Background
Emergency physicians who work in academic settings enjoy an expanding number of roles beyond that of the skilled clinician.Reference Frank 1 The traditional “clinician-educator” role,Reference Jouriles, Kuhn and Moorhead 2 , Reference Jones and Gold 3 both in the classroom and in clinical settings, is still a significant component of an academic physician’s careerReference Coates, Hobgood and Birnbaum 4 - Reference McLaughlin 6 . However, many administrative, research, scholarly, and advocacy-related roles are increasingly identified as important—if not mandatory—facets to an academic position in emergency medicine.
Yet few opportunities exist during medical training to formally develop these academic and professional skills;Reference Jouriles, Kuhn and Moorhead 2 , Reference McLeod and Steinert 7 instead, clinicians pick up skills “on the job” or seek post-residency training specific to their needs. Aside from formal certificate and degree programs, faculty development (FD) is the primary means of expanding beyond existing skill-sets. FD encompasses “the broad range of activities that institutions use to renew or assist faculty members in their multiple roles.” 8
Early forms of FD were offered at an institutional level and tied closely with promotion and tenure.Reference Jouriles, Kuhn and Moorhead 2 , Reference Beasley, Wright and Cofrancesco 9 , Reference Clark, Houston and Kolodner 10 More recently, the paradigm of FD has shifted; individual medical faculties are now offering FD curricula, the content and format of which is being informed by the faculty members themselves through focus groups and surveys.Reference Coates, Hobgood and Birnbaum 4 , Reference Steinert, Mann and Centeno 5 , Reference Baldwin, Levine and McCormick 11 - Reference Huwendiek, Mennin and Dern 23 These needs assessments are useful in identifying the specific gaps in knowledge or training that FD can address.Reference Adkoli, Al-Umran and Al-Sheikh 24 , Reference Holmboe, Ward and Reznick 25
Across the country, several medical faculties have conducted single-center needs assessment surveys, 18 - Reference Miedzinski, Davis and Al-Shurafa 20 though no comprehensive and uniform assessment has yet been completed in Canada. In contrast, a multi-centre European studyReference Huwendiek, Mennin and Dern 23 of medical educators, and multi-centre AustralianReference Dent, Weiland and Paltridge 26 and AmericanReference Farley, Casaletto and Ankel 16 studies of emergency medicine faculty, have been reported. These latter studies are also the only published multi-centre surveys of a FD needs assessment in emergency medicine and highlight a significant mismatch between the FD needs of and resources available to emergency medicine faculty.
However, none of these studies comprehensively evaluates the broader FD required to support the increasingly diverse needs of academic emergency physicians (AEPs), instead limiting research to medical education or topics of continuing professional development (CPD), i.e., clinical acumen. Similarly, the studies provide little insight into the FD needs of important segments of the EM community, such as senior faculty and female AEPs. Moreover, as country-specific differences exist both in the medical education systems and the practice of emergency medicine, identifying the Canadian perspective is important in providing the most relevant FD experience.Reference Jouriles, Kuhn and Moorhead 2 , Reference Steinert, Macdonald and Boillat 14
The goal of the current study was to address the hypotheses that AEPs’ interest in FD is expanding from the traditional focus of medical education to satisfy increasingly diverse academic needs; senior faculty have a continued interest in FD; female AEPs may have different FD interests than their male counterparts; and delivery of FD has to be at convenient times and locations. It provides the first nationally-representative, FD needs assessment of Canadian AEPs.
Methods
We conducted a multi-centre, cross-sectional survey of the current FD needs and interests of Canadian AEPs in order to: 1) determine their current FD activities, 2) provide a detailed understanding of their FD needs and interests, 3) elucidate the perceived barriers to and motivation for engaging in FD, and 4) identify preferred methods of delivery for FD activities.
