Drug treatment is normally considered as an adjunctive rather than a primary treatment for personality disorders (American Psychiatric Association, 2001), but there is no particular reason for making this judgement, as all the trials of drug treatment in personality disorder have been primary ones. These trials of drug treatment, although admittedly easier to carry out than those of psychological treatment, are at least as good as those of other interventions and the results, for some treatments, more impressive in the short-term; but treatment has seldom persisted beyond a few weeks and has limitations.
Almost all drug trials for personality disorders have been for borderline personality disorder. In evaluating the evidence for efficacy it needs to be stressed that when treating this disorder it is difficult to disentangle mental state from personality components, as depression and other mood disturbance, suicidal behaviour, paranoid ideation and other abnormal thinking may all be present in the condition. There is therefore some doubt, when a drug treatment is effective in this condition, whether it is dealing with the core component of the disorder or a secondary mental state aspect ‘picked out’ from the personality background and treated separately.
Why might drugs help those with personality disorders?
Several lines of argument support the notion that drugs might have a place in the treatment of personality disorders.
The sub-syndromal or spectrum argument
Personality disorders can be considered as part of a spectrum in which they are envisaged as one component on a continuum of mental disorders (Reference Siever and DavisSiever & Davis, 1991) – a sub-syndromal model (Table 1). In this construct, schizotypal and paranoid personality disorders (Cluster A) are a sub-syndrome of schizophrenia; borderline personality and other Cluster B disorders are similarly linked to other impulsive and aggressive disorders; and anxious/fearful personality disorder (Cluster C) to the common anxiety disorders such as phobic and generalised anxiety disorders. This argument has some face validity and is supported by the frequent associations (comorbidity) of each mental state disorder with its personality counterpart (Reference Tyrer, Gunderson and LyonsTyrer et al, 1997). It remains one of the arguments for dispensing with Axis II and collapsing it into Axis I in any future revision of the DSM.
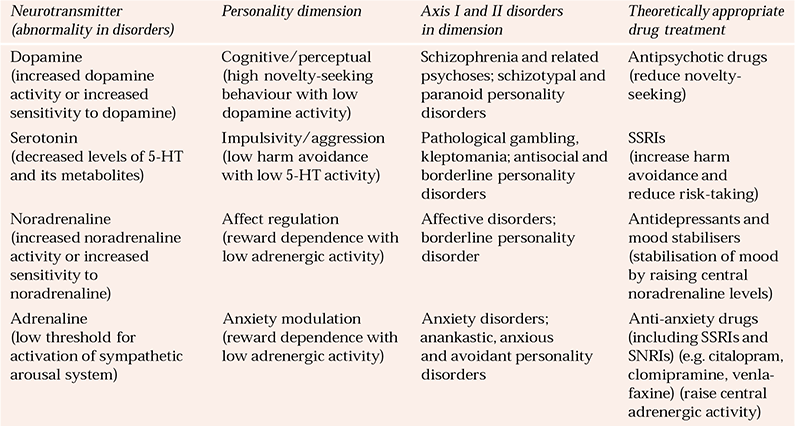
Table 1 Putative psychobiology of personality disorder, with implications for drug treatment
| Neurotransmitter (abnormality in disorders) | Personality dimension | Axis I and II disorders in dimension | Theoretically appropriate drug treatment |
|---|---|---|---|
| Dopamine (increased dopamine sensitivity to dopamine) | Cognitive/perceptual (high novelty-seeking behaviour with low dopamine activity) | Schizophrenia and related psychoses; schizotypal and paranoid personality disorders | Antipsychotic drugs (reduce novelty-seeking) |
| Serotonin (decreased levels of 5-HT and its metabolites) | Impulsivity/aggression (low harm avoidance with low 5-HT activity) | Pathological gambling, kleptomania; antisocial and borderline personality disorders | SSRIs (increase harm avoidance and reduce risk-taking) |
| Noradrenaline (increased noradrenaline activity or increased sensitivity to noradrenaline) | Affect regulation (reward dependence with low adrenergic activity) | Affective disorders; borderline personality disorder | Antidepressants and mood stabilisers (stabilisation of mood by raising central noradrenaline levels) |
| Adrenaline (low threshold for activation of sympathetic arousal system) | Anxiety modulation (reward dependence with low adrenergic activity) | Anxiety disorders; anankastic, anxious and avoidant personality disorders | Anti-anxiety drugs (including SSRIs and SNRIs) (e.g. citalopram, clomipramine, venlafaxine) (raise central adrenergic activity) |
A more elaborate model categorises personality disorder according to four dimensional constructs: cognitive/perceptual organisation, impulsivity/aggression, affective instability and anxiety/inhibition. Minor degrees of disorganisation are equivalent to personality disorder and major ones to mental illness. This notion has not achieved widespread support because it implies that personality disorganisation and disorder are precursors of (the more severe) mental illness, when in practice personality disorder often coexists with mental state disorders (Reference Tyrer, Gunderson and LyonsTyrer et al, 1997) but may also be quite separate from it.
