Depressive disorders in the perinatal period occur in women of all cultural and ethnic backgrounds. Empirical studies examining the frequency and causes of postnatal depressive disorders have been the focus of numerous researchers during the past 20 years (Reference O'Hara, Zekoski, Kumar and BrockingtonO'Hara & Zekoski, 1988; Reference O'Hara and SwainO'Hara & Swain, 1996). Studies using standardised diagnostic criteria to assess the prevalence of postnatal depression have primarily been conducted in the USA and Western European countries (Reference Kumar and RobsonKumar & Robson, 1984; Reference Watson, Elliott and RuggWatson et al, 1984; Reference O'Hara, Zekoski and PhilippsO'Hara et al, 1990; Reference Campbell and CohnCampbell & Cohn, 1991; Reference Cox, Murray and ChapmanCox et al, 1993). More recently, prevalence studies of postnatal depression have been conducted in non-Western sites such as Japan (Reference Okano, Nomura and KumarOkano et al, 1998; Reference Yoshida, Yamashita and UedaYoshida et al, 2001), Hong Kong (Reference Lee, Yip and ChiuLee et al, 2001), South Africa (Reference Cooper, Tomlinson and SwartzCooper et al, 1999) and Dubai (Reference Ghubash and Abou-SalehGhubash & Abou-Saleh, 1997) with women of more culturally diverse backgrounds.
Prevalence rates for postnatal depression in studies using randomly selected samples of women generally fall between 10% and 15%. A meta-analysis of 59 studies estimated the average prevalence of postnatal depression to be 13% (Reference O'Hara and SwainO'Hara & Swain, 1996). Varying rates across studies were related to the length of the postnatal period being examined and the method of assessment. Higher prevalence rates were significantly associated with longer periods of assessment and the use of self-report instruments, whereas lower rates of postnatal depression were associated with shorter periods of assessment and the use of interview-based measures (Reference O'Hara and SwainO'Hara & Swain, 1996). Although there have been numerous studies examining the frequency of postnatal depression over the years, none has directly compared rates of antenatal and postnatal depression in women from several different countries and cultural backgrounds within the same study. Conducting such a multi-site study eliminates potential confounding factors that exist when comparing rates from individual studies, such as the use of different diagnostic measures or systems, or different times of assessment. A multi-site study of postnatal depression also allows examination of the impact of potential psychosocial and cultural influences on rates of the disorder.
The Structured Clinical Interview for DSM-IV Axis I Disorders (SCID-I; Reference First, Spitzer and GibbonFirst et al, 1994) is a semi-structured diagnostic interview which has been widely used in psychiatric research studies (Reference Spitzer, Williams and GibbonSpitzer et al, 1992; Reference Williams, Gibbon and FirstWilliams et al, 1992a ), including cross-national epidemiological and treatment studies (Reference Williams, Spitzer and GibbonWilliams et al, 1992b ; Reference Weissman, Bland and CaninoWeissman et al, 1996). The interview consists of standardised diagnostic questions arranged in modules corresponding to each DSM-IV Axis I disorder (American Psychiatric Association, 1994). The test-retest reliability of SCID-I generally falls between reported values for similar instruments such as the Diagnostic Interview Schedule and the Schedule for Affective Disorders and Schizophrenia (Reference Williams, Gibbon and FirstWilliams et al, 1992a ; Reference First, Gibbon and SpitzerFirst et al, 1996). In an American study using videotaped interviews, paired raters made independent diagnoses of 75 psychiatric out-patients (Reference Riskind, Beck and BerchickRiskind et al, 1987). The percentage agreement between raters using the SCID-I was 82% (κ=0.72) for major depressive episode and 86% (κ=0.79) for generalised anxiety disorder.
Reliability studies involving the SCID-I have also been conducted in countries other than the USA. In a Norwegian study, interrater reliability was excellent for the diagnoses of major depressive episode and generalised anxiety disorder with reported κ values of 0.93 and 0.95, respectively (Reference Skre, Onstad and TogersenSkre et al, 1991). Similarly, adequate interrater reliability using a Portuguese translation of the SCID-I was demonstrated in a Brazilian study: for major depressive episode,κ=0.88 (Reference Del-Ben, Rodrigues and ZuardiDel-Ben et al, 1996). These two studies demonstrate that the SCID-I can be used reliably with non-American samples. High interrater reliability using the SCID-I and similar structured interviews has also been demonstrated in studies of women in the postnatal period (Reference O'Hara, Zekoski and PhilippsO'Hara et al, 1990; Reference Wenzel, Gorman and O'HaraWenzel et al, 2001). In an American study examining anxiety and depressive symptoms in women postpartum, interrater agreement for major depressive disorder using the SCID-I was 84%,κ=0.67 (Reference Wenzel, Gorman and O'HaraWenzel et al, 2001).
