On 27 July 2000 the NHS Executive published guidelines that explicitly required NHS mental health services to maintain links with mentally disordered offenders (MDOs) during imprisonment if previously subject to the Care Programme Approach (CPA; Reference AdamAdam, 2000). The involvement of NHS mental health services in ‘sound discharge planning’ for prisoners about to be released from prison was also required.
The Review of Health and Social Services for Mentally Disordered Offenders and Others Requiring Similar Services (Reference ReedReed, 1992) recommended the diversion of prisoners with mental illness to health or social services facilities wherever possible. Although high rates of psychiatric morbidity among prisoners have long been established (Reference Gunn, Maden and SwintonGunn et al, 1991; Reference Davidson, Humphreys and JohnstoneDavidson et al, 1995; Reference Brooke, Taylor and GunnBrooke et al, 1996), many prisoners are insufficiently ill to require diversion from custody (Reference LartLart, 1997) but continue to require ongoing psychiatric treatment during their period of incarceration. Historically, psychiatrists have had limited involvement with local prisons in many areas of the country, leaving prison health care staff to manage all but those with most severe mental illness within the confines of the custodial system and with little additional specialist psychiatric input.
The NHS Executive guidelines (Reference AdamAdam, 2000) high-lighted the shared responsibilities of prison and NHS mental health services in ensuring appropriate liaison in the care of MDOs. Pre-existing health care arrangements have done little to facilitate this approach and have at times led to confusion regarding the responsibilities of psychiatric services to patients, both in prison and on release.
We are unaware of any previous study evaluating the role of the consultant psychiatrist in the on-going care of previously known patients serving custodial sentences and we undertook this study to gain an impression of contemporary practice prior to the publication of the NHS Executive Directive.
The study aimed to estimate the level of liaison between prisons and consultant psychiatrists in general psychiatric services and to assess the consultants' perceptions of their role in the care of patients in prison.
Method
A questionnaire was sent to 100 randomly selected consultant psychiatrists in the West Midlands approved under Section 12(2) of the Mental Health Act 1983. Those in substantive posts, listed without sub-specialities in the Section 12(2) approved register, were contacted. There were four questions:
-
(1) If one of your patients was in prison, how often would you ever be made aware of this?
-
(2) If you were aware that your patient was in prison, what responsibility would you feel you had?
-
(3) If your patient was released from prison, what follow-up would you suggest?
-
(4) If you were contacted by prison diversion services or prison health care staff regarding serious concerns over the mental health of a prisoner previously unknown to you but about to be released, how would you respond?
Multiple responses are additional comments were invited. The survey was undertaken prior to the release of the NHS Executive guidelines.
Results
Fifty-nine consultants replied. Most (73%) felt that information regarding imprisoned patients was infrequently communicated. Twenty-five per cent (15) had never been made aware of a patient of theirs in prison. A further 42% (24) estimated they were informed less than half of the time. When asked about responsibility for imprisoned patients 10 consultants (17%) believed they had no responsibility in this situation. Sixty-one per cent (36) said they would offer information or advice to prison staff. Twenty-six per cent (15) would make contact with the patient in prison.
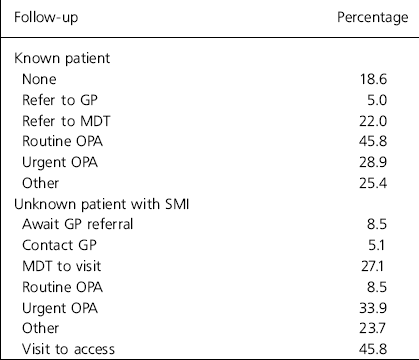
Table 1 shows choice of follow-up for (a) a known patient and (b) an individual with severe mental illness imminently due for release from prison. Some consultants stated that they would offer no direct input, four stating they believed the mental health needs of imprisoned patients with mental disorder were the remit of specialist forensic and prison health care services.
Table 1. Summary of preferred follow-up arrangements of prisoners with mental disorder
| Follow-up | Percentage |
|---|---|
| Known patient | |
| None | 18.6 |
| Refer to GP | 5.0 |
| Refer to MDT | 22.0 |
| Routine OPA | 45.8 |
| Urgent OPA | 28.9 |
| Other | 25.4 |
| Unknown patient with SMI | |
| Await GP referral | 8.5 |
| Contact GP | 5.1 |
| MDT to visit | 27.1 |
| Routine OPA | 8.5 |
| Urgent OPA | 33.9 |
| Other | 23.7 |
| Visit to access | 45.8 |
Comment
The results of this study suggest that liaison between prison and mental health services may be suboptimal: notification of imprisonment of patients with mental disorder generally being infrequent. The majority of consultants who responded did feel obliged to continue involvement in the care of known patients if notified of their imprisonment, but would take a case-by-case approach, seeking relevant information to determine the most appropriate course of action. A significant proportion of consultants believed that their responsibility to patients ended completely when a period of incarceration began, rejecting even involvement on a liaison/information-sharing basis. The scenarios upon which the survey questions were based are common and prison psychiatric liaison services may experience some resistance from general psychiatric services when patients are re-referred.
In most cases there is acknowledgement by consultant psychiatrists that general psychiatric services can play a useful part in the on-going care of MDOs in prison, but that the opportunity to do so may be limited by poor communication. In some cases a change in awareness of responsibilities may be required: by both NHS mental health care professionals and prison staff.
For the NHS Executive Directive to be implemented, a minimum requirement would be that CPA coordinators ‘remain in contact with the care and treatment of individuals receiving CPA who enter the prison system’ (Reference AdamAdam, 2000), being aware of their location and likely release date. Prison services must cooperate in the provision of appropriate mental health screening of prisoners and the communication of relevant information to appropriate agencies to ensure continuity of care and to facilitate discharge planning with the full involvement of the mental health care coordinator. A balance must be achieved to ensure that a multi-agency approach is practised rather than a shifting of duty of care between NHS and prison services.
High rates of psychiatric morbidity (Office for National Statistics, 1998) and poor health care arrangements in prisons (Reference Reed and LyneReed & Lyne, 1997) have been widely acknowledged, long-standing and persistent (Reference Reed and LyneReed & Lyne, 2000). Non-NHS provision of prison health care has encouraged neither a multi-disciplinary approach nor a working alliance with NHS services. This compounds the problems associated with the management of MDOs who are often difficult to engage in treatment. Existing arrangements for linking prisoners into community services on release are limited (National Association for the Care and Resettlement of Offenders, 1993) and the risk of patients with severe and enduring mental illness being lost to follow-up is high. The development of a closer partnership between prison and the NHS, and the extension of the CPA into prisons aims to limit this (HM Prison Service & NHS Executive, 1999).
Increasingly prompt, accurate, efficient communication between prison and psychiatric services is necessary in the transition to a seamless, multiagency approach to the care of imprisoned MDOs.
Inevitably there will be implications for service provision, funding and organisational structure. In the long term the aim should be to improve care of people with mental illness both in prison and in the community and for effective treatment and management opportunities to be maximised.




eLetters
No eLetters have been published for this article.