The biological argument
In this argument for drug treatment, personality disorders are deemed to reflect underlying biologically determined temperaments, purportedly linked to neurobiological predispositions and vulnerabilities. This is supported indirectly by evidence that personality traits, characteristics or dimensions – the allegedly persistent building blocks of personality organisation – have high rates of heritability of around 50% (Reference Livesley, Jang and JacksonLivesley et al, 1993; Reference Jang, Livesley and VernonJang et al, 1996). But agreement on the key dimensions still needs to be reached, and the continuity between them and personality disorder itself must be substantiated.
Robert Cloninger has had a major influence on the terminology of the neurobiology of personality disorders. Over 15 years ago he introduced the concepts of novelty-seeking, harm avoidance and reward dependence in a three-factor model of personality disorder (Reference CloningerCloninger, 1987). This linked together personality and neurobiological dimensions (Table 1) and gave some justification for drug treatment. Thus, for example, someone with an impulsive personality disorder who had brief episodes of depression after negative events could be regarded as having high novelty-seeking and low harm avoidance and therefore a candidate for treatment with both antipsychotic drugs and selective serotonin reuptake inhibitors (SSRIs) (Tables 2 and 3). Cloninger subsequently further developed this concept with his Temperament and Character Inventory (TCI), to describe normal and abnormal personality variation (Reference Cloninger, Svrakic and PryzbeckCloninger et al, 1993). This too can be linked to abnormalities in neurotransmitter function, and Cloninger and his colleagues argue that they also account for differences in regional brain activity, psychophysiological variables, neuroendocrine abnormalities and specific gene polymorphisms. The TCI describes seven temperaments (novelty-seeking, reward dependence, harm avoidance, persistence, self-directedness, cooperativeness and selftranscendence), which can be used to describe variations between different personality disorders. Genetic and psychobiological studies are alleged to have led to identification of biological correlates for each of the TCI dimensions of personality, but currently there is limited empirical support for this, despite its obvious theoretical attractions and research opportunities (Reference Mitropoulou, Trestman and NewMitropoulou et al, 2003).
Table 2 Symptomatic approach to treatment of personality disorder with drugs (after Reference SoloffSoloff, 1998)

| Type of symptom | Preferred drug treatment |
|---|---|
| Cognitive/perceptual | Antipsychotics |
| Suspiciousness, paranoid ideation, ideas of reference, odd communication, muddled thinking, magical thinking, episodic distortions of reality, derealisation, depersonalisation, illusions, stress-induced hallucinations | |
| Affective dysregulation | SSRIs, MAOIs |
| Lability of mood, ‘rejection sensitivity’, mood crashes, inappropriate intense anger, temper outbursts, chronic emptiness, dysphoria, loneliness, anhedonia, social anxiety and avoidance | |
| Impulsive-behavioural dyscontrol | Mood stabilisers, SSRIs |
| Sensation-seeking, risky or reckless behaviour, no reflective delay, low frustration tolerance, impulsive aggression, recurrent assaultiveness, threats, property destruction, impulsive binges (drugs, alcohol, food, sex, spending), recurrent suicidal threats and behaviour, some self-mutilation |
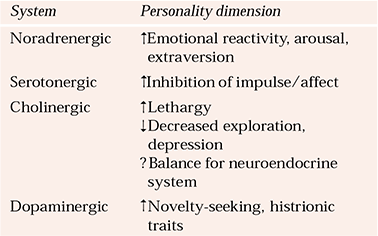
Table 3 Neurotransmitters and personality dimension
| System | Personality dimension |
|---|---|
| Noradrenergic | ↑Emotional reactivity, arousal, extraversion |
| Serotonergic | ↑Inhibition of impulse/affect |
| Cholinergic | ↑Lethargy |
| ↑Decreased exploration, depression | |
| ?Balance for neuroendocrine system | |
| Dopaminergic | ↑Novelty-seeking, histrionic traits |
In considering this evidence, the reader should be aware that neuropharmacology offers no clear guidance for the treatment of personality disorder with drugs: it is really a post hoc justification for treatment that has already been given. Abnormalities in neurobiological function found in personality disorder may not be central to the condition. For example, a patient with a personality disorder who is misusing drugs as well as taking some prescribed ones may show a set of abnormal neurotransmitter functions as a direct consequence only of the drug misuse. The best that pharmacology and physiology can offer is the justification for trying drug treatment: it cannot predict its efficacy. Even when a dimension is agreed (e.g. affective instability as a core feature of borderline personality disorder) its definition may vary. Some (Reference Cloninger, Svrakic and PryzbeckCloninger et al, 1993) see affective instability in terms of reward dependence, whereas others (Reference Van Reekum, Links, Federov and SilkVan Reekum et al, 1994) consider it as disinhibition. Which view is taken is of considerable importance when considering drug treatment. Cloninger sees novelty-seeking as being determined through genetic predisposition via the dopamine system, whereas many others consider affective disinhibition to be related to the serotonergic system. When no biological marker is linked clearly to diagnosis answers can only be speculative.
