Compelling evidence has accumulated in the past 20 years indicating that people with severe mental illness – and most particularly those with schizophrenia – are at increased risk (compared with the general population) of committing violent crime (Reference Hodgins, Mednick and BrennanHodgins et al, 1996). The association between schizophrenic disorder and aggressive behaviour is a robust finding: it has been reported by several independent research groups working in industrialised countries (Reference Swanson, Holzer and GanjuSwanson et al, 1990; Reference Arseneault, Moffitt and CaspiArseneault et al, 2000; Reference Brennan, Mednick and HodginsBrennan et al, 2000) and in low- to middle-income countries (Reference Vollavka, Laska and BakerVolavka et al, 1997) with distinctly different cultures, health, social service and criminal justice systems, in studies examining different cohorts and samples using various experimental designs including prospective, longitudinal investigations of birth cohorts (Reference Tiihonen, Isohanni and RäsänenTiihonen et al, 1997; Reference Arseneault, Moffitt and CaspiArseneault et al, 2000; Reference Brennan, Mednick and HodginsBrennan et al, 2000) and population cohorts (Reference Wallace, Mullen and BurgessWallace et al, 2004), follow-up studies comparing patients and their neighbours (Reference BelfrageBelfrage, 1998), random samples of incarcerated offenders (Reference Fazel and DaneshFazel & Danesh, 2002) and complete cohorts of homicide offenders (Reference Erb, Hodgins and FreeseErb et al, 2001). These findings reflect enormous suffering for both victims and perpetrators and a significant financial burden for society. Further, evidence also shows that people with severe mental illness are more likely than others to be the victims of physical assault (Reference Teplin, McClelland and AbramTeplin et al, 2005).
As this evidence has accumulated, there have been three important developments within the UK. One, official mental health policy has remained mute on the topic and has failed to acknowledge the evidence (Department of Health, 1999; National Collaborating Centre for Mental Health, 2003). Two, the number of forensic psychiatric beds has dramatically increased (Reference Priebe, Badesconyi and FiorittiPriebe et al, 2005). Three, evidence has emerged showing that most of the patients admitted to forensic in-patient services are men with schizophrenia with long histories of treatment in general adult services and of criminality (Reference Hodgins and Müller-IsbernerHodgins & Müller-Isberner, 2004; Reference Meltzer, Tom and BrughaMeltzer et al, 2004). In an effort to shed light on this situation, we examined aggressive behaviour, victimisation and criminality among people with severe mental illness receiving in-patient treatment from general adult services and compared the rates with those from other samples of in-patients and out-patients with severe mental illness and general population samples.
METHOD
Between July 2004 and April 2005 we approached all patients (n=325) on general adult wards of an inner-city mental health trust which provides service to a geographic catchment area of 1 105 200 inhabitants, to participate in our study. Patients with the following characteristics were invited to participate: legal resident; able to communicate in English; 18–65 years old; and a principal diagnosis of schizophrenia, schizoaffective disorder, bipolar disorder, major depression or alcohol- or drug-induced psychosis. Of the 325 patients, 49 did not meet the inclusion criteria: 21 had other diagnoses, 18 were not UK residents, 8 were too old or too young and 2 were mute. Of the remaining 276 patients, 21 (7.6%) were discharged before they could be invited to participate, 50 (18.1%) refused to participate and 205 consented. All 205 completed an interview, authorised their keyworker to provide information about them, and authorised access to their medical and criminal records. Each patient was counted only once.
The research team arranged with each ward to assess all patients during a 2-week period. Upon arrival on the ward, the team made a census of the patients. All patients meeting the eligibility criteria were invited to participate. If the patient consented, researchers read the patient's file, conducted the interview with the patient and then interviewed the keyworker. Patients too ill to consent were contacted when symptoms had remitted. Family members were contacted, most often by telephone, and if they agreed, the interview was completed. It quickly became apparent, however, that the majority of patients did not know how to contact their parents or elder siblings. Only two-thirds of the patients named an individual who they thought could provide information about them when they were children, and in only a fifth of cases was such a person found and interviewed. For another quarter of the patients a collateral was interviewed about the patient's aggressive behaviour and victimisation during the 6 months prior to the interview. Information was subsequently extracted from psychiatric and criminal records.
