There is evidence that following the introduction of neuroleptics in the 1950s there was a steady increase in the average dose of neuroleptic prescribed — ‘if it's good — give more of it’ (Reference ColeCole, 1982). Baldessarini et al's review in 1988 gave strong evidence that very high doses are overall countertherapeutic and produce excessive sedation, neurological extrapyramidal symptoms and iatrogenic negative symptoms. More recently a meta analysis has concluded that ‘moderate’ doses of neuroleptics (165-375 mg chlorpromazine equivalents) are preferable in long-term treatment of chronic patients with schizophrenia (Reference Bollini, Pampallona and OrzaBollini et al, 1994).
There are significant differences in the pharmacokinetics and pharmacodynamics of neuroleptics between individuals (Reference Ko, Korpi and LinnoilaKo et al, 1985; Reference Van TOL, Wu and GuanVan Tol et al, 1992) and across ethnic groups (Reference Lin, Anderson and PolandLin et al, 1995) — such that different people given the same oral dose will have widely differing blood levels of the drug and will respond differently. Response to neuroleptics is invariably measured according to subjective symptoms and signs, and there are no objective patient indicators to guide dose ranges for neuroleptic prescribing. For these reasons there is no clear relationship between neuroleptic dose and clinical response (Reference Baldessarini, Cohen and TeicherBaldessarini et al, 1988), and more scope for variation in dose to relate to prescriber habits. The few studies that have examined the relationship of neuroleptic dose to prescriber, environmental and patient history variables demonstrate an association of higher neuroleptic dose with a history of violence; recent disruptive or violent behaviour; treatment non-responsiveness; and longer duration of admission (Reference Krakowski, Kunz and CzoborKrakowski et al, 1993; Reference Chaplin and McGuiganChaplin & McGuigan, 1996; Reference Peraltav, Cuesta and CaroPeralta et al, 1994). These studies suggest higher dose prescription relates more to patients' history than to current variables such as age, weight, diagnosis or mental state. We examined the relationship between total neuroleptic prescribing and high dose neuroleptic prescribing against relevant patient and prescriber variables for all patients at a psychiatric hospital that had acute, rehabilitation and forensic patients.
Method
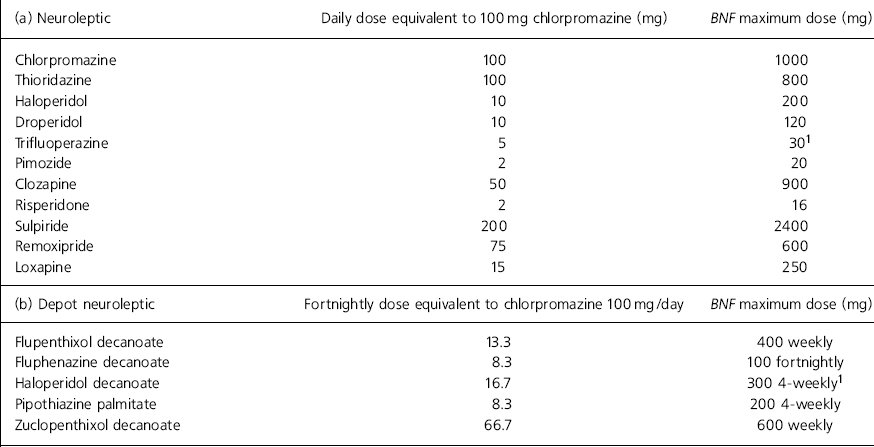
Over a 3-day period in mid-1994 we recorded a variety of historical, demographic and diagnostic information from the case notes of all patients in the acute, rehabilitation and forensic wards. This information was supplemented by interviewing the nursing staff to establish: the patients' ethnic grouping as defined by the UK Office of Population Censuses and Surveys; and the patients' behaviour over the past week. Regular oral, depot, as required and one-off neuroleptic doses given were converted into daily oral chlorpromazine equivalents according to generally used ratios (Reference FosterFoster, 1993; available from the author upon request) and the British National Formulary (BNF; British Medical Association & Royal Pharmaceutical Society, 1994) — see Table 1. For each patient a figure could thus be calculated for total daily neuroleptic dispensed in chlorpromazine equivalents. Any individual prescription of neuroleptics above or at the top of the BNF recommended dose range (BNF maximum) was also recorded. Because trifluoperazine and depot haloperidol are not given a BNF maximum dose, these were given BNF maximum doses of 30 mg/day and 300 mg 4 weekly, respectively.