The symptoms argument
All patients with personality disorders show high levels of symptomatic distress, and groups of symptoms may be defining features of the disorders themselves. Affective and dissociative symptoms and brief psychotic experiences are operational criteria for the definition of borderline personality disorder; and perceptual distortions are an alleged core symptom of paranoid personality disorder. Thus, it becomes possible to develop a symptom-specific approach to drug treatment (Table 2).
Reference SoloffSoloff (1998) proposed a classification that has been adopted in the American Psychiatric Association guidelines for the treatment of borderline personality disorder (Reference Oldham, Phillips and GabbardOldham et al, 2001). Medication is used according to the balance of symptoms, and much of it can be predicted from knowledge of drug effects in mental state disorders. Overall, the clinician needs to determine whether the primary symptoms summarised in Table 2 are related to problems of affect control, impulsivity and aggression, or cognitive/perceptual disturbance, and then prescribe accordingly. The danger with this approach is that, because all patients with personality disorder suffer symptomatically, prescribing in personality disorder has shifted from being an occasional intervention to ‘normal’ practice, with little scientific justification. There is also no independent justification for the algorithm beyond that of expert opinion (albeit a good one in the case of Soloff), and as borderline personality disorder is so heterogeneous it is far from clear which particular component is being treated.
The neurotransmitter argument
Neurobiological research on personality disorder (Table 3) suggests that impulsiveness, self-harm and outwardly directed aggression are associated with dysfunction within the serotonergic system (Reference Linnoila and VirkkunenLinnoila & Virkkunen, 1992), blunted neuroendocrine responses to fenfluramine (Reference Rinne, Westenberg and den BoerRinne et al, 2000), and hyper-responsiveness of the hypothalamic–pituitary–adrenal axis, especially in female patients with borderline personality disorder and a history of sustained abuse. This effect appears to be independent of a comorbid diagnosis of post-traumatic stress disorder (Reference Rinne, de Kloet and WoutersRinne et al, 2002). Other neurotransmitter systems have been implicated in emotional reactivity and other personality traits.
Which drugs?
There has been a change in attitude towards the use of drugs in the treatment of personality disorder over the past 30 years, moving from rare use of medication to the current practice of almost universal prescription at some time during treatment. In longitudinal follow-up studies of patients with borderline personality disorder, over 75% had received polypharmacy (Reference Zanarini, Frankenburg and HennenZanarini et al, 2003). Indeed, in borderline personality disorder it is now not unusual for patients assessed for specialist treatment to have received almost all the common types of psychotropic drug at some time during previous management.
Almost every psychotropic drug has been used for the treatment of personality pathology, from hallucinogens to new anti-epileptics such as lamotrigine. This probably represents clinical desperation rather than evidence-based prescribing, because the overwhelming proportion of the literature comprises case reports and open or uncontrolled studies of patients who are receiving many different types of therapy.
