1. Introduction
The current state of planetary health is alarming on multiple levels (Atwoli et al., Reference Atwoli, Baqui, Benfield, Bosurgi, Godlee, Hancocks, Horton, Laybourn-Langton, Monteiro, Norman, Patrick, Praities, Rikkert, Rubin, Sahni, Smith, Talley, Turale and Vázquez2021; McKay et al., Reference McKay, Staal, Abrams, Winkelmann, Sakschewski, Loriani, Fetzer, Cornell, Rockström and Lenton2022; Rockström et al., Reference Rockström, Gupta, Qin, Lade, Abrams, Andersen, Armstrong McKay, Bai, Bala, Bunn, Ciobanu, DeClerck, Ebi, Gifford, Gordon, Hasan, Kanie, Lenton, Loriani and Zhang2023; Rocque et al., Reference Rocque, Beaudoin, Ndjaboue, Cameron, Poirier-Bergeron, Poulin-Rheault, Fallon, Tricco and Witteman2021). This translates into a pressing need to restore the health of the planet, symbiotically benefiting the health of the human civilization. Healthcare systems, through their environmental footprint, are themselves co-responsible for the progressive deterioration of planetary health, in terms of climate breakdown, air pollution, scarce water use, and biogeochemical flows (Lenzen et al., Reference Lenzen, Malik, Li, Fry, Weisz, Pichler, Chaves, Capon and Pencheon2020). The environmental disruptions to which they contribute ultimately damage human health (Eckelman et al., Reference Eckelman, Sherman and MacNeill2018, Reference Eckelman, Huang, Lagasse, Senay, Dubrow and Sherman2020a). Hence, they cannot be considered, by any means, exempt from the global effort to transition to sustainability, especially considering their overarching mission to improve health (Health Care Without Harm & Arup, 2019). Furthermore, they must be climate-resilient, anticipating, responding to, coping with, recovering from and adapting to environmental and climate-related shocks (WHO, 2015). This scenario underscores the necessity to revise health system goals and operations, integrating the objective of promoting the health of the planet as essential to enhancing human health. The immense scale and severity of challenges confronting healthcare systems today elevate environmental sustainability, which previously received fragmented attention and relied largely on commendable yet isolated initiatives by various stakeholders, to a pivotal role. Ultimately, promoting planetary health must become a common denominator for all care processes, from prevention to treatment.
An established approach to designing healthcare systems, in order to optimize their performance, consists in the pursuit of multiple aims. In 2008, Berwick and colleagues introduced the Triple Aim framework (Berwick et al., Reference Berwick, Nolan and Whittington2008) outlining three goals that a health system must pursue simultaneously: improving population health, enhancing the patient experience of care, and reducing per capita costs related to health care, with the latter two outlined as symmetrically complementing the former. The disruptive importance of the triple aim theory lies essentially in a paradigm shift related to optimizing care performance and the strategy for improving the quality of care. While with the second aim, the purely individual perspective of the patient care experience, focused on the care process itself (in line with the six ‘improvement goals’ proposed by the Institute of Medicine (US) Committee on Quality of Health Care in America: Safety, Effectiveness, Patient-Centeredness, Timeliness, Efficiency, Equity) (Institute of Medicine (US) Committee on Quality of Health Care in America, 2001) remains, the first and third aims shift toward a systemic view.
Further versions emerged in 2014, with Bodenheimer and Sinsky's introduction of the Quadruple Aim (Bodenheimer & Sinsky, Reference Bodenheimer and Sinsky2014), and in 2022 with the inclusion of health equity in the framework (Nundy et al., Reference Nundy, Cooper and Mate2022).
Bodenheimer and Sisnski enriched the model with an additional component: improving care team well-being (Bodenheimer & Sinsky, Reference Bodenheimer and Sinsky2014). They identify the health care workforce burn-out as a disruptive element and a substantial obstacle to achieving patient-centeredness and triple aim. In fact, burn-out is linked to overutilization of resources with increased costs and worsening clinical outcomes.
The novel fifth aim, which proposes to advance health equity (Nundy et al., Reference Nundy, Cooper and Mate2022), highlights that quality improvement without equity represents a hollow victory. Accordingly, policymakers and practitioners ought to develop and put into practice evidence-based strategies to minimize health inequities, make investments in measuring them, and provide incentives.