Table 1. Oral and depot neuroleptic conversion chart and maximum British National Formulary (BNF) dose
| (a) Neuroleptic | Daily dose equivalent to 100 mg chlorpromazine (mg) | BNF maximum dose (mg) |
| Chlorpromazine | 100 | 1000 |
| Thioridazine | 100 | 800 |
| Haloperidol | 10 | 200 |
| Droperidol | 10 | 120 |
| Trifluoperazine | 5 | 301 |
| Pimozide | 2 | 20 |
| Clozapine | 50 | 900 |
| Risperidone | 2 | 16 |
| Sulpiride | 200 | 2400 |
| Remoxipride | 75 | 600 |
| Loxapine | 15 | 250 |
| (b) Depot neuroleptic | Fortnightly dose equivalent to chlorpromazine 100 mg/day | BNF maximum dose (mg) |
| Flupenthixol decanoate | 13.3 | 400 weekly |
| Fluphenazine decanoate | 8.3 | 100 fortnightly |
| Haloperidol decanoate | 16.7 | 300 4-weekly1 |
| Pipothiazine palmitate | 8.3 | 200 4-weekly |
| Zuclopenthixol decanoate | 66.7 | 600 weekly |
Chi-squared (χ2) analysis and analysis of variance were used to examine the relationship of the above variables to above and below BNF maximum prescribing and to chlorpromazine equivalent dose, respectively.
A stepwise logistic regression analysis was used entering aggression variables first including history of aggression; current verbal aggression, current physical aggression and 5-year history of neuroleptic prescription, the second step included entering current absconding and other current negative behaviour and self-harm. The predictor variables were regressed on, high v. low chlorpromazine equivalent patients. Cases were selected at the 75 percentile (1462 mg) to include 50 patients for the high chlorpromazine equivalents and the low, at the 25 percentile (400 mg) was represented by 56 patients. The same predictors were also used for above v. below BNF maximum dose cases. In the case of above BNF maximum dose, a random selection of below BNF maximum patients were matched to the above BNF maximum cases. The unique contribution of each predictor was observed in order to reduce type one error susceptibility with multiple univariate comparisons. Cell sizes for each group of high v. low chlorpromazine dose and above v. below BNF prescription were large enough to meet statistical power for each regression procedure (Reference Tabachnick and FidellTabachnick & Fidell, 1989). All tests were conducted using SPSS for Windows (Reference NorusisNorusis, 1994).
Results
Data were collected from 225 patients. Of these patients 202 (90%) were on regular depot or oral neuroleptic medication. Of these 77 (38%) were women and 125 (62%) men. The age range was 18-76, mean 39.9 years for the whole sample, 42.4 years for women and 38.3 years for men. For the 202 patients ICD—9 diagnoses (World Health Organization, 1978) were collapsed into seven broad diagnostic categories as follows: schizophrenia 147 (73%); other non-affective psychoses 16 (8%); bipolar affective disorder 14 (7%); affective and adjustment disorders 11 (5%); personality disorders 8 (4%); organic conditions 4 (2%); and other 2 (1%). Chlorpromazine equivalent dose ranged from 25 mg to 7500 mg, mean 1207 mg. Eleven consultants were responsible for the management of the 202 patients. Of the 202 patients a total of 41 patients were either at or above BNF maximum.
