With around 5000 people dying by suicide in England every year, suicide is a major public health issue (Department of Health, 2002). Luoma et al (Reference Luoma, Martin and Pearson2002) suggest that rates of contact by individuals before they died by suicide are significantly higher for primary care providers than for mental health service providers. In a systematic review of studies examining the extent to which individuals made contact with mental health and primary care providers before suicide, Luoma et al (Reference Luoma, Martin and Pearson2002) conclude that over half of those completing suicide had made contact with a primary care professional in the month before death, and around three-quarters had contact within 1 year of suicide.
Over recent years, the range of available primary care services in the UK has developed to include ‘fast access’ provision such as NHS ‘walk-in’ centres and NHS Direct. NHS Direct in particular is being increasingly used as a first point of contact for members of the public seeking health advice and information, with numbers of contacts averaging 500-600 000 calls a month (NHS Direct, 2005; Hansard, 2005). Calls relating to mental health form a small but significant proportion of this workload. NHS Direct operates as a telephone-based, ‘first level’ health screening and advice service. Clinical triage is performed by nurse advisors who use evidence-based algorithms within the NHS Clinical Assessment System to assess symptoms and provide advice, sign-posting and referral. A recent 3-month audit of the use of mental health algorithms showed that the depression screening algorithm was used 5374 times and the suicide algorithm was used 3976 times (NHS Direct unpublished data, details available from the authors on request).
This 2-year audit was designed to ascertain the proportion of suicides who had contacted NHS Direct in the year preceding their death, the reason for contact, the protocol used to assess the query and the advice given, and to compare characteristics of suicides in contact with NHS Direct with suicides in the same general population.
Method
Permission was obtained from all coroners in Hampshire and the Isle of Wight to allow NHS Direct to check names against NHS Direct databases. All persons who died by suicide (ICD-9 codes E950-959; World Health Organization, 1977) and deaths from similar causes on which an open verdict (ICD-9 E980-989, excluding E988.8) was recorded, collectively called ‘suicides’, were identified from coroners’ records in Hampshire and the Isle of Wight. Residents whose inquest was held outside the area were identified from mortality files (2002-2003) of the Office for National Statistics. A very few inquests held in 2003 and 2004 might have been missed because they did not appear on the 2003 mortality file or occurred outside the area during 2004. Names of those dying by suicide between 1 September 2002 and 31 August 2004 inclusive, who were either residents of Hampshire or the Isle of Wight, or whose inquest was held by a coroner in this area, were checked against the records of NHS Direct Hampshire and the Isle of Wight.
Results
Characteristics of suicides
A verdict of suicide or open verdicts were returned on 278 residents of Hampshire or the Isle of Wight who died between 1 September 2002 and 31 August 2004 inclusive. Thirty (10.8%) of these residents had telephoned NHS Direct within 12 months of their death.
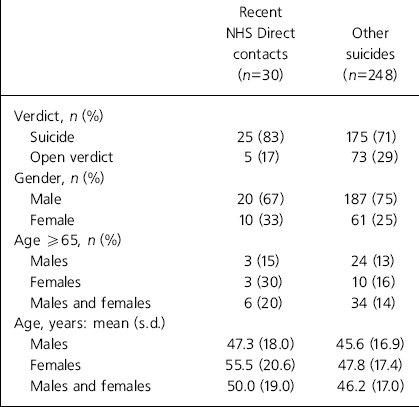
There was no significant difference between the 30 recent NHS Direct contacts and the other suicides with respect to the proportion of suicide (83 v. 71%), males (67 v. 75%), mean age (50 years (s.d.=19.0) v. 46.2 years (s.d.=17.0 years)) (Table 1), or cause of death (33% fatal overdose v. 27% fatal overdose). The only significant difference was in the greater proportion of Isle of Wight residents (25%) who had contacted NHS Direct compared with 8.4% of Hampshire residents dying by suicide (difference 16.6%, 95% CI 2.7-30.5, P=0.05).