Socio-demographic information was collected from patients and files. Histories of psychiatric treatment were documented from medical files. The interview with the patient included two modules (Conduct Disorder and Antisocial Personality Disorder) of the Structured Clinical Interview for DSM–IV (Reference First, Spitzer and GibbonFirst et al, 1996), and self-reports of aggressive behaviour using the MacArthur Community Violence Interview (Reference Steadman, Mulvey and MonahanSteadman et al, 1998) and of substance misuse using the Alcohol Use Disorders Identification Test (AUDIT; Reference Saunders, Aasland and BaborSaunders et al, 1993) and the Drug Use Disorders Identification Test (DUDIT; Reference Berman, Bergman and PalmstiernaBerman et al, 2005). Interviews also included measures of needs and insight not discussed in this report. Interviews were conducted by a consultant forensic psychiatrist, a specialist registrar in forensic psychiatry and two research workers with MSc degrees, one in psychology and one in criminology. Interviewers were trained to use each instrument.
As recommended, alcohol misuse was defined as an AUDIT score of 8 for men and 6 for women, alcohol dependence as an AUDIT score of 16, drug misuse as a DUDIT score of 6 for men and 2 for women, and drug dependence as a DUDIT score of 25 for men and women (Reference Saunders, Aasland and BaborSaunders et al, 1993; Reference Berman, Bergman and PalmstiernaBerman et al, 2005).
Serious assaults over the life span were defined as killing someone; injuring someone so seriously that the person required in-patient hospital care; or using a gun, knife or other object to injure someone. Any aggressive behaviour in the past 6 months was defined as throwing an object at someone; pushing, shoving, grabbing, slapping, kicking, biting, choking or hitting someone; trying to physically force someone to have sexual relations against his or her will; threatening someone with a knife, gun or other weapon; and any other violent act towards another person as reported by either the participant and/or the collateral. Serious violence in the past 6 months was defined as forcing someone to have sexual relations against his or her will; threatening someone with a weapon; using a gun or knife to injure someone; or inflicting any injury on another person. Victimisation was defined as having been a victim of any of the aggressive behaviours desribed above.
Criminal records were obtained from the Home Office Offenders Index and from the Police National Computer database. If an offence was recorded in only one of the databases, it was counted as an offence. Violent crimes were defined as crimes included in the Offenders Index categories ‘violence against the person’, ‘sexual offences’ minus prostitution-related offences, and ‘robbery’. All other crimes were defined as non-violent.
RESULTS
The characteristics of the participants are presented in Table 1. The patients were in their late thirties and more than a quarter of them had been born outside the UK. They were poorly educated. Almost half lived in their own homes and 14% of the men and 8% of the women were homeless. More than three-quarters of the men had a principal diagnosis of schizophrenia, whereas this was true of only 48% of the women. Only 43% of the men and 46% of the women did not misuse or abuse alcohol and/or illicit drugs. Most of the patients had a history of previous admissions. The current admission was involuntary for 63% of the men and 57% of the women. The average length of time on the ward prior to interview was 4 months.
Table 1 Characteristics of the patients

| Men (n=120)1 | Women (n=85)1 | |
|---|---|---|
| Age, years: mean (s.d.) | 37.2 (11.4) | 40.1 (13.3) |
| Born outside the UK, % (n) | 25 (30) | 33 (28) |
| Education, % (n) | ||
| GCSE | 42 (50) | 29 (25) |
| A-level or above | 23 (28) | 40 (34) |
| Accommodation, % (n) | ||
| Own home | 49 (58) | 59 (50) |
| Hostel | 14 (17) | 7 (6) |
| Parents' home | 11 (13) | 8 (7) |
| Homeless | 14 (17) | 8 (7) |
| Other | 12 (14) | 18 (15) |
| Have children, % (n) | 36 (43) | 46 (39) |
| Parents and/or siblings with | ||
| Mental illness, % (n) | 31 (37) | 40 (33) |
| At least one criminal conviction, % (n) | 23 (28) | 16 (13) |
| Principal diagnosis, % (n) | ||
| Schizophrenia | 77 (92) | 48 (41) |
| Schizoaffective disorder | 6 (7) | 13 (11) |
| Bipolar disorder | 13 (15) | 27 (23) |
| Depression | 4 (5) | 5 (4) |
| Other | 1 (1) | 7 (6) |
| Substance misuse, % (n) | ||
| No substance misuse | 43 (44) | 46 (39) |
| Alcohol misuse | 31 (32) | 38 (32) |
| Alcohol dependence | 15 (15) | 11 (9) |
| Drug misuse | 49 (50) | 39 (33) |
| Drug dependence | 13 (13) | 11 (9) |
| Prior in-patient treatment | ||
| Patients for whom this was the first admission, % (n) | 18 (13) | 15 (8) |
| Length of in-patient stay prior to interview, days: mean (s.d.) | 113.6 (144.6) | 116.6 (184.3) |
| Legal status at admission, % (n) | ||
| Involuntary admission | 63 (70) | 57 (45) |
| Civil sections | 54 (60) | 47 (37) |
| Forensic section | 6 (7) | 5 (4) |
| Police section | 3 (3) | 5 (4) |
Aggressive behaviour and victimisation
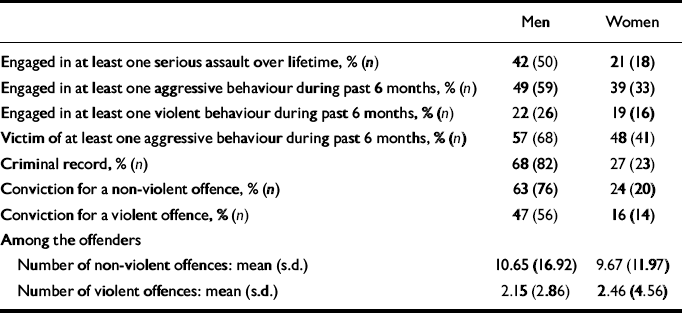
Aggressive behaviour towards others, victimisation and criminality were common and characterised more of the men than the women (Table 2). The risk of victimisation in the prior 6 months was increased (OR=6.57, 95% CI 3.51–12.28) by having engaged in aggressive behaviour in the same period. Foreign-born patients were no more likely than those born in the UK to have committed assaults, to have been the victim of assaults or to have a record of any crime, non-violent crime or violent crime.
