Background
In Sweden, as in many other countries, population ageing has become a political challenge as more people reach old age (Statistics Sweden, 2009). Old age often means a decline in personal, physical, psychological and social capacity (Grimby and Svanborg, Reference Grimby and Svanborg1996; Winblad et al., Reference Winblad, Jaaskelainen, Kivela, Hiltunen and Laippala2001; Sherman et al., Reference Sherman, Forsberg, Karp and Törnkvist2012) because of biological changes and health behavioural factors such as unhealthy eating habits, inactivity, smoking, excessive alcohol intake and previous work environment. In order to promote health and to prevent diseases, it is essential to enhance self-esteem, identify early symptoms of ill health and recognise risk factors for chronic diseases (Mehr and Tatum, Reference Mehr and Tatum2002; Sandhu and Barlow, Reference Sandhu and Barlow2002; Heikkinen, Reference Heikkinen2003; Mckevith, Reference Mckevith2005). Health promotion encompasses health education and health protection, as well as all environmental and legislative changes to promote good health in both the individual and the community. Disease prevention, on the other hand, refers to actions taken to reduce or eliminate risks of specific diseases (Janlert and Folkhälsoinstitutet, Reference Janlert2000). One method of promoting health and well-being among older persons is preventive home visits (PHVs). The aim of such visits is to prevent diseases, delay the onset of impairment and promote health. A PHV is a scheduled contact that aims to offer older persons the opportunity to discuss their health in a structured way, support personal resources, enhance empowerment and permit the health visitors to form an opinion of the older persons’ living environments (Hendriksen and Vass, Reference Hendriksen and Vass2005; Vass et al., Reference Vass, Avlund, Hendriksen, Philipson and Riis2007). Although the effects of PHVs have been studied for more than four decades, there is still no consensus about how to best perform them. The studies vary with regard to number of contacts (from 24-h telephone support to one PHV per year), follow-up periods (one to four years), age of older persons (⩾65, ⩾70, ⩾75, ⩾80 years), methods (assessment tools, interviews, education, future health plans, medication reviews and medical examinations), target group (healthy or frail older persons) and professionals performing the visits (volunteers, registered nurses, geriatric nurses, public health nurses, community nurses, social workers, physiotherapists and occupational therapists). Since 2000, eleven systematic reviews and meta-analyses (Byles, Reference Byles2000; van Haastregt et al., Reference Van Haastregt, Diederiks, Van Rossum, De Witte and Crebolder2000; Elkan et al., Reference Elkan, Kendrick, Dewey, Hewitt, Robinson, Blair, Williams and Brummell2001; Stuck et al., Reference Stuck, Egger, Hammer, Minder and Beck2002; Ploeg et al., Reference Ploeg, Feightner, Hutchison, Patterson, Sigouin and Gauld2005; Beswick et al., Reference Beswick, Rees, Dieppe, Ayis, Gooberman-Hill, Horwood and Ebrahim2008; Bouman et al., Reference Bouman, Van Rossum, Nelemans, Kempen and Knipschild2008; Fagerstrom et al., Reference Fagerstrom, Wikblad and Nilsson2008; Huss et al., Reference Huss, Stuck, Rubenstein, Egger and Clough-Gorr2008; Stuck and Kane, Reference Stuck and Kane2008; Mayo-Wilson et al., Reference Mayo-Wilson, Grant, Burton, Parsons, Underhill and Montgomery2014) and one literature review (Markle-Reid et al., Reference Markle-Reid, Browne, Weir, Gafni, Roberts and Henderson2006) on PHVs to older persons have been published. The main objective of these reviews was to determine whether such visits were effective with regard to an older person’s health and well-being, and/or ask whether PHVs could benefit society as a whole. The results of these reviews showed that PHVs can have favourable effects on outcomes, including improving functional status (Stuck et al., Reference Stuck, Egger, Hammer, Minder and Beck2002, Markle-Reid et al., Reference Markle-Reid, Browne, Weir, Gafni, Roberts and Henderson2006, Fagerstrom et al., Reference Fagerstrom, Wikblad and Nilsson2008, Huss et al., Reference Huss, Stuck, Rubenstein, Egger and Clough-Gorr2008), preventing falls (Beswick et al., Reference Beswick, Rees, Dieppe, Ayis, Gooberman-Hill, Horwood and Ebrahim2008) and increasing quality of life (Byles, Reference Byles2000; Fagerstrom et al., Reference Fagerstrom, Wikblad and Nilsson2008). The results also showed that PHVs reduce the number of hospital admission (Elkan et al., Reference Elkan, Kendrick, Dewey, Hewitt, Robinson, Blair, Williams and Brummell2001; Ploeg et al., Reference Ploeg, Feightner, Hutchison, Patterson, Sigouin and Gauld2005; Markle-Reid et al., Reference Markle-Reid, Browne, Weir, Gafni, Roberts and Henderson2006; Fagerstrom et al., Reference Fagerstrom, Wikblad and Nilsson2008; Huss et al., Reference Huss, Stuck, Rubenstein, Egger and Clough-Gorr2008), use of health and social services (Markle-Reid et al., Reference Markle-Reid, Browne, Weir, Gafni, Roberts and Henderson2006; Stuck and Kane, Reference Stuck and Kane2008), mortality (Elkan et al., Reference Elkan, Kendrick, Dewey, Hewitt, Robinson, Blair, Williams