For the Transcultural Study of Postnatal Depression (TCS-PND), the non-patient research version (SCID-I/NP) was adapted to make it more suitable for use with women in different countries and cultures. Major adaptations included deletion of modules that were not part of the project aims, the addition of new screening questions to the screening module, development of alternative psychosis and mania screening questions, insertion of a module to record the interviewee's smoking history, and replacement of the summary score sheets with a newly developed SCID recording form. Minor adaptations included rewording the original screening questions for alcohol misuse or dependence, substance misuse or dependence and obsessive-compulsive disorder, and revising the overview section to include an expanded section on psychiatric treatment history.
The final modified version used in this study for the assessment of postnatal depression, the SCID-PND, included the following modules: overview; smoking history; screening questions; major depression - current and past; dysthymia; alcohol use disorders; non-alcohol substance use disorders; panic disorder; agoraphobia; social phobia; specific phobia; obsessive-compulsive disorder; post-traumatic stress disorder; acute stress disorder; generalised anxiety disorder; somatisation disorder; anorexia nervosa; bulimia nervosa; and the mood differential module. Lifetime diagnoses of these disorders were assessed at the antenatal interview. At the postnatal interview the diagnostic assessment covered the period between the antenatal and postnatal interviews.
Transcultural Study of Postnatal Depression
The aim of the TCS-PND was to develop (or modify), translate and validate research instruments that could be used in future studies of postnatal depression in different countries and cultures. The instruments were chosen to assess key aspects of the maternity experience, namely clinical diagnosis, the psychosocial context of pregnancy and motherhood, maternal attachment style, mother-infant interaction, the child's environment, and health service structure, use, and its associated costs. The modified and translated research tools were piloted to test how well they worked in a perinatal setting and in different languages and populations. This paper reports on the development of the SCID-PND and its piloting on women from middle or late pregnancy to about 6 months after delivery.
METHOD
Study sites
Ten research centres in eight countries participated in this study: Bordeaux and Paris (France), Dublin (Ireland), Florence (Italy), Iowa City (USA), Keele and London (UK), Porto (Portugal), Vienna (Austria) and Zurich (Switzerland). Details are given by Asten et al (Reference Asten, Marks and Oates2004, this supplement).
Sample
Although recruitment methods varied among sites (Reference Asten, Marks and OatesAsten et al, 2004, this supplement), generally women who were in their second or third trimester of pregnancy were approached at antenatal clinics or childbirth preparation classes and invited to participate in a prospective study examining the psychosocial aspects of postnatal depression. Informed consent was obtained from those interested in participating. Antenatally 296 women were interviewed, 261 of whom also completed a postnatal interview. Demographic characteristics of the sample are described by Asten et al (Reference Asten, Marks and Oates2004, this supplement).
Procedure
Participants were first interviewed during the third trimester of pregnancy, on average at 34 weeks' gestation (mean 34.4 weeks, s.d.=3.5) across the ten centres. With the exception of the Zurich group, women were interviewed again, on average, at 26 weeks after delivery (mean 25.8 weeks, s.d.=6.5). Women in Zurich were interviewed at 17 weeks postnatally on average (mean 17.0 weeks, s.d.=1.6).
Other measures
The Edinburgh Postnatal Depression Scale (EPDS) is a ten-item self-report measure developed to screen and identify women who may be experiencing postnatal depression (Reference Cox, Holden and SagovskyCox et al, 1987). The measure has been used widely in European studies of postnatal depression (Reference Holden, Sagovsky and CoxHolden et al, 1989; Reference Murray and CarothersMurray & Carothers, 1990; Reference Thorpe, Dragonas and GoldingThorpe et al, 1992; Reference Cooper, Murray, Murray and CooperCooper & Murray, 1994; Reference Augusto, Kumar and CalheirosAugusto et al, 1996; Reference Wickberg and HwangWickberg & Hwang, 1996; Reference Appleby, Warner and WhittonAppleby et al, 1997; Guedeney & Fermanian, 1998; Reference Benvenuti, Ferrara and NiccolaiBenvenuti et al, 1999) and has been validated for use in postpartum studies of women in several other countries (Reference Boyce, Stubbs and ToddBoyce et al, 1993; Reference Pen, Wang and JinPen et al, 1994; Reference HoltHolt, 1995; Reference Areias, Kumar and BarrosAreias et al, 1996). Although the measure was developed as a screening instrument, a cut-off score of 12/13 identifies women who are most likely to be experiencing post-partum depression (Reference Cox, Holden and SagovskyCox et al, 1987). The measure also has been validated as a screening measure for depression during pregnancy (Reference Murray and CoxMurray & Cox, 1990).