Table 1. Characteristics of suicides in contact with NHS Direct in the year before death and other suicides in Hampshire and the Isle of Wight
| Recent NHS Direct contacts (n=30) | Other suicides (n=248) | |
|---|---|---|
| Verdict, n (%) | ||
| Suicide | 25 (83) | 175 (71) |
| Open verdict | 5 (17) | 73 (29) |
| Gender, n (%) | ||
| Male | 20 (67) | 187 (75) |
| Female | 10 (33) | 61 (25) |
| Age ⩾65, n (%) | ||
| Males | 3 (15) | 24 (13) |
| Females | 3 (30) | 10 (16) |
| Males and females | 6 (20) | 34 (14) |
| Age, years: mean (s.d.) | ||
| Males | 47.3 (18.0) | 45.6 (16.9) |
| Females | 55.5 (20.6) | 47.8 (17.4) |
| Males and females | 50.0 (19.0) | 46.2 (17.0) |
The male/female ratio for all suicides from Hampshire and the Isle of Wight and for those not in recent contact with NHS Direct was 3:1, which is similar to that in England and Wales. The gender profile among recent NHS Direct contacts (male/female ratio 2:1) is roughly the reverse of the usual gender profile for NHS Direct whereby female callers constitute about six of every ten calls.
Frequency of contact
Although 18 (60%) callers had made only one call, the number of calls made by an individual ranged from 1 to 12. More males (14: 70%) than females (4: 40%) made only one call but the gender difference was not significant.
Interval between last call and date of death
The interval between the last contact with NHS Direct and death ranged from 1 to 315 days. Significantly more females (5: 50%) than males (2: 10%) had contacted NHS Direct in the 2 weeks before death (difference 40%, 95% CI 6.3-3.7, P=0.05). There was no significant difference between the proportion of calls relating to physical health among the 7 calls made within 2 weeks of death (2: 28.6%) and the 23 calls made between 2 weeks and 12 months before death (14: 60.9%, difference 32.3%, 95% CI –71.3 to 6.7) or between the proportions of the mental health-related calls in the 2 weeks before death (3: 42.9%) and between 2 weeks and 12 months before death (6: 26.1%, difference 16.8%, 95% CI –24.0 to 57.6).
Reasons for calling and screening algorithms
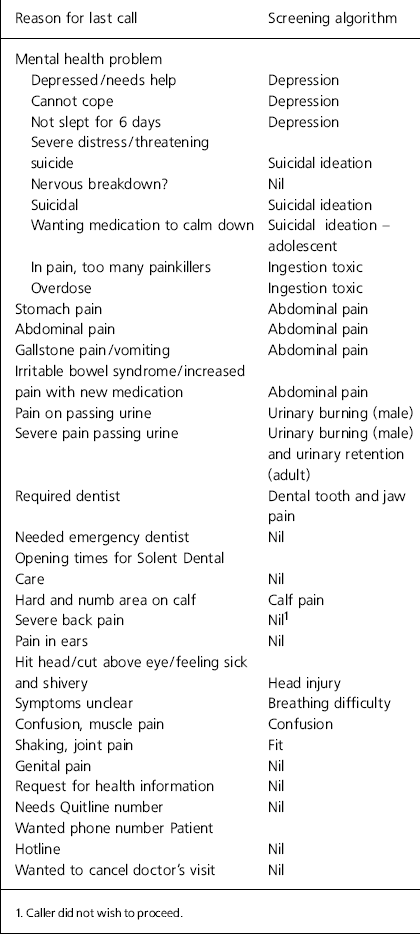
The ‘call reason’ is a brief description of the caller's presenting problem as logged by the call-handler prior to the call being passed either to a nurse advisor for clinical assessment of symptoms or - for non-symptomatic calls - to a health information advisor for provision of health information. Although mental health problems (including 3 reporting suicidal ideation) accounted for 9 of the last calls made by the 30 people dying by suicide (Table 2), physical health problems were the reason for the majority of calls (17). Pain was mentioned by 16 callers. Mental health algorithms were used in 8 of the 30 calls. However, the majority of calls appeared to be primarily about physical problems and this was reflected in the algorithms selected by the nurse advisors.