and Brummell2001; Stuck et al., Reference Stuck, Egger, Hammer, Minder and Beck2002; Ploeg et al., Reference Ploeg, Feightner, Hutchison, Patterson, Sigouin and Gauld2005; Markle-Reid et al., Reference Markle-Reid, Browne, Weir, Gafni, Roberts and Henderson2006; Fagerstrom et al., Reference Fagerstrom, Wikblad and Nilsson2008; Huss et al., Reference Huss, Stuck, Rubenstein, Egger and Clough-Gorr2008) and cut healthcare costs (Stuck et al., Reference Stuck, Egger, Hammer, Minder and Beck2002; Markle-Reid et al., Reference Markle-Reid, Browne, Weir, Gafni, Roberts and Henderson2006). In three of these reviews, no effect was found (van Haastregt et al., Reference Van Haastregt, Diederiks, Van Rossum, De Witte and Crebolder2000; Bouman et al., Reference Bouman, Van Rossum, Nelemans, Kempen and Knipschild2008; Mayo-Wilson et al., Reference Mayo-Wilson, Grant, Burton, Parsons, Underhill and Montgomery2014). Recent scientific research shows that it is important to use a holistic approach when assessing an older person’s physical, psychosocial, medical and environmental situation (Sahlen et al., Reference Sahlen, Dahlgren, Hellner, Stenlund and Lindholm2006, Bouman et al., Reference Bouman, Van Rossum, Nelemans, Kempen and Knipschild2008; Lofqvist et al., Reference Lofqvist, Eriksson, Svensson and Iwarsson2012). Other aspects of an effective intervention include follow-up contacts (Stuck et al., Reference Stuck, Egger, Hammer, Minder and Beck2002; Huss et al., Reference Huss, Stuck, Rubenstein, Egger and Clough-Gorr2008), use of well-educated personnel (Avlund et al., Reference Avlund, Vass, Kvist, Hendriksen and Keilding2007) and use of a multidisciplinary team in which members of different professions work together (Vass et al., Reference Vass, Avlund, Hendriksen, Philipson and Riis2007; Dapp et al., Reference Dapp, Anders, Von Renteln-Kruse, Minder, Meier-Baumgartner, Swift, Gillmann, Egger, Beck and Stuck2011; Gustafsson et al., Reference Gustafsson, Wilhelmson, Eklund, Gosman-Hedstrom, Ziden, Kronlof, Hojgaard, Slinde, Rothenberg, Landahl and Dahlin-Ivanoff2012). Moreover, the older person must be taken seriously; he or she must be involved in decision making and informed about the services offered by the healthcare and the social care systems (Hendriksen and Vass, Reference Hendriksen and Vass2005, Vass et al., Reference Vass, Avlund, Hendriksen, Philipson and Riis2007).
In 2006, the Executive Board of the Stockholm County Council, Sweden, decided to implement PHVs to 75-year-olds that were to be performed by district nurses (DNs). It was widely considered suitable for DNs to perform PHVs, as the task was in agreement with their daily work activities and as they work closely with family doctors and other staff at the healthcare centres (HCCs) and in the local community (Karolinska Institutet, 2010). The decision to focus on 75-year-olds was made because previous research showed that PHVs were most effective when they were performed before older persons reached the age of 77 years; in other words, before the older persons become too ill (Stuck et al., Reference Stuck, Egger, Hammer, Minder and Beck2002; Huss et al., Reference Huss, Stuck, Rubenstein, Egger and Clough-Gorr2008). In addition, many studies use the age 75 as a turning point when studying the effects of PHVs (Robichaud et al., Reference Robichaud, Herbert, Roy and Roy2000; Newbury et al., Reference Newbury, Marley and Beilby2001; Gill et al., Reference Gill, Baker, Gottschalk, Peduzzi, Allore and Byers2002; Henderson, Reference Henderson2005).
The lack of knowledge regarding the effectiveness of PHVs that DNs make to 75-year-olds makes it important to investigate this area further. Therefore, the aim of this study was to analyse the effects of PHVs by DNs on the self-reported health of 75-year-olds, including changes in self-reported health after the visits. The study also aimed to investigate whether the 75-year-old participants believed the visit was useful or not. To the best of our knowledge, no other study has focussed on the effects of preventive visits by DNs to 75-year-olds living at home.
Method
Study design
The study had a controlled design. Eight HCCs assigned to a study group (SG) and eight HCCs assigned to a control group (CG) were randomly selected from five geographical medical areas in the county of Stockholm. Data were collected between the first of March 2006 and the middle of March 2007 via a questionnaire sent to all 75-year-olds before and after the intervention. The SG received a PVH, whereas the CG was treated as usual.
Participants and settings
In 2006, the Stockholm County Council area included ∼2 million residents, 10 644 of whom were 75 years old (Sherman et al., Reference Sherman, Söderhielm Blid, Törnkvist, Karp and Wånell2007), and comprised five distinct geographical areas that included 190 HCCs. All five geographical areas had approximately the same number of residents (Statistics Sweden, 2009) and included both urban and rural communities. To be eligible for inclusion, an HCC had to have at least three DNs employed [at the time just over 900 DNs worked for the Stockholm County Council (Falk and Törnkvist, Reference Falk and Törnkvist2006)]. A total of 124 HCCs fulfilled this inclusion criterion.
