CLINICIAN’S CAPSULE
What is known about the topic?
There are concerns regarding unequal treatment towards First Nations people when engaged with health care services.
What did this study ask?
Whether quantitative differences in care exist between First Nations and non-First Nations patients in the ED.
What did this study find?
First Nations presenting with abdominal pain were found to have no difference in the time-related care parameters relative to non-First Nations patients.
Why does this study matter to clinicians?
Future quantitative and qualitative studies will be necessary to further understand the care inequality that has been expressed among First Nations patients.
INTRODUCTION
Historically, First Nations people of Canada have faced persecution and racial bias. Numerous concerns regarding the mistreatment of and prejudice towards First Nations people when engaged with services, including law enforcement, education, and healthcare, still exist in today’s society. One specific healthcare context where such bias towards First Nations patients may present is in the emergency department (ED).1 This negative dynamic potentially manifests both in time differences to appropriate care and the actual level of care that specific ethnic groups are given.1 More pointedly, the detection of such differences underscores voiced concerns that First Nations patients may not receive the same level of healthcare when compared to non-First Nations patients.Reference Johnson, Weaver and Borrero2, Reference Browne, Smye and Rodney3 The negative effects of such health–system-related disparities may already be evident as the social determinants of health, which include strong social predictors of well-being among Canadians such as employment status, income, education, gender, and Aboriginal status itself.Reference Mikkonen and Raphael4 Such discrepancies are a major problem because they represent both a potential violation of the Charter of Rights and Freedoms and a human dignity issue.
Locally, these questions and concerns have been raised by ED patients in Saskatoon, Saskatchewan to the Department of Emergency Medicine and Saskatoon Health Region (SHR) client representatives. Thus, ensuring that every individual receives equal care throughout their ED experience has become a very important issue within the SHR. In response, the study objective was to analyse these perceived differences quantitatively, with the hypothesis that differences in care exist between First Nations and non-First Nations ED patients.
METHODS
The present study, completed in partnership with the Saskatoon First Nations and Métis Health Council (FNMHC), the SHR, and with the approval of the University of Saskatchewan’s Biomedical Research Ethics Board, examined the level of care provided to Status First Nations patients in comparison with non-First Nations patients in two EDs in Saskatoon (Royal University Hospital [RUH] and St Paul’s Hospital [SPH]). Investigators were committed to conducting research in a respectful manner; OCAP principles and national ethical standards outlined by the Tri-Council policy were discussed with the FNMHC.5 An agreement was made with the FNMHC to follow these principles to the best of our ability. As such, stakeholders from the FNMHC were involved in all stages (ethics approval, idea formulation, analysing data, and reviewing final manuscripts). We did evaluate the hypothesis that care differences exist between Status First Nations and non-First Nations patients; however, the failure to detect such differences is not, by default, sufficient to prove the opposite conclusion of equivalent care. Thus, because certainty of care equality is a definitive study goal, the primary hypothesis tested was that meaningful differences in care do not exist between Status First Nations patients and non-First Nations patients when entering the ED, a more rigorous approach to proving group similarity.
We performed a retrospective chart review to evaluate the care provision among First Nations and non-First Nations patients. All subjects in the two groups had the same chief complaint of abdominal pain (a common presentation in the ED) and a Canadian Triage and Acuity Scale (CTAS) score of 3. The main outcome in this study was the time to physician assessment, because time to care is an objective factor reflecting the efficiency of ED care.
