Disorder of personality in adolescence is a complex concept. On the one hand, it may be hard to distinguish personality pathology from normal developmental impermanence and instability. A developmental perspective demands that we keep an open mind about pathology trajectories, and balance resilience against vulnerability factors (Reference WernerWerner 1993). On the other hand, a small subgroup of young people do seem to present with emerging psychopathology that resembles adult personality disorder, where early diagnosis is likely to lead to early interventions and thus improve prognosis. The challenge lies in getting the formulation right. An inaccurate diagnosis of personality disorder in a young person may focus attention away from interventions that improve the caregiving environment at home, or stigmatise a young person in ways which ultimately do more to increase their problems. In this article, we explore these issues in some detail, basing our views on our work in a residential secure unit for young people.
Difficulties in diagnosing personality disorder in adolescents
A key debate about the diagnosis of personality disorder in adolescents is between those who argue that personality is not fully formed until early adulthood, and those who argue that some personality traits are present and stable from early childhood.
Continuity and traits
Theories of personality development and continuity from childhood to adulthood are summarised by Reference Caspi, Roberts and ShinerCaspi et al (2005). Certain clusters of adult traits, such as neuroticism, extraversion, conscientiousness, agreeableness and openness (the so-called ‘Big Five’ personality traits; Reference Ehrler, Evans and McGheeEhrler 1999), have been identified in pre-school children. Their presence in childhood predicts later behaviours (Reference ShinerShiner 2005), suggesting continuity of certain traits. Other studies have described the longitudinal relationship between childhood behaviour and personality traits and adult personality traits (Reference John, Caspi and RobinsJohn 1994; Reference Caspi, Lynan and MoffittCaspi, 2003, Reference Caspi, Roberts and Shiner2005; Reference Shiner and CaspiShiner 2003).
A chief criticism of trait-based personality theory for adolescence is that it seems reductive and does not account for how personalities change over time. Prospective studies of the Big Five traits in children tend to use outcome data based on adult reports, which may reflect adult personality and mood, rather than the childhood trait (Reference Lewis, Pervin and JohnLewis 2001; Reference Kroes, Verman and Der BruynKroes 2005).
Change and development
Personality change from adolescence to adulthood is robustly reported in a variety of lifespan and longitudinal studies (Reference VaillantVaillant 1983; Reference Soldz and VaillantSoldz 1999; Reference Sroufe, Egeland and CarlsonSroufe 2005). There is also evidence that personality traits and diagnoses can change considerably in childhood and early adolescence (10–15 years), but that there is less change and more stability in later adolescence (16–21 years) (Reference Klimstra, Hale and RaaijmokenKlimstra 2009).
In adolescence, it may be more helpful to think of the personality as a complex organisation of various psychological functions, differentiated into hierarchical levels. It may be that change in adolescence takes place at a different level of personality function, especially at the levels of character adaptations or beliefs and values and cognitions (Reference McAdams and OlsenMcAdams 2010; Box 1). The narrative level of the personality is the level of meaning and subjective experience of identity, what Reference McAdams, John, Robins and PervinMcAdams (2008) has called the ‘storied self’. Such narratives begin to emerge in late adolescence and are crucially related to the development of a ‘moral’ identity that makes ethical choices in social groups (Reference TappanTappan 1989). The development of these moral narrative identities may be relevant to the issue of rule-breaking and conformity in adolescence.
BOX 1 Layers of personality functioning and interventions
Disorders may occur at any level: people with personality disorder typically have high levels of negative traits, limited sense of agency, and impoverished self-narratives characterised by passivity, hostility and a sense of threat.
Layer 1
The person as an actor: traits, dispositions, temperament (limited interventional options: medications for symptomatic relief)
Layer 2
The person as an agent: motivations, intentionality, individual characteristics (effective interventions address cognition, values, beliefs, goals, e.g. cognitive–behavioural therapy, dialectical behaviour therapy)
Layer 3
The person as an author: the storied, reflective self (effective interventions address the social and self-reflexive self: group therapies, therapeutic communities, mentalisation-based therapy, cognitive analytic therapy)
Attachment, abuse and disordered formation of the personality
Attachment theory-based studies of development have proved relevant to understanding how the caregiving environment can produce problematic behaviours in vulnerable children: behaviours that are the basis of the diagnosis of emerging personality disorder. The caregiving environment provided by parents and other adults acts as a growth medium in which the growing child’s forebrain will develop through a process of arborisation, dendritisation and neuronal pruning. If the milieu is hostile, frightening or absent through neglect, these neuronal processes are affected (Reference Rice and BaroneRice 2000; Reference SchoreSchore 2001).