Univariate analyses
Setting was divided into acute wards (n=86, 42.6%), rehabilitation wards (n=71, 35.1%) and forensic wards (n=45, 22.3%). There was a highly significant difference between consultants in chlorpromazine equivalents prescribed (F=3.61; df=201; P=0.0002). Post hoc analysis revealed that one forensic consultant prescribed significantly higher chlorpromazine equivalent doses than eight of the other 10 consultants. This consultant gave rise to a significantly higher chlorpromazine equivalent prescribing in the forensic compared to the acute setting (F=5.15; df=201; P=0.007), which disappeared when this consultant was removed from the comparison between settings.
Differences were observed between the two consultants within the rehabilitation setting for both above BNF (χ2=4.38; df=1; P=0.036) and chlorpromazine equivalents prescription (F=10.1; df=71; P=0.002), revealing that one rehabilitation consultant prescribed consistently higher than the other consultant despite similar patient numbers and profile.
The UK Office of Population Censuses and Surveys categories were collapsed into White, n=146 (72.3%), Black African or Caribbean, n=33 (16.3%), and other, n=23 (11.3%). No interaction effect was observed between ethnicity and chlorpromazine equivalent dose, nor did it discriminate between above and below BNF classifications.
Analysis of variance revealed a significant difference between diagnostic groups, with schizophrenia and other psychoses having higher average chlorpromazine doses prescribed (F=2.53; df=200; P=0.02).
Of the 202 patients 25 were on as required benzodiazepines and 13 on regular benzodiazepines. Neither of these categories contributed to any significant difference in chlorpromazine equivalent prescription.
Multivariate analyses
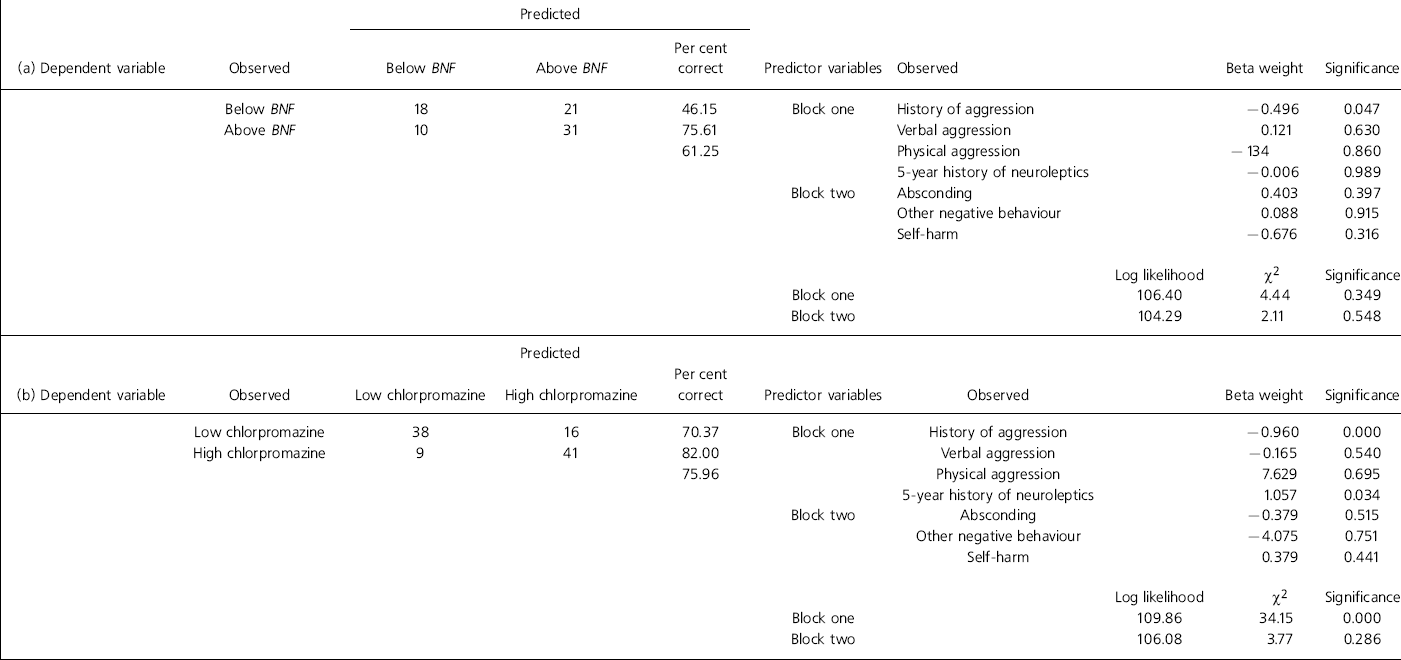
The stepwise logistic regression model for the above and below BNF maximum classifications did not significantly improve the constant with the classification table not providing above chance results (see Table 2). History of aggression was a significant predictor in the first block of variables (P<0.05). The other current behaviour variables did not contribute to above and below BNF dose classification.