The key question the most renowned Triple Aim framework attempts to answer is: what goals should a healthcare system strive for, from the perspective of the society it serves? The seemingly contradictory goals of improving population health and reducing per capita care costs suggest a revolutionary assumption of responsibility by the healthcare system. In a world with finite resources, the needs and well-being of the population extend beyond the boundaries of healthcare, necessitating an emphasis on social determinants of health such as education, housing, and transportation, to improve overall health and minimize disparities. This declaration of responsibility, thus, implies a moral obligation for health systems to combat the current climate and environmental crisis, which poses significant threats to global health and well-being. Population health inevitably depends on the health of Earth's natural systems: the climate crisis, among other planetary health crises, has a significant impact on human health. Rising temperatures increase heat-related mortality and morbidity, while increased frequency and intensity of storms result in increased injury, death, and psychological stressors (Romanello et al., Reference Romanello, Napoli, Drummond, Green, Kennard, Lampard, Scamman, Arnell, Ayeb-Karlsson, Ford, Belesova, Bowen, Cai, Callaghan, Campbell-Lendrum, Chambers, van Daalen, Dalin, Dasandi and Costello2022). In all, 22–39% of the global population is projected to be out of the human climate niche by 2080–2100, if current climate policies persist (Lenton et al., Reference Lenton, Xu, Abrams, Ghadiali, Loriani, Sakschewski, Zimm, Ebi, Dunn, Svenning and Scheffer2023). Climate variability may impact the distribution and abundance of vertebrate host species, leading to an increase of vector-borne and zoonotic diseases (Haines & Ebi, Reference Haines and Ebi2019). Carbon emissions and climate breakdown also affect global health via multiple direct and indirect pathways, including effects on agriculture and nutrition, notably contributing to the global burden of disease (Smith et al., Reference Smith, Mueller, Springmann, Sulser, Garibaldi, Gerber, Wiebe and Myers2022; Weyant et al., Reference Weyant, Brandeau, Burke, Lobell, Bendavid and Basu2018). Parallelly, air pollution, which largely shares both sources and solutions with the climate crisis (Campbell-Lendrum et al., Reference Campbell-Lendrum, Neville, Schweizer and Neira2023), is linked to a variety of health outcomes (WHO, 2021), with 6.67 million deaths attributed to it in 2019 (Fuller et al., Reference Fuller, Landrigan, Balakrishnan, Bathan, Bose-O'Reilly, Brauer, Caravanos, Chiles, Cohen, Corra, Cropper, Ferraro, Hanna, Hanrahan, Hu, Hunter, Janata, Kupka, Lanphear and Yan2022). Furthermore, recent evidence suggests an association between PM2.5 and clinical antibiotic resistance, which itself represents a major challenge for health systems as well as a threat to public health (Zhou et al., Reference Zhou, Shuai, Lin, Yu, Ba, Holmes, Xiao, Gu and Chen2023). Consistent with the ‘do no harm’ principle of medical professionals and ethical foundations, there can be no goal of health systems that does not take into account the effects that health interventions have on the environment.
Environmental sustainability of healthcare systems has been at the center of scientific debate for several years now. Scientific evidence and individual initiatives to improve the sustainability of healthcare interventions by healthcare organizations, at multiple levels, are numerous (Cook et al., Reference Cook, Goodwin, Porter and Collins2023; Keil et al., Reference Keil, Viere, Helms and Rogowski2023; Patel et al., Reference Patel, Turner, Alishahi Tabriz, Gonzalez, Oswald, Nguyen, Hong, Jim, Nichols, Wang, Robinson, Naso and Spiess2023; Sala et al., Reference Sala, Alcamo and Nelli2017; Somner et al., Reference Somner, Stone, Koukkoulli, Scott, Field and Zygmunt2008; Storz, Reference Storz2020). Indeed, it is now recognized that environmental impacts should be considered when measuring the value of health care. For example, sustainability in quality improvement (SusQI) is a framework that assesses the quality and value of health care not only through the lens of economic sustainability, but also that of social and environmental sustainability (Stanford et al., Reference Stanford, Barna, Gupta and Mortimer2023).
Though environmental sustainability has been suggested as an additional objective within a sextuple aim framework (Alami et al., Reference Alami, Lehoux, Miller, Shaw and Fortin2023), we stress that human health is inherently intertwined with the health of natural systems. For health systems, the primary objective of enhancing population health, as put forth by the Triple Aim framework, cannot be detached from a contextual and targeted action to preserve planetary health. By revisiting the first objective of the Quadruple Aim and enriching it with the more comprehensive notion of planetary health – ‘a solutions-oriented, transdisciplinary field and social movement focused on analyzing and addressing the impacts of human disruptions to Earth's natural systems on human health and all life on Earth’ (Planetary Health Alliance, n.d.) – we could provide a theoretical framework within which health systems can prioritize the array of activities aimed at mitigation of and adaptation to the multiple threats to earth system stability. This theoretical framework reflects a systemic approach that does not merely provide healthcare systems with the objective of promoting environmental sustainability (as suggested in the sextuple aim model), but rather, sustainability becomes a means through which to achieve the primary goal of any healthcare system: promoting and restoring health (both of the population and the planet).