To randomly select HCCs for the SG and CG, five boxes were prepared, one for each geographical area. The name of each HCC was written on a piece of paper and placed in one of the five boxes (20–30 HCCs in each box). Then 16 HCCs were randomly selected (between three and four HCCs from each box). Eight of these 16 HCCs were randomly assigned to the SG and the remaining eight to the CG.
Upon completion of the final stage of selection, the directors of the HCCs in the SG were contacted by telephone. They were given details about the study both orally and in writing. Thereafter, each director was asked to arrange a meeting between the researchers and the DNs working at the HCC. At the meeting, the DNs (n=35, three to seven DNs from each HCC) were given a full description of the study both orally and in writing. The DNs working at the HCCs in the CG were not given information about the study.
A description of the selection of HCCs and recruitment of 75-year-olds is shown in Figure 1.

Figure 1 Flow chart of the selection of the study participants
The 75-year-olds’ names and addresses were retrieved from the Stockholm county council’s database. A total of 385 older persons were registered at the eight HCCs in the SG and 405 at the eight HCCs in the CG. In March 2006, a study-specific questionnaire, an information letter and a self-addressed envelope were sent to the 75-year-old persons in the SG and CG. The letter informed them that participation was voluntary, explained how to answer the questionnaire and ensured them that their answers would be confidential. After two reminders, the response rate was 73% (n=280) in the SG and 75% (n=303) in the CG.
Between April and December 2006, each 75-year-old in the SG (n=385) was offered a PHV by a DN. A total of 59% (n=220) accepted the offer. Of those who declined (n=165), nine had died, five did not live at the address mentioned in their records, one lived in a nursing home, 23 could not be reached, 15 had dementia or had experienced a stroke, nine declared they were healthy and did not need a PHV, 85 had no interest in a PHV and 18 gave no reason for declining. The follow-up questionnaire was sent in March 2007 to the 75-year-olds in both the SG (then n=366) and the CG (then n=394). The response rate was 74% (n=271) in the SG and 73% (n=290) in the CG. In the case of the SG, the period between the PHV and the follow-up questionnaire ranged between 3 and 11 months. The median was 6 months, the first quartile was 5 months and the third quartile was 9 months. Of the 220 participants who received a PHV, 44 were excluded from the analysis because they did not return both questionnaires, as were 28 in the CG (marked as drop-outs on the flow chart). A total of 176 participants from the SG and 262 from the CG were included in the final analyses.
The intervention
The intervention took place over the course of one year and consisted of the following three parts: a one-day course for participating DNs on how to perform PHVs, the PHV and support for the 35 DNs during the intervention period.
The one-day course
The one-day course was specifically designed for DNs. In Sweden, DNs must complete a bachelor’s degree in nursing and 50 weeks of specialist training (the equivalent of 75 credits in the European Credit Transfer and Accumulation System). The DNs have comprehensive knowledge of primary healthcare nursing, disease prevention and health promotion and are skilled at meeting a number of medical and psychosocial healthcare needs. The specialization equips the DNs with the competence to care for people of all ages using a holistic approach in the patient’s home and/or at the HCC. DNs work closely with family doctors and other staff at the HCC and in the local community (Karolinska Institutet, 2010).
Learning outcomes of the one-day course were as follows:
∙ to identify the 75-year-olds’ health concerns and how these concerns were related to their living environment;
∙ to support the 75-year-olds’ self-care activities and help empower the 75-year-olds;
∙ to use a person-centred approach;
∙ to use nursing interventions and evaluate these interventions;
∙ to accurately document the PHV and update the medical records of the 75-year-olds.
During the course, the DNs received the following materials:
∙ A health dialogue guide adapted to the nursing process (Yura and Walsh, Reference Yura and Walsh1973) with keywords from the VIPS nursing documentation model (Ehnfors et al., Reference Ehnfors, Thorell-Ekstrand and Ehrenberg1991; Ehrenberg et al., Reference Ehrenberg, Ehnfors and Thorell-Ekstrand1996).
∙ Two books: Promoting health: a practical guide (in Swedish; Ewles and Simnett, Reference Ewles and Simnett2005) and Trends and health promotion in older people: an overview of current knowledge (in Swedish; Agahi, Reference Agahi2005).
∙ A folder with a template of a letter of invitation that offered a PHV, a brochure describing the process of record keeping in accordance with the VIPS model (Ehenfors et al., Reference Ehenfors, Angermo, Berring, Ehenberg, Lindhardt, Rotegard and Thorell-Ekstrand2006), a list of possible organizations and activities in the neighbourhood (eg, non-governmental organizations, leisure time activities, the local community service facilities and the county council facilities) and a brochure about safety at home for 75-year-olds.
∙ A list of the names and addresses of the 75-year-olds in the Stockholm county (list generated from the Stockholm county council database, ListOn).
Predetermined structure of the PHV
The DNs were asked to send a letter of invitation to the 75-year-olds in the SG to offer them a PHV. The nurses were instructed to wait for about two weeks and then contact the 75-year-olds to book a time for a PHV. During the PHV, the DNs were to follow the health dialogue guide prepared specially for the purpose of this study.
