Introduction
Although body piercing has historically been associated with risk-taking behaviour it has become a common form of body modification in individuals from a variety of social backgrounds [Reference Carroll1–Reference Forbes4]. A 2008 survey estimated that 10% of the population of England aged 16 and over have at least one body piercing, with nearly 50% of women aged 16–24 having had a piercing at a site other than earlobe [Reference Bone5]. Reasons for adolescents wanting body piercing include uniqueness, self-expression, fashion, curiosity and aesthetic reasons [Reference Armstrong2, Reference Quaranta6–Reference Majori8].
The relationship between body piercing and the transmission of blood-borne viruses is unclear, although a theoretical risk exists. It is a requirement in the UK to wait 4 months after having a body piercing before donating blood and additional checks are undertaken for potential donors having received a body piercing in the previous 4–12 months [9]. There is evidence of an association between body piercing and the transmission of hepatitis B and C [Reference Yang10, Reference Tohme and Holmberg11], although quantifying this risk is difficult as those that choose to have body piercings and tattoos often have other risk factors for blood-borne viruses [Reference Carroll1, Reference Deschesnes, Finès and Demers12, Reference Hwang13]. The potential for transmission of HIV through body piercing is also poorly understood, although a possible case linked to body piercing has been documented [Reference Puhatch, Mileno and Rich14]. Hepatitis B outbreaks had previously been associated with tattooing before stricter legislation was introduced [Reference Limentani15].
In November 2014, several individuals with serious pseudomonas skin infections were admitted to the Royal Gwent Hospital in Newport, South Wales. There were no other links between the cases other than all having received a piercing procedure at the same premises. Environmental Health Officers identified deficiencies in infection control and swabs from two ultrasonic water baths and a washbasin in the treatment area at the premises were found to be positive for Pseudomonas aeruginosa. Following a risk assessment where the UK Advisory Panel for Healthcare Workers Infected with Bloodborne Viruses (UKAP) [16] were consulted, it was agreed to undertake a look-back exercise to offer clients of the premises a test for hepatitis B, hepatitis C and HIV.
Here we characterise a cohort attending a body piercing and tattooing premises in South Wales and assess their health risks. We further investigated age fabrication in younger clients to assess possible barriers to age-based consent, to inform the drafting of legislation to prohibit piercing of intimate body sites in those under 18 years of age.
Methods
Identifying clients at risk
Consent forms were obtained from the piercing and tattooing premises for clients attending the premises between August 2013 and February 2015. These records were entered into an Excel spreadsheet and dates of birth, full names and addresses were checked against the Welsh Demographic Service (WDS) online database and Welsh Patient Administration System (PAS) held by Aneurin Bevan University Health Board. As part of the look-back exercise, client records were assigned a green/amber/red ‘index of certainty’ as a measure of confidence in the validity of the clients’ personal details obtained from the original consent form held by the piercing and tattooing premises. Records were assigned as ‘green’ where there was a match with the client list on full name, address and DOB (excluding year) in WDS, Welsh PAS or both. This was done manually to account for abbreviated or alternative spellings of names. Client records with no potential matches in the Welsh PAS or WDS were assigned as ‘red’ indicating a lack of confidence in the client record. The remaining ‘amber’ client records were examined in more detail and re-classified manually as ‘red’ or ‘green’ on a case-by-case basis. All ‘green’ clients were cross-checked with the clients’ general practice to obtain the most up to date address and ensure there was no clinical or ethical reason why the client should not be contacted. The validated clients resident in Wales were sent a letter inviting them to attend for a blood-borne virus screen. Where the client was under 16 years of age the letter was addressed to a parent/guardian. Social services also looked through the list so that any clients in their care could have their letter delivered by their key social worker. There was a press release and social media activity, asking people to call a helpline if they had attended the premises of interest even if they had not received a letter, as it was considered unlikely that the client list was exhaustive (Fig. 1) [17].
