CLINICIAN'S CAPSULE
What is known about the topic?
Community paramedics perform patient assessments to establish physical and psychosocial health, care needs, and health risks at intake.
What did this study ask?
What is assessed in community paramedicine home visit programs at intake, and does it vary across paramedic services?
What did this study find?
We found a wide range of assessment practices suggesting that there may be inconsistencies in care planning and resources across services.
Why does this study matter to clinicians?
Community paramedic training and practice guidelines can build from standardized descriptions of assessment practices to help avoid inconsistent patient care.
INTRODUCTION
Community paramedicine provides patients with access to scheduled or immediate healthcare in collaboration with other providers across the continuum of care.1 Community paramedicine programs are alternatives to traditional ambulance response and transportReference Jensen, Carter and Rose2–Reference Choi, Blumberg and Williams6 and aim to address overburdened emergency departments (ED) and fragmented primary care. They are broadly described by their activities, such as supporting transitions from the ED (e.g., hospital to home), assessing and referring to community-based programs, and providing direct preventive care and chronic disease management support.Reference Lau, Hollander and Cushman7–Reference Drennan, Dainty and Hoogeveen10 Growing evidence supports the effectiveness of community paramedicine programs in reducing 9-1-1 calls, improving chronic disease management, and enhancing access to community-based care.Reference Lau, Hollander and Cushman7–Reference Agarwal, McDonough and Angeles9,Reference Abrashkin, Washko and Zhang11 Despite growing evidence and funding, community paramedicine programs raise important questions about training, knowledge base, consistency of care, scope of care, and paramedic roles in the larger healthcare system.Reference Bigham, Kennedy, Drennan and Morrison3,Reference O'Meara4,Reference Choi, Blumberg and Williams6,12,Reference Leyenaar, Mcleod and Chan13
In the course of their duties, community paramedics perform patient assessments – often in a patient's home – to establish physical, psychological, and psychosocial healthcare needs and risks that may have negative impacts on patient health.Reference Agarwal, McDonough and Angeles9–Reference Abrashkin, Washko and Zhang11,Reference Crockett, Jasiak and Walroth14–Reference Mason, Wardrope and Perrin17 Assessment is the basis for determining an appropriate course of action, such as initiating preventive care, treatment, and/or referral. Community paramedics can identify patient health needs that may only be apparent in the home, including neglect and abuseReference O'Meara, Stirling and Ruest18,Reference Rosen, Lien and Stern19 and other safety concerns. What is assessed in any patient interaction is closely related to paramedic education and clinical training, thus serving as the basis to guide practice.Reference O'Meara, Stirling and Ruest18 Minimal available information on the assessment content and practices of community paramedicine programs limits training and development of care guidelines.
Our objective was to inspect and summarize the content of assessment instruments used at time of patient intake or enrolment in community paramedicine home visit programs to inform efforts to evolve community paramedicine program evaluation, training, continuing education, and care guidelines. We hypothesized that the content of community paramedicine assessments would vary markedly across programs, but that some health domains would be assessed consistently across programs.
METHODS
Study design
We conducted an environmental scan and content analysis of community paramedicine home visit programs in Ontario, Canada, between December 4, 2017, and March 15, 2018. Environmental scans establish a network of healthcare stakeholders and scan the network to better understand policies and practices.Reference Hatch and Pearson20–Reference Graham, Evitts and Thomas-MacLean22 Content analysis can be used to draw inferences about documents, picture, audio, and video.Reference Krippendorff23,Reference Elo and Kyngäs24 Directed content analysis of community paramedicine home visit assessment instruments was used to investigate the state of assessment content across programs.Reference Hsieh and Shannon25 This study was exempt from formal review by the Hamilton Integrated Research Ethics Board based on the lack of direct human participant data collection and low risk.
