Psychotropic medication use is common in industrialised countries. A cross-sectional telephone survey in France, Germany, Italy and the UK found that 6.4% of the population were using a psychotropic medication (Reference Ohayon and LaderOhayon & Lader, 2002). Furthermore, use of these medications appears to be increasing (Reference Middleton, Gunnell and WhitleyMiddleton et al, 2001; Reference Olfson, Marcus and DrussOlfson et al, 2002; Reference Helgason, Tomasson and ZoegaHelgason et al, 2004). Longitudinal birth cohort studies can bring a unique perspective to the study of these phenomena. They include not only population trends with respect to medication use, but also trends over time at the individual level, capturing age and period effects. We describe use of antidepressants, anxiolytics and hypnotics, and the associations between use of these medications and common mental disorder up to age 53 years in a general population birth cohort spanning the second half of the 20th century, the era of modern psychotropic drug treatments. We predicted that use of psychotropic medication would increase as the cohort aged, but that a substantial proportion of participants with evidence of depression and anxiety would remain untreated.
METHOD
Participants
The sample consisted of participants in the Medical Research Council National Survey of Health and Development (NSHD). This survey was originally conceived as a study of maternity, and included every child born in England, Scotland or Wales during the week of 3-9 March 1946 (Reference WadsworthWadsworth, 1991). From all the singleton births to married women a stratified sample of 5362 individuals was selected by taking a random 1 in 4 of all births to women married to manual workers, and all births to women married to non-manual and agricultural workers. That sample has been prospectively studied on 22 occasions up to age 53 years. Data included information on development, education, physical and mental health, employment and many other features (Reference WadsworthWadsworth, 1991; Reference Wadsworth, Butterworth and HardyWadsworth et al, 2003).
Follow-up of those alive and still resident in England, Scotland or Wales has been very successful; more than 80% have been followed throughout the cohort's adult years, excluding those who died, emigrated or have permanently withdrawn from the study (Reference Wadsworth, Butterworth and HardyWadsworth et al, 2003). Analyses show few significant biases between those who remained in the study and those who did not (Reference Wadsworth, Mann and RodgersWadsworth et al, 1992), and comparisons with census data suggest that the remaining cohort (n=3673 at age 53 years) is broadly representative of all native-born adults of a similar age and currently resident in England, Scotland or Wales (Reference Wadsworth, Butterworth and HardyWadsworth et al, 2003).
Psychiatric treatment
Survey members reported all prescription medication use in a postal questionnaire at age 31 years, and in person to a nurse interviewer at ages 36, 43 and 53 years. Medications recorded were then matched to a British National Formulary (BNF) code (British Medical Association & Royal Pharmaceutical Society of Great Britain, 2002) by a trained research nurse. Medications described in this report are those used for treatment of common psychiatric symptoms: hypnotics (BNF section 4.1.1), anxiolytics (BNF section 4.1.2) and antidepressants (BNF section 4.3). In addition, survey members were asked at age 36 years and age 43 years if they had visited a physician in the previous year for ‘nerves’.
Definitions
Throughout this paper we use the term ‘common mental disorder’ to describe cases of mental disorder characterised by symptoms of depression and/or anxiety (Reference GoldbergGoldberg, 1991).
Common mental disorder
Presence of adult common mental disorder was measured by the Present State Examination (PSE; Reference Wing, Cooper and SartoriusWing et al, 1974) at age 36 years, by the Psychiatric Symptom Frequency scale (PSF; Reference Lindelow, Hardy and RodgersLindelow et al, 1997) at age 43 years and by the 28-item General Health Questionnaire (GHQ; Reference Goldberg and HillierGoldberg & Hillier, 1979) at age 53 years. Survey members were categorised as cases at age 36 years if they scored 5 or higher on the Index of Definition on the PSE (Reference Wing, Mann and LeffWing et al, 1978), yielding a prevalence of 6%. Survey members were categorised as cases if they scored in the most severely affected 6% on the PSF and GHQ at ages 43 and 53 years respectively.
