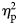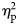Introduction
Medical Aid in Dying (MAID)Footnote 1 allows terminally ill patients to make a voluntary, informed decision to obtain a physician's prescription for oral medications to end their life. MAID is legal in 11 states in the USA (Pope, Reference Pope2020), representing 72 million people (or 22% of the US population). It is estimated that over 200 million people now have access to MAID around the world (Mroz et al., Reference Mroz, Dierickx and Deliens2021) and in most countries where MAID is legal, public opinion is overwhelmingly in support. Similarly, studies have shown strong public support for extending patient rights beyond MAID to include active euthanasia in some countries (e.g., Netherlands and Canada).
Although a growing number of people in the USA have access to MAID, general public opinion remains divided with 54% of the US population in support (Duckett, Reference Duckett2019). As a result, individuals engaging in MAID in the USA, and their loved ones, may fear being stigmatized by others (Srinivasan, Reference Srinivasan2019). Evidence from Switzerland suggests that families engaging in MAID may keep participation hidden, with potentially significant consequences for the bereaved family member if they feel they are alienated from social support as a consequence of the decedent's choice to use MAID (Wagner et al., Reference Wagner, Keller and Knaevelsrud2012; Gamondi et al., Reference Gamondi, Pott and Forbes2015, Reference Gamondi, Pott and Preston2018, Reference Gamondi, Pott and Preston2019). Thus, as access to MAID continues to expand, there is a need for research examining different facets of MAID, including public perceptions of those who utilize MAID and their family members.
Stigma is an aspect of public perception that is typically categorized as self-stigma and public stigma (Livingston and Boyd, Reference Livingston and Boyd2010; Eisma et al., Reference Eisma, te Riele and Overgaauw2019). This paper will focus on public stigma, but it is important to note that research has found that public stigma leads to self-stigma (Evans-Lacko et al., Reference Evans-Lacko, Brohan and Mojtabai2012). Researchers have generally defined public stigma as exhibiting negative emotions and attitudes toward, as well as a preference for social distance, an individual (Eisma, Reference Eisma2018; Eisma et al., Reference Eisma, te Riele and Overgaauw2019; Gonschor et al., Reference Gonschor, Eisma and Barke2020). Public stigma has been found to increase negative long-term outcomes for bereaved individuals whom the stigma is towards, including depression and suicide (Carpiniello and Pinna, Reference Carpiniello and Pinna2017; Eisma, Reference Eisma2018) and Prolonged Grief Disorder (Gonschor et al., Reference Gonschor, Eisma and Barke2020; Dennis et al., Reference Dennis, Eisma and Breen2021) (PGD). Stigmatizing public reactions, such as negative emotions about and attributions of the bereaved and a larger preferred social distance from the bereaved, are indicators of public stigma (Wagner et al., Reference Wagner, Keller and Knaevelsrud2012; Eisma, Reference Eisma2018; Gonschor et al., Reference Gonschor, Eisma and Barke2020; Dennis et al., Reference Dennis, Eisma and Breen2021). The provision of social support is regulated by norms, which are the rules that govern acceptable behavior, such as expectations about the expression of grief (Penman et al., Reference Penman, Breen and Hewitt2014).
Research has shown that bereaved persons are expected to show outward displays of intense grief, yet doing so leaves them open to public stigma (McLean et al., Reference McLean, Singer and Laurita2021) and often these individuals do not receive the quantity or quality of social support needed (Aoun et al., Reference Aoun, Breen and Howting2015) due to not following social norms. Not conforming to publics expectations of grief can lead to public stigma, which should be of concern, as it can result in a loss of social support, feelings of being ostracized, and risk of experiencing additional severe mental health problems (Johnson et al., Reference Johnson, First and Block2009; Chapple et al., Reference Chapple, Ziebland and Hawton2015; Pitman et al., Reference Pitman, Osborn and Rantell2016).