There is a body of evidence linking insecure attachment patterns to various forms of personality pathology (for a review see Reference Sarkar and AdsheadSarkar & Adshead 2006). An important longitudinal study is the Minnesota project by Reference Sroufe, Egeland and CarlsonSroufe et al (2005) which has followed up a high-risk group of children into early adulthood. These authors have focused on childhood as a time of developmental complexity, arguing that successful psychological maturity is associated with high degrees of differentiation and complexity in terms of representations of ‘self’ and ‘other’. In their sample, insecure attachment is strongly associated with the later development of personality pathology in adolescence. This confirmed earlier studies which found that dismissing attachment traits in adolescence is associated with elevated risk of developing traits of narcissistic and antisocial disorders, conduct disorder and substance misuse problems (Reference Rosenstein and HorowitzRosenstein 1996). In contrast, preoccupied adolescents were more likely to have traits of histrionic, borderline and schizotypal personality disorder.
Childhood and adolescent experience of trauma is also relevant to personality pathology, especially experiences that induce high levels of fear or shame, or both (Reference Lee, Scragg and TurnerLee 2001). Relevant evidence comes from the adolescent community surveys of Reference Johnson, Cohen and BrownJohnson and colleagues (1999), who have followed up a large cohort of children in the community into their early 20s. The strength of this research is that it starts from a study of the ‘normal’, i.e. not those selected because of perceived behavioural difficulties. This research group has shown clearly that childhood maltreatment, including neglect, substantially increases the risk of developing a personality disorder in adolescence (Reference Johnson, Cohen and KasenJohnson 2008). They found no difference between genders in terms of the range of maltreatment or the types of personality disorder that develop.
Neurobiology, genes and the development of the personality
There are neurological reasons why diagnosis of personality disorder in children and adolescents may be complex. The brain continues to develop throughout adolescence in terms of myelination and formation of synaptic networks (Reference Rice and BaroneRice 2000), which implies that the neural bases for many psychoregulatory systems will still be in development. Such systems will not be fully functional or yet fully ‘calibrated’ to the individual’s needs or environment, and may be expressed as immature psychological defenses such as denial or somatisation (Reference HeilbrunnHeilbrunn 1979; Reference Northoff, Bermpohl and SchoeeichNorthoff 2007). The development of the frontal lobe may continue to be influenced by the nature of attachment relationships in adolescence, which may be subject to change as parents get older or grandparents die (Reference SunderlandSunderland 2006).
Magnetic resonance imaging studies have found that when the brains of adolescents are compared with the brains of young adults there are significant maturational changes in the frontal lobes, temporal and occipital lobes (Reference Sowell, Thompson and HolmesSowell 1999). Areas of the brain responsible for response inhibition, emotion regulation, planning and organisation are continuing to develop, hence the increased impulsivity so often seen in adolescence. It has been suggested that adolescents are motivated to take part in novel adult experiences, but lack the contextual knowledge to guide their decision-making, seeming to be more impulsive (Reference Chambers, Taylor and PotenzaChambers 2003). Adolescent neural networks are also responding to exposure to high levels of sex hormones, with attendant effects on mood regulation. In contrast to pre-school children (where similar struggles with mood and impulse regulation are the norm), language, spatial awareness and sensory functions are largely mature by adolescence (Reference Blakemore and ChoudhuryBlakemore 2006).
Yet another problematic aspect of personality disorder diagnosis in childhood and adolescence is revealed by research into gene–environment interactions, which indicates that the caregiving environment influences the expression of genetic neuropharmacological vulnerability. For example, studies in boys have found evidence of an interaction between genetic vulnerability and an adverse environment. A hostile caregiving environment makes antisocial behaviour much more likely in boys with variations in allele length for serotonergic proteins than in those without this mutation (Reference Livesley, Jang and JacksonLivesley 1993; Reference Caspi, McClay and MoffittCaspi 2002; Reference Kim-Cohen, Caspi and TaylorKim-Cohen 2006).