Setting
We selected the province of Ontario in Canada to conduct the environmental scan given that it has a growing elderly population,26 a fragmented primary care structure,27,Reference Marchildon and Hutchison28 and we were aware that community paramedicine programs have been implemented across the province by many of the 52 paramedic services. In Ontario, community paramedicine programs are eligible for funding through Local Health Integration Networks (LHIN), which are regional administrative organizations of the Ministry of Health and Long-term Care responsible for funding hospitals, long-term care, and home and community care. In isolated instances, paramedic services may initiate community paramedicine programming through other funding sources (municipal, third-party grants, other healthcare partners). There are no mandated or regulated criteria for training, education, or certification for community paramedics. Both primary care and advanced care paramedics may be used to staff community paramedicine programs and conduct patient assessments. We focused on home visit programs given that they are a broadly implemented community paramedicine care model, target similar patients (frequent 9-1-1 users), and use a formal patient assessment at intake. Generalizations of assessment practices across other models of community paramedicine (such as referral or clinic-based programs) would be limited by a relatively small number of comparisons.
Data collection
A short questionnaire was used to determine basic characteristics of community paramedicine programming at each paramedic service (see Box 1). Two investigators (ML and BM) piloted the questionnaire on three services each and revised it after discussing initial responses. The questionnaire was used to request a blank copy of the intake assessment form used for each service's home visit programs (if services operated such a program). We obtained a list of all paramedic services from a roster of recent invitees to a provincial Community Paramedicine Forum (including management, providers, and administrative support) and then contacted each by phone. When required, voicemail messages were left, and follow-up email correspondence was sent. Our protocol stipulated that multiple attempts should be made to provide paramedic services with adequate opportunity to answer questions about their community paramedicine programs and to achieve a minimal response rate of 80% for the environmental scan. Responses were recorded in a securely shared Google form (G Suite for Education, Menlo Park, CA, 2018). Three reminder emails were sent to paramedic services who indicated that they were willing to share their community paramedicine assessment forms but had not done so.
Box 1. Content of the questionnaire used to conduct an environmental scan
1. Service name, contact name, contact position
2. Which statement best reflects community paramedicine programming in your service?
a. Currently providing, no plans for future expansion in the coming year
b. Currently providing, and planning future expansion in the coming year
c. Planning to implement in the coming year, but not presently providing
d. Not providing and not planning to provide in the coming year
3. If community paramedicine programming is presently implemented, which statement best reflects the type of program(s)?
a. Referral program (referral to care provided by other organizations)
b. Clinic-based program
c. Home visit program with remote patient monitoring (example: CPRPMReference Brohman, Green and Dixon29)
d. Home visit program without remote patient monitoring
e. Other
4. If you are planning new or additional community paramedicine programming, which statement best reflects the type of program(s)?
a. Referral program
b. Clinic-based program
c. Home visit program with remote patient monitoring
d. Home visit program without remote patient monitoring
e. Other
5. In general terms, what level of priority does community paramedicine have in your service?
6. Are you willing to share your home visit intake assessment form?
Content analysis
Our content analysis used the International Classification of Functioning, Disability, and Health (ICF), an internationally recognized taxonomy and common language for patient assessment content. The ICF, together with the International Classification of Diseases (ICD), form the Family of International Classifications of the World Health Organization.30 The ICF is a hierarchical taxonomy that categorizes individual assessment items into discrete domains and subdomains.31 It includes four primary domains (Impairments of Body Functions, Impairments of Body Structures, Activity Limitations and Participation Restriction, and Environmental Factors) as well as Demographic Information.31 Demographic Information can include pertinent information about social factors and fits within the ICF framework for providing context to the biopsychosocial model of classification. The domain, Impairments of Body Functions, for example, is divided into subdomains based on the body system involved (mental functions, sensory functions and pain, voice and speech functions, and so on). Each subdomain is further divided into categories according to specific functions of the specific system. For example, mental functions is further divided into specific categories such as consciousness, orientation, memory, and language (to name a few). Content from each of the assessment forms was classified at the category level, but for the purposes of this study, results were reported at the domain and subdomain levels to aid in comparison. We used a deductive approach to categorize paramedic assessment forms with the ICF by classifying each assessment item in each form according to the ICF.Reference Krippendorff23
Three reviewers with expertise in assessment practices (ML, BM, AC) completed the content analysis. The most comprehensive community paramedicine assessment form was used to calibrate processes for classification between the reviewers. Each blank fillable field was considered an assessment item, except where logic dictated that a field would not be filled (i.e., No Known Allergies [NKA] and a list containing medications such as aspirin, penicillin, sulfa). Any items that were determined to not fit within the ICF framework were then classified as “other.” After completing the calibration meeting, two reviewers (ML, BM) conducted content analysis independently following the same approach on all remaining assessment forms. Any items that were classified as “other” were then grouped together under descriptive headings and assigned to an ICF domain. An adjudication meeting was held to resolve any differences in classification by the third reviewer (AC), providing a final classification for all assessment items for all assessment forms. Agreement rates were calculated for the content analysed independently by the two reviewers against the final classification. Basic descriptive statistics were used to report the findings.
