Introduction
The global financial crisis that started in 2008 led to a period of economic contraction in many European countries, including Portugal. The economic recession had a severe macroeconomic impact in the country, such as loss of gross domestic product, rising deficit and significant levels of government debt (OECD, 2015). The annual unemployment rate of 16.4% in 2013 was one of the highest in Europe (Eurostat, 2018). In 2011, the Portuguese government signed a financial rescue programme with the European Union, European Central Bank and International Monetary Fund, a group of institutions commonly known as Troika (European Commission, 2014). The agreement imposed austerity measures aiming at the reduction of public expenditure and fiscal consolidation through substantial cuts in public funding, increase in taxes, labour market reforms and restrictions in welfare benefits (Karanikolos et al., Reference Karanikolos, Mladovsky, Cylus, Thomson, Basu, Stuckler, Mackenbach and McKee2013; European Commission, 2014; Zartaloudis, Reference Zartaloudis2014). The Portuguese population suffered a reduction in income, which disproportionately affected the lowest socioeconomic levels, and consequently, the number of people in poverty increased during the recession (Farinha Rodrigues et al., Reference Farinha Rodrigues, Figueiras and Junqueira2016). Despite being deeply affected by the economic recession and subsequent austerity measures, Portugal has received proportionally less attention than its Southern European counterparts regarding the consequences of these measures on health outcomes and social inequalities (Legido-Quigley et al., Reference Legido-Quigley, Karanikolos, Hernandez-Plaza, de Freitas, Bernardo, Padilla, Machado, Diaz-Ordaz, Stuckler and McKee2016).
Research on the mental health consequences of the economic recession has shown its detrimental effect through growing risk factors such as unemployment, financial hardship and precarious job conditions (Marmot et al., Reference Marmot, Bloomer and Goldblatt2013; Frasquilho et al., Reference Frasquilho, Matos, Salonna, Guerreiro, Storti, Gaspar and Caldas-de-almeida2016; Parmar et al., Reference Parmar, Stavropoulou and Ioannidis2016). However, little is known about the impact of this period in individuals with prior mental disorders, which may have been disproportionally affected (Evans-Lacko et al., Reference Evans-Lacko, Knapp, McCrone, Thornicroft and Mojtabai2013). Disparities in the labour market participation between people with and without mental disorders have been documented, due to higher levels of unemployment, sickness absence and early retirement in the first group (Cook, Reference Cook2006; Schofield et al., Reference Schofield, Shrestha, Percival, Passey, Callander and Kelly2011; Knudsen et al., Reference Knudsen, Harvey, Mykletun and Overland2013; Ekberg et al., Reference Ekberg, Wåhlin, Persson, Bernfort and Öberg2015; Lahelma et al., Reference Lahelma, Pietiläinen, Rahkonen and Lallukka2015). Additionally, periods of economic recession can be particularly challenging for individuals with mental disorders due to more competitive labour market conditions and social stigma attached to mental illness (Evans-Lacko et al., Reference Evans-Lacko, Knapp, McCrone, Thornicroft and Mojtabai2013). A study among 27 European Union countries, using data from 2006 and 2010, has shown that the unemployment gap between people with and without mental disorders significantly widened during the economic recession, suggesting that periods of economic recession may intensify the social exclusion of people with mental disorders (Evans-Lacko et al., Reference Evans-Lacko, Knapp, McCrone, Thornicroft and Mojtabai2013).
A dual causal pathway in the association between socioeconomic conditions and mental disorders, where social causation and social selection mechanisms operate concurrently, has been suggested (Saraceno et al., Reference Saraceno, Levav and Kohn2005; Lund et al., Reference Lund, Stansfeld, De Silva, Patel, Minas, Cohen and Prince2014; Elwell-Sutton et al., Reference Elwell-Sutton, Folb, Clark, Fairall, Lund and Bachmann2017). On one hand, studies indicate an association between low socioeconomic status and a higher risk of mental disorders (Fryers et al., Reference Fryers, Melzer and Jenkins2003; Allen et al., Reference Allen, Balfour, Bell and Marmot2014; World Health Organization and Calouste Gulbenkian Foundation, 2014). On the other hand, mental disorders have been associated with adverse economic outcomes such as financial deprivation and job loss, respectively (Kessler et al., Reference Kessler, Heeringa, Lakoma, Petukhova, Rupp, Schoenbaum, Wang and Zaslavsky2008; Lund et al., Reference Lund, Myer, Stein, Williams and Flisher2013; Mojtabai et al., Reference Mojtabai, Stuart, Hwang, Susukida, Eaton, Sampson and Kessler2015). Given that people with mental disorders may have faced wider social inequalities in comparison to the rest of the population, it is important to assess their socioeconomic trajectories during the economic recession.