To our knowledge, only one study has examined differences in stigma toward bereaved individuals whose family member died of illness as compared to MAID (Philippkowski et al., Reference Philippkowski, O'Connor and Eisma2021). This study was conducted in Australia and found that MAID did not elicit any more stigma toward family members than if a person died of a life-limiting illness. However, 80% of Australians support MAID (Duckett, Reference Duckett2019). In contrast, MAID has been a highly controversial and highly debated topic in the USA (White and Willmott, Reference White and Willmott2018; Pope, Reference Pope2020). It is possible that differences may emerge when comparing public stigma toward bereaved individuals who lost a loved one due to MAID, compared to other types of death in America.
One aspect that has affected the perception and attitudes toward MAID is the age of the person who utilized MAID. Studies have found that the general public and health professionals are more comfortable with older adults utilizing MAID rather than younger adults (Lamers and Williams, Reference Lamers and Williams2016), or children (Bevacqua and Kurpius, Reference Bevacqua and Kurpius2013; Stolz et al., Reference Stolz, Burkert and Großschädl2015). Philippkowski et al. (Reference Philippkowski, O'Connor and Eisma2021) identified age as an important factor to consider when examining stigma toward bereaved individuals whose family member utilized MAID. Their vignette-based study used 28- and 80-year-olds and found death at a young age (28 years) was significantly associated with stronger negative emotional reactions of fear and anger, two subcategories of stigma, than the 80-year-old. Using only 28-year- and 80-year-olds was a limitation identified by the authors, as other studies have found differences in the acceptability of MAID across many age ranges (Frileux, Reference Frileux2003; Rae et al., Reference Rae, Johnson and Malpas2015). Therefore, understanding differences in stigma across a greater range of ages and within key developmental periods (e.g., 70 and 80; 28 and 38) could improve the identification of bereaved individuals at higher risk of public stigma.
We aimed to replicate and extend the study of Philippkowski et al. (Reference Philippkowski, O'Connor and Eisma2021) by examining whether there were any differences in public stigma based on mode of death (i.e., MAID vs. illness), age of the deceased individual (i.e., 28, 38, 70, and 80 years of age), or the interaction of mode of death and age, in a sample of adults living in the USA. We hypothesized that bereaved individuals whose family member who is younger (i.e., 28 and 38) engaged in MAID would experience more stigma than bereaved individuals whose family member who is older (i.e., 70 and 80) died of an illness-related death or MAID. Also, we examined if expectations of grief differ between bereaved individuals whose family member utilized MAID compared to bereaved individuals whose family member died of an illness, and if that differs based on age of deceased. We hypothesized that participants would expect more grief symptoms among family members whose loved one was younger and had an illness-related death compared to family members whose loved one was older and utilized MAID.
Methods
Participants
A total of 428 participants (265 females) were enrolled in this study. An a priori power analysis (Faul et al., Reference Faul, Erdfelder and Lang2007) estimated that 146 participants would be required to achieve 95% power to detect a moderate (ƒ2 = 0.15) effect; thus, the study was sufficiently powered. The mean age of the sample was 42.54 (SD = 16.00), with a range of 18–93 years. The sample was predominantly White (n = 315; 73.6%), with small subsamples of African-American or Black (n = 270; 16.4%) and Asian-American (n = 27; 6.4%) adults.
Procedure
The study approval was granted by the Blinded for Review. The study utilizes cross-sectional data including demographics, vignettes, and stigma measures, which were collected on MTurk. We utilized a 2 (cause of death: MAID vs. illness-related death) × 4 (age of the deceased: 28-, 38-, 70-, and 80-year-olds) randomized between-groups, vignette-based experiment. We picked these ages in order to replicate the study of Philippkowski et al. (Reference Philippkowski, O'Connor and Eisma2021) participate in this study, participants had to have an MTurk account, be English proficient, a US resident, and 18 or older. Participants were credited $1.15 to their account upon completion of this 10-min survey. MTurk samples have been found to generalize in multiple fields, including trauma, suicide, depression, and addiction (Sheehan, Reference Sheehan2018; Klik et al., Reference Klik, Williams and Reynolds2019; Engle et al., Reference Engle, Talbot and Samuelson2020). MTurk has also been utilized in numerous studies examining stigma (e.g., Sheehan, Reference Sheehan2018; Goodyear and Chavanne, Reference Goodyear and Chavanne2021).
