People with schizophrenia show cognitive impairments on most cognitive domains from the very early phases of the disease (Reference Gonzalez-Blanch, Crespo-Facorro and Alvarez-JimenezGonzalez-Blanch et al, 2007). Since cognitive functions are not completely independent from each other, it is still unclear whether this generalised disturbed cognitive profile is a reflection of a widespread dysfunction or a consequence of a primary deficit in a core cognitive function. Speed of processing is a core cognitive process underlying cognitive dysfunction in normal ageing (Reference SalthouseSalthouse, 1993), traumatic brain injury (Reference Ríos, Periáńez and Munoz-CéspedesRíos et al, 2004), depression (Reference Egeland, Rund and SundetEgeland et al, 2003) and Parkinson's disease (Reference Rogers, Lees and SmithRogers et al, 1987). Deficits in speed of processing may determine impairments of declarative memory (Brébion et al, Reference Brebion, Amador and Smith1998, Reference Brebion, Smith and Gorman2000; Reference Holthausen, Wiersma and SitskoornHolthausen et al, 2003) or working memory (Reference Hartman, Steketee and SilvaHartman et al, 2002) in people with chronic schizophrenia. However, it remains to be elucidated whether these associations are already present in the early stages of schizophrenia. The aim of this study was to investigate the contribution of speed of processing to the cognitive deficits observed in a representative large sample with first-episode schizophrenia.
METHOD
Study setting
The data for these analyses were taken from a large epidemiological and longitudinal (3-year) intervention programme of first-episode psychosis (PAFIP) carried out in Cantabria, Spain (Reference Crespo-Facorro, Perez-Iglesias and Ramirez-BonillaCrespo-Facorro et al, 2006). The study was conducted at the out-patient clinic and the in-patient unit of the University Hospital Marques de Valdecilla in Santander (Cantabria). The study was designed and directed by B.C.-F. and J.L.V.-B., conformed to international standards for research ethics and was approved by the local institutional review board.
Participants
From February 2001 to October 2005 all referrals to PAFIP were screened for the following eligibility criteria: (a) aged 15–60 years; (b) meeting DSM–IV criteria (American Psychiatric Association, 1994) for a principal diagnosis of schizophrenia, schizophreniform disorder, schizoaffective disorder, brief reactive psychosis, schizotypal personality disorder or psychosis not otherwise specified; (c) no prior treatment with antipsychotic medication or, if previously treated, a total lifetime of adequate antipsychotic treatment of less than 6 weeks. Patients meeting these criteria and their families provided written informed consent for inclusion in the PAFIP programme. The diagnoses were confirmed using the Structured Clinical Interview for DSM–IV (SCID–I; Reference First, Spitzer and GibbonFirst et al, 2001) by an expert psychiatrist 6 months after the initial contact. Only those people with mental retardation (DSM–IV criteria) or drug dependence (DSM–IV criteria) were excluded.
Out of 174 consecutive admissions that met the criteria for enrolment, 43 people declined to participate in the study. A final sample of 131 patients (85 males, 46 females) completed the baseline neurocognitive assessment. No significant differences between patients who did and did not complete cognitive assessment were found in relevant variables such as age, gender, duration of illness, or clinical severity. From these 131 patients, only 126 with a final diagnosis of schizophrenia, schizophreniform disorder, brief psychotic disorder and psychosis not otherwise specified at 6 months by SCID–I were considered for this study.
At the time of the cognitive evaluation 42 patients were taking conventional (haloperidol) and 84 atypical antipsychotics (41 olanzapine and 43 risperidone). Clinical symptoms were rated using the Scale for the Assessment of Negative Symptoms (SANS; Reference AndreasenAndreasen, 1983) and the Scale for the Assessment of Positive Symptoms (SAPS; Reference AndreasenAndreasen, 1984). Duration of untreated illness was defined as the time from the first non-specific symptoms related to psychosis (for such a symptom to be considered, there should be no return to the previous stable level of functioning) to the initiation of adequate antipsychotic drug treatment. Duration of untreated psychosis was defined as the time from the first continuous (present most of the time) psychotic symptom to initiation of adequate antipsychotic drug treatment.
A sample of healthy controls (n=28) recruited from the local area through advertisement was submitted to the same cognitive assessment. Antecedents of psychiatric disturbance in the control group were excluded by means of the Comprehensive Assessment of Symptoms and History (CASH; Reference Andreasen, Flaum and ArndtAndreasen et al, 1992).
Neuropsychological assessment
Patients and controls were submitted to a broad neuropsychological battery. This was carried out once clinical stability had been achieved in order to maximise collaboration. This occurred typically at a mean of 10.72 (s.d.=3.97) weeks after intake into the programme.