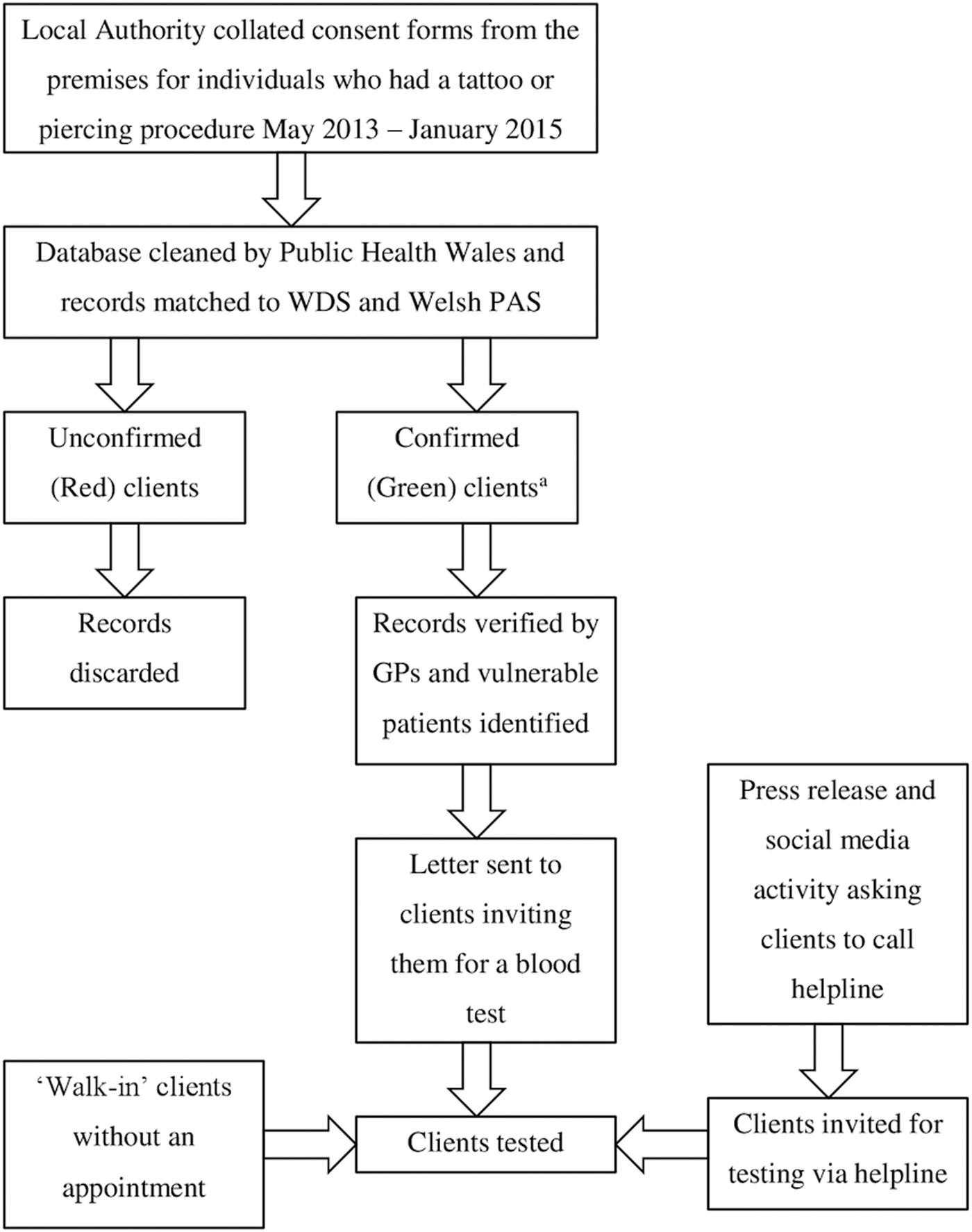
Fig. 1. Processes for identifying clients who had attended a piercing premises with insufficient hygiene practices in South Wales; 2015. aAnalysis of age fabrication was completed using these data.