Finally, given the prevalence of substance misuse among some adolescents, it is vital to consider the relevance of this in relation to psychopathology and diagnosis. Adolescents are motivated to use psycho-active substances that reduce anxiety, increase confidence and allow for attachment to peer groups. The immediate effects of drug and alcohol use on behaviour and social function are well documented, and are a major area of clinical and social work practice. However, the full and long-term extent of the effects of psychoactive substances on forming and developing neural networks, especially in the prefrontal cortex, is not yet known. It is possible that ethanol, in particular, may be neurotoxic to processes such as synaptogenesis or dendritisation, and makes the adolescent brain increasingly vulnerable to environmental challenges that in turn may make adult psychiatric disturbance more likely (Reference Olney, Farber and WozniakOlney 2000).
Emerging personality disorder and child and adolescent mental health services
The factors discussed in the previous section have two main implications for child and adolescent mental health services (CAMHS). First, if young people’s brains are changing, then any psycho-pathology is also likely to be changing. Therapeutic formulations and diagnoses need to be flexible and responsive to change. Axis I and Axis II disorders are commonly comorbid. In adolescence, this ‘transaction’ between Axis I and Axis II disorders is likely to be more pronounced, such that each makes the other more likely to develop, and both suggest a vulnerable psychological self-regulating system (Reference ShinerShiner 2009).
The other issue is that the parents’ state of mind or beliefs about how they provide care and how the child elicits care are key influences on the child’s development and behaviour (Reference Lewis, Pervin and JohnLewis 2001). It is not so much what parents do, as what parents believe about the child and their relationship with him/her that affects children’s behaviour. There is evidence that suggests it is the mother’s ‘mindedness’ about the child that affects the way in which the child develops an emotional language and theory of mind that are part of their personality structure (Reference MeinsMeins 1997). Support for the parents is therefore an important aspect of helping young people with emerging personality pathology. In addition, parents of children with conduct or hyperactivity problems are likely to have significant personality pathology themselves. (Reference Wolff and ActonWolff 1968; Reference Lahey, Piacentini and McBurnettLahey 1988; Reference Nigg and HinshawNigg 1997; Reference Kuperman, Schlosser and LidralKuperman 1999). The most die-hard genetic reductionist must accept that if personality problems are largely genetic, then both the genes and the environment come from the parents. If a child has, for example, callous and unempathic traits, then at least one of the parents probably does too, with potentially dire effects on the caregiving milieu in which the child grows up.
Current thinking about personality disorder favours a dimensional approach to understanding the pathology, i.e. personality disorders are extreme dimensions of normal traits that can vary in severity (Reference Tyrer and JohnsonTyrer 1996). If the traits of extraversion, conscientiousness, agreeableness, openness to experience and neuroticism are referred to as the Big Five, then it is possible to conceive of a set of ‘Bad Five’ traits (Box 2). These would include: avoidance of others and mistrust; impulsiveness and attentional problems; antisocial attitudes and contempt for others; rigidity of thinking and lack of curiosity about anything; and emotional dysregulation resulting in unmodulated and negative affect storms in response to unpredictable stimuli (Reference ShinerShiner 2009).
BOX 2 Positive and negative personality traits: Big Five v. Bad Five

| Big Five | Bad Five |
|---|---|
Found dimensionally in the general community
|
Found mainly in populations with personality disorder diagnoses and associated with significant harm: also dimensional
|
Reference ShinerShiner (2009) describes how these traits may be manifest in childhood and adolescence in terms of DSM-IV clusters (Table 1). Cluster A involves avoidance, rigidity and variations in reality testing (what Shiner calls the ‘peculiar factor’). Cluster C also involves avoidance and internalised emotional dysregulation, characterised by preoccupying anxieties. Cluster B (which, as in adult services, tends to draw most attention) combines antisocial attitudes and contempt for others, impulsivity and emotional dysregulation.