Training
Training in the use of the adapted SCID-I followed a standard approach that has been used to train clinical interviewers in various epidemiological and intervention studies over the past 20 years (O'Hara et al, Reference O'Hara, Zekoski and Philipps1990, Reference O'Hara, Stuart and Gorman2000). Research staff from all participating centres underwent at 2-day SCID-PND training workshop held in Keele (UK) in March 1998. Training included an overview of administration guidelines and descriptions of individual modules and symptom criteria for DSM-IV Axis I disorders (American Psychiatric Association, 1994). Workshop participants also viewed and rated a videotaped SCID-I interview. All centres were familiar with the user's guide for the SCID-I (Reference First, Spitzer and GibbonFirst et al, 1994). Subsequent workshops in Paris, the Tyrol, Florence, Manchester and Dublin allotted time to discuss administration and rating questions and issues related to the SCID-PND. No formal reliability analysis was conducted.
Analyses
Point and adjusted 6-month period prevalence rates were examined for three diagnostic categories of postnatal depression and anxiety and an additional non-diagnostic category that is likely to be indicative of perinatal depression. The broadest diagnostic category, ‘caseness’, included participants who met DSM-IV criteria for generalised anxiety disorder, minor depressive disorder or major depressive disorder. The second diagnostic category, ‘depression’, included participants who met DSM-IV criteria for minor or major depressive disorder. The third diagnostic category, ‘major depression’, included those who met criteria for major depressive disorder only. A final category, ‘EPDS 13+’, included participants who scored 13 or above on the EPDS. This is the cut-off score found to have the best specificity and sensitivity in detecting women who might be experiencing postnatal depression (Reference Cox, Holden and SagovskyCox et al, 1987).
Point prevalence rates were computed for each centre for caseness, depression, major depression and EPDS 13+ at both the antenatal and postnatal assessment points. Period prevalence rates covering the interval between the antenatal and postnatal interviews were computed for caseness, depression and major depression. However, owing to significant variation in the time between interviews among centres (range 21.4-40.4 weeks; F (7,246)=59.15, P<0.001), period prevalence rates were adjusted to estimated 6-month period rates and used in χ2 analyses (or Fisher's exact test when necessary) to compare rates between centres. Because the sample in Keele consisted of only five women, data from the Keele and London centres were combined.
RESULTS
Antenatal point prevalence rates
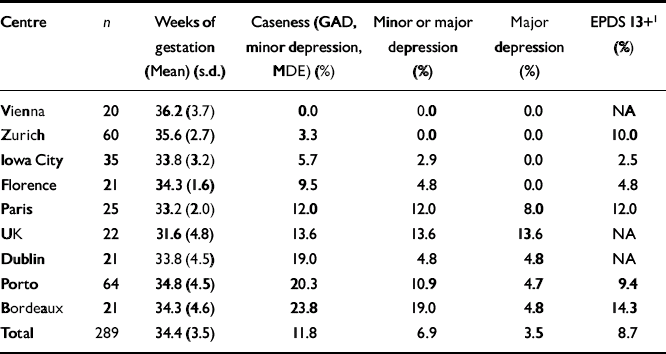
The overall antenatal point prevalence rate for caseness was 11.8%, the rate for depression was 6.9%, the rate for major depression was 3.5% and the rate for EPDS 13+ was 8.7%. Rates for each centre are presented in Table 1.