Prevalence of blood-borne virus
Clients were tested for hepatitis B surface antigen, hepatitis B core antibody, hepatitis C antibody and HIV antibody in an initial blood screen using Architect assay. If the test was confirmed reactive, a further blood test was completed using a combination of enzyme-linked immunosorbent assay and PCR methods to confirm the result. Clients who had a recent procedure at the premises were invited to return at 6 months post exposure to be tested for hepatitis B.
A questionnaire was completed for clients attending for screening by the nurse taking the blood sample. The questionnaire included: ‘source of appointment’, ‘history of testing’ for these three blood-borne viruses and whether or not they have been immunised for hepatitis B. Additional questions on risk factors associated with blood-borne viruses were also asked.
Skin infections associated with piercing
Clients attending for screening were asked to provide a full history of anybody piercing or tattooing procedures in the past 2 years, including ‘date of procedure’, ‘premises location’ and for body piercing, ‘where on the body the piercing was located’. This was followed by the questions ‘Have you had any skin infection following this [piercing\tattoo]?’, ‘If yes, did you contact your GP regarding this complaint?’, and ‘If yes, what did your GP advise?’. Questionnaires were entered into an Epidata (Odense Denmark, EpiData Association) database by two analysts. Differences between the proportion of under 18-year olds and those aged 18 years and over who reported visiting a healthcare professional following infection of their body piercing were compared using a two-sample test for differences between proportions.
Analysis of age fabrication
Data on self-reported age were available from the consent forms collected from the piercing/tattoo premises. The true age of the validated clients was calculated by subtracting true date of birth as recorded in WDS from date of the first recorded visit. The difference between true age and self-reported age at first recorded visit was described. Multivariate logistic regression was performed to determine the influence of age, gender and type of piercing (intimate or non-intimate) on the odds of providing a false age. For the purpose of this analysis, intimate piercing was defined as anus, breast (including the nipple and areola), buttock, natal cleft, penis (including the foreskin), perineum, pubic mound, scrotum, tongue or vulva. All sites are considered intimate, irrespective of gender. All calculations were carried out in Stata 13 (StataCorp LP, College Station, TX).
Ethics
Information in this paper was collected as part of an acute response to a serious public health incident. Research ethics approval was therefore not required.
Results
Description of clients at risk
In total, 1080 clients were identified who had attended the premises of interest for a piercing or tattooing procedure between August 2013 and February 2015. Six hundred and eighty-one (63%) of these were identified following validation of client records, 14 miscellaneous records were added at a later date including four individuals known to the local health protection team prior to the exercise and 333 (31%) were referred following a call to the Public Health Wales (PHW) helpline. Forty-four clients attended a screening session without an invite and source of referral was unknown for eight clients (Table 1).
Table 1. Source of referral for known clients, and the proportion of those who attended for BBV screening, following a look-back exercise at a tattoo and piercing premises with insufficient hygiene practices in South Wales; 2015
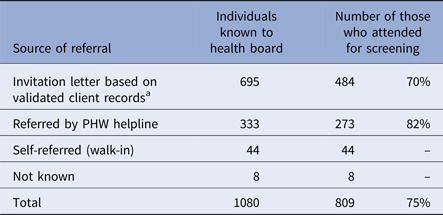
a Includes individuals who did not have a client record but were known to the local authority through a previous complaint.
In total, 809 (75%) clients attended for blood-borne virus screening (Table 1). Seventy-two per cent (581/809) of those attending for screening reported a piercing procedure at the premises of interest. Twenty-six per cent (210) had a tattoo at the premises but no piercing and piercing or tattoo was not recorded for 18 clients (2%) attending for screening. Of the 581 clients who had a body piercing, 511 (88%) were female, 69 (12%) male and gender was unknown for one client. The age of clients ranged from 2 to 52 years. In total, at the time of screening for those who had a body piercing, 94 clients (16%) were under 16 years of age, 264 (45%) were 16 or 17 years of age, 173 (30%) were between 18 and 25 years of age and 48 (8%) were over 25 years of age. Age at time of screening was unknown for two clients. The most common site of piercing was ear (34%), followed by nose (27%), nipple (21%) and navel (21%) (Fig. 2).