Study population
The study surveyed AEPs affiliated with eight centres across Canada: The University of British Columbia, The University of Alberta, The University of Calgary, McGill University, The University of Toronto, McMaster University, Queen’s University, and Dalhousie University. Eligibility required practice within a university-affiliated faculty, as an emergency medicine physician, having emergency medicine (CCFP and FRCP), pediatric emergency medicine (FRCP), or equivalent training, or certification as a pediatrician (FRCP) with emergency medicine sub-specialization.
Survey instrument and development
Survey development was conducted as an iterative process, 27 - Reference Lockyer 29 using feedback from FD leaders and collaborating researchers, with a draft instrument piloted amongst members of the Education Committee of the Department of Emergency Medicine at the University of Calgary. Survey questions were extracted from previous FD surveysReference Clark, Houston and Kolodner 10 , Reference Farley, Casaletto and Ankel 16 , 18 , Reference Egan-Lee, Harvey and Silver 19 , Reference Lockyer 29 and evaluated by collaborating experts. The final instrument was then pilot tested in Calgary prior to national release during December 2011–June 2012.
The five academic areas of interests were also obtained through an iterative process of faculty consultation and literature review, with the final topics refined in the pilot phase of the study. Education, leadership (encompassing both “administrative” and “professional” roles) and research were included as the traditional categories of FD. Scholarship was added to elucidate the broader role of academic communication, beyond the publishing of scientific journal articles, and including the ethical, social, and business aspects of medical practice. Social accountability, as it is used here, refers to the obligation of physicians to direct their educational, research, and service activities towards addressing the health concerns of the community, region, and/or nation they have a mandate to serve.Reference Boelen and Heck 34 Although elements of scholarship and social accountability were included in previous surveys under traditional category headings,Reference Farley, Casaletto and Ankel 16 , 18 - Reference Miedzinski, Davis and Al-Shurafa 20 , Reference Huwendiek, Mennin and Dern 23 , Reference Dent, Weiland and Paltridge 26 with increasing recognition that these are significant facets of an AEP’s career,Reference McLeod and Steinert 7 , Reference Steinert 13 , Reference Sánchez-Mendiola, Graue-Wiechers and Ruiz-Pérez 21 these latter two categories were added and expanded to allow for a more comprehensive evaluation.
An online survey instrument, consisting of a series of multiple-response or Likert-scale questions, was implemented through Surveymonkey.com.Reference Streiner and Norman 30 , Reference Iraossi 31 Multiple-selection questions permitted up to five responses. Questions using a 5-point Likert scale employed descriptive anchors for each point on the scale.Reference Mann 32 , Reference Meric and Wagner 33 Demographic information was collected using drop-down boxes. Each section also contained a free-form response for additional comments or selections. The survey required 10-15 minutes to complete and was anonymous; names were optionally collected on the consent page to aid with survey administration.
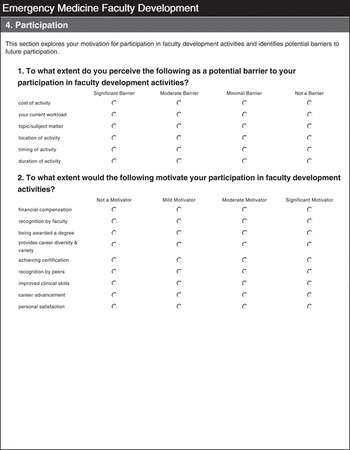
The survey (included in an online appendix) was formatted in five parts: 1) a brief appraisal of current participation in the areas of leadership, research, social accountability, scholarship, and education; 2) an in-depth assessment of interests/needs for future FD activities in these same areas; 3) a trio of questions to explore i) motivation for, ii) barriers to, and iii) methods for encouraging participation in FD activities; 4) a section on the logistics of FD delivery to delineate the optimal timing, location, and format of FD activities; and 5) a final section to capture limited demographic information (department, years of practice, gender, certifying body) for pre-specified sub-group analyses.