Table 1 Antenatal point prevalence rates
| Centre | n | Weeks of gestation (Mean) (s.d.) | Caseness (GAD, minor depression, MDE) (%) | Minor or major depression (%) | Major depression (%) | EPDS 13+1 |
|---|---|---|---|---|---|---|
| Vienna | 20 | 36.2(3.7) | 0.0 | 0.0 | 0.0 | NA |
| Zurich | 60 | 35.6(2.7) | 3.3 | 0.0 | 0.0 | 10.0 |
| Iowa City | 35 | 33.8(3.2) | 5.7 | 2.9 | 0.0 | 2.5 |
| Florence | 21 | 34.3(1.6) | 9.5 | 4.8 | 0.0 | 4.8 |
| Paris | 25 | 33.2(2.0) | 12.0 | 12.0 | 8.0 | 12.0 |
| UK | 22 | 31.6(4.8) | 13.6 | 13.6 | 13.6 | NA |
| Dublin | 21 | 33.8(4.5) | 19.0 | 4.8 | 4.8 | NA |
| Porto | 64 | 34.8(4.5) | 20.3 | 10.9 | 4.7 | 9.4 |
| Bordeaux | 21 | 34.3(4.6) | 23.8 | 19.0 | 4.8 | 14.3 |
| Total | 289 | 34.4(3.5) | 11.8 | 6.9 | 3.5 | 8.7 |
Antenatal point prevalence rates for caseness ranged from 0% in Vienna to 23.3% in Bordeaux. The rates of caseness in Bordeaux and Porto were significantly higher than the rate in Vienna (P=0.048 and P=0.032, respectively), and the rate in Zurich was significantly lower than rates in Porto (P=0.004), Dublin (P=0.037) and Bordeaux (P=0.011). Antenatal point prevalence rates for depression ranged from 0% in Vienna and Zurich to 19% in Bordeaux. Rates were significantly lower in Zurich than in Bordeaux (P=0.004), Paris (P=0.023), Porto (P=0.013) and the UK (P=0.017). Although Vienna had no case of depression at the antenatal interview, statistical comparisons with the other centres were not significant, probably because of the small sample sizes. For major depression, antenatal point prevalence rates ranged from 0% in Vienna, Zurich, Florence and Iowa City to 13.6% in the UK. The difference in rates was significant between only Zurich and the UK (P=0.017). The point prevalence rates of antenatal depression indicated by a score of 13+ on the EPDS ranged from 2.5% in Iowa City to 14.3% in Bordeaux, with no significant difference between centres.
Overall, the broadest diagnostic, caseness, had a higher point prevalence rate than the other two diagnostic categories, depression and major depression, at the assessment during pregnancy. This is not surprising since caseness included not only diagnoses of major and minor depression, but of generalised anxiety disorder as well. Vienna and Zurich had the lowest rates of antenatal depression and anxiety examined in this study, whereas Bordeaux, Porto and Dublin had the highest rates of antenatal depression and anxiety.
Postnatal point prevalence rates
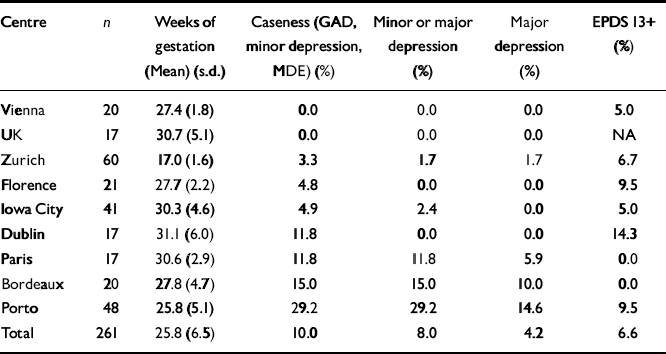
The overall postnatal point prevalence rate for caseness was 10.0%, that for depression was 8.0%, that for major depression was 4.2%, and that for EPDS 13+ was 6.6%. Rates for individual centres are presented in Table 2.
Table 2 Postnatal point prevalence rates
| Centre | n | Weeks of gestation (Mean) (s.d.) | Caseness (GAD, minor depression, MDE) (%) | Minor or major depression (%) | Major depression (%) | EPDS 13+ (%) |
|---|---|---|---|---|---|---|
| Vienna | 20 | 27.4(1.8) | 0.0 | 0.0 | 0.0 | 5.0 |
| UK | 17 | 30.7(5.1) | 0.0 | 0.0 | 0.0 | NA |
| Zurich | 60 | 17.0(1.6) | 3.3 | 1.7 | 1.7 | 6.7 |
| Florence | 21 | 27.7(2.2) | 4.8 | 0.0 | 0.0 | 9.5 |
| Iowa City | 41 | 30.3(4.6) | 4.9 | 2.4 | 0.0 | 5.0 |
| Dublin | 17 | 31.1(6.0) | 11.8 | 0.0 | 0.0 | 14.3 |
| Paris | 17 | 30.6(2.9) | 11.8 | 11.8 | 5.9 | 0.0 |
| Bordeaux | 20 | 27.8(4.7) | 15.0 | 15.0 | 10.0 | 0.0 |
| Porto | 48 | 25.8(5.1) | 29.2 | 29.2 | 14.6 | 9.5 |
| Total | 261 | 25.8(6.5) | 10.0 | 8.0 | 4.2 | 6.6 |
Postnatal point prevalence rates for caseness ranged from 0% in Vienna and the UK to 29.2% in Porto. Rates in Porto were significantly higher than those in five of the eight other centres (Vienna, P=0.007; UK, P=0.014; Zurich, P<0.001; Florence, P=0.027; Iowa City, P=0.003). Postnatal point prevalence rates for depression ranged from 0% in Vienna, Dublin, Florence and the UK to 29.2% in Porto. The rate in Porto was significantly higher than that in all the other centres, except Bordeaux and Paris (P range <0.001-0.014). The rate in Bordeaux was also significantly higher than that in Zurich (P=0.046). Current postnatal major depression rates reached a high of 14.6% in Porto with five of the other eight centres reporting no case of major depression at the time of the postnatal interview. The rate for Porto was significantly higher than rates in other centres only for Zurich and Iowa City (P=0.021 and 0.014, respectively), probably because of small sample sizes in the other centres. Postnatal point prevalence rates as indicated by EPDS 13+ ranged from 0% in Bordeaux and Paris to 14.3% in Dublin.