In order to reduce type I error on statistical analyses, variables obtained from neuropsychological tests were grouped into cognitive domains following results from previous factor analysis. A detailed description of the cognitive battery employed, the procedure for factor analysis and the final composition of cognitive factors is provided elsewhere (Reference Gonzalez-Blanch, Crespo-Facorro and Alvarez-JimenezGonzalez-Blanch et al, 2007).
From eight basic cognitive domains, we decided to examine those key cognitive dimensions with a more pronounced impairment (around 1 s.d. below healthy controls): executive functions, verbal memory, attention and motor dexterity were considered as dependent variables.
The Digit Symbol Substitution Test from the WAIS–III battery (Reference WeschlerWeschler, 1999) was employed as a measure of speed of processing (Reference SalthouseSalthouse, 1992; Reference Brebion, Amador and SmithBrébion et al, 1998) to be covaried on statistical analyses. This test was included in the executive functions dimension on previous factor analysis. Since a variable should not be used as a covariate and a dependent variable at the same time, we chose to examine tests related to executive function independently. Span of Backward Digits Test (Reference WeschlerWeschler, 1999), Trail-Making Test Part B (TMT–B; Reference LezakLezak, 1995) and a fluency test (FAS; Reference LezakLezak, 1995) were used as representative of working memory and executive functions.
Verbal memory was assessed using the Rey Auditory Verbal Learning Test (RAVLT; Reference ReyRey, 1964) immediate memory span, total learning, recall following short and long delay periods, and recognition. Motor dexterity was assessed using the grooved pegboard (both hands) and sustained attention/vigilance the Continuous Performance Test–Degraded Stimulus (CPT–DS; Reference Cegalis and BowlinCegalis & Bowlin, 1991) hits and reaction time and Brief Test of Attention (BTA; Reference Schretlen, Bobholz and BrandtSchretlen et al, 1996). The vocabulary test from WAIS–III was used to control for premorbid IQ (Reference LezakLezak, 1995).
Statistical analysis
The independent samples t-test was used to compare patients and controls on age, years of education and premorbid IQ. The χ2 test was used to compare gender distribution on both samples. Univariate analysis of covariance (ANCOVA) was used to compare both groups on each of the dependent variables separately. Univariate instead of multivariate ANCOVA was used because of missing data. This caveat precluded the use of multivariate testing since it involved an important loss of sample size. However, we considered the number of dependent variables small enough that errors derived from multiple comparisons would not be significant. Two sets of ANCOVA were carried out. On the first only those socio-demographic variables that differed between patients and controls were covaried. On the second results of the Digit Symbol Substitution Test (speed of processing) were also included as a covariate.
RESULTS
Sample
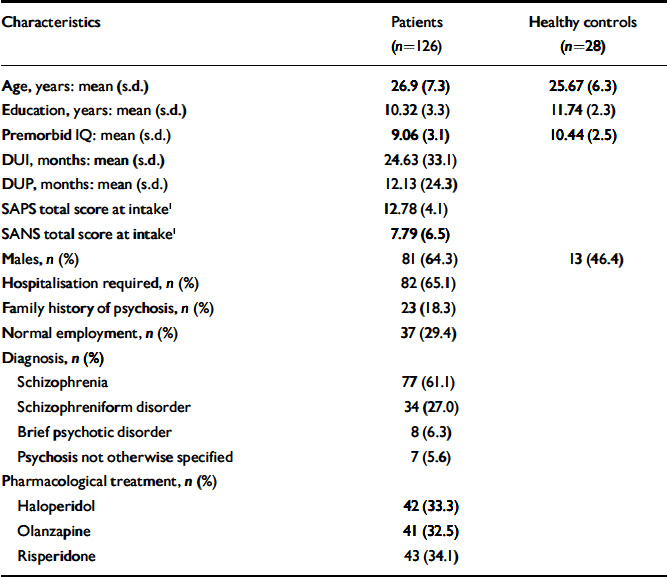
The socio-demographic and clinical characteristics of patients and controls are presented in Table 1. The two groups did not differ on age (t=0.63, d.f.=148, P=0.53) or gender distribution (χ2=3.07, P=0.08), although there was a trend-level difference. Patients and healthy controls differed in terms of years of education (t=–2.15, d.f.=148, P=0.03) and premorbid IQ (t=–2.27, d.f.=148, P=0.03). Therefore on the subsequent analysis, gender, years of education and premorbid IQ were always included as covariates.