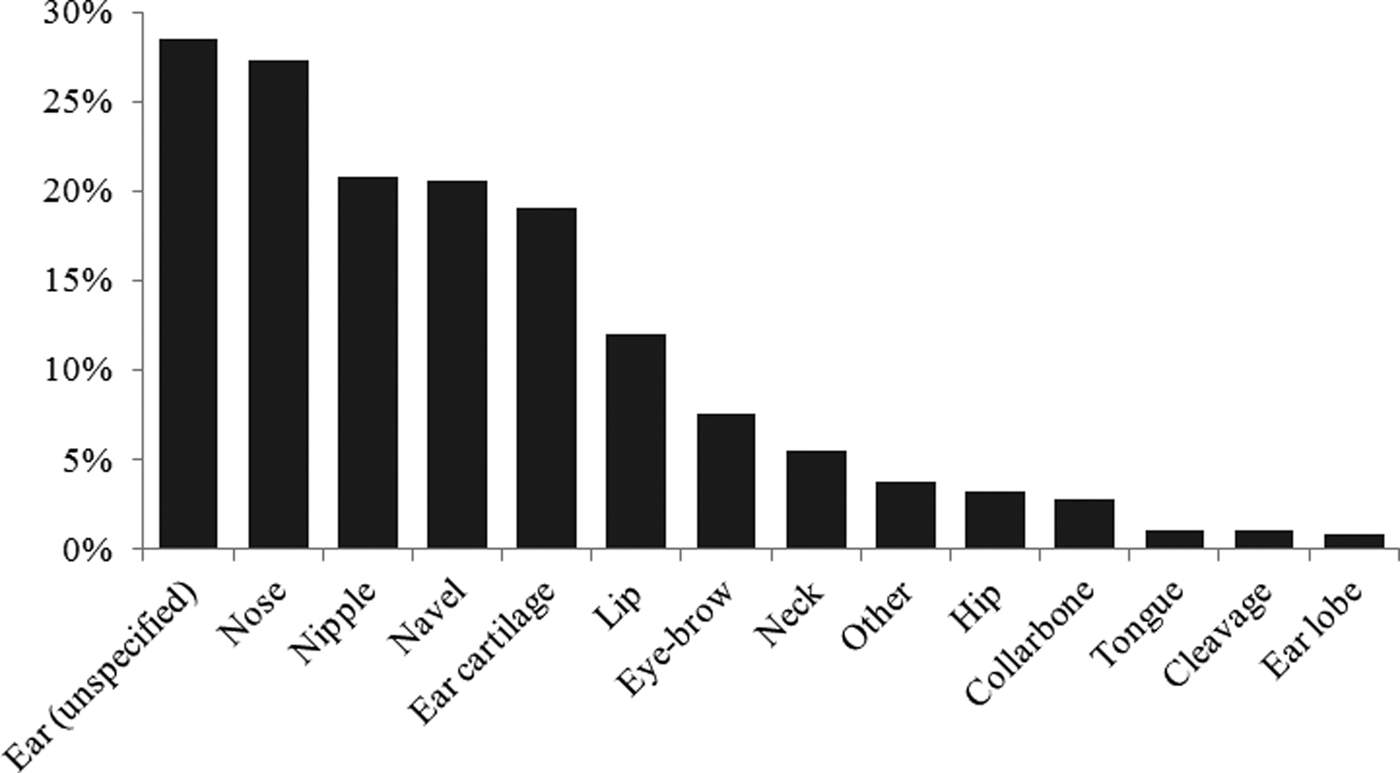
Fig. 2. Frequency of piercing sites in clients who attended a tattoo and piercing premises with insufficient hygiene practices in South Wales; 2015. aOther = Cheek, wrists, rib, back, genital, gum, under eye.
Prevalence of blood-borne viruses
Of those with history of a piercing procedure at the premises five individuals tested positive for hepatitis B core antibody (0.9%, 95% CI 0.3–2.0) one of which was also surface antigen positive (0.2%, 95% CI 0.004–1.0), three clients tested positive for hepatitis C (0.5%, 95% CI 0.1–1.5) and no individuals tested positive for HIV.