RESULTS
Responses from 43 of 52 paramedic services were received to achieve the predetermined response rate for the environmental scan of 80%. Non-responding paramedic services were from a mix of urban and rural areas and of varying sizes. Respondents represented a variety of job classifications from chief to front-line community paramedic. Responses to the level of priority community paramedicine held within a service were mixed. Thirty-seven (86%) paramedic services indicated that they were operating a community paramedicine program, and 28 indicated that they were planning expansion in the coming year. Twenty-six (70%) paramedic services indicated that they provided a home visit program. Of the 26 paramedic services, 24 (92%) indicated that they used a formal intake assessment, with 18 of 26 (69%) providing their intake assessment forms for content analysis. After preliminary screening, it was determined that two forms were actually intake forms that contained solely administrative information from outside referring agencies. Sixteen assessment forms were included for content analysis (Figure 1).
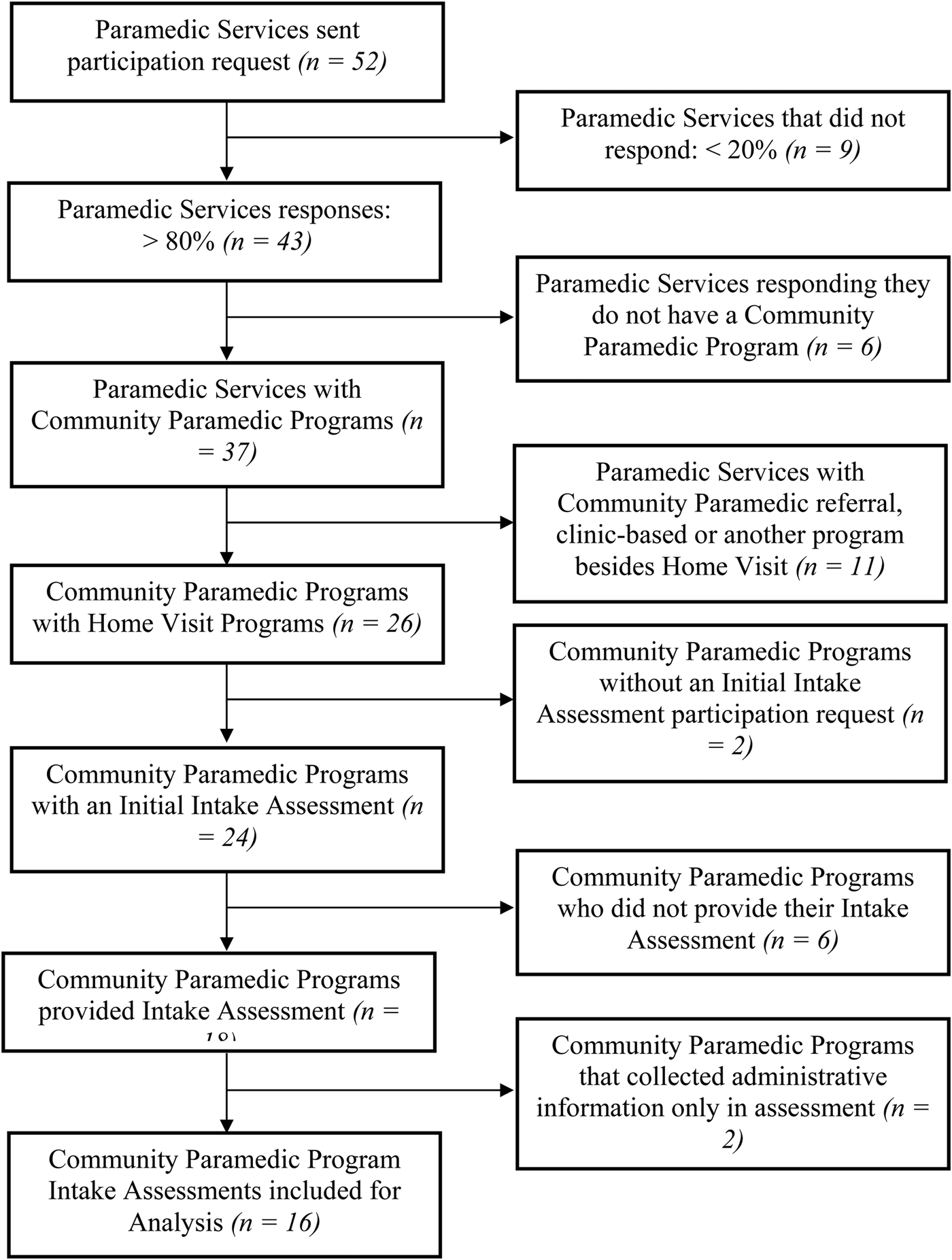
Figure 1. Flowchart illustrating results of environmental scan that produced 16 intake assessment forms for content analysis.
Thirteen assessment forms were either paper-based or fillable PDF format, and three were provided as screenshots from electronic forms. Assessment forms contained between 13 and 252 assessment items (median 116.5, IQR 134.5) (see Appendix A, Table 1). Two assessment forms were exact matches for content.
The agreement percentage at the domain and subdomain levels was high for both raters against the final classification. Rater 1 agreed with the final classification 99.0% and 95.1% of the time at the domain and subdomain levels, respectively. Rater 2 agreed with the final classification 92.6% and 89.1% of the time at the domain and subdomain levels, respectively. Kappa was not calculated because of the adjudication process; we were not interested in the two independent reviewers’ agreement with each other, but with the final classification that was discussed (biasing the element of chance).
