The prevalence of medication-resistant psychotic symptoms has led to psychological treatment being used alongside medication to reduce the impact of symptoms. Cognitive–behavioural therapy (CBT) for psychosis (CBTp) has been the dominant approach, but is lengthy and complex to deliver. Reference Thomas1 Substantial interest has grown in applying acceptance and mindfulness-based therapies, Reference Khoury, Lecomte, Fortin, Masse, Therien and Bouchard2 with acceptance and commitment therapy (ACT) – one of the most widely used manualised approaches Reference Hayes, Strosahl and Wilson3,Reference Hayes, Strosahl and Wilson4 – showing promise. Rather than effecting change by modifying the person's understanding of psychotic experiences, ACT targets the extent to which symptoms and related beliefs dominate conscious experience and behaviour. Reference Hayes5 Two randomised controlled trials (RCTs) have tested four-session ACT interventions in in-patients with acute psychosis, observing small-to-medium reductions in re-admission to hospital rates over 4–12 months in intention-to-treat analyses v. routine or enhanced routine care. Reference Bach and Hayes6–Reference Gaudiano and Herbert8 However, ACT has yet to be trialled for medication-resistant psychosis. The aim of this study was to test the efficacy of ACT in a sample of community-residing patients with persisting psychotic symptoms. This paper reports our results for primary and secondary outcome measures. Additionally, several process measures were included in order to examine hypothesised mechanisms of action (see study protocol Reference Thomas, Shawyer, Castle, Copolov, Hayes and Farhall9 ). Our hypotheses were that, compared with patients receiving equivalent clinician time in a comparison condition, patients who received ACT would show improvements in (a) overall mental state; (b) preoccupation, conviction, distress and disruption to life associated with positive symptoms; and (c) social functioning. We hypothesised that these changes would be achieved by the conclusion of therapy and maintained at 6-month follow-up. Outcomes were also examined in relation to service utilisation.
Method
Design
The study protocol, detailed in Thomas et al, Reference Thomas, Shawyer, Castle, Copolov, Hayes and Farhall9 is briefly described here. A prospective single (rater)-blind RCT compared two parallel groups: the intervention (ACT) v. a comparison condition (befriending). Assessments took place prior to randomisation (baseline), at post-therapy and 6 months after the end of therapy. The trial is registered at the Australian New Zealand Clinical Trials Registry: ACTRN12608000210370.
Participants
Recruitment took place over 3 years from public community mental health services, non-government psychiatric rehabilitation services and private providers in Melbourne, Australia, supplemented by media advertising. Inclusion criteria were: (a) aged 18–65 years; (b) current diagnosis of schizophrenia or schizoaffective disorder; (c) residual hallucinations or delusions associated with significant distress or disability (score ⩾4 on the Positive and Negative Syndrome Scale (PANSS) Reference Kay10 items P1 and/or P3); (d) these symptoms present continuously over the past 6 months; and (e) on therapeutic doses of antipsychotic medication over the past 6 months (clinician report). Exclusion criteria were: (a) any neurological disorder that may affect cognitive function; (b) insufficient conversational English; (c) Wechsler Test of Adult Reading (WTAR) Reference Wechsler11 estimated IQ <70; (d) change of antipsychotic medication within the previous 8 weeks or planned at the time of intake; (e) currently receiving other formal psychological treatment. Following consent, participants were interviewed to confirm eligibility and complete baseline assessment measures prior to randomisation.
Sample size
The target sample size of 53 participants per treatment arm was calculated to detect post-therapy between-group effects for overall mental state of d = 0.55 or greater with 80% power (α = 0.05). This effect size was slightly lower than the d = 0.60 reported in the TORCH Reference Shawyer, Farhall, Mackinnon, Trauer, Sims and Ratcliff12 and Gaudiano & Herbert Reference Gaudiano and Herbert8 trials for overall mental state, in view of the novel protocol.
Treatment conditions
ACT
Participants were offered eight 50 min ACT sessions, delivered weekly to fortnightly over around 3 months. ACT was conducted according to a local manual based on the (transdiagnostic) ACT manual Reference Hayes, Strosahl and Wilson3 with recommended adaptations for psychosis. Reference Bach and Hayes6,Reference Bach, Hayes and Strosahl13,Reference Thomas, Morris, Shawyer, Farhall, Morris, Johns and Oliver14 Participants were provided with handouts and sessions recorded onto compact discs for home review.
Befriending
Participants were offered eight 50 min sessions of the befriending intervention, Reference Bendall, Killackey, Jackson and Gleeson15 a manualised treatment previously used as a control condition in psychological intervention trials in psychosis, Reference Shawyer, Farhall, Mackinnon, Trauer, Sims and Ratcliff12,Reference Jackson, McGorry, Killackey, Bendall, Allott and Dudgeon16,Reference Sensky, Turkington, Kingdon, Scott, Scott and Siddle17 befriending involves engaging in conversation about everyday topics, while overtly avoiding discussion of symptoms and problems. It produces similar treatment expectancy and engagement to CBT, with similar drop-out rates. Reference Bendall, Jackson, Killackey, Allot, Johnson and Harrigan18 Befriending has shown some equivalence in outcomes to CBTp, suggesting that it has effectiveness as a treatment in its own right. Reference Shawyer, Farhall, Mackinnon, Trauer, Sims and Ratcliff12,Reference Jackson, McGorry, Killackey, Bendall, Allott and Dudgeon16,Reference Sensky, Turkington, Kingdon, Scott, Scott and Siddle17
In both conditions, therapy was provided by four clinical psychologists, experienced in psychological interventions for schizophrenia, with additional training in ACT and befriending. They attended weekly peer supervision led by J.F. or S.C.H. Local services managed medication, case management and other aspects of treatment.