Table 2 Violent acts, victimisation and criminal offending
| Men | Women | |
|---|---|---|
| Engaged in at least one serious assault over lifetime, % (n) | 42 (50) | 21 (18) |
| Engaged in at least one aggressive behaviour during past 6 months, % (n) | 49 (59) | 39 (33) |
| Engaged in at least one violent behaviour during past 6 months, % (n) | 22 (26) | 19 (16) |
| Victim of at least one aggressive behaviour during past 6 months, % (n) | 57 (68) | 48 (41) |
| Criminal record, % (n) | 68 (82) | 27 (23) |
| Conviction for a non-violent offence, % (n) | 63 (76) | 24 (20) |
| Conviction for a violent offence, % (n) | 47 (56) | 16 (14) |
| Among the offenders | ||
| Number of non-violent offences: mean (s.d.) | 10.65 (16.92) | 9.67 (11.97) |
| Number of violent offences: mean (s.d.) | 2.15 (2.86) | 2.46 (4.56) |
The prevalence of aggressive behaviour in this sample was compared with that documented for other samples of patients in studies using the same instrument and procedure to report on aggressive behaviour. The Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE) were conducted at 56 sites across the USA and included 1410 participants receiving outpatient treatment for schizophrenia who had experienced at least one prior episode (Reference Swanson, Swartz and Van DornSwanson et al, 2006). Compared with our UK in-patient sample, the participants in the CATIE study were similar in age (mean 40.5 years), more were living independently (77.6%), fewer were homeless (3.8%), many more had completed high school or college (74.6%) and fewer had received diagnoses of substance abuse and/or dependence (35.7%) and of misuse of alcohol and/or illicit drugs (24.5%). At baseline the CATIE trial participants reported on aggressive behaviour in the past 6 months. For the comparisons, we selected from our sample only patients with schizophrenia who had experienced at least one prior episode of illness. The men in our study had a four-fold increase in the odds of aggressive behaviour and a six-fold increase in the odds of serious violence compared with the men enrolled in the CATIE trial. Among the women, there was no significant difference in the proportions who engaged in any aggressive behaviour, but the women patients in the UK study had a six-fold increase in the odds of engaging in violence towards others.
The prevalence of aggressive behaviour in our sample was compared with that in an international sample of 62 general adult male patients with a similar range of diagnoses who participated in the Comparative Study of the Prevention of Crime and Violence by Mentally Ill Persons (CSMIV; Reference Hodgins and Müller-IsbernerHodgins & Müller-Isberner, 2004). This sample resembled the patients in the study reported here: all had been previously hospitalised at least once, they were of similar age (mean 36.8 years) and had a similar prevalence of lifetime abuse/dependence diagnoses. We found that the men in our study were seven times more likely to have engaged in aggressive behaviour and five times more likely to have engaged in violence towards others than general adult patients in this international sample (Table 3).
