Today, cognitive dysfunction is accepted as a feature of schizophrenia. As the patients age, this dysfunction is higher and harder to evaluate due to the interaction among aging, other somatic diseases, psychoactive drugs, etc.
We studied a group of 16 patients with severe schizophrenia, of 76.6 years of middle age, resistant to treatments, interned for 48.6 years on average, and with a very low cognitive level. This is part of the patients who survive the initial group of 30, who have been followed and evaluated by us for more than 31 years (Sanguino-Andrés et al., Reference Sanguino-Andrés2015). We want to know the current cognitive deterioration and make a differential diagnosis with the numerous pathologies that can influence, as well as with other neurocognitive disorders (Gladsjo et al., Reference Gladsjo, Eastham, Jeste, Hwang and Bermanzohn2003). For this, we collected variables, such as demographic, current cognitive state, computed tomography (CT) brain, blood analysis, clinical/neuropsychological explorations, present diseases, cardiovascular risk factors, pharmacological treatments, etc. We used descriptive and exploratory statistics, with a level of significance α ≤ 0.05 in the differences between the means of the different variables. Tables 1 and 2 shows the tests used and only the significant variables.
Table 1. Biological/analytical dimensions: contrast between patients presenting White Matter Lesions (WMLs) and those without WMLs

*p ≤ 0.05.
WML = White Matter Lesions
Table 2. Demographic, cognitive and clinical dimensions: contrast between patients with White Matter Lesions (WMLs) and those without WMLs
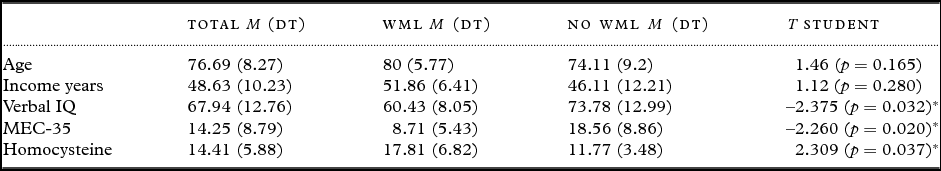
*p ≤ 0.05.
WML = White Matter Lesions; IQ = intelligence quotient; MEC-35 = Cognitive Mini.
The most important finding is the presence in cerebral CT of extensive and confluent white matter lesions (WMLs) in 43.8% of participants, and that this is related to cognitive deterioration. From the set of measures studied, we only observed that patients with WMLs have a significantly lower WAIS (Wechsler Adult Intelligence Scale) Verbal Intellectual Quotient than those who do not, lower average scores in the MEC-35 (Spanish version of the Folstein Mini-Mental), and upper average levels of homocysteine. There is no statistically significant relationship with cardiovascular risk factors present, or with other diseases, and even the relationship is negative with those with metabolic syndrome. Neither with the antipsychotics there is a relationship, nor with the number, dose, or type.
WMLs are focal or diffuse images that affect the periventricular or subcortical deep white matter. The etiopathogenesis of these lesions is not clear: chronic ischemia, rupture of the blood–brain barrier, endothelial dysfunction, or the combination of these elements (Medrano Martorella et al., Reference Medrano Martorella, Cuadrado Blázquez, García Figueredo, González Ortiza and Capellades Fonta2012). There were already studies communicating the relationship between WMLs and cognitive decline (Szoeke et al., Reference Szoeke, Campbell, Chiu, Ames, Weiner and Lipton2010). In relation to schizophrenia, there are also abundant studies of LSB, with chronic patients, with negative symptoms, with psychomotor symptoms, etc. In a recent work (Kelli et al., Reference Kelly2017) with magnetic resonance imaging (MRI) of the brain measured by DTI (diffusion tensor images), in 1,963 patients (36.22 years of average age), WML was found in its entirety and in several specific regions of the brain. Considering may be in part a disorder in which the connectivity of the brain structure is altered, with abnormal communication between different brain regions.
We believe that the finding of WML in elderly schizophrenic patients with deterioration is interesting, despite the size of the sample, not having a control group, and not using MRI instead of CT.
Conflict of interest
None.