Treatment fidelity
An independent assessor, masked to treatment allocation, rated a stratified random sample of treatment session audio files for adherence with each therapy protocol, and assigned each session to ACT or befriending. The Befriending Treatment Integrity Measure (BTIM) Reference Bendall, Killackey, Jackson and Gleeson15 was used to assess the quality of befriending sessions and to ensure that ACT sessions did not include befriending techniques. In the absence of a suitable ACT fidelity scale, we developed the six-item ACT for Psychosis Adherence and Competence Scale (APACS – see online supplement DS1), where adherence ratings reflect a composite of the presence and frequency of the six ACT processes defined in our manual. The APACS adherence subscale showed acceptable psychometric properties. Reference Pollard19
Assessments
Research assistants masked to treatment condition administered the eligibility and assessment measures in face-to-face interviews with participants. The Structured Clinical Interview for DSM-IV-TR Axis I Disorders Reference First, Spitzer, Gibbon and Williams20 and WTAR were completed at baseline to assess eligibility. Symptom outcome measures included the following: PANSS, assessing overall mental state including positive, negative and general symptoms; the Psychotic Symptom Rating Scales (PSYRATS), Reference Haddock, McCarron, Tarrier and Faragher21 assessing the frequency, preoccupation, conviction, distress and disruption to life associated with auditory hallucinations (PSYRATS-AH) and main delusions (PSYRATS-D); and the Peters Delusions Inventory (PDI) Reference Peters, Joseph, Day and Garety22 to assess the range/number of delusional beliefs held and overall degree of associated distress, preoccupation and conviction. The PSYRATS-AH do not include a specific item assessing preoccupation so we created an additional item assessing time spent thinking about voices. Psychosocial functioning was measured by the Social Functioning Scale (SFS). Reference Birchwood, Smith, Cochrane, Wetton and Copestake23 Service utilisation related to psychiatric hospital admissions and mental health consultations was also assessed. Reference Thomas, Shawyer, Castle, Copolov, Hayes and Farhall9
Process measures included the 16-item Acceptance and Action Questionnaire (AAQ) Reference Hayes, Strosahl, Wilson, Bissett, Pistorello and Toarmino24 to assess (a) acceptance of psychotic experiences as opposed to experiential avoidance, and (b) commitment to valued action; the Voices Acceptance and Action Scale (VAAS) Reference Shawyer, Ratcliff, Mackinnon, Farhall, Hayes and Copolov25 was used to assess acceptance and autonomous action in relation to auditory hallucinations; and the Recovery Style Questionnaire (RSQ) Reference Drayton, Birchwood and Trower26 to assess the degree to which participants ‘integrate’ their illness, acknowledging their illness experiences with interest, as opposed to ‘sealing over’, seeking to separate psychosis from themselves. Additional measures were administered Reference Thomas, Shawyer, Castle, Copolov, Hayes and Farhall9 but are not reported here.
Measures, and dose of antipsychotic medication, were assessed at each time point except for service utilisation, administered at baseline and follow-up. At the end of post-therapy assessments, participants were asked to rate therapy acceptability on the Client Satisfaction Questionnaire (CSQ) Reference Attkisson and Zwick27 (possible scores: 8–32). Additional therapy evaluation questions assessed emotional response to sessions and extent of improvement of problems related to psychosis. Rater's masking was preserved by participants returning responses in a sealed envelope. Baseline assessments commenced in October 2008 with the final follow-up conducted in November 2012.
Randomisation and masking
Randomisation Reference Thomas, Shawyer, Castle, Copolov, Hayes and Farhall9 was prepared by an independent statistician. Stratification was by site and recovery style (integration or sealing over) giving 18 factorial groups. Allocation was by a random permuted blocks procedure within Microsoft Excel, using a random number generator to choose each sequence of blocks of sizes 2, 4 and 6, without replacement. Numbered, sealed, opaque envelopes for each of the 18 groups' concealed allocations. Using the envelopes in order, for the appropriate group, an independent researcher allocated participants to treatment with a 1:1 allocation ratio in accordance with CONSORT guidelines.
Considerable efforts were made to maintain rater masking. Reference Thomas, Shawyer, Castle, Copolov, Hayes and Farhall9 Masking was assessed by asking raters to classify participants into a treatment condition after post-therapy and follow-up assessments and indicate their level of confidence. Breaches in masking were recorded and addressed by changing the rater wherever possible.
Primary and secondary outcomes
The primary outcome is PANSS total at post-therapy, with PANSS positive, negative and general subscales also reported. Secondary outcomes include PSYRATS-AH and PSYRATS-D preoccupation, conviction, distress and disruption to life, adjusting for the presence and frequency of symptoms; the SFS; and service utilisation.
Statistical analysis
The analyses were not masked. Where distributions were non-normal across time points, square-root transformations were applied; descriptive statistics are reported for back-transformed data. As a result of some outcome measures showing significant baseline differences between ACT and befriending, and between completers and non-completers, propensity score matching Reference Rosenbaum and Rubin28 was used to even out the distribution of the measured baseline characteristics across the intervention groups. This involved constructing a logistic regression model with treatment condition as the outcome, and baseline clinical variables and demographics as predictors, plus a ‘missing-at-post-therapy’ variable to index differential effects of attrition. Based on this model, the probability of being chosen for the ‘reference’ group (propensity score) was estimated for each participant, to provide a summary of the covariate imbalance between intervention and control participants. These propensity scores were included as a covariate in all analyses (excluding therapy evaluation measures). Reference Leon and Hedeker29 Intention-to-treat analyses using mixed regression models were the primary analytic approach. Compared with other techniques such as repeated measures analysis of variance, the mixed-model framework deletes randomly missing observations without dropping the participant. All participants randomised are included in the analysis; therefore, imputation methods such as last observation carried forward (LOCF) or expectation–maximisation are not applied. The within-groups factor was time (baseline, post-therapy, follow-up) and the between-groups factor was group (ACT, befriending). For service utilisation, the within-groups factor was time (baseline, follow-up). Reports are based on the covariance model with the fewest parameters that were not significantly different than the most complex model as determined by comparison of nested models through the restricted log-likelihood. Both mixed model repeated measures (MMRM), which treats time as categorical, and hierarchical linear modelling (HLM), which treats time as a linear covariate, were calculated and compared. In all cases MMRM provided a better fit to the data as determined by a comparison of the restricted log-likelihood, and thus MMRM results are reported throughout as the primary analysis. Because HLM better addresses overall trends across time, these analyses are reported if they conveyed additional information.