Despite greater use of drugs, most people with personality disorders do not wish to have treatment and the minority that do should not be regarded as typical. It may be useful to separate personality disorders into type R (treatment-resisting) and type S (treatment-seeking) ones (Reference Tyrer, Mitchard and MethuenTyrer et al, 2003), with only the latter accepting treatment (of any sort) for their disorder on a voluntary basis. Some of the considerable variation between the research evidence for the effectiveness of drug treatment for different personality disorders may be a consequence of different proportions of types R and S in the studies. Paranoid and schizoid personalities have been rarely studied, probably because only around 1 in 10 are willing to accept any form of treatment (Reference Tyrer, Mitchard and MethuenTyrer et al, 2003). One of the reasons why borderline personality disorder has been most intensively researched (see below) is that sometimes patients present persistently with requests, and sometimes demands, for treatment.
As there is little to indicate that any form of psychotropic drug treatment is specific to any one personality disorder it is best to examine each drug class for its usage in the group as a whole, although it is in borderline personality that we have the most evidence.
Typical antipsychotics
These have been studied more than any other drug group in the treatment of personality disorder, but seldom in a satisfactory way. Early open clinical studies suggested that in low dosage these drugs might be effective in the treatment of both schizotypal and borderline personality disorders (Reference Perinpanayagam and HaigPerinpanayagam & Haig, 1977; Reference Brinkley, Beitman and FriedelBrinkley et al, 1979), and details of these have been nicely summarised by Reference Stein, Tyrer and SteinStein (1993). Since then, six randomised controlled trials have been carried out (Table 4) which, although to some extent encouraging, pose more questions than they have answered. Low-dosage typical antipsychotic drugs have some advantages over placebo, but the most impressive of these studies (Reference Soloff, George and NathanSoloff et al, 1986), which showed superiority of haloperidol over placebo and amitriptyline, failed to be replicated in a continuation study for 16 weeks. Reference Cornelius, Soloff and PerelCornelius et al(1993) reported that haloperidol showed superiority over placebo only for the symptom of irritability, although it was generally less effective than phenelzine. The high drop-out rate (which is more than twice the rate for placebo) may also have contributed to the poorer outcome.
Table 4 Summary of randomised trials of antipsychotic drugs in the treatment of personality disorder

| Antipsychotic tested | Personality diagnosis | Author(s) | Type of study | Main results |
|---|---|---|---|---|
| Haloperidol | Borderline | Reference Soloff, George and NathanSoloff et al, 1986 | Randomised controlled trial | Haloperidol (7mg/day) superior to both amitriptyline and placebo |
| Trifluoperazine | Borderline | Reference Cowdry and GardnerCowdry & Gardner, 1988 | Cross-over trial | No clear advantages of trifluoperazine over other (active) treatments |
| Thiothixene | Borderline & schizotypal | Reference Goldberg, Shulz and ShulzGoldberg et al, 1986 | Randomised controlled trial | Thiothixene superior to placebo in both groups |
| Haloperidol | Borderline | Reference Cornelius, Soloff and PerelCornelius et al, 1993 | Randomised controlled trial | Haloperidol superior for irritability symptoms alone |
| Olanzapine | Borderline | Reference Zanarini and FrankenburgZanarini & Frankenburg, 2001 | Randomised controlled trial | Olanzapine superior to placebo, except for depression (only 9 patients received placebo) |
| Risperidone | Schizotypal | Reference Koenigsberg, Reynolds and GoodmanKoenigsberg et al, 2003 | Randomised controlled trial | Significant benefit of risperidone for PANSS |
Antipsychotics have also been used to prevent recurrent self-harm, and in one randomised study (Reference Montgomery and MontgomeryMontgomery & Montgomery, 1982) flupentixol was efficacious in preventing further episodes.
Atypical antipsychotics
Subsequent studies have, unsurprisingly, turned to the use of atypical neuroleptics, and two small trials with olanzapine and risperidone give some support for their efficacy (Reference Zanarini and FrankenburgZanarini & Frankenburg, 2001; Reference Koenigsberg, Reynolds and GoodmanKoenigsberg et al, 2003) (Table 4). There have also been encouraging open studies with clozapine, olanzapine and quetiapine (Reference Frankenburg and ZanariniFrankenburg & Zanarini, 1993; Reference Benedetti, Sforzini and ColomboBenedetti et al, 1998; Reference Zullino, Haefliger and StiglerZullino et al, 2002; Reference Walker, Thomas and AllenWalker et al, 2003) that suggest better compliance as well as efficacy with the atypical antipsychotics than with the typical ones. Olanzapine is currently being tested in a large-scale multicentre trial of borderline personality disorder.