The aim of the present study is to compare self-reported socioeconomic changes during the economic recession among people with and without 12-month mood or anxiety mental disorders. Three dimensions were assessed in order to capture the changes related to this period, namely employment situation, experiences of financial hardship and modifications in the relative social status an individual perceived to be in comparison to others. It is hypothesised that people diagnosed with any 12-month mental disorder in the beginning of the economic recession were more likely to report negative changes in socioeconomic position, such as becoming unemployed, reporting higher levels of financial hardship and loss of subjective social status.
Methods
Data sources
This study used data from the World Mental Health Survey Initiative (WMHS) Portugal, conducted in 2008/2009 (T 0) and from the National Mental Health Survey Follow-up, conducted in 2015/2016 (T 1).
World Mental Health Initiative Portugal (T 0)
The WMHS was carried out in Portugal in 2008/2009 and was designed to collect epidemiological data on the morbidity of psychiatric conditions, using worldwide standardised methods (Kessler et al., Reference Kessler, Aguilar-Gaxiola, Alonso, Chatterji, Lee, Ormel, Ustün and Wang2011; Caldas-de-Almeida et al., Reference Caldas-de-Almeida, Xavier, Cardoso, Pereira, Gusmão, Corrêa, Gago, Talina and Silva2013; Xavier et al., Reference Xavier, Baptista, Mendes, Magalhães and Caldas-de-Almeida2013).
The study design was based on a stratified multistage clustered area probability household sample and administered to a nationally representative sample of respondents. The participants were Portuguese-speaking adults aged 18 or above, residing in permanent private dwellings in the country's mainland (Xavier et al., Reference Xavier, Baptista, Mendes, Magalhães and Caldas-de-Almeida2013). Informed consent was obtained before the interviews and the procedures were approved by the Ethics Committee of the Nova Medical School (Nova University of Lisbon). The survey was administered by trained lay interviewers with a computer-assisted personal interview on a face-to-face setting. The questionnaire was divided in two parts to reduce respondent burden: part I included core diagnostic assessment of mental disorders (n = 3849). All respondents meeting the criteria for any DSM-IV disorder also completed the part II of the interview, as well as a 25% randomly selected sample of participants who did not meet the criteria for any disorder (n = 2060). Part I data were weighted to adjust differential probabilities of selection, between and within households, non-response bias and discrepancies between the sample and the socio-demographic and geographic data distribution from the census population. Part II was additionally weighted in order to adjust for the differential sampling of part I participants into part II (Xavier et al., Reference Xavier, Baptista, Mendes, Magalhães and Caldas-de-Almeida2013).
National Mental Health Survey Follow-up (T 1)
A follow-up study of the WMHS Portugal was conducted in 2015/2016 in order to compare epidemiological data on mental disorders, socioeconomic conditions and use of services before and after the economic crisis. All procedures were approved by the Ethics Committee of the Nova Medical School (Nova University of Lisbon) and written informed consent was obtained before the interviews. Fieldwork procedures were similar to those of the WMHS Portugal (Xavier et al., Reference Xavier, Baptista, Mendes, Magalhães and Caldas-de-Almeida2013). All individuals with a mental disorder diagnosis and a 20% random sample of those without a diagnosis that had participated in the part II of the survey were recruited to the follow-up survey (n = 911). A new weighting was created based on the part II weight of the previous survey in addition to the differential probability of selection in the follow-up.
