11), 9 foods from the official website of the GI and GI database from the Sydney University(12) and 20 communicated values for food (groups) with no equivalence in the sources mentioned previously (Wolever T & Brand-Miller J, personal communication). For the Foster-Powell table, a few adaptations were made according to a prioritised selection list of criteria developed by the FAO/WHO Expert Consultation. For example, the items that were not measured under standard conditions were excluded if the items analysed under standard conditions were already available in the table (standard conditions include the following: 50 g or, in the case of low carbohydrate-containing foods; 25 g of available carbohydrate, measurement time for healthy and diabetic subjects of 2 and 3 h, respectively; at least six participants)(Reference van Bakel, Slimani and Feskens9). All food items in the FFQ could be linked to a GI value in this GI database. For about 30 % (258 out of 764) of the items in the 24HDR, no direct link was possible. Therefore, a GI value from other sources had to be assigned. For this, the same sources of information and criteria as used in the compilation of the EPIC GI database were applied. Dietary GI and GL were calculated as the weighted mean of GI and GL from all foods consumed daily using the commonly used formulas(Reference Du, van der A and van Bakel3).
Statistical method
To assess the reproducibility, intra-class correlation coefficients were calculated.
To assess relative validity, Pearson correlation coefficients and weighted κ statistics were calculated for the first FFQ and the average of the 24HDR. Absolute agreement between two measurements was determined using the Bland–Altman method, in which the difference was plotted against the mean of the two dietary assessment methods. Linear regression analysis was performed to investigate whether the bias was proportional to the levels of GI and GL. Residual method was used to adjust for energy intake(Reference Willett13).
Statistical analyses were performed using Statistical Analysis Systems version 9.1 (SAS Institute, Cary, NC, USA) and SPSS 15.0 for Windows (SPSS, Inc., Chicago, IL, USA).
Results
Means and standard deviations of GI and GL as assessed by the FFQ and 24HDR are shown in Table 1. Both GI and GL were roughly normally distributed (data not shown).
Table 1 Mean glycaemic index (GI) and glycaemic load (GL) measured by the Dutch European Prospective Investigation into Cancer and Nutrition FFQ and 24-h dietary recalls (24HDR; n 121)
(Means values and standard deviations)
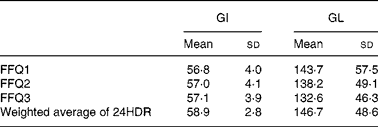
FFQ1, the first FFQ; FFQ2, the second FFQ; FFQ3, the third FFQ.
No sex differences were observed; therefore, analyses were performed in the combined population of men and women. Crude intra-class correlation coefficients between three repeated FFQ were 0·82 for GI and 0·86 for GL (Table 2). Adjusting for energy intake slightly attenuated the correlation coefficients to 0·78 for GI and 0·74 for GL.
Table 2 Reproducibility and relative validity of glycaemic index (GI) and glycaemic load (GL) measured by the FFQ used in the Dutch cohorts of the European Prospective Investigation into Cancer and Nutrition study (n 121)
(Mean values and 95 % confidence intervals)
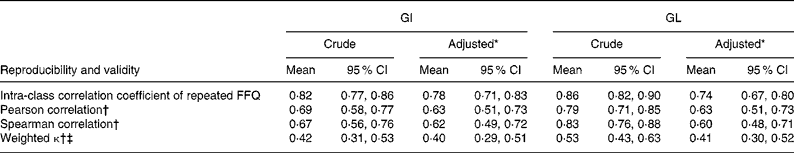
* Adjusted for energy intake.
† The first FFQ (FFQ1) was compared with the average of 24-h dietary recalls (24HDR).
‡ Agreement between quintiles of FFQ1 and the average of the 24HDR.
Pearson correlation coefficients between the first FFQ measurement and the average of 24HDR were 0·69 for GI and 0·79 for GL before adjusting for energy intake, and 0·63 for both GI and GL after the adjustment for total energy intake. Weighted κ values between the first FFQ and the average of 24HDR (in quintiles) were 0·42 for GI and 0·53 for GL. After the adjustment for energy intake, these values changed to 0·40 and 0·41, respectively.