At the domain level, all assessments included Demographic Information and assessment of Impairments of Body Functions (relating to different organ systems). Fifteen assessments included the assessment of Environmental Factors (such as physical living conditions or information about social supports). Fourteen assessments (88%) included the assessment of Impairments of Body Structures (relating to different organ systems) and assessment of Activity Limitations and Participation Restriction (such as exercise, hobbies, or taking care of one's health). Appendix A (published as supplementary material online) includes a summary of content within ICF domains and subdomains across community paramedicine home visit assessments.
Most assessments included multiple items classified within multiple subdomains of Impairments of Body Functions. All community paramedicine assessments included function of the cardiovascular, hematological, immunological or respiratory systems, whereas no assessments specifically assessed voice and speech function or functions of the skin and related structures and only one included neuromusculoskeletal and movement-related functions. For any specific subdomain of Impairments of Body Structures, less than half of the community paramedicine assessments included content, and the median number of items within this domain was 3.5 – lowest for any of the four domains. Within the Activity Limitations and Participation Restriction domain, the subdomains with the greatest amount of content were items classified under either mobility or self-care. Environmental Factors was the domain with the highest median number of items, 25. The subdomains within Environmental Factors that had the greatest amount of content were services, systems, and policies, and support and relationships.
Table 1 details the 164 assessment items across the 14 community paramedicine programs that could not be classified at the category level within the ICF (classified as Other). Items were assigned to the closest acceptable ICF domain wherever possible with any remaining items remaining with as a separate Other group. A median of nine items could not be classified for each assessment across three identified domains, Demographic Information, Activity Limitation and Participation Restriction, and Environmental Factors or the separate Other group. Most prevalent in the separate Other group was information about medications followed by information pertaining to either Do Not Resuscitate or Advance Care Planning.
