Knowledge of the extent of psychiatric morbidity is important for the planning of mental health services. Epidemiological studies designed to measure the prevalence of morbidity accurately are time consuming and costly to conduct. Hence, proxy measures are often used to determine the extent of psychiatric morbidity in a population. There is already an established association between rates of treated mental illness and area socioeconomic factors (Reference ThornicroftThornicroft, 1991). This has led to the use of socio-economic indices to help predict psychiatric morbidity in an area and the workload of mental health services. In particular, socio-economic indices have been used to predict admission rates for psychiatric disorders. Three of the more commonly used indices are the York index (Reference Carr-Hill, Hardman and MartinCarr-Hill et al, 1994; Reference Smith, Sheldon and MartinSmith et al, 1996), the Jarman index (Jarman, Reference Jarman1983, Reference Jarman1984) and the Townsend index (Reference Townsend, Phillimore and BeattieTownsend et al, 1988). The York index is useful at regional level and above but not at local level because its calculation requires the standardised mortality ratio, which is not routinely available at the local level. However, the other two are calculable from local area variables derived from the 1991 census. Jarman et al (Reference Jarman, Hirsch and White1992) and Thornicroft (Reference Thornicroft1991) investigated the relation between deprivation and psychiatric admission rates and found a high positive correlation. Thornicroft et al (Reference Thornicroft, Bisoffi and De Salvia1993) investigated the relation between deprivation and both psychiatric in-patient admissions and out-patient and community contacts. They found a high positive correlation for an urban area for both admissions and community contacts but for neither in a rural area. Melzer et al (Reference Melzer, Watters and Paykel1999) found a positive correlation between general practitioner (GP) referral rates and Jarman index and standardised morbidity ratio and a negative association between referral rates and higher hypnotic prescription rates by GPs and characteristics of community mental health teams (CMHTs). We investigated the association between the Jarman index and the Townsend index and referral rates to CMHTs and admission rates, and GP interpractice variation for referral rates.
Method
We carried out a retrospective survey of case notes on two groups of patients. The first group comprised all adult psychiatry community and out-patient referrals between April 1993 and March 1994 to the four CMHTs based in the London borough of Merton, and the second consisted of all adult psychiatry in-patient admissions under the four CMHTs during the same year.
The data collected on each patient in both groups included postcode, whether the patient was seen/ assessed, whether the patient was taken on for treatment or referred back, diagnostic category and profession of keyworker. Additional data collected on the in-patient sample included Mental Health Act use and length of stay in hospital. A Jarman index and a Townsend material deprivation index was allocated to each patient by linking his/her postcode to a census enumeration district (Reference Majeed, Cook and PolonieckiMajeed et al, 1995). Out-patient referral rates and in-patient admission rates were calculated by using the number of patients in each enumeration district as the enumerator and the total population of the enumeration district as the denominator. Using information from the local authority, each practice's referral rate to the four CMHTs was also calculated. Practices with less than 1000 patients were excluded from this analysis.
Statistical tests used were as follows: χ2 test for categorical data, unpaired t-test for normally distributed continuous data, Mann—Whitney U test (for two category variables) and Kruskal—Wallis test (for more than two category variables) for non-normally distributed continuous data and Spearman's correlation for analysing correlations between the indices of deprivation and the referrals and admissions rates (as both the referral and admission rates included 0 rates for several enumeration districts, resulting in considerable deviation from normal distribution). The Statistical Package for Social Sciences for Windows, 6.1 was used for analysis (SPSS, 1994).
Results
Community/out-patients referrals
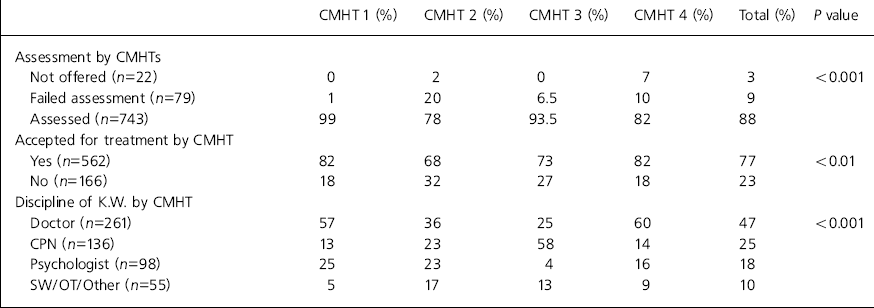
There were 928 (43% men) community/out-patient referrals. The proportion of patients assessed by the four CMHTs was 88% (varied from 82% to 99% between CMHTs) and accepted for treatment was 77% (varied from 68% to 82% between CMHTs). The proportion of patients keyworked by different professionals within the CMHTs differed significantly from 5% by social worker or occupational therapist to 60% by doctor (Table 1).
