Introduction
Structured diagnostic interviews, such as the Composite International Diagnostic Interview (CIDI; Wittchen, Reference Wittchen1994) and the revised Clinical Interview Schedule (CIS-R; Lewis et al. Reference Lewis, Pelosi, Araya and Dunn1992), are considered by many researchers to be the most valid and reliable methods for the assessment of mental disorders in populations according to diagnostic criteria (ICD-10 or DSM-IV). The CIS-R has been widely used in the UK (Brugha et al. Reference Brugha, Bebbington and Jenkins1999) whereas the CIDI has been more commonly used in the USA (Haro et al. Reference Haro, Arbabzadeh-Bouchez, Brugha, de Girolamo, Guyer, Jin, Lepine, Mazzi, Reneses, Vilagut, Sampson and Kessler2006). In comparisons with semi-structured clinical evaluations, the CIS-R has been shown to be a valid measure of mental disorders (Patton et al. Reference Patton, Coffey, Posterino, Carlin, Wolfe and Bowes1999; Jordanova et al. Reference Jordanova, Wickramesinghe, Gerada and Prince2004; Brugha et al. Reference Brugha, Meltzer, Jenkins, Bebbington and Taub2005; Pez et al. Reference Pez, Gilbert, Bitfoi, Carta, Jordanova, Garcia-Mahia, Mateos-Alvarez, Prince, Tudorache, Blatier and Kovess-Masfety2010).
However, structured interviews such as the CIDI and the CIS-R may be expensive and impractical to use in large, epidemiological studies. Large-scale surveys have therefore often relied on self-administered instruments to identify psychiatric illness and morbidity, despite concerns about the validity and reliability of these measures. Although some studies have demonstrated that self-administered instruments are valid in younger and middle-aged adults (Goldberg & Williams, Reference Goldberg and Williams1988; Stansfeld & Marmot, Reference Stansfeld and Marmot1992) and have compared self-completion and interviewer versions of either the CIS-R or the CIDI (Lewis et al. Reference Lewis, Pelosi, Glover, Wilkinson, Stansfeld, Williams and Shepherd1988; Lewis, Reference Lewis1994; Peters et al. Reference Peters, Clark and Carroll1998), few studies have investigated their validity in older populations.
In this study, we tested whether a computerized self-completion version of the CIS-R (Lewis et al. Reference Lewis, Pelosi, Glover, Wilkinson, Stansfeld, Williams and Shepherd1988) was a feasible and valid instrument for identifying mental disorders in older adults by comparing results with the interview-administered CIS-R, considered to be the reference standard in this study. In addition, we examined the sensitivity and specificity of two commonly used self-completion questionnaires, the Center for Epidemiologic Studies Depression Scale (CES-D; Radloff, Reference Radloff1977) and the General Health Questionnaire (GHQ; Goldberg, Reference Goldberg1972), as measures of psychiatric disorders in a UK population aged 58–80 years.
Method
The Whitehall II study
The Whitehall II study is a cohort of 10 308 originally London-based civil servants (6895 men and 3413 women) aged between 35 and 55 years in 20 London-based civil service departments, established between 1985 and 1988 (phase 1) (Marmot et al. Reference Marmot, Davey Smith, Stansfeld, Patel, North, Head, White, Brunner and Feeney1991). The validation study reported in this paper was conducted at phase 10 of the Whitehall II study in 2011. The main aims of phase 10 were to (1) validate self-completion measures of psychiatric morbidity, in addition to several other screening measures, in older people and (2) to invite a subsample of participants to take part in a neuroimaging study of late-onset depression cases and never-depressed controls.
Study sample
The sample (phase 10) was selected from the Whitehall II cohort. We drew a random sample of 255 persons, stratified by sex, age and social position (most recent employment grade) from among the 5390 cohort members who attended the phase 9 follow-up examination in 2008–2009. To obtain a sufficient number of depressed adults, we supplemented this sample by inclusion of all participants with evidence of late-onset depressive symptoms in the 2008–2009 follow-up.