The centrality of such a significant goal (and responsibility) is evident in how it decisively integrates and supports the pursuit of other objectives, from reducing healthcare costs to prioritizing the patient and their perspective in the care process, to enhancing the well-being of the care team. Continuous improvement in the quality of healthcare in the 21st century cannot disregard the pursuit of planetary health objectives. Our framework compellingly encompasses the wide-ranging aspects of the role of health systems in transitioning to societies aligned with planetary boundaries, propelling them to the core of the planetary health movement. Indeed, such a comprehensive approach, while holding healthcare systems fully accountable to their patients, their natural interlocutors, may generate mutual benefits in the interaction with other sectors, notably the economic sector, thus acting as a catalyst for comprehensive societal change.
2. Advancing planetary health as an aim for healthcare improvement
A health system that advances planetary health requires a systems-thinking approach, based on four main principles, contributing to tackling the current crisis of value and purpose that affects health systems worldwide (Larsson et al., Reference Larsson, Clawson and Howard2023): decreasing the demand for health services through health promotion and disease prevention; pursuing the delivery of appropriate care; abating the overall environmental footprint of health services (MacNeill et al., Reference MacNeill, McGain and Sherman2021); endorsing planetary health action across other sectors and the overall society (Karliner et al., Reference Karliner, Roschnik, Boyd, Ashby and Steele2021) (Figure 1).

Figure 1. A revised quadruple aim for healthcare improvement, centered on the advancement of planetary health.
In relation to the first principle, evidence-based health promotion and disease prevention programs, powered by engaging stakeholders from multiple sectors (Claflin & Aloia, Reference Claflin and Aloia2010), alleviate disease burden (Bandosz et al., Reference Bandosz, Ahmadi-Abhari, Guzman-Castillo, Pearson-Stuttard, Collins, Whittaker, Shipley, Capewell, Brunner and O'Flaherty2020; Rasella et al., Reference Rasella, Harhay, Pamponet, Aquino and Barreto2014; Soltani et al., Reference Soltani, Saraf-Bank, Basirat, Salehi-Abargouei, Mohammadifard, Sadeghi, Khosravi, Fadhil, Puska and Sarrafzadegan2021; Wang et al., Reference Wang, Hu, Zhao, Kuang, Zhao, Liu and Zhu2021) and, consequently, its environmental footprint (Bi & Hansen, Reference Bi and Hansen2018). Smart governance for health and wellbeing provides the framework for such an intense cross-sectoral cooperation to thrive (Kickbusch & Gleicher, Reference Kickbusch and Gleicher2012). Additionally, 16.4% of the world population is projected to be 65 years or older by 2050, nearly doubling the current share (Gerland et al., Reference Gerland, Hertog, Wheldon, Kantorova, Gu, Gonnella, Williams, Zeifman, Bay, Castanheira, Kamiya, Bassarsky, Gaigbe-Togbe and Spoorenberg2022), which is likely to push demand for health services even further. Investing in public health interventions is deemed an effective way to put a cap on this process, thus allowing health systems to effectively deliver services still needed, while curbing not only their attributable footprint on natural systems but also economic, social and personal costs (Masters et al., Reference Masters, Anwar, Collins, Cookson and Capewell2017; McDaid, Reference McDaid2018). Despite that, across countries belonging to the Organisation for Economic Co-operation and Development, preventive care expenditure accounted for just 0.24% of gross domestic product and 2.59% of current health expenditure in 2019, on average (OECD, 2023). Interventions addressing tobacco, meat consumption, obesity, and air pollution are projected to save approximately 1.5 gigatons of CO2e from 2014 to 2050 (Karliner et al., Reference Karliner, Roschnik, Boyd, Ashby and Steele2021). The push for integrated public health policies must address the challenges presented by short-sighted public systems and private healthcare systems in which diseases can unfortunately be perceived as revenue generators (McDaid, Reference McDaid2018; Missoni & Galindo, Reference Missoni and Galindo2020).