Measurements
Twelve-month mental disorders in 2008/2009
The presence of any mental disorder in the last 12 months in T 0 was considered as the independent variable. A dichotomous variable characterised the participants as having or not a 12-month mood or anxiety disorder diagnosis at the onset of the economic crisis. Mental disorders were assessed using the version 3.0 of the World Health Organization Composite International Diagnostic Interview (CIDI), a fully structured diagnostic interview (Kessler and Üstün, Reference Kessler and Üstün2004), which showed good concordance with the Structured Clinical Interview for DSM-IV (SCID) in a clinical reappraisal study (Haro et al., Reference Haro, Arbabzadeh-Bouchez, Brugha, De Girolamo, Guyer, Jin, Lepine, Mazzi, Reneses, Vilagut, Sampson and Kessler2006). The diagnoses were based in the criteria of the American Psychiatric Association's Diagnostic and Statistical Manual Disorders Fourth Edition (DSM-IV) (First and Gibbon, Reference First, Gibbon, Hilsenroth, Segal and Hersen2004) and included anxiety disorders (panic disorder, generalised anxiety disorder, social phobia, specific phobia, agoraphobia without panic disorder, post-traumatic stress disorder, obsessive–compulsive disorder and adult separation anxiety) and mood disorders (major depressive disorder, dysthymia and bipolar disorder, including bipolar I and II).
Changes in socioeconomic status during the economic crisis
Several questions were included in the National Mental Health Survey Follow-up (T 1) in order to capture the changes that occurred during the economic recession. Three dimensions were assessed and considered as dependent variables, namely reported changes in employment situation, financial hardship in the last 5 years and changes in subjective social status.
Employment situation
Employment situation was assessed in T 0 and T 1 and the participants were classified as follows: (1) working; (2) unemployed; (3) retired and ‘others’. The ‘others’ category includes, for example, homemakers and those on sickness absence.
The change in employment situation from T 0 to T 1 was evaluated with a new variable, which considered if the participants reported to be working on both periods or to have become a worker (1); reported to be unemployed on both periods or to have become unemployed (2) and to be retired or ‘others’ on both periods or to have become retired or ‘others’ (3).
Financial hardship during the last 5 years
Financial hardship was assessed through eight questions that evaluated financial difficulties over the last 5 years in the following domains: (1) food; (2) water, electricity or telephone bills; (3) rent; (4) car loan; (5) mortgage; (6) credit card debt; (7) clothing; (8) leisure activities. Response categories were presented through a Likert scale taking the options (1) never, (2) rarely, (3) sometimes and (4) frequently.
In order to reduce the number of variables listed above, Nonlinear Principal Component Analysis (NLPCA) was used. This method has been recommended for categorical variables (Manisera et al., Reference Manisera, Kooij and Dusseldorp2010). Two dimensions were obtained. The first dimension included the following items: food, water, electricity or telephone bills, rent, clothing and leisure activities. This sub-scale was designated as ‘daily life-related financial hardship’ and accounted for 35.9% of the variance in the optimally scaled matrix. The second dimension included the following items: car loan, mortgage and credit card debt. This sub-scale was designated as ‘debts-related financial hardship’ and accounted for 21.7% of the variance. The overall model (both dimensions) accounted for 57.5% of the variance in the optimally scaled matrix. The object scores for each individual were obtained by the component loadings for each dimension. In order to identify the participants with higher levels of financial hardship, the 90th percentile of the distribution was considered as a cut-off point for both sub-scales, indicating the presence of financial hardship.
Changes in subjective social status
Subjective social status was measured in T 0 and T 1 with the MacArthur subjective social status scale, an instrument widely used in epidemiological research that has shown good reliability and validity (Scott et al., Reference Scott, Al-Hamzaw, Andrade, Borges, Caldas-de-Almeida, Fiestas, Gureje, Hu, Karam, Kawakami, Lee, Levinson, Lim, Navarro-Mateu, Okoliyski, Posada-Villa, Torres, Williams, Zakhozha and Kessler2014). The scale consists in a stepladder with rungs numbered from 1 to 10, with the highest value at the top. Participants were asked to consider the ladder as representing the people in Portugal, where those at the top of the ladder would be better off, with most money, education and respected jobs. The answers provided by the participants were categorised as follows: (1) equal or higher social status and (2) lower social status in T 1 compared with T 0.
Covariates
The following baseline variables were considered as covariates: gender, age and presence of any physical disorder. Physical disorders were self-reported through a chronic disorders checklist that has shown good concordance with medical records (Knight et al., Reference Knight, Stewart-Brown and Fletcher2001). Moreover, in order to adjust for differences in socioeconomic position at baseline, as people with low socioeconomic position may be more affected by the negative outcomes of the economic recession (Marmot et al., Reference Marmot, Bloomer and Goldblatt2013), the models were adjusted for educational level, assessed by the number of years of educational attainment as a continuous variable, which is widely used as an indicator of socioeconomic position in epidemiological studies (Galobardes et al., Reference Galobardes, Shaw, Lawlor, Lynch and Davey Smith2006).