Table 1. Summary of community paramedicine home visit program assessment content (by number of items) classified as “other” by descriptive category (not ICF subdomain)
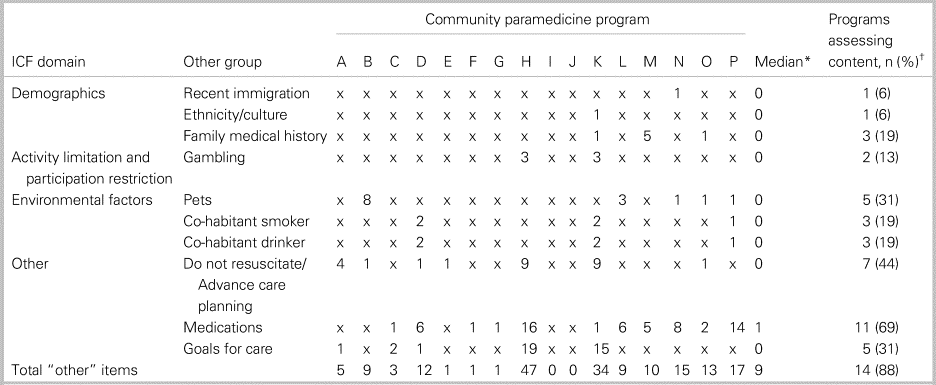
*Median total number of items in each domain and subdomain.
†Proportion of programs assessing at least one item from each category (domain and sub-domain).
XRepresented no data/zero items.
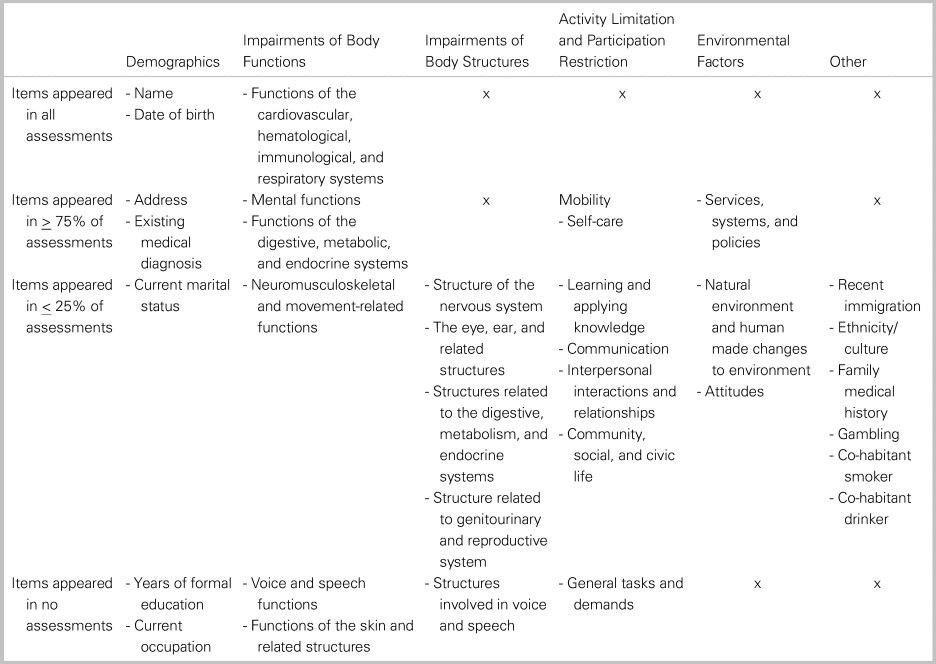
Table 2 summarizes assessment items found within each ICF subdomain by prevalence across community paramedicine home visit programs. Assessment items classified under a small number of subdomains were found to be highly prevalent. These were items pertaining to functions of the cardiovascular, hematological, immunological, and respiratory systems; mental functions; functions of the digestive, metabolic, and endocrine systems; mobility; self-care; services, systems, and policies; and existing medical diagnoses. Many more assessment items were found to be inconsistently assessed across ICF subdomains. The low prevalence for multiple subdomains is reflected in the bottom two rows of Table 2.