The second principle consists in delivering appropriate healthcare that responds to health needs according to evidence-based practice. This entails the cessation of superfluous exams and prescriptions (Kherad & Carneiro, Reference Kherad and Carneiro2022), as well as service delivery in the most efficient setting. Hospital care, which is intrinsically energy- and resource-intensive, has a larger carbon footprint than primary care (Malik et al., Reference Malik, Lenzen, McAlister and McGain2018; Nicolet et al., Reference Nicolet, Mueller, Paruta, Boucher and Senn2022; Pichler et al., Reference Pichler, Jaccard, Weisz and Weisz2019; Tennison et al., Reference Tennison, Roschnik, Ashby, Boyd, Hamilton, Oreszczyn, Owen, Romanello, Ruyssevelt, Sherman, Smith, Steele, Watts and Eckelman2021). Hence, striving to limit hospitalizations through appropriate care, ensuring accessibility and continuity across primary and community care settings, within the framework of secondary and tertiary prevention community-based programs, is in turn beneficial to the environment, as opposed to frequent hospital accesses, resulting from inadequate and chaotic care. Healthcare systems with Beveridge models and ex-ante reimbursement strategies tend to favor appropriate care, given the need to contain expenditure, whereas it may undermine profitability in private health care. Professionals' culture, specific patient requests, conflicts of interest, and care fragmentation all have a role in over-prescribing and over-treatment (Missoni & Galindo, Reference Missoni and Galindo2020).
The third principle is concerned with reducing the environmental impact of the high-value health services still needed to meet population health needs. The main production sectors responsible for that encompass energy supply, operational emissions, manufacturing, agriculture, and transport (Health Care Without Harm, 2019). Assessments of the healthcare environmental impact have been conducted on national and global scales, much as further methodological improvements are warranted (Eckelman et al., Reference Eckelman, Romanello, Sherman and Watts2020b; Steenmeijer et al., Reference Steenmeijer, Rodrigues, Zijp and der Loop2022). Globally, the environmental footprint of health care amounts to 4.4% of greenhouse gas emissions, 2.8% of particulate matter, 3.4% of nitrogen oxides, and 3.6% of sulfur dioxide (Lenzen et al., Reference Lenzen, Malik, Li, Fry, Weisz, Pichler, Chaves, Capon and Pencheon2020).
Lastly, health systems are in a strong position to steer societies and economies toward planetary health goals. Intensive climate action would lead to large health co-benefits (Campbell-Lendrum et al., Reference Campbell-Lendrum, Neville, Schweizer and Neira2023; Whitmee et al., Reference Whitmee, Green, Belesova, Hassan, Cuevas, Murage, Picetti, Clercq-Roques, Murray, Falconer, Anton, Reynolds, Waddington, Hughes, Spadaro, Jaber, Saheb, Campbell-Lendrum, Cortés-Puch and Haines2024) and thoroughly accomplish the system's mission. Health systems with a strong commitment to environmental sustainability can exert a guidance role, influencing other companies and the civil society, while leveraging their remarkable purchasing power (Howard et al., Reference Howard, MacNeill, Hughes, Alqodmani, Charlesworth, de Almeida, Harris, Jochum, Maibach, Maki, McGain, Miller, Nirmala, Pencheon, Robertson, Sherman, Vipond, Yin and Montgomery2023). Societies and economies, in turn, striving to operate within planetary boundaries, contribute to the health care's own sustainability and human health goals, as social and economic determinants improve and any-grade suppliers decarbonize. This influence is integral to a comprehensive process to augment and emphasize connections between health and other sectors.
3. How the planetary health goal contributes to other aims
The proposed aim of advancing planetary health contributes to each of the other interdependent aims (Bodenheimer & Sinsky, Reference Bodenheimer and Sinsky2014) (Figure 2). In fact, planetary health encompasses the health of human civilization, thus embracing the original aim of improving population health, while further expanding on it and acknowledging its being intertwined with the health of natural systems (Whitmee et al., Reference Whitmee, Haines, Beyrer, Boltz, Capon, de Souza Dias, Ezeh, Frumkin, Gong, Head, Horton, Mace, Marten, Myers, Nishtar, Osofsky, Pattanayak, Pongsiri, Romanelli and Yach2015).