Incidence of self-reported skin infection
Of the 579 individuals who answered the question on infection following their piercing procedure, 210 reported a subsequent skin infection, 36.3% (95% CI 32.3–40.3). The proportion of individuals reporting skin infection varied by age group, 28% of those under 16 at the time of screening reported a skin infection following their piercing compared to 38% of those age 16 years and over. Nineteen per cent 40/210 of those with self-reported infection, reported visiting a healthcare professional. Clients aged under 16 years at the time of screening were significantly less likely to seek medical attention following a skin infection (4% compared with 21% of those aged 16 years and over, P = 0.04) (Fig. 3). The type of infection varied from mild irritation to severe hospitalisation. Including the cases that led to the look-back exercise, there were nine hospital admissions in total. All needed incision and drainage and some needed reconstructive surgery. The minimum stay in hospital was three nights and three cases were in hospital for more than ten nights. Seven of the nine cases (78%) were under 18 years of age, seven (78%) had severe infections following an ear cartilage piercing, one (11%) a cheek piercing and one (11%) a nipple piercing.
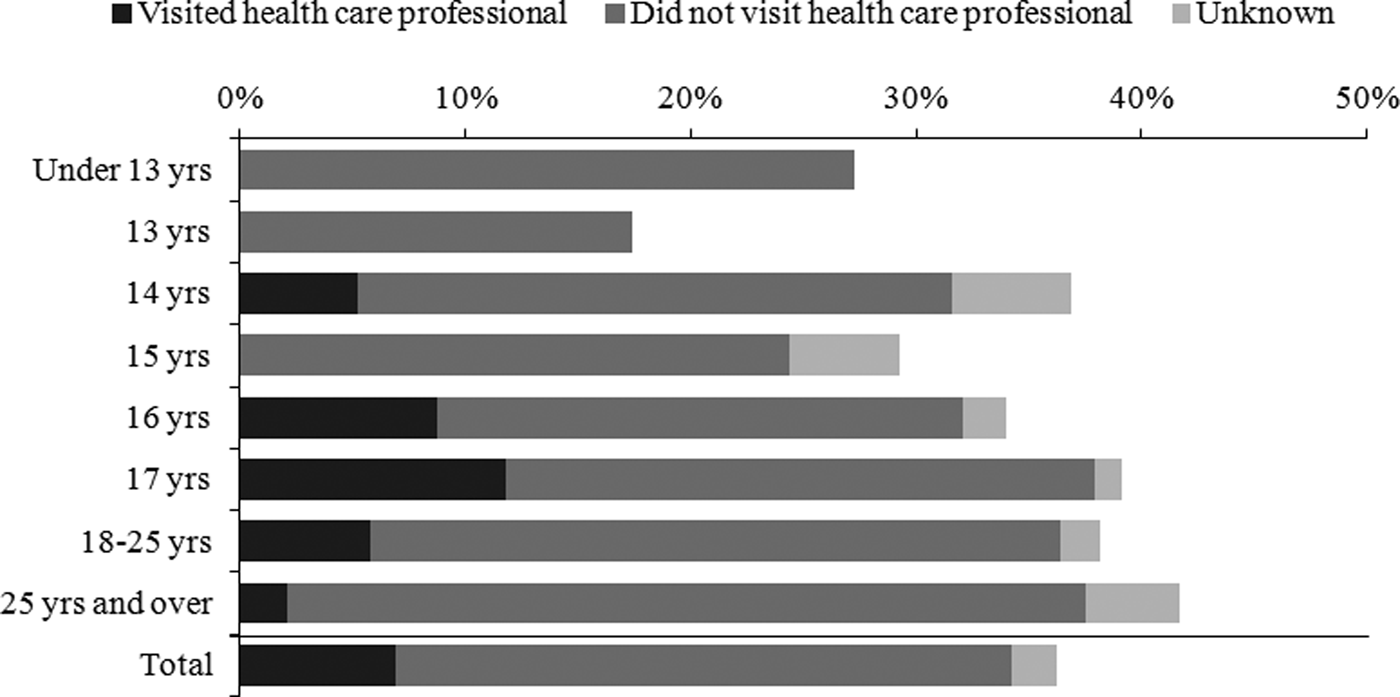
Fig. 3. Frequency of skin infection, by age group, following body piercing in clients who attended a tattoo and piercing premises with insufficient hygiene practices in South Wales; 2015.