The health dialogue followed the nursing process: assessment of health, planning, diagnosis of health needs, nursing intervention and evaluation of nursing care, first described by Yura and Walsh (Reference Yura and Walsh1973). This nursing process is a person-centred model focussing on the human being. According to this model, the PHV is a meeting between two people having a dialogue, in this case about the 75-year-olds’ health and well-being and potential health problems. The health dialogue guide, shown in Figure 2, used assessment areas (categories) with key words from the VIPS nursing documentation model. In addition, the DNs offered to check the participant’s blood pressure. If the DNs observed any potential health problems, it was possible to evaluate them using various assessment tools. Furthermore, the DNs could prescribe health aid products for participants with diabetes or incontinence, check the older persons’ medication and co-ordinate care if needed. The 75-year-olds were given information about activities in the area where they lived, local community and county council facilities and a brochure about safety at home. Then the 75-year-olds and the DNs could decide whether follow-up contact was needed. The PHV was expected to last 60 min and to be documented in the 75-year-olds’ medical records.

Figure 2 An overview of the health dialogue guide used during the preventive home visit (PHV)
Support for the DNs during the intervention
The researchers offered to visit the HCC twice. Moreover, the DNs were able to telephone the researchers for help and support whenever needed.
Outcomes measures and data collection
The variables measured in March 2006 and at the one-year follow-up were as follows: the health index (HI), general health, health behaviour, health problems, knowledge about and contact with the local community and the county council and use of medication. The variables were measured by a 78-item questionnaire on self-reported health. The questionnaire sent out in 2006 was used to collect baseline data. At the one-year follow-up (March 2007), two questions were added to the questionnaire for the participants in the SG. These questions were about the participants’ experiences of the PHV and opinion about the usefulness of the PHV. In addition, the 75-year-olds were asked to complete a questionnaire on socio-demographic status.
The questionnaire
Socio-demographic status
Socio-demographic status was determined using the following three questions: sex, living arrangements and education. Response alternatives for living arrangements were as follows: living alone or living with someone. Response alternatives for education were as follows: elementary school, upper secondary school or university.
HI
The HI included 10 questions about health and well-being. The HI has often been used as a clinical instrument (Forsberg and Bjorvell, Reference Forsberg and Bjorvell1993; Langius and Lind, Reference Langius and Lind1995; Törnkvist et al., Reference Törnkvist, Strender and Gardulf2003). The first nine questions concerned energy, mood, fatigue, loneliness, sleep, vertigo, bowel function, pain and mobility. The total minimum score for these questions was 9 and the maximum was 36. The higher the score, the better the person’s perceived health and well-being. The 10th question was about perceived health and well-being during the previous week. Response alternatives for all the10 questions were as follows: ‘very poor’=1, ‘fairly poor’=2, ‘fairly good’=3 and ‘very good’=4. The HI used in this study has been validated elsewhere (Nordstrom et al., Reference Nordstrom, Nyman and Theorell1992; Forsberg and Bjorvell, Reference Forsberg and Bjorvell1993).
General health
General health was determined by the responses to four questions about how the 75-year-old perceived his or her health. The questions were as follows: ‘How do you evaluate your general health?’, ‘How do you evaluate your physical health?’, ‘How do you evaluate your psychological health?’ and ‘In your opinion, how does your health compare to that of others of the same age?’. The response alternatives were ‘very poor’=1, ‘fairly poor’=2, ‘fairly good’=3 and ‘very good’=4.
Health behaviour
Health behaviour was determined using eight questions: ‘Are you strict with what you eat?’, ‘Are you physically active and are you active regarding activities such as crossword puzzles, reading books etc.?’. Response alternatives were as follows: ‘not at all’=1, ‘sometimes’=2, ‘often’=3 and ‘always’=4. There were also questions about smoking, use of snuff (moist powdered tobacco) and alcohol intake. Response alternatives were ‘Yes’ or ‘No’.
Health problems
A total of 38 questions based on the VIPS documentation model were used. VIPS is the Swedish acronym for ‘well-being’, ‘integrity’, ‘prevention’ and ‘safety’, which are all important goals of nursing care. The model, based on the nursing process (Yura and Walsh, Reference Yura and Walsh1973), has been validated in primary healthcare settings by Ehnfors and Nordstrand (Reference Ehnfors and Nordstrand1995) and for recording pain by Törnkvist et al. (Reference Törnkvist, Gardulf and Strender1997; Reference Törnkvist, Strender and Gardulf2003). Nursing status describes a patient’s present health situation and conditions and is divided into categories, each including a different number of key words (Ehnfors et al., Reference Ehnfors, Ehrenberg and Thorell-Ekstrand2000; Ehenfors et al., Reference Ehenfors, Angermo, Berring, Ehenberg, Lindhardt, Rotegard and Thorell-Ekstrand2006). The following key words were used: communication: the ability to understand and communicate through sensory organs as evinced by hearing, sight, speech and taste; cognition/development: the capacity for understanding and memory; breathing/circulation: respiratory problems such as difficulty in breathing, coughing, angina pectoris, oedema, cold feet and vertigo; nutrition: underweight or overweight, difficulties in swallowing and nausea; elimination: patterns regarding urine and faeces; skin/integument: changes and disorders of the skin, mouth blisters and mouth disorders, itching, problems with mucous membranes and wounds or ulcers; ADL: functional ability in daily life, including cleaning, climbing stairs, walking indoors, walking outdoors, shopping, having something meaningful to do during the day, the ability to shower/bathe and the ability to take care of personal finances; sleep: sleeping problems and fatigue; pain: acute or chronic pain or discomfort; sexuality: perceived disturbances, demands and expectations; psychosocial: problems with emotional and social functions such as anxiety, low-spiritedness and loneliness. The statements were as follows: ‘I have a problem with’, ‘I need help with’ and ‘Not applicable’. Response alternatives were ‘Yes’ or ‘No’.