Survey administration
Eligible faculty within each of the academic centres were approached using a modified Dillman technique.Reference Jenkins and Dillman 35 Subjects were initially recruited using email, where they were informed of the upcoming study and encouraged to enroll. In subsequent email contacts, links were provided to a video requesting participation in the research and to the survey itself. Ethics approval for the study was obtained through the University of Calgary’s Conjoint Health Research Ethics Board (CHREB Study #23862).
Data collection and analysis
Responses were automatically collected/collated as the survey progressed, and are reported here as pooled data. Descriptive statistics are used to calculate rates and averages. Multiple-selection questions are reported as the percentage of respondents selecting a particular response (frequency; range 0-100%). Questions using a 5-point Likert scale are reported as both mean and median values between 1 and 5. Pre-planned comparisons were made between demographic subgroups, using the Mann-Whitney U test with a significance level of p=0.05; these include female and male subgroups, cohorts 0-5 years and 20+ years into their careers, CCFP and FRCP training, and Canadian and US emergency medicine population demographics. 36 - Reference Watts, Promes and Hockberger 38
Results
Demographics
Nationally, 944 AEPs were surveyed, with 336 respondents completing the entire survey (response rate of 36%). As summarized in Table 1, the majority of participants were FRCP-certified, EM-specialized males within the first 15 years of practice. Of female respondents, over two-thirds were within the first 10 years of their careers. For comparison with the Canadian and American emergency medicine populations, demographics are provided from national surveys of the respective physician bodies. 36 - Reference Watts, Promes and Hockberger 38
Table 1 Respondent demographics and comparison with Canadian 36 and AmericanReference Kristal, Randall-Kristal and Thompson 37 , Reference Watts, Promes and Hockberger 38 EM physician populations: data from the National Physician Survey (NPS) and Society for Academic Emergency Physicians (SAEM)

* Comparison between the sample and the target Canadian population.
† N=1,209 for SAEM Years of Practice (based on 2004–5 survey).
Current activities
The current non-clinical activities of AEPs are reported in Table 2, broken down by academic area. Most AEPs participated in bedside teaching, the teaching of small groups, and in rounds presentations, with nearly universal participation in the supervision of medical trainees. Formal lecturing and educational leadership activities, such as curriculum or simulation development, were substantially less common. Scholarly participation showed high overall participation (76.5%); the most popular individual activities included participating in journal clubs, presenting at conferences, and guest lecturing. Overall participation in leadership activities was also high (81.0%), although this result was driven primarily through committee work (66% participation); no other activity in this category had more than 27% participation. Only half of respondents reported participation in research (50.9%) or activities related to social accountability (49.7%), with less than a third engaging in any one particular activity.
Table 2 Current participation by AEPs in non-clinical academic activities

Participation is rank ordered within each academic domain and reported as a percentage. Overall participation, defined as the total percentage of respondents selecting one or more of the listed activities in each domain, is also reported.
The major differences in the current non-clinical participation by demographic subgroups are illustrated in Figure 1. Despite their paucity of clinical experience, junior faculty participated more in educational activities (mean participation in 3.52 vs 2.76 activities, p<0.002) compared with senior faculty having 20+ years of experience. In contrast, junior faculty were significantly less active in leadership activities than their senior counterparts (1.05 vs 2.13, p<0.001). Whether this trend is the result of being closer to the educational experience at the start of a career or because entry into other academic areas requires more experience is unclear. A similar dearth of female AEPs in leadership positions was evident, compared with their male counterparts (1.35 vs 1.93, p=0.025). Aside from the 0-5 year cohort, where both males and females were underrepresented compared to senior faculty, this was independent of seniority (female 1.57 vs male 2.16 activities, p=0.015). As a cohort, CCFP-trained AEPs were less likely to be involved in all non-clinical academic domains than FRCP-trained AEPs (average difference 0.77 activities; all p<0.012), a gap most pronounced in educational (2.78 vs 3.84, p<0.001) and scholarship (1.25 vs 2.58, p<0.001) domains.