There was a systematic under-reporting in the FFQ for both GI (mean difference 2·2) and GL (mean difference 3·0) when compared with the average of 24HDR (Table 1). A positive association was found between the difference and mean of GI (β = 0·46, 95 % CI 0·28, 0·63; Fig. 1), suggesting the presence of proportional bias in the FFQ: under-reporting at lower GI level and overreporting at higher GI level. No such association was found for GL (β = 0·06, 95 % CI − 0·11, 0·24) (Fig. 2), although fairly wide limits of agreement were observed ( − 43·7 to 37·7). Logarithmic transformation, as proposed by Bland & Altman(Reference Bland and Altman14), did not remove the proportional bias in GI (data not shown).

Fig. 1 Bland–Altman plots of glycaemic index (GI) from the first FFQ and the weighted average of twelve 24-h dietary recalls (24HDR; n 121).

Fig. 2 Bland–Altman plots of glycaemic load (GL) from the first FFQ and weighted average of twelve 24-h dietary recalls (24HDR; n 121).
Discussion
We found good reproducibility and relative validity of GI and GL assessed by the FFQ used in the Dutch EPIC cohorts.
To our knowledge, only three dietary questionnaires have been evaluated for their validity of GI and GL measurements(Reference Barclay, Flood and Brand-Miller15–Reference Murakami, Sasaki and Takahashi17), of which the Swedish FFQ(Reference Levitan, Westgren and Liu16) and the Japanese dietary history questionnaire(Reference Murakami, Sasaki and Takahashi17) have also been evaluated for their reproducibility. The reproducibility of the present FFQ was higher than those found in these two studies. Reproducibility of questionnaires could be influenced by the time interval between administrations. Too long, real change in eating habits may occur, which may underestimate the reproducibility. On the other hand, if the interval is too short, participants may remember the previous questionnaire and therefore respond with the same answers, thus overestimating the reproducibility. Compared with the two previous studies, the time interval of the present study (6 months) is shorter than that from Levitan et al. (Reference Levitan, Westgren and Liu16) (1 year) but longer than the administration time of the Japanese dietary history questionnaire (3 months)(Reference Murakami, Sasaki and Takahashi17).Therefore, most likely the time interval is not the reason for the higher reproducibility observed in the present study.
The validity of dietary assessment methods can be tested with different statistical tools depending on the intended use. The Bland–Altman method has been suggested as the best method for assessing the agreement between two measurement methods(Reference Bland and Altman18). In our case, the plots indicate a systematic underestimation of GL by the FFQ, whereas for GI there is an underestimation at the lower GI level and an overestimation at the higher GI level. However, given that FFQ are, most of the time, used in association studies to rank individuals according to their intake level rather than for measuring the absolute level of intake, calculating correlation coefficients and weighted κ statistics is more appropriate(Reference Masson, McNeill and Tomany19). The validity of GI and GL in the present study, as indicated by the Pearson correlation coefficients, was similar to the results from three previous studies(Reference Barclay, Flood and Brand-Miller15–Reference Murakami, Sasaki and Takahashi17). Only one of these three studies used weighted κ values to assess the agreement between the modified Willett FFQ and three 4-d weighted food records(Reference Barclay, Flood and Brand-Miller15). Values from the present study were higher for GL (0·41 v. 0·30) but lower for GI (0·40 v. 0·53), when compared with their findings. It has been suggested that correlation coefficients of 0·5 or higher indicate that the FFQ has sufficient ability to rank individuals according to their nutrient intake as continuous variable, while for categorical variables, weighted κ values are recommended to be above 0·4 in order to draw valid conclusions(Reference Masson, McNeill and Tomany19).
In conclusion, the findings of the present study support the use of this FFQ in epidemiological studies in which associations of GI and GL, either as continuous or categorical variables, with disease risks are under investigation. However, the proportional bias should be taken into account when using this FFQ to assess absolute GI values.
Acknowledgements
The present study is supported by the DiOGenes project. DiOGenes is the acronym of the project ‘Diet, Obesity and Genes’ supported by the European Community (Contract No. FOOD-CT-2005-513946; http://www.diogenes-eu.org). H. D. conducted the statistical analyses and drafted the manuscript, under the supervision of D. L. v. d. A. and E. J. M. F. M. M. E. v. B. provided the EPIC GI database, L. D. M. V. worked on assigning GI values to the items in 24 HDR data and M. O. developed the FFQ. All co-authors provided comments and suggestions on the manuscript and approved the final version. We thank Vanessa Ginder from the Wageningen University for preparing the dataset ready to be used for the present analyses. None of the authors has a conflict of interest.