The PSYRATS analyses were conducted on individual items using ordinal regression models Reference Scott, Goldberg and Mayo30 to accommodate both within- and between-participant clustering. Analyses for PSYRATS-AH and PSYRATS-D scales included only data from participants reporting auditory verbal hallucinations or delusions, respectively, during the project. Analyses related to the PSYRATS-AH subscales included PSYRATS-AH frequency as a covariate. Analyses for the PSYRATS-D subscales included PSYRATS-D amount of preoccupation (frequency of delusional thinking) as a covariate.
Planned contrasts were used to compare changes from baseline under each intervention at post-therapy and follow-up. Chi-square tests were used to compare the number of participants in the ACT and befriending groups who achieved a clinically significant improvement on PANSS scores, defined as a 25% score reduction from baseline as recommended by Leucht. Reference Leucht31 Analyses were undertaken using SPSS 21 for Windows: the linear mixed-effects models (MIXED) procedure was used for the MMRM analyses. The ordinal regression model for the PSYRATS data was implemented in SAS 9.4 with the SAS Procedure PROC GLIMMIX. GLIMMIX was used to predict the probability of being in the lower category.
Results
Participant characteristics
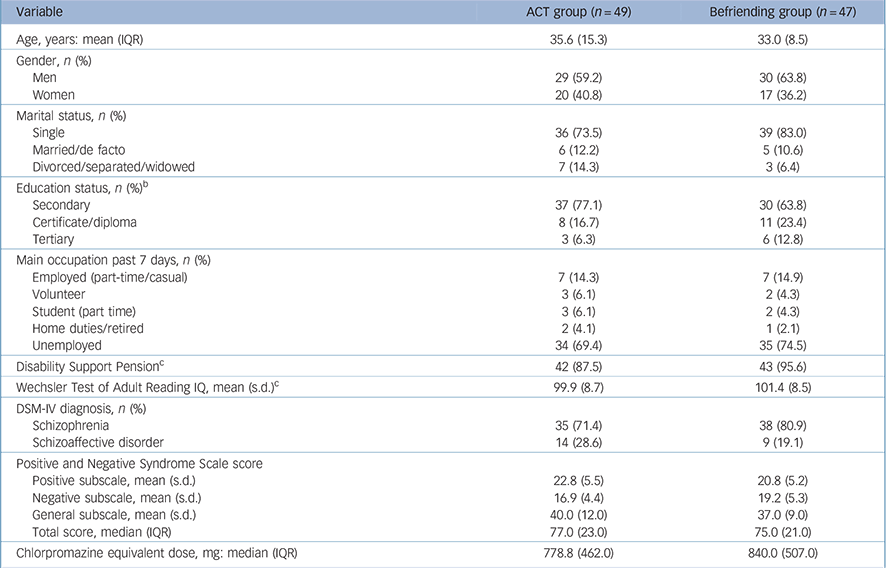
Participants included 59 males (61.5%) and 37 females (38.5%), mean age: 36.1 years (s.d. = 9.1, range 19–64). Baseline clinical and demographic characteristics are shown in Table 1.
Table 1 Demographic and clinical characteristics of acceptance and commitment therapy (ACT) and befriending groups at baseline a
| Variable | ACT group (n = 49) | Befriending group (n = 47) |
|---|---|---|
| Age, years: mean (IQR) | 35.6 (15.3) | 33.0 (8.5) |
| Gender, n (%) | ||
| Men | 29 (59.2) | 30 (63.8) |
| Women | 20 (40.8) | 17 (36.2) |
| Marital status, n (%) | ||
| Single | 36 (73.5) | 39 (83.0) |
| Married/de facto | 6 (12.2) | 5 (10.6) |
| Divorced/separated/widowed | 7 (14.3) | 3 (6.4) |
| Education status, n (%) b | ||
| Secondary | 37 (77.1) | 30 (63.8) |
| Certificate/diploma | 8 (16.7) | 11 (23.4) |
| Tertiary | 3 (6.3) | 6 (12.8) |
| Main occupation past 7 days, n (%) | ||
| Employed (part-time/casual) | 7 (14.3) | 7 (14.9) |
| Volunteer | 3 (6.1) | 2 (4.3) |
| Student (part time) | 3 (6.1) | 2 (4.3) |
| Home duties/retired | 2 (4.1) | 1 (2.1) |
| Unemployed | 34 (69.4) | 35 (74.5) |
| Disability Support Pension c | 42 (87.5) | 43 (95.6) |
| Wechsler Test of Adult Reading IQ, mean (s.d.) c | 99.9 (8.7) | 101.4 (8.5) |
| DSM-IV diagnosis, n (%) | ||
| Schizophrenia | 35 (71.4) | 38 (80.9) |
| Schizoaffective disorder | 14 (28.6) | 9 (19.1) |
| Positive and Negative Syndrome Scale score | ||
| Positive subscale, mean (s.d.) | 22.8 (5.5) | 20.8 (5.2) |
| Negative subscale, mean (s.d.) | 16.9 (4.4) | 19.2 (5.3) |
| General subscale, mean (s.d.) | 40.0 (12.0) | 37.0 (9.0) |
| Total score, median (IQR) | 77.0 (23.0) | 75.0 (21.0) |
| Chlorpromazine equivalent dose, mg: median (IQR) | 778.8 (462.0) | 840.0 (507.0) |
a. Medians (interquartile range (IQR)) reported where data are skewed.
b. n = 48 for the ACT group and n = 47 for the befriending group.
c. n = 48 for the ACT group and n = 45 for the befriending group.