As with overall rates of caseness, depression and major depression during pregnancy, postnatal point prevalence rates for caseness were higher than the rates for the pure categories of depression and major depression. At the postnatal assessment, it was clear that rates of diagnostic depression and anxiety were highest in Porto and Bordeaux. Ironically, Bordeaux along with Paris had the lowest rates of women scoring 13+ on the EPDS at post-partum assessment, although both centres recorded a significant number of women meeting DSM-IV criteria for major or minor depression at that interview. A possible explanation for this discrepancy is that the French validation study of the EPDS found lower cut-off scores to be appropriate in community postnatal assessments (Guedeney & Fermanian, 1998).
Six-month period prevalence rates
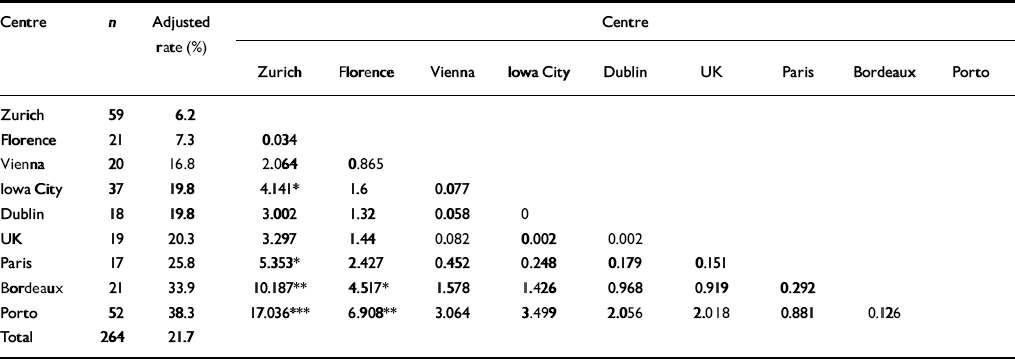
Prevalence rates covering the period between the antenatal and postnatal interviews were adjusted to 6-month period prevalence rates in order to control for the variation in interval between interviews among the different centres. The adjusted 6-month period prevalence rate for each country was calculated by dividing the actual prevalence rate by the average number of weeks between the antenatal and postnatal interview and then multiplying by 26 weeks (6 months). The adjusted 6-month prevalence rate was used to calculate the number of cases expected to occur given the sample size of the individual centre, which was then used in χ2 analyses to compare period prevalence rates between centres. Tables 3, 4 and 5 showχ2 values for adjusted 6-month period prevalence rates for caseness, depression and major depression. The adjusted 6-month period rates reflect cases that occurred during the latter part of pregnancy and the post-partum period, and assume an even distribution of depressive illness across the 26-week period.