Patient selection
Status First Nations patients were identified by their status number, given by the federal government to First Nations people who are registered as Status First Nations under the Indian Act of 1876. These numbers appear on the ED chart for insurance purposes and do not identify Métis or Inuit individuals. Included in the study were 95 charts from Status First Nations patients and 95 charts from non-First Nations patients seen at either RUH or SPH between January 1, 2013 and December 31, 2014. Sampling was performed by SHR’s data information service, Strategic Health Information and Performance Support (SHIPS), which presented Saskatoon health records with a list of 800 visits eligible for a review, based on a chief complaint of abdominal pain and a CTAS score of 3 during the study period. These cases were selected by a random sampling procedure that involved prior stratification of all presentations of this description by First Nations status and year. As such, 200 presentations of each ethnicity-year combination were available. From these, 95 charts from each ethnic cohort (Status First Nations and non-First Nations) were selected at random for analysis. These 190 charts arose from a total of 9,821 ED visits for abdominal pain with a CTAS score of 3 (1,356 Status First Nations patients and 8,465 non-First Nations patients) during the 2-year study period.
Data extraction
The study was investigator-blinded. One investigator created anonymity on the charts so that the second investigator could review without potential bias. Blocking names (and status number if applicable), addresses, and next of kin information by similarly taping over the information in all charts eliminated any identifying factors. Data were then collected on the following pre-determined outcome variables: time to doctor (primary outcome), time to analgesia given, length of stay (LOS), referral for consultation, bloodwork, imaging, and final disposition. Covariate data were also collected in regard to the patient’s age, sex, date of presentation, and hospital. Information was extracted by a medical student (RB) who was aware of the study hypotheses, under the supervision of the principal investigator (JS). Data were recorded directly into a pre-formatted electronic spreadsheet for analysis.
Sample size
Because testing the hypothesis that the selected care variables were equal between groups was the priority, the sample size calculation aimed for a sufficient number of participants for an equivalence testing (see Statistical analysis) of time to doctor. It was assumed that 15 minutes was a reasonable equivalence margin, that the difference in our sample might be as large as 7 minutes, and that the standard deviation would be approximately 20 minutes.Reference Sonnenfeld, Pitts, Schappert and Decker6-Reference Wheeler, Hardie and Klemm8 Power and alpha were set at 80% and 0.05, respectively. Under this scenario, 78 subjects per group were required. To account for potential inaccuracies in the assumed calculation parameters, approximately 20% was added, increasing the value to 95 subjects per group, totalling 190 cases.
Statistical analysis
Unadjusted group comparisons of continuous and categorical variables were initially assessed using the non-parametric Mann-Whitney U test and chi-square/Fisher exact tests, respectively. Characteristics differing between groups were viewed as possible confounders, potentially undermining the observed relationships between First Nations status and the outcomes evaluated. Adjustments for these possible effects were made using multiple regression; covariates showing a tendency towards group differences (Table 1), as evidenced by univariate p-values less than 0.20, were included in the multiple regression models. Due to skewness of the continuous outcomes (i.e., time to doctor, time to analgesia, and LOS), values were log-transformed for improved normality prior to modelling. Although patients had a similar complaint and triage score, underlying conditions, some potentially requiring more investigation/consultation than others, have confounding potential if not present in equal frequencies between the groups. As such, a repeat sensitivity analysis evaluating only the non-hospitalized patients, who were expected to have greater uniformity of conditions, was also undertaken.
Table 1. Patient demographic and treatment differences between Status First Nations and non-First Nations patients with an abdominal pain and a CTAS score of 3

IQR=interquartile range; LOS=length of stay.
* Group comparisons made by Mann-Whitney U test and chi-square test for comparisons of medians and proportions respectively unless otherwise indicated.
† Offered or administered.
‡ Undertaken or arranged.
§ Fisher exact test due to small expected cell sizes.
¶ Does not include the 8 subjects above who left without being seen/treated/against medical advice as their inclusion would underestimate true treatment LOS; among these, 7 had time of discharge recorded, with a median LOS (IQR) of 92 minutes (59, 152). Time to MD was missing in 12 Status First Nations (13%) and 11 non-First Nations (12%) patients; among those receiving analgesia, time from MD to analgesia was missing in 7 Status First Nations (13%) and 10 non-First Nations (18%) subjects. Discharge home frequencies do not sum to 95 in each group due to missing values. Variable percentages may not sum to 100% due to rounding.
