Clozapine is now well recognised as being more effective than conventional neuroleptics in reducing symptoms of patients with treatment-resistant schizophrenia (Reference Wahlbeck, Cheine and EssalWahlbeck et al, 1999). There are several reports indicating that the treatment costs for prescribing clozapine are more than offset by the saving in hospital admissions (Reference Honigfeld and PatinHonigfeld & Patin, 1990; Reference Hirsch and PurinHirsch & Purin, 1993; Reference Meltzer, Cola and WayMeltzer et al, 1993). This report is of the outcome, in terms of Clinical Global Impression scale (CGI; Reference GuyGuy, 1976), level of functioning and use of hospital resources for a group of 31 patients started on clozapine in Dorset Healthcare NHS Trust. Many previous papers report the outcome of clozapine use in the context of either randomised-controlled trials or within specialist centres. This paper focuses on the outcome for patients started on the drug in a local clinical service.
The study
Subjects
The first 31 patients with treatment-resistant schizophrenia to be treated with clozapine in the Dorset Healthcare NHS Trust are the subjects of this study. Demographic and clinical details of the patients are given in Table 1. All patients treated with clozapine were diagnosed as suffering from schizophrenia using the DSM-III-R (American Psychiatric Association, 1987) criteria. The patients had been resistant to at least two neuroleptics from different classes for at least six months for each agent in all cases.
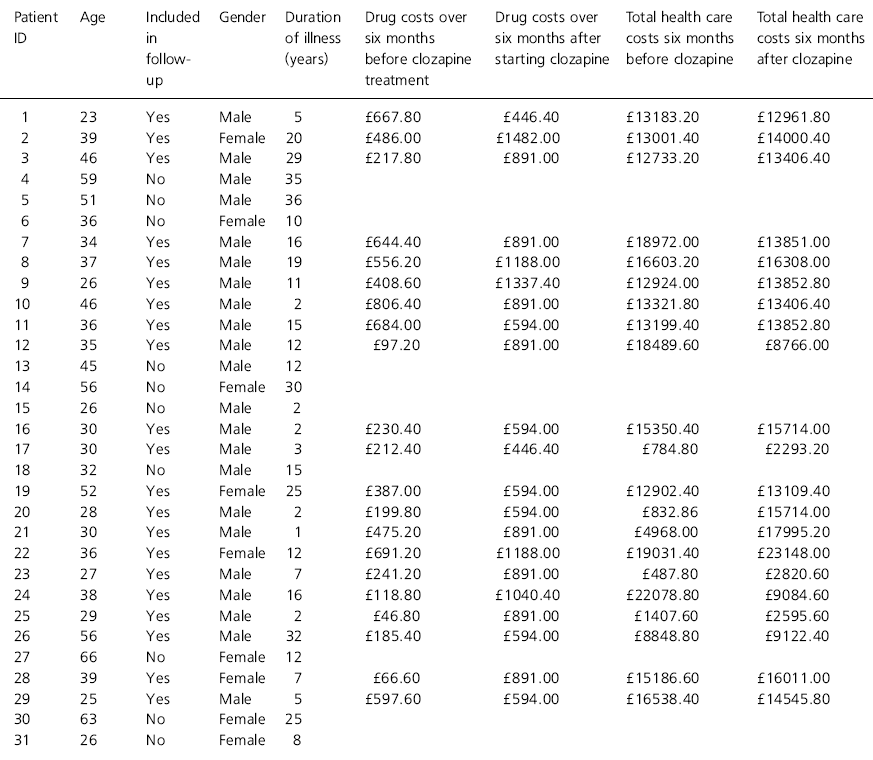
Table 1. Drug costs and total health care costs before and after starting clozapine
| Patient ID | Age | Included in follow-up | Gender | Duration of illness (years) | Drug costs over six months before clozapine treatment | Drug costs over six months after starting clozapine | Total health care costs six months before clozapine | Total health care costs six months after clozapine |
|---|---|---|---|---|---|---|---|---|
| 1 | 23 | Yes | Male | 5 | £667.80 | £446.40 | £13183.20 | £12961.80 |
| 2 | 39 | Yes | Female | 20 | £486.00 | £1482.00 | £13001.40 | £14000.40 |
| 3 | 46 | Yes | Male | 29 | £217.80 | £891.00 | £12733.20 | £13406.40 |
| 4 | 59 | No | Male | 35 | ||||
| 5 | 51 | No | Male | 36 | ||||
| 6 | 36 | No | Female | 10 | ||||
| 7 | 34 | Yes | Male | 16 | £644.40 | £891.00 | £18972.00 | £13851.00 |
| 8 | 37 | Yes | Male | 19 | £556.20 | £1188.00 | £16603.20 | £16308.00 |
| 9 | 26 | Yes | Male | 11 | £408.60 | £1337.40 | £12924.00 | £13852.80 |
| 10 | 46 | Yes | Male | 2 | £806.40 | £891.00 | £13321.80 | £13406.40 |
| 11 | 36 | Yes | Male | 15 | £684.00 | £594.00 | £13199.40 | £13852.80 |
| 12 | 35 | Yes | Male | 12 | £97.20 | £891.00 | £18489.60 | £8766.00 |
| 13 | 45 | No | Male | 12 | ||||
| 14 | 56 | No | Female | 30 | ||||
| 15 | 26 | No | Male | 2 | ||||
| 16 | 30 | Yes | Male | 2 | £230.40 | £594.00 | £15350.40 | £15714.00 |
| 17 | 30 | Yes | Male | 3 | £212.40 | £446.40 | £784.80 | £2293.20 |
| 18 | 32 | No | Male | 15 | ||||