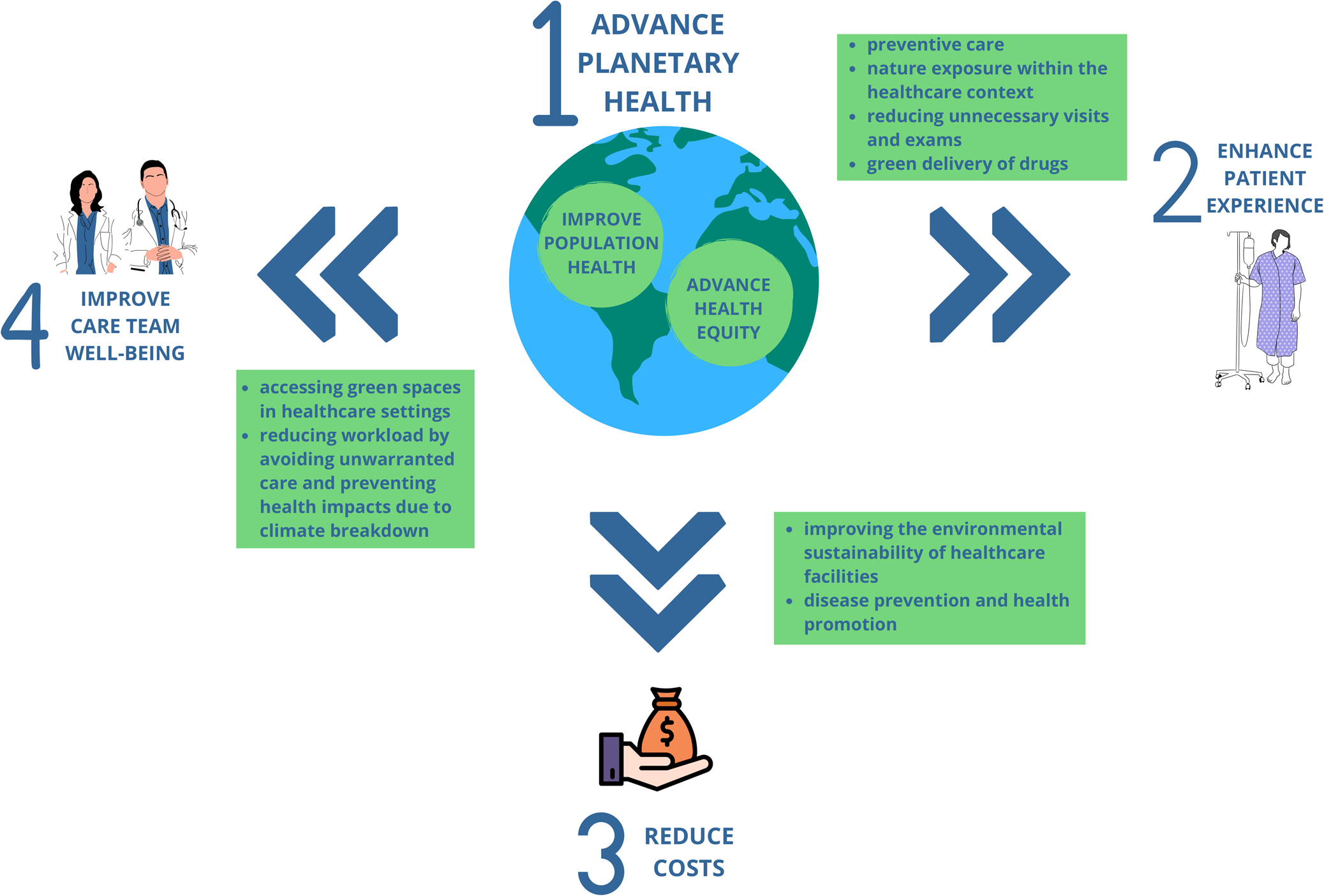
Figure 2. How advancing planetary health contributes to other healthcare improvement aims.
While equity was proposed as an aim for healthcare improvement (Nundy et al., Reference Nundy, Cooper and Mate2022), applying an equity and social justice lens to issues being addressed is a cornerstone of planetary health. This concept was proposed in 2023 by Rockström et al., as a set of safe and just Earth system boundaries (ESBs) (Rockström et al., Reference Rockström, Gupta, Qin, Lade, Abrams, Andersen, Armstrong McKay, Bai, Bala, Bunn, Ciobanu, DeClerck, Ebi, Gifford, Gordon, Hasan, Kanie, Lenton, Loriani and Zhang2023). These boundaries aim to maintain the resilience and stability of the Earth system (safe ESBs) while minimizing human exposure to significant harm from Earth system changes, a necessary but not sufficient condition for justice (Rockström et al., Reference Rockström, Gupta, Qin, Pedde, Broadgate and Warszawski2021). The consideration of health equity is linked to the widespread exposure to significant harm from planetary crises, with greater impacts on vulnerable populations, exacerbating existing inequities in disease burdens and premature mortality, and potentially leading to social unrest (Friel, Reference Friel2022; Intergovernmental Panel on Climate Change (IPCC), 2023). As a matter of fact, the brunt of environmental disruptions is primarily felt by low-income countries and individuals as well as racial minorities, who contribute less to causing them (Deivanayagam et al., Reference Deivanayagam, English, Hickel, Bonifacio, Guinto, Hill, Huq, Issa, Mulindwa, Nagginda, de Sato, Selvarajah, Sharma and Devakumar2023; Gore, Reference Gore2020; Hickel et al., Reference Hickel, O'Neill, Fanning and Zoomkawala2022; Lenton et al., Reference Lenton, Xu, Abrams, Ghadiali, Loriani, Sakschewski, Zimm, Ebi, Dunn, Svenning and Scheffer2023; Vicedo-Cabrera et al., Reference Vicedo-Cabrera, Scovronick, Sera, Royé, Schneider, Tobias, Astrom, Guo, Honda, Hondula, Abrutzky, Tong, de Sousa Zanotti Stagliorio Coelho, Saldiva, Lavigne, Correa, Ortega, Kan, Osorio and Gasparrini2021). A foundation that ensures minimum access to basic needs, including health, for all humans, alongside a safe and just ESB ceiling of maximum allowed human pressure on biophysical domains, could constitute a safe and just ‘corridor’ over time (Rockström et al., Reference Rockström, Gupta, Qin, Lade, Abrams, Andersen, Armstrong McKay, Bai, Bala, Bunn, Ciobanu, DeClerck, Ebi, Gifford, Gordon, Hasan, Kanie, Lenton, Loriani and Zhang2023). Hence, the uneven distribution of the effects of planetary crises calls for just and equitable solutions to advance planetary health.