TABLE 1 Personality disorder clusters (DSM-IV) and personality traits
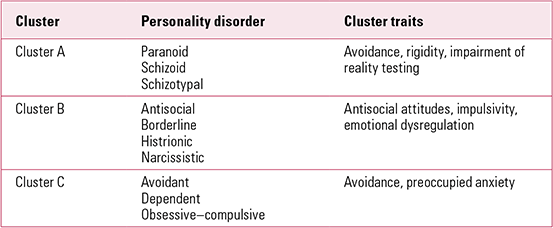
The self-destructive and antisocial aspects of personality disorder are of greatest concern, because they have the potential to cause most distress in adults around the young people, and are therefore most likely to generate referral to CAMHS and/or forensic services. However, children and adolescents are also vulnerable to developing other types of personality dysfunction. Young people with Cluster A and C disorders also need interventions, since any Axis II disorder increases the chance of developing an Axis I disorder (Reference Crawford, Cohen and FirstCrawford 2008). In addition, any personality disorder in adolescence increases the risk of violent acting out, with potentially disastrous consequences for the young person (Reference Johnson, Cohen and SmailesJohnson 2000).
Prevalence of personality disorder in children and adolescents
Despite scepticism about whether personality disorder can really exist in children, there are studies which indicate that personality disorder diagnoses in adolescents have validity and stability over time (Reference Brent, Zelenak and BuksteinBrent 1990; Reference Bernstein, Cohen and VelezBernstein 1993; Reference Levy, Becker and GriloLevy 1999).
The personality disorders that present to adolescent services appear to resemble those that present to adult services. As always, prevalence rates are affected by selection bias in relation to services selected for study, and the recruitment of participants. For example, the Reference Bernstein, Cohen and VelezBernstein et al (1993) study of personality disorder in a community-based sample of children and adolescents found a prevalence of 31%: the most common of which was obsessive–compulsive personality disorder. Only 17% of the cohort had a severe disorder; most commonly narcissistic personality disorder. By contrast, Reference Levy, Becker and GriloLevy et al (1999) found that 61% of an adolescent in-patient sample had a Cluster B personality disorder, mainly borderline personality disorder. There were very few patients with Cluster C diagnoses. Neither study screened for antisocial personality disorder.
Reference Kasen, Cohen and SkodolKasen et al (1999) completed a prospective longitudinal study of personality pathology in children aged 9–13 years over three follow-up points in a 10-year period. Their prevalence data indicate that about 15% of adolescents had a Cluster B personality disorder before young adulthood. Prevalence rates were comparable across genders. The prevalence of personality disorder at the start of the study was 9.6% for Cluster A, 16.7% for Cluster B, and 8.2% for Cluster C. However, the prevalence of the disorders changed over time: for example, at the start of the study, 7.6% of boys and 9.4% of girls had a Cluster B diagnosis, but 9 years later, the prevalence was 22.4% of boys and 11.9% of girls. The prevalence had increased in both genders, but considerably more for the boys.
Most studies of personality disorder in in-patient settings focus on Cluster B disorders: borderline or antisocial psychopathology. We have reviewed some of the data on antisocial personality symptoms here, but emphasise that other personality psychopathology may be emergent in adolescence yet ignored because it does not cause social disruption.
Emerging antisocial personality traits and related disorders
Conduct disorder in children, antisocial personality disorder and psychopathy are interrelated but are distinct clinical concepts. There has been considerable interest in the relationship of early childhood behavioural problems and later antisociality since the early studies of Reference RobinsRobins (1966) showed that a small subgroup of children with conduct disorder show persistently antisocial behaviour in adulthood. The diagnosis of antisocial personality disorder requires evidence of childhood history of rule-breaking and irresponsibility.
Frick and colleagues (Reference Frick, O'Brien and WoottonFrick 1994; Reference Salekin and FrickSalekin 2005) demonstrated that children with severe behavioural disturbance can sometimes show callous–unemotional traits, and that these traits are different from traits from the behavioural definitions for conduct disorder. Reference Frick, Cooke, Forth and HareFrick (1998) suggested that the co-existence of attention-deficit hyperactivity disorder, childhood-onset conduct disorder and callous–unemotional traits is highly correlated with the construct of psychopathy. However, there is no empirical data supporting the progression of these factors into adult psychopathy, which is characterised by affective deficits, multiple forms of criminality and increased risk of severe violence (Reference FrickFrick 2002).