Measures
Vignettes
We used vignettes developed by Philippkowski et al. (Reference Philippkowski, O'Connor and Eisma2021) and added four additional vignettes to include all levels of the independent variables. Vignettes have been used in hundreds of studies to approximate real-life responding, including articles that have examined stigma in different contexts (Hughes and Huby, Reference Hughes and Huby2004). Studies examining public stigma and expectations of grief symptomatology have used vignette-based experimental design and been validated in numerous studies (e.g., Penman et al., Reference Penman, Breen and Hewitt2014; Eisma, Reference Eisma2018; Logan et al., Reference Logan, Thornton and Kane2018; Eisma et al., Reference Eisma, te Riele and Overgaauw2019), including bereaved individuals whose loved one utilized MAID (Philippkowski et al., Reference Philippkowski, O'Connor and Eisma2021).
Stigma
Emotional Reactions Scale
Angermeyer and Matschinger (Reference Angermeyer and Matschinger2003) described three types of emotional reactions to people with mental illness: fear, anger, and pro-social reactions. The Emotional Reactions Scale was developed to assess each of these emotional reactions (Link et al., Reference Link, Yang and Phelan2004). For example, “When I read about C.G. I feel annoyed.” The Emotional Reactions Scale is a 13-item Likert response scale, with a range of 1 (strongly disagree) to 4 (strongly agree). This scale has been used in numerous studies examining stigma (Eisma, Reference Eisma2018; Eisma et al., Reference Eisma, te Riele and Overgaauw2019; Philippkowski et al., Reference Philippkowski, O'Connor and Eisma2021) and demonstrates good internal consistency in the general population, α = 0.85 (fear), α = 0.82 (anger), and α = 0.75 (prosocial behavior). Higher scores indicate more negative emotional reactions toward the person. The scale demonstrated good internal consistency in the current study (α = 0.89 (fear), α = 0.87 (anger), and α = 0.78 (prosocial)).
Social Distance Scale
The Social Distance Scale was derived by Link et al. (Reference Link, Phelan and Bresnahan1999) and is used to measure preferred social distance within a vignette. The scale used in this study has been used in other vignette-based studies (Eisma, Reference Eisma2018; Eisma et al., Reference Eisma, te Riele and Overgaauw2019; Philippkowski et al., Reference Philippkowski, O'Connor and Eisma2021). Questions investigate the degree to which a participant reports willingness to interact with the person/character in the vignette (e.g., “How would you feel having someone like C.G. as a neighbor?”). The Social Distance Scale is a 17-item scale, with responses ranging from 1 (definitely willing) to 4 (definitely unwilling). Higher scores indicate a need for social distance from the person. For further details, see Philippkowski et al. (Reference Philippkowski, O'Connor and Eisma2021). Internal consistency for this measure has been good in past studies (α = 0.84; Philippkowski et al., Reference Philippkowski, O'Connor and Eisma2021) and was α = 0.88 in the current study.
Expectations of Grief Symptomatology Scale
The Expectations of Grief Symptomatology Scale (Penman et al., Reference Penman, Breen and Hewitt2014) measures participant's expectations of the intensity of another person's grief. The Expectations of Grief Symptomatology scale is a 12-item scale, which is a modified version of the PG-13, a measure of PGD symptoms. Penman et al. (Reference Penman, Breen and Hewitt2014) modified the scale from the first to third person to allow for more general judgments of expectations of grief symptomology. Responses range from 1 (Never) to 4 (Always). Higher scores indicate that more intense grief was expected (Logan et al., Reference Logan, Thornton and Kane2018). Internal consistency for this measure has been good in the past (α = 0.87 (Penman et al., Reference Penman, Breen and Hewitt2014); α = 0.88 (Philippkowski et al., Reference Philippkowski, O'Connor and Eisma2021)) and was α = 0.94 in the current study.