| 19 | 52 | Yes | Female | 25 | £387.00 | £594.00 | £12902.40 | £13109.40 |
| 20 | 28 | Yes | Male | 2 | £199.80 | £594.00 | £832.86 | £15714.00 |
| 21 | 30 | Yes | Male | 1 | £475.20 | £891.00 | £4968.00 | £17995.20 |
| 22 | 36 | Yes | Female | 12 | £691.20 | £1188.00 | £19031.40 | £23148.00 |
| 23 | 27 | Yes | Male | 7 | £241.20 | £891.00 | £487.80 | £2820.60 |
| 24 | 38 | Yes | Male | 16 | £118.80 | £1040.40 | £22078.80 | £9084.60 |
| 25 | 29 | Yes | Male | 2 | £46.80 | £891.00 | £1407.60 | £2595.60 |
| 26 | 56 | Yes | Male | 32 | £185.40 | £594.00 | £8848.80 | £9122.40 |
| 27 | 66 | No | Female | 12 | ||||
| 28 | 39 | Yes | Female | 7 | £66.60 | £891.00 | £15186.60 | £16011.00 |
| 29 | 25 | Yes | Male | 5 | £597.60 | £594.00 | £16538.40 | £14545.80 |
| 30 | 63 | No | Female | 25 | ||||
| 31 | 26 | No | Female | 8 |
Outcome measures
Regular clinical assessments were performed using objective and subjective measures. The psychiatric assessments used were a seven-point CGI scale ranging from very much better to very much worse, and the Basic Everyday Living Skills (BELS) scale. The BELS scale is designed to assess the basic living skills of people who suffer from long-term mental illness (further details available from the author upon request). The scale measures change in the performance of daily living skills, while at the same time taking in to account changes in the patient's residential circumstances. The scale consists of 26 items which are divided into four categories: selfcare, domestic skills, community skills and activity and social relations. Each item is divided into two parts; the first rates the degree of opportunity for that function, and the second rates the actual performance for that function.
The 21 patients who completed at least a six-month course of clozapine treatment were followed up in terms of their bed use over the next four years.
Findings
Thirty-one patients were started on clozapine. Ten patients did not complete a six-month course of clozapine. The reasons for discontinuation were: haematological monitoring decision (n=3); patient consent withdrawn (n=2); unable to obtain blood sample (n=1); moved to another hospital (n=1); poor clinical response (n=1); poor adherence (n=1); patient died of myocardial infarction (n=1). For those patients who completed at least a six-month course of clozapine the dose range was 150-300 mg achieved between three and 25 weeks. All previous psychotropic medication was stopped during the introduction of clozapine, at six months, the 21 patients followed up were on clozapine alone.
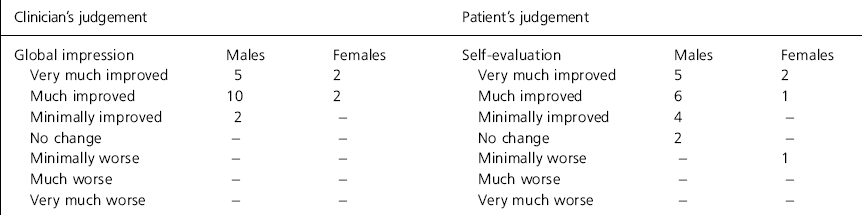
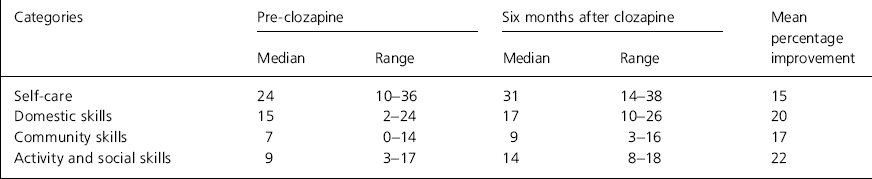
For those patients who completed a six-month course of clozapine the outcome at six months in terms of CGI and BELS scores are shown in Tables 2a and 2b. All patients improved according to the clinician's judgement, 18 out of 21 improved according to patient judgement. An improvement of between 15% and 22% was found on the four BELS scores.