Participant flow, attrition and reliability
Of 531 patients identified as possible candidates, 137 either declined participation before eligibility could be assessed or were unable to be assessed. The eligibility of 244 of the remaining 394 patients was confirmed, however 83 were unavailable for participation. Of the 161 eligible and available, 65 declined participation and 96 (60% of eligible candidates) proceeded to randomisation (Fig. 1). There were no significant group differences in rates of attrition (post-therapy: χ2(1) = 0.06, P = 0.81; follow-up: w2(1) = 0.76, P = 0.38). Completers (n = 77) at follow-up were compared with participants who did not complete the final assessment (n = 19) on baseline measures. Non-completers showed more frequent delusion-related distress (PSYRATS-D amount of distress), and lower acceptance (AAQ, VAAS-9). PANSS interrater reliability assessment included all participants with a second rating (n = 23). Median intraclass correlations ranged from 0.97 (PANSS-Total) to 0.84 (PANSS-General).

Fig. 1 Flow of participants through the study (CONSORT diagram).
a. Includes unstable mental state, unstable circumstances, discharge from service, move from area, risk issues, unreliable attendance and poor engagement with services.
ACT, Acceptance and Commitment Therapy; ITT, intention to treat.
Fidelity
A masked fidelity assessor correctly assigned to condition all 94 sampled sessions. The mean total APACS score across the 48 ACT sessions sampled was 7.06 (s.d. = 1.79) indicating, on average, that the majority of each session involved identifiable ACT processes. One sampled befriending session had a rated ACT component (values); no ACT sessions had a befriending component rated.
Masking
Only one assessment (at follow-up) was conducted unmasked during the trial (because no other rater was available). Data on raters' guess of treatment group were available for 33 interviews at post-therapy and 50 at follow-up. Using one-tailed binomial tests, neither post-therapy nor follow-up guesses were better than chance. Mean confidence ratings were 14.6 (s.d. = 18.7) at post-therapy and 17.8 (s.d. = 25.3) at follow-up, and were unrelated to accuracy.
Treatment exposure
Participants allocated to ACT completed an average of 7.0 (s.d. = 2.3) therapy sessions, compared with 7.2 (s.d. = 2.0) for befriending, Mann–Whitney U-test, P = 0.82. There was no group difference in duration of therapy (months) (ACT group 2.9, s.d. = 1.3; befriending group 2.6 (s.d. = 0.8), Mann–Whitney U-test, P = 0.36). There were no significant changes by group in chlorpromazine-equivalent antipsychotic medication dosages over the study period (time: F(2, 145.4) = 1.43, P = 0.24; group: F(1, 93.9) = 0.30, P = 0.59; group×time: F(2, 145.54) = 1.21, P = 0.30).
Main findings
Results of the MMRM and ordinal regression analyses for the key symptom, functioning and service utilisation outcomes are shown in Tables 2, 3 and 4.
Table 2 Means (95% CI), Cohen's d values and tests of group×time fixed effects in mixed-effects model repeated measures ANOVA for Positive and Negative Syndrome Scale (PANSS) primary outcome measures a

| ACT group | Befriending group | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Mean (95% CI) | Within group, d (95% CI), P | Mean (95% CI) | Within group, d (95% CI), P | Group × time | ||||||||
| Measures | Baseline | Post-therapy | Follow-up | Baseline to post-therapy |
Baseline to follow-up |
Baseline | Post-therapy | Follow-up | Baseline to post-therapy |
Baseline to follow-up |
F (d.f.) P | d (95% CI) |
| PANSS total b | 78.9 (74.5 to 83.4) |
74.2 (69.7 to 78.8) |
72.4 (67.6 to 77.0) |
0.33 (0.02 to 0.64) 0.03 |
0.46 (0.15 to 0.77) 0.003 |
77.6 (73.0 to 82.2) |
71.7 (67.2 to 76.3) |
73.3 (68.6 to 78.2) |
0.42 (0.11 to 0.73) 0.007 |
0.30 (−0.24 to 0.56) 0.07 |
0.63 (164.6) 0.54 |
0.16 (−0.24 to 0.56) |
| PANSS positive | 22.8 (21.3 to 24.4) |
20.5 (18.8 to 22.1) |
19.2 (17.5 to 21.0) |
0.64 (0.32 to 0.96) <0.001 |
0.79 (0.47 to 1.11) <0.001 |
20.8 (19.1 to 22.4) |
19.2 (17.5 to 20.9) |
19.7 (17.8 to 21.6) |
0.42 (0.11 to 0.73) 0.008 |
0.23 (−0.08 to 0.54) 0.19 |
2.82 (81.2) 0.07 |
0.37 (−0.03 to 0.77) |
| PANSS negative | 17.0 (15.6 to 18.4) |
16.9 (15.5 to 18.4) |
17.4 (15.9 to 18.9) |
−0.01 (−0.33 to 0.33) 0.94 |
−0.06 (−0.36 to 0.24) 0.67 |
19.0 (17.6 to 20.5) |
17.6 (16.1 to 19.1) |
17.6 (16.1 to 19.2) |
0.25 (−0.06 to 0.56) 0.098 |
0.24 (−0.07 to 0.55) 0.13 |
1.14 (166.0) 0.32 |
0.22 (−0.09 to 0.53) |
| PANSS general b | 39.2 (36.8 to 41.8) |
37.0 (34.5 to 39.5) |
35.9 (33.4 to 38.4) |
0.27 (−0.04 to 0.58) 0.07 |
0.41 (0.10 to 0.72) 0.008 |
38.1 (35.6 to 40.7) |
35.1 (32.6 to 37.6) |
36.0 (33.4 to 38.7) |
0.37 (0.06 to 0.68) 0.02 |
0.26 (−0.05 to 0.57) 0.11 |
0.65 (165.1) 0.52 |
0.16 (−0.24 to 0.56) |
ACT, acceptance and commitment therapy.
a. Propensity scores included as a covariate. Within-group negative d value indicates deterioration.
b. Analysis based on square root transformed data to correct positive skew; Pack-transformed means and confidence intervals are shown.