Statistical method
Prevalence of reported use of antidepressants, anxiolytics and hypnotics at ages 31, 36, 43 and 53 years is presented as crude data and as number of individuals per 1000 persons in the survey population. The trend in prevalence over these four ages was analysed using a chi-squared test for trend. Prevalence of antidepressant, anxiolytic or hypnotic use among those with common mental disorder is presented as a proportion, and associations between medication use and common mental disorder are presented using odds ratios and 95% confidence intervals. The association between severity of symptoms of common mental disorder and prevalence of antidepressant, anxiolytic or hypnotic use was analysed using a chi-squared test for trend. Prevalence of antidepressant, anxiolytic or hypnotic use and associations between medication use and common mental disorder over time are presented with proportions, ORs and 95% CIs. The focus of our analysis was common mental disorders, so we eliminated individuals who reported use of antipsychotics (BNF sections 4.2.1 and 4.2.2) or mood stabilisers (antimanic drugs; BNF section 4.2.3) at any time during the follow-up period (n=55). All analyses were performed using Stata version 8.0 for Windows.
RESULTS
Prevalence of antidepressant, anxiolytic and hypnotic use
Prevalence of any antidepressant, anxiolytic or hypnotic use increased significantly from 1977 (30.6 per 1000) through 1982 (44.6 per 1000) and 1989 (45.2 per 1000) to 1999 (59.1 per 1000) (χ2 test for trend, P<0.001), as the cohort aged (Table 1). Prevalence of individuals using more than one class of psychotropic medication was low: 5.4 per 1000 in 1977, 4.3 per 1000 in 1982, 4.7 per 1000 in 1989, to 7.1 per 1000 in 1999.
Table 1 Prevalence of antidepressant, anxiolytic and hypnotic use in the National Survey of Health and Development in 1977, 1982, 1989 and 1999

| Year | 1977 | 1982 | 1989 | 1999 |
|---|---|---|---|---|
| Age of cohort, years | 31 | 36 | 43 | 53 |
| Size of sample reporting, n | 3299 | 3272 | 3211 | 2945 |
| Medication use, n | ||||
| Any antidepressant, anxiolytic or hypnotic | 101 | 146 | 145 | 174 |
| More than one class | 18 | 14 | 15 | 21 |
| Hypnotics | 19 | 30 | 46 | 28 |
| Anxiolytics | 71 | 97 | 61 | 25 |
| Antidepressants | 33 | 35 | 58 | 144 |
| Tricyclic antidepressants | 31 | 30 | 56 | 77 |
| MAO inhibitors | 1 | 2 | 0 | 0 |
| Compound antidepressants | 0 | 1 | 0 | 2 |
| SSRIs | 0 | 0 | 1 | 61 |
| Other antidepressants | 1 | 4 | 3 | 10 |
MAO, monoamine oxidase; SSRIs, selective serotonin reuptake inhibitors
Use of specific classes of medications in 1977 (age 31), 1982 (age 36), 1989 (age 43) and 1999 (age 53) is shown in Table 1. Use of anxiolytic medications dropped from 1977 to 1999, whereas antidepressant use, in contrast, increased. With regard to specific medications, the most common drug in 1977, 1982 and 1989 was diazepam (13.9, 16.5 and 12.8 per 1000 respectively). In 1999 the most common medication was the tricyclic antidepressant amitriptyline (10.9 per 1000), followed by the selective serotonin reuptake inhibitor fluoxetine (9.2 per 1000).
Associations between antidepressant, anxiolytic or hypnotic use and common mental disorder
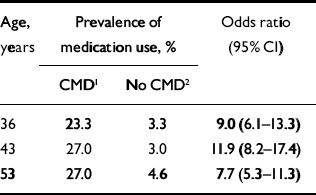
Table 2 shows the prevalence of antidepressant, anxiolytic or hypnotic use among individuals with and without common mental disorder at ages 36, 43 and 53 years. Prevalence of medication use among those with such disorder was relatively constant: 23.3% at age 36, 27.0% at age 43 and 27.0% at age 53. Those identified as having a common mental disorder were significantly more likely to be using these psychotropic medications than those below the cut-off for such disorder, with OR in the range 7.7-11.9 (Table 2).