Table 3 Six-month period prevalence rates for caseness (generalised anxiety disorder, major and minor depression): chi-squared comparisons
| Centre | n | Adjusted rate (%) | Centre | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Zurich | Florence | Vienna | Iowa City | Dublin | UK | Paris | Bordeaux | Porto | |||
| Zurich | 59 | 6.2 | |||||||||
| Florence | 21 | 7.3 | 0.034 | ||||||||
| Vienna | 20 | 16.8 | 2.064 | 0.865 | |||||||
| Iowa City | 37 | 19.8 | 4.141* | 1.6 | 0.077 | ||||||
| Dublin | 18 | 19.8 | 3.002 | 1.32 | 0.058 | 0 | |||||
| UK | 19 | 20.3 | 3.297 | 1.44 | 0.082 | 0.002 | 0.002 | ||||
| Paris | 17 | 25.8 | 5.353* | 2.427 | 0.452 | 0.248 | 0.179 | 0.151 | |||
| Bordeaux | 21 | 33.9 | 10.187** | 4.517* | 1.578 | 1.426 | 0.968 | 0.919 | 0.292 | ||
| Porto | 52 | 38.3 | 17.036*** | 6.908** | 3.064 | 3.499 | 2.056 | 2.018 | 0.881 | 0.126 | |
| Total | 264 | 21.7 | |||||||||
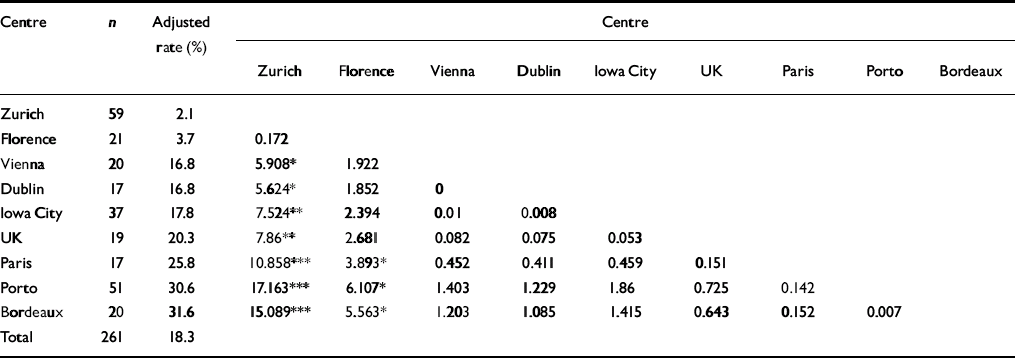
Table 4 Six-month period prevalence rates for depression (major and minor): chi-squared comparisons
| Centre | n | Adjusted rate (%) | Centre | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Zurich | Florence | Vienna | Dublin | Iowa City | UK | Paris | Porto | Bordeaux | |||
| Zurich | 59 | 2.1 | |||||||||
| Florence | 21 | 3.7 | 0.172 | ||||||||
| Vienna | 20 | 16.8 | 5.908* | 1.922 | |||||||
| Dublin | 17 | 16.8 | 5.624* | 1.852 | 0 | ||||||
| Iowa City | 37 | 17.8 | 7.524** | 2.394 | 0.01 | 0.008 | |||||
| UK | 19 | 20.3 | 7.86** | 2.681 | 0.082 | 0.075 | 0.053 | ||||
| Paris | 17 | 25.8 | 10.858*** | 3.893* | 0.452 | 0.411 | 0.459 | 0.151 | |||
| Porto | 51 | 30.6 | 17.163*** | 6.107* | 1.403 | 1.229 | 1.86 | 0.725 | 0.142 | ||
| Bordeaux | 20 | 31.6 | 15.089*** | 5.563* | 1.203 | 1.085 | 1.415 | 0.643 | 0.152 | 0.007 | |
| Total | 261 | 18.3 | |||||||||
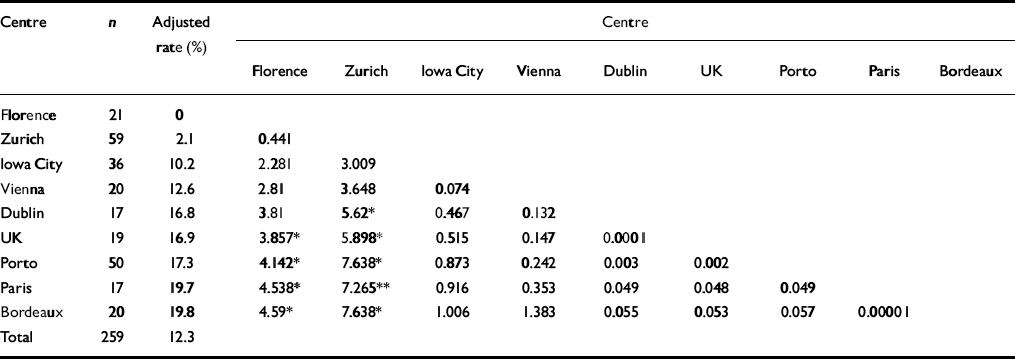
Table 5 Six-month period prevalence rates for major depression: chi-squared comparisons
| Centre | n | Adjusted rate (%) | Centre | ||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|
| Florence | Zurich | Iowa City | Vienna | Dublin | UK | Porto | Paris | Bordeaux | |||
| Florence | 21 | 0 | |||||||||
| Zurich | 59 | 2.1 | 0.441 | ||||||||
| Iowa City | 36 | 10.2 | 2.281 | 3.009 | |||||||
| Vienna | 20 | 12.6 | 2.81 | 3.648 | 0.074 | ||||||
| Dublin | 17 | 16.8 | 3.81 | 5.62* | 0.467 | 0.132 | |||||
| UK | 19 | 16.9 | 3.857* | 5.898* | 0.515 | 0.147 | 0.0001 | ||||
| Porto | 50 | 17.3 | 4.142* | 7.638* | 0.873 | 0.242 | 0.003 | 0.002 | |||
| Paris | 17 | 19.7 | 4.538* | 7.265** | 0.916 | 0.353 | 0.049 | 0.048 | 0.049 | ||
| Bordeaux | 20 | 19.8 | 4.59* | 7.638* | 1.006 | 1.383 | 0.055 | 0.053 | 0.057 | 0.00001 | |
| Total | 259 | 12.3 | |||||||||
The overall 6-month period prevalence rates for caseness, depression and major depression were 21.7%, 18.3% and 12.3%, respectively. These rates are consistent with previously reported rates of depression during pregnancy (Reference Cox, Connor and KendellCox et al, 1982; Reference Kumar and RobsonKumar & Robson, 1984; Reference O'HaraO'Hara, 1986; Reference Kitamura, Shima and SugarwaraKitamura et al, 1993) and the post-partum period (Reference O'Hara, Zekoski, Kumar and BrockingtonO'Hara & Zekoski, 1988; Reference O'Hara and SwainO'Hara & Swain, 1996).