Figure 1 Comparison of current participation in non-clinical activities (mean) by different subgroups of AEPs in the areas of scholarship, leadership and education. Under leadership, subgroups of those with six or more years of experience are included, revealing statistically different participation between males and females.
Interest in future FD
The need for, and interest in, FD was determined by asking AEPs which future activities they would be willing to attend (from a list of 14 possible choices). Table 3 outlines the results for each of the five non-clinical domains. Canadian AEPs continued to have a significant interest in improving their educational skill-set, with 87% of respondents willing to participate in at least one of the suggested FD activities. Perhaps owing to the changing technological nature of education, senior faculty reported greater need to develop computer skills (26.9% vs 4.8%, p<0.001) and improve their use of technology in the classroom (23.9% vs 4.8%, p<0.001). However, senior faculty reported that they were much less in need of skills to help the “resident in difficulty” (16.4% vs 42.9%, p<0.001).
Table 3 The needs and interests of Canadian AEPs

The percentage of respondents indicating they would attend each of the 14 proposed FD activities in each non-clinical, academic domain, listed in rank order of most interest to least interest.
In contrast, the areas of research and social accountability continued to see lower levels of interest compared to the domains of education, leadership, and scholarship. Moreover, the interest in research was skewed towards the interpretation of research and its application to clinical or educational settings, rather than in conducting the research itself. In the area of social accountability, AEPs preferred to deliver health care to marginalized populations, particularly in an international setting, more than developing policy development, advisory, or advocacy skill sets.
Though variations in current practice existed between junior versus senior, and CCFP-trained versus FRCP-trained AEPs (as mentioned above), there were few differences in their FD interests—all subgroups had consistently high (≥79%) overall interest. Of the subgroups, the only statistically significant differences were greater interest shown by females than males in pursuing educational (2.19 vs 1.87, p=0.016), leadership (1.82 vs 1.44, p<0.01), and research activities (1.32 vs 0.99, p=0.01). In leadership, this gender difference was independent of seniority: although female respondents to our survey were generally more junior than their male counterparts, female AEPs showed statistically greater interest in leadership activities, even when compared to males in the 0-5 year cohort (1.82 vs 1.50 activities, p=0.037). This is illustrated in Figure 2.

Figure 2 Comparison of the overall FD needs and interests of female versus male AEPs in the areas of leadership, education and research; bottom axis represents the average (mean) number of activities interested in. No significant difference was found between females and males in the first five years of practice in education or research.
Motivation for and barriers to FD
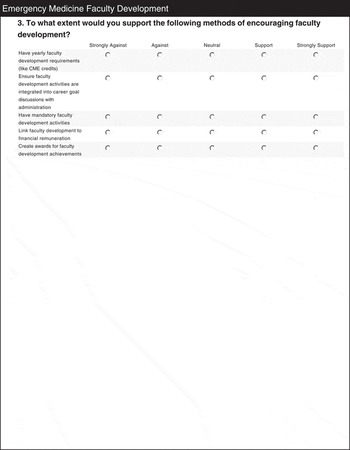
In addition to delineating the specific topics AEPs are most interested in, the survey explored which factors inhibit and promote participation in FD activities (Table 4).
Table 4 Factors that motivate or are barriers to FD participation

Mean and median Likert values on a 5-point scale are reported: for question A, topics are considered 1 = very unimportant and 5 = very important; for question B, 1 = strongly disagree and 5 = strongly agree with the statement; for question C, 1 = strongly oppose and 5 = strongly support the listed methods.
Delivery of FD activities
The preferred timing, location, and format of future FD activities is summarized in Table 5. Table 5A presents a rank-ordered list of the preferred FD activity formats. Table 5B lists the percentage of respondents who would attend an activity in a given location. Table 5C highlights that AEPs favoured activities of moderate duration, with two-thirds of respondents desiring activities between two hours to half a day in duration. Lastly, Table 5D reveals that normal business hours were the preferred time for FD activities, and that minimal support was found for weekend activities.