Table 1. Community mental health team (CMHT) response to community/out-patient referrals
| CMHT 1 (%) | CMHT 2 (%) | CMHT 3 (%) | CMHT 4 (%) | Total (%) | P value | |
|---|---|---|---|---|---|---|
| Assessment by CMHTs | ||||||
| Not offered (n=22) | 0 | 2 | 0 | 7 | 3 | <0.001 |
| Failed assessment (n=79) | 1 | 20 | 6.5 | 10 | 9 | |
| Assessed (n=743) | 99 | 78 | 93.5 | 82 | 88 | |
| Accepted for treatment by CMHT | ||||||
| Yes (n=562) | 82 | 68 | 73 | 82 | 77 | <0.01 |
| No (n=166) | 18 | 32 | 27 | 18 | 23 | |
| Discipline of K.W. by CMHT | ||||||
| Doctor (n=261) | 57 | 36 | 25 | 60 | 47 | <0.001 |
| CPN (n=136) | 13 | 23 | 58 | 14 | 25 | |
| Psychologist (n=98) | 25 | 23 | 4 | 16 | 18 | |
| SW/OT/Other (n=55) | 5 | 17 | 13 | 9 | 10 |
Seventy-five per cent of the assessed patients did not have psychoses (ICD-9 categories 300-316), 21% had psychoses (ICD-9 categories 290-299) and 4% were non-cases (World Health Organization, 1978). Non-psychotic disorder was significantly more common in women (80% compared to 68% in men) and psychotic disorder in men (28% compared to 16% in women; P<0.001). The proportion of referrals with and without psychotic disorder across the teams was not significantly different.
Admissions
There were 321 (54% men) in-patient admissions. Seventeen per cent of the admissions were involuntary but varied significantly from 11-30% between the CMHTs (P=0.01). The ratio of patients with or without psychoses for admissions was almost the reverse of that of community/out-patient referrals, 31% had non-psychotic disorders and 69% psychotic disorders. The proportion of admissions with or without psychoses across the CMHTs was not significantly different (P=0.57). More women had a non-psychotic disorder (35% compared to 27%) and more men had a psychotic disorder (73% compared to 63%), but these differences were not statistically significant (P=0.23). Mean length of stay of in-patients was 41 days (median=21, range 1-423). Length of stay was not significantly different between the CMHTs (P=0.17). The psychotic group had a longer length of stay (mean 50 days, median 33 days) than the non-psychotic group (mean 29 days, median 8) (P<0.0001).
Correlation between deprivation indices and referral and admission rates
The unit of analysis for correlation between indices of deprivation and area rates of referrals and admissions was the enumeration district. The enumeration district was preferred to the electoral ward as the unit of analysis because the latter would have reduced the sample size to 16. Also, as enumeration districts are substantially smaller than electoral wards, misclassification bias owing to the ecological fallacy is less likely to occur.
The four CMHTs served 271 enumeration districts. The mean Jarman index for these 271 enumeration districts was 6.1 (range -37.0 to 83.5) and the mean Townsend index was 0.2 (range -6.1 to 8.7). The mean crude community/out-patient referral rate per 1000 population per enumeration district for all patients was 7.8 (range 0-41). For referrals with psychoses it was 1.2 (range 0-24) and referrals without psychoses it was 4.6 (range 0-25). The mean crude in-patient admission rate (per 1000 population) per enumeration district for all patients was 2.6 (range 0-26); for admissions with psychoses, 1.1 (range 0-14), and admissions without psychoses, 0.42 (range 0-6).
There was a low positive correlation between overall community/out-patient referral rates and the Jarman index (ρ=0.13, P<0.05), but not with the Townsend index. There was low positive correlation between community/out-patient referral rates for psychosis and the Jarman index (ρ=0.17, P<0.01) and the Townsend index (ρ=0.15, P<0.05). There was no significant correlation between either of the indices and community/out-patient referral rates for non-psychosis. There was a low positive correlation between both the indices and admission rates for all diagnosis and non-psychosis (Table 2). There was no significant relationship between both the indices and admission rate for psychosis.
