It has been known for some time that Black and minority ethnic (BME) groups are overrepresented among psychiatric in-patients in the National Health Service (NHS).Reference Bhui, Stansfeld, Hull, Priebe, Mole and Feder1 The Count Me In census confirmed that this overrepresentation persists and may be becoming more pronounced.Reference Bhui, Stansfeld, McKenzie, Karlsen, Nazroo and Weich2 The census also consistently demonstrated significant variation between BME groups, with most having higher rates of admission but some having lower rates compared with the national average. These differences in admission rates are likely to be explained by three main factors: differences in the incidence and rates of mental disorder; service-related factors, such as pathways into in-patient care; and changes in the size and distribution of the ethnic minority groups in the UK.Reference Bhui, Stansfeld, Hull, Priebe, Mole and Feder1, Reference Boydell, Van Os, McKenzie, Allardyce, Goel and McCreadie3–5
Background
One of the earliest demonstrations of the ethnic density hypothesis was the study of psychiatric admission rates in Chicago by Faris and Dunham.Reference Das-Munshi, Becares, Dewey, Stansfeld and Prince6 Several subsequent studies have supported this idea of a ‘protective’ ethnic density effect, whereby individuals living in areas with a greater proportion of people of the same ethnicity have better health.Reference Duncan and Duncan7–Reference Glover, Arts and Babu10 However, not all studies have consistently found results that support the ethnic density hypothesis.Reference Halpern11 A study at a wider regional scale in England failed to show any effect within individual ethnic groups, although there was some evidence to support differences between ethnic groups.Reference Halpern and Nazroo12
In response, Halpern argued that within-group ethnic density operates at a local level, for example, by reducing levels of ethnic discrimination and increasing levels of social support, and may not be detected when the scale of investigation is at a regional or national level.Reference Karlsen, Nazroo and Stephenson13 Halpern made two predictions about between-group effects that might be evident at a larger scale: (a) smaller ethnic groups will tend to have higher psychiatric admission rates than larger groups, and (b) groups that have a stronger tendency to cluster together will tend to have lower admission rates. We aimed to empirically test these two predictions at a national level in England by linking NHS mental health admission rate data from 2005/06 to UK census ethnic group population estimates, and examining national level mental health admission rates for each BME group according to the population size of each group and the degree of clustering of each group across England.
Method
Rates of admission were calculated for the 16 ethnic groups as used in the UK census, while controlling for age and symptom type.
Population
The population size of each ethnic group was obtained from the ‘Understanding Population Trends and Processes’ section of the Ethnic Group Population Projection (ETHPOP) database. This is a web resource maintained by the University of Leeds, which provides projections of each ethnic group at various levels, including the national level.Reference Keown, Mercer and Scott14
The index of dissimilarity was used as a measure of clustering for each ethnic group.Reference Morgan, Charalambides, Hutchinson and Murray15 This ranges from 0 (indicating full integration) to 100 (indicating full segregation). An index of less than 40 indicates low levels of segregation, while one of 40 or more indicates moderate to high levels of segregation.Reference Parkinson, Champion, Simmie, Turok, Crookston and Katz16 Data were obtained from the Centre on Dynamics of Ethnicity website.Reference Rees, Wohland, Norman and Boden17
Number of admissions and symptom type
Routine clinical data were used. The numbers of in-patient episodes in the NHS (finished consultant episodes) in 2005/06 were obtained for three broad diagnostic groups: schizophreniform (schizophrenia and related disorders), mania (manic episodes) and depression (unipolar and bipolar depressive episodes).
Age at admission
Five age bands were created: 10–19, 20–29, 30–39, 40–49 and 50–59 years. The age range was restricted to 10–59 years for two reasons. First, there are far fewer admissions for these diagnostic groups prior to the teenage years. Second, beyond 60 years of age, the population size of several ethnic groups is so small, even at the national level, that there are too few admissions for the calculation of meaningful rates to be possible.
Rates
Rates of admission were calculated per 100 000 population for each ethnic group. Age standardisation was used to compare the 16 groups by assuming each group had the same population as the European standard.
Relative rates
The average rate of admission for BME groups was compared with the White British group to calculate relative rates for each of the 10-year age bands.
Outlier
One group (other Black) had rates that were consistently outside the spread of the other groups. Subsequent years of the Count Me In census showed that this was the one group that decreased in size as self-recording of ethnicity improved instead of staff recording of ethnicity. An adjustment was made by distributing the excess admissions among four other groups (Black Caribbean, Black African, mixed White and Black Caribbean, and mixed White and Black African).