Knowledge about and contact with the local community and the county council
The 75-year-olds were asked three questions about their knowledge of where to turn for assistance such as obtaining walking sticks or incontinence aid, home-help service and leisure time activities. They were also asked three questions about their contact with their local HCC and DN and two about home-help service, both current and past. Response alternatives were ‘Yes’ or ‘No’.
Use of medication
The 75-year-olds were asked 10 questions about medication. These concerned whether they used prescribed medicines or sleeping pills, believed they used too much medication, thought they knew too little about their prescribed medicines, had difficulty taking their medicines, experienced side effects, had difficulty keeping the medicines in order, had difficulty remembering to take the medicines, had any help with their medication and used any naturopathic medicine. Response alternatives were ‘Yes’ or ‘No’.
Usefulness of the PHV
The 75-year-olds in the SG were asked two questions about their opinion of the PHVs. The first was ‘Did you find PHVs useful?’. Response alternatives were ‘Not useful at all’=1, ‘Somewhat useful’=2, ‘Useful’=3 and ‘Very useful’=4. The second was ‘Describe your experience from the PHV’; this was an open-ended question.
The questionnaire was tested first on eight 75-year-olds by eight DNs, after which minor modifications were made.
Analyses
A cluster-adjusted (hcc) χ 2-test was applied to identify socio-demographic differences between the 75-year-olds in the SG and those in the CG in 2006.
Health and well-being (HI scores), general health and health behaviour were dichotomized (1–2=poor health, 3–4=good health). The results are shown as a difference (%) between 2007 and 2006 for the SG and the CG. The difference was assessed by conditional logistic regression, and the HCCs were included to the factor in clustering. Treatment effect (difference between differences) was assessed by the interaction between time and group using logistic regression and including the HCCs as a cluster variable. Difference between the differences was estimated by margins and lincom in STATA (StataCorp LP, 2011). Overall HI was analysed in the same way, but using Poisson regression including the HCC as a cluster variable. Treatment effect is expressed as the difference between differences in mean counts for the SG and CG. Reported health problems were grouped together in categories. The results are shown as the difference in the mean number of health problems between 2007 and 2006 for the SG and CG. Difference between 2007 and 2006 for SG and CG, expressed as a P-value, was analysed using Poisson regression. Treatment effect (difference between differences based on the interaction between time and group) for VIPS was estimated by a Poisson model including HCC as a cluster variable, except for pain (i) and sexuality (k), which were analysed using logistic regression. Knowledge about and contact with the local community and county council and use of medication were analysed in two steps. First, conditional logistic regression including HCC as a cluster variable was used to assess the difference between 2007 and 2006. The results are shown as a difference and a P-value. Second, treatment effects were as assessed by the interaction between time and group and by a logistic model including HCC as a cluster variable. Difference between the differences with 95% confidence interval was assessed by margins and lincom in STATA (StataCorp LP, 2011).
Sample size
Sample size for a cluster design was calculated at 80% statistical power (α=0.05), assuming a minimal interesting difference of one problem (SD=3.3) between groups in the VIPS variable ‘summarized health problems’. Furthermore, 25 75-year-old persons were drawn in average from each of the selected HCCs, with an interclass correlation coefficient (ρ) of 0.01. The ratio between SG and CG was set to 1.5. Given these assumptions, 157 people were needed in the SG and 236 in the CG, and at least 16 clusters were needed. The calculations were performed by the STATA modules sampsi and sampclus.
Qualitative description
To describe the 75-year-olds’ experiences of the PHV (one open-ended question), the comments were sorted and categorized (Hsieh and Shannon, Reference Hsieh and Shannon2005).
Results
Socio-demographic status
There were no differences between the SG and CG at baseline regarding sex, living situation or education (Table 1).
Table 1 The 75-year-olds’ socio-demographic status in 2006
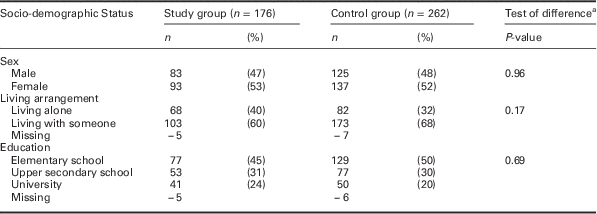
a P-value was estimated by a cluster-adjusted χ 2-test.
HI
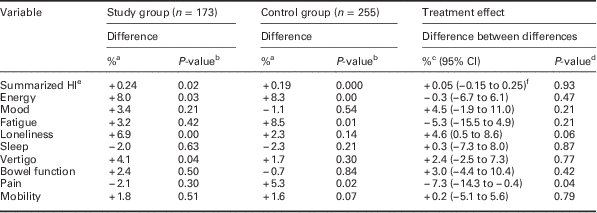
At follow-up, both the SG and CG reported a significant decline in health and well-being (based on overall HI scores, nine variables). In the SG, the variables energy, loneliness and vertigo were affected, whereas in the CG the variables energy, fatigue and pain were affected. The SG reported a significant reduction in pain as an effect of the PVH (Table 2).
Table 2 Difference (%) 2007–2006 and P-value in the study group and control group for 75-year-olds’ self-reported health and well-being (health index-scores), P-value for difference

HCC=healthcare centres; HI=health index.