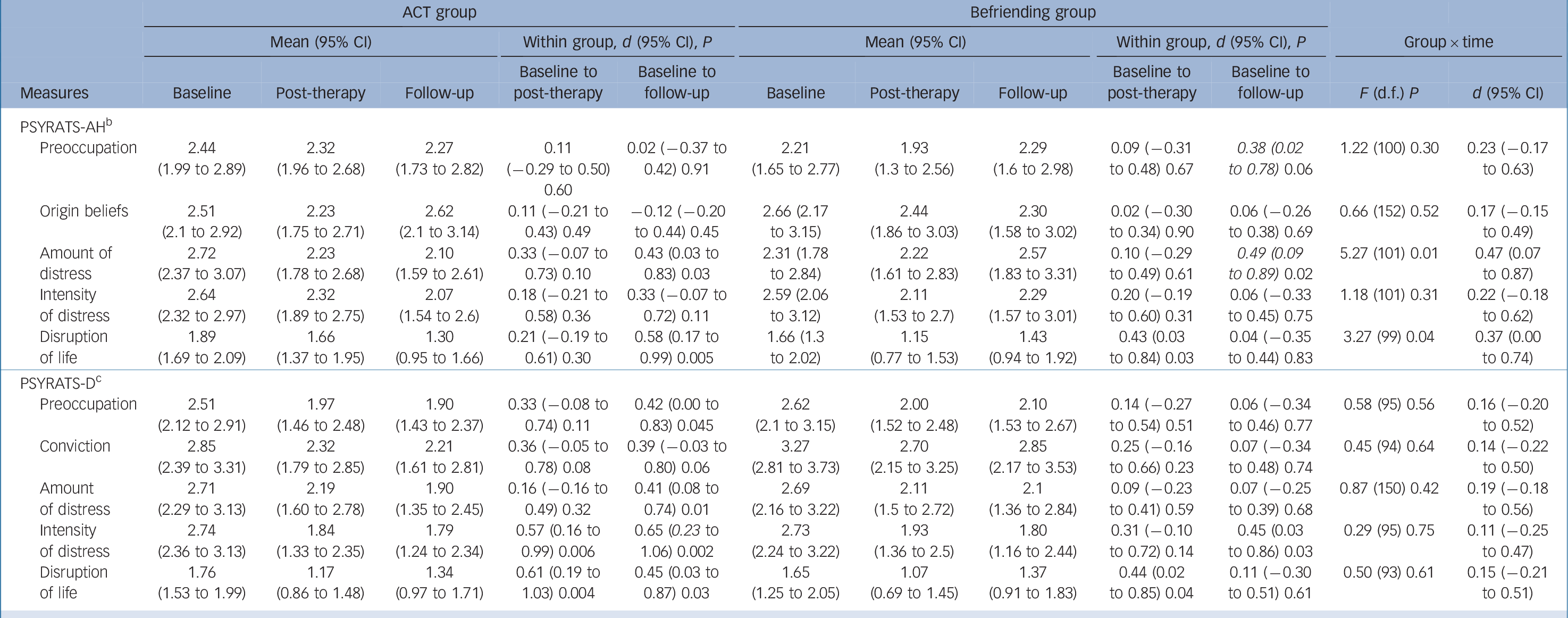
Table 3 Means (95% CI), Cohen's d values and group×time fixed effects in ordinal regression analyses for Psychotic Symptom Rating Scales (PSYRATS) secondary outcome measures a
| ACT group | Befriending group | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Mean (95% CI) | Within group, d (95% CI), P | Mean (95% CI) | Within group, d (95% CI), P | Group × time | ||||||||
| Measures | Baseline | Post-therapy | Follow-up | Baseline to post-therapy |
Baseline to follow-up |
Baseline | Post-therapy | Follow-up | Baseline to post-therapy |
Baseline to follow-up |
F (d.f.) P | d (95% CI) |
| PSYRATS-AH b | ||||||||||||
| Preoccupation | 2.44 (1.99 to 2.89) |
2.32 (1.96 to 2.68) |
2.27 (1.73 to 2.82) |
0.11 (−0.29 to 0.50) 0.60 |
0.02 (−0.37 to 0.42) 0.91 |
2.21 (1.65 to 2.77) |
1.93 (1.3 to 2.56) |
2.29 (1.6 to 2.98) |
0.09 (−0.31 to 0.48) 0.67 |
0.38 (0.02
to 0.78) 0.06 |
1.22 (100) 0.30 | 0.23 (−0.17 to 0.63) |
| Origin beliefs | 2.51 (2.1 to 2.92) |
2.23 (1.75 to 2.71) |
2.62 (2.1 to 3.14) |
0.11 (−0.21 to 0.43) 0.49 |
−0.12 (−0.20 to 0.44) 0.45 |
2.66 (2.17 to 3.15) |
2.44 (1.86 to 3.03) |
2.30 (1.58 to 3.02) |
0.02 (−0.30 to 0.34) 0.90 |
0.06 (−0.26 to 0.38) 0.69 |
0.66 (152) 0.52 | 0.17 (−0.15 to 0.49) |
| Amount of distress |
2.72 (2.37 to 3.07) |
2.23 (1.78 to 2.68) |
2.10 (1.59 to 2.61) |
0.33 (−0.07 to 0.73) 0.10 |
0.43 (0.03 to 0.83) 0.03 |
2.31 (1.78 to 2.84) |
2.22 (1.61 to 2.83) |
2.57 (1.83 to 3.31) |
0.10 (−0.29 to 0.49) 0.61 |
0.49 (0.09
to 0.89) 0.02 |
5.27 (101) 0.01 | 0.47 (0.07 to 0.87) |
| Intensity of distress |
2.64 (2.32 to 2.97) |
2.32 (1.89 to 2.75) |
2.07 (1.54 to 2.6) |
0.18 (−0.21 to 0.58) 0.36 |
0.33 (−0.07 to 0.72) 0.11 |
2.59 (2.06 to 3.12) |
2.11 (1.53 to 2.7) |
2.29 (1.57 to 3.01) |
0.20 (−0.19 to 0.60) 0.31 |
0.06 (−0.33 to 0.45) 0.75 |
1.18 (101) 0.31 | 0.22 (−0.18 to 0.62) |
| Disruption of life |
1.89 (1.69 to 2.09) |
1.66 (1.37 to 1.95) |
1.30 (0.95 to 1.66) |
0.21 (−0.19 to 0.61) 0.30 |
0.58 (0.17 to 0.99) 0.005 |
1.66 (1.3 to 2.02) |
1.15 (0.77 to 1.53) |
1.43 (0.94 to 1.92) |
0.43 (0.03 to 0.84) 0.03 |
0.04 (−0.35 to 0.44) 0.83 |
3.27 (99) 0.04 | 0.37 (0.00 to 0.74) |
| PSYRATS-D c | ||||||||||||
| Preoccupation | 2.51 (2.12 to 2.91) |
1.97 (1.46 to 2.48) |
1.90 (1.43 to 2.37) |
0.33 (−0.08 to 0.74) 0.11 |
0.42 (0.00 to 0.83) 0.045 |
2.62 (2.1 to 3.15) |
2.00 (1.52 to 2.48) |
2.10 (1.53 to 2.67) |
0.14 (−0.27 to 0.54) 0.51 |
0.06 (−0.34 to 0.46) 0.77 |
0.58 (95) 0.56 | 0.16 (−0.20 to 0.52) |
| Conviction | 2.85 (2.39 to 3.31) |
2.32 (1.79 to 2.85) |
2.21 (1.61 to 2.81) |
0.36 (−0.05 to 0.78) 0.08 |
0.39 (−0.03 to 0.80) 0.06 |
3.27 (2.81 to 3.73) |
2.70 (2.15 to 3.25) |
2.85 (2.17 to 3.53) |
0.25 (−0.16 to 0.66) 0.23 |
0.07 (−0.34 to 0.48) 0.74 |
0.45 (94) 0.64 | 0.14 (−0.22 to 0.50) |
| Amount of distress |
2.71 (2.29 to 3.13) |