To specifically test whether group comparisons supported the contrasting hypothesis, that the two populations are essentially equivalent on the time-related outcomes (i.e., have time differences that do not exceed a margin where they would be considered “close enough” to be regarded as the same), equivalence testing was also undertaken using the two one-sided test approach on the log-transformed times. Pre-specified margins of difference considered equivalent between the groups were 15 minutes, 15 minutes, and 30 minutes for time to doctor, time to analgesia, and LOS, respectively. Because log transformation requires the equivalence to be analysed using ratios, these margins were converted to percentages of the non-First Nations median times (e.g., a 15-minute margin beyond an expected 60-minute duration, resulting in a 75-minute upper equivalence boundary, would be converted to 75/60 or 1.25, a 25% margin, and then transformed to a natural log.) All statistical analyses used SAS software, version 9.4 (SAS Institute Inc., Cary, NC, USA). The significance level was set at alpha equal to 0.05.
RESULTS
Differences in characteristics and treatment are summarized in Table 1. The two groups were similar, with the only statistically significant univariate difference seen in the higher proportion of Status First Nations patients who left with an incomplete visit (8% versus 0%, p<0.007). However, Status First Nations subjects did show a tendency towards younger ages (<18 years: 23% versus 17%; 18 to 39 years: 55% versus 47%;≥40 years: 22% versus 36%; p=0.10) and weekend presentation (35% versus 23%, p=0.08), with covariates included in the adjusted models. Although care parameters were generally similar, marginally significant differences were again observed in Status First Nations versus non-First Nations subjects for imaging (46% versus 60%, p=0.06) and consultation (14% versus 23%, p=0.09). The former resolved on an adjustment for age and weekend presentation (p=0.24); the association between group and consultation also became non-statistically significant (p=0.17). Tables 2 and 3 provide information on univariate and adjusted models.
Table 2. Simple and multiple linear regression models

* Values are based on log transformed outcomes with estimates providing comparisons of time between the groups as relative proportions, rather than differences; se=standard error; CI=confidence interval; ref=reference group. Covariates were limited to age and weekend presentation because these were the only characteristics recognized to be substantially different between the groups under comparison and, as such, may confound the primary relationships under study (i.e., First Nations status association with care outcomes).
Table 3 Simple and multiple logistic regression models
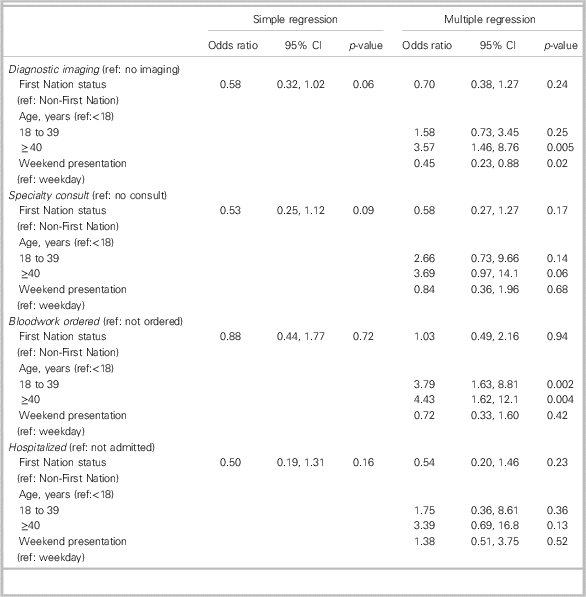
CI=confidence interval; ref=reference group; se=standard error. Covariates were limited to age and weekend presentation because these were the only characteristics recognized to be substantially different between the groups under comparison and, as such, may confound the relationships under study (i.e., First Nations status associated with care outcomes).