Data analysis
Descriptive statistics (frequencies) were carried out for all variables. Logistic regression models were conducted for binary outcomes, namely financial hardship-related daily life (yes/no), financial hardship related to debts (yes/no) and changes in subjective social status (equal or higher v. lower subjective social status). A multinomial regression model was used to evaluate the change in employment situation as the outcome. All models were adjusted for age, gender, education and presence of any physical disorder (T 0). Statistical significance was set at α = 0.05. All data analysis was conducted using Statistical Package for Social Sciences (SPSS) version 22.0 and R version 3.4.2.
Results
Table 1 describes the characteristics of the study population. The number of participants at baseline (T 0) and in the follow-up-study (T 1) was n = 911, from which 19.7% (n = 317) had any 12-month mental disorder before the economic crisis. Women were 50.4% (n = 583) of the participants. The mean age was 45.91(s.d. = 15.73) and the mean number of years of education was 9.22 (s.d. = 4.83) in T 0.
Table 1. Characteristics of the study sample

%, means and standard deviations (s.d.) calculated with weighting from follow-up study (T 1).
Regarding the changes in socioeconomic position, the majority of the participants stayed or became workers (76.1%; n = 540), 7.4% (n = 62) stayed or became unemployed, and 16.5% (n = 147) stayed or became retired or other during the economic recession. Financial hardship, established through the 90th percentile of the distribution as a cut-off point, was found in 9.7% of the participants (n = 115) in relation to daily life, and in 6.4% of the participants (n = 66) in relation to debts. As for perceived social status, 47.3% (n = 433) of the participants reported a lower social status in T 1 in comparison with T 0.
Table 2 presents the results of the multivariate regression models, in the form of odds ratio (OR) and respective confidence intervals (CI).
Table 2. Multivariate models on the association between financial hardship, subjective social position and changes in employment situation and presence of any mental disorder at baseline
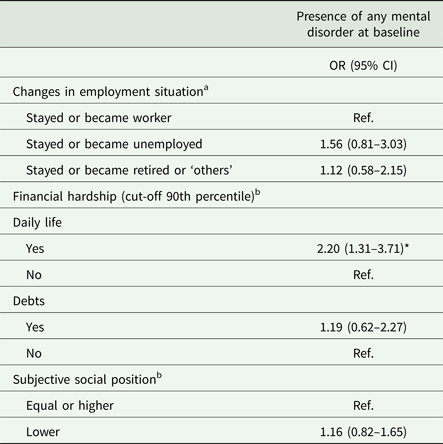
Follow-up weighting (T 1).
All models adjusted for age, gender, education and presence of any physical disorder.
*p < 0.01.
a Multinomial regression model.
b Logistic regression models.
The multinomial regression model presents the associations between the change in employment situation and presence of any 12-month mental disorder in T 0, which were found to be not statistically significant.
The logistic regression models evaluating the association between the two dimensions of financial hardship under study (daily life-related financial hardship and debt-related financial hardship) indicated that participants with any 12-month mental disorder in T 0 had 2.20 (95% CI 1.31–3.71) higher odds of reporting daily life-related financial hardship when compared with individuals without any 12-month mental disorder (P < 0.01). In relation to debt-related financial hardship, the association did not reach statistical significance. Regarding the logistic regression model assessing the changes in subjective social status, the results were also not statistically significant.
Discussion
This study provided an assessment of changes in individual socioeconomic status in the context of economic recession and their association with the presence of a prior mental disorder. As hypothesised, the results suggest that the presence of a 12-month mental disorder at the onset of the economic crisis may have had a negative effect in the socioeconomic position of these individuals. Specifically, people with any 12-month mental disorder at the onset of the economic recession were two times more likely to report daily life-related financial hardship over the previous 5 years, when compared with individuals without any mental disorder. Overall, despite the absence of statistical significance, the findings may suggest a pattern of increased socioeconomic disadvantage among people with any mental disorder at the beginning of the economic recession.
