In 1997, Dr Robert Kendell, then President of the Royal College of Psychiatrists, published a paper in this journal describing findings from a survey into the early retirement of consultant psychiatrists (Reference Kendell and PearceKendell & Pearce, 1997). The survey found that many factors contributed to early retirement, but the most important was the previous (Conservative) government’s National Health Service (NHS) reforms - rated higher than ill health, a wish to devote more time to other interests, and bed closures. Increasing bureaucracy and paperwork also scored highly.
In the summer of 2001, the Department of Health, still concerned about the large number of vacant consultant posts, commissioned the Royal College of Psychiatrists’ Research Unit to once again investigate retirement in consultant psychiatrists, as part of a wider programme of workforce planning research (Reference ApplebyAppleby, 2002). To this end, a questionnaire survey was used to gather data on current consultants’ retirement intentions, and the factors influencing their decisions.
Method
A focus group of consultants over 50 years old helped to develop the content of the questionnaire. College databases were used to identify all 1438 consultant psychiatrists over the age of 50 years practising in the UK, who were then sent a questionnaire divided into the following sections: ‘ About you’, ‘About your current post’ and ‘ Factors affecting your career intentions’. A final section asked respondents to specify, in their own words, what changes in their current post would encourage them to stay. The latter qualitative data were subjected to a content analysis: a member of the research team read through all the responses, extracting themes and creating a coding frame. When the frame was finalised (in negotiation with another member of the team), the researcher re-read the responses and coded them. Since most respondents made more than one statement, these were treated as separate responses.
Results
A total of 848 questionnaires were returned, some of which were blank; 13 (1.5%) respondents indicated that they were not yet 50 years old. The latter were not included in the calculations; thus 835 questionnaires were analysed, giving an adjusted response rate of 59% (835/1416).
Of the sample, 589 (71%) were men, and 137 (16%) were flexibly trained. The mean age of the sample was 56 years (s.d. 5.34), and the mean age at which the MRCPsych was gained was 33 years (s.d. 5.11). Over a third of respondents (289) had already retired; their responses for their last pre-retirement post are included in subsequent analyses. Over a fifth of respondents (187) reported that they had no firm plans for retirement. For those who gave an indication, the mean age of intended retirement was 60 years (range 48-78). The data showed that 496 respondents (59%) indicated that they would take (or had already taken) early retirement.
Asked to clarify the status of their current (or most recent) post, 616 (76%) reported that their post was full-time, 144 (18%) part-time, and 51 (6%) maximum part-time. Substantive posts dominated the sample (681, 84%); 43 (5%) were honorary posts, 11 (1%) fixed term, 62 (7%) locum and 25 (3%) other status. Nearly three-quarters (661; 72%) of respondents reported that they had Mental Health Officer (MHO) status; 201 (24%) held an academic post, and 161 (19%) an executive post (such as medical director). The number of NHS sessions worked varied from 0 to 14 (mean 9).
Respondents were given a list of factors that might influence their decision to retire or to remain in post, and were asked to rate how great an influence each factor might exert on their decision. The rating scale ran from 1 (little or no influence) to 5 (great influence). The mean was calculated for each of these rating variables, which were then ranked. Table 1 lists the factors encouraging staying in post, and Table 2 those encouraging retirement. Overall, 71% of respondents indicated that they would wish to work after retirement in some capacity (for example locum or court work).