Of the 5390 who attended the phase 9 screening examination, 88 participants were classified as having late-onset depressive symptoms; as six of these 88 were already selected in the random sample of 255, this gave a total supplemented sample of 337. Three of the 337 were living overseas and therefore were not invited to participate; a further four people died before being contacted. Thus, 330 people were eligible and were invited to participate at phase 10; of these, 277 took part (response rate 84%).
Study procedures and measures
Self-completion questionnaires, including the CES-D and the GHQ, were sent out in December 2010 along with invitation letters to attend a screening clinic. Participants were asked to bring along their completed questionnaires to hand in at the clinic. According to the recorded date of questionnaire completion, the majority of participants completed their postal questionnaires shortly before their screening clinic appointment (median 2 days apart, 87% less than 30 days apart). Between 31 January 2011 and 14 March 2011, participants attended screening where they completed both the interviewer-administered and the computerized self-completion versions of the CIS-R. We allocated participants randomly to complete either the interviewer version first or the computerized self-completion version first. A potential limitation of our study is that, to reduce respondent burden, both versions of the CIS-R were administered on the same day. However, participants were administered the other phase-10 measures in between the first and second CIS-R versions to reduce the risk that the respondent recalled their answer to the first version. Participants were offered tea and biscuits at the end of the phase-10 screening but no financial incentives were offered for participation. Ethical approval for the Whitehall II study was obtained from the University College London Medical School committee on the ethics of human research, and all participants gave informed written consent.
The CIS-R is a structured diagnostic interview for common mental disorders, formerly neurotic disorders (Lewis et al. Reference Lewis, Pelosi, Araya and Dunn1992), but because of the structured nature of the questions and responses in this measure, a computerized self-completion version is also available (Lewis et al. Reference Lewis, Pelosi, Glover, Wilkinson, Stansfeld, Williams and Shepherd1988). Both versions generate scores on 14 psychiatric symptoms (listed in Table 1), a total score and diagnoses of depressive and other common mental disorders based on the ICD-10 (diagnoses listed in Table 2), thus providing measures of severity and also presence or absence of mental disorders.
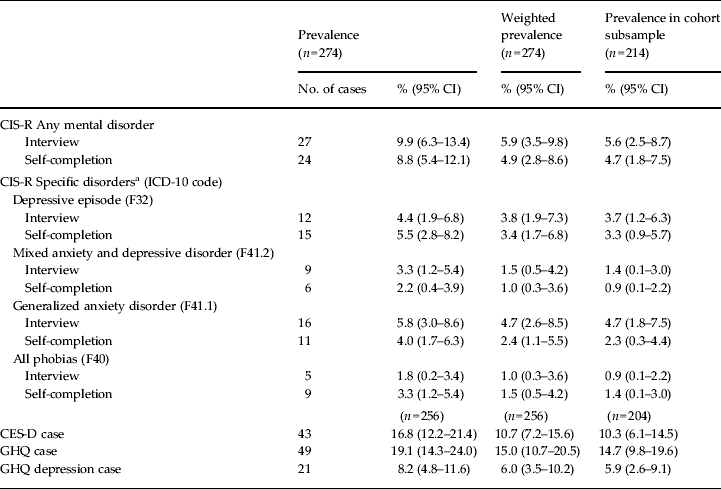
Table 1. Prevalence of mental disorders

CIS-R, Clinical Interview Schedule Revised; CI, confidence interval; CES-D, Center for Epidemiologic Studies Depression Scale; GHQ, General Health Questionnaire.
a There were two cases of panic disorder (ICD-10 F41.0) and no cases of obsessive–compulsive disorder (ICD-10 F42).
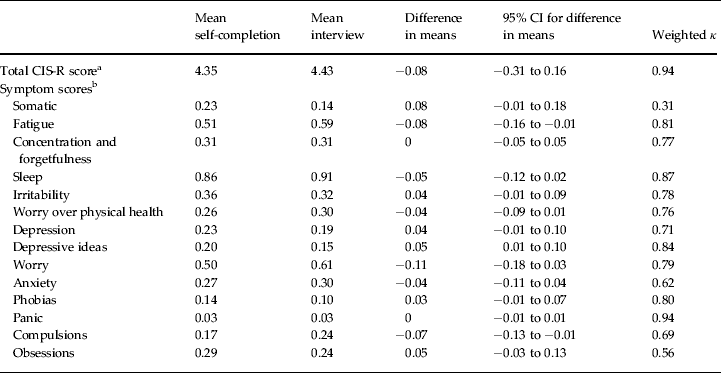
Table 2. Agreement between self-completion and interviewer versions for the total CIS-R score and symptom scores (n = 274)

CIS-R, Clinical Interview Schedule Revised; CI, confidence interval.
a Total score ranges from 0 to 57.
b Symptom scores range from 0 to 4 (depressive ideas symptom score 0 to 5).