Table 3 Comparisons of the prevalence of aggressive behaviour among the study sample and other samples of patients with schizophrenia or schizoaffective disorder

| Any aggressive behaviour1 | Serious violence1 | |||
|---|---|---|---|---|
| Men | Women | Men | Women | |
| UK urban in-patient sample | ||||
| Prevalence, % | 51.5 | 30.8 | 21.2 | 15.4 |
| CATIE trial2 | ||||
| Prevalence, % | 18.5 | 21.0 | 3.8 | 3.0 |
| OR (95% CI) | 4.40 (2.70-7.17) | 1.47 (0.65-3.31) | 6.08 (3.13-1.81) | 5.91 (1.91-18.24) |
| CSMIV general adult patients living in the community3 | ||||
| Prevalence, % | 12.9 | 0.0 | 4.8 | 0.0 |
| OR (95% CI) | 7.17 (3.09-16.62) | NA | 5.30 (1.51-18.59) | NA |
| CSMIV forensic patients living in the community3 | ||||
| Prevalence | 8.3 | 0.0 | 3.7 | 0.0 |
| OR (95% CI) | 11.69 (5.32-25.70) | NA | 7.00 (2.31-21.22) | NA |
| US study of general adult in-patients with schizophrenia or schizoaffective disorder4 | ||||
| Prevalence, % | ||||
| In past 10 weeks | 40.2 | 43.6 | 14.2 | 18.0 |
| Adjusted to 26 weeks | 73.7 | 77.4 | 32.8 | 40.2 |
| OR (95% CI) | 0.38 (0.20-0.72) | 0.35 (0.17-0.66) | 0.55 (0.26-1.20) | 0.27 (0.09-0.73) |
The CSMIV also included a sample of 108 forensic patients living in the community with similar age, diagnoses and a higher prevalence of past abuse/dependence diagnoses. Compared with this forensic patient sample, the men in our study were 12 times more likely to have engaged in aggressive behaviour in the previous 6 months and seven times more likely to have engaged in violence.
Finally, the prevalence of aggressive behaviour in our sample was compared with that recorded for a US in-patient sample recruited in three sites for the MacArthur study (Reference Monahan, Steadman and SilverMonahan et al, 2001). The data from this study are publicly accessible. From the MacArthur study sample we selected only the patients with schizophrenia and schizoaffective disorder: these included 127 men and 78 women, aged on average 31.4 and 31.1 years respectively; 41% of the men and 38% of the women had comorbid diagnoses of abuse and/or dependence. The patients reported on aggressive behaviour using the same instrument and procedure as in our study but only for incidents occurring during the previous 10 weeks. Rates for the MacArthur study sample were therefore adjusted (formula available from the authors) to 26 weeks so as to be comparable with those from the UK sample. Both men and women in the UK in-patient sample reported significantly lower levels of aggressive behaviour and violence than the patients in the US sample (Table 3).
Crime
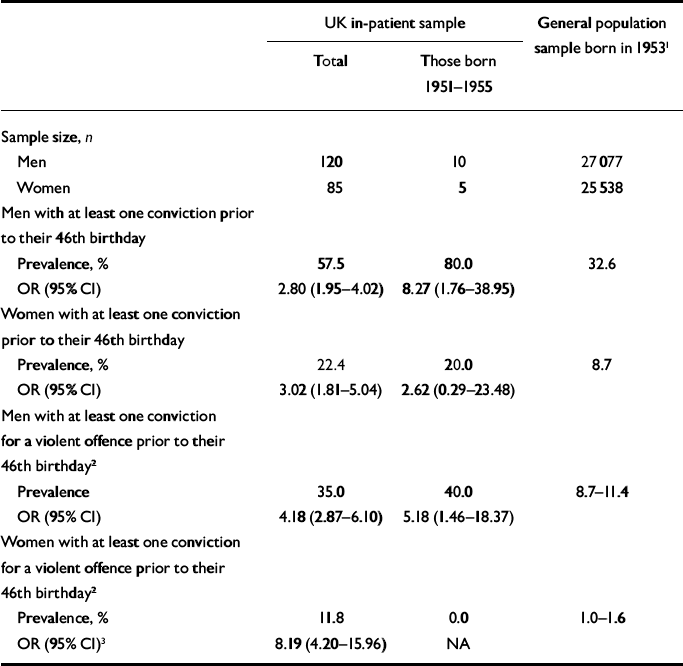
We compared the prevalence of offending and violent offending (as recorded in the Offenders Index) of the patients in the study with that reported for a UK general population sample born in four selected weeks in 1953 (Reference Prime, White and LirianoPrime et al, 2001). We made two comparisons, one for the patient sample as a whole and another that included only those patients born in the period 1951–1955. Male patients were between three and eight times more likely to have a record of criminal convictions and four to five times more likely to have a conviction for a violent offence than the men in the general population sample. The comparison of the entire female patient sample with the women in the general population sample showed a three-fold increase in risk of criminal convictions and an eight-fold increase in violent convictions among the female patients (Table 4).