Age fabrication
In total, there were 681 individuals identified and validated from client records. Information on piercing procedure at first recorded visit was available for 409/681 (59%). Gender was known for all 409 individuals, 87% (354/409) were female. Information on age at first visit was available for 288 individuals. The modal and median age at first recorded visit was 16 years. Age ranged from 10 to 46 years. In those where age at first visit was known, 77% (221/288) were under 18.
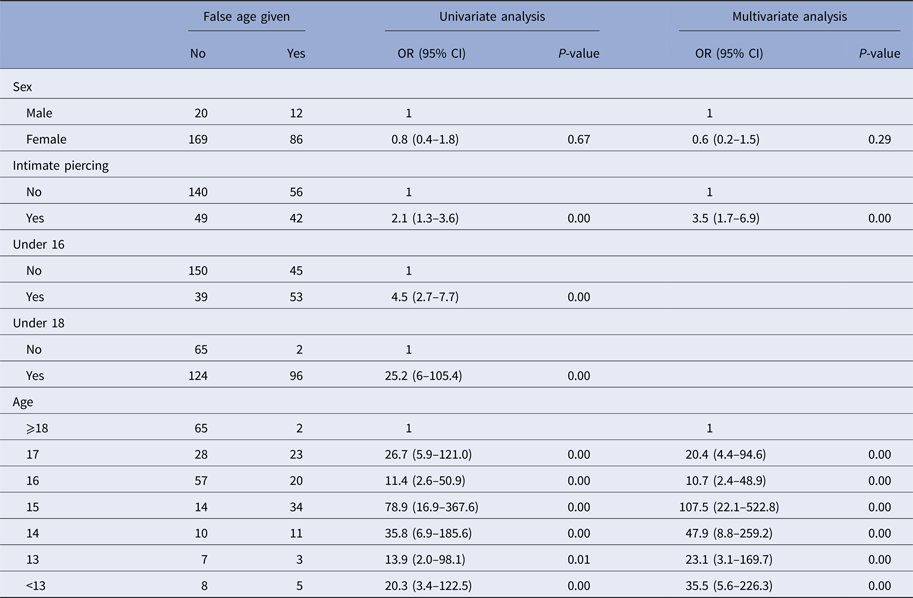
Data on true age at first visit, age given at first recorded visit, gender and piercing site were available for 287 clients. In total, 184/287 (64%) clients gave their correct age at their first recorded visit for a piercing procedure. The proportion of individuals providing a false age varied by age group, 73% (35/48) of 15-year olds provided a false age. In the univariate analysis, individuals were more likely to provide a false age if they had an intimate piercing (OR 2.1, 95% CI 1.3–3.6), were under 16 (OR 4.5, 95% CI 2.7–7.7) or under 18 (OR 25.2, 95% CI 6.0–105.4) (Table 2). Individuals aged 15 years of age were 79 times (95% CI 16.9–367.6) more likely to provide a false age compared with individuals aged 18 years and over. The odds of giving a false age for those aged 15 years increased after controlling for gender and piercing type (OR 107.5, 95% CI 22.1–522.8).
Table 2. Odds of reporting a false age in clients who attended a tattoo and piercing premises with insufficient hygiene practices in South Wales; 2015
Description of piercing sites
Using data from client forms the average number of piercings per visit ranged from 1.0 (under 13-year olds) to 1.3 (15, 16 and over 20-year olds). Piercing site varied with age. Ear cartilage was the most frequent piercing site in most age groups. In those aged under 13 years of age, the most frequently pierced sites were ear and navel. In 13-year olds, it was nose and navel. In 14 and 15-year olds, the sites were more widespread, the most frequently pierced sites were ear and nose. In those aged 16 and 17 years of age, ear and nipple piercing were the most frequent piercing sites (Table 3). For clients where piercing information was known, almost one-third (32%) had an intimate piercing. Seventy-five individuals (34%) under 18 years of age had an intimate piercing.