2.19 (1.60 to 2.78) |
1.90 (1.35 to 2.45) |
0.16 (−0.16 to 0.49) 0.32 |
0.41 (0.08 to 0.74) 0.01 |
2.69 (2.16 to 3.22) |
2.11 (1.5 to 2.72) |
2.1 (1.36 to 2.84) | 0.09 (−0.23 to 0.41) 0.59 |
0.07 (−0.25 to 0.39) 0.68 |
0.87 (150) 0.42 | 0.19 (−0.18 to 0.56) |
| Intensity of distress |
2.74 (2.36 to 3.13) |
1.84 (1.33 to 2.35) |
1.79 (1.24 to 2.34) |
0.57 (0.16 to 0.99) 0.006 |
0.65 (0.23 to 1.06) 0.002 |
2.73 (2.24 to 3.22) |
1.93 (1.36 to 2.5) |
1.80 (1.16 to 2.44) |
0.31 (−0.10 to 0.72) 0.14 |
0.45 (0.03 to 0.86) 0.03 |
0.29 (95) 0.75 | 0.11 (−0.25 to 0.47) |
| Disruption of life |
1.76 (1.53 to 1.99) |
1.17 (0.86 to 1.48) |
1.34 (0.97 to 1.71) |
0.61 (0.19 to 1.03) 0.004 |
0.45 (0.03 to 0.87) 0.03 |
1.65 (1.25 to 2.05) |
1.07 (0.69 to 1.45) |
1.37 (0.91 to 1.83) |
0.44 (0.02 to 0.85) 0.04 |
0.11 (−0.30 to 0.51) 0.61 |
0.50 (93) 0.61 | 0.15 (−0.21 to 0.51) |
ACT, acceptance and commitment therapy.
a. Propensity scores included as a covariate. Italicised d value indicates deterioration.
b. PSYRATS auditory hallucinations (PSYRATS-AH) frequency included as a covariate.
c. PSYRATS delusions (PSYRATS-D) amount of preoccupation included as a covariate.
Table 4 Means (95% CI), Cohen's d values and group×time fixed effects in mixed-effects model repeated measures ANOVA for social functioning and service utilisation a

| ACT group | Befriending group | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Mean (95% CI) | Within group, d (95% CI), P | Mean (95% CI) | Within group, d (95% CI), P | Group × time | ||||||||
| Measures | Baseline | Post-therapy | Follow-up | Baseline to post-therapy |
Baseline to follow-up |
Baseline | Post-therapy | Follow-up | Baseline to post-therapy |
Baseline to follow-up |
F (d.f.) P | d (95% CI) |
| Social Functioning Scale |
100.4 (97.7 to 103.2) |
99.7 (96.8 to 102.6) |
99.5 (96.6 to 102.4) |
−0.12 (−0.48 to 0.24) 0.43 |
−0.16 (−0.52 to 0.20) 0.32 |
99.6 (96.7 to 102.5) |
100.2 (97.2 to 103.1) |
99.7 (96.7 to 102.8) |
0.09 (−0.27 to 0.45) 0.54 |
0.03 (−0.33 to 0.39) 0.88 |
0.57 (158.8) 0.57 |
0.15 (−0.21 to 0.51) |
| Service utilisation, number of consultations b |
26.7 (21.1 to 33.0) |
– | 26.6 (20.5 to 33.5) |
– | 0.01 (−0.35 to 0.37) 0.96 |
27.4 (21.6 to 34.0) |
– | 19.5 (14.0 to 25.9) |
– | 0.40 (0.03 to 0.77) 0.02 |
2.82 (75.1) 0.097 |
0.39 (−0.07 to 0.85) |
| Service utilisation, length of consultations, b min |
792.0 (618.8 to 986.5) |
– | 970.0 (672.4 to 1322.0) |
– | −0.18 (−0.54 to 0.18) 0.27 |
775.5 (600.3 to 973.1) |
– | 713.1 (443.7 to 1046.1) |
– | 0.01 (−0.35 to 0.37) 0.69 |
1.12 (70.1) 0.29 |
0.25 (−0.22 to 0.73) |
ACT, acceptance and commitment therapy.
a. Propensity scores included as a covariate. Wrthin-group negative d value indicates deterioration.
b. Analysis based on square root transformed data to correct positive skew; Pack-transformed means and confidence intervals are shown.