Table 4 Prevalence of criminal convictions noted in the Offenders Index among the UK in-patient sample compared with a general UK population sample of people born in 1953
| UK in-patient sample | General population sample born in 19531 | ||
|---|---|---|---|
| Total | Those born 1951-1955 | ||
| Sample size, n | |||
| Men | 120 | 10 | 27 077 |
| Women | 85 | 5 | 25 538 |
| Men with at least one conviction prior to their 46th birthday | |||
| Prevalence, % | 57.5 | 80.0 | 32.6 |
| OR (95% CI) | 2.80 (1.95-4.02) | 8.27 (1.76-38.95) | |
| Women with at least one conviction prior to their 46th birthday | |||
| Prevalence, % | 22.4 | 20.0 | 8.7 |
| OR (95% CI) | 3.02 (1.81-5.04) | 2.62 (0.29-23.48) | |
| Men with at least one conviction for a violent offence prior to their 46th birthday2 | |||
| Prevalence | 35.0 | 40.0 | 8.7-11.4 |
| OR (95% CI) | 4.18 (2.87-6.10) | 5.18 (1.46-18.37) | |
| Women with at least one conviction for a violent offence prior to their 46th birthday2 | |||
| Prevalence, % | 11.8 | 0.0 | 1.0-1.6 |
| OR (95% CI)3 | 8.19 (4.20-15.96) | NA | |
Finally, we attempted to understand whether the elevations in risks of any conviction and of violent convictions observed in the UK in-patient sample compared with the UK general population sample were similar to those observed in other studies. We examined the risks of any criminal conviction and of convictions for violence of in-patients with severe mental illness, compared with the general population where they lived, in three studies. In all three studies, official records of crime by people with severe mental illness who had been admitted to hospital at least once are compared with those of a general population sample. Our UK in-patient sample was compared with the UK general population sample of persons born in 1953 (Reference Prime, White and LirianoPrime et al, 2001). The Swedish cohort included all 15 117 persons born in Stockholm in 1953 (Reference HodginsHodgins, 1992). The Danish cohort included all 358 000 persons born in Denmark from 1944 through 1947 (Reference Hodgins, Mednick and BrennanHodgins et al, 1996). Only convictions up to age 30 years are compared (Table 5). Across the three samples and among both men and women, a two-fold increase in the odds for convictions for any criminal offence was found. Among men, an almost five-fold increase in violent convictions emerged for the UK and Swedish samples, with a much lower increase for men with severe mental illness in the Danish sample. Among women, the pattern of results across the three studies differed. For any conviction, the women with severe mental illness in the UK in-patient sample showed a smaller increase in risk compared with the general population cohort than either the Swedish or the Danish women with severe mental illness. In contrast, the women with severe mental illness in the UK sample had much higher odds of conviction for violent offences than was found for women with severe mental illness in the Swedish or Danish samples.
Table 5 Criminal convictions up to age 30 years: comparison of general population samples with in-patient samples with severe mental illness from three countries

| UK1 | Sweden2 | Denmark3 | |
|---|---|---|---|
| OR (95% CI) | OR (95% CI) | OR (95% CI) | |
| Men | |||
| Conviction for a criminal offence | 2.72 (1.90-3.90) | 2.15 (1.39-3.33) | 2.59 (2.37-2.84) |
| Conviction for a violent criminal offence | 4.86 (3.30-7.16) | 4.74 (2.84-7.91) | 2.49 (2.10-2.95) |
| Women | |||
| Conviction for a criminal offence | 2.85 (1.63-4.98) | 3.78 (2.13-6.69) | 3.48 (2.96-4.08) |
| Conviction for a violent criminal offence | 17.24 (8.18-36.32) | 11.18 (4.30-29.13) | 5.89 (3.60-9.63) |
DISCUSSION
Among a sample of in-patients with severe mental illness, 49% of the men and 39% of the women had engaged in assaultive behaviours in the previous 6 months. This finding suggests that aggressive behaviour is a prevalent problem among patients with severe mental illness who require hospitalisation. The assaults took place when patients were living in the community and indicate a need for interventions designed to reduce aggressive behaviour and increase prosocial skills. Aggressive behaviour has many negative consequences, including incarceration in prisons where violence is common, increased contact with antisocial peers, and rejection by family members and friends. Further, aggressive behaviour limits the already small chances of a person with severe mental illness obtaining and maintaining employment and limits access to certain types of supported accommodation and specialised treatment services. As this study and others have shown (Reference Walsh, Moran and ScottWalsh et al, 2003; Reference Silver, Arseneault and LangleySilver et al, 2005), aggressive behaviour is also associated with an increased risk of being the victim of an assault.