Table 1. Factors encouraging psychiatrists to stay in post

| Rank | Factor | Score Mean (s.d.) |
|---|---|---|
| 1 | I enjoy my work | 4.01 (1.24) |
| 2 | I have a good team around me | 3.83 (1.19) |
| 3 | Money | 3.24 (1.44) |
| 4 | Too early to retire | 2.89 (1.50) |
| 5 | Departure would leave team understaffed | 2.45 (1.41) |
Table 2. Factors encouraging psychiatrists to retire
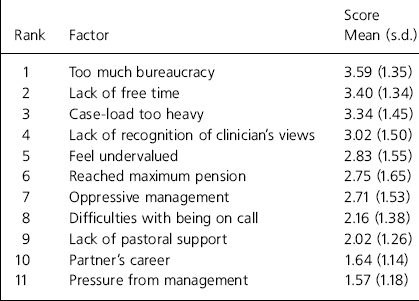
| Rank | Factor | Score Mean (s.d.) |
|---|---|---|
| 1 | Too much bureaucracy | 3.59 (1.35) |
| 2 | Lack of free time | 3.40 (1.34) |
| 3 | Case-load too heavy | 3.34 (1.45) |
| 4 | Lack of recognition of clinician’s views | 3.02 (1.50) |
| 5 | Feel undervalued | 2.83 (1.55) |
| 6 | Reached maximum pension | 2.75 (1.65) |
| 7 | Oppressive management | 2.71 (1.53) |
| 8 | Difficulties with being on call | 2.16 (1.38) |
| 9 | Lack of pastoral support | 2.02 (1.26) |
| 10 | Partner’s career | 1.64 (1.14) |
| 11 | Pressure from management | 1.57 (1.18) |
Analysis of variance was used to identify factors most likely to influence early retirement. Men intended to (or did) retire slightly later than women (mean retirement age: men 59.99 years, s.d. 4.37; women 59.08 years, s.d. 3.57; F=12.66, d.f.=1, P<0.01), as did those who trained flexibly (mean retirement age 60.18 years, s.d. 4.28) compared with those whose training had been full-time (mean retirement age 59.62 years, s.d. 4.14; F=9.237, d.f.=1, P<0.01), although having MHO status had a more substantial effect upon intended and actual retirement: mean age 59.14 years (s.d. 3.70) for those with MHO status compared with 62.88 years (s.d. 5.00) for those without (F=55.245, d.f.=1, P<0.01). Although no statistically significant interaction was observed, the data did suggest that flexibly trained men anticipated a later retirement age than all other groups, with a mean retirement age of 62.32 years (s.d. 5.53).
One free response question on the survey form asked the respondents what changes in their current post would encourage them to stay. It was answered by 538 respondents yielding 1078 individual responses. The themes on the coding frame were divided into those primarily concerning the service in which the respondent worked, and those that affected the respondent personally. The most commonly found themes are shown in Table 3 (service themes) and Table 4 (personal themes). Few respondents (27; 3%) indicated that nothing would encourage them to remain in post, and still fewer (12; 1%) indicated that they were completely satisfied with their work and would change nothing.
Table 3. Changes that would encourage retention: service themes
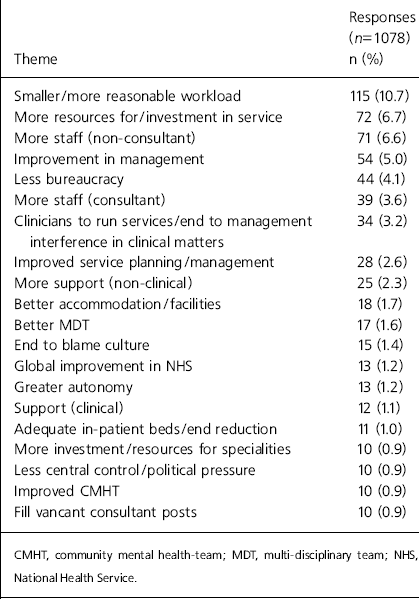
| Theme | Responses (n=1078) n (%) |
|---|---|
| Smaller/more reasonable workload | 115 (10.7) |
| More resources for/investment in service | 72 (6.7) |
| More staff (non-consultant) | 71 (6.6) |
| Improvement in management | 54 (5.0) |
| Less bureaucracy | 44 (4.1) |
| More staff (consultant) | 39 (3.6) |
| Clinicians to run services/end to management interference in clinical matters | 34 (3.2) |
| Improved service planning/management | 28 (2.6) |
| More support (non-clinical) | 25 (2.3) |
| Better accommodation/facilities | 18 (1.7) |
| Better MDT | 17 (1.6) |
| End to blame culture | 15 (1.4) |
| Global improvement in NHS | 13 (1.2) |
| Greater autonomy | 13 (1.2) |
| Support (clinical) | 12 (1.1) |
| Adequate in-patient beds/end reduction | 11 (1.0) |
| More investment/resources for specialities | 10 (0.9) |
| Less central control/political pressure | 10 (0.9) |
| Improved CMHT | 10 (0.9) |
| Fill vancant consultant posts | 10 (0.9) |
Table 4. Changes that would encourage retention: personal themes
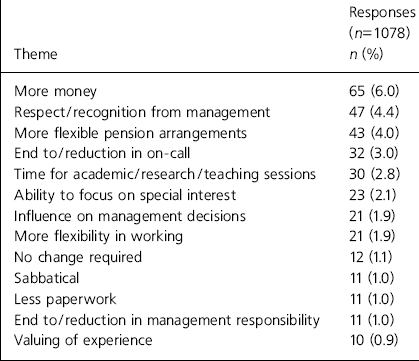
| Theme | Responses (n=1078) n (%) |
|---|---|
| More money | 65 (6.0) |
| Respect/recognition from management | 47 (4.4) |