Table 2. Summary of reason for last call to NHS Direct and screening algorithm used
| Reason for last call | Screening algorithm |
|---|---|
| Mental health problem | |
| Depressed/needs help | Depression |
| Cannot cope | Depression |
| Not slept for 6 days | Depression |
| Severe distress/threatening suicide | Suicidal ideation |
| Nervous breakdown? | Nil |
| Suicidal | Suicidal ideation |
| Wanting medication to calm down | Suicidal ideation - adolescent |
| In pain, too many painkillers | Ingestion toxic |
| Overdose | Ingestion toxic |
| Stomach pain | Abdominal pain |
| Abdominal pain | Abdominal pain |
| Gallstone pain/vomiting | Abdominal pain |
| Irritable bowel syndrome/increased pain with new medication | Abdominal pain |
| Pain on passing urine | Urinary burning (male) |
| Severe pain passing urine | Urinary burning (male) and urinary retention (adult) |
| Required dentist | Dental tooth and jaw pain |
| Needed emergency dentist | Nil |
| Opening times for Solent Dental Care | Nil |
| Hard and numb area on calf | Calf pain |
| Severe back pain | Nil1 |
| Pain in ears | Nil |
| Hit head/cut above eye/feeling sick and shivery | Head injury |
| Symptoms unclear | Breathing difficulty |
| Confusion, muscle pain | Confusion |
| Shaking, joint pain | Fit |
| Genital pain | Nil |
| Request for health information | Nil |
| Needs Quitline number | Nil |
| Wanted phone number Patient Hotline | Nil |
| Wanted to cancel doctor's visit | Nil |
Advice given
Over half the calls resulted in a referral to general practitioner (GP) services. Eleven callers were advised to contact their GP urgently (as soon as possible or within 4 hours) and one was advised to attend an accident and emergency department as soon as possible. Over a quarter of calls resulted in the provision of health information as opposed to onward referral.
Discussion
The similarities between the NHS Direct callers and other suicides in Hampshire and the Isle of Wight suggest that the callers are a representative sample. The high incidence of physical problems, particularly problems associated with pain, relative to mental health problems in this population was unexpected and merits further investigation. Since it has been reported that suicidal intent is discussed in only 22% of last primary care consultations (Reference Isometsa, Heikkinen and MarttunenIsometsa et al, 1995), the identification of such intent in NHS Direct contacts presents a challenge.
Conclusions
The information gleaned from this small sample of calls highlights the potential role of NHS Direct in the identification, assessment and referral of individuals who may be at risk of suicide. The preliminary findings suggest a higher than expected number of completed suicides of individuals presenting with purely physical symptoms. There is clearly scope for examining the extent to which the current NHS Direct screening process succeeds in identifying and assessing suicidal symptoms, and how it could be developed to elicit suicidal ideation which might be masked by a somatic presentation.
The NHS Direct system of routinely recording all patient contacts as part of the clinical case record provides a unique and hitherto untrodden path into the field of suicide research, as it offers the potential to listen to the voice of the individual at a critical time prior to death. Clearly, the length of the interval between the last call and the date of death will be a significant factor in selecting those calls which could benefit from examination. A formal analysis of such calls made within a defined time frame using qualitative research methods may provide valuable clues to the caller's mental state at the time of the call and offer the potential to develop improvements in service response to such callers.
Declaration of interest
None.
Acknowledgements
We thank the coroners in Hampshire and the Isle of Wight; Anna Walker (formerly Mental Health Lead at NHS Direct, Hampshire) who acted as liaison between NHS Direct and the University of Southampton Mental Health Group and who, with the assistance of Caren Sargant (nurse advisor), matched the names provided by the coroner to records in the NHS Direct database; the NHS Direct Mental Health Team and all other staff at NHS Direct for providing valuable feedback on the preliminary drafts.





eLetters
No eLetters have been published for this article.