Period prevalence rates for caseness ranged from a low in Zurich of 6.2% to a high in Porto of 38.3%. The Zurich sample contained significantly fewer women meeting criteria for generalised anxiety disorder or minor or major depression than did Iowa City, Bordeaux, Paris or Porto. Florence also had significantly fewer women meeting caseness criteria than did Bordeaux and Porto. Depression period prevalence rates ranged from 2.1% in Zurich to 31.6% in Bordeaux. The Zurich rate was significantly lower than that in all other centres except Florence. Florence also had significantly lower rates compared with Bordeaux, Paris and Porto for depression. Period prevalence rates for major depression ranged from 0% in Florence to 19.8% in Bordeaux. Rates in Florence and Zurich were significantly lower than those in the UK, Porto, Paris and Bordeaux. Zurich also had significantly fewer cases of major depression than did Dublin.
Overall, 6-month period prevalence rates revealed lower rates of perinatal depression and anxiety in Florence and Zurich and higher rates in Porto, Bordeaux and Paris. Interestingly, although no woman in the Viennese sample met criteria for current generalised anxiety disorder or depression at the time of the antenatal and postnatal interviews, the period prevalence rate indicates that a high percentage of women (16.8%) experienced generalised anxiety disorder and/or major or minor depression during the last part of pregnancy and the early post-partum period.
Other disorders
Period prevalence rates for other disorders were extremely low, at less than 1% overall for agoraphobia, anorexia and bulimia nervosa, and 1-2% for panic disorder and obsessive-compulsive disorder. There was no case of alcohol or substance misuse.
DISCUSSION
The findings from this pilot study are important in that they suggest that a transcultural comparison of antenatal and postnatal prevalence rates of depression and anxiety using a single measure can be accomplished successfully.
Interestingly, the overall estimated 6-month period prevalence rate of major depression obtained from the current study (12.3%) is almost identical to the prevalence rate calculated by O'Hara & Swain (Reference O'Hara and Swain1996) in a meta-analysis of 59 postpartum depression studies conducted in several countries - European, Western and non-Western - during the past 20 years. The average prevalence rate for postnatal depression obtained in the meta-analysis was 12% when depression was assessed using standardised interview-based measures. It should be noted that the 6-month prevalence rate obtained in our study reflects not only cases of major depression during the post-partum period, but also cases occurring during the latter part of pregnancy. However, at least 88% of the women who experienced a major depressive disorder between the antenatal and postnatal interviews reported its onset after delivery.
There were significant differences in prevalence rates of perinatal depression among women participating in the various centres. There may be several explanations for the higher rates of perinatal depression observed in Porto, Paris and Bordeaux and the lower rates found in Zurich and Florence. First, it is possible that these differences occurred by chance, given the relatively small sample sizes in some centres. However, there is evidence that rates of depression and psychiatric illness do vary among countries and cultures. Weissman et al (Reference Weissman, Bland and Canino1996) reported wide variation in lifetime rates of major depression across ten countries participating in a cross-national epidemiological survey (USA, Canada, Puerto Rico, France, West Germany, Italy, Lebanon, Taiwan, Korea and New Zealand). In that study, sample size was not a concern as approximately 38 000 persons participated.