Table 2. Correlation of Jarman and Townsend indices with community/out-patient referral and admission rates

| Jarman index | Townsend index | |
|---|---|---|
| Community/out-patient referral rate: all diagnoses | ρ=0.13 | ρ=0.11 |
| P<0.05 | P=0.07 | |
| Community/out-patient referral rate: psychosis | ρ=0.17 | ρ=0.15 |
| P<0.01 | P<0.05 | |
| Community/out-patient referral rate: non-psychosis | ρ=0.04 | ρ=0.02 |
| P=0.52 | P=0.72 | |
| Admission rate: all diagnoses | ρ=0.20 | ρ=0.24 |
| P<0.01 | P<0.001 | |
| Admission rate: psychosis | ρ=0.08 | ρ=0.11 |
| P=0.22 | P=0.08 | |
| Admission rate: non-psychosis | ρ=0.15 | ρ=0.13 |
| P<0.05 | P<0.03 |
GP referral rates
There was a nearly 40-fold variation in general practice referral rates to the four CMHTs, from 0.26-10.2 per 1000 patients aged 16-64 years (practices with fewer than 1000 patients excluded). There was a non-significant negative correlation between the Townsend index for the practice and the referral rate to CMHTs (R=-0.30, P=0.10). There were no significant differences in referral rates between practices with and without a practice manager or practice nurse or between fundholding and non-fundholding general practices.
Discussion
Perhaps the most striking finding of this study was the 40-fold variation in general practice referral rates to CMHTs. This variation may have a number of causes. The number of referrals from many of the practices included was relatively small (range 1-91) and hence there will inevitably be some random variation. There will also be differences in the clinical and socio-economic characteristics of the patients registered with each practice. The most important factor, however, is likely to be the clinical practice of the GP. This large variation in clinical practice probably masks an association between deprivation and psychiatric morbidity at community service level, particularly for referrals without psychoses. Melzer et al (Reference Melzer, Watters and Paykel1999) did, in fact, find a negative association between GP referral rates and higher rates of prescriptions for hypnotics by GPs. However, they found smaller variation in inter-practice referral rates. The extent of inter-practice variations in referral rates and how clinical practice of GPs might influence it requires further investigation, perhaps in different settings.
The Jarman index was consistently positively associated with a number of measures of psychiatric morbidity, including community/out-patient referral rate for all diagnoses and for illness; and admission rates for all diagnoses and non-psychosis. However, the correlation coefficients were relatively low. The Townsend index showed similar low positive correlations with admission rates for all diagnosis and psychosis, but was only significantly correlated with community/out-patient referral rates for psychosis.
Our findings suggest that both Jarman and Townsend indices would be moderately useful for planning in-patient provision. For planning community/out-patient services, the Jarman index seems more useful than the Townsend index. Hence, given the wide coverage by the CMHT model (Reference Johnson and ThornicroftJohnson & Thornicroft, 1993) in the UK (where the same team is responsible for both in-patient and community care), the Jarman index would be the indicator of choice. Its value is further enhanced by its ready availability at enumeration district level.
Such a detailed and flexible prediction of workload is of increasing importance in the context of the reorganisation of primary care and the requirement for coordination with secondary mental health services. The other important area that needs to be addressed in planning community psychiatric services is links with primary health care teams, particularly in ensuring that teams make appropriate use of services. For some primary health care teams, this may mean increasing their referrals to community psychiatric services. However, neither the Jarman index nor Townsend index performed as well as was expected. This may be partly owing to some of their constituent variables being inappropriate for the purpose. The more recently developed Mental Illness Needs Index (MINI) appears to be an improvement, containing epidemiologically more meaningful variables for prediction of admission, at both local and regional levels (Reference Glover, Robin and EmamiGlover et al, 1998). This also deserves more extensive investigation in relation to both admission and referrals rates.
This study has a number of limitations. It uses retrospectively collected data from case notes and the comparison of psychiatric morbidity and socio-economic factors used an ecological design. The relatively low correlations between deprivation and referral and admission rates may reflect the importance of a range of other factors at the primary—secondary care interface. CMHTs increasingly have well-established liaison with local GPs (Reference Strathdee and WilliamsStrathdee & Williams, 1984; Reference Burns and BaleBurns & Bale, 1997), which profoundly affects these rates. The therapeutic style of individual consultants and their teams has also been shown to impact admission rates (Reference Croudace, Beck and HarrisonCroudace et al, 1997).
Most of the previous research on the association between psychiatric workload and socio-economic factors has concentrated on admission rates. Now that most of the workload of psychiatry services takes place in the community, more research is needed on community and primary care services for psychiatric disorders, and on factors that predict psychiatric workload in the community.





eLetters
No eLetters have been published for this article.