Prevalence of aggressive behaviour towards others
In an effort to understand whether the magnitude of the problem confronting general adult services in UK inner-city areas was comparable to that challenging psychiatric services elsewhere, we compared prevalence rates of aggressive behaviour of the UK patients with those reported for other samples of patients with severe mental illness. Patient samples were similar as to age and principal diagnosis, and the same instrument and procedure had been used to collect information on aggressive behaviour in all studies. Both men and women in this UK urban in-patient sample reported higher rates of aggressive behaviour and violence towards others than patients in the CATIE trial and than both general adult and forensic patients in the CSMIV. In contrast, when rates of aggressive behaviour among UK patients were compared with a sample of in-patients with schizophrenia and schizoaffective disorder in the USA, the prevalence of any aggressive behaviour and of violence was much lower among the UK than the US patients. It is essential to note, however, that the comparison of the two in-patient samples is based on a statistical extrapolation to make the time periods equivalent.
In the UK700 study, 22% of the patients committed an assault during a 2-year period (Reference Walsh, Gilvarry and SameleWalsh et al, 2001). In a study of a general UK population sample, using a similar definition of physical aggression but covering the previous 5 years, 12% of the participants reported engaging in aggressive behaviour and 4% acknowledged injuring a victim (Reference Coid, Yang and RobertsCoid et al, 2006). Thus, the rates of aggressive behaviour for the UK in-patients were considerably higher than those for other out-patient samples and for a general population sample. We did not include a comparison group composed of healthy adults living in the same neighbourhood as the patients. In our experience it is almost impossible to recruit a comparison sample that is representative of the general population as to aggressive behaviour and criminality. This is because the most frequent offenders – young men and women with a childhood history of conduct disorder, adult antisocial personality disorder and substance misuse – are unlikely to volunteer to participate in a research study.
The patients in the CATIE trial and general adult services patients from the CSMIV were characterised by higher levels of education and lower levels of substance misuse/dependence than the UK patient sample. The higher level of substance misuse among the UK in-patient sample, however, is unlikely to explain the differences in the prevalence of aggressive behaviour. In all four samples that were used for the comparisons, it has been shown that substance misuse/dependence was not associated with aggressive behaviour after controlling for conduct problems prior to age 15 years (Reference Hodgins, Tiihonen and RossHodgins et al, 2005; Reference Swanson, Swartz and Van DornSwanson et al, 2006). Similarly, among the women in the UK700 study, substance misuse was not associated with violence towards others (Reference Dean, Walsh and MoranDean et al, 2006).
The difference in the prevalence of conduct problems prior to illness onset may, however, explain, at least in part, the differences in rates across samples. In the UK in-patient sample, 42% of the men and 22% of the women fulfilled criteria for a diagnosis of conduct disorder before the age of 15 years (further details available from the authors). These prevalence rates are higher than those reported for other samples of general adult and forensic patients with schizophrenia (Reference Hodgins, Cote, Toupin, Cooke, Forth and HareHodgins et al, 1998). In a follow-up of the Dunedin birth cohort at age 26 years, 40% of those who had developed a schizophrenic disorder displayed conduct disorder prior to mid-adolescence (Reference Kim-Cohen, Caspi and MoffittKim-Cohen et al, 2003). It is known that within the UK, rates of conduct disorder are elevated in socio-economically deprived neigbourhoods (Reference Meltzer, Gatwood and GoodmanMeltzer et al, 2000). Since among men with schizophrenia, childhood conduct disorder continues to be associated with aggressive behaviour and violent crime into middle age (Reference Hodgins, Tiihonen and RossHodgins et al, 2005; Reference Swanson, Swartz and Van DornSwanson et al, 2006), the elevated prevalence rate of childhood conduct disorder prior to age 15 years in the sample studied may explain, at least in part, the elevated rates of aggressive behaviour and violent crime.
To conclude, rates of aggressive behaviour of the UK in-patient sample with severe mental illness were similar to rates reported for in-patients with similar diagnoses in a US general hospital sample, and higher than rates for samples of community patients in the USA and in Europe. Rates of childhood conduct disorder and substance misuse were higher than those reported for other samples. The high rates of involuntary hospitalisation of the sample suggest that people with severe mental illness who require hospitalisation may be less cooperative and more aggressive than those who are treated at home.