Results
Rates of admissions
The average (s.d., range) age standardised rates of admission per 100 000 were 139.3 (89.9, 46.7–335.0) for schizophreniform disorders, 30.0 (16.3, 6.6–53.5) for mania and 66.9 (23.9, 21.9–106.6) for depression. There was an eightfold difference in rates of schizophreniform and mania admissions, and a fivefold difference in the rate of depression admissions, between ethnic groups. The rate of admission in the White British group was within the range for all three types of admission, albeit at the lower end of the range for schizophreniform (59.3) and mania admissions (14.3), and the middle of the range for depression (63.7).
Relative rate of admission
In each of the 10 year age bands, the average relative rate of admission for BME groups was higher than that of the White British group for schizophreniform and mania admissions, but not for depression. These differences were most pronounced in younger age bands and tended to decrease with age. The relative rate of admission for mania dropped the most, from 3.5 (1.6–5.4) to 1.7 (1.2–2.3). The relative rate of admission for schizophreniform disorders dropped from 2.9 (2.0–4.0) to 2.3 (1.6–3.1). In depression, the relative rate was 1.5 (0.9–2.2) in those aged 10–19 years and 1.1 (0.8–1.3) in those aged 50–59 years (Fig. 1).

Fig. 1 Average relative rates (with confidence intervals) of admissions for BME groups compared with the White British group. Data are shown separately for schizophreniform (red), mania (blue) and depression (black) admissions. Data are for England 2005/6.
Association of rate of admission with group size and clustering
The mean (s.d.) index of dissimilarity score for the 16 ethnic groups (including White British) was 46% (13) with a range of 27–67%. The average population size for those aged 10–59 years was 2116 k with a range of 65 k to 28 170 k. There was a moderate positive rank correlation between the index of dissimilarity score and rates of admission for schizophreniform disorders, and a weak correlation with rates of admission for mania, and no correlation with rates of admission for depression. By contrast, there was a weak or moderate negative rank correlation between the size of each of the 16 ethnic groups and the corresponding age-standardised rate of each category of admission (Table 1).
Table 1 Spearman's correlation between age-standardised rates of admission and ethnic group population size and the index of dissimilarity score for each group
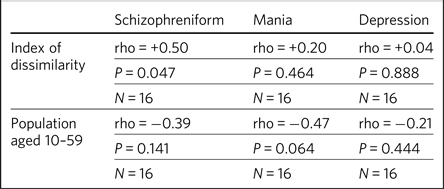
The data are for 16 ethnic groups in England.
Ethnic groups with populations aged between 10 and 59 years that were larger than half a million had relatively low rates of admission. Smaller ethnic groups with low levels of clustering (<40% index of dissimilarity) also tended to have lower rates of admission. Smaller ethnic groups with high levels of clustering (>40% index of dissimilarity) had higher rates of admission.
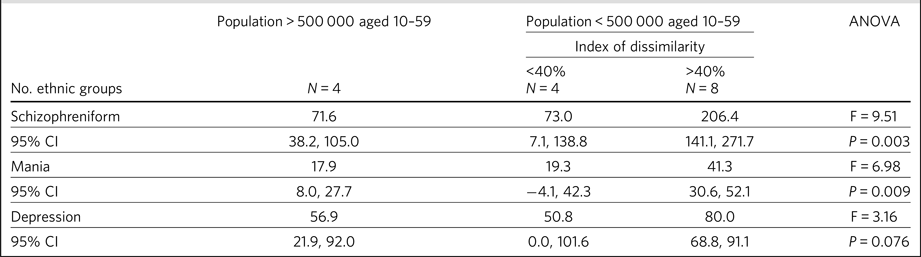
This pattern was most evident in schizophreniform admissions, where rates were on average three times higher in small clustered groups than the rates in groups with a larger population size. The rates of admission for mania were twice as high in smaller ethnic groups with high levels of clustering when compared with rates of admission for mania in ethnic groups with a larger population. The increase was least evident in depression admissions, where rates were about 40% higher in small clustered groups than the rates in groups with a larger population size (Table 2).
Table 2 The rate of admission in 16 ethnic groups including White British for schizophreniform, mania and depression admissions, according to large or small group population size and high or low group clustering.
Discussion
In line with previous studies, our results demonstrate an increased rate of admission in the majority of BME groups. There was significant variation in admission rates between ethnic groups, and there appeared to be an interaction with age. According to our results, the greatest increase in admission rates was in teenagers and young adults. By contrast, the AESOP study indicated that the incidence of psychosis remains raised in ethnic minority groups throughout the age range of our study.Reference Simpson18 This may indicate a reduced risk of (re)admission with increasing age in BME groups relative to the White British population.