Table 2 Association between antidepressant, anxiolytic or hypnotic use and common mental disorder at ages 36, 43, and 53 years
| Age, years | Prevalence of medication use, % | Odds ratio (95% CI) | ||
|---|---|---|---|---|
| CMD 1 | No CMD 2 | |||
| 36 | 23.3 | 3.3 | 9.0 (6.1–13.3) | |
| 43 | 27.0 | 3.0 | 11.9 (8.2–17.4) | |
| 53 | 27.0 | 4.6 | 7.7 (5.3–11.3) | |
CMD, common mental disorder
1. Sample n=189 at age 36, n=200 at age 43, n=174 at age 53 years
2. Sample n=3057 at age 36, n=2994 at age 43, n=2925 at age 53 years
Among those using an antidepressant, anxiolytic or hypnotic, only 30.6% were identified as having a common mental disorder at age 36, 37.5% at age 43 and 27.2% at age 53 years. Figure 1 shows that those using an antidepressant, anxiolytic or hypnotic who did not reach the threshold for common mental disorder might have been experiencing sub-threshold or partially treated symptoms. A significant trend can be seen between severity of symptoms and prevalence of medication use at ages 36, 43 and 53 years (χ2 test for trend; P<0.001 for all three ages).

Fig. 1 Association between previous antidepressant, anxiolytic or hypnotic use and severity of common mental symptoms at ages 36, 43, and 53 years. GHQ, General Health Questionnaire; PSE, Present State Examination; PSF, Psychiatric Symptom Frequency.
Physician visits for ‘nerves’
At age 36 years, 10.6% of survey members reported seeing a physician for treatment of ‘nerves’ in the past year, and 5.3% reported seeing a physician for the same reason at age 43. Less than half of those with common mental disorder reported visiting a physician for treatment of nerves in the previous year (43.3% and 38.2% at age 36 and age 43 respectively). Among those who had a common mental disorder at age 36 and had seen a physician for treatment of nerves in the previous year, 47.9% were using an antidepressant, anxiolytic or hypnotic, whereas the corresponding figure at age 43 was 57.4%. Finally, among those who were currently using an antidepressant, anxiolytic or hypnotic, 37.0% and 43.7%, at age 36 and 43 respectively, did not report having seen a physician for treatment of nerves in the past year.
Antidepressant, anxiolytic and hypnotic use over time
Investigation of medication use over time revealed that previous use of antidepressants, anxiolytics or hypnotics was a strong predictor of future use (Table 3). Individuals who used such medications at age 31 were 14.5 times more likely to use them at age 36 than those not using these drugs at age 31. Similar associations could be seen from age 36 to age 43, and from age 43 to age 53. Longer-term associations were also evident - individuals who used antidepressants, anxiolytics or hypnotics at age 31 were 9.8 times more likely to use these medications at age 53 than those not using them at age 31.
Table 3 Association between previous antidepressant, anxiolytic or hypnotic use and current use at ages 36, 43 and 53 years

| Odds ratios for medication use | |||||
|---|---|---|---|---|---|
| Age 36 years OR (95% CI) | Age 43 years OR (95% CI) | Age 53 years OR (95% CI) | |||
| Previous antidepressant, anxiolytic or hypnotic use at age | |||||
| 31 years | 14.5 (9.0–23.4) | 8.5 (5.0–14.4) | 9.8 (5.8–16.5) | ||
| 36 years | 10.0 (6.4–15.6) | 8.6 (5.5–13.3) | |||
| 43 years | 8.8 (5.7–13.6) | ||||
During an episode of common mental disorder, individuals were more likely to use antidepressants, anxiolytics or hypnotics if they had used such medications in the past (Table 4). Individuals at age 36, for example, were 8.6 times more likely to use antidepressants, anxiolytics or hypnotics during an episode of common mental disorder if they had used these drugs at age 31. Similar results were observed for those with common mental disorder at ages 43 and 53, although the effect was less pronounced at each subsequent age. It is notable that the proportion of individuals who had used antidepressants, anxiolytics or hypnotics in the past and continued to use them in a subsequent episode of common mental disorder dropped as the cohort aged. For example, only 40.0% of individuals who had previously used an antidepressant, anxiolytic or hypnotic chose this treatment during an episode of common mental disorder at age 53.