| More flexible pension arrangements | 43 (4.0) |
| End to/reduction in on-call | 32 (3.0) |
| Time for academic/research/teaching sessions | 30 (2.8) |
| Ability to focus on special interest | 23 (2.1) |
| Influence on management decisions | 21 (1.9) |
| More flexibility in working | 21 (1.9) |
| No change required | 12 (1.1) |
| Sabbatical | 11 (1.0) |
| Less paperwork | 11 (1.0) |
| End to/reduction in management responsibility | 11 (1.0) |
| Valuing of experience | 10 (0.9) |
Discussion
A number of older consultants are choosing to take early retirement, and the reasons are complex, multi-dimensional and highly individual. Factors are pulling in opposite directions: some towards encouraging retirement (too much bureaucracy, lack of free time and workload), some towards remaining in post (enjoyment of psychiatry, having a good team, and money). Changes that would encourage consultants to remain in post echoed these findings: older psychiatrists want smaller case-loads, more resources, more (non-consultant) staff, more money and better management.
This study supports the previous survey by Kendell & Pearce (Reference Kendell and Pearce1997) in so far as sizeable numbers of consultant psychiatrists consider - and take - early retirement, with a mean intended (or actual) age of retirement of 60 years. Apart from the role of the Conservative government’s changes to the NHS, the reasons given for early retirement overlap at least in part with the previous survey. These figures continue to represent significant losses from the profession and clearly contribute to the current shortage of consultant psychiatrists.
The majority of respondents reported an intention to continue working in some capacity following retirement, many in a locum position, which theoretically would allow the enjoyable tasks of psychiatry to be maintained while obviating the onerous aspects. When viewed in conjunction with high locum fees and a pension boosted by MHO status, the logic of this course of action is undeniable.
The data from our survey show that of our sample of consultants over 50 years old, 97.7% intend to be (or are) working at the age of 55 years. By the age of 65 years, only 12% will still be working. Extrapolating these numbers to the population of all consultants over 55 years old (1438 individuals), this equates to 1404 working at age 55 years and 259 still working at age 65 years, a gradual and cumulative loss of 1145 consultants in this 10-year period. Assuming a linear fall, this equates to an overall loss of 5725 consultant years. If we assume a potential 30-year career as a consultant psychiatrist (35–65 years of age), this figure is equivalent to a reduction in overall consultant numbers of 191, approximately a 5% reduction in the total consultant workforce (the estimated total is 3865, taken from Royal College of Psychiatrists records). If the NHS pays to fill these 191 posts with locums, and assuming the average additional cost of a locum consultant is £50 000 more than the cost of a substantive appointment, the NHS is losing at the very least an extra £10 million per year as a result of early retirement. The figure could well be much higher than this.
These findings represent significant losses from the profession, not just in terms of numbers, but also in terms of experience and skill. It is hard to escape the possibility that as vacancies increase, so consultants will feel more overburdened and overworked, leading to an increase in early retirement, with the risk that those remaining feel more overburdened still. With the perverse incentive created by MHO status and the high fees paid to locums, early retirement will become ever more attractive. Redesigning consultant roles and improving resources and supports, especially for older consultants, may prove to be cost-effective.







eLetters
No eLetters have been published for this article.