Table 2. Results of the logistic regression analysis for maximum British National Formulary (BNF) dose and chlorpromazine dose
| Predicted | |||||||||
| (a) Dependent variable | Observed | Below BNF | Above BNF | Per cent correct | Predictor variables | Observed | Beta weight | Significance | |
| Below BNF | 18 | 21 | 46.15 | Block one | History of aggression | -0.496 | 0.047 | ||
| Above BNF | 10 | 31 | 75.61 | Verbal aggression | 0.121 | 0.630 | |||
| 61.25 | Physical aggression | -134 | 0.860 | ||||||
| 5-year history of neuroleptics | -0.006 | 0.989 | |||||||
| Block two | Absconding | 0.403 | 0.397 | ||||||
| Other negative behaviour | 0.088 | 0.915 | |||||||
| Self-harm | -0.676 | 0.316 | |||||||
| Log likelihood | χ2 | Significance | |||||||
| Block one | 106.40 | 4.44 | 0.349 | ||||||
| Block two | 104.29 | 2.11 | 0.548 | ||||||
| Predicted | |||||||||
| (b) Dependent variable | Observed | Low chlorpromazine | High chlorpromazine | Per cent correct | Predictor variables | Observed | Beta weight | Significance | |
| Low chlorpromazine | 38 | 16 | 70.37 | Block one | History of aggression | -0.960 | 0.000 | ||
| High chlorpromazine | 9 | 41 | 82.00 | Verbal aggression | -0.165 | 0.540 | |||
| 75.96 | Physical aggression | 7.629 | 0.695 | ||||||
| 5-year history of neuroleptics | 1.057 | 0.034 | |||||||
| Block two | Absconding | -0.379 | 0.515 | ||||||
| Other negative behaviour | -4.075 | 0.751 | |||||||
| Self-harm | 0.379 | 0.441 | |||||||
| Log likelihood | χ2 | Significance | |||||||
| Block one | 109.86 | 34.15 | 0.000 | ||||||
| Block two | 106.08 | 3.77 | 0.286 | ||||||
In the stepwise logistic regression model for high v. low chlorpromazine dose the first group of variables significantly contributed to the classification (χ2=34.15, P<0.0001) with history of aggression (P<0.001) and history of 5-year neuroleptic prescription (P<0.05) being significant predictors (see Table 2). When the second block of variables were entered into the equation they did not improve the fit of the model observing a non-significant χ2 result. The classification results demonstrated the 70% of high and 82% of low chlorpromazine equivalent patients being correctly classified with an overall classification of 76%.