Table 2. Prevalence of specific assessment items found within each International Classification of Functioning, Disability, and Health (ICF) domain across community paramedicine home visit assessments
DISCUSSION
We found that most ICF assessment domains are being considered to varying lengths and depths in almost all community paramedicine assessments. The fact that some ICF subdomains were assessed in some community paramedicine programs with one or two items, whereas other community paramedicine programs assessed most ICF subdomains with many items, demonstrates this variety. That all of the included community paramedicine programs had assessment items in the ICF subdomain, functions of the cardiovascular, hematological, immunological, and respiratory systems, suggests that patients enrolled in community paramedicine home visit programs likely have a high prevalence of diseases and conditions associated with these systems such as diabetes, heart disease, chronic obstructive pulmonary disease, or congestive heart failure. Examples of these assessment items included basic vital signs and other diagnostics within a primary care paramedic scope of practice, such as pulse oximetry, 12-lead EKG, or blood glucometry. In general, paramedic training and education includes an emphasis on the life-threats associated with these systems, which likely also contributed to the prevalence of assessment items aligned with this subdomain.32
Limitations
Community paramedicine home visit programs are a new service model for paramedic practice with a relative paucity of clinical guidelines to anchor practice.Reference Bigham, Kennedy, Drennan and Morrison3 Determining the state of current community paramedicine assessment practice through an investigation of intake assessment forms using content analysis relies on certain assumptions about documentation standards and quality assurance processes, which have not necessarily been formalized. By using the ICF as a mechanism to classify content, we also assumed that some baseline criteria for assessment practice could be identified between different paramedic services that may employ paramedics with differing scopes of practice or whose community paramedicine programs may have different designs or objectives. One characteristic of community paramedicine programs is that they are designed in response to locally identified needs,Reference Bigham, Kennedy, Drennan and Morrison3,Reference O'Meara4,Reference Leyenaar, Mcleod and Chan13 meaning that finding differences in assessment practices would be likely. Although this suggests that inherent differences should be expected, a recent review of case management and care planning in community paramedicine home visit programs found that common attributes existed in the patient populations served by these programs across multiple jurisdictions.Reference Leyenaar, Mcleod and Chan13 Although our study was conducted in one province only, sampling 16 different community paramedicine home visit programs likely demonstrates that many of the differences in the scope of paramedic practice and in program design would be expected in a national sample.
Our content analysis of assessment items is an investigation of the opportunity to document assessment findings. It is assumed that the intake assessment conducted by a community paramedic in a home visit program should be completed in full and would be comprehensive enough to direct subsequent care planning without requiring secondary or subsequent assessment. Formalizing the assessment training process for community paramedics and developing assessment guidelines may address whether or not this is true. Even so, differences between community paramedicine program assessments at the subdomain level were observed in many areas. For example, falls prevention is a common focus of community paramedicine programs.1 Falls prevention is a complex and multi-faceted approach where the benefits of assessment of falls risk have been demonstrated.Reference Gillespie, Robertson and Gillespie33 We found that most community paramedicine home visit programs included an assessment of mobility (see Table 2), suggesting a consistency of focus in this area. However, only one of the community paramedicine home visit programs assessed structures related to the genitourinary and reproductive system and genitourinary and reproductive functions. Urinary incontinence is associated with increased odds of fallingReference Chiarelli, Mackenzie and Osmotherly34–Reference Noguchi, Chan and Cumming37 and has been identified as an area of falls prevention programs that requires improved assessment and surveillance,Reference Gillespie, Robertson and Gillespie33 which means that it is a strong area for guideline development and education in the future. Determining whether or not assessment of continence should or should not be assessed by community paramedics requires further inquiry. Similar arguments can be made about the rationale for many of the ICF subdomains where items were not assessed consistently across the community paramedicine home visit programs that participated in our study. If community paramedics are indiscriminately conducting assessments based on ICF subdomains that they perceive as valuable without evidence informed guidelines or education, then it is possible that some may be missing out on key areas that may help them achieve their intended goals for care.