Victimisation
Many of the men (57%) and the women (48%) in our study had been the victim of aggressive behaviour in the preceding 6 months. This was true of 20% of the CATIE trial participants (Reference Swanson, Swartz and Van DornSwanson et al, 2006), 18% of men in the CSMIV general psychiatric sample and 12% of men in the CSMIV forensic sample. In the MacArthur study 54% of the men and 52% of the women with schizophrenia or schizoaffective disorder reported victimisation in the preceding 10 weeks (Reference Monahan, Steadman and SilverMonahan et al, 2001). Thus, the rates of victimisation in the UK sample of in-patients are higher than those reported for other samples of patients with similar diagnostic profiles who are receiving community care, but similar to those for a US sample of in-patients with similar disorders. These findings add to a growing body of evidence showing that people with severe mental illness are at increased risk of becoming victims of aggressive behaviour or of crime, after socio-demographic factors are controlled for (Reference Walsh, Moran and ScottWalsh et al, 2003; Reference Silver, Arseneault and LangleySilver et al, 2005; Reference Teplin, McClelland and AbramTeplin et al, 2005). Rates of victimisation among people with severe mental illness vary from place to place (Reference Honkonen, Henriksson and KoivistoHonkonen et al, 2004).
In our study, engaging in aggressive behaviour significantly increased the risk of being a victim of a physical assault. Similarly, in the UK700 study, physical victimisation was found to be associated with aggressive behaviour towards others, illicit drug use, comorbid personality disorder, symptomatology, and homelessness (Reference Walsh, Moran and ScottWalsh et al, 2003). In a study that included the entire sample of patients from the MacArthur study the association between victimisation and aggressive behaviour was again identified. In addition, living in a deprived neighbourhood contributed independently to the risk of victimisation (Reference Silver, Mulvey and SwansonSilver et al, 2002). Taken together, these results suggest that certain environments foster, even teach, the use of aggressive behaviour to solve problems. Research is urgently needed to understand the link between victimisation and aggressive behaviour among people with severe mental illness and to identify the factors associated with reductions in both.
Prevalence of convictions for violent crime
In this study almost half of the men and 17% of the women had at least one conviction for a violent crime. The mental health trust studied provides services to four boroughs; in the period that patients were recruited into the study, two of these boroughs had crime rates higher than the national average and two had similar rates (Reference Nicolas, Povey and WalkerNicolas et al, 2005). In addition, these boroughs rank relatively high on a measure of social deprivation (Office of the Deputy Prime Minister, 2004). Consequently, the proportions of patients with criminal records and who experienced victimisation may be higher than in similar samples recruited from areas with lower crime rates. The patients had higher rates of convictions for any crime and for violent crimes than a UK general population sample. As presented in Table 5, this finding is consistent with the evidence that has been accumulating in the scientific literature since the early 1990s concerning the increase in risk of violent crime among patients with severe mental illness compared with the general population where they live.
Implications for services
If replicated, the results of this study indicate that general adult in-patient wards are now treating a subset of adults with severe mental illness who present multiple problems. The findings concur with a substantial body of evidence that has accumulated indicating that a subgroup of people with severe mental illness repeatedly engage in aggressive behaviour towards others while living in the community. In our view, it is time to begin building an evidence base concerning the assessment, management and treatment of this subgroup. We have developed a series of testable propositions for interventions that are briefly outlined below. The proposals are based on knowledge of aggressive individuals with schizophrenia, and of effective treatments for schizophrenia, substance misuse among people with schizophrenia, and violence.
The extant literature suggests that an integrated and coordinated package of interventions specifically targeting each of the problems is necessary in order to effect positive outcome (Reference Hodgins and Müller-IsbernerHodgins & Müller-Isberner, 2000; Reference Mueser and McGurkMueser & McGurk, 2004). Further, evidence suggests that among those who engage in aggressive behaviour and violent crime there are distinct subgroups who require different packages of treatments. Patients with a history of conduct problems (and often crime) prior to illness onset present antisocial attitudes and ways of thinking and a lack of prosocial skills from a young age, but may be less compromised neurologically than other patients with schizophrenia (Reference Hodgins, Tiihonen and RossHodgins et al, 2005; Reference Naudts and HodginsNaudts & Hodgins, 2006). These patients differ from those whose aggressive behaviour onsets with illness (Mueser et al, Reference Mueser, Rosenberg and Drake1999, Reference Mueser, Crocker and Frisman2006), and also from a third type who engage in no aggressive behaviour until many years after illness onset and then commit serious violence, usually against a carer (Reference Hodgins, Soothill, Dolan and RogersHodgins, 2007).
We propose that general adult services assess the history of aggressive and antisocial behaviour among patients with severe mental illness. This is done relatively easily and quickly using structured interviews assessing conduct disorder. This procedure would identify the patients most likely to continue to engage in aggressive behaviour and violent crime. The routine and continued use of structured risk assessment tools, such as the Historical, Clinical and Risk Scale (Reference Webster, Douglas and EavesWebster et al, 1997), would provide treatment teams with targets for managing the risk of aggressive behaviour and a way to assess progress over time. However, this tool would not identify the third type of patient who apparently ‘out of the blue’ engages in serious violence. Such patients are rare, and the only available evidence suggests that they may become progressively more callous prior to engaging in violence (further details available from the authors). Naturalistic follow-up studies indicate good outcome for even high-risk patients who are treated in highly structured community programmes that manage risk continually (Reference Heilbrun, Peters, Hodgins and Müller-IsbernerHeilbrun & Peters, 2000; Reference Lamberti, Weisman and FadenLamberti et al, 2004).