Table 5 Summary of the preferences of AEPs for the format and delivery of future FD activities

Willingness to participate was scored on a balanced, 5-point Likert scale, where 1 = very unwilling and 5 = very willing. Other responses are the percentage of participants willing to participate/attend for each activity format, location, or time.
Regional/institutional variation
In this multi-centre study, regional and institutional variability was found, though in most instances the heterogeneity was minor/statistically insignificant. The major outliers are detailed below: in research, need was highest in the Eastern and lowest in the Western institutions (University of Calgary, University of British Columbia, University of Alberta), based both on the average number of topics each respondent was interested in (0.95 topics vs 1.15) and the overall desire to participate in research-related FD (52.7% vs 69.2%). This did not correlate with demographic trends. In the area of social accountability, interest in future faculty development was weakest in McGill and Queen’s Universities, where AEPs were interested in 0.61 topics (vs 1.25 topics for the remaining sites) and had an overall interest of 37.0% (vs 69.2%). This difference correlated with seniority (the respondents in both schools had a higher rate of participation from senior faculty when compared to other schools), and was supported by the subgroup analysis showing junior AEPs had greater need for FD in this area than senior faculty. Institutional differences were found in leadership-oriented FD activities, with Queen’s and the University of Toronto expressing the greatest overall interest (1.95 activities, 86.7% interest) and Dalhousie and the University of Calgary showing the least overall interest (mean of 1.46 activities, 73.0% interest), though these were not correlated with any demographic differences. In contrast, interest in scholarly FD activities was quite uniform across the country, although Queen’s University exhibited much lower interest than other centres (1.35 vs 1.53 activities and 65.0% vs 81.1% overall interest).
Discussion
This survey of Canadian academic emergency physicians, with a 36% response rate significantly weighted towards faculty with under 15 years of experience, and with a higher proportion of female respondents when compared to current demographics, suggests that traditional domains of education, leadership, and scholarship remain strong, but there is a growing need for FD in research and social accountability. Furthermore, as in previous studies,Reference Coates, Hobgood and Birnbaum 4 - Reference McLaughlin 6 , Reference Farley, Casaletto and Ankel 16 our results show that medical education was the core of an AEP’s non-clinical duties in the population sampled, with respondents reporting over 98% participation in this activity. AEPs expressed a need for better individual and bedside teaching skills, including teaching around cases and providing effective feedback. This differs from a European study of medical educators,Reference Huwendiek, Mennin and Dern 23 which found greater interest in curriculum development and evaluation, learning research methodologies in medical education, and the use of computer-based training. This difference in focus likely reflects that most Canadian AEPs are clinicians who regularly interact with medical trainees, as compared to the aforementioned study, with a surveyed population heavily weighted towards academics.
At the same time, our results are also congruent with the recognized need for FD support of academic roles beyond the “clinician-educator.”Reference Steinert, Mann and Centeno 5 , Reference McLeod and Steinert 7 , Reference Steinert 13 The trend in these areas is towards the acquisition of skills translatable between all academic domains, primarily communication and people skills. For example, AEPs’ interests in scholarly activities were centered on improving public speaking and oral presentation skills, rather than writing for journal publication or other print media. For future leadership activities, we found that AEPs preferred to improve their ability to facilitate groups and manage teams, rather than engage in learning more narrow topics, such as financial or strategic planning. The results suggest a desire to participate in a breadth of activities, more than simply the committee work that most AEPs are currently involved with.
In these three traditional domains, our results parallel those in Dent et al.’s surveyReference Dent, Weiland and Paltridge 26 of fellows of the Australian College, with an emphasis on applying teaching acumen in everyday practice, managing conflict, and utilizing research results, more than conducting the research itself. However, much of their paper was oriented strongly towards CPD, whereas our results expand on the FD needs of AEPs outside of the retention/development of clinical skills.