Planetary health interventions are also associated with cost reduction. Evidence suggests that both improving the environmental sustainability of healthcare facilities and disease prevention and health promotion lead to cost savings (Ashton et al., Reference Ashton, Schröder-Bäck, Clemens, Dyakova, Stielke and Bellis2020; Masters et al., Reference Masters, Anwar, Collins, Cookson and Capewell2017; McCullough, Reference McCullough2018; NHS England and NHS Improvement, 2022; Pisters et al., Reference Pisters, Bien, Dankner, Rubinstein and Sheriff2017; Storz, Reference Storz2020; Sullivan et al., Reference Sullivan, Petit, Reiter, Westrick, Hu, Dunn, Gulack, Shah, Dsida and Raval2023).
In terms of patient experience, several associations are highlighted. Patient experience is associated with preventive care (Doyle et al., Reference Doyle, Lennox and Bell2013) and nature exposure within the healthcare context (Tseung et al., Reference Tseung, Verweel, Harvey, Pauley and Walker2022; Weerasuriya et al., Reference Weerasuriya, Henderson-Wilson and Townsend2018). For example, having access to hospital green spaces significantly improves overall satisfaction with the facility, a sentiment shared by both patients and staff members alike (Kim et al., Reference Kim, Hwang, Lee and Corser2015; O'Hara et al., Reference O'Hara, Miller, Spinks, Seifert, Mills and Tuininga2022; Sadatsafavi et al., Reference Sadatsafavi, Walewski and Taborn2015).
Reducing unnecessary visits and exams and green delivery of drugs also enhance patient experience (El-Hallal et al., Reference El-Hallal, Shah, Nath, Eksambe, Theroux, Amlicke, Steele, Krief and Kothare2021; Kelendar et al., Reference Kelendar, Faisal and Mohammed2020; NHS, n.d.; Rizan et al., Reference Rizan, Das, Low, Harden, Groves, Flaherty, Welland and Bhutta2019). Patients aware of planetary health issues might find comfort in receiving care in facilities transitioning to environmentally sustainable processes.
Pursuing the promotion of planetary health also affects the wellbeing of health professionals. Accessing green spaces and reducing workload by avoiding unwarranted care are suggested as positive drivers of health and wellbeing in the healthcare community (Centre for Sustainable Healthcare, 2020; Marusic, Reference Marusic2023).
The climate breakdown is already impacting health in a myriad of ways, including by leading to death and illness from increasingly frequent extreme weather events, such as heatwaves, storms, and floods, the disruption of food systems, increases in zoonoses and food-, water-, and vector-borne diseases, and mental health issues. Health professionals are at the forefront of responding to these health impacts, and their own wellbeing is also affected by the changing climate. They are exposed to the same health risks as the general population, but they also face additional stressors, such as increased workload, longer working hours, and exposure to traumatic events (Agache et al., Reference Agache, Sampath, Aguilera, Akdis, Akdis, Barry, Bouagnon, Chinthrajah, Collins, Dulitzki, Erny, Gomez, Goshua, Jutel, Kizer, Kline, LaBeaud, Pali-Schöll, Perrett and Nadeau2022). As with patients, professionals with environmental values may find sustainable work practices more rewarding, easing potential discomfort and anxiety generated by the environmental footprint of their working practices. Further links, in this space, can be identified by reviewing the Covid-19 experience. Indeed, Covid-19 is regarded as an Anthropocene disease (O'Callaghan-Gordo & Antó, Reference O'Callaghan-Gordo and Antó2020), spurred by the degraded status of planetary health (Myers & Frumkin, Reference Myers and Frumkin2020). It heavily strained healthcare systems worldwide, with consequences being felt in terms of healthcare professionals' mental health, as well (Aymerich et al., Reference Aymerich, Pedruzo, Pérez, Laborda, Herrero, Blanco, Mancebo, Andrés, Estévez, Fernandez, Salazar de Pablo, Catalan and González-Torres2022; Galanis et al., Reference Galanis, Vraka, Fragkou, Bilali and Kaitelidou2021). Protecting the health of nature and humans through large-scale solutions may help avoid similar disastrous events and their wide-ranging aftermath (Myers & Frumkin, Reference Myers and Frumkin2020).