All three subtypes of patients require antipsychotic medication. The ‘early starters’, however, who are characterised by antisocial behaviours, attitudes and ways of thinking, present a special challenge to staff who attempt to educate them about their illness and the need for medication. Further, early-onset conduct problems are in part genetically determined (Reference Rhee and WaldrumRhee & Waldrum, 2002). The parents and siblings of men with schizophrenia and a history of childhood conduct disorder, compared with men with schizophrenia and no history of conduct problems prior to illness onset, display higher rates of crime and substance misuse (Reference Hodgins, Tiihonen and RossHodgins et al, 2005; further details available from the authors), suggestive (but not proof) of a distinct genetic profile. Since response to neuroleptics is partially determined by individual genetic profiles (Reference Illi, Mattila and KampionIlli et al, 2003), further research is needed to determine whether a better therapeutic response in this subgroup would be achieved with specific medications. One study has shown that aggressive patients with schizophrenia show greater reductions in positive and negative symptoms with clozapine, whereas patients who do not engage in aggressive behaviour benefit most from other medications (Reference Volavka, Czobor and NolanVolavka et al, 2004).
Once the optimal medication has been identified, compliance must be ensured before any other interventions are begun. Community care orders coupled with adequate treatment are associated with reductions in aggressive behaviour among patients living in the community (Reference Swartz and SwansonSwartz & Swanson, 2004). Two other studies have demonstrated reductions in aggressive behaviour in the community with the use of atypical antipsychotic medications (Swanson et al, Reference Swanson, Swartz and Elbogen2004a ,Reference Swanson, Swartz and Elbogen b ). Once compliance with medication has been achieved, the ‘early starter’ patients may benefit from a cognitive–behavioural intervention aimed at reducing antisocial behaviour, attitudes and ways of thinking. Such programmes are effective with non-mentally-ill offenders (Reference Tong and FarringtonTong & Farrington, 2006) and are currently being evaluated in patients with severe mental illness (Reference Fahy, Clarke and WalwynFahy et al, 2004). Once a reduction in antisocial behaviours and attitudes has been achieved, these patients need further learning-based programmes to reduce aggressive behaviour and substance misuse and to develop prosocial skills. Their relative cognitive proficiency makes them good candidates for employment training programmes that have proved effective with patients with schizophrenia (Reference Cook, Leff and BlylerCook et al, 2005; Reference McGurk, Mueser and PascarisMcGurk et al, 2005).
Patients who began engaging in aggressive behaviour at illness onset, once compliance with medication has been achieved, may benefit from a cognitive–behavioural intervention aimed at reducing aggressive behaviour. Again, such programmes have been found to be effective with nonmentally-ill individuals, and need to be adapted and their effectiveness measured in people with severe mental illness. Some authors have suggested that this subgroup of patients require structured interventions to reduce substance misuse (Mueser et al, Reference Mueser, Rosenberg and Drake1999, Reference Mueser, Crocker and Frisman2006) and the effectiveness of some programmes has been demonstrated (Reference Mueser, Noordsy and DrakeMueser et al, 2003; Reference Bellack, Bennett and GearonBellack et al, 2006).
The results of our study also show the need for general adult services to assess victimisation among patients with severe mental illness and to intervene to help patients protect themselves. A recent study reported that current victimisation contributed to substance misuse, demoralisation and increased levels of psychotic symptoms among people with severe mental illness (Reference Shahar, Wisher and ChinnmanShahar et al, 2004). We have found only one study assessing interventions for victimisation: adherence to treatment that resulted from community treatment orders for patients with severe mental illness was associated with a reduction in victimisation (Reference Hiday, Swartz and SwansonHiday et al, 2002).
Our findings paint a dramatically different picture of the problems presented by people with severe mental illness from that in the National Service Framework for Mental Health (Department of Health, 1999) or the National Institute for Health and Clinical Excellence clinical guidelines for schizophrenia (National Collaborating Centre for Mental Health, 2003). Both policy and practice currently fail to recognise that aggressive behaviour and victimisation are problems for many patients with severe mental illness. Consequently, general adult services are not given sufficient resources to treat these problems, and increasing numbers of patients are transferred to expensive forensic services.








eLetters
No eLetters have been published for this article.