Complementing the interest in the traditional FD domains, our results also suggest a growing need for FD in research and social accountability. This is detailed in Figure 3, where we compare the current overall participation in non-clinical activities with the FD needs in each domain. For example, in this sampling of AEPs, current participation in educational pursuits was 98%, while overall interest in educational FD activities was 87% (roughly 11% less); current participation in research activities was 51%, whereas 63% of AEPs had an interest in future research-related FD (roughly 11% more). A similar difference was found in social accountability (roughly 13% more interest). Unlike other studies, which present a paucity of data in these domains, this work indicates that there is proportionately more interest in research and social accountability than current practice suggests, and hence there is a gap in knowledge or training that FD can address. Table 3 delineates the needs of AEPs in these domains for those administering FD programs. However, the lack of particularly strong interest in any single topic suggests that a multifaceted approach to building FD in these areas may be required.

Figure 3 Current overall participation by AEPs in each of the non-clinical domains (solid bars), compared with the needs and interests for future FD activities in these same areas (white bars), showing relatively less need in the domain of education and relatively increased need in research and social accountability domains (grey bars).
Senior faculty, female AEPs, and CCFP-trained AEPs all have important FD needs
An important finding in this study was that few differences existed between the demographic subgroups analyzed. More specifically, the results suggest that senior AEPs continue to have a need for FD despite their accumulated experience. With the evolution of a career, the FD needs of senior AEPs shift from educational activities towards those in leadership and social accountability. This supplements the information provided by Farley et al.Reference Farley, Casaletto and Ankel 16 about junior emergency medicine physicians.
Similarly, CCFP-trained AEPs participated less in non-clinical activities than their FRCP-trained colleagues. While the trend towards limiting academic emergency medicine positions to FRCP training may obviate this discrepancy, our results show that the FD interests of CCFP-AEPs were the same as those for FRCP-AEPs. As currently one-third of Canadian AEPs are CCFP-trained, this represents an under-utilized resource for academic programs. Furthermore, though some CCFP-AEPs working in academic centers may not wish to participate in non-clinical work, the results of our survey suggest otherwise.
In contrast, female AEPs expressed greater need for FD to develop their leadership skill-set. Farley et al.Reference Farley, Casaletto and Ankel 16 suggested gender differences exist by providing three FD topics of particular interest to female emergency physicians at the start of their careers. Our results show that this is a trend across the academic domains of leadership, education and research. However, as shown in Figure 3, these trends are statistically significant only for FD in leadership; in research and education this increase is accounted for by a greater proportion of junior faculty amongst the female cohort. A likely contributor to the increased desire for FD in leadership is the reported underrepresentation of women in leadership activities/positions (Figure 1).
FD activities need to be relevant and convenient
In the past, the need for FD was frequently underestimated by clinicians, and the benefits of FD equally unrecognized.Reference Jouriles, Kuhn and Moorhead 2 , Reference Skeff, Stratos and Mygdal 39 However, this study illustrates that AEPs find value in FD participation. AEPs were motivated to participate in FD activities because it was personally satisfying, provided career diversity, and enhanced both teaching and leadership skills. Unlike Huwendiek et al.’s study,Reference Dent, Weiland and Paltridge 26 which suggested that a lack of academic recognition is a barrier to FD participation, Canadian AEPs were ambivalent about peer or faculty recognition for FD participation. Moreover, AEPs opposed making FD activities mandatory (Likert response: 2/5).
In contrast, the importance of delineating the content of future FD activities is well understood: AEPs rated subject matter as the most important factor when considering whether or not to participate in FD (Likert response: 5/5). Convenience was also of great importance. Most AEPs preferred to attend FD activities on weekdays, particularly during “business hours.” This is intuitive, when AEPs have a preponderance of evening shifts. More than two-thirds of those surveyed preferred activities between two hours and half a day in duration, with only 15% seeking activities an hour or less in duration, suggesting that traditional lunchtime rounds may not be as effective for AEPs compared to, for example, an afternoon workshop (though both formats are supported). Additionally, AEPs wanted activities to occur in the hospital where they work (97%) rather than farther afield.