Reference FarringtonFarrington (2005a,Reference Farringtonb) reports a prospective study of 400 boys up to adulthood using the Hare Psychopathy Checklist Screening Version (PCL-SV). His group found that high PCL-SV scores at age 48 years were predicted by childhood environmental (rather than personality) factors between ages 8 and 10, including physical neglect, poor parental supervision, a disrupted family, large family size, a convicted parent, and a mother with depression. Such studies confirm the importance of childhood adversity as a good predictor of later antisociality, and being as important as any genetic influence.
Delinquency in young women is often overlooked. In a meta-analytic review, Reference Fontaine, Carbonneau and VitaroFontaine et al (2009) examined 46 empirical studies that examined the developmental trajectories of antisocial behaviour in females. They found similar trajectories to the adolescent male research, with the addition of a further category, adolescent-delayed onset, where females had apparently not shown antisocial behaviour until later in adolescence. The emergence of antisocial behaviour at this time was considered to be associated with a decrease in familial and school control over the young women, an association with delinquent peer groups and hormonal changes due to puberty. Reference Caspi, Lynan and MoffittCaspi et al (1993) suggest that there may be specific biological risk factors for delinquency in women (e.g. early menarche).
Offending and personality disorder in adolescents
The peak age for minor offending is 17–18 and so it is not unusual to find an adolescent male who has committed an offence. However, there is a subgroup of adolescent offenders who commit the majority of offences. These can be divided into:
-
• those who behave antisocially only during adolescence (and effectively ‘grow out’ of their antisocial behaviour);
-
• those that persist in acting antisocially as they get older.
Research into offending trajectories indicates that only 5–10% of adolescents who show antisocial characteristics follow the trajectory into adulthood. They are referred to as the early-onset life course group (Reference Moffitt and CaspiMoffitt 2001; Reference Laub and SampsonLaub 2003). This group are clinically distinct and have a poorer prognosis when compared with the adolescence-limited group, who engage in antisocial behaviour for only a limited period during adolescence. The latter are believed to show antisocial behaviour as a part of gaining independence, seeking status and becoming free of parental supervision.
The evidence indicates that the early-onset group have experienced severe family adversity and a coercive parenting style (Reference Moffitt and CaspiMoffitt 2001). This group are thought to be exposed to severe environmental adversity over a prolonged period of time. A follow-up study of males who had been aggressively antisocial in childhood, but had shown little delinquency in adolescence, reported that at age 26 they tended to be socially isolated and to have adjustment and mood problems and financial difficulties, rather than severe antisocial behaviour per se (Reference Moffitt, Caspi and HarringtonMoffitt 2002).
Reference Vizard, French and HickeyVizard et al (2004) propose the existence of severe personality disorder in children and adolescents, on the basis of studies of the characteristics of young people who have committed sexual assaults or other serious crimes. They hypothesise that callous and unemotional personality traits arise as a consequence of a combination of genetic, perinatal and early developmental difficulties which become progressively more disabling as the individual matures. The authors outline a multifactorial pathway for the development of severe personality disorder involving early attachment difficulties, poor peer relationships, and early and serious child abuse, which are then manifest as aggression and sexualised behaviours in childhood. They emphasise the therapeutic importance of early detection.
Assessment of personality in childhood and adolescence
Given that the diagnostic process is complex for adolescents, it is not clear whether assessment tools that are based on adult assessment of personality disorder will be either valid or reliable. Nor is it clear whether there is value in assessment tools that are standardised on clinical populations. In children, both temperament and behaviour can be assessed using a variety of tools, although these are rarely used outside research protocols. Most research studies of emerging personality pathology have utilised assessment tools based on adult assessment tools (Reference Shiner, Masten and RobertsShiner 2003). There is uncertainty about the use of such tools in ordinary clinical services.