Treatment effect expressed as the difference between change in the two groups with 95% confidence interval and P-value for treatment effect.
a Plus sign in difference indicates impaired health.
b Difference was tested by conditional logistic regression with HCC included as a cluster variable (2–10).
c Plus sign indicates larger decline in study group and minus sign larger decline in control group.
d Treatment effect was tested by logistic regression with HCC included as a cluster variable. Difference between differences was estimated by margins in STATA (2–10).
e Treatment effect was tested by poisson regression with HCC included as a cluster variable. Difference between differences was estimated by margins in STATA (1).
f Difference between differences in mean count (1).
At follow-up, there were no significant changes in or effects on the responses to the question about perceived health and well-being during the previous week.
General health
At follow-up, no effects on or changes in perceived general health were found. Persons in the SG reported significantly lower levels of general health than those of the same age in the CG (P<0.05). The PHV had no significant effect on general psychological or physical health in either group (data not shown).
Health behaviour
At follow-up, the SG reported a significant decrease in physical activity (P<0.02). There were no changes regarding leisure time activities such as doing crossword puzzles and participating in study circles. Both the SG (P<0.03) and the CG (P<0.03) reported significantly more alcohol use in 2007 than in 2006. The PVH was not associated with changes in or effects on smoking, use of snuff, eating habits or BMI (data not shown).
Health problems
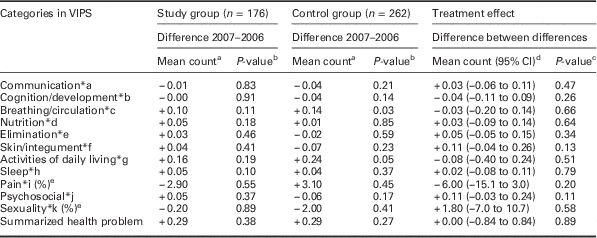
At follow-up, the CG reported a significant increase in health problems in the categories breathing/circulation and ADL (Table 3).
Table 3 Differences in mean count 2007–2006 in 75-year-olds’ self-reported health problems in the categories of well-being, integrity, prevention and safety (VIPS) and P-value difference from 2006 to 2007

HCC=healthcare centres.
One person could live with one or a number of health problems simultaneously.
*a. Hearing, sight, speech and taste (4 key words); *b. Understanding of health and illnesses and memory (2 key words); *c. Breathing, cough, angina pectoris, oedema, cold feet and vertigo (6 key words); *d. Under or overweight, difficulties in swallowing, nausea (3 key words); *e. Urine, faeces (2 key words); *f. Blisters in the mouth, changes and disorder of skin, itching, problems with the mucous membranes and wounds or ulcers (6 key words); *g. Cleaning, climbing the stairs, walking indoors, walking outdoors, food shopping, something meaningful to do during the day, shower/bath, economy (8 key words); *h. Sleep and fatigue (2 key words); *i. Pain (1 key word); *j. Anxiety, low-spirited, loneliness, tobacco and alcohol use (5 key words); *k. Sexuality (1 key word).
a Plus sign in difference indicates impaired health.
b Difference was tested by Poisson regression with HCC included as a cluster variable.
c Treatment effect (interaction between time and group) was tested by Poisson regression with HCC included as a cluster variable. Difference between differences was estimated by margins in STATA.
d Plus sign indicates larger decline in the study group and minus sign larger decline in the control group.
e Treatment effect was tested by logistic regression with HCC included as a cluster variable. Difference between differences was estimated by margins in STATA.
Knowledge about and contact with the local community and county council
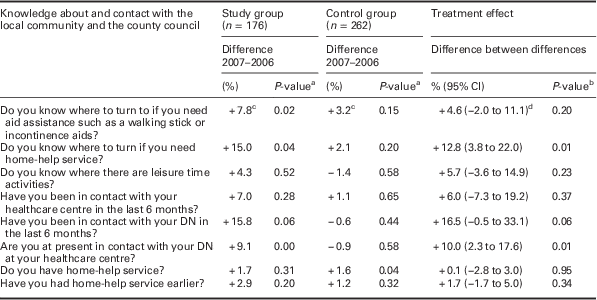
At follow-up, the SG reported a significant increase in knowledge about where to turn if in need of home-help service and the services offered by the county council. There was a significant effect on level of knowledge about the local community and the value of staying in contact with the local HCC (Table 4).
Table 4 Difference (%) 2007–2006 and P-value in 75-year-olds’ self-reported knowledge about and contact with the local community and the county council

Treatment effect (%) expressed as difference between differences.
a Difference was tested by conditional logistic regression with HCC included as a cluster variable.
b Treatment effect (interaction between time and group) was tested by logistic regression with HCC included as a cluster variable. Difference between differences was estimated by margins in STATA.
c Plus sign indicates an increase between 2007 and 2006.
d Plus sign indicates larger increase in the study group, and minus sign indicates larger increase in the control group.