The jury is still out on the claim that antipsychotic drugs are effective in the treatment of personality disorder, but it seems likely that they have a place in treatment that remains to be defined adequately. They are clearly likely to be effective in the presence of psychotic symptoms. As these are most prominent in people with borderline and schizotypal personality disorders the practitioner needs to be aware of this group of drugs as having some therapeutic potential.
Tricyclic antidepressants and selective serotonin reuptake inhibitors
In the original study by Reference Soloff, George and NathanSoloff et al(1986), amitriptyline was not helpful in the treatment of borderline personality disorder (indeed, it was of less value than haloperidol even in the treatment of depression) and its lack of value has become the accepted view. However, it is fair to note than there have been very few studies of tricyclic antidepressants in the treatment of personality disorder and none of the recent ones has included a tricyclic control. In a randomised trial of the treatment of common anxiety and depressive disorders that continued for 2 years after the formal trial was over, those allocated to the tricyclic antidepressant dothiepin had the same outcome irrespective of whether or not they had a personality disorder, whereas those allocated to psychological treatments (self-help and cognitive–behavioural therapy) fared worse if they had comorbid personality disorder (Reference Tyrer, Seivewright and FergusonTyrer et al, 1993). It is possible that this is because the drug treatment also positively influenced personality status, which has been suggested in another study (Reference Ekselius and Von KnorringEkselius & Von Knorring, 1998).
In contrast, the selective serotonin reuptake inhibitors have been widely assessed against placebo control in formal trials. They have been found to be effective in reducing aggressive, impulsive and angry behaviour in those with borderline and aggressive personality disorders, as the biological theories would suggest (Reference Salzman, Wolfson and SchatzbergSalzman et al, 1995; Reference Coccaro and KavoussiCoccaro & Kavoussi, 1997) (Table 4). The benefit of these drugs is unlikely to be a direct consequence of their antidepressant effect, although it could be connected – a similar study of fluoxetine in patients with depression and alcoholism showed improvement in both depression and drinking behaviour compared with placebo (Reference Cornelius, Salloum and EhlerCornelius et al, 1997). Although personality disorder was not measured in this study, it is likely that a substantial proportion – about 50%, from prevalence figures in this clinical population (Reference Bowden-Jones, Iqbal and TyrerBowden-Jones et al, 2004) – had this condition.
Self-harm may be a form of anger – self-directed anger – and this too is reduced by SSRIs, with paroxetine giving the best evidence, but again in a population in which personality disorder was highly prevalent but was not recorded (Reference Verkes, Van der Mast and HengeveldVerkes et al, 1998).
Against this evidence, the prescriber should be aware of the current controversy over the possibility that suicidal behaviour may be provoked by SSRIs in a minority of patients (Reference HealyHealy, 2003).
Monoamine oxidase inhibitors
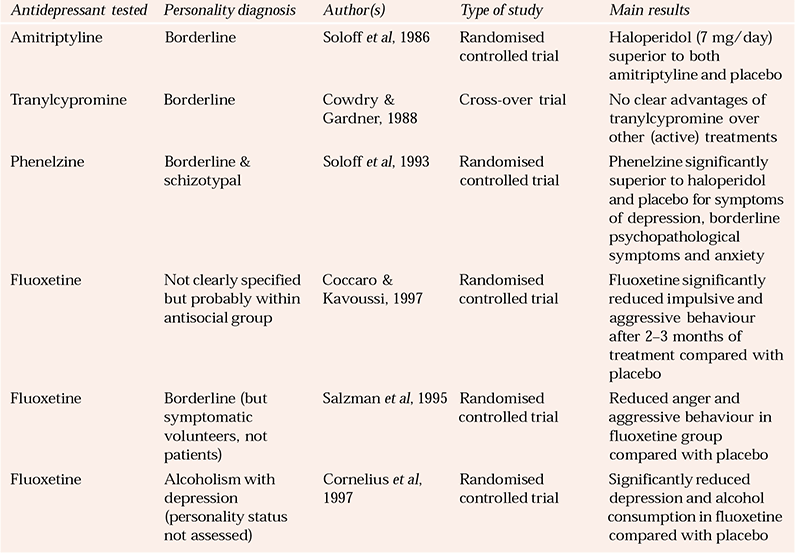
Monoamine oxidase inhibitors (MAOIs) are now used relatively infrequently in treatment despite an impressive record of efficacy (Reference Tyrer and Harrison-ReadTyrer & Harrison-Read, 1990), but there is some evidence that tranylcypromine and phenelzine are efficacious in borderline personality disorder (Reference Cowdry and GardnerCowdry & Gardner, 1988; Reference Soloff, Cornelius and GeorgeSoloff et al, 1993) (Table 5). However, the high frequency of self-harm and the risks of overdose with these drugs are likely to inhibit prescription. The newer reversible MAOI moclobemide has not been studied in the treatment of personality disorder.