A CIS-R total score ⩾12 was used to define cases with any common mental disorder (Lewis et al. Reference Lewis, Pelosi, Araya and Dunn1992). The wording of the questions and responses was the same in the computerized self-completion and interviewer-administered versions but interviewers used show cards listing response options for questions that were sensitive or had several possible responses. Both versions were administered using the program PROQSY (Lewis et al. Reference Lewis, Pelosi, Glover, Wilkinson, Stansfeld, Williams and Shepherd1988). A laptop computer was used for the interviewer version with interviewers reading questions from the screen and entering responses directly. A desktop computer was used for the self-completion version. Start and end times were recorded so that completion times could be compared. Interviewers were given 2 hours of training in the use of the CIS-R, which included a practice session. All interviewers were given a written protocol to follow and had the opportunity for further practice interviews during the pilot of the phase-10 data collection. Less than 1% of participants were given help with the computerized version because of eyesight problems or other problems with using a computer.
The 20-item CES-D is a short self-report questionnaire designed to measure depressive symptoms in the general population (Radloff, Reference Radloff1977). Participants were asked to score the frequency of occurrence of specific symptoms during the previous week on a four-point scale, where 0 = ‘less than 1 day’, 1 = ‘1–2 days’, 2 = ‘3–4 days’ and 3 = ‘5–7 days’. These were summed to yield a total score between 0 and 60. Participants scoring ⩾16 were categorized as cases of CES-D depression (Stansfeld et al. Reference Stansfeld, Head, Bartley and Fonagy2008). The CES-D was included at phases 7, 9 and 10.
The 30-item GHQ is a well-established screening questionnaire for common mental disorder, suitable for use in general population samples (Goldberg, Reference Goldberg1972). The GHQ was included in all study phases 1–10 with the exception of phase 4. At phase 1 of the study, this was validated against the CIS in a subsample and, on the basis of receiver operating characteristic (ROC) analysis, those scoring ⩾5 were deemed GHQ cases (Stansfeld & Marmot, Reference Stansfeld and Marmot1992). A four-item depression subscale (Cronbach's α = 0.88) was identified from the 30-item GHQ on the basis of factor analysis and comparison with the items of the depression subscale of the 28-item GHQ (Goldberg & Hillier, Reference Goldberg and Hillier1979). A total depression score (ranging from 0 to 12) was derived by summing responses to these four items using Likert scoring (0 to 3) for each item. Participants scoring ⩾2 were categorized as cases of GHQ depression (Stansfeld et al. Reference Stansfeld, Head and Marmot1998).
A measure of early-onset depressive symptoms was derived from GHQ measures at phases 1–9 and defined as two or more reports of GHQ caseness and/or two or more reports of GHQ depression subscale caseness before age 60. Late-onset depression was defined as being a CES-D case at phase 9 AND having no early-onset depressive symptoms AND no prevalent serious chronic conditions (coronary heart disease, cancer, stroke).
Statistical analysis
For each mental disorder we computed estimates of raw prevalence, weighted prevalence to adjust for oversampling of depressed cases and prevalence in the randomly selected cohort subsample. Differences in prevalence estimates between the self-completion measures and interviewer CIS-R were tested using McNemar's χ 2 test. Differences in mean total scores and specific symptom scores between the self-completed and interviewer CIS-R were examined with the paired t test. The agreement of scores between the two versions was assessed with the weighted κ statistic. Linear regression with difference in CIS-R score between the two versions was used to test for evidence that differences in method of administration were related to age, sex, employment grade or presence of chronic physical illness. We performed ROC analysis to compute estimates of sensitivity, specificity, positive predictive value (+PV), negative predictive value (–PV) and area under the ROC curve (AUC) for all self-completion measures of any mental disorder and specific mental disorders using the interviewer-administered CIS-R as the criterion. Based on published guidelines, we considered AUC values ⩾0.90 to indicate excellent validity and values ⩾0.80 but < 0.90 to indicate good validity (Metz, Reference Metz1978). We checked the cut-off points of scores ⩾16 and scores ⩾5 used to define CES-D and GHQ cases respectively by ROC analyses. Analyses were performed using Stata version 12 (StataCorp, USA).