Data analysis
First, we calculated means and standard deviations of measures of stigma, which were used as the dependent variables in this study. We used a two-way multivariate analysis of variance (MANOVA) and interpreted Roy's Largest Root to determine significance. Mode of death (i.e., MAID and illness-related death) and age of the deceased (i.e., 28, 38, 70, and 80), as well as their interaction, were entered as fixed factors. Anger, fear, prosocial emotions, social distance, and expectations of grief symptomatology were entered as outcome variables. If any significant multivariate effects were identified, univariate ANOVAs were used to identify which outcome variables differed between the group(s) and in which direction. For all results, partial eta-squared (![]() $\eta _{\rm p}^2$) is presented as a measure of effect. A value of η p>0.06 is considered a “medium” effect, and η p > 0.14 considered a “large” effect (Cohen, Reference Cohen2013).
$\eta _{\rm p}^2$) is presented as a measure of effect. A value of η p>0.06 is considered a “medium” effect, and η p > 0.14 considered a “large” effect (Cohen, Reference Cohen2013).
Results
Table 1 documents the means and standard deviations of measures of stigma. There were no differences in age, sex, race/ethnicity, and education between groups (p > 0.05).
Table 1. Demographics: participants’ characteristics and vignettes

MANOVA identified a significant interaction effect between age of the deceased and the mode of death (Roy's Largest Root = 3.62, F(5, 400), p = 0.001, ![]() $\eta _{\rm p}^2$ = 0.06) on indicators of stigma and a statistically significant main effect for age of the deceased (Roy's Largest Root = 3.50, F(5, 401), p = 0.004
$\eta _{\rm p}^2$ = 0.06) on indicators of stigma and a statistically significant main effect for age of the deceased (Roy's Largest Root = 3.50, F(5, 401), p = 0.004 ![]() $\eta _{\rm p}^2$ = 0.04) on indicators of stigma. The mode of death was unrelated to indicators of stigma (Roy's Largest Root = 0.771, F(5, 401), p = 0.57,
$\eta _{\rm p}^2$ = 0.04) on indicators of stigma. The mode of death was unrelated to indicators of stigma (Roy's Largest Root = 0.771, F(5, 401), p = 0.57, ![]() $\eta _{\rm p}^2$ = 0.01).
$\eta _{\rm p}^2$ = 0.01).
Following the MANOVA, post-hoc ANOVAs were used to examine the interaction between age and the mode of death on expectations of grief symptomatology, emotional reactions (i.e., fear, prosocial, and anger), and social distance (see Table 2). Post-hoc ANOVAs revealed that participants expected the bereaved individual whose 28-year-old spouse died from an illness-related death (M = 44.12, SD = 12.03) would experience more maladaptive grief symptoms than a bereaved individual whose 28-year-old (M = 39.3, SD = 11.56; p = 0.01) or 38-year-old (M = 38.71, SD = 11.56; p = 0.007) spouse who utilized MAID. Also, participants expected the bereaved individual whose 70-year-old spouse died from an illness-related death (M = 44.32, SD = 10.29) would experience more maladaptive grief symptoms than a bereaved individual whose 28 (M = 39.3, SD = 11.56; p = 0.02) or 38-year-old (M = 38.71, SD = 11.56; p = 0.008) spouse who utilized MAID. The interaction effects between age and the mode of death on emotional reactions (i.e., fear, prosocial, and anger) and social distance were not significant (p > 0.05).