Table 2a. Six monthly outcome measures for the Clinical Global Impression scale
| Clinician's judgement | Patient's judgement | ||||
|---|---|---|---|---|---|
| Global impression | Males | Females | Self-evaluation | Males | Females |
| Very much improved | 5 | 2 | Very much improved | 5 | 2 |
| Much improved | 10 | 2 | Much improved | 6 | 1 |
| Minimally improved | 2 | - | Minimally improved | 4 | - |
| No change | - | - | No change | 2 | - |
| Minimally worse | - | - | Minimally worse | - | 1 |
| Much worse | - | - | Much worse | - | - |
| Very much worse | - | - | Very much worse | - | - |
Table 2b. Six monthly outcome measures for the Basic Everyday Living Skills scale
| Categories | Pre-clozapine | Six months after clozapine | Mean percentage improvement | ||
|---|---|---|---|---|---|
| Median | Range | Median | Range | ||
| Self-care | 24 | 10-36 | 31 | 14-38 | 15 |
| Domestic skills | 15 | 2-24 | 17 | 10-26 | 20 |
| Community skills | 7 | 0-14 | 9 | 3-16 | 17 |
| Activity and social skills | 9 | 3-17 | 14 | 8-18 | 22 |
The drug costs and total health care costs (1994 prices) for each patient who completed a course of clozapine are shown in Table 1 for the six months before and the six months after the drug was started.
The mean total drug cost in the six months before starting clozapine was £382. The mean total drug cost in the six months after starting clozapine was £849. Mean total health care costs (including in-patient and community support) was £11 945 over six months prior to starting clozapine and £12 503 over six months after starting clozapine. Thus, the introduction of clozapine was initially approximately cost neutral.
In the two years prior to clozapine use, the 21 patients had a total of 857 in-patient days in acute wards and 2919 in-patient days in the rehabilitation unit. In the first and second years of clozapine treatment, the figures were 245 in-patient days (acute ward) and 4022 in-patient days (rehabilitation unit). In the third and fourth years post-clozapine treatment, the figures were no in-patient days (acute ward) and 563 in-patient days (rehabilitation unit).
Comment
It is important to note that 10 out of 31 patients did not stay on the drug and hence did not have the opportunity to benefit from it. This is a sizeable proportion of the group. It is important in the planning of services to recognise that even with clozapine, there will be a significant number of patients, who will not or do not wish to take the drug. However, three of the 10 who discontinued treatment before six months were successfully restarted on the drug at a later stage. Thus, initial failure does not preclude eventual success.
The second point to note is that at the six month evaluation, there was an improvement across the range of activities of daily living and most of the patients were either much improved or very much improved according to the CGI rating of the clinician. Interestingly, patients themselves reported their overall improvement as being somewhat less.
The clinician's judgement as to improvement did not lead immediately to discharge from hospital, however. In the first two years following the start of the drug, inpatient use of the acute admission unit and the rehabilitation unit was greater than in the two years prior to starting clozapine. It was only in the third and fourth years of treatment that there was a marked reduction in hospital bed usage. This finding is important. We suggest it reflects the fact that the improvement in symptoms resulting from clozapine use enables the patient to benefit more from active rehabilitation. Thus, there is more incentive both for the patients and staff to actively engage with the patient and start pushing forward a treatment plan. It is only after such rehabilitation that the patient is able to move into the community.
The third point is that the initial introduction of clozapine was in fact cost neutral. Although savings in bed use did not occur until the third and fourth years, the cost of clozapine was offset by a reduction in other drug costs and a reduction in overall health care use. It is important to note that the community resources available for these patients were not markedly different after the introduction of clozapine than before. The rehabilitation services offered initial community support after hospital discharge with eventual transfer to a generic local community mental health team.
Acknowledgements
We would like to thank Professor Julian Leff, Mr Christopher Gooch and Miss Rowena Kendall for permission to use the Basic Everyday Living Skills rating scale. We would also like to thank Sandra Hayward for her help in collecting the data.






eLetters
No eLetters have been published for this article.