Use of medication
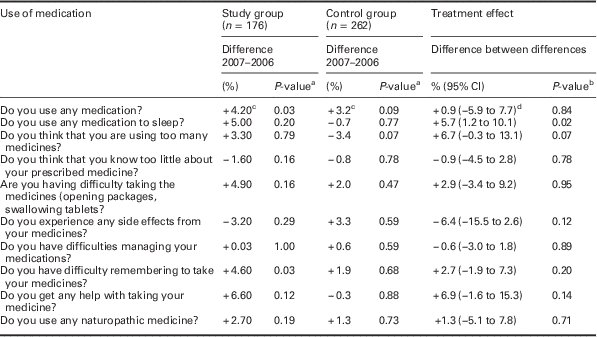
At follow-up, the participants in the SG used significantly more medication than at baseline and reported more difficulties in taking their medicines. There was a significant effect on the use of sleeping medication among participants in the SG (Table 5).
Table 5 Difference (%) 2007–2006 and P-value in 75-year-olds’ self-reported use of medication and P-value difference between 2006 and 2007

HCC=healthcare centres.
Treatment effect (%) expressed as difference between differences.
a Difference was tested by conditional logistic regression with HCC included as a cluster variable.
b Treatment effect (interaction between time and group) was tested by logistic regression with HCC included as a cluster variable. Difference between differences was estimated by margins in STATA.
c Plus sign indicates an increase between 2007 and 2006.
d Plus sign indicates larger increase in the study group, and minus sign indicates larger increase in control group.
Usefulness of the PHV
Of the 139 (79%) persons in the SG who answered the question about the usefulness of the PHV, 18 (13%) reported it was very useful, 65 (47%) that it was useful, 33 (24%) that it was of somewhat useful and 23 (16%) that it was not useful at all. Of the 139 persons, 91 (66%) contributed 113 comments (110 positive and 3 negative) on the usefulness of the PHV in response to the open-ended question. The comments are categorized as follows.
Positive experience
There were 49 comments that described the PHV as a good, very good or pleasant meeting: ‘It is good that somebody cares about older people and is interested in how we manage at home’.
Guidance
There were 18 comments about the PHV being informative – for example, with regard to activities in the local community and where to turn for assistance. There were six comments about the helpfulness of the PHV: ‘The DN has helped me with my problems regarding hearing, sexuality and sleeping problems’.
Caring meeting
There were 16 comments about how good it was to get to know the DN and about how getting to know the DN made the participants feel safe. There were eight comments about how society cared about older people: ‘It was nice to talk to somebody who cared about my health’. There were 12 comments about how the older people felt validated by the DN and that the DN was competent in her work.
No benefit
There were three comments in which persons expressed his or her feeling that the PHV was not helpful: ‘Didn’t lead to anything’, ‘Zero’, ‘Non-existent’.
Discussion
The results showed some positive changes in and effects on the 75-year-olds’ health and well-being, health problems and knowledge about services and resources offered by the county council and local community. However, no changes in or effects on health behaviour were found. The study showed a reduction in pain among 75-year-olds in the SG. In addition, health problems such as problems with breathing/circulation and ADL increased among participants in the CG but remained unchanged for those in the SG. Pain and ADL problems often manifest together (Jakobsson et al., Reference Jakobsson, Hallberg and Westergren2007) and are likely to have a negative effect on an older person’s health and well-being (Low and Molzahn, Reference Low and Molzahn2007). One effect of the PVH was an increase in knowledge among those in the SG about where to turn to for assistance and home-help service. The PHV also provided the 75-year-olds with opportunities to improve their contact with both the DN and the HCC. This, in turn, may have had a positive effect on health by enabling the DN to identify health problems and unmet needs early. Such early identification might be the reason why the SG reported an increase in medication and sleeping pill use after the PHV. The findings of this study request the question of how to work more effectively with health behaviour changes, as the result showed a decrease in physical activity among participants in the SG and an increase in alcohol intake in both the SG and CG. According to health professionals and public health scientists, the increase in alcohol intake amongst older persons is a worrying sign, as alcohol use is a risk factor for ill health (Stevenson, Reference Stevenson2005; Mehta et al., Reference Mehta, Moriarty, Proctor, Bird and Darling2006).
In this study, 75-year-olds were offered a PHV not because they were ill or had any disease but because they were independent, lived at home and were registered at one of the HCCs in the study. The PHV followed a predetermined structure that tracked the nursing process and followed a person-centred approach. The structure called for one visit and, if needed, follow-up contacts. Fifty per cent of the participants needed a follow-up contact at the HCC or at home for a variety of reasons such as checking blood pressure or providing information on nutrition, diabetes and how to get in contact with the local community services (Karp et al., Reference Karp, Wånell, Lagerin, Rydeman, Sherman, Söderhielm Blid and Törnkvist2009; Sherman et al., Reference Sherman, Söderhielm Blid, Karp and Wånell2010). In this study, the participants reported increased contact with both the DN and the HCC. This result differs from the results of many studies of PHVs, which show a decrease in utilization of healthcare resources after PHVs (Shapiro and Taylor, Reference Shapiro and Taylor2002; Hendriksen and Vass, Reference Hendriksen and Vass2005; Markle-Reid et al., Reference Markle-Reid, Browne, Weir, Gafni, Roberts and Henderson2006; Sahlen et al., Reference Sahlen, Lofgren, Hellner and Lindholm2008; Stuck and Kane, Reference Stuck and Kane2008). This result was expected, however, as the DNs performed the PHV the same year as the questionnaires were completed.