Primary outcomes
There were no significant group×time differences on the primary outcome measure, PANSS total (Table 2). The group×time result for PANSS positive showed an effect size of d = 0.37, which fell just short of significance. Further examination, with planned contrasts indicated that the participants in the ACT group had a significantly greater and medium improvement compared with the befriending group at follow-up, t(79.4) = −2.33, P = 0.02, d = 0.52 (95% CI 0.07–0.98) but not at post-therapy (P = 0.30). HLM analyses showed a statistically significant difference in slopes of improvement between conditions (group×time F = 5.59, d.f. = 84.35, P = 0.02, effect size 0.48 (95% CI 0.06–0.89)). Reference Feingold32 Including IQ scores from the WTAR as a covariate strengthened findings also (group×time result for MMRM analysis: F = 3.30, d.f. = 78.25, P = 0.04, effect size 0.41 (95% CI 0.07–0.74); ACT v. befriending planned contrast at follow-up: t(76.6) = −2.85, P = 0.01, d = 0.59 (95% CI 0.17–1.00)).
Secondary outcomes
There were significant group×time interactions for PSYRATS-AH amount of distress (the amount of time voices are distressing) and PSYRATS-AH disruption to life (Table 3). Planned baseline to follow-up contrasts indicated that, compared with the befriending group, the participants in the ACT group reported significantly less voice-related distress, with a medium effect size, t(101) = −3.25, P = 0.002, d = 0.65 (95% CI 0.24–1.06). The voice-related disruption to life contrast showed a small effect size and did not reach significance, t(99) = 1.75, P = 0.08, d = 0.35 (95% CI −0.05 to 0.75). There were no significant group×time interactions for the remaining PSYRATS subscales or for the SFS (Table 4). Although the study was not powered to assess changes to rates of hospital admssion, Reference Thomas, Shawyer, Castle, Copolov, Hayes and Farhall9 these appeared similar at follow-up to baseline in both groups. (See online Table DS3 for untransformed means and standard deviations for primary and secondary measures.)
Other outcomes. On the remaining outcome measures, only the PDI distress subscale showed a significant group×time interaction (F(151.3) = 3.46, P = 0.03, d = 0.38), with the befriending group reporting a medium and significantly lower level of delusion-related distress at follow-up, t(155.9) = 2.62, P = 0.01, d = 0.62, but not at post-therapy (P = 0.32).
Clinical significance. At follow-up, 51.2% (21/41) of the ACT group showed a clinically significant reduction in positive symptoms (i.e. a 25% reduction in PANSS positive), compared with only 22.2% (8/36) of the befriending group (χ2(1, n = 77) = 6.89, P = 0.009, d = 0.63). There were no significant group differences on PANSS total or the other PANSS subscales (see online Table DS4).
Process measures. There were no significant group×time interactions for any of these measures (see online Table DS5) precluding exploration of mechanisms.
Therapy evaluation. Based on data from the CSQ, mean levels of satisfaction with therapy were significantly higher in the ACT group (mean 26.6, s.d. = 3.9, n = 40) compared with the befriending group (mean 23.9, s.d. = 4.5, n = 41), with a medium effect size; t(79) = −2.97, P = 0.004, d = 0.65). The ACT group also endorsed significantly higher levels of problem improvement (76.9%, n = 39 v. 43.2%, n = 37, χ2 = 9.0, P = 0.003, d = 0.73) and emotional improvement (89.7%, n = 39 v. 59.5%, n = 37, χ2 = 9.3, P = 0.002, d = 0.75), both with medium effect sizes.
Discussion
Compared with the befriending group, the participants in the ACT group were more satisfied with therapy and reported greater subjective benefit. Hypothesised greater gains for the ACT group on masked ratings were, however, only partially supported. There were no group differences on PANSS total, and the difference on PANSS positive using MMRM analyses fell just short of significance. Despite not meeting this convention, several findings are suggestive of a relationship favouring the ACT group for PANSS positive: the relationship was significant using HLM analyses and with MMRM when IQ scores were added as a covariate, and the original planned comparison estimated a medium effect size in favour of ACT at follow-up. Further, around half the ACT group achieved clinically significant improvement on PANSS positive at follow-up compared with less than a quarter of the befriending group (P<0.05). These findings were consistent with the ACT group showing significantly greater improvements at follow-up for PSYRATS-AH amount of distress. These changes correspond to the treatment focus on persisting positive symptoms, and the effect sizes appear comparable with the small-to-medium effects observed in similar trials of CBTp. Reference Burns, Erickson and Brenner33,Reference van der Gaag, Valmaggia and Smit34 However, caution is warranted because no significant group differences in favour of ACT were observed for the other outcome measures, and the befriending group unexpectedly showed significantly greater improvement in reported delusional distress, with a medium effect at follow-up. Additionally, no group differences were evident for any of the process measures.
Effect on positive symptoms
In considering the possibility of benefits specific to hallucinations, it is notable that the improvements in re-admission to hospital rate reported in the Bach & Hayes trial Reference Bach and Hayes6 were stronger for participants with auditory hallucinations (ACT group 11.8%; treatment as usual 58.9%) than those with delusions (ACT group 38.5%, treatment as usual 28.5%). The Gaudiano & Herbert trial Reference Gaudiano and Herbert8 also reported favourable findings for participants with auditory hallucinations (hallucination-related distress) but had too few self-ratings of delusions (n = 8) for analysis. It is possible that dose may be a factor here also with delusions potentially requiring longer therapy contact, as was suggested by Bach & Hayes. Reference Bach and Hayes6 Although we considered that eight sessions, twice the number of Bach & Hayes, would provide a more comprehensive treatment for our chronically affected sample, this is substantially fewer than in trials of CBTp. Reference Turkington, Dudley, Warman and Beck35 Indeed, compared with the acute phase, when normal coping has been disrupted, it may be more challenging to facilitate change with what may be well-developed and entrenched ways of adapting to symptoms during the chronic phase. Examining mean scores across the 14 symptom measures (Tables 2–3) shows a pattern of linear improvement over the three time points for nine measures in ACT but only two in befriending. In contrast, a pattern of improvement to post-therapy then loss of gain at follow-up is observed for ten measures in befriending but only two in ACT. Although speculative, it is possible that a longer follow-up period is needed to demonstrate clear group differences.