Results
Of the 330 persons invited, 277 attended the examination (response rate 84%) and 274 had complete data on both interviewer-administered and self-completion versions of the CIS-R. The mean age was 69.1 (s.d. = 5.8) years for participants allocated to the self-completion CIS-R version first and 68.3 (s.d. = 6.2) for participants allocated to the self-completion CIS-R version second. Among participants allocated to the self-completion version first (second), 31% (28%) were female; the most recent employment grade was high for 42% (47%), middle for 45% (41%) and low for 13% (13%); the proportion classified as GHQ cases was 21% (21%) and the proportion classified as CES-D cases was 17% (16%). Similarly, CIS-R mean total scores did not differ significantly according to order of administration of the two CIS-R versions.
Table 1 presents the prevalence for each of the mental health measures. Based on the interviewer-administered CIS-R, 27 participants were diagnosed as having any mental disorder. The numbers of participants diagnosed as having specific disorders were: 12 depressive episode; nine mixed anxiety and depressive disorder; 16 generalized anxiety disorder; five phobia; and two panic disorder. No participants were diagnosed with obsessive–compulsive disorder.
Validity of self-completion CIS-R
Table 2 shows the mean value for the total CIS-R score and each of the 14 symptom scores. The mean difference in the total score between self-completion CIS-R and interviewer CIS-R was small, the mean scores on the two versions were 4.35 and 4.43 respectively [95% confidence interval (CI) for difference in means −0.31 to 0.16, p = 0.26, paired t test]. For 12 of the 14 symptom scores, differences in symptom scores did not differ according to method of administration. Differences for both fatigue and compulsions were statistically significant, with slightly lower scores on the self-completion version than the interviewer version. In a linear regression model, the difference in total CIS-R score between the two versions was not related to age, sex, social position or presence of chronic physical illness.
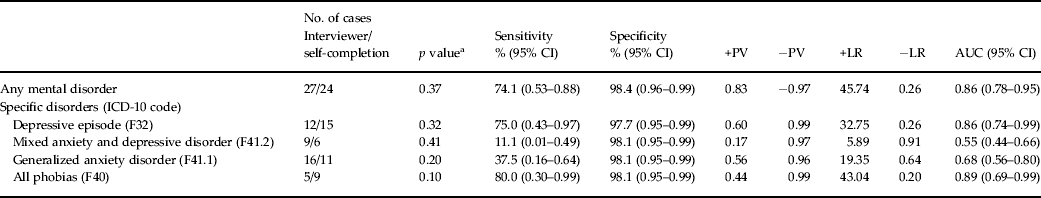
Table 3 presents sensitivity and specificity figures for the self-completion CIS-R measures of any mental disorder and specific mental disorders. The sensitivity for any mental disorder was 74.1% and specificity 98.4%. The corresponding figures for depressive episode were 75.0% and 97.7% respectively. The self-completion CIS-R was also a sensitive and specific measure of all phobias (80%/98.1%), but its sensitivity was low for mixed anxiety and depressive disorder and for generalized anxiety disorder. The specificity (> 97%) was very high for all diagnostic categories.
Table 3. Sensitivity and specificity for the self-completion CIS-R assessment of mental disorders with the interviewer-administered CIS-R as the criterion (n = 274)

CIS-R, Clinical Interview Schedule Revised; CI, confidence interval; +PV, positive predictive value; −PV, negative predictive value; +LR, positive likelihood ratio; −LR, negative likelihood ratio; AUC, area under the receiver operating characteristic (ROC) curve.
a McNemar's χ 2 test for difference in prevalence between interviewer and self-completion versions.