Implications
Community paramedicine home visit assessment forms vary in depth, suggesting that assessment practices and, potentially, care vary across services sampled in Ontario. Previously published studies about community paramedicine programs in OntarioReference Drennan, Dainty and Hoogeveen10,Reference Ruest, Stitchman and Day15 suggest that specific program aims likely contribute to this variation. But, if community paramedicine home visit programs do share similar characteristics (in terms of population served and goals for care), yet assess patients differently, it is difficult to expect that the resulting referrals, care planning, treatments, or interventions will be similar. In turn, such differences will also likely result in inequalities in patient care between different locations. General health assessment practices have evolved to consider multiple disease processes across multiple care settings with the ability to integrate with other care providersReference Wellens, Deschodt and Flamaing38 – all criteria that should guide assessment practices in community paramedicine because patient assessment is foundational to managing care plans, collaborating with other care providers, and providing interventions.Reference Wears and Wolfson39–Reference Colbeck, Maria and Eaton41 The importance of assessment has been demonstrated in traditional paramedic practiceReference Colbeck, Maria and Eaton41 and often underlies program delivery in community paramedicine.Reference Bigham, Kennedy, Drennan and Morrison3,Reference O'Meara4,Reference Leyenaar, Mcleod and Chan13,Reference O'Meara, Stirling and Ruest18 Future work regarding the minimum threshold for intake assessments in community paramedicine home visit programs should engage stakeholders to determine the appropriateness of the assessment areas that have been summarized here.
CONCLUSION
Community paramedicine home visit program assessments cover all domains of the ICF, yet the number of assessment items is often limited and highly variable across services. Relative consistency was observed for the assessment of the functions of the cardiovascular, hematological, immunological or respiratory systems. Other commonly assessed subdomains were mental functions; functions of the digestive, metabolic, and endocrine systems; mobility; self-care; and utilization of support services, systems, and policies. Identifying a minimum threshold for patient assessment and consolidating assessment practices could promote the development of community paramedic training and contribute to clinical guidelines for community paramedic practice. By summarizing the content of assessment instruments and describing the state of current practice in community paramedicine home visit programs, it is possible for community paramedicine programs to reflect on specific assessment domains that may be contributing to achieving their goals for patient care.
Acknowledgements
The authors would like to acknowledge the following Ontario paramedic services and thank them for providing content for analysis; County of Brant Ambulance Services, Dufferin County Paramedic Service, Essex-Windsor Emergency Medical Services, Grey County Paramedic Services, Hamilton Paramedic Services, Lambton Emergency Medical Services, Lanark County Paramedic Services, Leeds-Grenville Paramedic Service, Niagara Emergency Medical Services, Norfolk County Paramedic Services, Prescott Russell Paramedic Service, County of Renfrew Paramedic Services, Superior North Emergency Medical Services, Greater Sudbury Paramedic Services, Toronto Paramedic Services, and York Region Paramedic Services.
Competing interests
None declared.
Prior presentations
2018 Achieving Excellence Together, Annual Conference of Health Shared Services Ontario, Toronto, ON, June 19, 2018
Funding
ML received support for this research from the Canadian Frailty Network, Mitacs, Canadian Institute for Health Research, and the Hamilton Niagara Haldimand Brant Local Health Integration Network (formerly the Hamilton Niagara Haldimand Brant Community Care Access Centre).
Author contributions
ML, AC, and BM conceived the study. ML and BM developed and performed the survey. SP managed survey responses and follow-up. ML, AC, and BM performed the content analysis. ML prepared the first draft of the manuscript. All authors contributed substantially to the design and methodology of the study and to the writing and critical editing of this manuscript.
SUPPLEMENTARY MATERIAL
The supplementary material for this article can be found at https://doi.org/10.1017/cem.2019.379