Table 2. Age × mode of death interaction univariate ANOVAs

Post-hoc ANOVAs were used to further examine the main effects of age (28, 38, 70, and 80 years) on the outcome variables (see Table 3). There were no significant main effects of age on social distance, anger, prosocial behavior, or fear (all Fs < 1.57, all ps > 0.05). However, there was a significant main effect of age on grief expectations (F(1,400) = 3.72, p = 0.010, ![]() $\eta _{\rm p}^2$ = 0.03). Specifically, participants expected the bereaved 38-year-old (M = 38.88, SD = 10.97) to experience less maladaptive grief than a bereaved 28-year-old (M = 44.27, SD = 12.20; p = 0.02) or 70-year-old (M = 44.32, SD = 10.29; p = 0.01), irrespective of how their family member died. There was no significant difference between the 80-year-old family member, no matter type of death, compared to other ages (ps > 0.05).
$\eta _{\rm p}^2$ = 0.03). Specifically, participants expected the bereaved 38-year-old (M = 38.88, SD = 10.97) to experience less maladaptive grief than a bereaved 28-year-old (M = 44.27, SD = 12.20; p = 0.02) or 70-year-old (M = 44.32, SD = 10.29; p = 0.01), irrespective of how their family member died. There was no significant difference between the 80-year-old family member, no matter type of death, compared to other ages (ps > 0.05).
Table 3. Age main effect from univariate ANOVAs

Discussion
There is a well-documented negative opinion toward MAID in the USA (Verbakel and Jaspers, Reference Verbakel and Jaspers2010; Duckett, Reference Duckett2019). Yet, MAID is legal in 11 states and more legislation is being written to legalize MAID in other states (Pope, Reference Pope2020). With an increase in utilization and access to MAID, a greater number of bereaved individuals will be grieving the loss of their family member via this method. This is the first study, to our knowledge, to investigate the effects of mode of death (MAID vs. illness-related death) and age of death (28, 38, 70, and 80 years) on American adults’ public stigma and expectations of grief symptoms toward bereaved individuals. Interestingly, there was no interaction of effects on direct stigma (i.e., emotional reactions and public stigma). These results indicate that, though there is a public criticism of use of MAID (Duckett, Reference Duckett2019), individuals are unlikely to stigmatize the family members and loved ones of individuals who decide to use MAID. It is possible that the general public attributes the decision to use MAID to the patient, rather than their loved ones; therefore, they may believe that bereaved individuals should not be stigmatized for a decision that is not entirely in their control.
There were, however, significant interactions when examining expectations of grief symptoms. The data showed two significant interactions between age and the type of death. First, participants felt that bereaved individuals whose 28-year-old spouse dies from an illness would experience more maladaptive grief symptoms than bereaved individuals whose 28-year-old or 38-year-old spouse utilized MAID. Second, participants endorsed that bereaved individuals whose 70-year-old spouse passed away from an illness-related death would experience more maladaptive grief symptoms than bereaved individuals whose 28-year-old or 38-year-old spouse utilized MAID. These results, in addition to research showing that more intense grief reactions are likely to elicit public stigma (Eisma, Reference Eisma2018; Gonschor et al., Reference Gonschor, Eisma and Barke2020; Dennis et al., Reference Dennis, Eisma and Breen2021), suggest that bereaved individuals who lost someone to an illness will be stigmatized more. However, it could be hypothesized that bereaved individuals who lost someone to MAID are expected to grieve less and accept the death easier than a bereaved individual who lost someone due to illness. This perception could lead to a lack of support provided to bereaved individuals who lost someone to MAID as the layperson's perception is “they should be fine” following the loss.