4. Pathways for health systems to advance planetary health
Aiming to foster planetary health as a health system operationally translates into a series of intertwined pathways (Figure 3).

Figure 3. Main principles and pathways to advancing planetary health as the leading aim for quality improvement in healthcare systems.
With regard to disease prevention and preventable disease burden, enablers can be identified in strong political dedication to public health priorities, effective institutional structures to guide and organize essential public health functions (EPHFs), multisectoral responsibility, assessment of the provision of EPHFs, sufficient workforce and funding (WHO, 2022a, 2022b). Given the increasing urbanization and the need to enhance disease prevention at the city level, political engagement, addressing urban determinants of health, policy debate and institutional reforms are demanded for the shift to health-promoting cities (WHO, 2020).
To increase care appropriateness, active multi-component initiatives proved their effectiveness in reducing unnecessary care (George & Joshi, Reference George and Joshi2022; Rose et al., Reference Rose, Crosbie and Stewart2021). Effective elements, either as single or multi-interventions, include care pathways, educational interventions, organizational culture, audit and feedback and reminders (Pereira et al., Reference Pereira, Silva, Carvalho, Zanghelini and Barreto2022). Policy statements and guidelines from associations, patient and physician education, leadership and peer support feature among the facilitators of the patient–planetary health co-benefit prescribing framework (Redvers et al., Reference Redvers, Wright, Hartmann-Boyce and Tonkin-Crine2023).
Pathways toward decarbonized and low-pollution healthcare broadly encompass green energy supply across both own operations and supply chain, decline in energy demand, professionals' behaviors change, shift to low-impact drugs and devices (Andersen et al., Reference Andersen, Nielsen and Sherman2023; Blom et al., Reference Blom, Eissa, Mattijsen, Sana, Haines and Whitmee2024; Keil et al., Reference Keil, Viere, Helms and Rogowski2023; Pernigotti et al., Reference Pernigotti, Stonham, Panigone, Sandri, Ferri, Unal and Roche2021), sustainable travel, telemedicine, optimal waste management, nature-based solutions, and low-impact food supply chains (Karliner et al., Reference Karliner, Roschnik, Boyd, Ashby and Steele2021; Purohit et al., Reference Purohit, Smith and Hibble2021). Promoting gender balance in healthcare management and leadership generally, reallocating environmentally damaging investments to planetary health solutions (Howard et al., Reference Howard, MacNeill, Hughes, Alqodmani, Charlesworth, de Almeida, Harris, Jochum, Maibach, Maki, McGain, Miller, Nirmala, Pencheon, Robertson, Sherman, Vipond, Yin and Montgomery2023), embedding carbon emissions into existing priority processes (Bhopal & Norheim, Reference Bhopal and Norheim2021), all fall under the scope of returning healthcare to a healthy balance with natural systems. In addition, integrating environmental information into Health Technology Assessment could help refine health system decision making about technologies or interventions. These decisions would be based on data on environmental effects as well as clinical outcomes and costs (Pinho-Gomes et al., Reference Pinho-Gomes, Yoo, Allen, Maiden, Shah and Toolan2022; Toolan et al., Reference Toolan, Walpole, Shah, Kenny, Jónsson, Crabb and Greaves2023).
The advocacy function of health systems spans leading by example through healthcare professionals' individual behaviors, signing treaties promoting the cessation of fossil fuels use and the spread of plant-based diets, the endorsement of institutional and national commitments to achieve net zero emissions in healthcare, including the implementation of procurement policies, of a 100% renewables energy strategy within nations, of ambitious nationally determined contributions complying with the Paris Agreement, of enhanced climate finance (Howard et al., Reference Howard, MacNeill, Hughes, Alqodmani, Charlesworth, de Almeida, Harris, Jochum, Maibach, Maki, McGain, Miller, Nirmala, Pencheon, Robertson, Sherman, Vipond, Yin and Montgomery2023).