Table 4 Association between previous antidepressant, anxiolytic or hypnotic use and current use among those with common mental disorder at ages 36, 43 and 53 years

| Age, years | Prevalence of medication use during episode of CMD, % | Odds ratio (95% CI) | ||
|---|---|---|---|---|
| Previous use 1 | No previous use 2 | |||
| 36 | 62.5 | 16.2 | 8.6 (3.4–22.2) | |
| 43 | 51.6 | 20.5 | 4.1 (1.8–9.5) | |
| 53 | 40.0 | 19.3 | 2.8 (1.3–6.2) | |
CMD, common mental disorder
1. Sample n=24 at age 36, n=31 at age 43, n=40 at age 53 years
2. Sample n=136 at age 36, n=127 at age 43, n=109 at age 53 years
DISCUSSION
Population trends in use of psychotropic medications
Since their birth in 1946, members of the Medical Research Council National Survey of Health and Development have lived through an age of tremendous change in the treatment of mental disorders. The use of antidepressants, anxiolytics and hypnotics by cohort members over the past 30 years reflects general population trends as provided by prescription data in other studies. With regard to antidepressant use by members of the survey, for example, there was a significant increase from 1977 to 1999, as has been reported elsewhere (Reference Middleton, Gunnell and WhitleyMiddleton et al, 2001; Reference Olfson, Marcus and DrussOlfson et al, 2002; Reference Helgason, Tomasson and ZoegaHelgason et al, 2004). This period also saw the initiation of the Defeat Depression Campaign in Britain, during which there was increasing awareness of depression and treatment with antidepressants among the British population (Reference Paykel, Hart and PriestPaykel et al, 1998). Although the dramatic increase in antidepressant use can be attributed to the introduction of selective serotonin reuptake inhibitors, this has not resulted in a corresponding drop in the use of tricyclic antidepressants (Reference Middleton, Gunnell and WhitleyMiddleton et al, 2001; Reference Helgason, Tomasson and ZoegaHelgason et al, 2004). At the same time, however, the cohort has been ageing. The use of psychotropic medications increases with age, as has been demonstrated in several countries (Reference Middleton, Gunnell and WhitleyMiddleton et al, 2001; Reference Ohayon and LaderOhayon & Lader, 2002; Reference Bebbington, Brugha and MeltzerBebbington et al, 2003). Consequently, the increase observed in our study probably reflects both an ageing effect and a time-period effect.
Mental disorder and use of antidepressants, anxiolytics and hypnotics
The associations between mental disorder among members of the NSHD and psychiatric treatment are notable. At ages 36 and 43, less than half of those with common mental disorder had visited a physician for treatment for nerves in the previous year. Less than a third of individuals with common mental disorder were using a psychotropic medication at ages 36, 43 and 53. These results mirror studies from numerous countries that show that less than half of individuals with common mental disorder seek physician treatment (Reference Howard, Cornille and LyonsHoward et al, 1996; Reference Lefebvre, Lesage and CyrLefebvre et al, 1998; Reference Andrews, Henderson and HallAndrews et al, 2001; Reference Spijker, Bijl and de GraafSpijker et al, 2001; Reference Bebbington, Brugha and MeltzerBebbington et al, 2003; Reference Burns, Eichenberger and EichBurns et al, 2003), and less than 40% use psychotropic medications (Reference Spijker, Bijl and de GraafSpijker et al, 2001; Reference Bebbington, Brugha and MeltzerBebbington et al, 2003; Reference Simon, Fleck and LucasSimon et al, 2004; Reference Patten, Williams and WangPatten et al, 2005).
It is less clear why the majority of individuals with evidence of common mental disorder are not treated for it. There is a strong body of evidence suggesting that an important factor is patient perception of the need for help. In the National Comorbidity Survey in the USA, only 34% of 1792 individuals with mood and/or anxiety disorders perceived a need for professional help (Reference Mojtabai, Olfson and MechanicMojtabai et al, 2002). Regardless of reasons that influence the decision to seek care, it appears that Goldberg & Huxley's seminal model of the pathway to psychiatric care (Reference Goldberg and HuxleyGoldberg & Huxley, 1980) remains pertinent: it is only a fraction of individuals with common mental disorders who seek help, a smaller fraction have their disorder recognised by their physician, and a yet smaller fraction receive appropriate care.
It is notable that the majority of individuals using a psychotropic medication do not reach the threshold for common mental disorder. Similar results have recently been reported in a Canadian study (Reference Patten, Williams and WangPatten et al, 2005). Without data describing the course of their illness, it is unclear whether these are patients whose symptoms have recently subsided, patients who are on successful maintenance therapy, or patients who are being treated more aggressively than may be necessary. Our results, however, showing a strong association between severity of symptoms and likelihood of treatment with psychotropic medication suggest that individuals who do not meet the threshold for common mental disorder but are using psychotropic medications are probably experiencing sub-threshold symptoms and their treatment may be appropriate.