Regardless of the mode of death, there was a significant main effect of age on participants’ perceptions of the bereaved individual's grief response. Interestingly, participants endorsed that they expect bereaved family members of 38-year-olds to experience less maladaptive grief symptoms than bereaved family members of 28- or 70-year-olds. Contrary to the findings of Philippkowski et al. (Reference Philippkowski, O'Connor and Eisma2021), we did not find any difference in negative emotional reactions of fear or anger when assessing age differences between 28- and 80-year-old decedents. It is important to note that the mean age of study participants was 42, and therefore, participants may have identified most closely with the vignettes describing 38-year-old decedents. Young middle-aged (e.g., 38-year-old) individuals in America may be perceived to have a greater range of resources to support socioemotional functioning. Research has shown that individuals in their middle to late 20s or between 65 and 70s are in transition periods, characterized by instability and stress (Beaujot, Reference Beaujot2017; Hawkley and Kocherginsky, Reference Hawkley and Kocherginsky2018). For example, 28-year-olds are more likely to be newly engaged/married (average age of marriage in the USA is 28), not have children, and not be financially stable or have job security (Rudolph et al., Reference Rudolph, Rauvola and Costanza2021; U.S. Census Bureau, Decennial Censuses, 1890 to 1940, and Current Population Survey, Annual Social and Economic Supplements, 1947 to 2020, 2020). Therefore, 28-year-olds may have historically received most of their positive reinforcement from their spouse who passed away, whereas 38-year-olds may have children, which is a protective factor for maladaptive grief symptoms (Hibberd et al., Reference Hibberd, Elwood and Galovski2010; Heeke et al., Reference Heeke, Stammel and Heinrich2017). Also, research has found that, as age increases, a person has more work satisfaction and feels more secure in their job (Rudolph et al., Reference Rudolph, Rauvola and Costanza2021). These multiple identities that exist outside of young middle-aged marriages (e.g., having children; work success) have been shown to be protective factors against maladaptive grief symptoms (Papa and Lancaster, Reference Papa and Lancaster2016). Regarding the difference between 38-year-olds and 70-year-olds, a similar argument could be made, as Carstensen's Socioemotional Selectivity Theory (Carstensen, Reference Carstensen1992) states that, as a person ages, their social network decreases and their relationships become more important. Therefore, a person might perceive a 70-year-old to have a smaller social network, which could result in expectations of higher grief symptoms following the loss of a spouse, a key member of their social network. It is imperative to directly explore whether public perceptions and stigma may be guided by developmental theories explaining changes in socioemotional resource capacity across the lifespan.
Limitations
There were limitations in this study that should be considered in interpreting the study findings. First, this was an online study and results might not generalize to samples recruited using other methods. It should be noted, however, that MTurk has been used in other studies (e.g., suicide; stigma) and with findings comparable to the general population (Sheehan, Reference Sheehan2018; Klik et al., Reference Klik, Williams and Reynolds2019; Engle et al., Reference Engle, Talbot and Samuelson2020). Second, this study does not provide insights into the underlying reason(s) for individuals’ perceptions regarding differences in stigma depending on bereaved person's age and the type of death. Third, this study only focused on spousal bereavement. Participants’ perceptions of stigma, including their assumptions about the emotional reactions of bereaved individuals, might differ based on the bereaved individual's relationship to their loved one. Fourth, we cannot comment on differences in stigma toward bereaved family members depending on the race of the participant.
Conclusions
This is the first study to examine public stigma and expectations of grief symptomology toward bereaved individuals whose family member utilized MAID with an American sample. Results were similar to Philippkowski et al.'s study with Australian adults that concern MAID elicits direct public stigma appear unfounded. However, unlike Philippkowski et al., individuals in the USA expect more maladaptive grief symptoms when grieving the death of a younger person from illness. Such expectations of grief displays might leave them susceptible to indirect stigma. Future research should examine additional factors that may influence public perceptions of grief reactions to MAID, specifically more granular ages, gender, and relationship of the bereaved, and race, ethnicity, and other sociocultural factors. In addition, studies should investigate the experience of stigma for bereaved family members of those using MAID at various ages. Finally, based on the findings, it may be important to better understand the grieving process for bereaved individuals who have lost someone to MAID and educate clinicians and the public about their possible unique grieving process.
Funding statement
This research received no specific grant from any funding agency, commercial, or not-for-profit sectors.
Conflicts of interest
All authors have nothing to disclose.