Table 5 Summary of randomised trials of antidepressant drugs in the treatment of personality disorder
| Antidepressant tested | Personality diagnosis | Author(s) | Type of study | Main results |
|---|---|---|---|---|
| Amitriptyline | Borderline | Reference Soloff, George and NathanSoloff et al, 1986 | Randomised controlled trial | Haloperidol (7 mg/day) superior to both amitriptyline and placebo |
| Tranylcypromine | Borderline | Reference Cowdry and GardnerCowdry & Gardner, 1988 | Cross-over trial | No clear advantages of tranylcypromine over other (active) treatments |
| Phenelzine | Borderline & schizotypal | Reference Soloff, Cornelius and GeorgeSoloff et al, 1993 | Randomised controlled trial | Phenelzine significantly superior to haloperidol and placebo for symptoms of depression, borderline psychopathological symptoms and anxiety |
| Fluoxetine | Not clearly specified but probably within antisocial group | Reference Coccaro and KavoussiCoccaro & Kavoussi, 1997 | Randomised controlled trial | Fluoxetine significantly reduced impulsive and aggressive behaviour after 2–3 months of treatment compared with placebo |
| Fluoxetine | Borderline (but symptomatic volunteers, not patients) | Reference Salzman, Wolfson and SchatzbergSalzman et al, 1995 | Randomised controlled trial | Reduced anger and aggressive behaviour in fluoxetine group compared with placebo |
| Fluoxetine | Alcoholism with depression (personality status not assessed) | Reference Cornelius, Salloum and EhlerCornelius et al, 1997 | Randomised controlled trial | Significantly reduced depression and alcohol consumption in fluoxetine compared with placebo |
Mood stabilisers
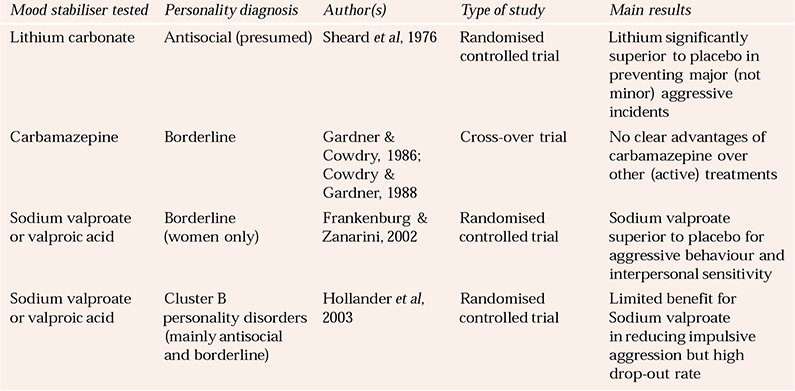
All known mood stabilisers have been used in the treatment of personality disorder and, to some extent, evaluated formally, but again almost entirely in borderline personality disorder, which is characterised by marked fluctuations in mood (Table 6). Lithium may stabilise the serotonergic system and, as an effective mood stabiliser, is also an empirically sensible pharmacotherapy to investigate in personality disorders. The evidence for the efficacy of lithium is small, but relatively good. In an early study, Reference Sheard, Martin and BridgesSheard et al(1976) showed that lithium reduced aggression markedly in prisoners with personality disorder (but not formally assessed for the condition), and other studies (Reference Tyrer, Walsh and EdwardsTyrer et al, 1984; Reference Links, Steiner and BoiagoLinks et al, 1990) support its anti-aggressive properties. Carbamazepine has also some presumptive evidence of efficacy, but this is not well established as the trials have been limited in numbers (Reference Gardner and CowdryGardner & Cowdry, 1986; Reference De La Fuenta and LostraDe La Fuenta & Lostra, 1994). Valproate in the form of divalproex sodium has been assessed in the treatment of borderline personality disorder and other disorders in the Cluster B group and two small randomised trials support its efficacy compared with placebo (Reference Frankenburg and ZanariniFrankenburg & Zanarini, 2002; Reference Hollander, Tracy and SwannHollander et al, 2003).