Table 3. Frequency of piercing site, by age group, in clients who attended a tattoo and piercing premises with insufficient hygiene practices in South Wales; 2015a
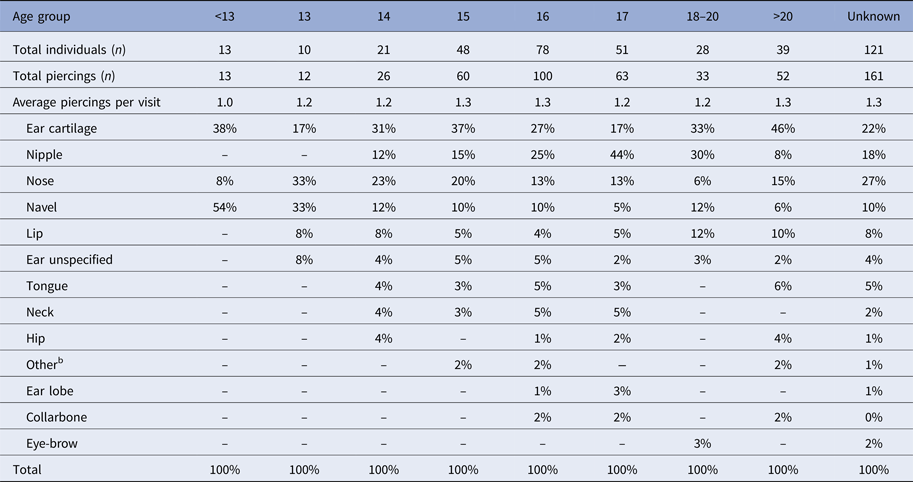
a Data from client lists found at the premises, includes age and piercings received as at first recorded visit. Average is arithmetic mean.
b Other = Cheek, wrist, cleavage, genital.
Discussion
A higher proportion of females attended for body piercing at this premises. These gender differences have been frequently reported in other studies that exclude or include earlobe piercing [Reference Quaranta6, Reference Majori8, Reference Mayers18, Reference Deschesnes, Demers and Finès19]. People of a wide range of ages attended for body piercing and very young children were also taken to have their ears pierced. Piercing sites on the body varied, particularly in those aged 14 and 15 years of age, and approximately one-third of those aged under 18 years of age had a piercing at an intimate site.
A small number of individuals tested positive for hepatitis B and C, it was not known whether these were linked to the premises of interest, as all of these individuals had other risk factors. However, we identified a high level of self-reported skin infection following body piercing.
The increased risk of skin infection following body piercing at this particular premises is difficult to estimate, as there is a lack of data on background incidence of skin infection. There have been a number of studies looking at dermatological complications following body piercing, with frequently reported complications including oedema, bleeding, keloid scarring and infection [Reference Tweeten and Rickman20–Reference Levin and Zadik24]. Perichondritis incidence has increased with increasing popularity of piercing of the upper ear [Reference Rowshan25, Reference Hanif26]. Self-reported history of complications relating to body piercing as reported in cross-sectional studies ranges from 9% to 31%, although rates will inevitably vary depending on how many piercings an individual has had [Reference Bone5, Reference Quaranta6, Reference Mayers18]. Infectious complications may occur due to poor technique or inadequate after care, and depending on the site of the piercing can take many months to heal [Reference Stirn22]. The cluster of pseudomonas skin infections that led to this look-back exercise was identified as all cases were seen at the same hospital in Newport, South Wales. Clusters of pseudomonas skin infection following body piercing have occurred elsewhere. In 2016, a number of pseudomonas skin infections following body piercing in England were linked to a cleansing solution [27]. We recommend that infection following piercing or tattooing should be added to the list of notifiable conditions so that future clusters can be identified more rapidly [28].