Table 1 Socio-demographic and clinical characteristics of patients with a first episode of non-affective psychosis and healthy controls
| Characteristics | Patients (n=126) | Healthy controls (n=28) |
|---|---|---|
| Age, years: mean (s.d.) | 26.9 (7.3) | 25.67 (6.3) |
| Education, years: mean (s.d.) | 10.32 (3.3) | 11.74 (2.3) |
| Premorbid IQ: mean (s.d.) | 9.06 (3.1) | 10.44 (2.5) |
| DUI, months: mean (s.d.) | 24.63 (33.1) | |
| DUP, months: mean (s.d.) | 12.13 (24.3) | |
| SAPS total score at intake1 | 12.78 (4.1) | |
| SANS total score at intake1 | 7.79 (6.5) | |
| Males, n (%) | 81 (64.3) | 13 (46.4) |
| Hospitalisation required, n (%) | 82 (65.1) | |
| Family history of psychosis, n (%) | 23 (18.3) | |
| Normal employment, n (%) | 37 (29.4) | |
| Diagnosis, n (%) | ||
| Schizophrenia | 77 (61.1) | |
| Schizophreniform disorder | 34 (27.0) | |
| Brief psychotic disorder | 8 (6.3) | |
| Psychosis not otherwise specified | 7 (5.6) | |
| Pharmacological treatment, n (%) | ||
| Haloperidol | 42 (33.3) | |
| Olanzapine | 41 (32.5) | |
| Risperidone | 43 (34.1) |
There were no differences in socio-demographic and cognitive characteristics when patients with schizophrenia and with other psychoses were compared (data not shown).
Cognitive performance
Patients and controls differed greatly on performance on the Digit Symbol Substitution Test (t=–7.51, d.f.=148, P<0.001). This significant difference remained after controlling for gender, years of education and premorbid IQ (ANCOVA: F=52.40, P<0.001) and for all socio-demographic and cognitive variables together (ANCOVA: F=16.552, P<0.001).
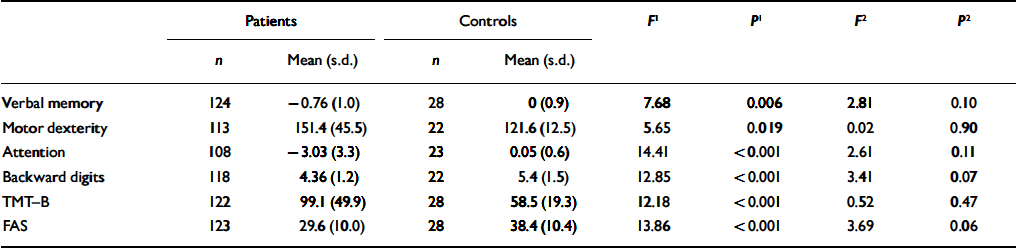
Differences in cognitive performance between patients and controls remained when gender, education and premorbid IQ were included as covariates. After inclusion of the speed of processing as an additional covariate, none of the differences reached the established significance. Table 2 shows the results of ANCOVA before and after controlling for speed of processing.
Table 2 Cognitive functioning in patients and healthy controls with and without controlling for speed of processing
| Patients | Controls | F 1 | P 1 | F 2 | P 2 | |||
|---|---|---|---|---|---|---|---|---|
| n | Mean (s.d.) | n | Mean (s.d.) | |||||
| Verbal memory | 124 | -0.76 (1.0) | 28 | 0 (0.9) | 7.68 | 0.006 | 2.81 | 0.10 |
| Motor dexterity | 113 | 151.4 (45.5) | 22 | 121.6 (12.5) | 5.65 | 0.019 | 0.02 | 0.90 |
| Attention | 108 | -3.03 (3.3) | 23 | 0.05 (0.6) | 14.41 | <0.001 | 2.61 | 0.11 |
| Backward digits | 118 | 4.36 (1.2) | 22 | 5.4 (1.5) | 12.85 | <0.001 | 3.41 | 0.07 |
| TMT—B | 122 | 99.1 (49.9) | 28 | 58.5 (19.3) | 12.18 | <0.001 | 0.52 | 0.47 |
| FAS | 123 | 29.6 (10.0) | 28 | 38.4 (10.4) | 13.86 | <0.001 | 3.69 | 0.06 |
DISCUSSION
The current study was driven by the hypothesis that deficits in cognition in schizophrenia may be determined by a slower speed of processing of cognitive performance. We compared the cognitive performance of people with schizophrenia and controls before and after controlling for the effect of speed of information processing on cognitive functioning. Interestingly, the results showed that when the influence of speed of processing was removed the cognitive deficits observed in people with first-episode schizophrenia disappeared. Moreover, the significant differences between patients and healthy volunteers in the performance of the Digit Symbol Substitution Test reveal that speed of processing is severely impaired in the early phases of psychosis. Taken together these results suggest that speed of information processing may be a core cognitive deficit in schizophrenia and might mediate a broader diversity of cognitive disturbances.