Another possible explanation for the difference in prevalence rates involves rates of previous episodes of depression among women from the various centres. Previous history of depression is a powerful predictor of perinatal depression (Reference O'Hara, Schlechte and LewisO'Hara et al, 1991). There were significant differences between centres in rates of previous depression, ranging from 10% or less in Vienna and Zurich to 50% and over in Iowa City, Paris and the UK. Overall, there were strong associations between previous depression and period prevalence of caseness (χ2=7.72, P=0.005), depression (χ2=9.39, P=0.002) and major depression (χ2=16.58, P<0.001). However, when results for individual centres were examined, these associations were significant only in the UK and Vienna, and controlling for past history did not remove the differences between centres. It did not appear, therefore, that different rates of previous depression could explain the higher rates of perinatal depression found in Porto, Paris and Bordeaux, or the lower rates in Zurich and Florence.
Third, there were differences in the demographic characteristics of the sample, notably in terms of social class, with Porto having a much lower proportion of women categorised as ‘non-manual class’ (43% compared with 64% or more elsewhere). ‘Manual class’ women were more likely to experience perinatal caseness (χ2=10.91, P=0.001), depression (χ2=6.84, P=0.009) and major depression (χ2=5.38, P=0.02), but again, controlling for this variable did not remove the differences between centres.
A fourth hypothesis is that factors related to psychosocial variables associated with depression might have contributed to the higher rates of perinatal depression in Porto, Bordeaux and Paris (Reference Bernazzani, Conroy and MarksBernazzani et al, 2004, this supplement). Both stressful life events and low levels of emotional support have been associated with postnatal depression (Reference O'Hara and SwainO'Hara & Swain, 1996). Women in Paris experienced more severe life adversity in the form of acute negative life events and chronic daily stresses during their pregnancy and after delivery compared with women in other centres (Reference Bernazzani, Conroy and MarksBernazzani et al, 2004, this supplement). Poor emotional support following delivery, another psychosocial variable associated with depression, was reported by a higher percentage of women in Porto than women in other centres (Reference Bernazzani, Conroy and MarksBernazzani et al, 2004, this supplement).
With regard to the low rates of perinatal depression observed in Florence and Zurich, perhaps psychological factors, such as having a positive attitude towards the pregnancy or having a secure maternal attachment style, buffered women from experiencing depression during this period. Women in both Florence and Zurich reported fewer negative feelings towards the pregnancy than women in other centres (Reference Bernazzani, Conroy and MarksBernazzani et al, 2004, this supplement). Also, fewer women in Zurich had markedly insecure maternal attachment styles and were perhaps less vulnerable to depression during this transitional period in their life. More insights regarding the validity of these hypotheses can be found in Bernazzani et al (Reference Bernazzani, Conroy and Marks2004, this supplement) and Bifulco et al (Reference Bifulco, Figueiredo and Guedeney2004, this supplement).
Finally, differences in health care systems (see Reference Chisholm, Conroy and Glangeaud-FreudenthalChisholm et al, 2004, this supplement) may also have contributed to centre differences.
In sum, one of the major aims of the TCS-PND was accomplished in that psychiatric researchers were able to use a standardised, structured diagnostic instrument, the SCID-PND, to assess women from varying cultural backgrounds both during pregnancy and postnatally. Although the overall rate of perinatal depression across centres replicated findings from previous individual studies, cross-cultural comparisons of antenatal and postnatal prevalence rates of depression revealed differences in rates between centres. These findings require verification in larger, multi-centre studies.
Clinical Implications and Limitations
CLINICAL IMPLICATIONS
-
▪ Among women from several European countries and the USA, overall rates of depression during pregnancy and the postnatal period (6.9% and 8.0%, respectively) are significant and deserve clinical attention.
-
▪ Observed differences in rates of perinatal depression among women from different countries and cultural backgrounds are intriguing and require investigation into the possible contribution of psychosocial factors and variations in health care delivery systems.
-
▪ The Structured Clinical Interview for DSM–IV Axis I Disorders is a standardised diagnostic tool with demonstrated utility in cross-cultural research settings and in populations of pregnant and postnatal women.
LIMITATIONS
-
▪ Small samples limit broader generalisations of the findings, pending verification in a large multi-centre study.
-
▪ Questions remain regarding the prevalence of antenatal and postnatal depression in women from developing countries and more diverse cultural backgrounds.
-
▪ Point prevalence rates reflecting antenatal depression in late pregnancy and postnatal depression at approximately 6 months after delivery, leave open the question of prevalence rates of depression early in pregnancy and up to 1 year in the postnatal period.








eLetters
No eLetters have been published for this article.