A number of recent large-scale surveys have reported high rates of psychiatric morbidity in remanded prisoners in England and Wales, with rates of psychotic illness ranging from 5 to 13% (Reference Brooke, Taylor and GunnBrooke et al, 1996; Birmingham et al, 1996; Reference Singleton, Meltzer and GatwardSingleton et al, 1998). However, although all prisoners are screened for the presence of mental disorder on entry into prison, the efficacy of present screening techniques has been shown to be poor - with about 75% of major mental illnesses in men, and 66% in women, missed during the screening process (Birmingham et al, 1996; Reference Parsons, Walker and GrubinParsons et al, 2001).
Working with the Prison Health Directorate and based on the findings of Birmingham et al (1996), Grubin et al (Reference Grubin, Birmingham and Mason1998), and Parsons et al (Reference Parsons, Walker and Grubin2001), we have modified the basic reception health questionnaire used for screening on entry into prison. Initial pilot studies in six prisons found that this instrument detected over 80% of new remands who were suffering from severe mental illness. Inmates were considered to have ‘screened positive’ if affirmative answers were recorded for one or more of the following questions: history of treatment from a psychiatrist, past prescription of psychotropic medication, history of self-harm or a charge of homicide.
The research on which the screening process was based suggests that about 40% of new admissions will screen positive for serious mental illness (Reference Birmingham, Mason and GrubinBirmingham et al, 1997; Reference Grubin, Birmingham and MasonGrubin et al, 1998). In terms of the proposed new screening protocol, individuals who ‘screen positive’ are further assessed by a psychiatric nurse, who will then determine the most appropriate course of action. As many of these cases would previously not have given rise to psychiatric assessment, there are clear resource implications in relation to the psychiatric provision needed to service the initial remand period.
This study was designed to clarify the nature and extent of psychiatric provision that would be needed if the new health screening protocol were to be introduced. It aimed to determine the number of new admissions to a male remand prison who would be expected to screen positive for serious mental illness, and to establish how many of these men would potentially need further psychiatric input.
Method
The study was carried out at HMP Holme House in Stockton-on-Tees, a local prison taking both remand and sentenced male prisoners, primarily from the Teeside area.
In line with national prison policy, all new inmates are seen on reception by a member of prison health care staff using a standard prison questionnaire, designed to screen for physical and mental health problems. The screening questionnaires for every inmate coming into the prison over a 15-week period were reviewed for a positive answer to one of the following four questions:
-
• • Is the inmate charged with homicide?.
-
• • Has the inmate ever received treatment from a psychiatrist for any form of mental health problem (not including treatment only in prison or one-off assessments)?
-
• • Has the inmate ever received antidepressant or anti-psychotic medication (outside prison only)?
-
• • Has the inmate ever deliberately harmed himself (DSH)?
Each Wednesday during this 15-week period, one of us (N.G.) attended the prison with the intention of assessing further those admitted within the previous 2 days who had screened positive to one of the above questions.
The assessments, which lasted between 15 and 30 minutes, were voluntary and confidential, with informed written consent obtained. The assessments took the form of a semi-structured interview that focused on both mental state and the circumstances associated with the positive response to the screening question(s). Further information was sought in particular about past psychiatric history and current mental state.
In cases where preliminary diagnoses were reached, further management was determined by a panel comprising the three authors (two psychiatrists and one nurse). The aim was to model how further input would be provided within the prison setting; for example, in cases where transfer to hospital was thought likely, the recommendation would be for urgent assessment by a psychiatrist. It was also noted from the healthcare records what, if any, follow-up had been arranged by the prison. In addition, the location of the prisoner, on the wing or in the healthcare centre, was noted.
Results
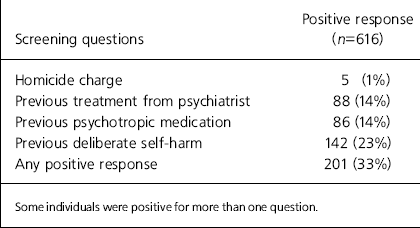
During the 15-week period, there were 616 new receptions to the prison. Prison screening questionnaires for each of these inmates were seen. Of these, 201 (33%) screened positive to one or more of the four questions. A breakdown of the results of the five questions is shown in Table 1.
Table 1. Positive responses to each of the five mental health screening questions
| Screening questions | Positive response (n=616) |
|---|---|
| Homicide charge | 5 (1%) |
| Previous treatment from psychiatrist | 88 (14%) |
| Previous psychotropic medication | 86 (14%) |
| Previous deliberate self-harm | 142 (23%) |
| Any positive response | 201 (33%) |
Of the 201 new receptions who screened positive, 96 had come into the prison in the 2 days prior to the research assessment. Of these, we were able to assess 39 (41%) in the time available. A further two inmates were asked to participate, but refused. In addition, four inmates were seen who had in fact been admitted between 2 and 4 days earlier. Overall, therefore, 43 (19%) of the new receptions who screened positive were interviewed.
Prevalence of mental disorder
Evidence was sought for the presence of mental illness, personality disorder, substance dependency and learning disability.