Results for delusions have also been less consistent using CBTp. A recent meta-analysis examining CBTp effects in auditory hallucinations and delusions Reference Hayes, Strosahl and Wilson3 found evidence of greater amenability to change of hallucinations v. delusions. If so, future studies may best examine more targeted methods and effects rather than examine effects on positive symptoms in combination. Reference van der Gaag, Valmaggia and Smit34,Reference Birchwood, Michail, Meaden, Tarrier, Lewis and Wykes36–Reference Trower, Birchwood, Meaden, Byrne, Nelson and Ross38
It should also be noted that ACT protocols vary with problem presentation Reference Hooper and Larsson39 and ACT for psychosis is still in its infancy thus further protocol refinement is likely required. For example, entrenched avoidant adaptation is a key challenge in chronic presentations: our preliminary recommendation is that dose be consistent with the 15 plus sessions established for CBTp and that the procedures on cost of current coping and engendering hope for change be extended. It has been suggested from an ACT perspective that hallucinations are often a target of experiential avoidance, Reference Bach and Hayes6 whereas delusions are a means of avoidance – if adopting an ACT approach, each symptom may require different strategies. For example, given the observed reduction in delusional distress and reduced service use in the befriending group, an ACT protocol tailored to delusions might prioritise focus on valued living.
Processes of change
The fact that our ACT process measures did not change differentially in the ACT group leaves unclear the processes leading to improvements with hallucinations, making the current study more a test of a protocol than the underlying model. It suggests a need for additional protocol development given that psychological flexibility changes with ACT interventions in other populations, and in people with psychosis. The process of change is unlikely to be intrusion of cognitive strategies used in CBTp: session ratings using the Revised Cognitive Therapy for Psychosis Adherence Scale Reference Rollinson, Smith, Steel, Fowler, Steel and Jolley40 suggested that very few cognitive techniques were used. Reference Pollard19 It is also possible that more general processes, such as using a structured collaborative approach to respond adaptively to hallucinations, is an effective ingredient, aside from specific ACT interventions.
A qualitative study with a subset of ACT participants showed that although some participants were able to articulate an understanding of ACT processes and attribute positive change to these, others found it difficult to understand exercises and were ambivalent about the usefulness of some aspects of ACT. Reference Bacon, Farhall and Fossey41 In future work, it will be worthwhile identifying for whom ACT is most suited. For example, participants with cognitive impairments appeared to struggle with the specific ACT intervention tested in this trial. Adding WTAR scores as a covariate slightly improved outcomes for ACT in the area of positive symptoms suggesting, at least, a role for verbal learning in responsiveness to ACT as used in this study. Alternatively, simpler methods of teaching ACT concepts may need to be developed for this subpopulation.
Negative symptom change and functioning
Contrary to hypotheses, ACT had no significant impact on negative symptoms and functioning. This contrasts with the Gaudiano & Herbert trial, Reference Gaudiano and Herbert8 which reported greater improvements in social functioning for ACT, and a pilot (n = 27) trial by White et al, Reference White, Gumley, McTaggart, Rattrie, McConville and Cleare42 who reported small improvements in negative symptoms following up to ten ACT sessions. These differences could be because of population, protocol, comparison condition or other factors.
Strengths and limitations
This is the first study to test ACT in an out-patient population with chronic medication-resistant psychotic symptoms. Although trial rigour was high, randomisation was not completely successful and drop-out rates were relatively high. The absence of a treatment-as-usual comparison means that the extent to which the observed main effect of time on many measures is attributable to specific effects of each therapy or to other factors cannot be determined, although some effectiveness of the befriending condition has been previously reported. Reference Shawyer, Farhall, Mackinnon, Trauer, Sims and Ratcliff12,Reference Jackson, McGorry, Killackey, Bendall, Allott and Dudgeon16,Reference Sensky, Turkington, Kingdon, Scott, Scott and Siddle17
Befriending
Although befriending was developed originally as a control condition, the present results and previous findings Reference Bendall, Killackey, Jackson and Gleeson15–Reference Sensky, Turkington, Kingdon, Scott, Scott and Siddle17 suggest that befriending may warrant further research attention and analysis. This population is highly stigmatised, even at times in treatment settings, Reference Thornicroft, Rose and Kassam43 and the opportunity to talk to healthcare providers about matters other than symptoms may itself be helpful to some.
Summary and directions for future research
In conclusion, objectively measured benefits of a brief ACT intervention for medication-resistant psychotic symptoms showed a moderate effect for hallucinations above those of an active control, without an effect for overall mental state or delusions. There were medium effects in favour of ACT on satisfaction and self-reported symptom benefits. The changes in process measures observed by other studies were not found here. Symptom-specific therapy refinements, improved investigation of process and attention to cognitive functioning and dose are warranted in future research.
Funding
Funded by the National Health and Medical Research Council of Australia (Project Grant ). We acknowledge the support of: Alfred Health, Austin Health, Eastern Health, Healthscope, Melbourne Health, Mercy Health, MIND Australia, Monash Health, NEAMI, Peninsula Health and St Vincent's Health.
Acknowledgements
This trial was undertaken through La Trobe University. We acknowledge the (non-financial) support of: Alfred Health, Austin Health, Eastern Health, Healthscope, Melbourne Health (NorthWestern Mental Health), Mercy Health, MIND Australia, Monash Health, NEAMI, Peninsula Health and St Vincent's Health. We express our gratitude to the participants.








eLetters
No eLetters have been published for this article.