Figure 1 shows the group distributions of time to physician, time from physician to analgesia (if offered or received) and emergency visit duration. These times were not different on univariate testing (see Table 1) and showed no meaningful change in their associations with a patient group on adjustment (see Table 2). On equivalence testing, time to doctor for First Nations patients was found to not exceed the proposed 15-minute margin (p=0.007); LOS trended similarly (p=0.06), although time to analgesia was less conclusive (p=0.10). The actual difference in median times for the groups was well within the margins (time to doctor: 58 versus 61 minutes; time to analgesia: 40 versus 45 minutes; LOS: 259 versus 277 minutes) with non-First Nations patients having slightly shorter median durations on all three times. Because the LOS among subjects who left prior to a formal discharge was markedly shorter compared to the median group LOS durations, these values were not included in the LOS analysis to avoid artificially decreasing the median time among the First Nations subjects. Findings were not changed on the sensitivity analysis, which excluded those subjects requiring admission (data are not shown).

Figure 1. Group distributions of times: A) from registration to physician, B) from physician to the first analgesic (offered or administered), and C) for emergency room length-of-stay. Vertical lines represent median times.
DISCUSSION
Social determinants of health (culture, income, education, gender, employment, etc.) play a major part in one’s well-being, and it is known that First Nations populations face many barriers that negatively impact their health.Reference Mikkonen and Raphael4 Although a number of factors clearly influence differential health levels, it is also important to address the health system question as to whether or not First Nations patients receive the same care. Because patient satisfaction has been shown to be directly related to wait times, our goal was to address this question by looking at the problem from a quantitative perspective.Reference Anderson, Camacho and Balkrishnan9 Undertaking a retrospective chart review, we collected and analysed data based on specific criteria (CTAS 3 and a chief complaint of abdominal pain, through the years of 2013 and 2014 at RUH and SPH in Saskatoon).
Locally, the discussion regarding emergency care equality began after a number of First Nations individuals expressed dissatisfaction around their level of care. As healthcare professionals, our duty partly involves determining whether indeed there is an issue in the system and how it can be fixed.
The analysis did not show any statistically significant differences between the two population subsets in regard to the selected care parameters. In comparison to U.S.-based studies, which showed a significant difference in wait times across different racial/ethnic groups, our study shows no significant difference between First Nations patients and non-First Nations patients in terms of time-related level of care.Reference Johnson, Weaver and Borrero2, Reference Sonnenfeld, Pitts, Schappert and Decker6, Reference Park, Lee and Epstein10 In contrast, equivalence testing in our sample provided statistical support for the belief that times to doctor in First Nations patients are not prolonged relative to non-First Nations patients. LOS also neared significance on an equivalence assessment, whereas time to analgesia was less certain, potentially underpowered because only approximately half of the subjects received pain medication or had documented a time of offer. The observed difference in consultation likelihood trending towards significance has not been described in the literature when comparing Status First Nations patients to non-First Nations patients. The younger age of our First Nations sample likely contributed to this observation because the adjustment did substantially decrease the statistical significance of the relationship. Past Canadian studies have reported a poor specialist follow-up with First Nations populations in the context of cardiopulmonary disease; however, this pertained to the outpatient setting.Reference Sin, Wells, Svenson and Man11, Reference Bresee, Knudtson and Zhang12 Notably, difference in consultation may have been overestimated in our study by the allocation of those who left without a physician’s clearance to the non-referred group, even though a consultation might have occurred if the visit had been completed. These departures (n=8) all occurred among the First Nations subjects.