Until now, most research has evaluated the impact of the economic recession on mental health outcomes due to socioeconomic risk factors, such as unemployment, precarious work conditions and financial hardship, as previously referred (Frasquilho et al., Reference Frasquilho, Matos, Salonna, Guerreiro, Storti, Gaspar and Caldas-de-almeida2016; Parmar et al., Reference Parmar, Stavropoulou and Ioannidis2016). However, few studies have assessed the impact of the economic recession on people with previous mental disorders (Evans-Lacko et al., Reference Evans-Lacko, Knapp, McCrone, Thornicroft and Mojtabai2013). Several mechanisms may contribute to an increased vulnerability of this group during a period of economic recession, such as more competitive labour market conditions or stigma and misconceptions related to mental disorders (Evans-Lacko et al., Reference Evans-Lacko, Knapp, McCrone, Thornicroft and Mojtabai2013). For instance, disability has been established as a major consequence of mental disorders, which affects several dimensions of daily life (Alonso et al., Reference Alonso, Angermeyer, Bernert, Bruffaerts, Brugha, Bryson, de Girolamo, Graaf, Demyttenaere, Gasquet, Haro, Katz, Kessler, Kovess, Lépine, Ormel, Polidori, Russo, Vilagut, Almansa, Arbabzadeh-Bouchez, Autonell, Bernal, Buist-Bouwman, Codony, Domingo-Salvany, Ferrer, Joo, Martínez-Alonso, Matschinger, Mazzi, Morgan, Morosini, Palacín, Romera, Taub and Vollebergh2004; Whiteford et al., Reference Whiteford, Degenhardt, Rehm, Baxter, Ferrari, Erskine, Charlson, Norman, Flaxman, Johns, Burstein, Murray and Vos2013). In particular, the consequences of mental disorders on work performance are well established (Alonso et al., Reference Alonso, Petukhova, Vilagut, Chatterji, Heeringa, Üstün, Alhamzawi, Viana, Angermeyer, Bromet, Bruffaerts, de Girolamo, Florescu, Gureje, Haro, Hinkov, Hu, Karam, Kovess, Levinson, Medina-Mora, Nakamura, Ormel, Posada-Villa, Sagar, Scott, Tsang, Williams and Kessler2011; De Graaf et al., Reference De Graaf, Tuithof, Van Dorsselaer and Ten Have2012; Ervasti et al., Reference Ervasti, Vahtera, Pentti, Oksanen, Ahola, Kivimäki and Virtanen2013; Knudsen et al., Reference Knudsen, Harvey, Mykletun and Overland2013; Cardoso et al., Reference Cardoso, Xavier, Vilagut, Petukhova, Alonso, Kessler and Caldas-De-Almeida2017). The inability of people with mental disorders to adjust to a more precarious labour market and stigma from employers may be related with increased difficulties maintaining or finding a job (Evans-Lacko et al., Reference Evans-Lacko, Knapp, McCrone, Thornicroft and Mojtabai2013). For those that had a job, absenteeism and restrictions in the access to sickness absence benefits (Zartaloudis, Reference Zartaloudis2014) may have contributed to loss of income.
The results of this study may suggest that the period of economic recession aggravated the socioeconomic disadvantage of people with mental disorders, particularly regarding the experience of financial hardship. Notwithstanding, it is important to critically reflect upon the results obtained in this study. From the indicators evaluated, a statistically significant association was only found between daily life-related financial hardship and the presence of any mental disorder in T 0. Although the tendency of risk found in relation to other indicators of socioeconomic position being in line with the study's hypothesis and other research (Evans-Lacko et al., Reference Evans-Lacko, Knapp, McCrone, Thornicroft and Mojtabai2013), conclusions must be carefully drawn.
The adverse consequences of the economic recession at the labour market level and wider social inequalities may offset some of the differences between people with and without mental disorders. The findings of this study may also reflect structural characteristics of the context. Portugal has been characterised by a relatively low level of income, alongside one of the highest levels of internal income inequality in the European Union (Carmo et al., Reference Carmo, Carvalho and Cantante2015). Moreover, similar to other Southern European countries, its welfare system provides the smallest public expenditure per capita in social protection in Western Europe, with the benefits’ provision distributed across several schemes and heavily relying on families (Bambra, Reference Bambra2011). This scenario was further aggravated by austerity measures that restricted access and generosity of welfare benefits (Zartaloudis, Reference Zartaloudis2014), which may also have contributed to the findings regarding daily life-related financial hardship.