Discussion
This study aimed to tease out factors contributing to high dose neuroleptic prescription. Studies of this nature necessarily have to deal with neuroleptic equivalents, for which there is no absolute and agreed method of derivation. This needs to be borne in mind when interpreting the results. Another potential criticism of the study is the use of nurses' subjective ratings of behaviour over the week — we reasoned that although this was a ‘rough and ready’ measure that might miss some minor behaviour problems, it would reasonably accurately detect major problems because these are invariably a matter of note for nursing staff.
At the time of the study 20% (41/202) of in-patients on neuroleptics were prescribed at or above BNF maximum, indicating that it is not uncommon for patients to be prescribed at or above the top of the therapeutic range, particularly when forensic and rehabilitation patients are included in the sample.
This study demonstrates the importance of individual consultants in determining neuroleptic prescription. This is supported by two results. First, one consultant was found to prescribe significantly higher chlorpromazine equivalence than eight of the other ten consultants. This cannot be explained merely by a difference in this consultant's case-load because despite the fact this consultant was prescribing in a forensic setting, the allocation of patients to the four forensic consultants was random. When this consultant was taken out of the analysis the difference between the forensic and acute settings became non-significant, indicating this consultant's prescribing habits were solely responsible for the observed difference between the forensic and acute settings. Second, within the rehabilitation setting one consultant prescribed consistently more both in terms of above BNF maximum and chlorpromazine equivalents, despite both consultants having demographically and diagnostically equivalent case-loads.
Ethnicity did not contribute to differences in neuroleptic prescription. It has been suggested that Black patients are medicated to a higher degree than White patients (Reference Strakowski, Shelton and KobrenerStrakowski et al, 1993) — this study found no evidence to support this. Unlike an earlier study (Krakowsi et al, 1993) we did not demonstrate an effect of length of admission on neuroleptic prescription, but noted a significant but small contribution of increased age and length of illness to higher chlorpromazine equivalent prescription. This may relate to the possibility that as a psychotic illness progresses, neuroleptic dose is frequently increased by a succession of different doctors, but is less often reduced — on the basis that ‘they must be on that dose for a good reason’. Having age and length of illness as significant predictors for chlorpromazine equivalent prescription indicates that patients accumulate higher doses of medication as an index of time rather than the severity of their illness.
The logistic regression clearly confirmed previous findings that history of violence predicts higher neuroleptic prescription (Reference Krakowski, Kunz and CzoborKrakowski et al, 1993; Reference Chaplin and McGuiganChaplin & McGuigan, 1996), but did not demonstrate any contribution of disturbed behaviour during the last week on neuroleptic prescription, unlike previous studies (Reference Krakowski, Kunz and CzoborKrakowski et al, 1993; Reference Chaplin and McGuiganChaplin & McGuigan, 1996; Reference Peraltav, Cuesta and CaroPeralta et al, 1994). This suggests that patients' reputation and history influences neuroleptic prescription far more than their current presentation. The only other significant predictor of high neuroleptic prescription was a positive history of larger than 5-years' neuroleptic prescription. Again this supports the notion that over time the dose of neuroleptic is frequently increased to limit patients' undesirable behaviour and is not then subsequently lowered for fear of the behaviour returning, as previously suggested (Reference Van PUTTEN, Marder and MintzVan Putten et al, 1992). An alternative explanation is that patients with longer illnesses are on higher doses because there was a previous trend to prescribe higher doses, which they have remained on. If this was the case it still supports the argument that regular review and education of neuroleptics does not occur.
In summary this study shows three things: certain consultants prescribe higher doses of neuroleptics than others; patients with a history of aggression get prescribed higher doses of neuroleptics; and third, patients who have been on neuroleptics longer than 5 years get prescribed higher doses. As our study did not look at patients over time it is possible that patients with a history of aggression had previously not responded to lower doses of neuroleptics and subsequently responded to higher doses. However, the alternative explanation is that psychiatrists are prescribing on the basis of prejudice relating to patients' previous behaviour, if this is true — then who are we treating?





eLetters
No eLetters have been published for this article.