Limitations
This study is a cross-sectional survey and has several limitations inherent to this design. It also represents the opinions of AEPs during the period of October 2011–June 2012 (including the Calgary pilot), and may no longer be a valid representation of their current FD needs and interests. However, given that most of the respondents are likely still in practice and that similar results regarding FD needs/interests have been reported in the literature,Reference Farley, Casaletto and Ankel 16 , Reference Amin, Eng and Seng 17 , Reference Dent, Weiland and Paltridge 26 our results are likely still very relevant. Moreover, the demographics of our respondents make it unlikely that this interval will change the relevance of our results. Most respondents are EM-specific, FRCPC-trained AEPs, and academic centers are increasingly recruiting AEPs with these credentials. More than two-thirds of the respondents were in the first 15 years of their careers, and only respondents from two centers (McGill and Queens) had significant participation from senior faculty. This suggests a participation bias towards those early in their careers, where perhaps the need for faculty development is greater. There was a disproportionately higher response from female AEPs, compared to the demographics of the target population. This may reflect a gender bias towards an interest in faculty development; however, our sub-group analyses show that females generally had the same FD interests as males, and the results highlight the specific gender differences that are likely to be more relevant now than at study initiation.
One area that was not broadly addressed in this survey, and has since become popular, involves the use of social media. The rapidity with which sessions on podcasting, tweeting, and providing online content fill up suggest that this is a new need that FD can address, and that it should be further investigated.
Across the eight centres surveyed, both regional and institutional heterogeneity was evident, which may reflect local culture/practices or be evidence of selection bias. However, this typically did not correlate with demographic differences between faculties, nor was there consistency in the institutional heterogeneity (i.e., no one centre had more or less need across all the academic domains).
The survey was administered in an online format only; this provided rapid, cost-effective dissemination, but may have obviated participation by those of low computer literacy, which is more likely to bias the responses towards those of junior faculty.
In addition, the survey was administered to over 950 AEPs nationally, of which 36% responded, meaning that the results may be affected by sampling bias and not represent FD interests across the country. This may reflect an under-appreciation of FD by senior faculty, whose participation was lowest (those with 20+ years seniority had a 16% response rate, compared with the most junior faculty, who had a 67% response rate) or simply greater survey burnout. Moreover, when interpreting this low response rate, it may be argued that respondents to a FD survey were more likely to have an interest in FD participation. Hence, these results are more likely to be reflective of the needs and interests of future participants and less biased by the views of those with no intention to participate. Lastly, though low, the response rate (RR) is comparable to other multi-centre studies. Farley et al.Reference Farley, Casaletto and Ankel 16 surveyed approximately the same number of people (roughly 950), with a 25% RR (vs our 36% RR). Dent et al.Reference Dent, Weiland and Paltridge 26 had a 58% RR, although this was the Australian College’s sponsored survey of its members, its survey was far shorter than ours, and financial incentives were provided for completing the study, all of which may account for the higher RR. Huwendiek et al.’s studyReference Huwendiek, Mennin and Dern 23 of European medical educators had a purview much broader than ours (both in terms of multidisciplinary medical faculty and dozens of countries included), and thus it had a higher overall number of respondents, yet its RR was far lower than ours (4.8%).
Conclusions
This study is the first comprehensive national FD needs assessment in a sample of Canadian academic emergency physicians. It demonstrates that in addition to their clinical work, AEPs who responded to the survey were engaged in educational activities, and this suggests the greatest FD needs remain in the educational domain. However, our results highlight that AEPs who responded to the survey were increasingly interested in developing their other, non-clinical skill-sets, particularly for activities in research and social accountability. Moreover, this study details these FD interests across a broad range of academic pursuits and provides insight as to where FD resource allocation and programming efforts should be focused.
Competing Interests: The corresponding author (Lang) has a position as chair of the RCPSC Scholars Subcommittee for CanMEDs 2015 as a potential conflict of interest; no authors have financial interests relating to this manuscript.
APPENDIX