Table 6 Summary of randomised trials of mood stabilisers in the treatment of personality disorder
| Mood stabiliser tested | Personality diagnosis | Author(s) | Type of study | Main results |
|---|---|---|---|---|
| Lithium carbonate | Antisocial (presumed) | Reference Sheard, Martin and BridgesSheard et al, 1976 | Randomised controlled trial | Lithium significantly superior to placebo in preventing major (not minor) aggressive incidents |
| Carbamazepine | Borderline | Reference Gardner and CowdryGardner & Cowdry, 1986; Reference Cowdry and GardnerCowdry & Gardner, 1988 | Cross-over trial | No clear advantages of carbamazepine over other (active) treatments |
| Sodium valproate or valproic acid | Borderline (women only) | Reference Frankenburg and ZanariniFrankenburg & Zanarini, 2002 | Randomised controlled trial | Sodium valproate superior to placebo for aggressive behaviour and interpersonal sensitivity |
| Sodium valproate or valproic acid | Cluster B personality disorders (mainly antisocial and borderline) | Reference Hollander, Tracy and SwannHollander et al, 2003 | Randomised controlled trial | Limited benefit for Sodium valproate in reducing impulsive aggression but high drop-out rate |
Other drugs
A number of benzodiazepines, particularly alprazolam (Reference Reich, Noyes and YatesReich et al, 1980; Reference Cowdry and GardnerCowdry & Gardner, 1988), have been tested in the treatment of personality disorder, but their use is generally discouraged because of dependence risks. Despite this, in clinical practice benzodiazepines are prescribed widely, and people with personality disorders are much more likely to take them long-term than those without (Reference Seivewright, Tyrer and CaseySeivewright et al, 1991). This might be considered a negative consequence but it might also suggest continued efficacy despite the worry about dependence.
Naltrexone (Reference Roth, Ostroff and HoffmanRoth et al, 1996) and venlafaxine (Reference Markovitz and WagnerMarkovitz & Wagner, 1995) have also been claimed to be of value, but no satisfactory studies have yet been carried out in personality disorder.
Prescribing in clinical practice
Recommendations regarding prescribing practice in personality disorder can be made on the basis of research trial data and clinical consensus (Box 1). In trials, drop-out rates are high and non-compliance with medication dosage and frequency is common. These findings concur with clinical experience and can sometimes lead to despair. Many patients with personality disorder (particularly in the Cluster B group) take medication intermittently, fail to follow prescribing guidance and may use prescribed medication in overdose when in crisis. These facts alone suggest that prescribing must be done carefully and preferably within the context of a trusting therapeutic relationship.
Box 1 Summary of guidelines for psychopharmacological treatment
Consider the primary symptom complex (e.g. affect dysregulation, impulsivity, cognitive/perceptual disturbance) and current transference and countertransference themes
Discuss implementation of medication with the treatment team
Educate the patient about reasons for medication, possible side-effects and expected positive effects
Make a clear recommendation but allow the patient to take the decision; do not try to persuade the patient to take the medication
Agree a length of time for trial of medication (unless intolerable side-effects) and do not prescribe another drug during this time, even if the patient stops taking the drug
Prescribe within safety limits, e.g. give prescriptions weekly
See the patient at agreed intervals to discuss medication and its effects: initially, this may be every few days to encourage compliance, to monitor effects and to titrate the dose
Do not be afraid to suggest stopping a drug if no benefit is observed and the patient experiences no improvement
The use and effects of medication need to be discussed with patients prior to prescribing, the target symptoms clearly identified, an agreement made about how long a drug is to be used and a method to monitor its effect on symptoms established. Most important is the patient's agreement to take medication in the first place, and the role of the doctor is initially to provide information and to remain neutral. After information has been given to the patient the prescriber may make a recommendation, but should not become overly engaged in persuading the patient to follow advice. The more a prescriber attempts to convince a patient to take a drug, the greater the patient's resistance may be, and a patient bullied into taking a medication is not likely to maintain its consumption spontaneously. The physician should not, of course, remain neutral if there is a reason to advise against a specific drug.