The lack of a non-response analysis for those who did not return the questionnaires (∼25%) was a limitation of this study. However, a thorough non-response analysis of the 75-year-old persons who declined a PHV was performed. The analysis showed that some participants believed they were too healthy or too ill for a PHV or that they were not interested in a PHV, a result in agreement with the results of earlier studies (Byles, Reference Byles2000; Minder et al., Reference Minder, Muller, Gillmann, Beck and Stuck2002; Sherman et al., Reference Sherman, Söderhielm Blid, Karp and Wånell2010). The intention to treat may have been influenced by internal drop-outs. However, data on all individuals with one missing value, either at baseline or at follow-up, were used in all the analyses (with the exception of the analyses presented in Table 1); methods allowing non-response on one of the two occasions were used. Another potential source of internal bias may have been the answers given in the questionnaire. The 75-year-olds may not have mentioned all their health problems because (a) they were not aware of them, (b) they had learnt to live with them, (c) they did not want to talk about them or (d) their memory was failing them, all of which may have resulted in incorrect answers to the questions. The gap in time between the PHV and the follow-up questionnaire may have influenced the SG’s answers, as the PHVs were performed at different times (from the end of April to the middle of December). Some participants received information or treatment more recently than others and some may have forgotten what was discussed at the PHV by the time they responded to the follow-up questionnaire. Either of these circumstances could have influenced the effects found in the analyses. The gap in time was due to the time required for the DNs to fit the PHVs into their normal work schedules at the HCCs.
The strengths of this study include the lack of significant differences in the socio-demographic characteristics of the SG and the CG and the focus on one age group (75-year-olds). The use of data on self-reported health was also a strength, as self-reported health is a predictor of diseases, death and future healthcare needs (Idles et al., Reference Idles, Kasl and Lemke1990; Bowling, Reference Bowling2003). Finally, the study had sufficient statistical power to detect clinically important differences.
When evaluating the small effect of a PHV on a person’s health, researchers need to consider certain factors. One is the importance of understanding the difference between DNs’ everyday work and performing a PHV. Although DNs’ education includes training in health promotion and disease prevention, their daily work often focusses on medical health problems. In a PHV, this medical focus must change in that the DN has to use a salutogenic approach (Antonovsky, Reference Antonovski1993) that concentrates on the older person’s own health resources and wishes to change his or her health behaviour. A one-day course on how to perform PHVs was probably not sufficient to change this focus, especially as the DNs in this study were new to PHVs. The PHVs were also integrated in an already activity-heavy organization. Another factor that may have limited the study’s results is that there was only one home visit. Previous research shows that follow-up contacts are important for older persons’ health and well-being (Stuck et al., Reference Stuck, Egger, Hammer, Minder and Beck2002; Sahlen et al., Reference Sahlen, Dahlgren, Hellner, Stenlund and Lindholm2006; Huss et al., Reference Huss, Stuck, Rubenstein, Egger and Clough-Gorr2008; Gustafsson et al., Reference Gustafsson, Wilhelmson, Eklund, Gosman-Hedstrom, Ziden, Kronlof, Hojgaard, Slinde, Rothenberg, Landahl and Dahlin-Ivanoff2012), particularly to changing health behaviour, as it takes time to change one’s life habits (Shinitzky and Kub, Reference Shinitzky and Kub2001). The literature on PHVs includes a lively discussion of the key conditions for successful PHVs, and many healthcare professionals argue that good contact between the older person and the health visitor is a necessity for a positive visit (Vass et al., Reference Vass, Avlund, Hendriksen, Philipson and Riis2007). It is difficult to know whether the PHVs per se had an effect or it was the caring visits that did the job. Perhaps it is as Clark (Reference Clark2001) argues that the effectiveness of PHVs cannot be judged by randomized controlled trials.
At present, the PHV programme is county-wide in that all 75-year-olds in the Stockholm county council area are invited to a PHV by a DN. As the study was completed, the preparatory course has been extended to two days, and PHVs have been further developed. The course contains one day of training in how to apply the theoretical model for performing PHVs.
After this day-long training, the DN carries out a PHV with a 75-year-old in the older person’s home. After about four weeks, the DNs gather in groups to reflect (Biggs and Tang, Reference Biggs and Tang2007) on the different parts of the PHV. They discuss what was easy, what was hard, how they can learn from each other and how they can best work with a salutogenic approach. To encourage older people to adopt a salutogenic approach is an important component of health promotion efforts directed towards older people (Lezwijn et al., Reference Lezwijn, Vaandrager, Naaldenberg, Wagemakers, Koelen and Van Woerkum2011). In addition, the researchers developed a health plan for the 75-year-olds to keep at home.
Conclusions
The results suggests that, in the Swedish healthcare context, PVHs to 75-year-olds by DNs may be effective in reducing pain, increasing knowledge about services and resources offered by the county council and local community and improving contacts with the HCCs. Our results also showed that ADL problems and breathing/circulation problems increased in the CG but not in the SG during the year between the PHV and follow-up. Additional education for DNs on how to encourage changes in health behaviours may be warranted, as the results of this study showed that the PHVs had no effect in these areas. When asked about their experience of the PHV, the majority of the 75-year-olds reported that it was useful and that it made them feel more secure.
Acknowledgements
The authors thank Hassan Farhad Alinaghizadeh and to Sven-Erik Johansson for valuable statistical counselling.
Conflicts of Interest
The author(s) declare that they have no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Ethical Standards
The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national and institutional guidelines on human experimentation, the ethics committee at the Karolinska Institutet (2005/1377-31/2) and with the Helsinki Declaration of 1975, as revised in 2008.