However, some specialist services for adolescents do use personality assessment tools (Box 3). These include the NEO Personality Inventory – Revised (NEO-PI-R; Reference Costa and McCraeCosta 1992), which assesses Big Five traits in adolescents (Reference De Clercq and De FruytDe Clercq 2003; Reference Allik, Laidra and RealoAllik 2004), and the Millon Adolescent Clinical Inventory (MACI; Reference Millon, Millon and DavisMillon 2006). The MACI is a self-report measure based on the Millon Clinical Multiaxial Inventory. Constructs have been validated against DSM-IV diagnostic criteria and address three different types of reported difficulties: personality trait, expressed concerns and behaviours.
BOX 3 Some personality disorder assessment tools used in adolescence
-
• Hare Psychopathy Checklist – Youth Version: young people’s version of standard measure of psychopathy (Reference Forth, Grisso, Vincent and SeagraveForth 2005)
-
• Millon Adolescent Clinical Inventory: developed to be used in teenagers (Reference Millon, Millon and DavisMillon 2006)
-
• Minnesota Multiphasic Personality Inventory – Adolescence (MMPI-A): an empirically based measure of adolescent psychopathology (Reference Butcher, Williams and GrahamButcher 2006)
-
• NEO Personality Inventory – Revised: a general measure of Big Five personality traits (Reference Costa and McCraeCosta 1992)
Measures of attachment may be helpful in terms of making sense of personality pathology and suggesting interventions in family dynamics. A variety of measures of both attachment and personality disorder in adolescents are described by Reference Westen, Thomas and NakashWesten et al (2006).
Forensic CAMHS and some youth offender services use youth versions of risk assessment instruments, such as the Hare Psychopathy Checklist – Youth Version (PCL-YV; Reference Forth, Grisso, Vincent and SeagraveForth 2005) and the Structured Assessment of Violence Risk in Youth (SAVRY; Reference Borum, Bartel, Forth, Grisso, Vincent and SeagraveBorum 2005). There are ethical concerns about their routine use because they can be used in stigmatising ways that reduce young people’s access to general adolescent services.
Management of adolescent personality disorder
Work with children and adolescents differs from that with adults, in that services take a more systemic approach. An especially significant difference from adult services is the statutory involvement of the education system, and the need to work with family members who are still involved in the young person’s social network. However, the treatment of a young person with an emerging personality disorder should follow the principles of CAMHS generally. In particular, it is important to screen for Axis I disorders such as depression or psychotic disorders, especially in children and adolescents with emerging borderline personality disorder where depression is likely to be a comorbid condition.
Specific interventions for personality disorder in adolescents are similar in principle to those for adults, although few have been subjected to the same level of empirical evaluation. The National Institute for Health and Clinical Excellence (NICE) guidelines for borderline personality disorder noted that there has been only one published randomised controlled trial of interventions for adolescents with personality disorder, which may be because clinicians are reluctant to diagnose young people with the disorder (National Collaborating Centre for Mental Health 2009a). Similarly, there is no mention of any evidence relating to the treatment of comorbid personality disorders in young people with depression or eating disorders, even though these are common comorbidities in adulthood. Such a lack of evidence makes treatment complex, especially since the transition between adolescence and adulthood may be a critical period for intervention.
Dialectical behaviour therapy
Dialectical behaviour therapy (DBT) has been adapted for a wide range of clinical populations, including adolescents. Programmes offering DBT to adolescents have been adapted in a number of ways, but no one version has been shown to be superior.
There is preliminary evidence to support an adapted version of DBT with adolescents who meet criteria for borderline personality disorder (Reference Rathus and MillerRathus 2002). Adolescent DBT (DBT-A) differs from adult DBT in that it is designed to be delivered over fewer sessions (24 sessions over 12 weeks, compared with typically weekly sessions over 12 months for adults), includes parents in the therapy programme, places a greater emphasis on the family, and focuses on teaching a smaller number of skills. The language used is adapted to be more appropriate for an adolescent (Reference Rathus and MillerRathus 2002).
Involvement of the family or carers in skills training is common to many of these adaptations. Teaching other family members skills can enable them to act as skills coaches to generalise these skills in young person’s everyday environment. Although individuals are encouraged to work towards changing their own environment during DBT, it is recognised that adolescents may not always have the autonomy to effect these.