The implementation of circular economy (CE) strategies could provide a significant boost toward achieving all four of the described aims (advancing planetary health, enhancing the patient experience of care, reducing costs in the long-term and improving care team well-being), thus playing a central role in improving the quality of healthcare. CE can be described as an economic system that supplants the traditional ‘end-of-life’ concept (‘take-make-waste’) by emphasizing the reduction, reuse, recycling, and recovery of materials throughout the production, distribution, and consumption processes (Kirchherr et al., Reference Kirchherr, Reike and Hekkert2017). The traditional linear model has been shown to be inherently unsustainable because large-scale production and consumption play a significant role in global environmental degradation, producing excess solid waste, greenhouse gases, and other harmful emissions (MacNeill et al., Reference MacNeill, Hopf, Khanuja, Alizamir, Bilec, Eckelman, Hernandez, McGain, Simonsen, Thiel, Young, Lagasse and Sherman2020). These effects threaten public health through air pollution, water and soil contamination, ozone layer depletion, biodiversity loss, and devastating climate change. The CE transformative concept, which strives to eliminate waste through the continual use of resources, is reshaping industries and business models across the board (Sohal & Vass, Reference Sohal and Vass2022), with the healthcare sector being no exception (Kane et al., Reference Kane, Bakker and Balkenende2017). In healthcare, CE is interpreted as an inclusive economic system that adopts the principles of designing out waste and pollution (Lansink, Reference Lansink2018; Stewart & Niero, Reference Stewart and Niero2018), keeping products and materials in use, and regenerating natural systems. These principles permeate all facets of healthcare, from the design and manufacture of medical devices and equipment to the operation of healthcare facilities and the management of health-related waste. A comprehensive and collaborative approach is key in successfully implementing circularity in healthcare. These include end-of-life management (Lansink, Reference Lansink2018), business model innovation (Han et al., Reference Han, Heshmati and Rashidghalam2020), circular product design (MacNeill et al., Reference MacNeill, Hopf, Khanuja, Alizamir, Bilec, Eckelman, Hernandez, McGain, Simonsen, Thiel, Young, Lagasse and Sherman2020), localization of food chains (Health Care Without Harm, 2016), sustainable supply chain practices (United Nations Development Programme, 2020), resource recovery (Stewart & Niero, Reference Stewart and Niero2018), education (Soares et al., Reference Soares, Buttigieg, Couto, Bak, McFadden, Hughes, McClure, Rodrigues and Bravo2023), and collaboration.
5. Conclusion
We argue that shifting to a revised quadruple aim for healthcare improvement, as warranted in the present paper, is quintessential to health systems at the current time. However, while advocacy from health systems may be powerful, the current planetary emergencies are best tackled through shared goals in other adaptive complex systems, such as society, economy, and politics. We assert that advancing planetary health should be at the core of policies that address societal and economic issues (Campbell-Lendrum et al., Reference Campbell-Lendrum, Neville, Schweizer and Neira2023). Framing this with a focus on mutual benefits between sectors may increase feasibility and amplify successes (European Observatory on Health Systems and Policies, 2023; WHO, 2023).
Despite their inner contradictions, the sustainable development goals, along with an economy anchored to a degrowth and post-growth vision, aspiring to wellbeing and sustainable prosperity (Brand-Correa et al., Reference Brand-Correa, Brook, Büchs, Meier, Naik and O'Neill2022; D'Alessandro et al., Reference D'Alessandro, Cieplinski, Distefano and Dittmer2020; Wiedmann et al., Reference Wiedmann, Lenzen, Keyßer and Steinberger2020) – rather than to perpetually inflate gross domestic product – are desirable partners of a renewed health system. Recently, the Covid-19 pandemic reaction illustrated the viability of significant and quick changes that demand the participation of governments, private businesses, civil society, and households (Myers & Frumkin, Reference Myers and Frumkin2020; Ringsmuth et al., Reference Ringsmuth, Otto, van den Hurk, Lahn, Reyer, Carter, Magnuszewski, Monasterolo, Aerts, Benzie, Campiglio, Fronzek, Gaupp, Jarzabek, Klein, Knaepen, Mechler, Mysiak, Sillmann and West2022). Such coordination between systems, on a national and international level, with the shared goal of enhancing planetary health, may lay the foundation of an authentic planetary health system (Prasad, Reference Prasad2023).
Acknowledgments
The authors would like to thank Prof. Samuel S. Myers, Faculty Director of the Planetary Health Alliance and of the Johns Hopkins Institute for Planetary Health, for reviewing the paper and providing his valuable feedback.
Authors contributions
AP conceived and framed the initial idea, reviewed the literature, drafted and revised the paper, and generated figures. AA contributed to framing the initial idea, reviewed the literature, drafted and revised the paper, and generated figures. CC revised the paper and provided oversight of the project. AGdB and WR provided oversight of the project. All authors approved the final version.
Funding statement
This research received no specific grant from any funding agency, commercial, or not-for-profit sectors.
Competing interests
None to be declared.