Validity of the CES-D and GHQ
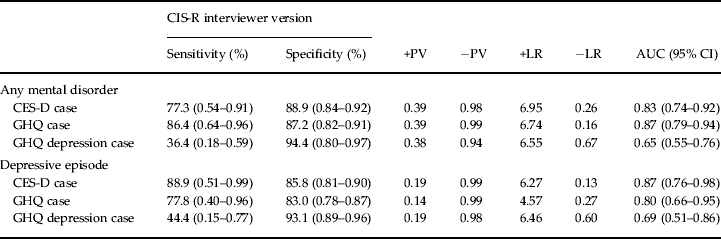
Table 4 shows that the CES-D is a sensitive and specific measure of any mental disorder (sensitivity/specificity 77%/89%) and depressive episode (sensitivity/specificity 89%/86%). This is also the case for the GHQ caseness (86%/87% for any mental disorder; 78%/83% for depressive episode). By contrast, the GHQ depression measure constructed from four items of the 30-item GHQ was not a sensitive measure for depressive episode, although the ROC analysis indicated that sensitivity for depressive episode was somewhat improved for a cut-point ⩾2 (sensitivity/specificity 56%/90%) in place of the cut-point ⩾3 used in earlier studies (sensitivity/specificity 44%/93%).
Table 4. Sensitivity and specificity for the self-completion CES-D and the GHQ as measures of any mental disorder and depressive episode with the interviewer-administered CIS-R as the criterion (n = 256)

CES-D, Center for Epidemiologic Studies Depression Scale; GHQ, General Health Questionnaire; CIS-R, Clinical Interview Schedule Revised; +PV, positive predictive value; −PV, negative predictive value; +LR, positive likelihood ratio; −LR, negative likelihood ratio; AUC, area under the receiver operating characteristic (ROC) curve; CI, confidence interval.
Discussion
Data from men and women aged 58–80 years show reasonably high sensitivity and specificity, varying between 74% and 98%, for the CES-D, the 30-item GHQ and the computerized self-completion version of the CIS-R as measures of any mental disorder and depressive episode. The computerized self-completion CIS-R was additionally a sensitive and specific measure of phobias and accurately detected symptom severity in 12 specific psychiatric symptoms. These findings suggest that several self-administered instruments, with reasonable criterion validity, may be used to screen for common mental disorders and depression in populations aged ⩾60 years. Furthermore, the mean total score from the computerized self-completion version and the structured interview version were very similar.
An earlier comparison of the computerized self-completion version of the CIS-R against the structured psychiatric interview in this population when they were aged 35–55 years showed slightly higher sensitivity (82%) and lower specificity (84%) (Lewis et al. Reference Lewis, Pelosi, Glover, Wilkinson, Stansfeld, Williams and Shepherd1988). Previous studies on this measure have shown good agreement in severity score and case definition for any psychiatric disorder in primary care and occupational settings but these studies did not examine agreement for specific ICD-10 disorders such as depressive episode (Lewis et al. Reference Lewis, Pelosi, Glover, Wilkinson, Stansfeld, Williams and Shepherd1988; Lewis, Reference Lewis1994). We found that symptom scores were significantly lower on the self-completion version than the interviewer version for both fatigue and compulsions. This is in contrast to an earlier study where the only significant difference in the 14 symptom scores was for sleep symptoms (Lewis, Reference Lewis1994). It is possible that these findings are due to chance.
According to a review of 28 studies, previous investigations on the CES-D and GHQ have reported validity estimates comparable to those we observed (Williams et al. Reference Williams, Noel, Cordes, Ramirez and Pignone2002). Our current findings are also in agreement with those obtained over 20 years ago for this cohort. At the baseline of the Whitehall II study when the participants were aged 35–55 years, the sensitivity of the GHQ against the CIS was 73% although specificity was slightly worse at 78% (Stansfeld & Marmot, Reference Stansfeld and Marmot1992). In a vulnerable, very old population living in residential homes in The Netherlands, sensitivity for CES-D for depressive and/or anxiety disorders exceeded 80% but specificity was lower, at 61% (Dozeman et al. Reference Dozeman, van Schaik, van Marwijk, Stek, van der Horst and Beekman2011). Among postpartum women, a 60% sensitivity and 90% specificity was observed for the CES-D (Boyd et al. Reference Boyd, Le and Somberg2005). However, the validity of the CES-D has been lower in some (Klinkman et al. Reference Klinkman, Coyne, Gallo and Schwenk1997; Thomas et al. Reference Thomas, Jones, Scarinci, Mehan and Brantley2001) but not all clinical samples (Stahl et al. Reference Stahl, Sum, Lum, Liow, Chan, Verma, Chua and Chong2008).