Our findings provide support for the hypothesis that larger ethnic groups have lower rates of admission. This is a between-group effect rather than a within-group effect. In this study, located in England, which has a population aged 10–59 years of 40 million, ethnic groups with populations over half a million had lower rates of admission. Our findings do not support the hypothesis the more clustered groups have lower rates of admission. In fact, they suggest the opposite: groups with low clustering had lower admission rates. Again, it is important to emphasise that this study only looked at between-group effects and did not investigate within-group effects.
The BME population in the UK is increasing in size and becoming less clustered.Reference Parkinson, Champion, Simmie, Turok, Crookston and Katz16 Our results suggest that both of these factors should ameliorate the overrepresentation of BME groups among psychiatric in-patients. However, the Count Me In census indicated that this overrepresentation continues. The answer may lie in changes in the delivery to mental health services. We have previously shown that that although rates of admission have fallen across England, one of the largest reductions has been in admissions for depression, whereas admissions for schizophrenia and mania have shown only a modest, if any, reduction.Reference Singh, Greenwood, White and Churchill19
In this work, we have shown that the increased rate of admission for BME groups was confined to schizophreniform disorders and mania, but was not found in depression. Therefore, all other things being equal, reducing the rate of admissions for depression alone will have the unintended consequence of increasing the overrepresentation of BME groups in the psychiatric in-patient population. The same applies to interventions that are more effective in reducing admissions in adults over 35 years of age than in younger adults, such as crisis resolution home-based treatment (http://www.ethpop.org).
Limitations
Gender-specific data were not available; hence, standardisation by gender was not possible. The diagnostic information was from routine clinical practice. For the majority of patients, ethnicity was self-determined, but for a minority of patients the ethnicity category would have been picked by staff.
It is impossible to avoid the ecological fallacy when analysing population level data. This ecological study was undertaken at a national level and, therefore, the results may be affected by the ecological fallacy (i.e. associative results observed at this national level are not necessarily replicated at the individual or smaller geographical levels.Reference Robinson20 However, the finding of an association between ethnic groups and higher rates of detention is fully consistent with a number of studies that have found higher rates of psychosis and admission among individuals from BME groups.
Local area of residence is likely to reflect aspects of group membership dynamics, such as local ethnic density, dissimilarity and sense of membership. These are likely to be more fluid than individual-level variables. We argue that ethnicity may operate at various levels, including those of the individual, local area, region, and nation, and perhaps even beyond national boundaries; however, our national-level data did not allow us to investigate these nuances.
This study included information on the number of admissions in England for each ethnic group. It did not have access to any individual-level data or local area data. A further study is required with a more detailed data-set, including detention outcomes recorded at individual, local area, regional and national levels, and corresponding explanatory variables as in our previous study.Reference Weich, McBride, Twigg, Duncan, Keown and Crepaz-Keay21 Dual diagnoses, specific substance use and multiple admissions should all be considered in future studies.
Clinical implications
If these associations are replicated, then this study has several implications. The first is that as ethnic groups increase in size and become more evenly spread, relative rates of admission will fall.
Second, any change in the pattern of admission, according to broad diagnostic group, symptom type or age, is likely to affect the ethnic make-up of the psychiatric in-patient population. For example, home-based treatment as an alternative to admission has been shown to be more effective for depression and for adults over the age of 35. An indirect consequence of this could be an exacerbation of the overrepresentation of BME groups among the remaining in-patient population.
Future research in this area will model the effects that population change and changes in psychiatric practice since 2005/6 have had on the psychiatric in-patient population over the subsequent decade.
About the authors
Gayathri Venkatesan is a Consultant Neuropsychiatrist at Walkergate Park, Newcastle, UK; Scott Weich is a Professor of Mental Health at the Division of Mental Health and Wellbeing, Warwick Medical School, University of Warwick, Coventry, UK; Orla McBride is a Lecturer in Psychology at the School of Psychology, University of Ulster, County Londonderry, Ulster, UK; Liz Twigg is a Professor of Human Geography at the Department of Geography, University of Portsmouth, Buckingham Building, Portsmouth, UK; Helen Parsons is a Senior Research Fellow at the Division of Health Sciences, Warwick Medical School, University of Warwick, Coventry, UK; Jan Scott and Patrick Keown are Consultant Psychiatrists at Newcastle University, Academic Psychiatry, Campus for Ageing & Vitality, Newcastle, UK; and Kamaldeep Bhui is a Professor of Cultural Psychiatry and Epidemiology at the Centre for Psychiatry, Barts and The London School of Medicine and Dentistry, Queen Mary University of London, UK.






eLetters
No eLetters have been published for this article.