Reference Rathus and MillerRathus & Miller (2002) found that adolescents engaging in DBT were admitted to hospital less often, had higher rates of treatment completions, reduction in suicidal ideation and symptoms of borderline personality disorder when compared with treatment as usual. There was a significant reduction in behavioural incidents when DBT was used on an adolescent in-patient unit, when compared with a unit run on psychodynamically oriented principles (Reference Katz, Cox and GunasekaraKatz 2004). Reference James, Winmill and AndersonJames et al (2011) offered DBT to a community sample of adolescents in the ‘looked after’ system (i.e., in the care of the Local Authority). The authors found a significant reduction in self-report depression scores (Beck Depression Inventory), hopelessness (Beck Hopelessness Scale) and episodes of self-harm.
Dialectical behaviour therapy has also been shown to have some positive effects in female juvenile rehabilitation settings (Reference Trupin, Stewart and BeachTrupin 2002). This study highlighted both the impact of DBT on the young people and changes in the staff’s reactions to them. Staff who had completed in-depth training in DBT showed a reduction in punitive interventions.
STEPPS
Another programme for improving emotion regulation is Systems Training for Emotional Predictability and Problem Solving (STEPPS; Reference Blum, Bartels and St JohnBlum 2009). This has been used with adolescents to good effect (Reference Schuppert, Giesen-Boo and van GemertSchuppert 2009). Compared with treatment as usual, adolescents who completed the STEPPS programme reported feeling a greater sense of control over their mood swings. The STEPPS programme, like DBT-A, involves training not just the young persons, but also family, friends and professionals with a shared understanding of the skills, so that the network of people closest to the young person can learn to reinforce and support the newly acquired skills.
Treatments for conduct disorder
A variety of interventions for conduct disorder have been evaluated both in the USA and the UK (Reference Breston and EyberBreston 1998; National Collaborating Centre for Mental Health 2009b). These include parent training, cognitive problem-solving training with young people, programmes that combine work with parents and children, family therapy, and treatment in foster care. All these interventions have been shown to be effective for selected groups. Family therapy and treatment in foster care have both been found to reduce behaviour problems and offending. There is a large evidence base for group-based training programmes for parents, probably due to an effect on parental negativity towards their child.
Multisystemic therapy
Multisystemic therapy is used with children and adolescents at risk of antisocial behaviours. It has been subject to a number of treatment trials, and shown to be effective with selected groups of young people and their families. It is a family- and community-based treatment programme, with the aim of improving communication, parenting skills, prosocial peer relationships, school performance and social networks. The outcome is to keep young people in their family homes rather than incarcerated in prison settings or hospitals (Reference Henggeler, Melton and SmithHenggeler 1992; Reference LittellLittell 2005). Families have reported increased family cohesion, and young people have fewer arrests and self-reported offences.
Are psychological therapies effective?
It is possible to provide adolescents with psychological interventions that improve problematic behaviours. However, it is not clear whether these interventions effect change in underlying personality structures. Given the importance of insecure attachment for the development of disordered personalities, it seems important to provide a secure base for therapy, and to promote curiosity and learning of new cognitions and appraisals, both of self and others. Young people with different attachment styles may present with different symptom profiles and behavioural challenges.
Conclusions and questions
It seems clear that for a small number of adolescents, a diagnosis of personality disorder can be confidently made. There is significant health morbidity among affected adolescents. Just as for adults, young people who have a personality disorder have high rates of early mortality, especially among those with borderline personality disorder and antisocial personality disorder (Reference Kjelsberg and DahlKjelsberg 1998; Reference PajerPajer 1998). Therefore, these disorders are deserving of more time and attention from researchers, clinicians and policy makers.
However, the diagnosis of personality disorder is a double-edged sword (Box 4). Although early identification and treatment are likely to ameliorate a lifetime of potential suffering for the individual and society, a personality disorder diagnosis is a stigmatising label that can follow a young person for a considerable time and paradoxically block their access to treatment and services (Reference CastilloCastillo 2000). An alternative lexicon has sprung up in recent decades, with clinicians appearing to prefer to use diagnoses that emphasise trauma rather than challenging behaviours, such as the widespread use of the term ‘complex post-traumatic stress disorder’ instead of emerging borderline personality disorder, particularly when there is a history of prolonged trauma as an antecedent. Similarly, young people with significant antisocial traits continue to be labelled as having conduct disorder or mixed disorder of conduct and emotions or even reactive attachment disorder, rather than antisocial personality disorder.