Limitations and strengths of the study
A limitation of this study is that participants were recruited from an occupational cohort so our findings may not apply to people who have not had paid employment. Our sample was relatively healthy and consisted of people able to travel to our London clinic. Estimates of sensitivity were imprecise for specific anxiety disorders because of the small number of people diagnosed with these disorders in this sample. We considered the interviewer-administered version to be the ‘gold standard’ criterion although this is somewhat arbitrary as it is possible that people may be more likely to under-report symptoms in an interviewer-administered version than in a self-completion version. Given this limitation, our study could alternatively be described as a reliability, method-comparison or concordance study. Furthermore, the GHQ and the CES-D self-completion questionnaire were posted to participants so that differences between the GHQ/CES-D and the CIS-R may be attributable not only to the instrument but also to the mode of administration and setting, such as completion at home rather than in a clinic. A further limitation is that, although the majority of participants completed their postal questionnaires shortly before their screening clinic appointment (median 2 days apart, 87% within 1 month), the gap of more than a month for some participants may mean that the results were influenced by changes in symptoms. It is possible that this partially accounted for our results showing that sensitivity was poor for both mixed anxiety and depressive disorder and for generalized anxiety disorder.
The strengths of this study are that our sample was selected randomly from a large cohort study, and was large enough to demonstrate that the similar severity scores obtained from the two methods of administration were consistent for men and women, across age groups, for different employment grades and for people with and without a chronic physical illness. Additionally, we demonstrated that it is feasible to use a computerized self-completion version in studies of older participants as response rates were identical for the two versions.
An advantage of self-completion instruments is that they are less expensive to administer than interviewer instruments. At the time of writing this paper, more than 1500 participants had been screened in the sixth medical examination of the Whitehall II study. Respondents attended the clinic where physiological measures, blood tests, cognitive function and the self-completion version of the CIS-R were administered. A member of the clinic staff introduced the respondent to the self-completion computerized CIS-R version. This took no more than a few minutes. Several computers were available in a quiet room so that up to six respondents could complete the CIS-R at any one time. We estimate that using the self-administered CIS-R procedure reduced staff costs by at least 60% compared to using the interviewer version, where it would be necessary to schedule appointments about 30 to 45 minutes apart. Based on preliminary data from the first 1500 participants at phase 11, 0.5% were given reading glasses and 0.5% were helped by clinic staff because of poor eyesight or physical difficulty using a computer.
Implications
Taken together, these findings suggest that the computerized self-completion CIS-R provides a feasible and less expensive alternative to the interviewer-administered CIS-R to identify any common mental disorder and depressive episode according to ICD-10. The CES-D and 30-item GHQ also have reasonable criterion validity as measures of common mental disorders and depression.
Acknowledgements
We thank all participating civil service departments and their welfare, personnel and establishment officers; the Occupational Health and Safety Agency; the Council of Civil Service Unions; all participating civil servants in the Whitehall II study; and all members of the Whitehall II study team.
The Whitehall II study has been supported by grants from the Medical Research Council (MRC) G8802774; the British Heart Foundation; the Health and Safety Executive; the Department of Health; the National Heart, Lung, and Blood Institute (R01HL036310); the National Institute on Aging, National Institutes of Health (NIH) (R01AG013196 and R01AG034454); and the Agency for Health Care Policy and Research (grant HS06516). J. Head was supported in part by the National Institute on Aging, NIH (R01AG013196). M. Kivimäki was supported by the MRC, the Academy of Finland, and a professorial fellowship from the Economic and Social Research Council, UK. C. Allan received support from Oxford University Clinical Academic Graduate School (OUCAGS).
Declaration of Interest
None.