We saw the highest rate of self-reported skin infection in those aged over 25 years, but those under 16 years of age were significantly less likely to seek medical advice. Four individuals attending for screening as part of this look-back exercise were referred for further treatment for infected piercings, one of which was advised to go straight to the accident and emergency department. Younger children may be more prone to complications due to being unable to care for their pierced site [Reference Macgregor29]. Body piercing can result in serious complications, reports include a fatal case of toxic shock syndrome as a result of home nipple piercing, Fournier's gangrene leading to septicaemia and DIC following male genital piercing, Ludwig's angina, and a number of reported cases of infective endocarditis following oral piercing [Reference Yu, Minnema and Gold30–Reference Ekelius33]. There is a need for improved regulatory powers for the enforcement of hygiene measures in body piercing premises and for clients of all ages to be better informed on the risks associated with body piercing, including when and where to seek medical advice.
Hygiene practices in the premises were questionable and those attending for screening were aware of this from the publicity of the look-back exercise so may have been more likely to come forward. Individuals were asked whether they recalled having a skin infection following the piercing procedure and interpretation of infection may have varied between clients. Some individuals may have had trauma to the piercing site or a reaction to the materials in the piercing ornament which was recorded as infection, especially if they went on to mention symptoms such as mild irritation. This may have led to an overestimate of skin infection following body piercing at this premises. Detailed descriptions of symptoms were not routinely collected in this study and more work needs to be done to quantify the incidence of skin infection following body piercing in the UK.
There may be bias in the age of those who attended for screening. It has not been possible to compare the age distribution of those attending for screening to the age distribution as at the time of piercing, using data from client forms. This is because the exact date of piercing was not known for all those who attended for screening, the date of body piercing could have been up to 2 years prior to the blood-borne virus screen.
Given the increasing popularity, body piercing represents an emerging public health risk and the need for stricter hygiene and licensing controls in the UK has been discussed for a number of years [Reference Jordan and Finlay34]. Despite there being no legal age limit for body piercing in Wales, we have shown that many individuals were willing to fabricate their age to receive a procedure, even more so if they were requesting an intimate piercing. This could have been due to fear of being turned away, as local councils can issue recommendations on age limits or premises may have their own rules for piercing [Reference Smith35]. Further qualitative work would be necessary to understand younger client's motives for providing a false age. Piercing intimate areas in minors is a safeguarding breach and individuals performing body piercing should be required to hold a licence to ensure they are sufficiently trained. The findings from this exercise were used to support the drafting of the Public Health (Wales) Bill which proposed better regulation of piercing premises and the need to provide documented proof of being over 18 years of age before having a piercing in an intimate site. The Public Health (Wales) Bill, which was passed in July 2017, requires individuals performing body piercing and other special procedures to be licensed and demonstrate knowledge of infection control, hygiene and first aid [36]. In an industry that has been poorly regulated we hope that changes in policy will help protect both the clients and those who perform body piercing.
Acknowledgements
We acknowledge all who contributed to the look-back exercise known as Exercise Seren; Ceri Harris Health Protection Nurse, Kelly Lee Environmental Health Officer, Newport City Council. Mererid Bowley who chaired the Co-ordinating Hub, Lorraine Morgan, Sarah Barnes and members of the Local Public Health team. Peter Carr and Zoe Couzens who directed helpline groups and Wendy Warren who directed the clinical response. Richard Griffiths, Tracey Deacon, Claire Griffiths and Yasmin Smith who helped with the preparation of the technical report and the communications teams from Aneurin Bevan University Health Board, Public Health Wales and Newport City Council. Lisa Chichester directed laboratory work. Nicola Morgan, Daniel Grenyer, Sharon Lord and Cynthia Henderson provided essential guidance on clinical systems, the database, the booking helpline and medical records in addition to the data matching against Welsh PAS. Kimberly Cann and Lorraine Morgan assisted with methods for applying the ‘index of certainty’ to client records.
Author contributions
MP, HL and DT wrote the manuscript. MP and DT performed the analysis. BM and GR provided comments and oversaw the look-back exercise.
Conflicts of interest
None.