Some patients with personality disorders seek quick results, yet the effects of medication (e.g. antipsychotics and antidepressants) may take some time to become apparent. It is therefore necessary to warn patients of likely delay, so that drugs will not be stopped if there is no benefit initially. The best way to do this is to take an interest in how the patient responds to the tablets and to arrange regular meetings to discuss symptom change, side-effects and changes in dose. In general, patients should expect to take medication for at least 2–4 weeks (unless there are intolerable side-effects) and this ‘rule’ is best agreed when prescription is started. If the patient stops a drug unilaterally before the agreed time, no other drug should be prescribed until the 2–4 week period is completed. This reduces the demand for drug after drug when no effect occurs within a few days and prevents ‘creeping’ polypharmacy. Reference Soloff, Cornelius and GeorgeSoloff and colleagues (1993) have suggested that the exception to rules of this type is antipsychotic medication such as haloperidol, as the benefits may occur rapidly but wane within a few weeks. Discontinuation may therefore be appropriate after a short period, although there remains little information on the use of newer antipsychotics.
Discontinuation of medication needs to be done carefully. Many clinicians believe that patients with borderline personality disorder are not only more prone than other patients to placebo responsiveness (Reference Soloff, Cornelius and GeorgeSoloff et al, 1993) but are also more sensitive to the side-effects and withdrawal effects of medication, although there is little evidence that this is the case. Nevertheless, reducing medication slowly, even when another is being introduced simultaneously, is probably the best course.
Transference and countertransference
Maintaining sensible rules is harder than it sounds, because patient demand and clinician judgement are influenced by transference and countertransference phenomena. Psychiatrists are not immune from countertransference responses, even if their task is solely to look after medication. They may find it difficult to process their feelings and prescribe in a desire to ‘rescue’ a patient or in a vain attempt to ‘do something’. These reactions may account for the high number of medications that patients with borderline personality disorder take over time, even though polypharmacy is rarely recommended (Reference Zanarini, Frankenburg and HennenZanarini et al, 2003). Conversely, a patient who wishes to stop medication may be persuaded to continue it because of the psychiatrist's fear of relapse. Often it is patients themselves who ask to reduce the number of medications that they are taking, and many begin taking tablets on an intermittent basis without telling their psychiatrist, for fear of causing disappointment.
Conclusions
Despite many reservations, it is clear that medication will continue to be used in the treatment of personality disorder and that it has the potential to be an important intervention. This has recently been formally acknowledged in official guidelines for the treatment of one group, patients with borderline personality disorder (American Psychiatric Association, 2001), but drugs are suggested only as an adjunctive treatment. However, if recommendations are based on the evidence alone, there is no reason why drug treatment should be regarded as secondary and psychological treatment primary (Reference TyrerTyrer, 2002). Nevertheless, the general level of adherence to drug treatment and its acceptability to patients are low, and if drugs are to be prescribed more consistently this problem needs to be addressed.
MCQs
-
1 Drug treatment for personality disorders:
-
a is well established as an effective treatment
-
b is more often used in patients with borderline personality disorder
-
c is usually associated with good adherence to treatment
-
d interferes with the success of psychological therapies
-
e can be linked to biological abnormalities.
-
-
2 Antipsychotic drugs prescribed for personality disorder:
-
a are more effective in higher than lower dosages
-
b are contraindicated in those with brief psychotic episodes
-
c are better given as depot than oral preparations
-
d are generally better given to patients with borderline disorder rather than to those with dependence
-
e are associated with paradoxical aggression.
-
-
3 The following drugs have some evidence of efficacy (excluding open studies) in the personality disorders:
-
a lithium
-
b diazepam
-
c sodium valproate
-
d fluoxetine
-
e carbamazepine.
-
-
4 Personality disorders should not normally be treated with drug therapy when:
-
a there is evidence of affective instability
-
b there are limited means of monitoring progress
-
c there is a history of persistent drug misuse
-
d there is comorbid mental state disorder
-
e there is concurrent learning disability.
-
-
5 The following drugs have been shown to be of benefit in preventing recurrence of self-harm:
-
a moclobemide
-
b paroxetine
-
c amitriptyline
-
d olanzapine
-
e lithium.
-
MCQ answers

| 1 | 2 | 3 | 4 | 5 | |||||
|---|---|---|---|---|---|---|---|---|---|
| a | F | a | F | a | T | a | F | a | F |
| b | T | b | F | b | F | b | T | b | T |
| c | F | c | F | c | T | c | T | c | F |
| d | F | d | T | d | T | d | F | d | F |
| e | T | e | F | e | T | e | F | e | F |








eLetters
No eLetters have been published for this article.