Further limitations should be acknowledged. First, the results of this study cannot be generalised to the Portuguese population. Second, assessment of indicators may have limited the robustness of the results. Third, the number of individuals in T 1 limited the evaluation of factors such as severity, disability and treatment of the diagnosed mood or anxiety disorders in T 0. Furthermore, it was not possible to obtain information about the illness course, including remission or recurrent episodes, from T 0 to T 1. Related to this limitation, participants with mental health problems in T 1 may be more likely to report negative events, leading to potential recall bias (Prince, Reference Prince, Wright, Stern and Phelan2012). Fourth, the socioeconomic position at baseline is likely to influence the trajectories of the individuals. It has been suggested that the health and economic consequences varied across social groups, affecting disproportionally those already more disadvantaged, which has been established in the Portuguese population (Marmot et al., Reference Marmot, Bloomer and Goldblatt2013; Farinha Rodrigues et al., Reference Farinha Rodrigues, Figueiras and Junqueira2016). The multivariate models were adjusted for the number of years of education at baseline, a reliable indicator of socioeconomic position (Galobardes et al., Reference Galobardes, Shaw, Lawlor, Lynch and Davey Smith2006). However, this may be considered a limitation since some authors argue that social inequalities emerge from a complex process between several indicators, such as education, occupation and income, in specific temporal order, which were not considered in the analysis (Lahelma, Reference Lahelma2004). Fifth, the assessment of employment situation did not allow the inclusion of possible changes such as transition from a full- to a part-time job or temporary work. Moreover, by only comparing the employment situation in T 0 and T 1, fluctuations in employment situation during the two periods were also not evaluated. Finally, the cut-off point for assessing financial hardship on daily life and debts, which was set at the percentile 90th, may have underestimated the presence of financial difficulties in both domains.
In spite of these limitations, to our knowledge, this study is the first to assess how the presence of any mental disorder may have influenced socioeconomic changes during the economic recession, using the same sample of individuals. Furthermore, it provides an innovative contribution to the literature by establishing the presence of any mood or anxiety disorder before the onset of the economic crisis as a predictor of negative socioeconomic changes during this period. Similar to other research (Evans-Lacko et al., Reference Evans-Lacko, Knapp, McCrone, Thornicroft and Mojtabai2013), our findings may suggest that the period of economic recession was particularly challenging for individuals with mental disorders and have intensified their social exclusion. Research should further evaluate the mechanisms associated with the increased vulnerability of people with mental disorders during times of economic recession and its long-term consequences. Access to adequate treatment, social protection measures and alleviation of financial hardship for people with mental disorders comprise some of the policy responses needed during periods of economic crisis to prevent further inequalities. Efforts to target and support people with mental disorders should be a priority in times of economic recession, in order to ensure their fair inclusion in all axes of society.
Acknowledgements
The authors wish to thank the World Mental Health Survey Initiative staff for their assistance with instrumentation, fieldwork and data analysis. A complete list of funding support and publications can be found at: http://www.hcp.med.harvard.edu/wmh.
Financial support
AA receives a grant from the Portuguese Foundation for Science and Technology (FCT) (grant number PD/BD/105822/2014). The Portuguese Mental Health Study was carried out by the Department of Mental Health, NOVA Medical School, NOVA University of Lisbon, with collaboration of the CESOP–Portuguese Catholic University and was funded by the Champalimaud Foundation, the Gulbenkian Foundation, the Foundation for Science and Technology (FCT) and the Ministry of Health. The Portuguese Mental Health Study was carried out in conjunction with the World Health Organization WMH Survey Initiative which is supported by the National Institute of Mental Health (NIMH; R01MH070884), the John D. and Catherine T. MacArthur Foundation, the Pfizer Foundation, the US Public Health Service (R13-MH066849, R01-MH069864 and R01 DA016558), the Fogarty International Center (FIRCA R03-TW006481), the Pan American Health Organization, Eli Lilly and Company, Ortho-McNeil Pharmaceutical, GlaxoSmithKline and Bristol-Myers Squibb. The National Mental Health Survey Follow-up was funded by the Public Health Initiatives Programme (PT06), financed by EEA Grants Financial Mechanism 2009–2014. For further information, please visit http// www.eeagrants.gov.pt/.
Conflict of interest
None.
Ethical standards
The authors assert that all procedures contributing to this work comply with the ethical standards of the relevant national and institutional committees on human experimentation and with the Helsinki Declaration of 1975, as revised in 2008.
Availability of data and materials
The authors do not have permission to share the data of this study.