First Nations patients leaving the ED prior to a visit completion have been described before in a 2016 Canadian study.Reference Ospina, Rowe and Voaklander13 These departures may impact health outcomes and warrant future studies. The median time to physician in the First Nations group may also have been slightly underestimated by incomplete visits, because the times spent waiting in emergency among the six patients who did not see a physician prior to leaving exceeded the median group’s time to physician in four cases. The interval from arrival to registration was not evaluated in our study; a disproportionately long wait at arrival among First Nations patients would represent another care inequality and could contribute to premature self-discharge. Other studies that have evaluated wait times and racial disparities in the ED have excluded patients who left without being seen, although we felt it necessary to consider how frequently self-discharge occurred and how this factor might affect care comparisons.5, Reference Park, Lee and Epstein10, Reference Mills, Shofer and Boulis14
Even with our findings, the treatment of First Nations patients still remains a major concern. A qualitative study in Vancouver, Canada was able to show that Aboriginal patients feel judged for being Aboriginal, as having illegitimate pain issues, and that their reason for coming to the ED is inappropriate.Reference Browne, Smye and Rodney15, Reference Dell, Firestone, Smylie and Vaillancourt16 Clearly, there are other important factors that need to be examined.
Several limitations characterize our study. First and most importantly, we were only able to separate the two populations based on patients’ status numbers on the charts. This creates a potential selection bias. Specifically, there is a possibility that First Nations, Métis, and Inuit patients, who would self-identify as First Nations, were included in the non-First Nations group, diminishing our ability to recognize existent differences in ED treatment. There was no way around this limitation at the time of the study; however, SPH is now adding the ability to self-identify at arrival. This is of value because it will potentially allow us to better separate the two populations into groups that are respectively more homogenous in regard to social factors impacting health; although, this approach is also not without possible misclassification. Secondly, because this was a retrospective study, inaccuracies and omissions in documentation likely affected the calculated time intervals, although it is expected that these differences would have influenced both subgroup assessments similarly. A third limitation is that a diagnosis could not be considered as a confounder, although the similarity of sensitive analysis findings is somewhat reassuring. However, if First Nations patients were to actually require increased levels of care due to more concerning underlying conditions, equal care will not ensure appropriate care. Fourthly, we examined only one chief complaint of abdominal pain. A more complete overview of ED quality requires examination of a range of priority conditions, yielding a more comprehensive picture. Finally, every observation was assumed to be independent from one another, but it is possible that some patients had the same experience because they were seen on the same shift or they saw the same doctor.
Quality improvement
Because this was a quality improvement project, our goal was to use its findings to improve the health services offered in our health region. However, as our results suggested no clear difference between the groups in how tests, analgesia, and the basics of care are carried out, there were no priority recommendations that could be operationalized immediately. However, this does not mean that the analysis of healthcare equality stops here. We are currently planning a qualitative study of First Nation perspectives of care, aiming to identify both perceived difficulties in the ED and the attitudes of healthcare providers. This may also help us understand our finding of more incomplete visits in the Status First Nations group. This project will be designed and implemented in collaboration with local First Nations and Métis Health authorities.
CONCLUSION
Status First Nations patients presenting to the ED with a CTAS 3 score and abdominal pain were not found to differ substantially in time to care through the allotted variables of time to doctor (primary outcome), time to analgesia, LOS, bloodwork, imaging, specialist consultation, and final disposition. Additional studies, both quantitative and qualitative, will be necessary to further understand how to mitigate the subjective sense of care inequality that has been expressed among First Nations patients in our emergency rooms.
Acknowledgements
Thanks to the University of Saskatchewan and College of Medicine. Appreciation is also expressed to the First Nations and Métis Health Council for their guidance, which includes Gabe Lafond, Tania Lafontaine, and Valerie McLeod. A special thanks to Aimee Goss from Health Record Services for her help with the chart review. Further acknowledgement is directed towards Dr. Rhonda Bryce from the Clinical Research Support Unit. Thank you to Dr. Phil Davis, Dr. Brent Thoma, and Dr. Thomas Graham for providing insight and feedback.
Financial support
This study was funded as a Dean’s Summer Research Project, College of Medicine, University of Saskatchewan for a total of $5,800. This money has been used to pay the lead author for the entirety of the project, which consisted of obtaining ethics approval, collecting medical charts, extracting and comparing data, and writing the manuscript.
Competing interests
JS (regional department head), MAS-H, and TOO are all physicians in Saskatoon emergency departments.