Individual use of antidepressants, anxiolytics and hypnotics over time
Presenting data from 1977 to 1999 gives a unique perspective on individuals' use of psychotropic medications over time. Psychotropic medication use at any time was strongly predictive of future use, even 22 years later. In addition, as retrospective studies have suggested (Reference Blumenthal and EndicottBlumenthal & Endicott, 1996; Reference Burns, Eichenberger and EichBurns et al, 2003), previous use of psychotropic medication is a strong predictor of whether individuals would seek pharmaceutical treatment during a future episode of mental disorder. It was notable, however, that this association became weaker as the cohort aged. Not using a treatment during an episode of mental disorder that had been previously employed may indicate a treatment failure in the past. Individuals may be requesting non-pharmaceutical treatments such as cognitive-behavioural therapy, or simply not seeking treatment at all.
Limitations and strengths of the study
One limitation of our study is that we do not have information on non-pharmaceutical treatment of mental disorder among the survey members. The fact that approximately 40-50% of individuals in our investigation who had a common mental disorder and saw a physician for ‘nerves’ in the past year were not taking psychotropic medication suggests that some might have been treated with psychotherapy or other non-pharmacological approaches. Results from a British study show that psychotherapeutic treatment is almost as common as treatment with psychotropic medication among individuals with a neurotic mental disorder who consulted a primary care physician in the previous year (Reference Bebbington, Brugha and MeltzerBebbington et al, 2003), and similar results have been reported in the USA (Reference Olfson, Marcus and DrussOlfson et al, 2002). There is evidence to support some psychotherapeutic approaches, such as cognitive-behavioural therapy, as an alternative or adjunct to pharmacotherapy for depression (DeRubeis et al, Reference DeRubeis, Gelfand and Tang1999, Reference DeRubeis, Hollon and Amsterdam2005), so it is possible that the proportion of individuals who are receiving appropriate treatment for their mental disorder is higher than the proportions using psychotropic medication reported here. In addition, it is worth noting that the majority of cases of depression remit without any form of psychiatric treatment (Reference Wells, Burnam and RogersWells et al, 1992).
Another limitation of this study is that we do not measure distinct DSM disorders separately. Given the comorbidity between many DSM mental disorders (Reference Kessler, McGonagle and ZhaoKessler et al, 1994), we do not expect this to affect our results significantly. Evidence suggests, for example, that mixed and/or comorbid anxiety and depression are more common than either disorder alone (Reference Singleton, Bumpstead and O'BrienSingleton et al, 2003), symptoms of anxiety are frequently successfully treated with selective serotonin reuptake inhibitor antidepressants (Reference Kapczinski, Lima and SouzaKapczinski et al, 2003) and individuals with numerous anxiety and depressive disorders have increased use of antidepressants, anxiolytics and hypnotics (Reference Bebbington, Brugha and MeltzerBebbington et al, 2003; Reference Ohayon and LaderOhayon & Lader, 2002). Furthermore, all classes of psychotropic medications (antidepressants, anxiolytics and hypnotics) in our study were significantly associated with our measure of common mental disorder (further information available from the authors upon request).
A final limitation is that we did not know the stage of illness of the participants with mental disorder. It is possible that individuals who had not sought treatment were at an early phase of their mental illness and would have sought treatment as the illness continued. All comparable studies in this area face this limitation, the only solution being an intensive prospective study of the onset of illness and whether individuals subsequently seek treatment.
The study design of the NSHD also offers some notable methodological strengths. This survey has a large sample that is population-based, with all data being prospectively collected over a 53-year period. This has allowed us to present data on population trends of antidepressant, anxiolytic and hypnotic use, associations between antidepressant, anxiolytic and hypnotic use and common mental disorder, and trends in individual use of these medications over time. These results confirm that although psychotropic medication use is rising, the majority of individuals with an identifiable common mental disorder are not being treated with drugs.
Acknowledgements
The authors are grateful for funding from the Institute for Social Studies in Medical Care (I.C.), the UK Medical Research Council (M.E.J.W., T.J.C., P.B.J.) and the Stanley Medical Research Institute (P.B.J.).








eLetters
No eLetters have been published for this article.