BOX 4 Pros and cons of personality disorder diagnosis

| Pros | Cons |
|---|---|
|
|
This approach illustrates the continuing reluctance of clinicians to diagnose personality disorder in young people whose personalities are still developing. Clearly, it is unprofessional to use diagnoses in thoughtless and unhelpful ways, and it is valuable to promote recovery and coping skills in all mental disorders, including personality disorder. The difficulty with not using the personality disorder diagnosis is that it may obscure clinical need, often in relation to the most difficult symptoms such as hostility and rage attacks. It may also allow professionals to avoid looking at their own negative reactions to difficult young people, especially those who have been cruel or hostile to others.
Whichever diagnostic descriptors are used, clinicians are likely to meet young people with symptoms and signs of antisocial or borderline personality disorder. Therefore there must be more debate and consensus on which descriptive diagnoses are most useful. A move from purely categorical to more dimensional diagnostic systems would help to overcome this. Adolescents with these syndromes must not be denied interventions and treatments merely because of the fears of labelling and perpetuation of stigma.
There are a number of research questions to pursue. The principal of these regard the prevention of antisocial personality disorder in adolescence and the identification of high-risk cases (Reference Harrington and BaileyHarrington 2004). We also do not know why girls subjected to trauma are more likely to develop borderline personality disorder, whereas boys are likely to develop conduct disorder and eventually antisocial personality disorder. Nor can we identify which young people will present with which disorder, at which point in their lives and why. Related to this are ethical questions about identifying children and adolescents as being at ‘high risk’ or antisocial, especially on the basis of their genes.
Research in the area of personality disorder in the young is bound to focus on the aetiology and pathogenesis of these disorders. In recent years, gene–environment interactions have received increasing attention as efforts are made to unravel the complex interplay between them. However, future research must focus on bridging the gap between gene and environment since a purely genetic or purely environmental view is unlikely to provide the answer. Since it is also unlikely that we will be able to alter genetic profiles any time soon, we may be under an extra duty to intervene in children’s adverse environments.
On this basis, services should be designed to intervene early and with the adolescent’s environment – the home, school and neighbourhood. Therapeutic interventions for children and adolescents must focus on helping to increase their resilience as much as on treating the disorder, and on the development of a prosocial identity. The emphasis must shift to the preventive, in the form of interventions for parents and caregivers. Environmental adversity in childhood increases the risk of the development of a whole range of problems (Axis I and Axis II disorders) in childhood and adolescence that may persist into adulthood. These disorders are costly, not only for the young people and their families but for all of us.
MCQs
Select the single best option for each question stem
-
1 Personality disorder in adolescence:
-
a is easily diagnosed
-
b does not exist
-
c is exactly the same as adult personality disorder
-
d is only found in in-patient settings
-
e is often comorbid with Axis I disorders.
-
-
2 The prevalence of personality disorder in adolescence:
-
a is the same as adult rates
-
b is the same in in-patient and community settings
-
c changes over time
-
d cannot be estimated reliably
-
e finds rates of 17% for severe disorders.
-
-
3 Personality disorder in adolescence:
-
a is genetically determined
-
b has no association with adult disorders
-
c does not increase the risk of violence
-
d is associated with child-rearing problems in adulthood
-
e is untreatable.
-
-
4 Which of the following is not an established treatment for personality disorder in adolescence?
-
a dialectical behaviour therapy
-
b STEPPS
-
c multisystmeic therapy
-
d mentalisation-based therapy
-
e family therapy.
-
-
5 Determinants of personality disorder in adolescence do not include:
-
a diet
-
b genetic vulnerability
-
c parental psychopathology
-
d childhood adversity
-
e childhood neuroticism.
-
MCQ answers

| 1 | e | 2 | c | 3 | d | 4 | d | 5 | a |






eLetters
No eLetters have been published for this article.