A preliminary diagnosis of mental illness was made in 10 (24%) of those seen. Of these three (7%) were acutely psychotic, six (14%) suffered from major depression, and one (2%) was diagnosed as suffering from minor depression. No diagnoses of mental illness were reached in three-quarters of those seen.
In terms of personality disorder, five of the 43 seen (12%) showed signs of gross personality dysfunction. Of these, three also showed evidence of substance dependency, one of whom was also diagnosed as having a major depressive illness. Two inmates (5%) were suspected of having a learning disability based on their performance at interview. Both were also comorbid for substance dependency. In relation to substance dependency, 24 of the 43 (56%) men reported symptoms suggestive of dependence on alcohol, heroin or amphetamines. Many of these also reported symptoms of low mood, but only four reached the threshold for a depressive episode at the time of interview.
Two inmates were thought to be at a high suicide risk. One had been identified by the prison, but the other had been missed. In this latter case, the prison medical officer was informed with the prisoner's agreement and he was transferred to the health care centre.
Prisoners of no fixed abode
Because homelessness is often associated with mental illness, we examined this as a separate variable. Of the 50 who were of no fixed abode 10 were interviewed. Of these, only two suffered from serious mental illness, both of whom also screened positive on one of the other four screening questions.
Recommended follow-up
Recommendations for psychiatric follow-up are shown in Table 2.
Table 2. Psychiatric follow-up recommended for each of the 43 inmates seen

| Psychiatric follow-up recommended | Number (%) |
|---|---|
| None | 19 (44%) |
| Prison doctor | 1 (2%) |
| Psychiatric nurse | 11 (26%) |
| Psychiatrist (routine) | 6 (14%) |
| Psychiatrist (urgent) | 3 (7%) |
| Collect further information | 1 (2%) |
| Learning disability assessment | 2 (5%) |
Assessment by a psychiatrist was recommended where a diagnosis of major mental illness was suspected. Those recommended for review by a psychiatric nurse were those in whom symptoms were unclear, resolving or thought to be secondary to substance misuse. Referral to the prison substance misuse team was recommended for all 24 inmates who were dependent on drugs or alcohol (some of whom might then have been reviewed by a psychiatric nurse). One inmate had recently been released from a psychiatric unit, but the reasons for his detention were unclear and recommendations could not be made in the absence of more information about him.
Comparing recommendations with practice
Our recommendations for follow-up based on the clinical assessments were compared with what had been arranged in practice by the prison. Of the nine inmates thought to require psychiatric assessment, four had been referred. Two who had not been identified by the prison were thought to require urgent assessment (and with their agreement, arrangements were made for this to take place, with both subsequently moved to the healthcare centre). All 24 inmates with dependency problems had been referred to the prison drug and alcohol service, although not all took up the offer.
Discussion
The findings in terms of numbers of new receptions screening positive for mental illness, and those in fact suffering from serious mental illnesses, were both in the range predicted from our earlier research, and are in line with prevalence rates described in large-scale remand prison surveys (Reference Singleton, Meltzer and GatwardSingleton et al, 1998). We therefore believe that our sampling procedure produced results from which generalised conclusions can be reached.
In total, 201 men (36% of the sample) screened positive for serious mental illness. If the new screening protocol were in place, this group would have required further review by a psychiatric nurse. As the 201 inmates were admitted over a 15-week period, about 15 psychiatric nursing assessments would be required each week on average.
Of those interviewed, diagnoses of mental illness were made in 10 (23%), of whom severe mental illness was identified in nine. Therefore, assuming that 23% of all those who screen positive suffer from mental illness (i.e. there was nothing special about the group who were interviewed), then mental illness would be detected in 8% of all new admissions (in this time-frame, 52 inmates). Given that we believe the screening process will miss 20% of those with mental illness, this suggests a total of 65 new receptions with serious mental illness, or 11% of total admissions, which is in line with prevalence surveys of remand prisoners.
Including the factor of being of no fixed abode in the screen would detect little in the way of severe psychiatric disorder not already identified by the other screening questions. Although a tempting inclusion, adding this as a screening variable would only reduce the specificity of the screen.
Based on our assessment, about 21% of those who initially screened positive would require input from a psychiatrist, 7% urgently (within 24 hours). This suggests that over a 15-week period, about 16 newly-received prisoners would require urgent psychiatric review (one per week), and a further 32 would need to be seen by a psychiatrist in the days following admission (two per week). An additional 26%, or 59 new receptions, would require further psychiatric nursing follow-up over the ensuing weeks.
Although this assessment was not primarily concerned with substance misuse, there is clearly a much bigger demand for treatment in respect of this, with over half of those screening positive for severe mental illness in fact having problems with substance misuse. We do not know how many additional inmates would have screened positive for substance misuse without first having screened positive for mental illness.
Based on this analysis, it does not appear that large demands will be placed on psychiatric resources if the proposed new reception health screening processes were in place, although a reorganisation of the way in which services are delivered will almost certainly be required.





eLetters
No eLetters have been published for this article.