Our results confirm and extend previous findings in chronic schizophrenia on the influence of speed of information processing on memory and working memory (Brébion et al, Reference Brebion, Amador and Smith1998, Reference Brebion, Smith and Gorman2000; Reference Hartman, Steketee and SilvaHartman et al, 2002). We have also found that a more diverse range of cognitive functions, including attention, motor dexterity and executive functions, are also influenced by speed of processing, and that this is already evident during the early phases of the disease. It has been proposed that age-related cognitive decline might be associated with a decrease in the speed with which many processing operations can be executed and that this reduction leads to impairments in cognitive functioning (Reference SalthouseSalthouse, 1996).
Andreasen and colleagues (Reference Andreasen, Paradiso and O'Leary1998) proposed the cognitive dysmetria model in schizophrenia. This posits that a neural misconnection in cortical–cerebellar–thalamic–cortical circuitry in people with schizophrenia leads to an impairment in synchrony or the smooth coordination of mental processes. When synchrony is impaired, there is cognitive dysmetria, and the impairment in this basic cognitive process defines the phenotype of schizophrenia and produces its diversity of symptoms. We hypothesise that processing speed is one ‘candidate cognitive dysfunction’ that could explain the myriad symptoms of schizophrenia.
Neuroimaging studies in multiple sclerosis (Reference Sanfilipo, Benedict and Weinstock-GuttmanSanfilipo et al, 2006), stroke (Reference Jokinen, Kalska and MantylaJokinen et al, 2005) and normal ageing (Reference Gunning-Dixon and RazGunning-Dixon & Raz, 2000) have demonstrated that deficits in speed of processing are associated with abnormalities in cerebral white matter. It is noteworthy that abnormalities in white matter have also been related to deficits in processing speed in schizophrenia (Reference Antonova, Kumari and MorrisAntonova et al, 2005).
In accordance with the cognitive dysmetria hypothesis, a deficit in speed of processing in schizophrenia might reflect the disruption of neural activation transmission owing to white matter alteration. This might secondarily affect higher-order processing, leading to functional disturbances. Cognitive impairment in schizophrenia has great relevance for the evolution of the illness, especially the level of general functionality and autonomy that patients eventually achieve (Reference GreenGreen, 1996). This emphasises the potential value of addressing cognitive dysfunction as a primary target of therapeutic intervention. Cognitive remediation in schizophrenia has already proved to be valuable in terms of amelioration of problems with social functioning (Reference Wykes, Reeder and WilliamsWykes et al, 2003). If our hypothesis proves to be true, pharmacological or neurorehabilitation-based therapeutic approaches aimed at remediating specific cognitive deficits (e.g. memory or executive functions) should take into account the effects of an impaired speed of information processing which might may be understood as a core cognitive deficit.
One of the limitations of this study might be the validity of the test used to measure speed of processing. Although the Digit Symbol Substitution Test has been traditionally used as a measure of processing speed (Salthouse, Reference Salthouse1992, Reference Salthouse1993; Reference Lindenberger, Mayr and KlieglLindenberger et al, 1993; Reference Brebion, Amador and SmithBrébion et al, 1998), it might also be measuring a large number of other cognitive processes. This limitation applies to most of the neuropsychological tasks and emphasises the need for more specific cognitive tasks for research purposes. A second limitation of this study is that patients had been treated prior to cognitive evaluation. Although treatment was minimal, antipsychotics might have produced changes in cognition. If medication had some particular significant effect on speed of information processing this might have biased the interpretation of our results. However, to our knowledge there are no reports of a specific effect of antipsychotics on speed of processing. Therefore, the significant relationship between cognitive functioning and processing speed is unlikely to be due to medication.
In conclusion, we suggest that speed of processing might be a core cognitive function in schizophrenia. Thus, cognitive deficits described in people with schizophrenia from the very early stages of the illness might be determined by a slower speed of information processing. Our findings provide further support for recent theories of a neural basis of schizophrenia, such as the cognitive dysmetria theory, and suggest new strategies for neurorehabilitation research.
Acknowledgements
We thank the PAFIP researchers who helped with data collection and during the investigations and the study participants and their families.
This study was performed under the grant support of: Instituto de Salud Carlos III, FIS 00/3095, 01/3129, PI020499 and SENY Fundació Research Grant CI 2005-0308007, 0308007, Fundación Marqués de Valdecilla A/02/07.





eLetters
No eLetters have been published for this article.